Acute Median Nerve and Flexor Tendon Injury: A Distal Forearm Laceration Case Study
Key Takeaway
An acute distal forearm laceration often presents with profound sensory deficits in the median nerve distribution (thumb, index, middle, radial ring fingers) and specific motor deficits like inability to flex the thumb IP, index/middle DIP joints, or abduct the thumb. Diagnosis involves detailed clinical neurological and musculoskeletal assessment, supported by imaging to rule out fractures or foreign bodies.
Patient Presentation and History
A 32-year-old right-hand dominant male presented to the emergency department trauma bay approximately 2.5 hours after sustaining a sharp laceration to his left volar distal forearm. The mechanism of injury involved an accidental collision with a broken architectural glass pane while the patient was performing extensive home renovations. The patient reported immediate, significant arterial and venous bleeding at the site of the laceration, which was initially controlled by direct, sustained pressure applied by himself and a bystander. Following the cessation of pulsatile bleeding, the patient noted profound numbness radiating into his hand, specifically involving the thumb, index, and middle fingers, accompanied by a complete inability to actively flex these digits.
The patient is a self-employed electrician. This occupational detail highlights the critical importance of bimanual dexterity, fine motor control, and tactile sensibility for his livelihood. The functional demands of his profession require precise manipulation of small-gauge wires, utilization of hand tools, and the ability to work in confined spaces where proprioception and sensory feedback are paramount. Consequently, the potential for long-term disability secondary to a combined neurotendinous injury in the non-dominant hand remains a significant clinical concern that dictates aggressive and meticulous surgical management.
His past medical history was notable for well-controlled essential hypertension, managed effectively with amlodipine 5mg daily. He denied any history of diabetes mellitus, peripheral neuropathy, autoimmune disorders, or congenital coagulopathies. The absence of metabolic or microvascular disease is a favorable prognostic indicator for peripheral nerve regeneration and tendon healing. He was a non-smoker, which further optimizes microcirculatory perfusion to the healing tissues, and consumed alcohol occasionally. There were no known drug allergies. Tetanus immunization status was confirmed to be up-to-date, having received a booster within the last five years.
Upon initial assessment in the emergency department, the patient was hemodynamically stable, afebrile, and alert, though visibly anxious regarding the extent of his injury and its implications for his career. Initial vital signs demonstrated a blood pressure of 135/85 mmHg, a heart rate of 88 beats per minute, a respiratory rate of 16 breaths per minute, and oxygen saturation of 99% on room air. Examination revealed a bulky, blood-soaked circumferential compressive dressing applied by pre-hospital emergency medical services. There was no active strike-through bleeding noted at the time of the initial trauma bay evaluation.
Clinical Examination Findings
Following the administration of adequate systemic analgesia and the removal of the temporary pre-hospital dressing under sterile conditions, a focused, systematic neurovascular and musculoskeletal assessment of the left upper extremity was performed. The examination was conducted in a well-lit trauma bay utilizing a standardized approach to identify the precise anatomical structures compromised within the zone of injury.
Inspection of the Volar Forearm
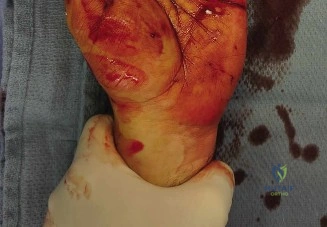
A jagged, approximately 5 cm oblique laceration was present on the volar aspect of the left distal forearm. The wound was positioned just proximal to the distal wrist crease, extending from the radial aspect of the forearm coursing obliquely towards the central volar midline. This anatomical location corresponds to Zone V of the flexor tendon classification system. There was evidence of active, non-pulsatile venous oozing from the wound bed. No obvious skeletal deformity, gross radiocarpal instability, or exposed osseous structures were noted. The overlying skin edges appeared viable, without signs of pallor, cyanosis, or significant avulsion flaps. The resting posture of the hand demonstrated an abnormal cascade; the normal progressive flexion of the digits from the index to the little finger was disrupted. Specifically, the thumb, index, and middle fingers rested in an extended posture relative to the ring and little fingers, immediately raising clinical suspicion for complete disruption of the respective flexor tendons.

