Right Shoulder Pain? Avoid This Common X-ray Mistake.

Key Takeaway
Your ultimate guide to Right Shoulder Pain? Avoid This Common X-ray Mistake. starts here. For acute right shoulder pain following a fall with limited range of motion, and an initial AP X-ray, the next most appropriate step is to obtain an axillary view x-ray. A single AP view is insufficient to conclusively rule out a fracture or a shoulder dislocation, which an axillary view helps to diagnose, guiding proper management.
Comprehensive Introduction and Patho-Epidemiology
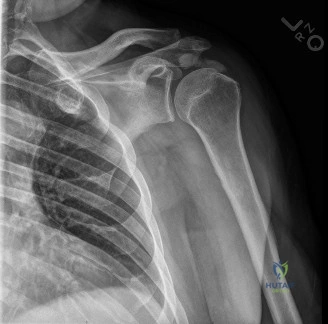
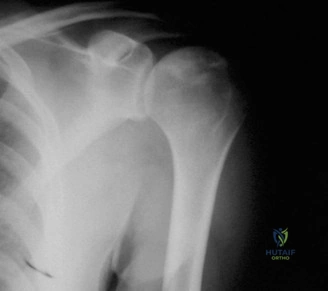
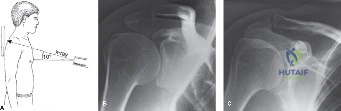
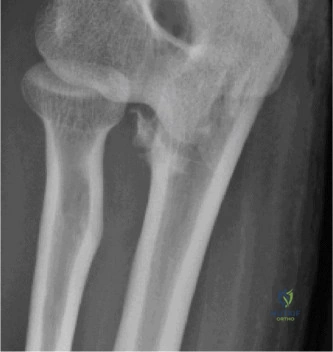
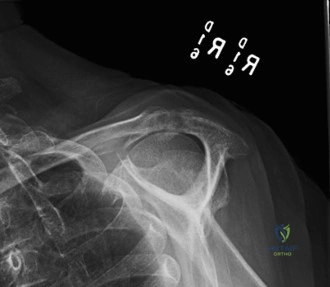
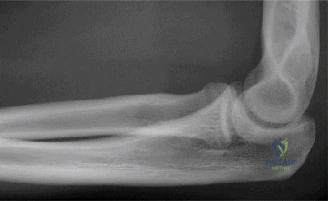
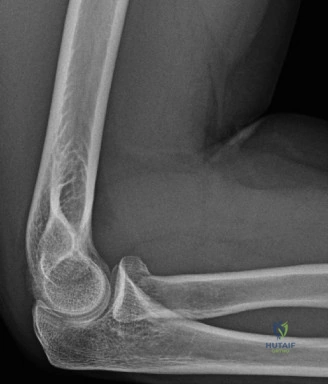
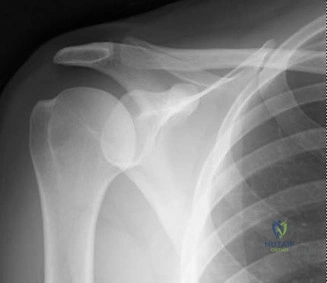
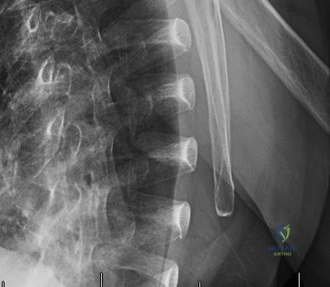
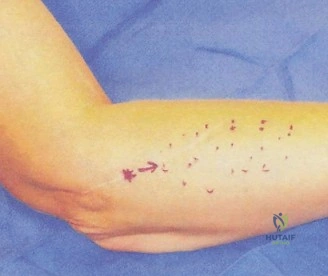
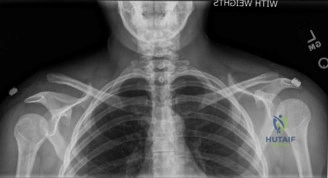
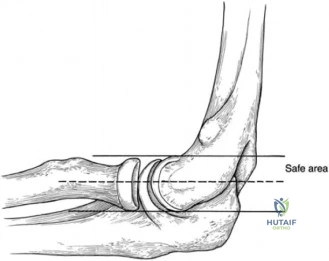
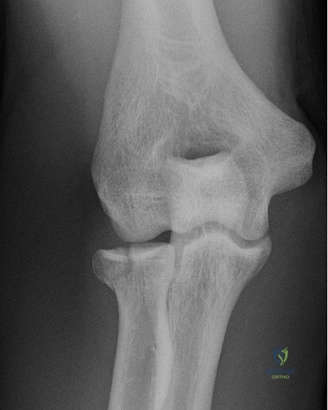
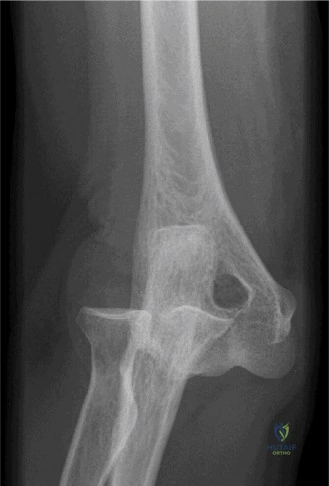
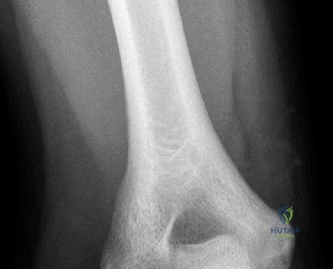
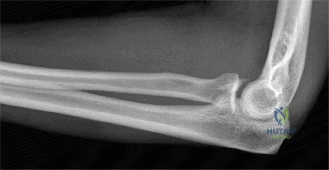
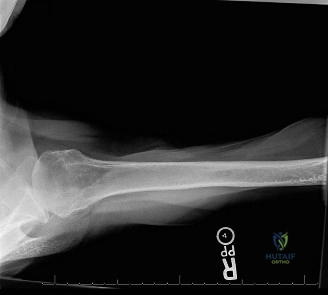
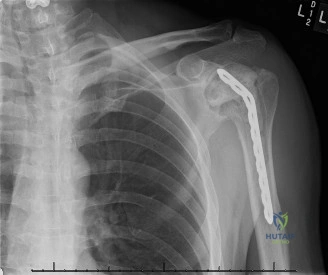
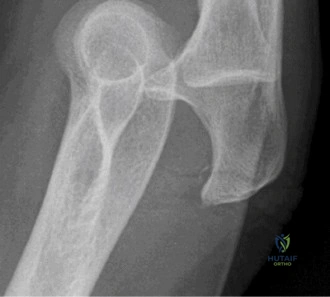
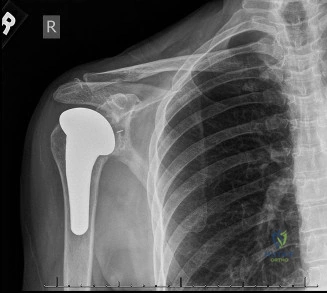
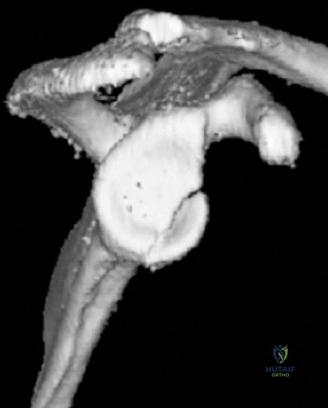
