High-Energy Talar Neck Fracture: Diagnostic Insights & Crucial MRI Sagittal Analysis
Key Takeaway
MRI sagittal views are crucial for high-energy talar neck fractures, offering indispensable insights beyond CT. They exquisitely detail soft tissue injuries, including ligamentous integrity (deltoid, calcaneofibular, interosseous talocalcaneal ligaments) and articular cartilage status. This comprehensive assessment aids in surgical planning, prognostication, and evaluating avascular necrosis risk.
Introduction and Epidemiology
High-energy talar neck fractures represent a formidable challenge in orthopedic trauma surgery, demanding a meticulous understanding of hindfoot anatomy, precise diagnostic imaging, and exact surgical execution. The talus is a unique osseous structure, devoid of muscular or tendinous attachments, with approximately sixty percent of its surface area covered by articular cartilage. This anatomical reality makes the talus highly susceptible to avascular necrosis following injury, as its blood supply is inherently tenuous and easily disrupted by fracture displacement.
Talar fractures account for approximately one percent of all fractures and three to six percent of all foot fractures. Of these, talar neck fractures are the most common, comprising roughly fifty percent of all talar injuries. These fractures typically result from high-energy mechanisms, most classically an axial load applied to a dorsiflexed foot, such as in motor vehicle collisions or falls from significant heights. The talar neck is driven against the anterior lip of the tibial plafond, acting as a fulcrum that results in a vertical shear or oblique fracture pattern. Subsequent continuation of the deforming force leads to progressive subluxation or dislocation of the subtalar, talonavicular, and tibiotalar joints, forming the basis of the classic Hawkins classification system. Management of these injuries requires urgent evaluation to mitigate soft tissue compromise, restore articular congruity, and optimize the biological environment for fracture union and revascularization.
Clinical Presentation and Initial Evaluation
A 38-year-old male, generally fit and healthy, presented to the emergency department following a fall from a height of approximately 15 feet while working on a construction site. He landed directly on his feet. He reported immediate, severe pain in his right ankle and foot, rendering him unable to bear weight. He denied any head injury, loss of consciousness, or other significant traumatic injuries. His past medical history was unremarkable, with no known allergies or regular medications. He was a non-smoker and consumed alcohol socially. The mechanism of injury, a high-energy axial load with possible varus or valgus component, immediately raised suspicion for complex intra-articular injuries to the hindfoot or ankle.
Upon arrival, the patient was hemodynamically stable.
- Inspection: The right ankle and foot were markedly swollen and ecchymotic, particularly dorsally and medially. There was a palpable deformity over the midfoot/hindfoot area. Skin integrity was preserved, with no open wounds, significant blistering, or areas of impending skin necrosis observed at initial presentation. However, the skin was tense, indicating significant soft tissue swelling.
- Palpation: Diffuse tenderness was elicited over the anterior ankle joint, talar neck, medial and lateral malleoli, and sinus tarsi. There was significant pain with any attempt to palpate the calcaneus or midfoot. Crepitus was noted with gentle manipulation. The integrity of the deltoid and lateral collateral ligament complexes was difficult to ascertain definitively due to pain and swelling, but gross instability was not appreciated.
- Range of Motion: Actively, the patient was unable to perform any ankle or subtalar motion due to excruciating pain. Passively, gross range of motion was severely limited and painful.
- Neurological Assessment: Sensation to light touch was intact in all major dermatomes (sural, saphenous, superficial peroneal, deep peroneal, medial and lateral plantar nerves). Great toe extension and ankle dorsiflexion/plantarflexion were possible but severely limited by pain.
- Vascular Assessment: Dorsalis pedis and posterior tibial pulses were palpable and strong bilaterally. Capillary refill was brisk in all toes. Compartment pressures were not initially elevated, but the extremity was closely monitored for any signs of developing compartment syndrome given the high-energy mechanism and significant swelling.
- Systemic Assessment: No other obvious injuries were identified on initial secondary survey.
