Detailed Patient Presentation and Mechanism of Injury
A 29-year-old, left-hand-dominant male presents to the orthopedic trauma and sports medicine clinic complaining of severe left arm and anterior shoulder pain that has persisted for the past three days. The patient is an avid, competitive weight-lifter who was in the midst of a high-intensity training cycle. He reports that the injury occurred specifically while performing the barbell bench press. During the eccentric phase of the lift—lowering the heavy barbell to his chest—he experienced a sudden, sharp tearing sensation accompanied by an audible "pop" in his left anterior axilla. This was immediately followed by a precipitous loss of power, forcing his spotter to rescue the weight to prevent further catastrophic injury. Since the event, he has been utilizing cryotherapy and strict rest, which has provided only marginal relief. He notes profound inability to utilize the left upper extremity for anything beyond carrying trivial, light-weight objects, and he specifically highlights significant functional deficit and sharp pain when attempting activities of daily living, such as donning or doffing a t-shirt.
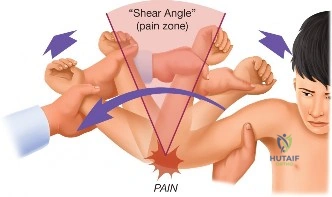
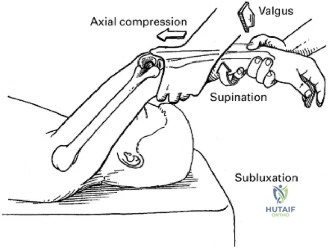
To fully appreciate the pathophysiology of this injury, one must understand the exact biomechanics of the barbell bench press and the precise kinematic chain involved. The bench press places the glenohumeral joint in a position of combined extension, abduction, and external rotation during the eccentric descent of the bar. In this position, the pectoralis major muscle—specifically the sternocostal head—is subjected to immense eccentric loading. The sternocostal head is uniquely vulnerable due to its complex anatomical twisting; the inferior fibers of the sternocostal head rotate 180 degrees to insert proximally and deep to the clavicular head on the lateral lip of the bicipital groove. Consequently, when the arm is extended and externally rotated, these inferior fibers are stretched to their absolute maximum excursion, creating a mechanical disadvantage that predisposes them to catastrophic tensile failure under heavy eccentric loads.
Furthermore, the patient’s demographic and activity profile strongly correlate with the classic epidemiological presentation of this injury. Pectoralis major ruptures are overwhelmingly seen in males in their third to fourth decades of life who engage in heavy resistance training. While the patient in this scenario did not explicitly disclose the use of anabolic-androgenic steroids (AAS), it is a critical historical point to consider and gently inquire about, as AAS use is a well-documented risk factor. Anabolic steroids induce rapid muscle hypertrophy that outpaces the physiological adaptation and tensile strength of the tendinous insertion, leading to a profound mismatch between the contractile force generated by the muscle belly and the load-bearing capacity of the myotendinous junction and bony footprint. This disparity significantly lowers the threshold for acute rupture during maximal eccentric contraction.
Comprehensive Clinical Examination Findings
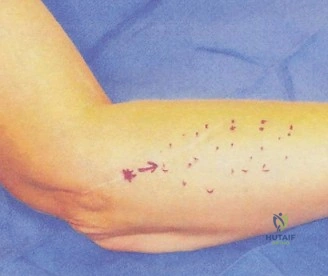
Upon physical examination, the patient presents with classic, textbook signs of a severe anterior shoulder girdle injury. Inspection reveals profound asymmetry of the anterior chest wall, characterized by the pathognomonic loss of the normal anterior axillary fold on the left side. There is extensive ecchymosis extending from the anterior axilla down the medial aspect of the brachium, a result of gravity pulling the hematoma through the fascial planes of the arm. The muscle belly of the pectoralis major appears retracted medially toward the sternum, creating a visible defect or "hollow" in the deltopectoral groove region. When the patient is asked to press his hands together in an isometric contraction (the prayer test), the medialization of the muscle belly becomes starkly exaggerated, highlighting the loss of lateral tethering at the humeral insertion.