Vascular Assessment
Palpation around the wound margins elicited moderate tenderness. Despite the proximity of the laceration to major vascular structures, both the radial and ulnar pulses were strong, bounding, and symmetrically palpable at the wrist compared to the contralateral extremity. An Allen test was attempted but was limited by the patient's inability to actively form a tight fist due to the tendinous deficits; however, digital compression of the ulnar and radial arteries sequentially demonstrated rapid reperfusion of the palmar arch. Capillary refill in the sterile nail beds of all five digits was brisk, estimated at less than 2 seconds. The digits were warm and well-perfused, indicating that the superficial and deep palmar arches remained hemodynamically intact and that the injury did not result in critical limb ischemia.
Musculoskeletal and Tendon Evaluation
A meticulous evaluation of the extrinsic flexor musculature was conducted to isolate individual tendon function.
* Wrist Flexion and Extension: Active range of motion was pain-limited but present for both radiocarpal flexion and extension. The preservation of wrist flexion suggested that the flexor carpi ulnaris (FCU) and potentially the flexor carpi radialis (FCR) remained at least partially intact, though pain inhibited maximal exertion. Passive range of motion was full but elicited significant guarding at the extremes of extension, likely secondary to traction on the transected tendon stumps.
* Thumb Excursion: The patient exhibited a complete inability to actively flex the interphalangeal (IP) joint of the thumb, confirming a complete laceration of the flexor pollicis longus (FPL) tendon. Furthermore, there was a profound inability to abduct the thumb perpendicularly away from the palm (abductor pollicis brevis) or oppose the thumb to the little finger (opponens pollicis), indicating severe median nerve motor compromise.
* Index Finger Excursion: Examination revealed a complete inability to actively flex the distal interphalangeal (DIP) joint while the proximal interphalangeal (PIP) joint was stabilized, indicating a transection of the flexor digitorum profundus (FDP) tendon to the index finger. When the other digits were held in extension to block the deep flexors, the patient demonstrated a complete inability to flex the PIP joint of the index finger, confirming a concomitant laceration of the flexor digitorum superficialis (FDS) tendon to the index finger.
* Middle Finger Excursion: Similar to the index finger, targeted testing demonstrated a complete absence of active flexion at both the DIP and PIP joints, confirming the transection of both the FDP and FDS tendons to the middle finger.
* Ring and Little Finger Excursion: Active flexion of the DIP and PIP joints of the ring and little fingers was intact against mild resistance. This clinical finding suggested the preservation of the ulnar-innervated muscle bellies of the FDP to these digits, as well as their respective FDS tendons, which are anatomically positioned more ulnarly within the distal forearm.
Neurological Assessment of the Upper Extremity
A detailed neurological examination was critical for localizing the nerve injury and establishing a preoperative baseline. The proximity of the laceration to the central volar forearm strongly implicated the median nerve.
* Median Nerve Sensory Function: The patient demonstrated complete anesthesia to light touch, pinprick, and static two-point discrimination over the classic median nerve distribution. This included the palmar aspect of the thumb, index finger, middle finger, and the radial hemi-pulp of the ring finger. Furthermore, sensation was absent on the dorsal aspect of the distal phalanges of the index and middle fingers, corresponding to the terminal sensory branches of the median nerve.
* Median Nerve Motor Function: As noted during the tendon evaluation, there was absent active thumb abduction (abductor pollicis brevis) and opposition (opponens pollicis). The lumbricals to the index and middle fingers were also paralyzed, though this is difficult to isolate clinically in the setting of concurrent FDP/FDS transections.
* Ulnar Nerve Function: Sensory function was completely intact in the ulnar distribution, encompassing the palmar and dorsal aspects of the little finger and the ulnar hemi-pulp of the ring finger. Motor function was similarly preserved, with intact intrinsic muscle function demonstrated by strong finger abduction (dorsal interossei) and adduction (palmar interossei), as well as a negative Froment's sign.
* Radial Nerve Function: Sensation over the dorsal radial aspect of the hand and the anatomical snuffbox was intact. Active extension of the wrist, thumb, and metacarpophalangeal (MCP) joints of all digits was preserved, confirming intact radial nerve motor function.
