Solve Shoulder & Elbow Cases: When a Patient Presents to Clinic
Key Takeaway
We review everything you need to understand about Solve Shoulder & Elbow Cases: When a Patient Presents to Clinic. When a 72-year-old male with a history of diabetes presents to clinic 8 months post-total shoulder arthroplasty with worsening pain, a CT arthrogram of the left shoulder is the most appropriate initial next step. This imaging helps evaluate for component loosening, which can indicate an underlying infection or mechanical issue, guiding further management despite other negative findings.
Detailed Patient Presentation and Mechanism of Injury
The patient is a 72-year-old, right-hand-dominant male who presents to the orthopaedic clinic seeking a second opinion for insidious, worsening left shoulder pain. His surgical history is significant for a left anatomic total shoulder arthroplasty (TSA) performed eight months prior at an outside institution for primary glenohumeral osteoarthritis. According to the patient and his available medical records, the index procedure was technically uncomplicated, and the immediate postoperative recovery period was devoid of major acute complications such as dislocation, periprosthetic fracture, or catastrophic wound dehiscence. However, the patient reports a highly concerning historical detail: he has never been completely pain-free since the surgical intervention. The pain has progressively transitioned from a dull, deep ache to a sharp, mechanically limiting pain that exacerbates with any attempted active or passive motion. He explicitly denies any recent traumatic events, falls, or sudden lifting injuries that would suggest an acute mechanical failure or periprosthetic fracture.
A thorough review of systems reveals a complete absence of constitutional symptoms. The patient denies fevers, chills, night sweats, unexplained weight loss, or any history of drainage, erythema, or delayed healing at the surgical incision site. His past medical history is highly relevant, featuring type 2 diabetes mellitus (HbA1c currently at 7.8%), essential hypertension, and coronary artery disease requiring a previous percutaneous coronary intervention. The presence of type 2 diabetes is a critical factor in this presentation; the microvascular compromise and altered host immune response inherent to diabetes significantly elevate the risk of both acute and indolent periprosthetic joint infections (PJI). Furthermore, the patient's demographic profile—an older male—places him in a higher risk category for specific low-virulence shoulder infections.
The mechanism of the current pathology is not driven by acute macrotrauma but rather by a chronic, insidious biological or biomechanical failure. In the context of a painful shoulder arthroplasty that has never achieved a pain-free state, the surgeon must maintain an exceedingly high index of suspicion for an indolent periprosthetic infection, particularly caused by Cutibacterium acnes (formerly Propionibacterium acnes) or coagulase-negative Staphylococcus. These organisms are notorious for their ability to form robust biofilms on orthopaedic implants without eliciting a robust systemic inflammatory response. Unlike highly virulent organisms such as Staphylococcus aureus, which typically present with acute erythema, fluctuance, and systemic sepsis, indolent organisms often present merely as persistent pain, progressive stiffness, and subtle radiographic loosening, masquerading as aseptic failure.
Comprehensive Clinical Examination Findings
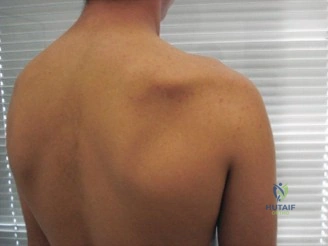
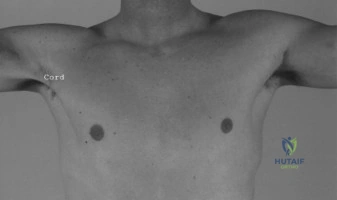
Upon physical examination, the patient’s left shoulder demonstrates a well-healed standard deltopectoral surgical incision. There is absolutely no evidence of current or prior wound breakdown, sinus tract formation, erythema, or localized calor. The soft tissue envelope appears intact, though there is mild, diffuse tenderness to deep palpation extending over the anterior joint line and the proximal humerus. Palpation of the acromioclavicular joint and the biceps groove does not elicit focal point tenderness, helping to rule out isolated pathology in these specific anatomical zones. The absence of a prominent anterior soft tissue mass or fluctuance further supports the lack of a fulminant, purulent infectious process.
Range of motion (ROM) testing reveals profound deficits in both active and passive arcs, indicative of global capsular contracture or mechanical impingement secondary to component loosening. Active forward elevation is limited to 70 degrees, with passive forward elevation reaching only 85 degrees before a firm, painful endpoint is encountered. External rotation with the arm at the side is remarkably restricted to 5 degrees actively and 10 degrees passively, compared to 45 degrees on the contralateral, non-operative side. Internal rotation is limited to the sacrum. This significant discrepancy between expected postoperative ROM and the patient's current stiffness is a hallmark of the "stiff, painful arthroplasty," which demands rigorous investigation to differentiate between adhesive capsulitis, component malposition, and occult infection.
Neurologic and vascular examinations of the left upper extremity are entirely within normal limits. The axillary nerve is clinically intact, evidenced by robust, symmetric contraction of the anterior, middle, and posterior heads of the deltoid, with no areas of localized atrophy. Evaluation of the remaining rotator cuff musculature is challenging due to pain but is critical. The belly-press and lift-off tests for subscapularis integrity are equivocal; the patient exhibits weakness, but it is difficult to ascertain whether this is due to true tendinous failure (a known complication of the deltopectoral approach) or pain inhibition. Supraspinatus testing via the empty can test yields profound pain but suggests continuity of the tendon. Distal pulses (radial and ulnar) are 2+ and symmetric, with brisk capillary refill, confirming adequate distal perfusion despite the patient's history of coronary artery disease and diabetes.
