Acute Flexor Tendon Laceration (FDS/FDP) in Zone II: A Detailed Clinical Case Study
Key Takeaway
Acute FDS and FDP lacerations in Zone II are diagnosed via patient history and detailed clinical examination. Key findings include inability to actively flex PIP/DIP joints, indicating tendon disruption. Neurological assessment is crucial for associated digital nerve injury. Plain radiographs rule out fractures, with advanced imaging reserved for complex cases.
Patient Presentation and History
A 32-year-old right-hand dominant male presented to the emergency department approximately 2 hours after sustaining a deep laceration to the volar aspect of his left middle finger. The mechanism of injury involved a kitchen knife accident while preparing food. He reported immediate severe pain, profuse bleeding, and an inability to bend the affected finger, specifically noting a lack of motion at the middle and distal interphalangeal joints. He applied direct pressure to the wound at home prior to arrival.
His past medical history was unremarkable, with no known chronic illnesses, allergies, or previous surgeries. He denied smoking, illicit drug use, and consumed alcohol socially. He was not on any regular medications. His tetanus immunization status was up to date. He works as an office administrator, making fine motor control and dexterity of his dominant hand crucial for his occupation. The prompt presentation and clear mechanism suggested a high likelihood of significant soft tissue injury requiring urgent assessment.
A critical aspect of the history in flexor tendon injuries is the position of the digit at the exact moment of laceration. Upon further targeted questioning, the patient confirmed that his left middle finger was tightly flexed around a spherical object (an avocado) when the knife slipped and struck the volar surface. This biomechanical detail is paramount; when a flexor tendon is lacerated in a flexed position, the distal stump remains near the laceration site, but the proximal stump retracts significantly proximal to the skin wound once the finger is extended. This discrepancy between the skin laceration and the actual tendon stump location dictates the surgical approach and the extent of proximal exploration required.
Initial emergency department management included copious irrigation of the wound with sterile saline, application of a sterile compressive dressing to manage minor capillary oozing, and the administration of prophylactic intravenous antibiotics (first-generation cephalosporin) to mitigate the risk of deep space infection, particularly given the avascular nature of the flexor tendon sheath which acts as a conduit for rapid proximal bacterial spread.
Clinical Examination Findings
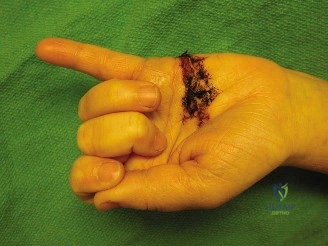
Upon initial inspection, a clean, transverse laceration measuring approximately 2.5 cm was noted on the volar aspect of the left middle finger, overlying the middle phalanx, consistent with Flexor Tendon Zone II. The wound edges were sharp, and there was minimal active bleeding at the time of examination, suggesting the primary injury was a direct cut rather than a crush or avulsion. There was moderate swelling around the wound, but no obvious hematoma or signs of active infection. The finger presented in a relatively extended posture compared to adjacent digits, losing the natural "cascade" of the hand.

Palpation and Vascular Assessment
Tenderness was localized to the laceration site. No crepitus was elicited, and no bony abnormalities were palpable. Distal warmth and capillary refill were brisk (<2 seconds), suggesting adequate macrovascular perfusion. Digital pulses were palpable, and capillary refill was brisk in all digits including the injured middle finger, confirming no significant digital artery transection. An Allen's test was not performed as the primary concern was not main arterial supply compromise to the entire hand, but focused on the affected digit's perfusion.
Range of Motion and Tendon Isolation
- Active ROM:
- The patient was unable to actively flex the left middle finger at the proximal interphalangeal (PIP) joint against resistance, despite attempting to isolate the flexor digitorum superficialis (FDS) by holding the other fingers in full extension. There was a subtle attempt at PIP flexion, but no active motion against gravity or resistance, indicative of FDS disruption.