Imaging and Diagnostics
While the diagnosis of a combined flexor tendon and median nerve laceration in Zone V (often referred to as a "spaghetti wrist" variant, depending on the number of structures involved) is primarily clinical, appropriate imaging and diagnostic adjuncts are mandatory to rule out occult skeletal injuries, retained foreign bodies, and to assist in preoperative planning.
Radiographic Evaluation
Standard orthogonal radiographs of the left forearm and wrist, including anteroposterior (AP), lateral, and oblique views, were obtained in the emergency department. The primary indication for plain radiography in the setting of a glass laceration is the detection of radiopaque foreign bodies. Most modern architectural and automotive glass contains sufficient density to be visualized on standard soft-tissue or bone windows.
The radiographic evaluation revealed no evidence of acute fractures, dislocations, or radiocarpal instability. The osseous structures demonstrated normal trabecular patterns and joint spaces. Crucially, close inspection of the soft tissue shadows adjacent to the volar laceration revealed two small, distinct radiopaque densities measuring approximately 2 mm and 4 mm in maximum diameter, located deep within the volar compartment musculature. These findings confirmed the presence of retained glass fragments, necessitating meticulous intraoperative exploration and fluoroscopic guidance to ensure complete extraction and prevent postoperative foreign body reactions or secondary tendon attrition.
Advanced Imaging Modalities
In the acute setting of an open volar forearm laceration with unequivocal clinical signs of tendon and nerve transection, advanced imaging modalities such as Magnetic Resonance Imaging (MRI) or high-resolution ultrasonography are generally not indicated. The clinical examination provides sufficient diagnostic certainty to proceed with surgical exploration.
However, high-resolution ultrasound can occasionally be utilized in the trauma bay to map the proximal retraction of the transected tendon stumps. In this case, ultrasound was not performed, as the Zone V location typically limits the proximal retraction of the FDS and FDP tendons due to the intact lumbrical origins distally and the constraints of the forearm fascia proximally, unlike Zone II injuries where tendons can retract significantly into the palm. MRI is reserved for chronic or delayed presentations where the exact location of retracted nerve stumps, the presence of neuromas, or the degree of muscle atrophy needs to be assessed prior to secondary reconstruction or tendon transfer procedures.
Laboratory and Preoperative Diagnostics
Routine preoperative laboratory investigations were obtained, including a complete blood count (CBC), basic metabolic panel (BMP), and coagulation profile (PT/INR/aPTT). The results were entirely within normal physiological limits, confirming the absence of underlying coagulopathy or systemic infection. A preoperative electrocardiogram (ECG) was unremarkable, demonstrating normal sinus rhythm. Given the patient's age and lack of significant cardiopulmonary comorbidities, further medical clearance was not required, and the patient was prepared for urgent surgical intervention.
Differential Diagnosis
The presentation of an acute, deep volar forearm laceration with associated motor and sensory deficits necessitates a precise differential diagnosis to ensure all injured structures are identified and managed appropriately. The primary challenge lies in differentiating between isolated tendinous injuries, isolated neurological injuries, and combined neurotendinous injuries, as well as ruling out evolving compartment syndrome.