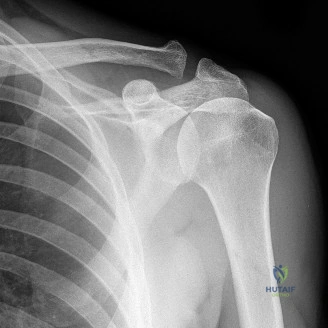
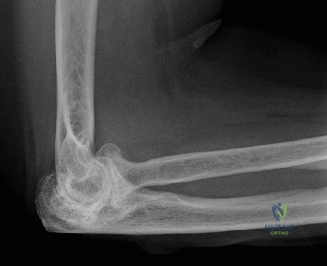
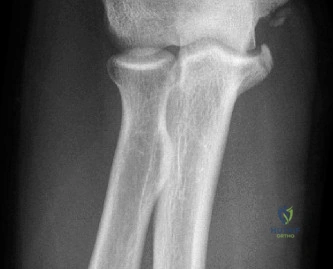
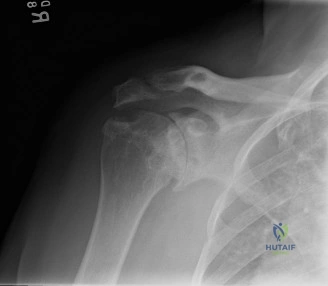
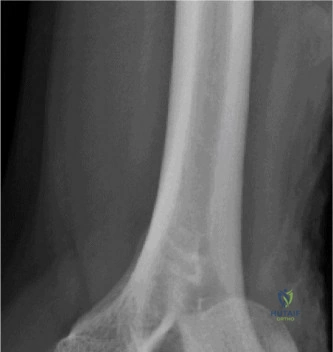
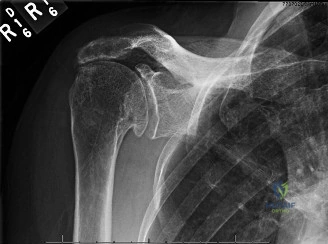
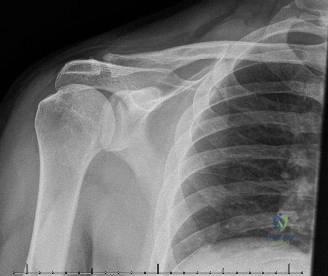
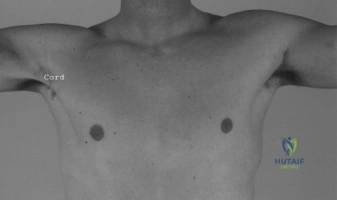
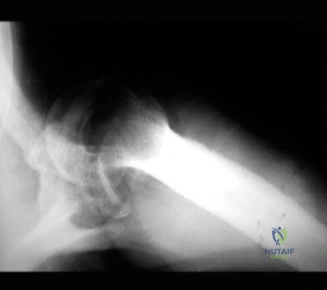
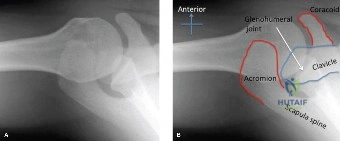
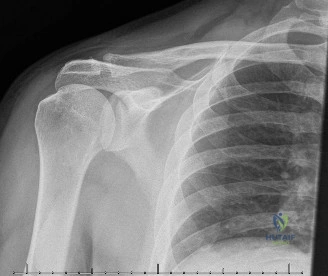
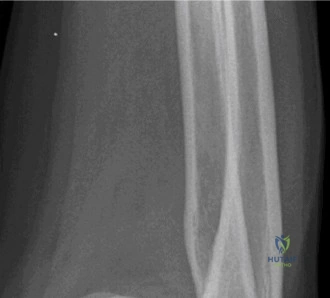
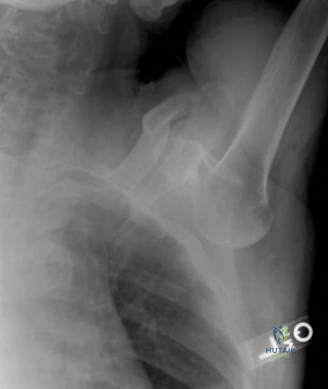
The evaluation of acute shoulder trauma in the emergency department (ED) or urgent care setting is fraught with diagnostic pitfalls, the most egregious of which is the reliance on a single anteroposterior (AP) radiograph. As demonstrated in the clinical scenario of a 33-year-old male presenting after a traumatic sports injury, the acceptance of an isolated AP view is a cardinal error in orthopedic surgery. True orthogonal projections are non-negotiable. The axillary lateral view, or a modified trauma axillary (Velpeau) view, is absolutely critical to accurately assess glenohumeral concentricity. Failure to obtain this view routinely leads to missed posterior dislocations—often masquerading as the deceptive "lightbulb sign" on an AP view—as well as missed anterior subluxations, surgical neck fractures, and lesser tuberosity avulsions. The axiom remains: one view is no view.
