High-Energy Syndesmotic Ankle Injury: Clinical Presentation & Diagnostic Insights
Key Takeaway
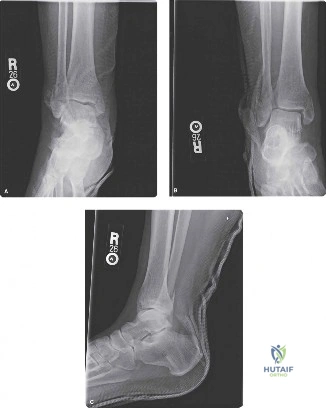
Diagnosis of a high-energy syndesmotic ankle injury involves a detailed clinical exam, positive special tests like the Squeeze and External Rotation Stress tests, and critical imaging. Radiographs typically reveal a distal fibular fracture (e.g., Weber C), widened tibiofibular clear space, and reduced tibiofibular overlap, indicating syndesmotic disruption and instability.
Introduction and Epidemiology
High-energy syndesmotic ankle injuries represent a complex and challenging subset of orthopedic trauma, demanding precise diagnostic acumen and meticulous surgical execution. The distal tibiofibular syndesmosis is critical for maintaining the structural integrity of the ankle mortise. Disruption of this ligamentous complex, particularly in high-demand athletic populations, significantly alters ankle biomechanics and load transmission. Failure to recognize or anatomically restore the syndesmosis invariably leads to chronic instability, altered contact stresses across the tibiotalar joint, and accelerated post-traumatic osteoarthritis.
A paradigmatic clinical presentation involves a 32-year-old male, semi-professional soccer player, presenting to the emergency department following a high-energy rotational injury to the left ankle during a competitive match. The patient reported being tackled from behind while the foot was planted and externally rotated, resulting in immediate severe pain, inability to bear weight, and rapid swelling. The chief complaint was exquisite pain in the left ankle and foot, rated 9/10 on the Visual Analogue Scale. The absence of prior significant ankle injuries or surgeries, combined with an unremarkable past medical history, underscores the acute and high-energy nature of the trauma. Given the patient's athletic background, achieving a prompt and effective return to high-level function constitutes the primary consideration for management.
The mechanism described—a pronation-external rotation force—is highly suggestive of a syndesmotic injury, often accompanied by associated fractures, aligning with the Lauge-Hansen classification system. The energy of the injury implies a potential for significant soft tissue damage, necessitating careful evaluation for impending compartment syndrome or open wounds. The patient's age and activity level underscore the imperative for anatomical reduction and stable fixation to optimize long-term outcomes.
Epidemiologically, syndesmotic injuries account for approximately 10% to 20% of all ankle injuries, but this incidence rises to nearly 30% in athletic populations engaged in collision sports. High-energy variants are frequently associated with rotational ankle fractures, specifically Weber B and Weber C fibular fractures. The recognition of subtle or purely ligamentous syndesmotic disruptions remains a diagnostic challenge, emphasizing the need for a high index of suspicion based on mechanism of injury and clinical examination.
Surgical Anatomy and Biomechanics
Osteology of the Distal Tibiofibular Joint
The distal tibiofibular joint is a fibrous syndesmosis formed by the articulation between the convex medial surface of the distal fibula and the concave lateral surface of the distal tibia, known as the incisura fibularis. The incisura is bounded anteriorly by the Chaput tubercle and posteriorly by the Volkmann tubercle. The corresponding articular facets on the fibula are the Wagstaffe tubercle anteriorly and the posterior fibular tubercle. The precise anatomical congruence of these osseous structures is fundamental to the stability of the ankle mortise.
Ligamentous Anatomy
The syndesmotic complex is composed of four primary ligamentous structures:
1. Anterior Inferior Tibiofibular Ligament (AITFL): Originates from the Chaput tubercle of the tibia and inserts onto the Wagstaffe tubercle of the fibula. It courses obliquely in a distal and lateral direction. The AITFL is the weakest of the syndesmotic ligaments and is typically the first to fail during an external rotation injury.
2. Posterior Inferior Tibiofibular Ligament (PITFL): A robust structure originating from the Volkmann tubercle and inserting onto the posterior aspect of the lateral malleolus. It is significantly stronger than the AITFL and provides the majority of the resistance to posterior translation of the fibula.
3. Transverse Tibiofibular Ligament (TTFL): Often considered the deep, inferior component of the PITFL, it extends from the posterior tibial margin to the osteochondral junction of the fibula, acting as a labrum to deepen the articular surface of the tibial plafond.