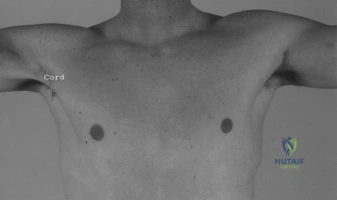
Palpation of the anterior axilla reveals a critical clinical pitfall that often confounds inexperienced examiners. One can palpate what feels like a prominent, continuous, cord-like structure spanning the axilla, which may be erroneously interpreted as an intact pectoralis major tendon. However, this structure actually represents the intact superficial fascia of the pectoralis major, which remains continuous with the brachial fascia and the medial antebrachial septum. Relying on this pseudotendon can lead to a disastrous missed diagnosis. True palpation deep to this fascial layer reveals a distinct void where the robust, broad tendinous insertion of the pectoralis major should attach to the lateral lip of the bicipital groove. The area is exquisitely tender to palpation, particularly over the expected footprint and the retracted myotendinous stump.
Range of motion and strength testing further solidify the clinical suspicion. The patient exhibits profound weakness and apprehension with resisted shoulder adduction and internal rotation. To differentiate between the heads of the pectoralis major, the examiner can test adduction at different angles of elevation. Resisted adduction with the arm elevated at 90 degrees primarily isolates the sternocostal head (which is typically weak and painful in this scenario), while resisted adduction with the arm at the side isolates the clavicular head (which may remain relatively intact, depending on the extent of the tear). Crucially, the patient has a negative Hawkins-Kennedy sign and a negative Neer impingement