Imaging and Diagnostic Insights
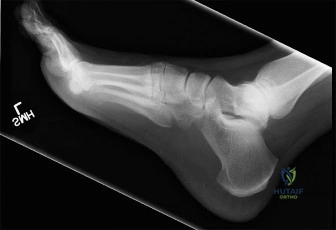
Initial plain radiographs of the right ankle and foot were obtained in the emergency department to establish the baseline skeletal injury pattern.
- Anteroposterior Ankle View: Demonstrated widening of the medial clear space, suggesting a potential deltoid ligament injury or medial malleolar fracture, though a clear fracture line was not visualized.
- Mortise View: Showed subtle widening of the syndesmosis and increased talar tilt.
- Lateral Ankle View: Revealed a comminuted fracture involving the talar neck, with significant displacement and angulation. The fracture line extended into the subtalar joint. There was evidence of dorsomedial displacement of the talar head relative to the body, consistent with a severe talar neck injury. The body of the talus appeared posteriorly displaced and plantarflexed within the ankle mortise.
Given the complex nature of the injury and the significant articular involvement, a Computed Tomography scan of the right ankle and foot was immediately performed for comprehensive characterization of the fracture pattern and surgical planning.
- CT Scan Findings Axial Views: Confirmed a comminuted talar neck fracture with extension into the talar body and significant articular disruption of both the ankle and subtalar joints. Identified multiple small comminuted fragments.
- CT Scan Findings Coronal Views: Provided excellent visualization of the subtalar joint posterior facet, revealing a vertically oriented fracture line with significant articular step-off and impaction of the lateral process.
- CT Scan Findings Sagittal Views: Allowed for precise measurement of the talar neck angulation and the degree of comminution along the inferior neck, which is critical for understanding the risk of varus malunion.
Crucial Magnetic Resonance Imaging Sagittal Analysis
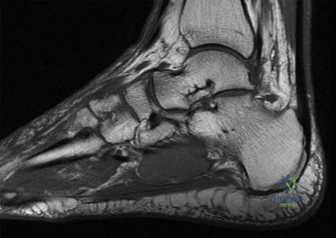
While Computed Tomography remains the gold standard for acute fracture morphology and operative planning, Magnetic Resonance Imaging provides unparalleled diagnostic insights into the soft tissue envelope, ligamentous integrity, and, most importantly, the vascular status of the talar body. In the subacute setting, or when evaluating for delayed complications, sagittal MRI sequences are indispensable.
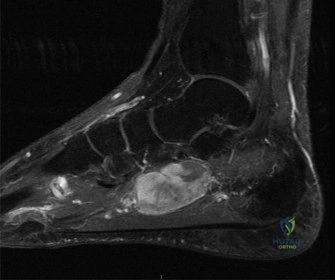
Sagittal T1-weighted images are highly sensitive for evaluating bone marrow signal. Normal fatty marrow exhibits high signal intensity on T1 sequences. Following a high-energy talar neck fracture, a drop in T1 signal within the talar body can indicate an interruption of the intraosseous blood supply. When coupled with Short Tau Inversion Recovery or T2-weighted fat-suppressed sequences, the surgeon can differentiate between transient bone marrow edema (which shows high T2 signal and intermediate T1 signal) and established avascular necrosis (which demonstrates a geographical area of low signal on both T1 and T2 sequences, often bordered by a serpiginous line of sclerosis).
Furthermore, sagittal MRI analysis allows for the detection of occult osteochondral lesions of the talar dome that may not be visualized on standard CT. These lesions, if left untreated, can become a significant source of post-traumatic morbidity. The integrity of the interosseous talocalcaneal ligament and the cervical ligament within the sinus tarsi can also be directly visualized, providing a more comprehensive understanding of the subtalar instability that frequently accompanies Hawkins Type II and III fractures.
Surgical Anatomy and Biomechanics
A profound understanding of talar vascular anatomy is non-negotiable for the orthopedic trauma surgeon. The talus is perfused by an extraosseous anastomotic ring formed by the three major arteries of the lower leg, which then give rise to specific intraosseous networks.
Vascular Supply Networks
The posterior tibial artery provides the most significant contribution via the artery of the tarsal canal. This vessel branches approximately one centimeter proximal to the bifurcation of the medial and lateral plantar arteries, entering the talus inferiorly and supplying the majority of the talar body (the middle and lateral thirds). The deltoid branch, also arising from the posterior tibial artery, supplies the medial third of the talar body. Preservation of the deltoid ligament during surgical exposure is therefore critical to maintaining this vascular lifeline, especially in displaced fractures where other sources are compromised.
