Complex Ankle Fracture Case Study: PER Stage IV & Posterior Malleolus Management
Key Takeaway
A complex ankle fracture, such as a PER Stage IV or AO/OTA 44-C3 variant, involves multi-ligamentous and multi-bony injuries, often including syndesmotic disruption and significant posterior malleolar fragments. Diagnosis relies on detailed clinical examination, standard X-rays (AP, mortise, lateral), and crucially, CT imaging for precise assessment of fracture patterns, articular involvement, and pre-operative planning.
Patient Presentation and History
Mechanism of Injury and Demographics
A 48-year-old male construction worker presented to the Level I trauma center emergency department following a high-energy fall from a height of approximately 10 feet. The mechanism of injury involved a direct axial load combined with a rotational vector upon landing primarily on the left foot. The patient reported immediate, severe, and incapacitating pain in the left ankle, accompanied by an absolute inability to bear weight and rapid, progressive localized edema. Secondary survey was negative for concomitant injuries; the patient denied head trauma, loss of consciousness, axial spine pain, or other appendicular skeletal trauma.
The mechanism of injury is highly consistent with a complex rotational ankle fracture, specifically involving a pronated foot subjected to an external rotation force. The addition of the axial load from a 10-foot fall significantly increases the risk of articular impaction, particularly at the posterior tibial plafond, elevating this from a standard rotational ankle fracture to a high-energy pilon-variant injury.
Comorbidities and Risk Stratification
The patient’s past medical history is significant for Type 2 Diabetes Mellitus, diagnosed five years prior and currently managed with oral hypoglycemic agents. He also has a 20-pack-year smoking history, currently consuming half a pack per day. Social history includes active employment in physically demanding labor and regular daily alcohol consumption of 2 to 3 units.
From an orthopedic trauma perspective, this comorbidity profile presents substantial perioperative challenges. Diabetes mellitus, even when ostensibly well-controlled, introduces microvascular compromise and altered cellular responses that significantly elevate the risk of surgical site infection, wound dehiscence, and delayed union or nonunion. The presence of advanced glycation end-products alters collagen cross-linking, compromising the mechanical integrity of the healing soft tissue envelope.
Concurrently, the patient's active tobacco use introduces nicotine-induced vasoconstriction, cellular hypoxia, and carbon monoxide-mediated competitive inhibition of oxyhemoglobin binding. This synergistic compromise of the microcirculation demands meticulous soft tissue handling, potential delays in definitive surgical intervention to allow for soft tissue resuscitation, and a highly rigid fixation construct to mitigate the elevated risk of nonunion.
Clinical Examination Findings
Visual Inspection and Soft Tissue Envelope
Upon initial assessment in the trauma bay, the patient was alert, oriented, and hemodynamically stable. Visual inspection of the left lower extremity revealed marked, circumferential edema extending from the midfoot to the proximal third of the leg. Significant ecchymosis was present, predominantly distributed over the medial and lateral malleoli, tracking proximally along the fibular shaft.
The soft tissue envelope was critically compromised. The skin was taut and glossy, with loss of normal skin lines. Early fracture blisters, predominantly clear-fluid filled, were developing over the lateral malleolus, indicating a Tscherne Grade II closed soft tissue injury. There was no gross angular deformity, open wounds, or evidence of skin tenting that would necessitate emergent reduction to prevent impending necrosis. However, the severity of the edema dictated that immediate definitive internal fixation was contraindicated due to the unacceptable risk of wound breakdown.
Palpation and Provocative Testing
Palpation elicited exquisite, diffuse tenderness circumferentially around the ankle mortise. Point tenderness was maximal over the distal fibula, the medial malleolus, and deeply along the posterior aspect of the distal tibia. Crepitus and gross instability were readily appreciated with minimal manipulation.
Crucially, palpation of the proximal fibula and fibular head yielded no tenderness, effectively ruling out a classic Maisonneuve fracture pattern. The entire tibial shaft was non-tender. Examination of the foot revealed no tenderness over the base of the fifth metatarsal, the Lisfranc joint complex, or the navicular, reducing the likelihood of associated midfoot or forefoot injuries. Provocative syndesmotic testing, such as the external rotation stress test or the squeeze test, was deferred acutely due to the obvious clinical and radiographic instability, as such maneuvers would inflict unnecessary pain without altering the immediate management algorithm.