Advanced Imaging and Diagnostics (X-ray, CT, MRI, Templating)
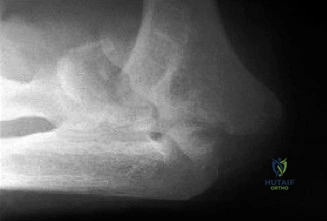
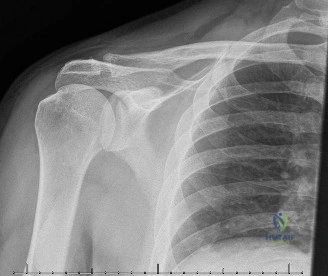
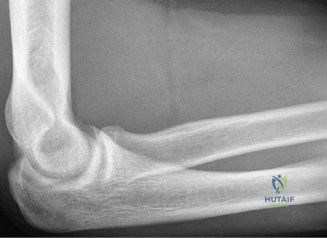
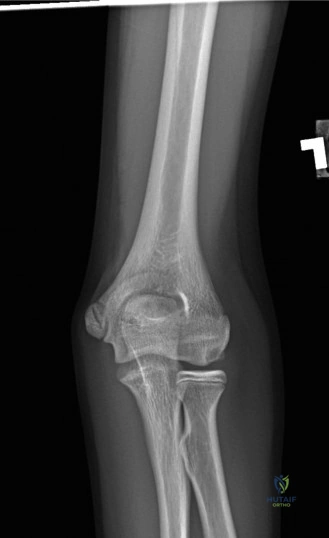
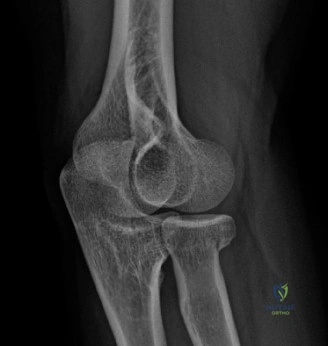
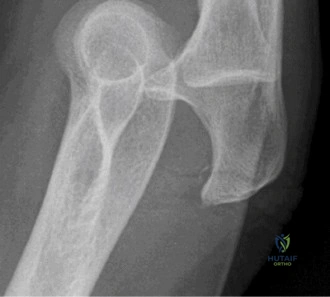
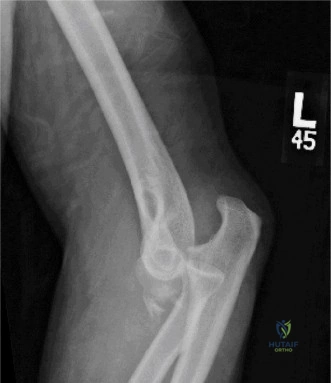
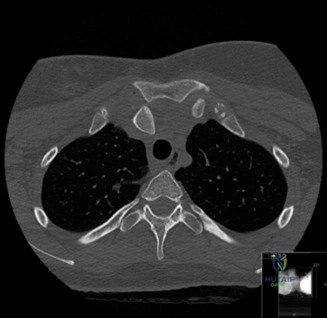
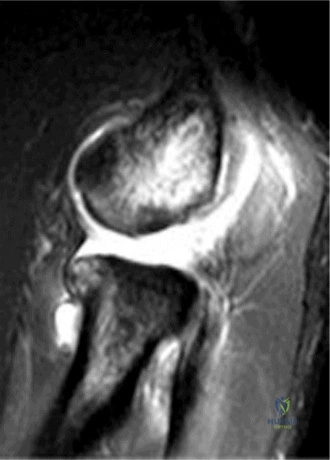
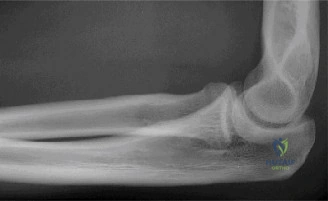
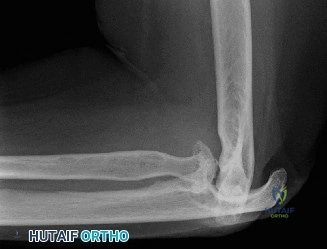
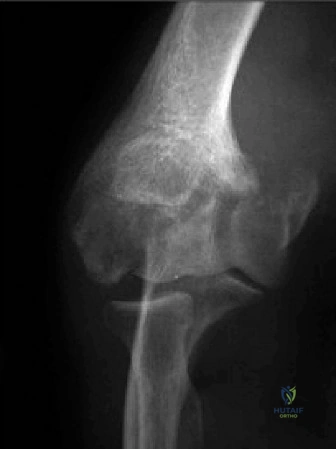
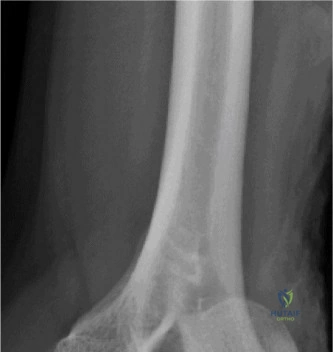
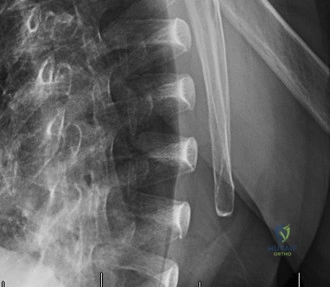
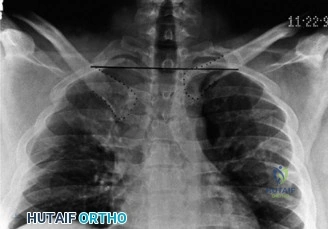
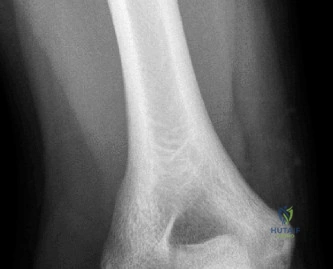
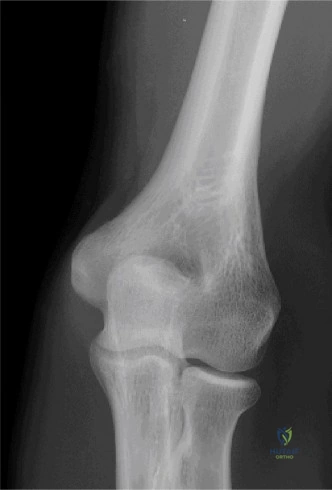
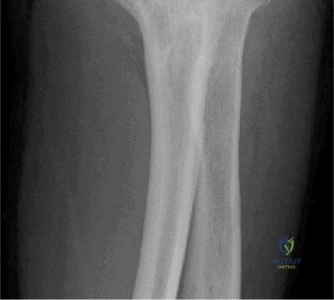
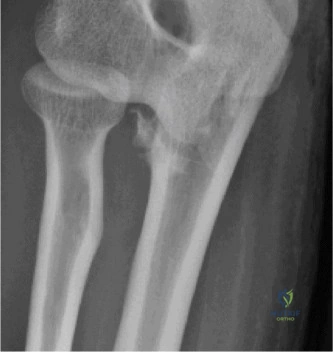