sign, significantly lowering the probability of an acute rotator cuff tear. Furthermore, a negative Yergason test and a negative Speed’s test help rule out primary pathology of the long head of the biceps tendon, which resides in close proximity to the pectoralis insertion.
Advanced Imaging and Diagnostics
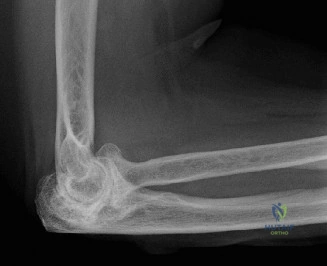
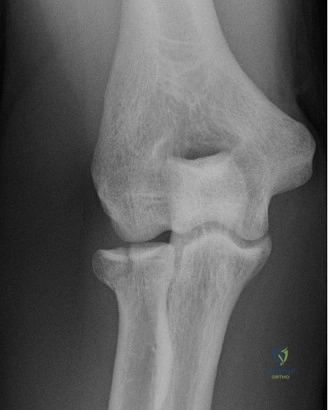
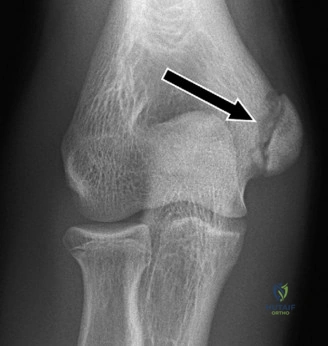
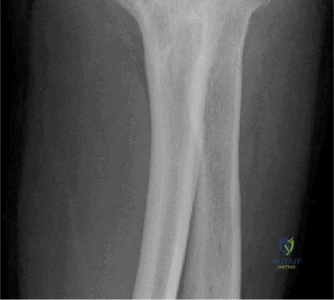
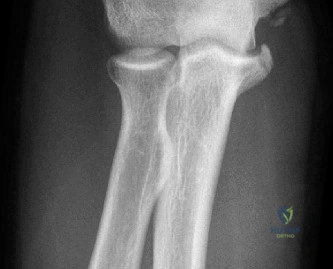
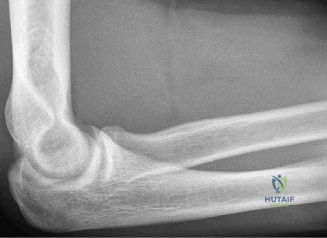
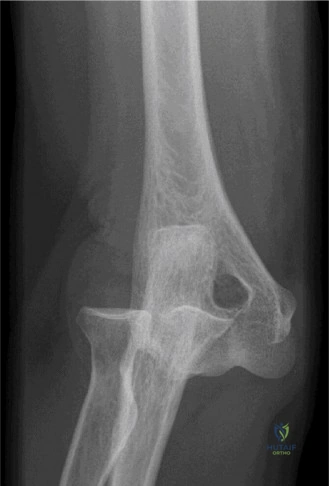
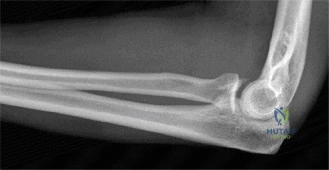
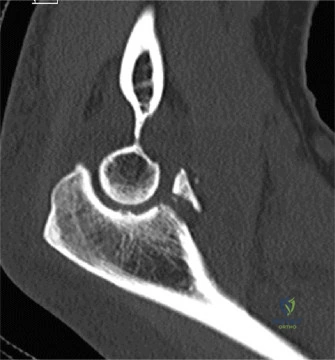
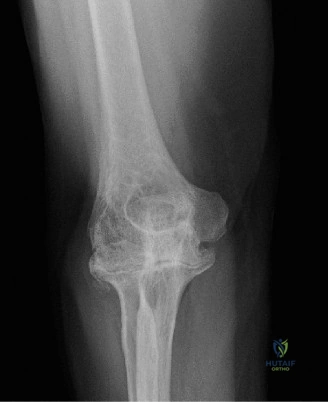
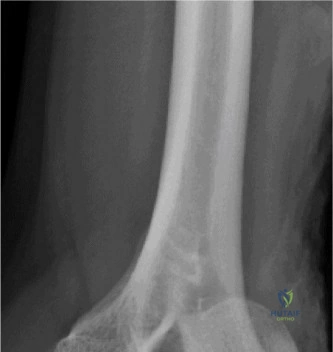
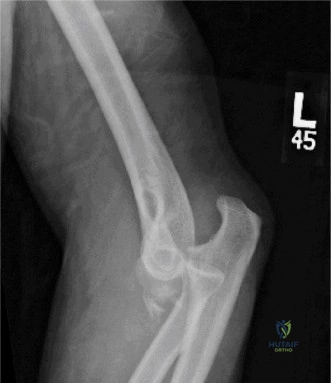
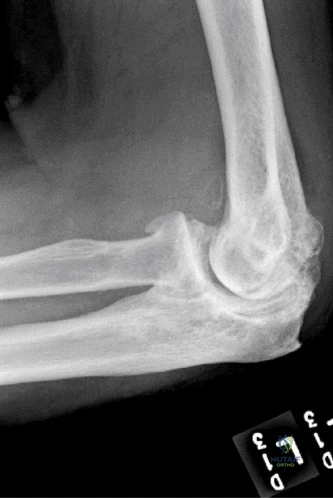
Despite the classic clinical presentation, advanced imaging is paramount for surgical planning, confirming the exact anatomic location of the tear, and assessing the degree of chronicity and retraction. The initial step in the diagnostic algorithm involves standard orthogonal radiographs of the shoulder, including an anteroposterior (AP) view, a true scapular Y view, and an axillary lateral view. In the vast majority of pectoralis major ruptures, these radiographs will be entirely unremarkable, as was the case with this patient. However, they are essential to rule out associated osseous trauma, such as a bony avulsion fracture from the lateral lip of the bicipital groove, anterior glenohumeral dislocation, or underlying neoplastic processes weakening the bone.