- When attempting to isolate the flexor digitorum profundus (FDP) by holding the PIP joint in full extension, the patient was unable to actively flex the distal interphalangeal (DIP) joint. This confirmed FDP involvement.
- Active flexion and extension were preserved at the metacarpophalangeal (MCP) joint, suggesting intact extrinsic flexors proximal to the injury site and intrinsic muscle function.
- Full passive ROM was achievable at both the PIP and DIP joints, confirming that joint integrity was preserved and there was no mechanical block.
Neurological Assessment
Light touch and two-point discrimination were assessed on both the radial and ulnar aspects of the middle finger distal to the laceration. Sensation was diminished but not entirely absent along the radial digital nerve distribution, indicating a partial or neuropraxia-level injury, while the ulnar digital nerve sensation appeared intact. Static two-point discrimination on the radial aspect measured 8 mm (abnormal), compared to 4 mm on the ulnar aspect (normal). This suggested a highly probable associated radial digital nerve laceration. Motor function of the ulnar, median, and radial nerves proximal to the hand was assessed and found to be intact.
Based on the clinical findings, the complete inability to actively flex both the PIP and DIP joints against resistance definitively localized the injury to a complete transection of both the FDS and FDP tendons within Zone II. Furthermore, the diminished two-point discrimination strongly indicated a concomitant radial digital nerve injury requiring microsurgical repair.
Imaging and Diagnostics
While the diagnosis of an acute flexor tendon laceration is primarily clinical, radiological assessment remains a mandatory component of the comprehensive trauma workup.
Standard Radiography
Standard posteroanterior (PA), true lateral, and oblique radiographs of the left hand and specifically the left middle finger were obtained. The primary indications for plain film radiography in the setting of a sharp penetrating injury include:
1. Exclusion of Foreign Bodies: Although the patient reported a knife injury, ruling out retained radiopaque foreign bodies (such as metallic shards or glass) is essential before closing the wound or proceeding to the operating room.
2. Assessment of Osseous Integrity: It is imperative to rule out associated phalangeal fractures, cortical nicking by the blade, or bony avulsions. A careful review of the volar aspect of the middle and distal phalanges is required to ensure no occult avulsion fractures (such as a bony Jersey finger variant) complicate the clinical picture.
3. Joint Congruency: Ensuring the PIP and DIP joints are concentrically reduced without evidence of subluxation secondary to volar plate or collateral ligament disruption.
In this patient, the radiographs demonstrated normal osseous architecture, concentrically reduced joints, and no evidence of radiopaque foreign bodies. Soft tissue swelling was noted on the volar aspect of the middle phalanx, correlating with the clinical examination.
Advanced Imaging Considerations
In the acute setting of an open laceration with clear clinical deficits, advanced imaging such as Magnetic Resonance Imaging (MRI) or high-resolution Ultrasound (US) is generally not indicated and unnecessarily delays definitive surgical management.
However, for academic completeness during Grand Rounds, it is worth discussing their utility. High-resolution dynamic ultrasound (using a 15-18 MHz linear transducer) is an excellent, cost-effective modality for assessing tendon continuity, measuring the gap between retracted tendon ends, and evaluating the integrity of the annular pulleys in closed injuries or delayed presentations. MRI, while highly sensitive for soft tissue pathology, is typically reserved for chronic cases where the degree of tendon retraction, muscle belly atrophy, and the viability of the tendon for delayed primary repair versus staged tendon reconstruction (using a Hunter rod) must be meticulously planned. In this acute presentation, the clinical diagnosis was unequivocal, and surgical exploration served as both the definitive diagnostic and therapeutic modality.