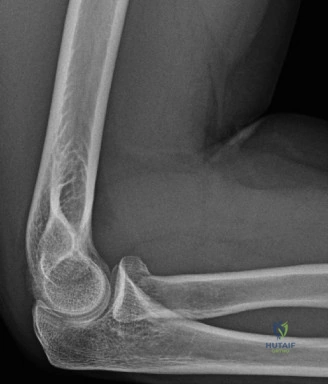
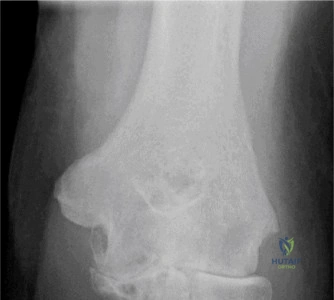
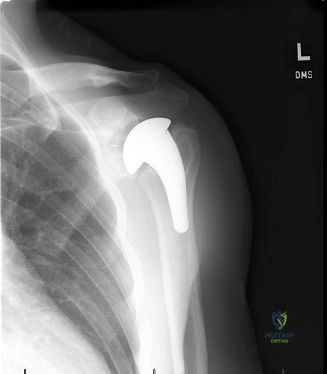
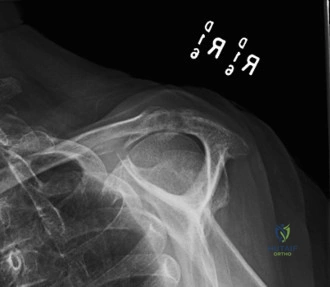
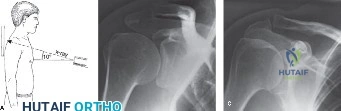
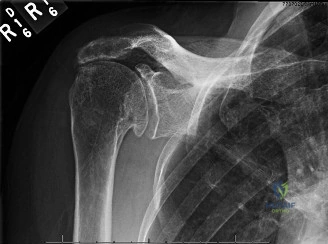
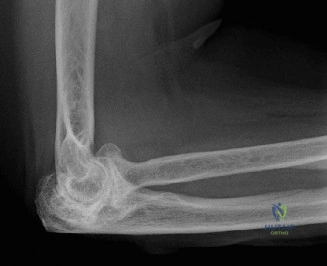
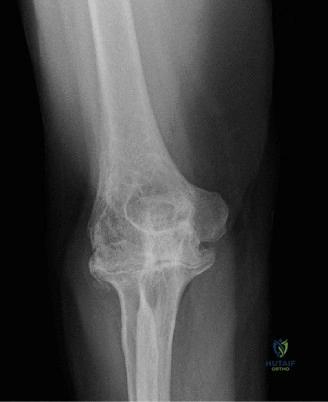
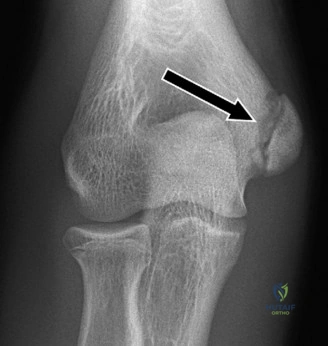
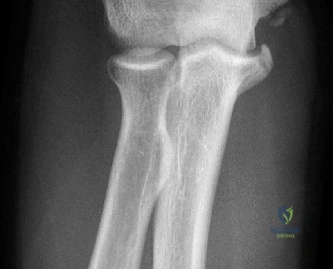
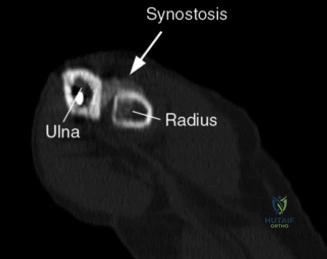
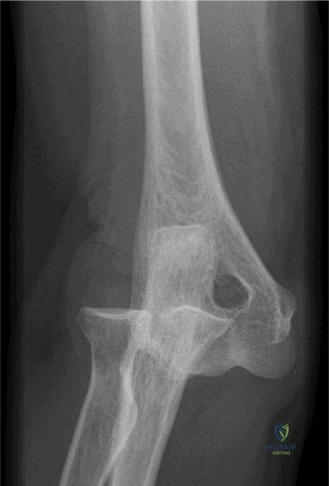
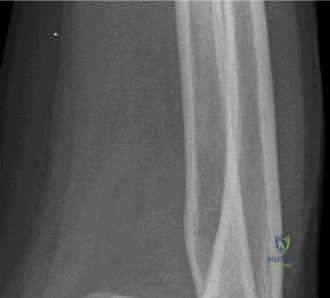
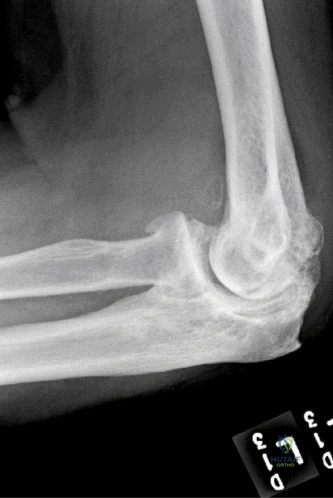
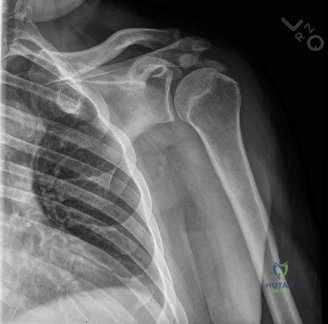
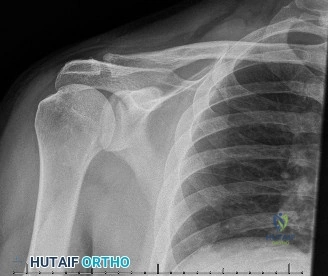
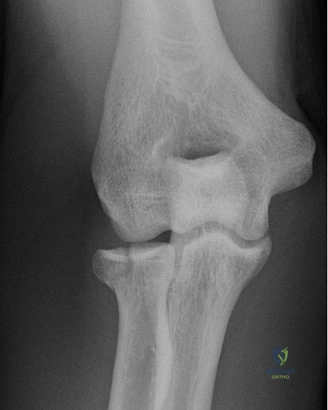
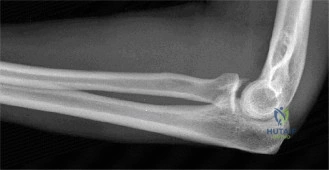
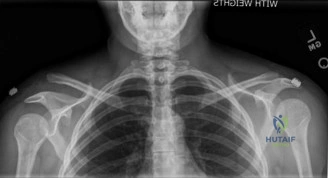
The diagnostic algorithm for a painful total shoulder arthroplasty must be methodical and exhaustive. Initial evaluation begins with high-quality, orthogonal plain radiographs, including a true anteroposterior (Grashey) view, an axillary lateral view, and a scapular Y view. In this patient, radiographs reveal the presence of an anatomic total shoulder construct. Careful scrutiny of the bone-implant interfaces is paramount. While the humeral stem appears well-fixed with no obvious subsidence or radiolucent lines, the glenoid component demonstrates a subtle, 1.5 mm continuous radiolucent line surrounding the central peg and peripheral keels. This finding is highly suspicious for glenoid component loosening, which is the most common mode of mechanical failure in anatomic TSA, but in this clinical context, it raises the specter of septic loosening.