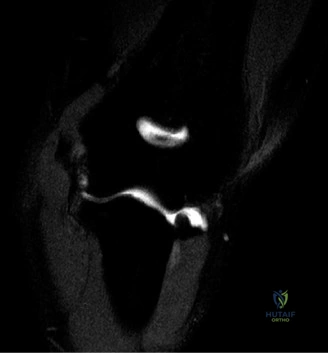
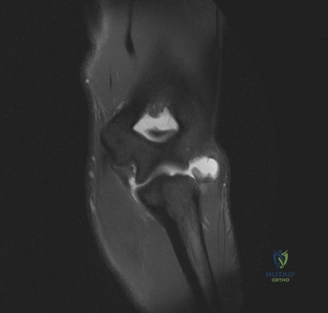
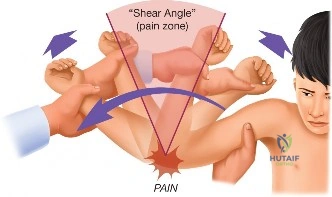
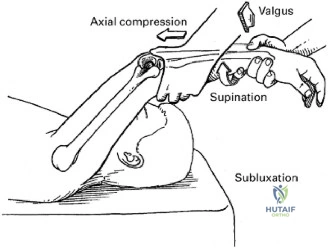
Traumatic anterior instability is a highly prevalent orthopedic pathology, representing the most common major joint dislocation in the human body. Epidemiological data indicates an estimated incidence of 1.7% in the general population, with a significantly higher predilection in young, active, and athletic cohorts. The nomenclature of "instability" encompasses a spectrum of pathology ranging from frank, locked dislocations requiring urgent closed reduction under conscious sedation, to transient, incomplete subluxations that spontaneously reduce on the field of play. Irrespective of the magnitude of the initial displacement, the traumatic event imparts significant sheer and tensile forces across the anteroinferior capsulolabral complex, invariably leading to structural failure.
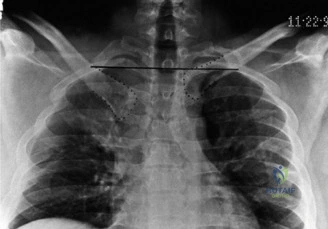
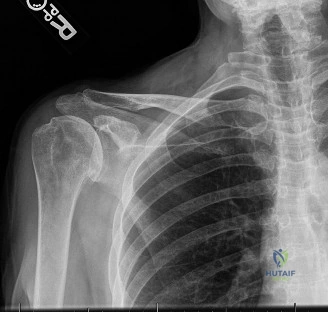
Understanding the natural history and patho-epidemiology of anterior instability is paramount, as it directly dictates the treatment algorithm. The most critical prognostic variable for recurrent instability is the patient's age at the time of the index dislocation. The literature demonstrates a stark, inversely proportional relationship between age and recurrence risk. Patients under the age of 20 face a staggering 90% risk of recurrent dislocation if managed non-operatively. Those between 20 and 40 years of age exhibit a roughly 60% recurrence rate, whereas patients over the age of 40 have a drastically reduced recurrence risk of approximately 10%, though they are at a uniquely high risk for concomitant rotator cuff tears (the "unhappy triad" of the shoulder).
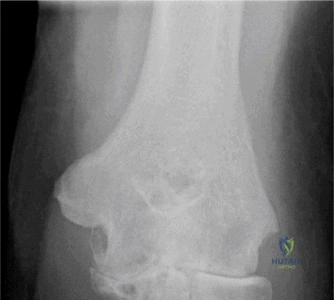
This age-dependent recurrence phenomenon is driven by the robust, highly elastic nature of the collagenous capsule in younger patients, which tends to avulse directly from the glenoid rim (the classic Bankart lesion) rather than stretching or tearing mid-substance. Recurrent instability events are not benign; each subsequent dislocation inflicts cumulative damage to the anterior glenoid rim and the posterolateral humeral head, exacerbating bipolar bone loss. Furthermore, recurrent instability is a well-documented independent risk factor for the development of early-onset glenohumeral osteoarthritis (dislocation arthropathy). Consequently, the modern orthopedic paradigm has shifted toward aggressive, early surgical stabilization in young, high-demand patients to alter the natural history of the disease.
Detailed Surgical Anatomy and Biomechanics
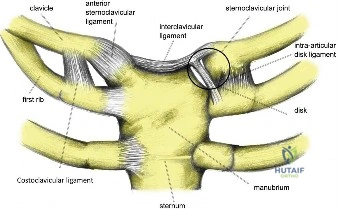
The glenohumeral joint is a masterpiece of evolutionary biomechanics, sacrificing intrinsic bony stability for an unparalleled global range of motion. The osseous anatomy is famously likened to a golf ball sitting on a golf tee. The glenoid fossa is relatively flat, retroverted an average of 2 to 8 degrees, and possesses a surface area that is only one-third that of the articulating humeral head. This inherent osseous incongruity dictates that the joint must rely heavily on a complex interplay of static and dynamic soft-tissue stabilizers to maintain concentric reduction during the extremes of motion required in athletic activities.
The static stabilizers are comprised of the glenoid labrum, the articular capsule, and the glenohumeral ligaments. The labrum is a fibrocartilaginous ring that circumscribes the glenoid rim, effectively deepening the socket by 50% and increasing the articular surface area. It serves as the critical attachment site for the glenohumeral ligaments. The inferior glenohumeral ligament (IGHL) complex is the most biomechanically vital structure in the prevention of anterior instability. Composed of an anterior band, a posterior band, and an interposed axillary pouch, the IGHL functions as a hammock. When the arm is placed in the provocative position of abduction and external rotation (ABER), the anterior band of the IGHL becomes taut, serving as the primary restraint to anterior and inferior humeral translation.