4. Interosseous Tibiofibular Ligament (ITFL): The distal continuation of the interosseous membrane, consisting of short, dense ligamentous fibers spanning the incisura. It acts as a primary stabilizer against lateral translation of the fibula.
Biomechanical Principles
The syndesmosis functions to maintain the relationship between the tibia and fibula under physiological loads while allowing necessary micromotion. During normal ankle dorsiflexion, the wider anterior dome of the talus engages the mortise, necessitating the fibula to undergo a complex motion profile: it translates laterally by 1 to 2 millimeters, translates proximally, and externally rotates by approximately 2 to 5 degrees.
The fibula transmits approximately 16% of the axial load applied to the lower extremity. Disruption of the syndesmosis drastically alters this load-sharing mechanism. Biomechanical studies have demonstrated that even a 1-millimeter lateral shift of the talus secondary to syndesmotic diastasis decreases the tibiotalar contact area by 42%, exponentially increasing peak contact stresses and predisposing the joint to rapid cartilaginous degeneration. Therefore, the primary biomechanical goal of surgical intervention is the absolute anatomical restoration of the fibula within the incisura fibularis to restore normal contact mechanics.
Indications and Contraindications
The decision-making process for operative versus non-operative management of syndesmotic injuries hinges on the presence of mechanical instability within the ankle mortise. Purely ligamentous injuries without dynamic instability may be managed conservatively, whereas any evidence of diastasis necessitates surgical stabilization.
| Clinical Scenario | Management Strategy | Key Diagnostic Criteria |
|---|---|---|
| Stable Sprain (Grade I/II) | Non-Operative | Tenderness over AITFL; Normal radiographs; Negative gravity/external rotation stress views; No medial clear space widening. |
| Latent Instability | Operative | Normal static radiographs; Widening of medial clear space (>4mm) or tibiofibular clear space (>5mm) on stress radiographs or intraoperative hook test. |
| Frank Diastasis | Operative | Obvious widening of the syndesmosis on static AP/Mortise radiographs; Associated unstable medial malleolus fracture or deltoid rupture. |
| Maisonneuve Fracture | Operative | Proximal fibula fracture with associated syndesmotic disruption and medial injury; High risk of severe instability. |
| Associated Fractures | Operative | Weber B or C fibular fractures with intraoperative evidence of syndesmotic instability after fibular fixation. |
Operative Indications
Surgical stabilization is unequivocally indicated for acute syndesmotic injuries demonstrating frank or latent instability. Radiographic parameters dictating operative intervention include a medial clear space greater than 4 millimeters, a tibiofibular clear space greater than 5 millimeters, or a tibiofibular overlap of less than 1 millimeter on the mortise view. Intraoperative assessment utilizing the Cotton test (lateral traction on the fibula) or external rotation stress test is critical for identifying instability following the fixation of associated malleolar fractures.
Contraindications
Absolute contraindications to immediate internal fixation primarily involve severe soft tissue compromise. The presence of hemorrhagic fracture blisters, gross edema, or active localized infection necessitates a delay in definitive surgical management. In such instances, temporary stabilization via a spanning external fixator may be required until the soft tissue envelope permits safe surgical incisions. Non-ambulatory status or severe peripheral vascular disease represent relative contraindications, requiring a careful risk-benefit analysis tailored to the individual patient.
Pre Operative Planning and Patient Positioning
Clinical Presentation and Initial Assessment
Upon initial assessment in the emergency department, the high-energy nature of the injury dictates a comprehensive evaluation. In the representative case of the 32-year-old athlete, the left ankle presented with marked swelling encompassing the entire ankle joint, extending into the foot and distal leg. Significant ecchymosis was evident circumferentially, particularly prominent on the lateral aspect. While gross deformity or skin tenting was absent, palpable tension in the soft tissues suggested considerable edema. Crucially, the absence of open wounds or skin blisters at the initial evaluation allows for the consideration of early definitive fixation, provided the soft tissue envelope remains compliant.
Palpation is a critical diagnostic tool. Exquisite tenderness elicited along the AITFL and PITFL regions is highly consistent with syndesmotic involvement. Tenderness over the distal fibula and medial malleolus indicates associated osseous or deltoid ligament injuries. The entire length of the fibula must be palpated to definitively rule out a proximal fibular fracture (Maisonneuve injury). Furthermore, the base of the fifth metatarsal and navicular bone must be assessed to exclude concomitant midfoot pathology.