Differential Diagnosis
When evaluating a patient with loss of active digit flexion following trauma, the differential diagnosis must encompass various anatomical structures and injury patterns. The following table delineates the primary differentials considered in this case.
| Condition | Clinical Presentation | Imaging Findings | Management Strategy |
|---|---|---|---|
| Complete Zone II Flexor Tendon Laceration (FDS & FDP) | Loss of active PIP and DIP flexion. Loss of normal digital cascade. Palpable gap in tendon sheath possible. Associated digital nerve injury common. | Normal X-rays (usually). US/MRI shows fluid in sheath and discontinuity of both FDS and FDP tendons with gap formation. | Urgent surgical exploration and primary tendon repair (within 7-10 days). Microsurgical nerve repair if indicated. |
| Partial Flexor Tendon Laceration | Pain with active flexion against resistance. Intact but potentially weakened active PIP/DIP flexion. Triggering or catching may occur during motion. | Normal X-rays. US may show partial discontinuity or hematoma within the tendon substance. | Non-operative with protective splinting if <60% cross-sectional area involved. Operative exploration and repair/debridement if >60% or catching occurs. |
| Flexor Digitorum Profundus Avulsion (Jersey Finger) | Inability to actively flex the DIP joint. PIP flexion remains intact. Tenderness along the volar aspect of the digit, potentially retracting into the palm. | X-rays may show a bony avulsion fragment from the volar base of the distal phalanx (Leddy-Packer classification). | Surgical reinsertion of the FDP tendon to the distal phalanx via pull-out suture, suture anchor, or fracture fixation depending on fragment size. |
| Isolated Digital Nerve Laceration | Intact active PIP and DIP flexion. Loss of sensation or abnormal two-point discrimination (>6mm) distal to the laceration site. | Normal X-rays. US may show discontinuity of the digital nerve bundle. | Microsurgical epineurial repair using 8-0 or 9-0 non-absorbable suture under magnification. |
| Extrinsic Flexor Muscle Belly Injury (Forearm) | Weakness or loss of flexion depending on the extent of muscle damage. Injury is proximal to the wrist. Hand cascade may be altered. | Normal hand X-rays. MRI of forearm shows muscle disruption, hematoma, or edema. | Surgical repair of the muscle fascia/epimysium if significant, followed by prolonged immobilization and rehabilitation. |
Surgical Decision Making and Classification
The management of flexor tendon injuries is heavily dictated by the anatomical zone of injury. In 1953, Claude Verdan popularized the division of the flexor tendon system into five distinct zones to guide surgical treatment and prognosis.
Anatomical Classification
This patient's injury occurred in Zone II, which extends from the proximal edge of the A1 pulley (at the level of the distal palmar crease) to the insertion of the FDS on the middle phalanx. Historically, Sterling Bunnell referred to this area as "No Man's Land" because the FDS and FDP tendons are tightly constrained within the fibro-osseous digital sheath. Early attempts at primary repair in this zone frequently resulted in catastrophic adhesions, leading surgeons to favor delayed tendon grafting.
However, modern advancements in suture materials, biomechanical understanding of core suture configurations, atraumatic surgical techniques, and the advent of early active motion rehabilitation protocols have shifted the paradigm. Primary repair within Zone II is now the gold standard and is expected to yield good to excellent functional outcomes when performed by a skilled hand or orthopedic surgeon.
Furthermore, Tang et al. subdivided Zone II into subzones (IIA, IIB, IIC, IID) based on the relationship of the laceration to the Camper chiasm and the specific pulleys involved. A laceration over the middle phalanx typically falls into Zone IIA or IIB, where the FDP tendon lies volar to the FDS slips, or where the FDS decussates. Understanding this intricate anatomy is critical for anatomical restoration during surgery.
Timing of Surgical Intervention
The decision to proceed with operative management was clear given the complete loss of FDS and FDP function. The timing of the surgery is classified as an urgent, primary repair. Primary repair is ideally performed within the first 7 to 10 days post-injury. Delaying beyond this window allows for significant proximal retraction of the tendon stumps, myostatic contracture of the flexor muscle bellies in the forearm, and swelling of the tendon ends, making end-to-end approximation exceedingly difficult and increasing the risk of postoperative rupture due to high tension.