| Diagnostic Consideration | Clinical Presentation | Examination Findings | Diagnostic Differentiators |
|---|---|---|---|
| Combined Median Nerve and Flexor Tendon Laceration (Zone V) | Acute volar laceration, immediate loss of digit flexion, profound numbness in thumb/index/middle fingers. | Absent FPL, FDP (index/middle), FDS (index/middle) function. Anesthesia in median nerve distribution. Loss of APB/opponens motor function. | The definitive diagnosis for this case. Simultaneous loss of extrinsic flexors and intrinsic median nerve motor/sensory function directly correlating with the anatomical path of the laceration. |
| Isolated Flexor Tendon Lacerations with Compressive Neuropraxia | Volar laceration with loss of digit flexion. Numbness may be present but is often transient or incomplete. | Absent specific tendon function (e.g., FPL, FDP). Sensation may be diminished but not completely absent. Intrinsic motor function (APB) may be weakened due to pain but structurally intact. | Neurological deficits are secondary to hematoma, edema, or traction rather than transection. Serial examinations may show fluctuating sensory findings. Surgical exploration confirms nerve continuity. |
| Anterior Interosseous Nerve (AIN) Transection | Deep penetrating trauma to the proximal/mid forearm. Loss of pinch grip. | Inability to flex thumb IP joint (FPL) and index DIP joint (FDP). Crucially, sensation in the hand is completely normal. Intrinsic median motor function (APB) is intact. | The AIN is a pure motor branch. The presence of profound sensory loss in the median distribution and loss of thenar intrinsic function rules out an isolated AIN injury. |
| Acute Forearm Compartment Syndrome | Severe, disproportionate pain, tense forearm compartments, pain with passive extension of digits. | Pain out of proportion, firm volar compartments, paresthesias (late finding), pulselessness (very late finding). | While trauma can cause compartment syndrome, the immediate onset of specific, isolated motor and sensory deficits corresponding to a laceration path points to direct anatomical transection rather than ischemic neuropraxia. |
Surgical Decision Making and Classification
The clinical diagnosis of a Zone V combined median nerve and multiple flexor tendon laceration constitutes an absolute indication for urgent surgical exploration and primary repair. The goals of surgical intervention are to restore anatomical continuity of the transected structures, maximize the potential for functional recovery, prevent secondary complications such as joint contractures or neuromas, and meticulously remove the radiographically identified retained foreign bodies.
Indications for Urgent Surgical Exploration
Non-operative management has no role in the treatment of complete nerve and tendon transections in the distal forearm. Delaying surgical intervention beyond the acute window (typically 7 to 14 days) results in progressive retraction of the tendon stumps, myostatic contracture of the muscle bellies, and Wallerian degeneration of the distal nerve segment with subsequent endoneurial tube collapse. Early primary repair, ideally performed within the first 48 to 72 hours, facilitates direct end-to-end approximation without undue tension, optimizing the biological environment for healing. In this case, the presence of an open, contaminated wound with retained glass fragments further accelerated the timeline, necessitating urgent irrigation, debridement, and repair to mitigate the risk of deep space infection.
Classification of Flexor Tendon Injuries
The injury is anatomically classified as a Zone V flexor tendon injury. The flexor tendon system is divided into five zones based on the distinct anatomical and biomechanical properties of each region.
* Zone I: Distal to the FDS insertion.
* Zone II: "No Man's Land" - from the A1 pulley to the FDS insertion, where FDS and FDP coexist within a tight fibro-osseous sheath.
* Zone III: Lumbrical origin in the palm.
* Zone IV: Carpal tunnel.
* Zone V: Proximal to the carpal tunnel in the distal forearm.
Injuries in Zone V are frequently associated with major neurovascular compromise due to the superficial and clustered arrangement of the tendons, the median and ulnar nerves, and the radial and ulnar arteries. The prognosis for tendon gliding in Zone V is generally more favorable than in Zone II, as the repairs are not constrained within a rigid synovial sheath, reducing the risk of restrictive peritendinous adhesions. However, the outcomes are often dictated by the success of the concomitant nerve repair, as profound sensory deficits or intrinsic muscle paralysis can severely limit the functional utility of the hand despite excellent tendon excursion.
Preoperative Planning and Consent
Preoperative discussions with the patient were extensive and focused on managing expectations regarding the prolonged recovery trajectory. The patient was informed that while tendon healing typically requires 8 to 12 weeks of structured rehabilitation, nerve regeneration is a significantly slower process, occurring at a rate of approximately 1 mm per day following the initial latent period. Complete sensory recovery is rarely achieved in adult patients sustaining complete median nerve transections, and some degree of permanent tactile deficit or cold intolerance should be anticipated. The surgical consent included exploration of the left forearm, primary repair of multiple flexor tendons (FPL, FDS, FDP), primary neurorrhaphy of the median nerve under microscopic magnification, extraction of foreign bodies, and the potential need for carpal tunnel release if severe swelling dictated prophylactic decompression.