Neurological and Vascular Assessment
Neurological examination demonstrated intact sensation to light touch across all major dermatomal distributions of the foot and ankle, including the superficial peroneal, deep peroneal, sural, saphenous, and tibial nerves. Motor function was assessed indirectly due to pain-limited excursion; the patient demonstrated the ability to recruit the extensor hallucis longus, tibialis anterior, and gastrocnemius-soleus complex, confirming gross continuity of the major motor units.
Vascular assessment revealed palpable and symmetric dorsalis pedis and posterior tibial pulses, graded as 2+ bilaterally. Capillary refill at the distal tufts of the toes was brisk, occurring in under two seconds. The foot remained warm and well-perfused. While there were no immediate clinical signs of acute compartment syndrome of the leg or foot, the high-energy nature of the axial load and the rapidly progressive edema necessitated vigilant serial examinations and a low threshold for intracompartmental pressure monitoring.
Imaging and Diagnostics
Initial Radiographic Evaluation
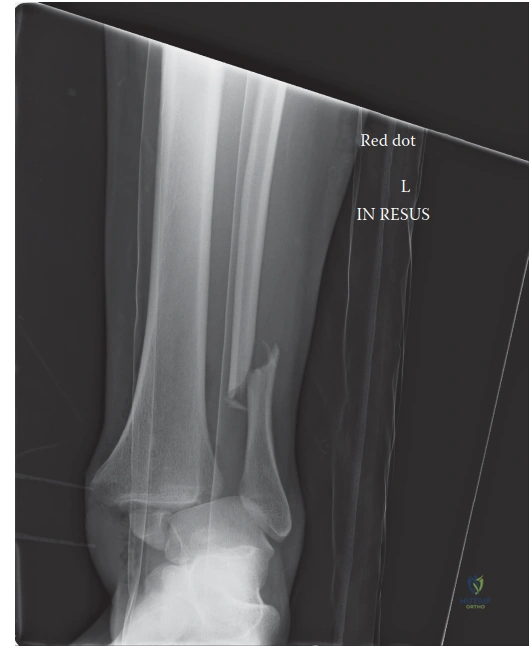
Initial radiographic assessment included standard anteroposterior, mortise, and lateral views of the left ankle. Due to the acute trauma and inability to bear weight, these were obtained non-weight-bearing.

The radiographic findings were diagnostic of a highly unstable, multi-column injury to the ankle mortise.
* The anteroposterior view demonstrated an oblique fracture of the distal fibula originating proximal to the level of the syndesmosis.
* The mortise view revealed critical widening of the medial clear space, measuring greater than 4 millimeters, indicative of complete deltoid ligament complex rupture. Furthermore, there was overt syndesmotic diastasis, evidenced by a tibiofibular clear space exceeding 6 millimeters and a complete loss of normal tibiofibular overlap.
* The lateral view was particularly revealing, demonstrating significant posterior subluxation of the talus relative to the longitudinal axis of the tibia. A large posterior malleolar fracture fragment was identified, involving an estimated 30 to 35 percent of the distal tibial articular surface, with proximal displacement. The fibula appeared shortened and posteriorly displaced.
Advanced Cross Sectional Imaging
Given the presence of a large posterior malleolar fragment and the high-energy axial load mechanism, a non-contrast Computed Tomography scan of the ankle with multi-planar reconstructions is an absolute requirement for preoperative planning. Plain radiographs notoriously underestimate the size, complexity, and articular comminution of posterior malleolar fractures.
The CT scan is utilized to define the fracture morphology according to the Bartoníček-Rammelt or Haraguchi classification systems. It is essential for identifying the presence of a posteromedial extension, intercalary articular fragments (die-punch fragments) that require elevation, and the exact orientation of the primary fracture lines. Furthermore, cross-sectional imaging allows for the assessment of the syndesmotic incisura; avulsion fractures of the anterior or posterior inferior tibiofibular ligaments (Chaput or Volkmann fragments, respectively) dictate specific fixation strategies that differ from purely ligamentous disruptions.
Preoperative Templating and Planning
Digital templating is performed utilizing the multi-planar CT reconstructions and calibrated plain radiographs. The primary surgical goals are the anatomic restoration of the fibular length and rotation, anatomic reduction of the posterior malleolus to restore the incisura fibularis and the posterior articular facet, and the stabilization of the syndesmosis and medial column.
Templating involves selecting the appropriate length and contour for a posterolateral fibular plate (typically an anatomic locking plate or a one-third tubular plate applied in an anti-glide fashion). For the posterior malleolus, depending on the fragment morphology, planning includes either posterior-to-anterior lag screws or a posterior buttress plate. Given the patient's diabetic status and the need for robust fixation, buttress plating of the posterior malleolus is strongly favored over isolated screw fixation to prevent secondary displacement.