Anesthesia and Patient Positioning Considerations
A crucial decision in modern flexor tendon surgery is the choice of anesthesia. Historically, these procedures were performed under general anesthesia or axillary regional blocks with an upper arm pneumatic tourniquet.
Currently, the Wide Awake Local Anesthesia No Tourniquet (WALANT) technique is increasingly favored for flexor tendon repairs. WALANT utilizes a mixture of lidocaine for anesthesia and epinephrine for hemostasis, injected locally into the hand and digit. The profound advantage of WALANT in Zone II repairs is the ability to communicate with the conscious patient intraoperatively. Once the tendon repair is complete, the surgeon can ask the patient to actively flex and extend the digit. This allows for real-time assessment of the repair construct's strength, direct observation of tendon gliding through the pulleys, and the immediate identification and resolution of any triggering or catching before closing the skin.
For this patient, given the isolated nature of the injury and the patient's cooperative demeanor, the WALANT technique was selected to optimize intraoperative assessment of the tendon glide.
Surgical Technique and Intervention
The patient was brought to the operating room and positioned supine with the left arm extended on a radiolucent hand table.
Anesthesia and Preparation
The WALANT mixture, consisting of 1% lidocaine with 1:100,000 epinephrine buffered with 8.4% sodium bicarbonate (to reduce injection pain), was administered. Approximately 20 cc was injected into the palm proximal to the A1 pulley, and 10 cc was injected along the volar aspect of the middle finger, ensuring complete anesthesia and profound hemostasis. A minimum of 30 minutes was allowed to elapse prior to incision to maximize the vasoconstrictive effect of the epinephrine. The hand was then prepped and draped in a standard sterile fashion.
Surgical Approach and Exposure
The existing 2.5 cm transverse laceration was incorporated into a volar Bruner zigzag incision. Extending the incision proximally and distally via Bruner flaps prevents the formation of linear scar contractures across the flexion creases of the digit.
Upon elevating the skin flaps, the subcutaneous tissues were meticulously dissected. The radial digital nerve was identified and found to be approximately 80% transected, confirming the clinical suspicion of a severe partial laceration. The ulnar digital nerve and both digital arteries were visually inspected and confirmed to be intact.
Attention was then turned to the flexor tendon sheath. The sheath was incised, taking extreme care to preserve the critical annular pulleys. The A2 pulley (located over the proximal phalanx) and the A4 pulley (located over the middle phalanx) are biomechanically vital to prevent tendon bowstringing and must be preserved or reconstructed. In this case, the laceration occurred between the A2 and A4 pulleys, primarily involving the A3 pulley and the cruciform pulleys, which can be vented or excised without significant biomechanical detriment.
Tendon Retrieval and Management
The distal stumps of the FDS and FDP were readily visible within the wound bed. However, as anticipated from the history of a flexion injury, the proximal stumps had retracted proximally into the palm.
To retrieve the proximal stumps, a small transverse counter-incision was made in the distal palmar crease over the A1 pulley. A pediatric feeding catheter was passed retrograde from the digital wound, through the intact A2 pulley, and out the palmar incision. The proximal tendon stumps were identified in the palm. The FDP tendon was temporarily secured to the feeding catheter using a core suture, and the catheter was gently pulled distally, threading the proximal tendon stumps back through the A2 pulley into the primary wound bed. A 25-gauge hypodermic needle was passed transversely through the tendon and the adjacent A2 pulley to temporarily pin the tendon in place, relieving tension and facilitating an atraumatic repair.
Tendon Repair Construct
The biomechanical strength of a flexor tendon repair is directly proportional to the number of core suture strands crossing the repair site. Modern early active motion protocols require a robust repair, typically a 4-strand or 6-strand construct.
For the FDP tendon, a 4-strand modified Kessler core suture technique was utilized using a 3-0 braided non-absorbable suture (FiberWire). The needle was passed meticulously to ensure the suture grasped the volar half of the tendon, preserving the dorsal vascular supply from the vincula. The core stitches were tied with the knots buried within the repair site to minimize friction against the pulleys.