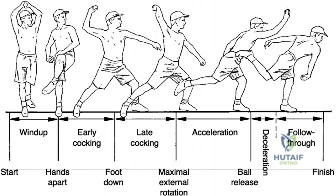
Dynamic stabilization is provided by the rotator cuff musculature and the long head of the biceps tendon. The rotator cuff (supraspinatus, infraspinatus, teres minor, and subscapularis) functions through the mechanism of "concavity compression." By firing symmetrically, these muscles compress the humeral head directly into the deepened concavity of the glenoid fossa, maintaining the center of rotation regardless of the arm's position in space. The subscapularis, in particular, provides a dynamic anterior buttress, while the long head of the biceps acts to depress the humeral head, resisting superior migration during abduction.
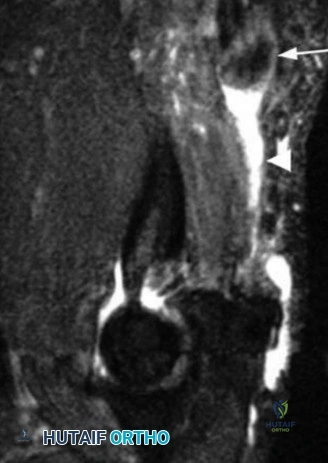
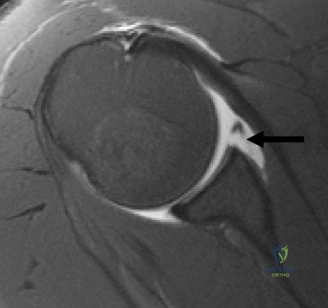
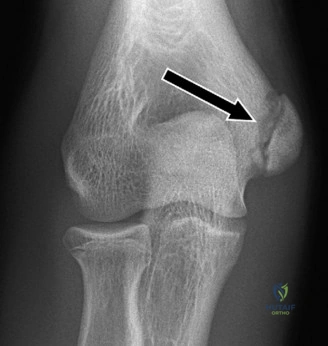
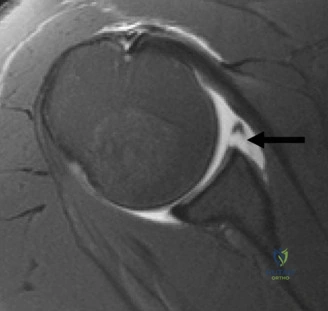
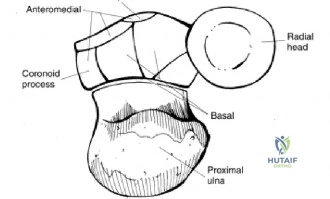
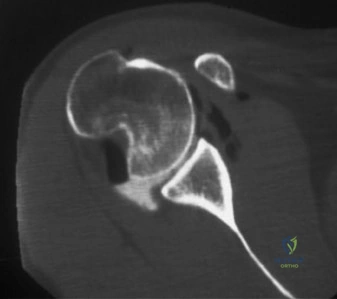
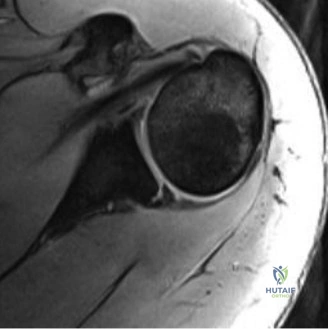
The pathoanatomy of anterior instability involves the catastrophic failure of these stabilizing mechanisms. The essential lesion is the Bankart tear—an avulsion of the anteroinferior capsulolabral complex from the glenoid rim, obliterating the anterior band of the IGHL's anchor point. Variations include the ALPSA (Anterior Labroligamentous Periosteal Sleeve Avulsion) and the GLAD (Glenolabral Articular Disruption) lesions. Concomitantly, as the humeral head dislocates anteriorly, its posterolateral aspect impacts the hard anterior glenoid rim, creating an impaction fracture known as a Hill-Sachs lesion. If the anterior glenoid rim fractures or undergoes attritional wear, the "inverted pear" glenoid morphology develops. The biomechanical interplay between glenoid bone loss and the Hill-Sachs lesion dictates whether the lesion is "engaging" or "non-engaging," fundamentally altering the surgical approach.

Exhaustive Indications and Contraindications
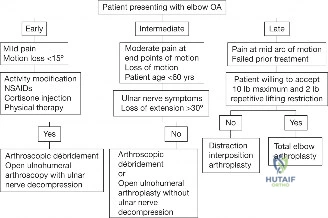
The decision-making process for the surgical management of anterior shoulder instability is highly nuanced, requiring a synthesis of patient demographics, activity demands, and precise pathoanatomical characterization. The primary goal is to restore stability while minimizing the loss of external rotation and preventing the onset of secondary osteoarthritis. The indications for surgical intervention have expanded over the last two decades, moving away from a purely conservative initial approach toward early operative stabilization, particularly in high-risk cohorts.
Indications for Arthroscopic Soft Tissue Stabilization
Arthroscopic Bankart repair is indicated for patients with recurrent anterior instability, or as a primary intervention in young (under 25 years old), highly active individuals or contact athletes following a first-time dislocation. The ideal candidate possesses robust, healthy capsulolabral tissue and minimal osseous defects. Specifically, arthroscopic soft tissue stabilization is appropriate when glenoid bone loss is quantified at less than 15% of the inferior glenoid diameter, and when any concomitant Hill-Sachs lesion is deemed "on-track" (non-engaging). In cases where the Hill-Sachs lesion is large but the glenoid bone loss is minimal, an arthroscopic Bankart repair may be augmented with a Remplissage procedure (capsulotenodesis of the infraspinatus into the humeral defect) to prevent engagement.