Surgical Technique and Intervention
The patient was transferred to the operating room and positioned supine on the operating table with the left upper extremity extended on a radiolucent hand board.
Patient Positioning and Anesthesia
Given the anticipated length of the procedure and the need for meticulous microsurgical repair, general anesthesia was induced and maintained. While Wide Awake Local Anesthesia No Tourniquet (WALANT) techniques have gained popularity for isolated tendon repairs to allow for intraoperative active motion testing, the complexity of a combined neurotendinous "spaghetti wrist" repair, the need for extensive proximal exploration, and the requirement for absolute immobility during microscopic neurorrhaphy made general anesthesia the preferred modality.
A well-padded pneumatic tourniquet was placed high on the left brachium. The left upper extremity was prepped and draped in a standard sterile fashion. The limb was exsanguinated using an Esmarch bandage, and the tourniquet was inflated to 250 mmHg to provide a bloodless surgical field. Intraoperative prophylactic intravenous antibiotics (Cefazolin 2g) were administered prior to tourniquet inflation.
Surgical Approach and Wound Extension
The initial step involved thorough irrigation of the traumatic wound with copious amounts of sterile normal saline to remove superficial clot and debris. The jagged, 5 cm oblique laceration was then incorporated into a formal surgical approach. To gain adequate exposure of the retracted proximal and distal stumps, the wound was extended proximally and distally using Brunner-type zigzag incisions. This approach prevents the formation of straight-line longitudinal scars crossing the wrist crease, which can lead to debilitating flexion contractures.
The skin and subcutaneous tissues were carefully elevated as full-thickness flaps. The antebrachial fascia was incised longitudinally, revealing a disorganized, hematoma-filled compartment. Meticulous hemostasis was achieved using bipolar electrocautery.
Foreign Body Extraction
Prior to definitive structural repair, intraoperative fluoroscopy (C-arm) was utilized to localize the radiopaque glass fragments identified on preoperative imaging. Careful dissection through the hematoma allowed for the identification and safe extraction of two sharp glass shards embedded deep to the FDS muscle bellies. The wound was re-irrigated to ensure no microscopic particulate matter remained.
Tendon Identification and Repair
The anatomy of the distal volar forearm is complex, and systematic identification of all structures is paramount. The superficial structures were evaluated first. The palmaris longus (PL) tendon was identified and found to be completely transected. The flexor carpi radialis (FCR) and flexor carpi ulnaris (FCU) were inspected and found to be intact, confirming the preoperative clinical assessment.
Attention was then directed to the extrinsic digital flexors. The distal stumps of the transected tendons were identified resting just proximal to the carpal tunnel. The proximal stumps had retracted approximately 3 to 4 cm into the mid-forearm. Each stump was carefully mobilized, and the hematoma within the paratenon was debrided.
To ensure correct anatomical matching, the tendons were identified based on their anatomical layers and distal insertions.
1. Flexor Pollicis Longus (FPL): Located most radially in the deep compartment. Traction on the distal stump confirmed thumb IP flexion.
2. Flexor Digitorum Profundus (FDP): Located in the deep compartment, ulnar to the FPL. The FDP to the index and middle fingers were identified as distinct slips and confirmed by traction resulting in DIP flexion.
3. Flexor Digitorum Superficialis (FDS): Located in the intermediate compartment. The FDS tendons to the middle and ring fingers are anatomically superficial to those of the index and little fingers. The transected slips to the index and middle fingers were identified and confirmed.
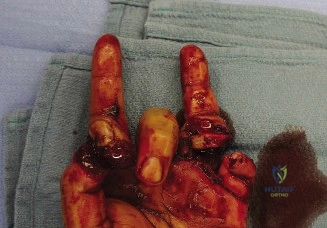
The repairs were performed sequentially, beginning with the deepest structures to avoid compromising completed repairs during subsequent dissection. The FDP tendons to the index and middle fingers were repaired first, followed by the FPL, and finally the FDS tendons to the index and middle fingers.