Differential Diagnosis
The clinical and radiographic presentation of a complex ankle fracture requires precise classification to guide surgical decision-making. The differential diagnosis centers on the specific vector of force applied to the ankle mortise.
| Diagnosis | Mechanism of Injury | Key Radiographic Findings | Clinical Distinctions |
|---|---|---|---|
| Pronation External Rotation Stage IV | Pronated foot subjected to external rotation force. | Medial clear space widening or medial malleolus fracture, anterior syndesmotic disruption, high fibular fracture (above incisura), posterior malleolus fracture or PITFL rupture. | Severe medial soft tissue injury. Fibula fracture is typically short oblique or spiral, located well above the joint line. High rate of syndesmotic instability. |
| Supination External Rotation Stage IV | Supinated foot subjected to external rotation force. | AITFL rupture, oblique/spiral fibula fracture at the level of the syndesmosis, posterior malleolus fracture, medial malleolus fracture or deltoid rupture. | Most common ankle fracture. Fibula fracture begins anteriorly at the joint line and extends posterosuperiorly. |
| Pronation Abduction Stage III | Pronated foot subjected to an abduction force. | Medial malleolus fracture or deltoid rupture, syndesmotic disruption, transverse or short oblique fibular fracture above the syndesmosis. | Fibula fracture is typically transverse or comminuted (butterfly fragment) due to bending forces, rather than spiral from rotational forces. |
| Maisonneuve Fracture | External rotation force transmitted through the interosseous membrane. | Medial clear space widening, syndesmotic diastasis, proximal third fibular shaft or fibular neck fracture. | Requires full-length tibia/fibula radiographs. Proximal fibular tenderness is the clinical hallmark. Ankle radiographs may only show isolated medial clear space widening. |
Surgical Decision Making and Classification
Fracture Classification Systems
This injury pattern is classically described by the Lauge-Hansen classification as a Pronation-External Rotation Stage IV fracture. The sequence of failure in a PER injury begins medially with a transverse fracture of the medial malleolus or a rupture of the deltoid ligament (Stage I). The force then progresses to rupture the anterior inferior tibiofibular ligament and the interosseous membrane (Stage II). Continued external rotation results in a short oblique or spiral fracture of the fibula proximal to the level of the syndesmosis (Stage III). Finally, the force disrupts the posterior inferior tibiofibular ligament or avulses the posterior malleolus (Stage IV).
Under the AO/OTA alphanumeric classification system, this is categorized as a 44-C3 variant. The "C" designates a syndesmotic disruption with a fibular fracture proximal to the syndesmosis, and the "3" indicates a complex fibular lesion or a very proximal fibular fracture associated with extensive syndesmotic and interosseous membrane tearing, combined with medial and posterior column failure.
Indications for Operative Intervention
Operative intervention is definitively indicated for this patient. Non-operative management of a PER Stage IV fracture with a large posterior malleolus fragment and syndesmotic diastasis universally leads to post-traumatic osteoarthritis, chronic instability, and severe functional impairment. The specific indications for surgery in this case include:
1. Displacement of the weight-bearing articular surface (posterior malleolus > 2 millimeters step-off or gap).
2. Posterior subluxation of the talus, indicating failure of the primary posterior stabilizers.
3. Syndesmotic diastasis, leading to uncoupling of the distal tibiofibular articulation.
4. Fibular shortening and malrotation, which alters the kinematics of the talocrural joint.
5. Medial clear space widening indicative of deep deltoid ligament incompetence.
Soft Tissue Timing and Staging
The timing of surgical intervention is dictated entirely by the condition of the soft tissue envelope. Given the presence of extreme edema and early fracture blisters, immediate open reduction and internal fixation carries a prohibitively high risk of wound dehiscence and deep infection, particularly in a diabetic smoker.
The standard of care for this presentation is a staged protocol. The patient should undergo immediate closed reduction of the talar subluxation in the emergency department, followed by the application of a well-padded, multi-layer posterior and U-shaped sugar-tong splint. If the reduction cannot be maintained in a splint, or if the soft tissues are critically threatened by residual displacement, a spanning joint-bridging external fixator (delta frame configuration) is applied. Definitive internal fixation is delayed until the soft tissue edema has resolved, typically indicated by the return of skin wrinkles (the "wrinkle sign") and the re-epithelialization of fracture blisters, a process that may take 10 to 21 days.