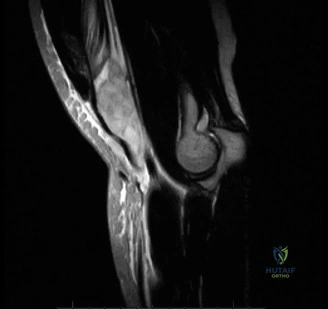
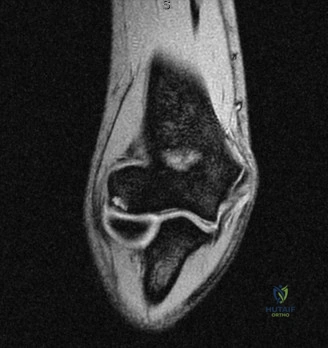
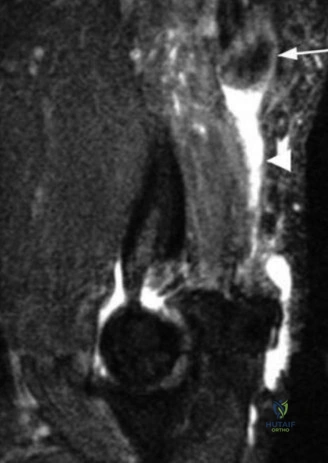
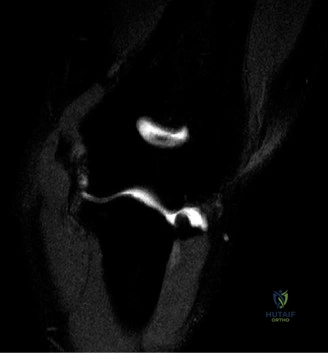
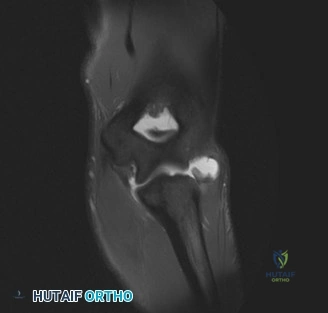
When radiographs are normal, Magnetic Resonance Imaging (MRI) is the undisputed gold standard for evaluating pectoralis major injuries. To optimize the diagnostic yield, the MRI should ideally be performed with the patient in a specialized position—often with the arm slightly abducted and externally rotated, if tolerated—to place the remaining tendon under mild tension, thereby accentuating the defect. T2-weighted fluid-sensitive sequences (such as STIR or fat-suppressed T2) in the axial and coronal oblique planes are the most critical for identifying acute edema, hemorrhage, and the exact site of failure. The axial images are particularly adept at demonstrating the medial retraction of the muscle belly and the empty footprint on the humerus, while the coronal images help differentiate between isolated sternocostal head tears and combined sternocostal/clavicular head avulsions.
The MRI must be meticulously scrutinized to classify the tear anatomically, as this dictates the surgical approach. The radiologist and the orthopedic surgeon must collaboratively determine if the tear is located at the muscle belly (rare and usually treated non-operatively), the myotendinous junction (challenging to repair directly), the tendinous portion, or if it is a pure avulsion from the humeral footprint (the most common surgical indication). In this specific patient, the MRI would likely reveal a complete avulsion of the sternocostal head from its humeral insertion, with a fluid-filled gap and medial retraction of the tendon stump, while the clavicular head might remain partially attached but attenuated. Ultrasound is a viable, cost-effective alternative in the acute setting and offers the advantage of dynamic assessment, but it is highly operator-dependent and generally provides less comprehensive anatomical detail for preoperative templating compared to MRI.
Exhaustive Differential Diagnosis
When evaluating a young, athletic male presenting with acute anterior shoulder pain and weakness following a heavy lifting event, the differential diagnosis must be broad but systematically narrowed through precise clinical examination and imaging. While a pectoralis major rupture is the leading hypothesis, several other pathologies can mimic this presentation and must be definitively excluded to avoid inappropriate management.
The most critical alternative diagnoses include acute rotator cuff tears (specifically the subscapularis), ruptures of the long head of the biceps tendon, and rare congenital or traumatic anomalies of the regional musculature. A subscapularis tear can present with profound weakness in internal rotation; however, it is typically associated with increased passive external rotation and positive specific tests such as the lift-off or belly-press tests, which differ from the adduction weakness seen in pectoralis tears. A long head of the biceps rupture often presents with an audible pop and ecchymosis, but the classic "Popeye" deformity is located distally in the anterior brachium, and supination strength is primarily affected.