Following the core repair, a continuous epitendinous suture was placed circumferentially around the repair site using a 5-0 monofilament non-absorbable suture (Prolene) in a simple running fashion. The epitendinous suture serves two critical functions: it increases the overall tensile strength of the repair by 20-30%, and it neatly tucks in the exposed collagen fibrils at the tendon ends, creating a smooth surface that minimizes gliding resistance and prevents postoperative adhesions.
The FDS slips were repaired individually using a simpler 2-strand core technique with 4-0 non-absorbable suture, as the primary functional goal is FDP continuity, and an overly bulky FDS repair within Zone II can lead to impingement and stiffness.
Intraoperative Active Testing
With the WALANT anesthesia, the patient was instructed to actively flex and extend the middle finger. The repair was directly visualized. The FDP and FDS tendons glided smoothly through the preserved A2 and A4 pulleys. Full active flexion to the distal palmar crease was achieved without gap formation at the repair site, and full extension was achieved without triggering. This intraoperative validation is the hallmark benefit of the WALANT approach.
Digital Nerve Repair
Following the tendon repair, microsurgical repair of the radial digital nerve was performed. Under operating microscope magnification, the epineurial edges of the partially transected nerve were trimmed to healthy fascicular tissue. An epineurial repair was completed using four interrupted 8-0 nylon sutures, ensuring tension-free coaptation of the fascicles.
Closure
The wound was irrigated with sterile saline. The skin flaps were approximated using 5-0 nylon in a simple interrupted fashion. Deep dermal sutures were strictly avoided to prevent the formation of adhesions between the skin and the underlying repaired tendons. A sterile, non-adherent dressing was applied.
Post Operative Protocol and Rehabilitation
The success of a Zone II flexor tendon repair is arguably 50% dependent on the surgical execution and 50% dependent on the postoperative rehabilitation protocol. The delicate balance between protecting the repair from rupture and applying sufficient mechanical stress to prevent restrictive adhesions requires a rigorous, closely monitored therapy regimen supervised by a Certified Hand Therapist (CHT).
Immobilization Phase (Weeks 0-4)
Immediately postoperatively in the operating room, a custom thermoplastic dorsal blocking splint was fabricated and applied. The splint positioning is critical to relieve tension on the flexor apparatus:
* Wrist: 20 to 30 degrees of palmar flexion.
* Metacarpophalangeal (MCP) Joints: 50 to 70 degrees of flexion.
* Interphalangeal (PIP and DIP) Joints: Full extension (neutral).
Historically, protocols like the Kleinert (active extension against a rubber band, passive flexion) or Duran (strictly passive motion) were utilized. However, given the robust 4-strand core repair reinforced with an epitendinous suture, an Early Active Motion (EAM) protocol, such as the Belfast or Sheffield protocol, was initiated within 3 to 5 days post-surgery.
The EAM protocol involves the patient performing "place-and-hold" exercises. The therapist passively flexes the digits into the palm, and the patient lightly contracts their flexor muscles to actively hold the fist position for a few seconds before actively extending the digits back to the limits of the dorsal blocking splint. This active contraction generates intrinsic tendon healing and creates differential glide between the FDS and FDP tendons, which is essential to prevent cross-adhesions in Zone II.
Intermediate Phase (Weeks 4-6)
At 4 weeks postoperatively, the tensile strength of the healing tendon begins to increase as it enters the fibroblastic and early remodeling phases. The dorsal blocking splint is typically transitioned to a wrist-neutral splint, or discontinued entirely during the day, though night splinting may continue.
Active composite flexion and extension exercises are increased in frequency. Tendon gliding exercises, including hook fist, straight fist, and full composite fist, are emphasized to maximize the differential excursion of the FDS and FDP. Blocking exercises (holding the PIP joint to isolate DIP flexion) are introduced cautiously to specifically target FDP excursion.