Surgical Technique and Intervention
Patient Positioning and Anesthesia
Once the soft tissue envelope permits definitive fixation, the patient is brought to the operating room. General anesthesia is typically induced, supplemented by a regional popliteal and saphenous nerve block for postoperative analgesia.
Given the necessity to address the posterior malleolus, the fibula, and potentially the medial column, patient positioning is critical. The prone position is highly advantageous for this specific injury pattern. It allows direct, orthogonal access to the posterior malleolus and the posterolateral fibula through a single incision. The patient is positioned prone on a radiolucent Jackson table with all bony prominences meticulously padded. A thigh tourniquet is applied. The ipsilateral hip is slightly bumped to internally rotate the leg, bringing the fibula into a more accessible plane. Fluoroscopy is positioned to allow for unobstructed anteroposterior, mortise, and lateral imaging.
Surgical Approaches
A posterolateral approach is utilized to access both the posterior malleolus and the fibula. The incision is placed longitudinally midway between the posterior border of the fibula and the lateral border of the Achilles tendon.
The superficial dissection requires careful identification and protection of the sural nerve and the lesser saphenous vein, which typically cross the operative field from medial to lateral in the proximal aspect of the incision. The deep fascia is incised in line with the skin incision.
The internervous plane is developed between the peroneal tendons (innervated by the superficial peroneal nerve) laterally and the flexor hallucis longus (innervated by the tibial nerve) medially. Retracting the peroneal tendons anteriorly exposes the posterolateral border of the fibula. Retracting the flexor hallucis longus medially protects the posteromedial neurovascular bundle (tibial nerve and posterior tibial artery) and exposes the posterior aspect of the distal tibia and the posterior malleolar fragment.
Posterior Malleolus Reduction and Fixation
Historically, posterior malleolus fractures were only fixed if they involved greater than 25 to 33 percent of the articular surface. Modern orthopedic trauma principles dictate that the posterior malleolus should be anatomically reduced and fixed regardless of size if it contributes to syndesmotic instability or articular incongruity. The posterior malleolus houses the attachment of the posterior inferior tibiofibular ligament; anatomical fixation of the bone fragment restores the ligamentous tension and provides up to 70 percent of the stability of the syndesmosis.
Through the posterolateral approach, the posterior malleolar fracture site is debrided of hematoma and interposed periosteum. The joint is inspected for osteochondral debris or intercalary die-punch fragments, which must be elevated and bone-grafted if necessary.
The primary posterior fragment is reduced using a dental pick or a ball-spiked pusher. Reduction is confirmed fluoroscopically and via direct visualization of the cortical read at the metaphyseal apex. Provisional fixation is achieved with Kirschner wires. Definitive fixation is performed using a posterior buttress plate (e.g., a 2.7mm or 3.5mm pre-contoured distal tibia plate or a flattened one-third tubular plate) applied in an anti-glide fashion. This biomechanically superior construct resists the proximal shear forces generated by the talus during weight-bearing.
Fibular and Syndesmotic Reconstruction
Following posterior malleolar fixation, attention is turned to the fibula. The fracture is debrided and anatomically reduced, ensuring precise restoration of length and rotation. Provisional reduction is held with reduction forceps. Depending on the fracture morphology (oblique vs. comminuted), a lag screw may be placed perpendicular to the fracture plane.
A posterolateral plate is then applied. Utilizing the posterolateral surface of the fibula allows for an anti-glide plating technique, which biomechanically limits the proximal migration of the distal fragment and provides a robust soft tissue coverage layer compared to direct lateral plating.
Once the fibula and posterior malleolus are stabilized, the syndesmosis must be dynamically assessed. The "Cotton test" is performed by applying a lateral traction force to the fibula using a bone hook while visualizing the mortise under fluoroscopy. Because the posterior inferior tibiofibular ligament has been restored via the posterior malleolus fixation, the syndesmosis is often found to be stable. If residual diastasis is present (indicating severe anterior inferior tibiofibular ligament and interosseous membrane disruption), trans-syndesmotic fixation is required. This can be achieved with either flexible suture-button constructs or rigid metallic screws (typically one or two 3.5mm or 4.5mm screws placed parallel to the joint line across three or four cortices).
Medial Column Management
The final step is the evaluation of the medial column. In this PER Stage IV variant, the medial clear space widening is due to a complete rupture of the deltoid ligament complex. With anatomic restoration of the lateral and posterior columns, the talus typically centralizes within the mortise, and the medial clear space reduces anatomically.