Below is a comprehensive comparison of the primary differential diagnoses:
| Differential Diagnosis | Key Historical Feature | Differentiating Clinical Signs | Diagnostic Imaging Findings |
|---|---|---|---|
| Pectoralis Major Rupture | Bench press injury; eccentric loading. | Loss of anterior axillary fold; weakness in adduction/internal rotation. | MRI: Medial retraction of PMM tendon; empty humeral footprint. |
| Subscapularis Tear | Forced external rotation of an adducted arm. | Increased passive ER; positive lift-off and belly-press tests. | MRI: Disruption of subscapularis tendon at lesser tuberosity; biceps subluxation. |
| Long Head Biceps Rupture | Sudden load on flexed elbow; older demographic. | "Popeye" muscle deformity in mid-arm; weakness in supination. | MRI/US: Empty bicipital groove; retracted biceps tendon distally. |
| Pectoralis Minor Rupture | Direct trauma or violent shoulder extension. | Tenderness over coracoid process; scapular dyskinesia. | MRI: Edema/disruption at coracoid attachment; PMM intact. |
| Poland Syndrome | Congenital; present since birth. | Unilateral hypoplasia of chest wall; syndactyly often present. | Clinical diagnosis; imaging shows complete absence of PMM without edema. |
Complex Surgical Decision Making and Classifications
The decision to proceed with operative intervention in pectoralis major ruptures is predicated on a combination of the patient's functional demands, chronicity of the injury, and the precise anatomic location of the tear. For this young, highly active, weight-lifting patient, the indication for surgical repair is absolute. Non-operative management in this demographic yields unacceptably poor outcomes, with patients experiencing a permanent 30% to 50% deficit in adduction and internal rotation strength, persistent cosmetic deformity, and an inability to return to high-level athletic endeavors. Conversely, acute surgical repair (performed within 3 to 6 weeks of injury) reliably restores near-normal strength, function, and cosmesis.
To guide the surgical strategy, the injury is typically categorized using the Tietjens classification or the Bak classification system. These systems classify injuries based on the anatomical site of failure: Type I (muscle contusion), Type II (muscle belly tear), Type III (myotendinous junction tear), Type IV (tendinous tear), Type V (tendon avulsion from bone), and Type VI (bony avulsion). Our patient likely presents with a Type V injury—a pure tendinous avulsion from the humeral footprint. This is the most amenable to primary anatomic repair. Myotendinous junction tears (Type III) present a more complex surgical challenge, often requiring complex suturing techniques (such as a Mason-Allen or Krackow stitch) to grasp the friable muscle-tendon interface, and may necessitate augmentation with allograft tissue if tissue quality is poor.
Timing is a critical variable in the surgical decision-making matrix. Acute repairs, defined as those undertaken within the first 3 to 4 weeks post-injury, allow for direct mobilization of the tendon stump and primary fixation to the bone. However, if the diagnosis is delayed and the injury becomes chronic (greater than 6 weeks), the muscle belly undergoes significant contracture, and the tendon stump becomes encased in dense, fibrotic scar tissue. In chronic cases, direct primary repair is often impossible due to the inability to mobilize the tendon back to its native footprint without excessive, repair-compromising tension. These scenarios demand advanced reconstructive techniques utilizing allografts—commonly Achilles tendon with a bone block, or robust hamstring autografts/allografts—to bridge the defect between the retracted muscle and the humerus. Given our patient's presentation at day three, he is in the optimal window for an acute, primary anatomic repair.
Step-by-Step Surgical Technique and Intervention
The surgical repair of a pectoralis major avulsion is a meticulous procedure that requires a thorough understanding of the anterior shoulder anatomy and precise execution of soft tissue fixation. The patient is typically placed in the beach-chair position, though a supine position with a radiolucent arm board can also be utilized depending on surgeon preference. The entire upper extremity is prepped and draped free to allow for dynamic manipulation of the shoulder during the procedure. A standard deltopectoral approach is utilized. The skin incision is made following the Langer lines over the deltopectoral groove, extending from the coracoid process distally toward the deltoid tuberosity.
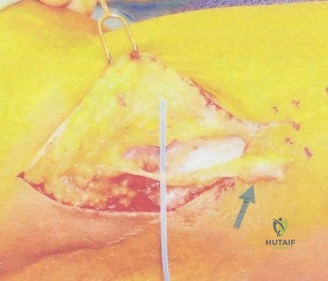
Upon dividing the subcutaneous tissues, the cephalic vein is identified. It is generally mobilized laterally with the deltoid to protect its venous drainage, though medial retraction is acceptable if the venous tributaries dictate. The deltopectoral interval is developed, revealing the underlying clavipectoral fascia. At this stage, the hematoma is typically encountered and evacuated. The surgeon must then locate the retracted stump of the pectoralis major tendon. In acute cases, the stump is usually found medially, tethered by the intact superficial fascia. Heavy, non-absorbable traction sutures (such as #2 FiberWire or equivalent high-tensile strength suture) are placed into the tendon edge using a locked, running Krackow or grasping Mason-Allen configuration. This allows the surgeon to apply lateral traction and assess the excursion of the tendon. Care must be taken during medial mobilization to identify and protect the medial and lateral pectoral nerves, which innervate the muscle.