The anterior tibial artery continues as the dorsalis pedis, giving off branches to the dorsal talar neck. These vessels supply the head and the dorsal aspect of the neck. The perforating peroneal artery anastomoses with the dorsalis pedis to form the artery of the sinus tarsi, which supplies the anterolateral aspect of the talar body and the lateral process. High-energy talar neck fractures frequently disrupt the artery of the tarsal canal and the intraosseous anastamoses, leaving the talar body entirely dependent on the deltoid branch.
Biomechanical Considerations
Biomechanically, the talus functions as a critical force distributor between the leg and the foot. It dictates the kinematics of the ankle, subtalar, and talonavicular joints. The talar neck is naturally angled medially (approximately 15 to 20 degrees) and plantarward. Comminution typically occurs on the medial and inferior aspects of the neck during axial loading. If this comminution is not anatomically reconstructed, the fracture will collapse into varus and dorsiflexion. A varus malunion alters the biomechanical axis of the hindfoot, locking the transverse tarsal joint, restricting subtalar eversion, and leading to rapid, debilitating post-traumatic arthritis of the hindfoot and midfoot.
Indications and Contraindications
The management of talar neck fractures is dictated by the degree of displacement, the condition of the soft tissue envelope, and the overall physiological status of the patient. Anatomical reduction is the paramount goal to minimize the risk of avascular necrosis and post-traumatic arthritis.
| Management Strategy | Primary Indications | Contraindications and Considerations |
|---|---|---|
| Non-Operative Management | Hawkins Type I fractures (strictly non-displaced on CT scan); Non-ambulatory patients; Severe medical comorbidities precluding anesthesia. | Any displacement (>2mm); Subtalar subluxation; Open fractures; Impending skin necrosis. |
| Urgent Operative Intervention | Open fractures; Fractures with skin tenting or impending necrosis; Irreducible dislocations (e.g., irreducible Hawkins III or IV). | Hemodynamic instability requiring damage control orthopedics (temporize with external fixation). |
| Early Operative Intervention | Hawkins Type II, III, and IV fractures; Displaced Hawkins Type I fractures; Concomitant ipsilateral lower extremity injuries requiring mobilization. | Active soft tissue infection; Unresolving extreme soft tissue swelling (temporize with splint/ex-fix until wrinkle sign appears). |
Pre Operative Planning and Patient Positioning
Pre-operative planning relies heavily on the three-dimensional understanding of the fracture provided by the CT scan. The surgeon must anticipate the need for dual surgical approaches, as a single approach is rarely sufficient to visualize and reduce both the medial and lateral aspects of the talar neck accurately.
The patient is typically positioned supine on a radiolucent operating table. A bump is placed under the ipsilateral hip to internally rotate the leg, bringing the foot into a neutral, upward-facing position. This allows unhindered access to both the medial and lateral aspects of the ankle. A non-sterile thigh tourniquet is applied to provide a bloodless surgical field, which is essential for identifying small articular fragments and preserving the delicate microvasculature.
Fluoroscopy is positioned to enter from the contralateral side of the table. The surgeon must ensure that clear anteroposterior, mortise, lateral, and Canale views can be obtained without obstruction. The Canale view (obtained by maximally plantarflexing the ankle, pronating the foot 15 degrees, and angling the x-ray beam 75 degrees cephalad from the horizontal) is critical for assessing the medial talar neck for varus alignment.
Detailed Surgical Approach and Technique
Surgical management of displaced talar neck fractures almost universally requires a dual-incision technique to ensure anatomic reduction of both cortical cortices and to prevent the dreaded varus malunion.
Anteromedial Approach
The anteromedial approach provides access to the medial talar neck, the medial aspect of the talar body, and the talonavicular joint. The incision is centered between the tibialis anterior and the anterior aspect of the medial malleolus.