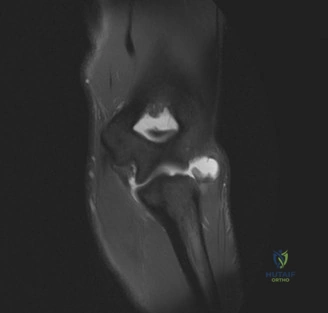
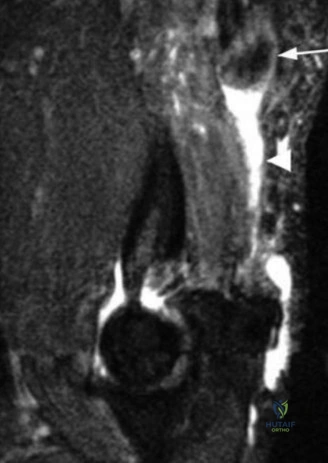
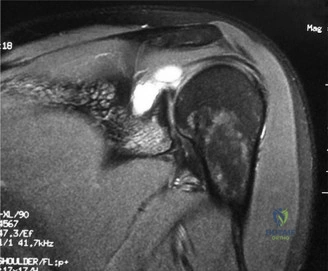
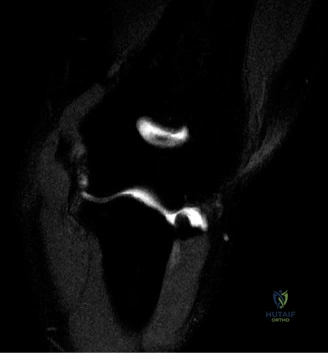
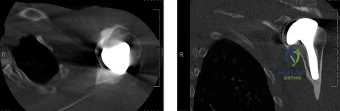
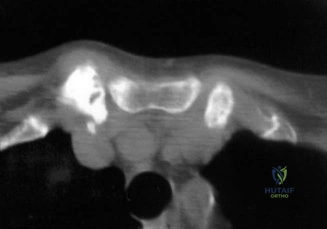
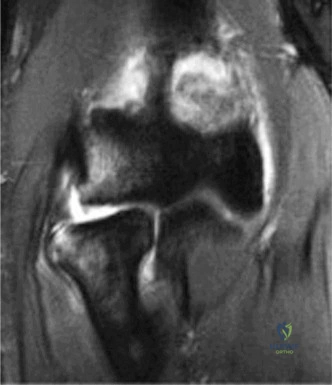
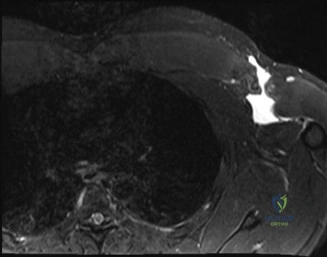
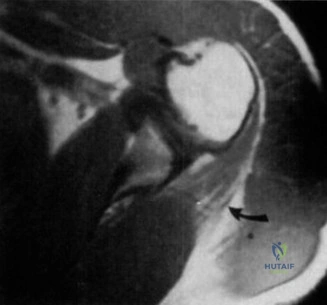
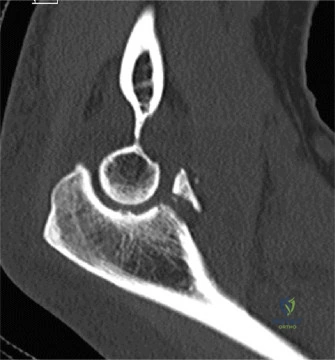
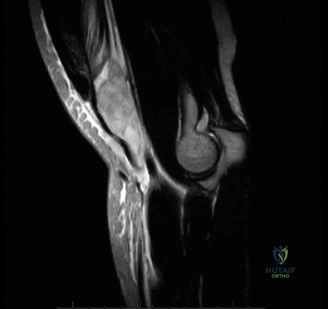
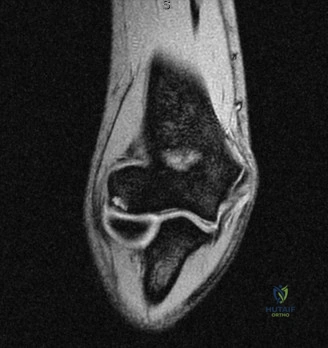
To further delineate the pathology, a CT arthrogram of the left shoulder is ordered. This is the most appropriate next step in management, as established in the primary clinical vignette. The CT arthrogram serves a dual purpose: it provides unparalleled high-resolution, three-dimensional assessment of periprosthetic bone stock and component micro-motion, while the intra-articular contrast allows for the evaluation of capsular integrity and the presence of loosening. If contrast is seen tracking between the glenoid component and the native bone bed, loosening is definitively confirmed. Furthermore, the CT arthrogram is superior to MRI in this specific scenario because standard MRI is heavily degraded by metal artifact (even with MARS protocols), making the assessment of the immediate periprosthetic interface difficult. The CT scan confirms contrast extravasation behind the glenoid component, confirming gross loosening, and demonstrates eccentric posterior wear of the polyethylene, suggesting altered joint kinematics.