Attention is then turned to the humeral footprint. The native insertion site is located on the lateral lip of the bicipital groove, lateral to the long head of the biceps tendon. The footprint is meticulously cleared of residual soft tissue and decorticated using a high-speed burr or a curette to expose a bleeding, cancellous bone bed, which is vital for robust tendon-to-bone healing. Fixation can be achieved via several methods: traditional bone troughs, suture anchors, or cortical button fixation. Recent biomechanical studies have demonstrated that unicortical button fixation (using a pectoralis-specific plate or button) combined with high-strength sutures provides superior ultimate load-to-failure and minimizes gap formation compared to traditional anchor constructs.
If using cortical buttons, drill holes are placed along the decorticated footprint. The traction sutures from the tendon are passed through the buttons, which are then shuttled through the near cortex and flipped against the far cortex (or endosteal surface, depending on the specific implant design). The arm is then positioned in slight internal rotation and adduction to remove tension from the repair. The sutures are tensioned and tied sequentially, bringing the broad tendon stump firmly down to the bleeding bone bed. The surgeon then takes the shoulder through a gentle, controlled range of motion to confirm the security of the repair and to establish the safe postoperative limits of external rotation and abduction. The wound is irrigated copiously and closed in layers, often utilizing a subcutaneous drain to prevent hematoma accumulation.
Strict Post-Operative Protocol and Rehabilitation Stages
The postoperative rehabilitation protocol following a pectoralis major repair is a delicate balance between protecting the healing tendon-to-bone interface and preventing debilitating adhesive capsulitis. The protocol is strictly phased and requires immense patient compliance, which can be challenging in a highly motivated, weight-lifting demographic eager to return to the gym.
Phase 1: Maximum Protection (Weeks 0 to 6)
Immediately post-operatively, the patient is placed in a specialized shoulder immobilizer or a sling with an abduction pillow, maintaining the arm in internal rotation and slight anterior flexion. Absolute immobilization is maintained for the first 2 weeks, with the exception of elbow, wrist, and hand range of motion exercises to prevent distal stiffness. At week 3, gentle passive range of motion (PROM) is initiated. The absolute limits during this phase are strictly defined by the intraoperative tension assessment: typically, forward flexion is limited to 90 degrees, and external rotation is strictly limited to neutral (0 degrees) with the arm at the side. Active internal rotation, extension, and adduction are completely prohibited to prevent premature eccentric loading of the repair.
Phase 2: Active-Assisted and Active ROM (Weeks 6 to 12)
At the 6-week mark, the sling is formally discontinued. The patient transitions from passive to active-assisted range of motion (AAROM), utilizing pulleys and wand exercises. External rotation is gradually progressed, aiming for 30 to 40 degrees by week 8, and full symmetric external rotation by week 12. Active range of motion (AROM) is initiated around week 8, focusing on concentric motion without resistance. The physical therapist must closely monitor for compensatory scapular dyskinesia, ensuring the patient is not substituting periscapular motion for true glenohumeral kinematics. Submaximal isometric strengthening for the rotator cuff and deltoid can begin late in this phase, but direct pectoralis major loading remains contraindicated.
Phase 3: Progressive Strengthening (Months 3 to 6)
Once full, painless active range of motion is achieved (typically around 12 weeks), the patient enters the strengthening phase. This begins with light, high-repetition isotonic exercises using resistance bands and light dumbbells. The focus is on muscular endurance and restoring the functional kinetic chain. Closed kinetic chain exercises, such as wall push-ups, can be introduced at month 4, gradually progressing to modified floor push-ups. Heavy eccentric loading and explosive plyometric movements are strictly avoided.
Phase 4: Return to Sport and Heavy Lifting (Months 6+)
Return to heavy resistance training, specifically the barbell bench press, is not permitted until at least 6 months post-operatively, and often closer to 9 months for maximal loads. When the patient is cleared to return to the bench press, strict biomechanical modifications must be enforced to prevent re-rupture. The patient must adopt a narrower grip to reduce the lever arm and limit the degree of shoulder abduction and external rotation. Furthermore, the depth of the eccentric phase should be restricted; utilizing a "floor press" technique or placing a board on the chest (board presses) prevents the humerus from extending past the coronal plane of the torso, thereby protecting the vulnerable sternocostal fibers from maximal excursion.