Range of motion is typically severely limited by pain and effusion. Special tests for syndesmotic instability, though limited by acute pain, provide vital diagnostic clues. The Squeeze Test, involving compression of the tibia and fibula at the mid-calf, elicits sharp pain distally at the syndesmosis, indicating interosseous membrane disruption. The External Rotation Stress Test, performed with the knee flexed to 90 degrees and the ankle in neutral dorsiflexion, reproduces severe pain over the distal tibiofibular joint when the foot is gently externally rotated. The Cotton Test, assessing lateral translation of the talus, is often limited by patient guarding in the acute setting.
A rigorous neurological and vascular assessment is mandatory. Dorsalis pedis and posterior tibial pulses must be palpable and strong bilaterally, with brisk capillary refill. Sensory examination should confirm intact light touch sensation across the superficial and deep peroneal, saphenous, sural, and tibial nerve distributions. Motor function, though hindered by pain, should demonstrate gross ability for dorsiflexion and plantarflexion.
Radiographic Evaluation
Standard radiographic evaluation includes weight-bearing (if tolerated) or non-weight-bearing anteroposterior (AP), lateral, and mortise views of the ankle. Full-length tibia-fibula radiographs are imperative if a Maisonneuve fracture is suspected.

If static radiographs appear normal but clinical suspicion remains high, gravity stress views or external rotation stress views are indicated to unmask latent instability. Computed Tomography (CT) is increasingly utilized in the preoperative planning phase for high-energy injuries to assess the exact fracture morphology, identify small avulsion fractures (e.g., Chaput or Volkmann fragments), and evaluate the congruency of the incisura fibularis. Magnetic Resonance Imaging (MRI) is highly sensitive for purely ligamentous injuries but is rarely required in the acute trauma setting when osseous instability is evident.
Patient Positioning and Setup
The patient is positioned supine on a radiolucent operating table. A bump is placed under the ipsilateral hip to internally rotate the leg, bringing the lateral malleolus anteriorly and facilitating access to the fibula. A thigh tourniquet is applied but inflated only if necessary for visualization. The contralateral leg must be protected and positioned to allow unimpeded access for the C-arm fluoroscopy unit, which is typically brought in from the contralateral side. The entire lower extremity is prepped and draped in a standard sterile fashion, allowing for intraoperative manipulation of the knee and ankle.
Detailed Surgical Approach and Technique
Surgical Approaches and Internervous Planes
The surgical approach is dictated by the associated fracture pattern. For a standard PER injury with a fibular fracture, a direct lateral or posterolateral approach to the fibula is utilized.
1. Lateral Approach: An longitudinal incision is made directly over the fibula. The internervous plane lies between the superficial peroneal nerve (anteriorly) and the sural nerve (posteriorly). Care must be taken during the distal dissection to identify and protect the terminal branches of the superficial peroneal nerve, which often cross the surgical field.
2. Medial Approach: If a medial malleolus fracture is present, a standard medial incision is utilized. If a deltoid ligament rupture is suspected and the medial clear space fails to reduce after fibular and syndesmotic fixation, a medial approach is necessary to clear interposed soft tissue (often the deltoid ligament or posterior tibial tendon) from the medial gutter.
Step-by-Step Surgical Technique
Step 1 Fibular Reduction and Fixation
Anatomical reduction of the fibula is the absolute prerequisite for syndesmotic reduction. The fibula dictates the lateral border of the ankle mortise; any shortening, malrotation, or angular deformity will preclude accurate seating of the fibula within the incisura. The fracture is exposed, the hematoma evacuated, and the fracture ends debrided. Reduction is achieved using pointed reduction forceps. Fixation is typically accomplished using a lag screw and a neutralization plate, or a bridging plate for highly comminuted patterns.
Step 2 Medial Malleolar Fixation
If a medial malleolus fracture is present, it is addressed next. Anatomical reduction and fixation with partially threaded cancellous screws or a tension band construct restore the medial buttress of the mortise.
Step 3 Intraoperative Assessment of the Syndesmosis
Following osseous fixation, the stability of the syndesmosis must be rigorously tested. The "Hook Test" or "Cotton Test" is performed under direct fluoroscopic visualization. A bone hook is placed around the fibula at the level of the joint line, and a lateral traction force is applied. Widening of the tibiofibular clear space or the medial clear space confirms syndesmotic incompetence requiring fixation.