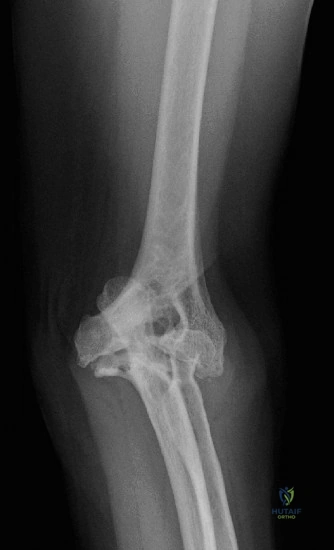
Laboratory diagnostics are subsequently obtained, yielding a C-reactive protein (CRP) of <3 mg/L (normal) and an erythrocyte sedimentation rate (ESR) of 45 mm/hr (mildly elevated). This discordant inflammatory marker profile is a classic trap in shoulder orthopaedics. Unlike hip and knee PJI, where ESR and CRP are highly sensitive, shoulder infections—particularly those driven by C. acnes—frequently present with completely normal serum inflammatory markers. Relying solely on these labs will lead to a missed diagnosis. Because the patient continues to have debilitating pain and glenoid loosening is confirmed, an arthroscopic biopsy is performed to obtain deep tissue cultures. The frozen section reveals <5 polymorphonuclear leukocytes (PMNs) per high-power field, and the initial Gram stain is negative. Again, this does not rule out infection. C. acnes is an anaerobic, slow-growing, intracellular bacterium that resides deep within the dermal sebaceous glands and forms tenacious biofilms. Cultures must be held for a minimum of 14 days, as growth often does not occur until days 7 through 11.
Exhaustive Differential Diagnosis
When evaluating a patient with persistent pain and stiffness following a total shoulder arthroplasty, the differential diagnosis must be systematically divided into intrinsic (implant/joint related) and extrinsic (neurologic/cervical) etiologies. The primary intrinsic categories include infection, aseptic loosening, soft tissue failure (rotator cuff tear), and component malposition/instability. Given the patient's presentation of unremitting pain since the time of surgery and radiographic evidence of glenoid loosening, the clinical suspicion heavily leans toward an indolent biological process or a fundamental biomechanical failure.
Aseptic loosening of the glenoid component is the most frequent long-term complication of anatomic TSA, typically driven by eccentric loading, polyethylene wear debris, and subsequent macrophage-mediated osteolysis. However, aseptic loosening usually presents several years postoperatively. Early loosening within the first year, as seen in this 72-year-old patient, is highly abnormal and strongly suggests a failure of initial fixation, thermal necrosis during cementation, or, most critically, an unrecognized periprosthetic joint infection. Soft tissue failure, specifically of the subscapularis tendon, is another major consideration. The subscapularis is typically taken down and repaired during the deltopectoral approach. Failure of this repair leads to anterior instability, weakness in internal rotation, and significant pain. While our patient exhibits some weakness, the primary issue is global stiffness and diffuse pain, making isolated subscapularis failure less likely to be the sole culprit.
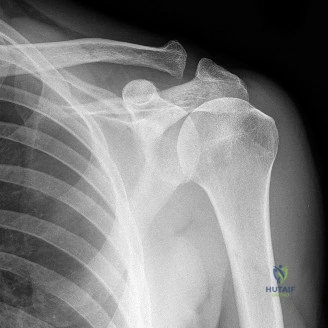
Periprosthetic joint infection (PJI) remains the most devastating and diagnostically challenging differential. The shoulder is a unique microbiological environment, heavily colonized by Cutibacterium acnes, a lipophilic, anaerobic Gram-positive rod. The typical presentation of a C. acnes PJI lacks the classic hallmarks of infection; there is rarely a draining sinus, fever, or acute erythema. Instead, the patient presents exactly like the one in our case: progressive stiffness, unremitting deep pain, and early radiographic loosening. The negative frozen section and normal CRP must be interpreted with extreme caution, as they are notoriously unreliable for low-virulence shoulder pathogens.
| Differential Diagnosis | Key Clinical Findings | Radiographic / Imaging Hallmarks | Laboratory / Pathologic Indicators |
|---|---|---|---|
| Periprosthetic Joint Infection (Indolent) | Unremitting pain since surgery, global stiffness, absence of systemic infectious signs. | Early component loosening (glenoid > humerus), periosteal reaction (rare in shoulder). | Normal/mildly elevated ESR/CRP. Cultures require 14-day hold. Positive alpha-defensin or next-gen sequencing. |
| Aseptic Glenoid Loosening | Pain with active use, feeling of "clunking," typically presents >5 years post-op. | Radiolucent lines >2mm around glenoid peg/keel, component shift, subsidence. | Normal ESR/CRP. Negative intraoperative cultures. Histology shows polyethylene wear debris and macrophages. |
| Subscapularis Repair Failure | Anterior shoulder pain, weakness with internal rotation, increased passive external rotation. | Anterior subluxation of the humeral head on axillary lateral X-ray. | Normal labs. MRI or Ultrasound shows discontinuity of the subscapularis tendon at the lesser tuberosity. |
| Complex Regional Pain Syndrome (CRPS) | Exquisite, disproportionate pain, allodynia, vasomotor changes (skin color/temperature asymmetry). | Periarticular osteopenia on plain radiographs (patchy demineralization). | Normal inflammatory markers. Clinical diagnosis based on Budapest criteria. |
Complex Surgical Decision Making and Classifications
The surgical decision-making process in this scenario is incredibly complex and hinges on the interpretation of the 2018 International Consensus Meeting (ICM) criteria for Shoulder PJI. The shoulder criteria were specifically adapted from the hip and knee guidelines to account for the unique behavior of C. acnes. Under the ICM criteria, definitive PJI is diagnosed if there is a sinus tract, gross purulence, or two positive cultures of the same organism. However, in cases of "probable" or "possible" PJI—where labs are equivocal and frozen sections are negative—the surgeon must rely on clinical judgment and the macroscopic appearance of the joint during surgical exploration. Given the patient's early glenoid loosening and unremitting pain, surgical intervention is mandated.