High-Yield Clinical Pearls and Pitfalls
Mastering the diagnosis and management of pectoralis major ruptures requires an appreciation of several nuanced clinical pearls and the avoidance of common, potentially devastating pitfalls.
Pearl 1: The Anatomy of the Footprint. The most critical anatomical concept for the surgeon is the bilaminar nature of the pectoralis major insertion. The clavicular head inserts anteriorly and distally, while the sternocostal head twists to insert posteriorly and proximally. When performing an anatomic repair, the surgeon must recreate this broad, overlapping footprint to restore the native biomechanics. Failure to recognize the proximal extent of the sternocostal insertion will result in a non-anatomic repair that alters the length-tension relationship of the muscle, leading to permanent weakness and increased risk of failure.
Pitfall 1: The "Intact Fascia" Illusion. As highlighted in the clinical examination section, the most common reason for a missed diagnosis in the emergency department or primary care setting is the palpation of the intact superficial fascia. Examiners feel this tight band in the axilla and erroneously conclude the tendon is intact. Always palpate deep to this fascial layer and rely on the loss of the axillary fold and specific weakness in adduction/internal rotation.
Pearl 2: Suture Management in Friable Tissue. In cases where the tear occurs at the myotendinous junction rather than a clean bony avulsion, standard simple sutures will pull through the friable muscle tissue. The surgeon must utilize locking, grasping stitch configurations like the Krackow or Mason-Allen, and consider incorporating a biological patch (such as an acellular dermal matrix) to augment the repair and distribute the tension across a wider surface area of the muscle belly.