Step 4 Open Reduction of the Syndesmosis
Historically, syndesmotic reduction was performed percutaneously or indirectly. However, current academic consensus strongly advocates for direct open visualization of the incisura fibularis. A limited anterior arthrotomy is performed through the lateral incision to visualize the joint line. The fibula is manually manipulated into the incisura. The surgeon must ensure that the fibula is not over-compressed, anteriorly translated, or internally rotated—common errors when relying solely on reduction clamps.
Step 5 Placement of the Reduction Clamp
A large Weber clamp or pelvic reduction forceps is utilized to hold the reduction. The placement of the clamp tines is critical. The lateral tine is placed on the fibular ridge, and the medial tine is placed on the anteromedial tibia. The clamp should be applied at the level of the planned fixation, typically 2 to 3 centimeters proximal to the joint line. The vector of compression must be parallel to the joint line and directed slightly anteriorly (approximately 20 to 30 degrees relative to the coronal plane) to match the anatomical axis of the syndesmosis. Clamp pressure should be gentle to avoid irogenic over-compression of the mortise.
Step 6 Syndesmotic Fixation Options
The surgeon must choose between static fixation (screws) and dynamic fixation (suture button constructs).
- Trans-syndesmotic Screws: The traditional gold standard. A 3.5mm or 4.5mm fully threaded cortical screw is utilized. The screw is placed 2 to 3 centimeters proximal to the joint line, directed from posterolateral to anteromedial (30 degrees anterior to the coronal plane). The screw is not intended to act as a lag screw; it functions as a position screw. Therefore, the fibula is not over-drilled. The debate between tricortical (engaging two fibular and one tibial cortex) and quadricortical fixation remains ongoing, with tricortical fixation theoretically allowing more physiological motion and reducing the risk of symptomatic hardware breakage.
- Suture Button Constructs: Increasingly preferred for high-energy athletic injuries. These dynamic devices consist of a heavy non-absorbable suture spanning the syndesmosis, secured by metallic buttons on the lateral fibula and medial tibia. They permit physiological micromotion, potentially accelerating rehabilitation and eliminating the need for routine hardware removal.
Step 7 Final Fluoroscopic and Clinical Verification
Following fixation, the clamp is removed. Comprehensive fluoroscopic imaging (AP, lateral, and mortise views) is obtained to confirm the restoration of the medial clear space, tibiofibular clear space, and tibiofibular overlap. The ankle is taken through a full range of motion to ensure no impingement or over-constraint exists.
Complications and Management
The management of high-energy syndesmotic injuries is fraught with potential complications. Meticulous surgical technique and rigorous postoperative surveillance are required to mitigate these risks.
| Complication | Estimated Incidence | Etiology and Clinical Presentation | Management and Salvage Strategies |
|---|---|---|---|
| Syndesmotic Malreduction | 15% - 52% | Failure to anatomically reduce the fibula into the incisura (often anterior or over-compressed). Presents as chronic pain, stiffness, and early osteoarthritis. | Pre-operative CT planning; Direct open visualization of the incisura during surgery. Post-operative CT to confirm reduction. Revision surgery (osteotomy or revision fixation) if identified early. |
| Hardware Failure (Screw Breakage) | 10% - 30% | Normal physiological stresses across the syndesmosis during weight-bearing cause rigid screws to fatigue and break. | Often asymptomatic and left in situ. If symptomatic or if breakage occurs within the joint space, surgical extraction is required. Consider suture button constructs to prevent this. |
| Tibiofibular Synostosis | 2% - 10% | Heterotopic ossification of the interosseous membrane due to severe trauma, hematoma, or drilling debris. Presents as severe stiffness and loss of dorsiflexion. | Observation if asymptomatic. Surgical excision of the synostosis is considered only after the bone has fully matured (typically >12 months) and if functional limitation is severe. |
| Wound Dehiscence / Infection | 2% - 5% | Compromised soft tissue envelope, particularly in high-energy trauma or patients with comorbidities (diabetes, smoking). | Aggressive local wound care, targeted antibiotic therapy. Deep infections require prompt surgical debridement and potential hardware removal once fracture union is achieved. |
| Post-Traumatic Osteoarthritis | Variable | Direct cartilage damage at the time of injury or secondary to chronic altered biomechanics from malreduction. | Conservative management (NSAIDs, bracing, injections). End-stage salvage procedures include ankle arthrodesis or total ankle arthroplasty. |
The Malreduction Paradigm
Malreduction remains the most critical complication. Historical reliance on two-dimensional fluoroscopy resulted in unacceptably high rates of malreduction, as plain films are notoriously insensitive to minor rotational or sagittal plane translational errors. The advent of intraoperative 3D imaging (O-arm) and routine postoperative CT scanning has highlighted this issue. If malreduction is identified in the early postoperative period, prompt revision surgery is mandatory to prevent rapid joint destruction.