The dissection proceeds through the subcutaneous tissues, taking care to identify and retract the saphenous vein and nerve. The extensor retinaculum is incised, and the tibialis anterior tendon is retracted laterally. The capsule of the talonavicular joint and the anterior ankle joint are incised longitudinally. It is imperative to avoid dissecting inferiorly along the medial aspect of the talar body to prevent iatrogenic injury to the deltoid branches of the posterior tibial artery. The fracture site is debrided of hematoma and interposed periosteum using a curette and copious irrigation.
Anterolateral Approach
The anterolateral approach exposes the lateral talar neck, the lateral process, and the anterior aspect of the subtalar joint. The incision is made in line with the fourth ray, extending from the Chaput tubercle of the distal tibia to the base of the fourth metatarsal.
Subcutaneous dissection must carefully identify and protect the branches of the superficial peroneal nerve. The extensor digitorum brevis muscle belly is identified and elevated from its origin on the calcaneus, reflecting it distally. The internervous plane is technically between the peroneal nerve innervated structures and the deep peroneal nerve innervated structures. The capsule of the talonavicular joint and the subtalar joint are exposed. The artery of the sinus tarsi is often already disrupted by the initial trauma, but care should be taken not to extend dissection unnecessarily into the sinus tarsi.
Reduction and Fixation Strategy
Once both approaches are open, the fracture is visualized in its entirety. Medial comminution is frequently observed. Reduction is often facilitated by placing a 2.5 millimeter Schanz pin into the talar head and another into the talar body to act as joysticks. If the talar body is difficult to control, a pin can be placed into the calcaneus to manipulate the subtalar joint.
In cases of severe comminution or impaction, a femoral distractor or a mini-external fixator spanning the medial column (medial cuneiform to the medial malleolus or calcaneus) can be utilized to restore length and correct varus deformity. The fracture is provisionally stabilized with multiple 1.6 millimeter or 2.0 millimeter Kirschner wires.

Fixation is typically achieved using headless compression screws or countersunk cortical screws. Biomechanical studies suggest that posterior-to-anterior screw trajectory provides superior biomechanical stability; however, this requires a separate posterolateral approach and is technically demanding. Therefore, anterior-to-posterior screw placement is most commonly utilized.
Screws must be placed outside the articular cartilage whenever possible, or countersunk below the cartilage surface if articular placement is unavoidable. Typically, two or three screws are required. If there is significant medial comminution that cannot be bridged with lag screws, a small low-profile neutralization plate (such as a 2.0 millimeter or 2.4 millimeter mini-fragment plate) should be applied to the medial talar neck to act as a buttress against varus collapse. Fluoroscopic evaluation, particularly the Canale view, is essential prior to final closure to confirm anatomic alignment and appropriate hardware placement.
Complications and Management
The complication profile for high-energy talar neck fractures is significant, directly correlating with the initial energy of the injury and the quality of the surgical reduction.
| Complication | Estimated Incidence | Pathophysiology and Clinical Presentation | Salvage and Management Strategies |
|---|---|---|---|
| Avascular Necrosis | Hawkins I: 0-13%; Hawkins II: 20-50%; Hawkins III: 50-100%; Hawkins IV: ~100% | Disruption of intraosseous and extraosseous blood supply. Presents as sclerosis on radiographs. | Protected weight-bearing. If collapse occurs: Blair fusion, tibiotalocalcaneal (TTC) arthrodesis, or total talus replacement. |
| Post-Traumatic Arthritis | 40-90% (Subtalar joint most common) | Initial chondral injury at impact, or altered biomechanics from imperfect reduction. Presents as chronic pain and stiffness. | Conservative: Bracing, injections. Surgical: Subtalar arthrodesis, triple arthrodesis, or pantalar arthrodesis depending on joint involvement. |
| Varus Malunion | 10-30% | Failure to recognize or stabilize medial neck comminution. Results in locked transverse tarsal joint and lateral foot overload. | Medial opening wedge osteotomy of the talar neck (if joints preserved) or corrective triple arthrodesis. |
| Nonunion | 2-10% | Poor biological environment, inadequate mechanical stability, or infection. | Revision open reduction internal fixation with autologous bone grafting. |
| Infection | 5-15% (Higher in open fractures) | Compromised soft tissue envelope. Presents with erythema, drainage, and elevated inflammatory markers. | Aggressive surgical debridement, hardware removal if loose, targeted intravenous antibiotics, and soft tissue coverage flaps if necessary. |
A critical radiographic marker in the postoperative period is the Hawkins sign. This is a subchondral radiolucent band visible on the AP or mortise radiograph of the ankle, typically appearing six to eight weeks post-injury. The presence of the Hawkins sign indicates subchondral osteopenia secondary to active hyperemia, confirming that the talar body has maintained or regained its vascular supply. Conversely, the absence of a Hawkins sign suggests, but does not definitively prove, the development of avascular necrosis.