Pitfall 2: Iatrogenic Nerve Injury. During the medial mobilization of a chronically retracted tendon stump, aggressive blunt dissection can easily stretch or avulse the medial and lateral pectoral nerves. The medial pectoral nerve, which pierces the pectoralis minor to innervate the sternocostal head of the pectoralis major, is particularly vulnerable. Meticulous, sharp dissection and direct visualization are mandatory when mobilizing the muscle belly from the underlying chest wall to prevent devastating denervation of the repaired muscle.
By adhering to these rigorous diagnostic algorithms, respecting the complex anatomical biomechanics, and executing a meticulous surgical repair followed by a disciplined rehabilitation protocol, orthopedic surgeons can reliably return these high-demand athletes to their pre-injury levels of performance.
Clinical & Radiographic Imaging Archive
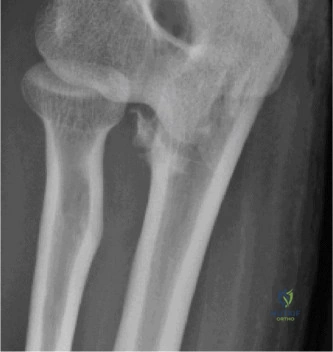
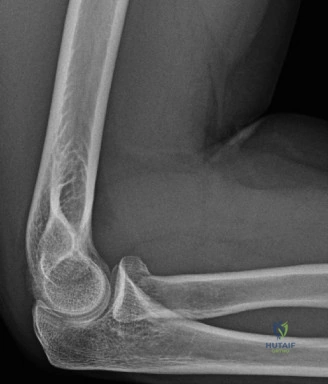
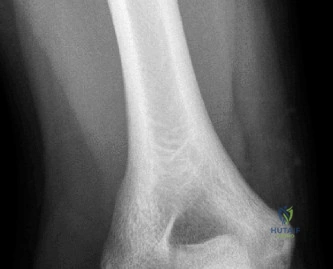
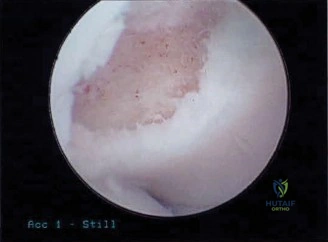


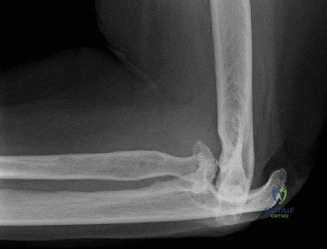
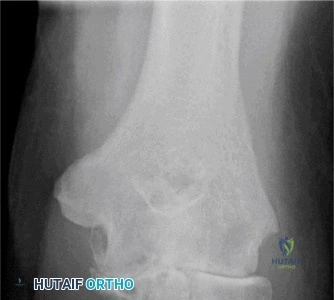
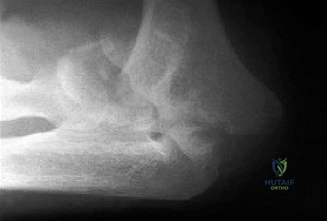
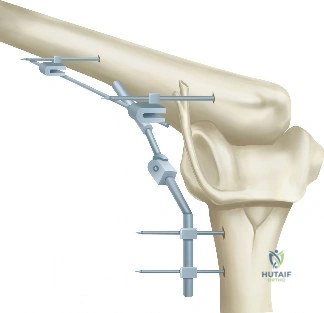
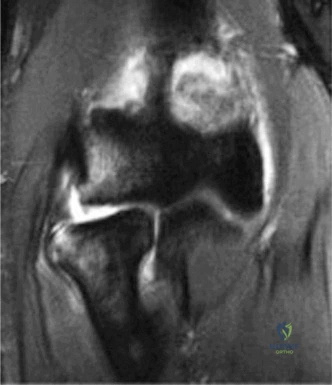
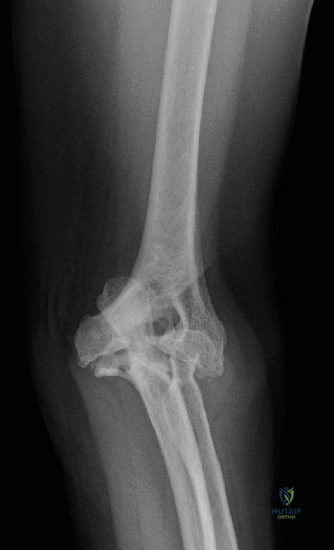
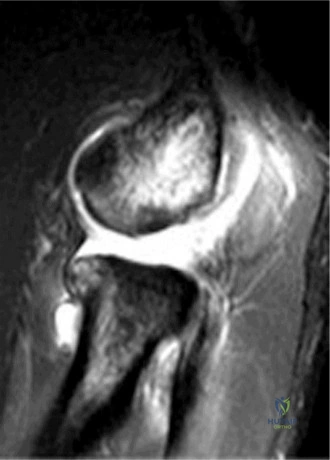
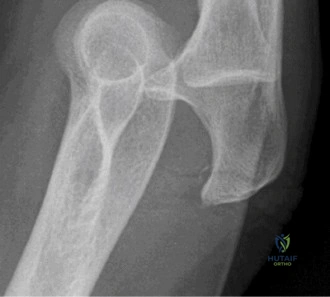
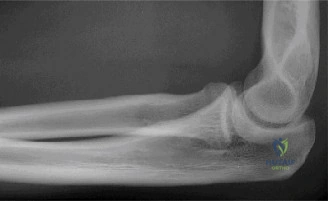
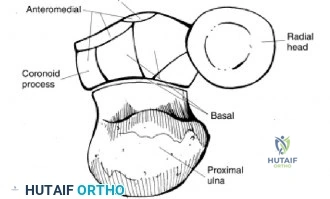
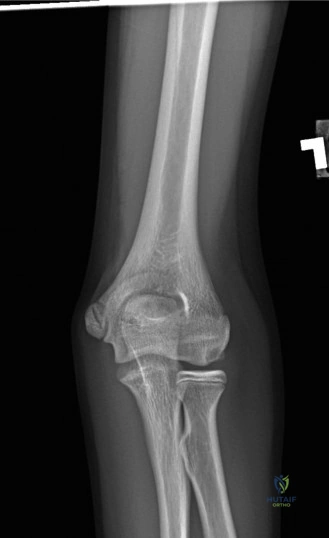
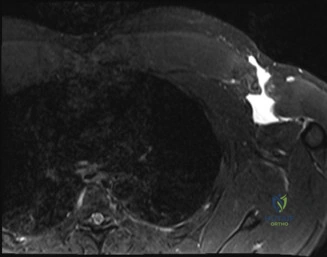
Detailed Chapters & Topics
Dive deeper into specialized chapters regarding shoulder-and-elbow-cases-4