Indications for Bony Augmentation Procedures
Bony augmentation, most commonly the Latarjet procedure (coracoid transfer) or distal tibial/iliac crest allografting, is indicated in the presence of critical bone loss. The threshold for "critical" bone loss has historically been cited as 20-25% of the glenoid width, but recent literature suggests that subcritical bone loss (13.5% to 20%) in high-demand contact athletes may also warrant bony augmentation due to unacceptable failure rates with soft-tissue repair alone. The Instability Severity Index Score (ISIS) is frequently utilized; a score of greater than 6 strongly suggests a high risk of recurrence with arthroscopic Bankart repair, thus indicating a Latarjet procedure. Bony procedures are also the gold standard for revision stabilization following a failed prior arthroscopic repair.
Contraindications to Surgical Stabilization
Absolute contraindications to surgical stabilization include active local or systemic infection, severe medical comorbidities precluding anesthesia, and voluntary dislocators with underlying psychiatric overlay who can dislocate their shoulder at will without trauma. Relative contraindications include multidirectional instability (MDI) in the absence of a dedicated, prolonged (minimum 6 months) trial of aggressive physical therapy focused on periscapular and rotator cuff strengthening. Operating on unrecognized MDI with an isolated anterior Bankart repair frequently leads to surgical failure and exacerbated posterior or inferior instability.
| Parameter | Arthroscopic Bankart Repair | Open Latarjet / Bony Augmentation |
|---|---|---|
| Primary Indication | Recurrent instability, young first-time dislocators | Critical bone loss (>15-20%), revision surgery |
| Bone Loss Criteria | < 15% glenoid bone loss, "On-track" Hill-Sachs | > 15-20% glenoid bone loss, "Off-track" Hill-Sachs |
| Patient Profile | Non-contact athletes, overhead athletes | Contact athletes (rugby, football), ISIS score > 6 |
| Contraindications | Critical bone loss, engaging Hill-Sachs, poor tissue | Seizures (relative), elderly patients with cuff tears |
| Expected ROM Loss | Minimal to moderate loss of External Rotation | Minimal loss of External Rotation |
Pre-Operative Planning, Templating, and Patient Positioning
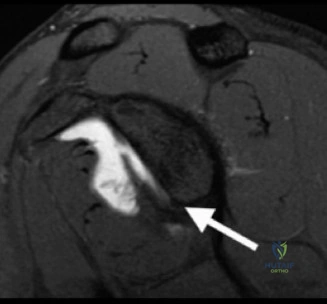
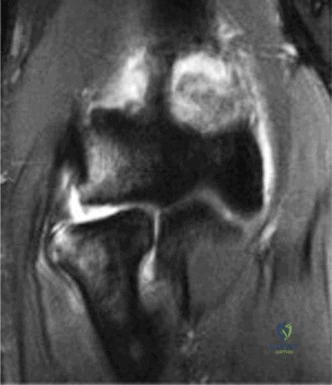
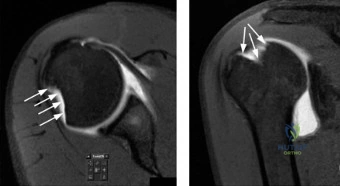
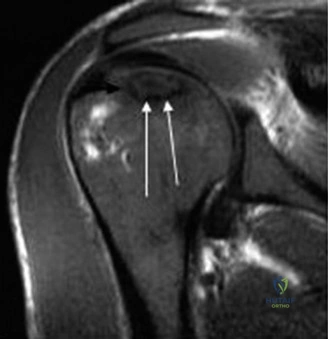
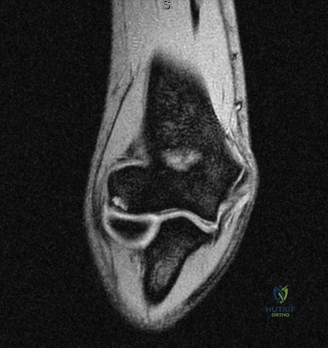
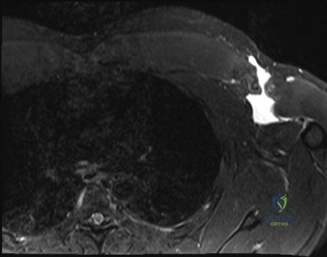
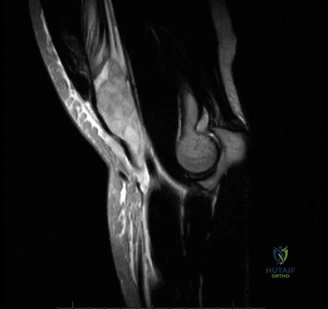
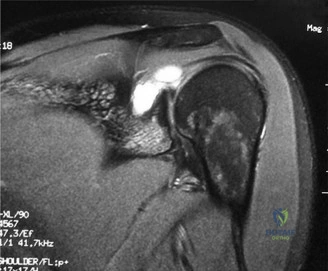
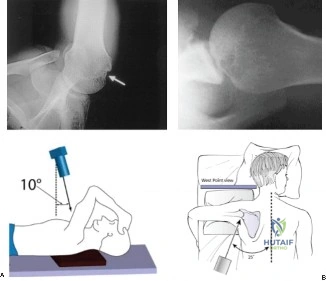
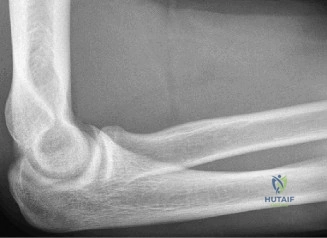
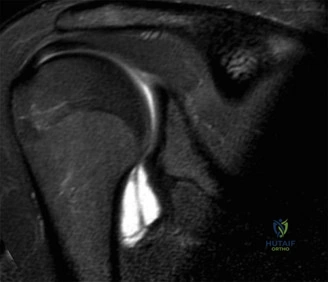
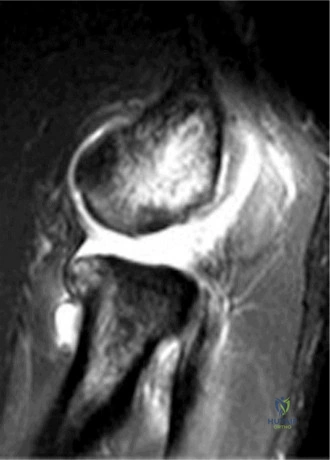