The primary decision tree involves choosing between a single-stage exchange, a two-stage exchange arthroplasty, or Debridement, Antibiotics, and Implant Retention (DAIR). DAIR is strictly contraindicated in this patient. The DAIR protocol is reserved for acute postoperative infections (typically within 4 weeks of the index procedure) or acute hematogenous seeding in a previously asymptomatic joint. Because this patient has been symptomatic for 8 months ("never completely pain-free"), the infection is chronic, and a mature polymicrobial biofilm has undoubtedly formed on the polyethylene and titanium surfaces. Attempting a DAIR in this setting carries an unacceptably high failure rate, approaching 80-90% in some series.
Therefore, the debate centers on a single-stage versus a two-stage exchange. Single-stage exchange (removing implants, debriding, and immediately placing new implants with antibiotic-loaded cement) is gaining traction in Europe for specific organisms with known sensitivities. However, in North America, particularly for a diabetic patient with early, gross loosening where the organism is technically unidentified at the time of surgery (pending 14-day cultures), the gold standard remains the two-stage exchange arthroplasty. The first stage involves complete explantation of all hardware, radical synovectomy, and placement of an antibiotic-loaded cement spacer. This approach maximizes the eradication of the biofilm, allows for local delivery of high-dose antibiotics, and provides a window to identify the offending pathogen and tailor systemic antimicrobial therapy before reimplantation.
Step-by-Step Surgical Technique and Intervention
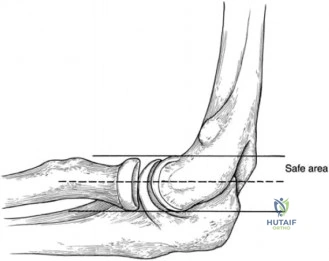
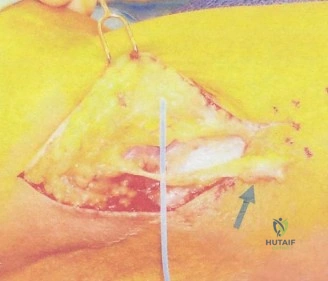
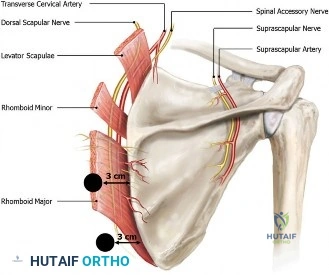
The patient is brought to the operating room and positioned in the modified beach chair position. General endotracheal anesthesia is administered, supplemented by an interscalene regional nerve block for postoperative pain control. Intravenous antibiotics are deliberately withheld until multiple deep tissue cultures are obtained to maximize the diagnostic yield. The previous deltopectoral incision is utilized. Meticulous dissection is required to navigate through the dense, organized scar tissue. The cephalic vein is identified and retracted laterally with the deltoid to preserve its integrity. The clavipectoral fascia is incised, and the conjoined tendon is retracted medially. The axillary nerve is identified at the inferior border of the subscapularis and protected throughout the case.
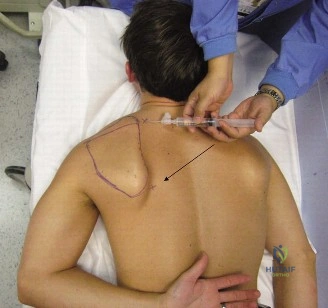
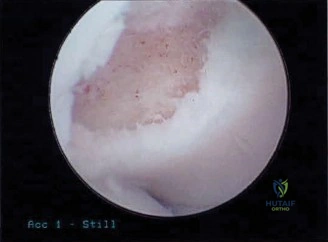
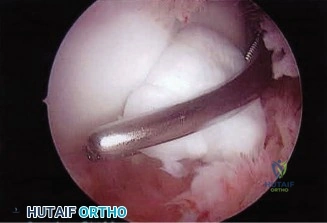
Upon entering the glenohumeral joint, the macroscopic appearance is evaluated. Even in the absence of gross purulence, hypertrophic, friable synovium is highly suggestive of infection. Before any irrigation is utilized, at least five to six distinct deep tissue samples are harvested using clean instruments for each sample. These are sent for aerobic, anaerobic, fungal, and mycobacterial cultures, with explicit instructions to the microbiology laboratory to hold the cultures for 14 days to monitor for C. acnes. Next, the subscapularis is taken down, often revealing compromised tissue quality due to the chronic inflammatory state. The humeral head component is dislocated. If the humeral stem is well-fixed, specialized extraction devices, flexible osteotomes, and potentially an extended deltopectoral approach or a vertical humeral osteotomy may be required to remove the stem without causing a catastrophic periprosthetic fracture.