When avascular necrosis leads to structural collapse of the talar dome, salvage procedures become necessary. The Blair tibiotalar arthrodesis involves a sliding anterior tibial bone graft placed into the talar neck, bypassing the necrotic body. More contemporary approaches utilize a retrograde intramedullary nail for a tibiotalocalcaneal arthrodesis, often requiring structural allograft or a femoral head allograft to restore height if the talar body must be completely excised. Recently, custom 3D-printed total talus replacements have emerged as a viable joint-sparing salvage option for complete talar collapse.
Post Operative Rehabilitation Protocols
The postoperative rehabilitation protocol must balance the need for early joint mobilization to prevent stiffness with the absolute requirement to protect the tenuous fixation and allow for revascularization.
Immediately postoperatively, the patient is placed in a well-padded short leg splint in neutral dorsiflexion. The patient is made strictly non-weight-bearing on the operative extremity. Elevation and strict edema control are paramount during the first two weeks.
At the two-week follow-up, sutures are removed, and the patient is transitioned to a removable controlled ankle motion boot. Active and active-assisted range of motion exercises for the ankle and subtalar joints are initiated. Passive stretching is generally avoided initially to prevent undue stress on the fracture site. The patient remains strictly non-weight-bearing.
Radiographic evaluation is performed at six to eight weeks to assess for the presence of the Hawkins sign and to monitor fracture consolidation. If clinical and radiographic signs of healing are progressing appropriately, the patient may begin a graduated weight-bearing protocol in the boot, typically starting at twenty-five percent body weight and advancing over the subsequent four to six weeks. Full weight-bearing without the boot is rarely permitted before twelve weeks postoperatively, and often longer in cases of severe comminution or delayed union. Return to high-impact activities or heavy manual labor may take up to a year, and patients must be counseled that some degree of permanent stiffness and residual pain is common.
Summary of Key Literature and Guidelines
The foundational understanding of talar neck fractures stems from L.G. Hawkins' seminal 1970 paper, which classified these injuries based on the degree of displacement and correlated the fracture pattern with the subsequent risk of avascular necrosis. This classification remains the cornerstone of clinical communication and prognostic expectation today.
Subsequent literature has heavily focused on surgical approach and reduction techniques. Vallier et al. have published extensively on the necessity of dual surgical approaches. Their work demonstrated that relying solely on a medial or lateral approach frequently results in unrecognized malreduction of the opposite cortex, leading to the high rates of varus malunion seen in historical cohorts. They advocate for the routine use of both anteromedial and anterolateral incisions to visualize the entire talar neck.
Biomechanical studies by Halvorson and others have investigated optimal fixation constructs. While posterior-to-anterior screw placement offers superior compressive forces and pull-out strength due to engagement of the denser bone of the talar head, the anterior-to-posterior technique remains the standard of care due to its lower risk profile and technical feasibility. The literature strongly supports the addition of medial plating in the presence of medial comminution to prevent late varus collapse, a concept that has significantly reduced the incidence of malunion in modern trauma centers.
Finally, the management of avascular necrosis continues to evolve. Sanders et al. provided critical long-term outcome data on operative management, noting that even with anatomic reduction, the rate of post-traumatic subtalar arthritis remains exceedingly high. Current guidelines emphasize that while anatomic reduction minimizes the risk of AVN, it does not eliminate it, and surgeons must maintain a high index of suspicion and a low threshold for advanced imaging (MRI) if patients develop late-onset pain or radiographic sclerosis.