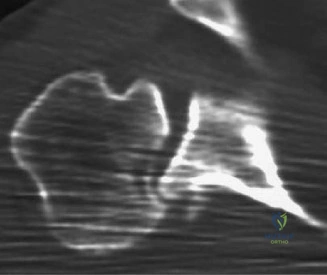
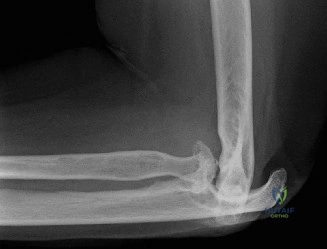
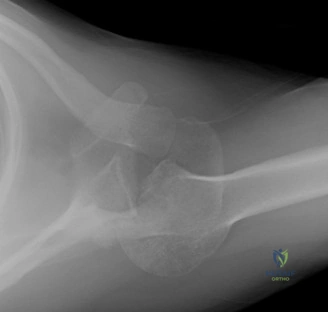
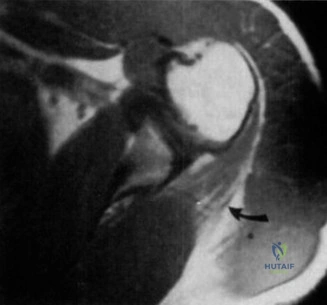
Thorough pre-operative planning begins with advanced imaging. While the initial ED evaluation mandates true orthogonal radiographs (AP and Axillary views) to confirm joint concentricity and rule out fractures, definitive surgical planning requires cross-sectional imaging. Magnetic Resonance Imaging (MRI), preferably an MR Arthrogram with intra-articular gadolinium, is the gold standard for evaluating the soft tissues. It allows for the precise identification of Bankart, ALPSA, and SLAP lesions, assesses the volume and integrity of the capsular tissue, and evaluates the rotator cuff.
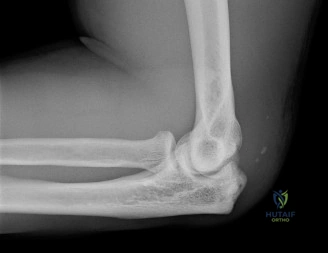
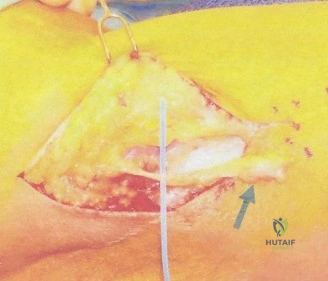
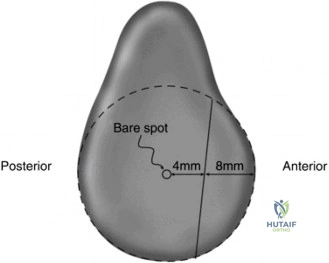
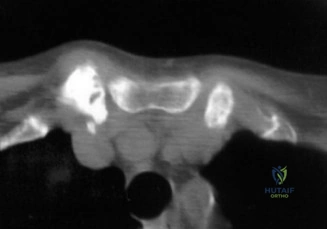
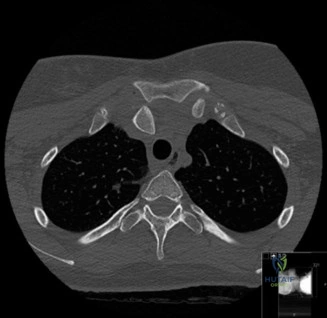
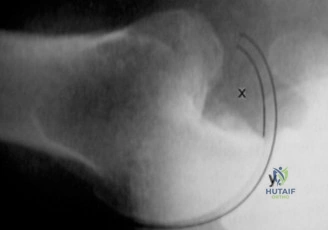
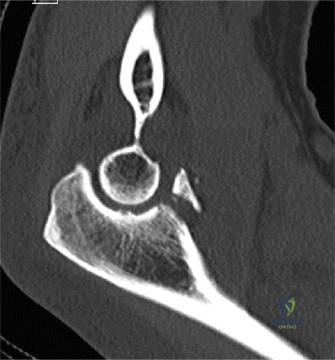
To accurately quantify bipolar bone loss, a non-contrast 3D Computed Tomography (CT) scan with digital subtraction of the humeral head is mandatory. Glenoid bone loss is calculated using the "best-fit circle" method on the en face sagittal view of the glenoid. The width of the inferior glenoid is compared to the expected diameter of the intact posterior rim. Simultaneously, the Hill-Sachs lesion is evaluated to determine if it is "on-track" or "off-track." The glenoid track is calculated as 83% of the intact glenoid width, minus the measured anterior glenoid bone loss. If the medial margin of the Hill-Sachs lesion extends medial to this track, it is deemed "off-track" and will engage the anterior glenoid rim during abduction and external rotation, necessitating either a Remplissage or a Latarjet.
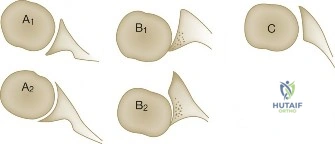
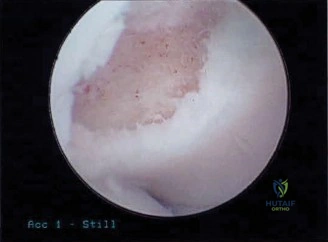
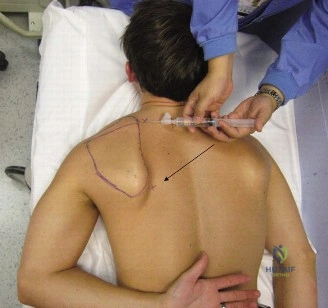
Anesthesia generally consists of a regional interscalene nerve block for post-operative pain control, combined with general endotracheal anesthesia to ensure complete muscle relaxation. Patient positioning is a matter of surgeon preference, with both the beach chair and lateral decubitus positions being widely utilized. The lateral decubitus position offers superior visualization of the anteroinferior glenoid and facilitates easier access for inferior anchor placement due to longitudinal and lateral traction (typically 10-15 lbs). It also expands the joint space. Conversely, the beach chair position allows for a more anatomical orientation, easier conversion to an open procedure if necessary, and unencumbered evaluation of the shoulder's range of motion during the procedure.