Routine primary repair of the deltoid ligament is controversial and generally not indicated if the mortise is anatomically reduced and stable. However, if there is residual medial clear space widening following lateral and posterior fixation, or if there is soft tissue interposition preventing talar reduction, a medial incision is required. The deep deltoid ligament is explored, interposed tissue is removed, and a direct repair using suture anchors into the medial malleolus may be performed to restore medial stability.
Post Operative Protocol and Rehabilitation
Immediate Postoperative Care
Following wound closure, a sterile dressing is applied, and the extremity is immobilized in a well-padded, short-leg posterior splint with a U-shaped stirrup, maintaining the ankle in a neutral position (zero degrees of dorsiflexion). The patient is admitted for 24 to 48 hours for intravenous antibiotics (typically a first-generation cephalosporin for 24 hours), pain management, and strict elevation of the affected extremity.
Given the patient's risk factors (diabetes, smoking, and operative trauma), mechanical and pharmacological deep vein thrombosis prophylaxis is initiated. Chemical prophylaxis, such as low-molecular-weight heparin or a direct oral anticoagulant, is continued for a minimum of two to four weeks, depending on institutional protocols and patient mobility. Strict non-weight-bearing status is enforced.
Early Rehabilitation Phase
At the two-week postoperative mark, the patient returns to the clinic for a wound check and suture removal. Given the diabetic status, the surgical incisions must be meticulously inspected for any signs of marginal necrosis or delayed healing.
If the wounds are healing appropriately, the splint is transitioned to a removable controlled ankle motion (CAM) boot. The patient remains strictly non-weight-bearing. However, early active and active-assisted range of motion exercises of the ankle and subtalar joint are initiated to prevent arthrofibrosis and promote cartilage nutrition. Physical therapy focuses on gentle dorsiflexion and plantarflexion, avoiding aggressive inversion or eversion that might stress the syndesmotic or deltoid repairs.
Advanced Weight Bearing and Functional Recovery
Radiographic evaluation is performed at six weeks postoperatively to assess for callus formation and maintenance of reduction. If clinical and radiographic progression of healing is satisfactory, a graduated weight-bearing protocol is initiated.
The patient begins with partial weight-bearing (approximately 25 percent of body weight) in the CAM boot, progressing by 25 percent each week until full weight-bearing is achieved. Physical therapy is escalated to include proprioceptive training, intrinsic foot muscle strengthening, and closed-kinetic-chain exercises.
For a complex pilon-variant injury with a large posterior malleolus fragment, maximal medical improvement and return to heavy labor (such as construction) may take six to twelve months. The patient must be counseled that some degree of permanent stiffness and a risk of post-traumatic osteoarthritis are inherent to this high-energy articular injury.
Clinical Pearls and Pitfalls
Optimization of Surgical Outcomes
- CT Scanning is Mandatory: Never attempt to fix a complex rotational ankle fracture with a suspected posterior malleolus component without a preoperative CT scan. Plain radiographs fail to demonstrate the true articular comminution, the presence of die-punch fragments, and the exact orientation of the fracture lines necessary for precise plate contouring and screw trajectory.
- Posterior First Approach: When utilizing the prone posterolateral approach, addressing the posterior malleolus before the fibula often simplifies the procedure. The posterior malleolus provides a broad metaphyseal read that is easier to reduce anatomically. Once fixed, it restores the posterior inferior tibiofibular ligament, which subsequently assists in the indirect reduction of the fibula and the syndesmosis.
- Anatomic Fibular Length: The most critical factor in restoring ankle kinematics is the anatomic restoration of fibular length. Even one millimeter of fibular shortening results in significant lateral shift of the talus, decreasing the tibiotalar contact area by up to 42 percent, rapidly accelerating the onset of post-traumatic arthritis.
Avoidance of Common Complications
- Soft Tissue Disasters: The most devastating complication in this patient population (diabetic smokers) is wound breakdown leading to deep infection and osteomyelitis. Never rush definitive fixation. Wait for the soft tissue envelope to declare itself safe (positive wrinkle sign). If in doubt, utilize a spanning external fixator.
- Syndesmotic Malreduction: Malreduction of the syndesmosis is the leading cause of poor functional outcomes following operative fixation of ankle fractures. Direct visualization of the anterior syndesmotic incisura or the use of intraoperative bilateral fluoroscopic imaging or 3D fluoroscopy (O-arm) is highly recommended to confirm anatomic reduction before final fixation.
- Hardware Prominence: When plating the posterior malleolus, ensure the plate is positioned as distally as possible to buttress the fragment, but avoid encroaching on the posterior joint capsule or the flexor hallucis longus tendon sheath, which can lead to postoperative tenosynovitis or restricted hallux excursion.