A robust core suture technique is essential to withstand the forces of early active rehabilitation. A 4-strand modified Kessler core suture using 3-0 non-absorbable braided polyester (Ethibond) was placed in each transected tendon. The core sutures were placed with a slight volar bias to optimize the biomechanical strength and prevent gap formation. Following the core sutures, a running epitendinous repair using 6-0 monofilament polypropylene (Prolene) was performed circumferentially around each repair site. The epitendinous suture significantly increases the ultimate tensile strength of the construct, reduces the cross-sectional area of the repair, and provides a smooth gliding surface, mitigating the risk of peritendinous adhesions. The palmaris longus was not repaired, as its absence does not result in functional deficit and the stump can serve as a potential future graft source if needed.
Median Nerve Exploration and Neurorrhaphy
Following the completion of the tenorrhaphies, attention was directed to the median nerve. The median nerve was found to be completely transected approximately 4 cm proximal to the distal wrist crease. The nerve ends were cleanly lacerated by the glass, with minimal crush component or contusion extending beyond the immediate zone of injury.
The proximal and distal nerve stumps were mobilized gently to allow for a tension-free repair. The operating microscope was brought into the field to facilitate precise fascicular alignment. The epineurium of both stumps was trimmed minimally to expose healthy, pouting fascicles. Proper rotational alignment is critical for functional recovery and was achieved by matching the longitudinal epineurial blood vessels and the distinct fascicular topography. The palmar cutaneous branch of the median nerve, which typically branches radially proximal to the carpal tunnel, was identified and found to be intact.
A primary epineurial repair was performed. Four cardinal sutures of 8-0 nylon were placed in the epineurium at the 12, 3, 6, and 9 o'clock positions to establish alignment. Additional interrupted 8-0 nylon sutures were placed circumferentially to ensure complete coaptation of the nerve ends without excessive tension or buckling of the fascicles. Fibrin glue was not utilized in this case, as the epineurial repair provided excellent structural stability.
Wound Closure and Splinting
Following the completion of all repairs, the tourniquet was deflated. The total tourniquet time was 115 minutes. Hemostasis was meticulously achieved using bipolar electrocautery. The wound was irrigated a final time. The antebrachial fascia was left open to prevent the development of postoperative compartment syndrome. The skin flaps were loosely approximated using interrupted 4-0 nylon sutures. A small Penrose drain was placed deep in the wound bed to prevent hematoma accumulation and was planned for removal on postoperative day one.
Sterile, non-adherent dressings were applied to the wound. A custom-molded fiberglass dorsal blocking splint was fabricated and applied in the operating room. The splint positioned the wrist in 20 degrees of palmar flexion, the metacarpophalangeal (MCP) joints in 70 degrees of flexion, and the interphalangeal (IP) joints in full extension. This specific posture relieves tension on the flexor tendon repairs and the median nerve neurorrhaphy while preventing collateral ligament contractures at the MCP joints.
Post Operative Protocol and Rehabilitation
The success of complex neurotendinous repairs in the distal forearm is highly dependent on a rigorous, structured, and closely monitored postoperative rehabilitation program. The primary challenge is balancing the biomechanical need to protect the fragile tendon and nerve repairs from excessive tension with the biological need to initiate early controlled motion to prevent restrictive peritendinous adhesions and joint contractures.
The patient was admitted overnight for observation, pain management, and elevation of the operative extremity. The Penrose drain was removed on postoperative day one, and the patient was discharged with strict instructions regarding splint wear, elevation, and the avoidance of any active flexion or passive extension of the involved digits.
Early Passive Mobilization Phases (Weeks 1-4)
The patient commenced specialized hand therapy on postoperative day 3. A modified Duran protocol was instituted. The dorsal blocking splint was worn continuously.
* Passive Range of Motion: The patient was instructed to perform passive flexion and active extension of the digits within the confines of the splint. Active extension against the splint allows the extensor mechanism to pull the flexor tendons proximally, promoting intrinsic tendon healing and minimizing adhesions without loading the repair site.
* Synergistic Wrist Motion: By week 2, the therapist introduced controlled synergistic wrist and finger motion. As the wrist is passively extended, the fingers are allowed to passively flex, and as the wrist is passively flexed, the fingers are actively extended. This tenodesis effect maximizes tendon excursion while minimizing active tension.
*