Regardless of positioning, meticulous attention to detail during setup is required. Bony prominences must be heavily padded to prevent compressive neuropathies (e.g., peroneal nerve in lateral decubitus). An Examination Under Anesthesia (EUA) is the critical first step before prepping and draping. The surgeon must meticulously assess anterior, posterior, and inferior translation (sulcus sign) and compare it to the contralateral, uninjured shoulder to confirm the diagnosis and rule out unrecognized multidirectional instability, which would drastically alter the surgical plan.
Step-by-Step Surgical Approach and Fixation Technique
Arthroscopic Bankart Repair Technique
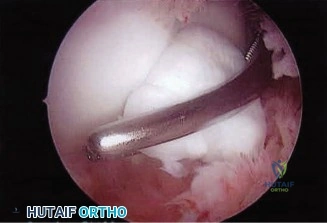
The arthroscopic Bankart repair begins with the establishment of standard portals. A standard posterior viewing portal is created, followed by the establishment of an anterosuperior portal (typically via an outside-in spinal needle localization just anterior to the biceps tendon) and an anteroinferior working portal (just superior to the subscapularis tendon). Diagnostic arthroscopy is performed to evaluate the articular cartilage, rotator cuff, biceps anchor, and the extent of the labral tear. The drive-through sign (easy passage of the arthroscope between the humeral head and glenoid) is a hallmark of capsular laxity.
The most critical step of the procedure is the adequate mobilization of the capsulolabral complex. Using an arthroscopic elevator or a radiofrequency wand, the torn labrum and the scarred, medially healed capsule (in the case of an ALPSA lesion) must be thoroughly elevated from the anterior glenoid neck. The tissue must be mobilized until the subscapularis muscle belly is clearly visualized beneath the capsule. Failure to adequately mobilize this tissue is the leading cause of surgical failure. Following mobilization, the anterior glenoid rim is decorticated using a motorized burr or rasp to create a bleeding, cancellous bone bed to promote robust biological healing of the labrum.
Fixation is achieved using modern biocomposite or all-suture anchors. The first anchor is placed at the most inferior aspect of the tear, typically at the 5:30 or 6:00 position (for a right shoulder). A curved drill guide is often necessary to achieve the proper trajectory, aiming slightly medial to the articular margin to avoid penetrating the articular cartilage. Suture passage is performed using a curved suture shuttle device, taking a healthy bite of the inferior capsule and labrum to effect a superior and lateral shift. This plicates the IGHL and eliminates the redundant axillary pouch. Subsequent anchors are placed sequentially superiorly at the 4:30 and 3:00 positions. The knots are tied (or knotless mechanisms tensioned) to recreate the anatomical labral bumper.
Open Latarjet Procedure
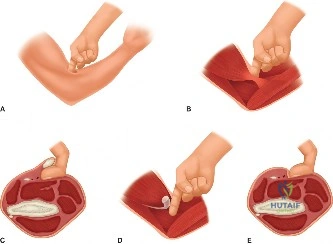
When critical bone loss is present, the open Latarjet procedure is utilized. A standard deltopectoral approach is utilized to expose the coracoid process. The coracoacromial ligament is released, and the pectoralis minor is detached from the medial aspect of the coracoid. An osteotomy of the coracoid is performed at its base (the "knee"). The subscapularis is then split longitudinally at the junction of its superior two-thirds and inferior one-third. The capsule is incised vertically, exposing the anterior glenoid. The glenoid neck is prepared with a burr to create a flat bleeding surface. The coracoid graft is then passed through the subscapularis split and secured flush with the anterior glenoid articular cartilage using two partially threaded cancellous screws. This provides the "triple blocking effect" described by Patte: bone block augmentation, the dynamic sling effect of the conjoint tendon, and capsular repair to the coracoacromial ligament stump.
Complications, Incidence Rates, and Salvage Management
Despite meticulous surgical technique, the management of shoulder instability carries a distinct complication profile. The most devastating and common complication is recurrent instability. Following arthroscopic Bankart repair, recurrence rates range from 5% to 15%, heavily dependent on patient selection. Recurrence is almost universally tied to unrecognized critical bone loss, failure to address an off-track Hill-Sachs lesion, inadequate tissue mobilization, or premature return to contact sports. When an arthroscopic repair fails, the salvage procedure of choice is universally a bony augmentation (Latarjet or distal tibial allograft), as revision arthroscopy yields unacceptably high failure rates.
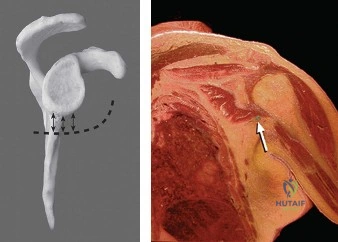
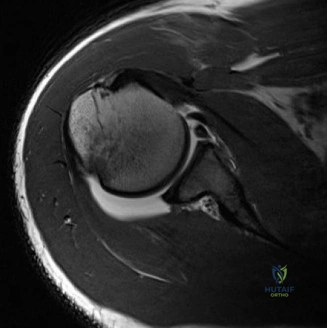
Post-operative stiffness, specifically a loss of external rotation, is another frequent complication. While a slight loss of external rotation (5-10 degrees) is expected and often desirable to prevent recurrence, severe stiffness can be functionally debilitating, particularly for overhead throwing athletes. This is typically caused by over-plication of the capsule, placing anchors too far medially on the glenoid neck, or prolonged post-operative immobilization. Management begins with an aggressive, structured physical therapy regimen. If non-operative measures fail after 6 months, an arthroscopic capsular release may be indicated.