Post Operative Rehabilitation Protocols
Rehabilitation following high-energy syndesmotic fixation must balance the need for early mobilization to prevent stiffness with the necessity of protecting the biological healing of the syndesmotic ligaments. The protocol varies slightly depending on whether rigid screws or dynamic suture buttons were utilized.
Phase 1 Acute Protection (Weeks 0-2)
The primary goals are edema control, wound healing, and pain management. The patient is placed in a well-padded short leg splint or a rigid fracture boot. The patient is strictly non-weight-bearing (NWB) on the operative extremity. Elevation and cryotherapy are heavily emphasized. Sutures are typically removed at 14 days postoperatively.
Phase 2 Early Mobilization (Weeks 2-6)
Once the incisions have healed, the patient is transitioned to a removable controlled ankle motion (CAM) boot.
* Weight-Bearing: For screw fixation, patients generally remain NWB or touch-down weight-bearing (TDWB) to protect the hardware. For suture button constructs, early progressive weight-bearing may be initiated at the surgeon's discretion, as the dynamic nature of the implant accommodates physiological loading.
* Range of Motion: Active and active-assisted range of motion exercises are initiated, focusing strictly on sagittal plane motion (dorsiflexion and plantarflexion). Inversion and eversion are strictly prohibited, as these motions place direct rotational stress on the healing syndesmosis.
Phase 3 Progressive Loading and Strengthening (Weeks 6-12)
Radiographic evaluation is performed at 6 weeks to assess maintenance of reduction and fracture healing.
* Weight-Bearing: Patients are transitioned to full weight-bearing (FWB) in the CAM boot, and gradually weaned into a supportive athletic shoe.
* Physical Therapy: Rehabilitation focuses on restoring normal gait mechanics, proprioception, and progressive strengthening of the peroneal and tibial musculature. Closed kinetic chain exercises are introduced.
Phase 4 Advanced Rehabilitation and Return to Sport (Weeks 12+)
For high-demand athletes, such as the 32-year-old soccer player in the clinical vignette, sports-specific training is initiated once full, painless ROM and near-normal strength are achieved. Plyometrics, cutting drills, and sport-specific functional testing are utilized to determine readiness for return to play.
The Hardware Removal Controversy
The routine removal of trans-syndesmotic screws prior to weight-bearing is a subject of intense academic debate. Historically, screws were removed at 8 to 12 weeks to prevent breakage and restore physiological mortise motion. However, modern literature suggests that routine removal is unnecessary, exposes the patient to the risks of a second surgery, and carries a risk of recurrent diastasis. Currently, screw removal is generally reserved for symptomatic hardware, prominent screw heads, or specific athletic requirements. Suture button constructs circumvent this dilemma entirely, as they do not require removal.
Summary of Key Literature and Guidelines
The surgical management of syndesmotic injuries has evolved significantly over the past decade, driven by rigorous biomechanical and clinical research.
Current academic consensus heavily emphasizes the superiority of Computed Tomography over plain radiography for assessing the accuracy of syndesmotic reduction. Seminal work by Gardner et al. demonstrated that plain radiographs fail to identify significant syndesmotic malreductions in up to half of cases, establishing postoperative CT as the gold standard for evaluating the incisura fibularis.
Regarding fixation modalities, the debate between rigid screws and dynamic suture buttons has been largely clarified by recent prospective randomized controlled trials and meta-analyses. Studies consistently demonstrate that suture button constructs yield equivalent or superior functional outcome scores (e.g., AOFAS, Olerud-Molander) compared to screw fixation. Furthermore, dynamic fixation is associated with a lower incidence of syndesmotic malreduction, as the implant allows the fibula to auto-center within the incisura during the healing phase. The elimination of routine hardware removal surgeries further bolsters the health-economic argument for dynamic fixation in appropriate patients.
Despite these advancements, the fundamental principles remain unchanged: high-energy syndesmotic injuries demand a high index of clinical suspicion, meticulous anatomical restoration of the fibular length and rotation, direct visualization of the syndesmotic reduction, and stable fixation to ensure the long-term survivorship of the ankle joint. Continuous adherence to these biomechanical imperatives is essential for optimizing patient outcomes in this complex trauma population.