Once the humeral stem is successfully explanted, attention is turned to the glenoid. The loose polyethylene glenoid component is easily removed. A radical, aggressive synovectomy is performed, excising all devitalized tissue, capsule, and scar. The medullary canal of the humerus and the glenoid vault are sequentially reamed and thoroughly irrigated with 9 liters of pulsatile lavage containing dilute betadine or chlorhexidine. Following debridement, a functional, articulating antibiotic cement spacer is fabricated. Polymethylmethacrylate (PMMA) bone cement is mixed with high doses of heat-stable antibiotics—typically 4 grams of Vancomycin and 3.6 grams of Tobramycin per 40-gram bag of cement. Because C. acnes is suspected, some surgeons may also incorporate Ceftriaxone. The spacer is molded to resemble a humeral head and stem, inserted into the canal, and allowed to cure. The subscapularis is loosely approximated, a surgical drain is placed, and the wound is closed in standard layered fashion.
Strict Post-Operative Protocol and Rehabilitation Stages
The immediate postoperative phase (Weeks 0-6) is focused on infection eradication and protecting the soft tissue envelope. The patient is immobilized in a standard shoulder sling. Physical therapy is strictly limited to passive range of motion (PROM) within a safe zone to prevent debilitating stiffness while ensuring the antibiotic spacer does not dislocate or cause secondary bone loss. Active range of motion (AROM) and heavy lifting are absolutely contraindicated. Concurrently, the patient is evaluated by the Infectious Disease service. Once the 14-day cultures inevitably return positive for C. acnes (as is classic for this clinical picture), a targeted intravenous antibiotic regimen is initiated. This typically involves 6 weeks of IV Penicillin G or Ceftriaxone, administered via a Peripherally Inserted Central Catheter (PICC) line.
The intermediate phase (Weeks 6-12) involves the cessation of intravenous antibiotics followed by an "antibiotic holiday" of 2 to 4 weeks. During this period, the patient is closely monitored clinically for recurrent pain, swelling, or erythema. Serial inflammatory markers (ESR and CRP) are drawn. While these markers may have been normal initially, a significant spike during the antibiotic holiday would indicate failure of eradication. If the clinical exam is benign, the wound is perfectly healed, and the inflammatory markers remain stable, the patient is cleared for Stage 2 of the revision process: reimplantation.
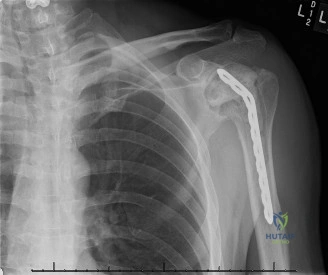
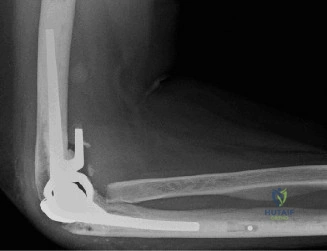
Stage 2 reimplantation nearly always involves conversion to a Reverse Total Shoulder Arthroplasty (rTSA). The rationale for rTSA is multifold: the subscapularis is almost universally incompetent after multiple surgeries and chronic infection, the rotator cuff may be compromised, and there is often significant glenoid bone loss requiring bone grafting and baseplate lateralization. Following the rTSA, the rehabilitation protocol shifts. The patient remains in a sling for 4 weeks to protect the subscapularis repair (if attempted) and baseplate fixation. Early therapy focuses on deltoid isometric recruitment and passive elevation. By week 6, active-assisted ROM begins, progressing to full active ROM and gentle strengthening by week 10-12. The ultimate goal is functional overhead reach and pain-free activities of daily living, though patients must be counseled that their ROM will never equal that of a native, healthy shoulder.
High-Yield Clinical Pearls and Pitfalls
Pearl: Always maintain a high index of suspicion for Cutibacterium acnes in any patient presenting with a stiff, painful shoulder arthroplasty, particularly in males. The absence of classic infectious signs (fever, erythema, elevated CRP) does not rule out a PJI. The history of "never being pain-free" since the index operation is the most reliable clinical indicator of an occult infection.
Pitfall: Relying on intraoperative frozen sections and Gram stains to dictate surgical management in shoulder arthroplasty. C. acnes will almost universally yield a negative Gram stain and a low PMN count on frozen section due to its intracellular nature and biofilm formation. A negative frozen section should never deter the surgeon from performing a thorough debridement and obtaining 14-day cultures.
Pearl: The CT arthrogram is an invaluable tool in the diagnostic workup of the painful TSA. It provides superior visualization of component micro-motion, polyethylene wear, and capsular integrity compared to standard MRI, which is heavily obscured by metal artifact. Contrast extravasation at the implant-bone interface is pathognomonic for loosening.
Pitfall: Attempting a Debridement, Antibiotics, and Implant Retention (DAIR) procedure on a chronic periprosthetic joint infection. If the patient's symptoms have been present for more than 4 weeks, the biofilm is mature and impenetrable to systemic antibiotics. DAIR in this setting will fail, subjecting the patient to unnecessary repeated surgeries and further bone loss. A two-stage exchange is the definitive treatment.
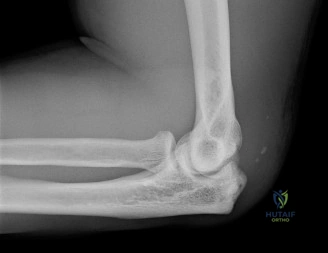
Clinical & Radiographic Imaging Archive