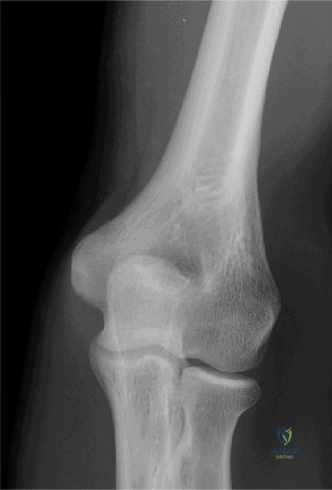
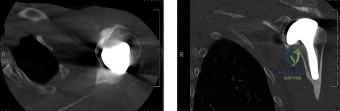
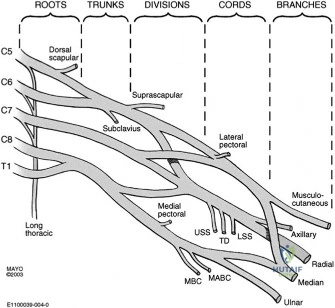
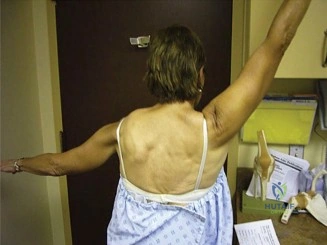
Neurologic injury is a rare but severe complication. In arthroscopic stabilization, the axillary nerve is at risk during inferior capsular release and anchor placement at the 6:00 position. In the Latarjet procedure, the musculocutaneous nerve (entering the conjoint tendon 3-5 cm distal to the coracoid tip) and the axillary nerve (during subscapularis splitting and glenoid preparation) are highly vulnerable. Hardware complications also exist; prominent anchors can cause devastating rapid-onset glenohumeral chondrolysis, while Latarjet screws can break, migrate, or cause impingement if placed too laterally.
| Complication | Estimated Incidence | Primary Etiology | Salvage / Management Strategy |
|---|---|---|---|
| Recurrent Instability | 5% - 15% (Bankart) | Unrecognized bone loss, poor tissue | Revision with Latarjet or Bone Allograft |
| Loss of External Rotation | 10% - 20% | Over-plication, medial anchor placement | Aggressive PT, Arthroscopic Capsular Release |
| Hardware Prominence / Chondrolysis | < 2% | Proud anchor placement, screw back-out | Immediate hardware removal, chondral debridement |
| Neurologic Injury (Axillary/Musculocutaneous) | 1% - 3% | Retractor pressure, aberrant portal placement | Observation, EMG at 3 months, Nerve exploration |
| Coracoid Graft Non-union (Latarjet) | 5% - 10% | Poor compression, smoking, early motion | Revision fixation, bone grafting |
Phased Post-Operative Rehabilitation Protocols
The post-operative rehabilitation following surgical stabilization is as critical to the final outcome as the surgical procedure itself. The protocol must delicately balance the need to protect the healing soft tissues with the necessity of preventing debilitating stiffness. The rehabilitation is strictly phased, guided by the biological timeline of tissue healing. Phase I (Weeks 0-4) is the period of maximum protection. The patient is strictly immobilized in a standard sling or a slight abduction sling. Active range of motion of the elbow, wrist, and hand is encouraged immediately to prevent distal edema. Pendulum exercises may be initiated, but active shoulder motion, particularly external rotation and abduction, is strictly prohibited to protect the anteroinferior repair.
Phase II (Weeks 4-8) marks the transition to moderate protection. The sling is discontinued. The primary goal is the gradual restoration of passive and active-assisted range of motion. Forward flexion is progressively advanced, while external rotation is slowly introduced, typically limiting ER to 30 degrees at the side until week 6, and then gradually progressing. Submaximal isometric strengthening of the rotator cuff and periscapular stabilizers is initiated. Aggressive stretching or forced manipulation is strictly avoided to prevent stretching out the newly repaired capsulolabral complex.
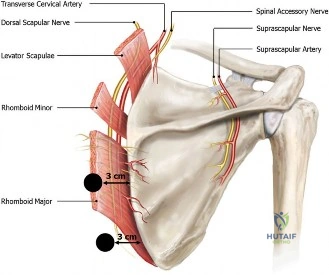
Phase III (Weeks 8-12) focuses on early dynamic strengthening. Passive range of motion should be nearly symmetric to the contralateral side by this stage. Isotonic strengthening of the rotator cuff and scapular retractors (rhomboids, middle/lower trapezius) is advanced using resistance bands and light weights. Closed kinetic chain exercises are incorporated to enhance proprioception and dynamic joint stability. The focus remains on muscular endurance and establishing normal scapulohumeral rhythm, correcting any compensatory dyskinesia that developed during the period of injury and immobilization.
Phase IV (Months 3-6) is the advanced strengthening and return-to-sport phase. Plyometric exercises and sport-specific drills are introduced. For overhead athletes, a structured interval throwing program is initiated. Return to unrestricted contact sports is generally not permitted until 5 to 6 months post-operatively. Objective criteria must be met prior to clearance: full, painless range of motion, isokinetic strength testing demonstrating greater than 90% symmetry compared to the uninjured limb, and a completely negative apprehension and relocation test. Premature return to sport is the leading modifiable risk factor for catastrophic failure of the repair.
Summary of Landmark Literature and Clinical Guidelines
The evolution of shoulder instability management is deeply rooted in several landmark studies that have fundamentally shifted orthopedic practice. Historically, the management of first-time dislocators was universally conservative. However, the seminal work by Kirkley et al. (1999) and later confirmed by multiple randomized controlled trials, demonstrated that early arthroscopic stabilization in young, highly active first-time dislocators significantly reduced the rate of recurrent instability and improved long
Clinical & Radiographic Imaging Archive