Strengthening and Remodeling Phase (Weeks 6-12)
By 6 weeks, the repair is generally strong enough to withstand light resistance. Gentle strengthening exercises, such as using soft therapy putty or light gripping exercises, are initiated. Passive extension stretching is also introduced to address any residual PIP joint flexion contractures, a common complication following volar hand injuries.
At 8 weeks, progressive resistive exercises are advanced. The patient is typically cleared for light functional activities of daily living.
Return to heavy manual labor, contact sports, or activities requiring forceful gripping is strictly prohibited until at least 10 to 12 weeks postoperatively, allowing the tendon collagen to fully remodel and align along the lines of mechanical stress.
Clinical Pearls and Pitfalls
Managing Zone II flexor tendon injuries is fraught with potential complications. A deep understanding of hand biomechanics is required to navigate these pitfalls successfully.
The Quadrigia Effect
The Flexor Digitorum Profundus muscle has a common muscle belly in the proximal forearm that gives rise to the tendons of the middle, ring, and small fingers. Because these tendons act in concert, over-advancing the FDP tendon during repair (typically by more than 1 cm) will artificially shorten that specific tendon. When the patient attempts to make a fist, the shortened repaired tendon reaches maximum excursion early, physically blocking the common muscle belly from contracting further. This prevents the adjacent, uninjured fingers from achieving full flexion—a phenomenon known as the Quadrigia effect. Surgeons must ensure end-to-end repairs without excessive tension or shortening to avoid this debilitating complication.
Lumbrical Plus Finger
The lumbrical muscles originate from the FDP tendons in the palm and insert onto the extensor expansion. If an FDP tendon is lacerated distal to the lumbrical origin (as in this Zone II injury) and the proximal stump retracts, the lumbrical muscle is pulled proximally, increasing its resting tension. If the tendon is not repaired, or if the repair ruptures, subsequent attempts by the patient to actively flex the finger using the FDP will paradoxically transmit force through the tightened lumbrical to the extensor hood. This results in paradoxical extension of the PIP joint when the patient attempts to grip—the classic "Lumbrical Plus" posture.
Adhesions vs. Rupture
The most common complications following flexor tendon repair are adhesion formation (leading to stiffness) and tendon rupture.
* Adhesions: Manifest as a discrepancy between active and passive range of motion (passive ROM is full, active ROM is limited). If adhesions occur, they are initially managed with aggressive hand therapy. Surgical tenolysis (freeing the tendon from scar tissue) should never be performed before 3 to 6 months post-injury, as the tendon needs time to achieve maximal tensile strength, and the scar tissue must mature and soften. Premature tenolysis carries a high risk of iatrogenic tendon rupture.
* Rupture: Typically occurs between days 7 and 21, the phase when the tendon is at its weakest due to inflammatory softening before collagen remodeling provides strength. A rupture presents as a sudden loss of previously present active flexion, often accompanied by a "pop." Unlike adhesions, a suspected rupture demands immediate surgical re-exploration and revision repair.
Tendon Handling and the Epitenon
Flexor tendons must be handled with a strict "no-touch" technique. The epitenon, a thin cellular layer surrounding the tendon, is crucial for intrinsic healing and smooth gliding. Forceps should only be used to grasp the cut ends of the tendon that will be incorporated into the repair. Grasping the lateral aspects of the tendon with toothed forceps creates micro-trauma that serves as a nidus for dense adhesion formation.
Preservation of the Vincula
The flexor tendons receive their blood supply via two mechanisms: diffusion from the synovial fluid within the sheath, and direct vascular perfusion via the vincula (vincula brevia and longa), which are tiny mesenteric folds carrying vessels from the digital arteries. During surgical exploration, aggressive dissection on the dorsal aspect of the tendon must be avoided to preserve these fragile vincula. Disruption of the vincula severely impairs the intrinsic healing capacity of the tendon, increasing the risk of rupture and relying entirely on adhesion-forming extrinsic healing pathways.
