Solve Orthopedic Cases: Extensor Carpi Radialis Brevis & Elbow Pain
Key Takeaway
This topic focuses on Solve Orthopedic Cases: Extensor Carpi Radialis Brevis & Elbow Pain, Valgus extension overload (VEO) in athletes, like baseball pitchers, presents as posteromedial elbow pain exacerbated by throwing. It involves chronic stress, leading to chondrolysis and osteophyte formation, with cubital tunnel syndrome being a common neurologic complication. While distinct, issues affecting the extensor carpi radialis brevis, such as lateral epicondylitis, also cause activity-related elbow discomfort.
Detailed Patient Presentation and Mechanism of Injury
History of Present Illness
Welcome, colleagues, to this week’s Grand Rounds. Today, we are dissecting a highly complex and classic presentation of elbow pathology in the overhead throwing athlete. Our patient is a 16-year-old right-hand-dominant male competitive high school baseball pitcher who presents to the orthopedic clinic for the evaluation of insidious, progressively worsening right elbow pain. The patient strictly denies any acute traumatic event, popping sensation, or sudden loss of velocity that would suggest an acute ligamentous rupture. Instead, the pain is localized precisely to the posteromedial aspect of his dominant elbow and is profoundly exacerbated by the act of throwing, specifically during the deceleration phase of his pitching mechanics.
The symptomatology has been present for approximately six months, correlating with an increase in his pitching volume during the summer showcase circuit. However, the pain has become markedly more severe and performance-limiting over the past three months. He reports an inability to "finish" his pitches, resulting in a loss of command and a slight dip in peak velocity. He has attempted conservative measures, including localized cryotherapy, over-the-counter non-steroidal anti-inflammatory drugs (NSAIDs), and a brief, unstructured period of rest, all of which provided only transient relief.
Biomechanics of the Throwing Motion
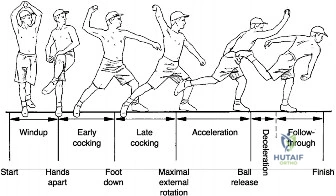
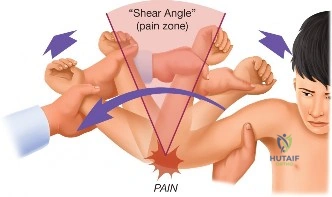
To truly comprehend the pathoanatomy of this patient's presentation, we must rigorously analyze the biomechanics of the overhead throw. The pitching motion is divided into six distinct phases: wind-up, early cocking, late cocking, acceleration, deceleration, and follow-through. During the late cocking and early acceleration phases, the elbow is subjected to tremendous valgus torque, often exceeding the ultimate tensile strength of the anterior bundle of the ulnar collateral ligament (UCL). The body compensates for this via dynamic stabilization from the flexor-pronator mass.
However, as the arm transitions into the deceleration phase, the elbow rapidly extends from approximately 90 degrees of flexion to near full extension at angular velocities exceeding 2,500 degrees per second. This generates massive posterior shear forces. The olecranon process is violently driven into the posteromedial olecranon fossa. Over time, this repetitive microtrauma leads to the constellation of symptoms we observe in this patient.
Pathoanatomy of Valgus Extension Overload
The repetitive valgus stress and extreme extension inherent in pitching create a biomechanical triad known as Valgus Extension Overload (VEO) syndrome. This triad consists of medial tension, lateral compression, and posterior shear. Medially, the UCL experiences chronic microtearing and attenuation. Laterally, the radiocapitellar joint undergoes compressive forces that can lead to osteochondral defects or loose body formation. Posteriorly, the repetitive impingement of the olecranon tip against the medial wall of the olecranon fossa results in reactive osteophyte formation, chondromalacia, and eventually, mechanically symptomatic loose bodies.
In this 16-year-old patient, the posteromedial pain is a direct result of this posterior shear and osteophyte impingement. The reactive bone formation alters the congruency of the olecranon fossa, leading to a mechanical block to terminal extension and localized synovitis. Understanding this triad is paramount, as focusing solely on the posterior osteophyte without evaluating the medial ligamentous structures can lead to catastrophic surgical failures.
Comprehensive Clinical Examination Findings
Inspection and Palpation
A meticulous physical examination is the cornerstone of diagnosing elbow pathology in the throwing athlete. Upon inspection, the patient exhibits a mild resting flexion contracture of approximately 10 degrees, a common adaptive change in pitchers due to anterior capsular contracture and posterior osseous impingement. There is a subtle, localized effusion palpable in the posterior soft spot, indicative of active synovitis.
Palpation reveals exquisite, pinpoint tenderness over the posteromedial tip of the olecranon. Moving medially, the medial epicondyle and the sublime tubercle (the insertion of the anterior bundle of the UCL) are remarkably non-tender, suggesting that while the UCL is subjected to stress, it is not the primary source of acute nociception. Furthermore, palpation over the lateral epicondyle and the origin of the extensor carpi radialis brevis (ECRB) yields no pain, effectively ruling out lateral epicondylitis, which can occasionally present with referred pain patterns in the elbow.
Range of Motion and Provocative Testing
Range of motion testing reveals a loss of terminal extension compared to the contralateral non-throwing arm, with firm, bony end-feel and reproduction of the patient's sharp posteromedial pain upon forced terminal extension. This is the hallmark clinical sign of Valgus Extension Overload. Flexion, pronation, and supination are within normal limits and pain-free.
Provocative ligamentous testing is critical. The valgus stress test, performed at 30 degrees of elbow flexion to unlock the olecranon from its fossa, demonstrates a firm endpoint with no gross laxity or pain, indicating a clinically intact UCL. The moving valgus stress test (O'Driscoll's test) is also negative, further corroborating the stability of the medial column. Resisted wrist flexion and forearm pronation elicit no pain, effectively ruling out medial epicondylitis (flexor-pronator tendinopathy).
Neurological and Vascular Assessment
Given the proximity of the ulnar nerve to the medial and posterior compartments of the elbow, a thorough neurological assessment is mandatory. The patient has a negative Tinel's sign over the cubital tunnel. There is no palpable subluxation or dislocation of the ulnar nerve out of the retrocondylar groove during active or passive elbow flexion. Motor function of the intrinsic muscles of the hand (interossei, lumbricals) and sensory distribution in the ring and small fingers are entirely intact.
Vascular examination reveals strong and symmetric radial and ulnar pulses. Capillary refill is brisk, and there are no signs of effort thrombosis or vascular compromise that could mimic deep, aching elbow pain. The isolated nature of the pain to the posteromedial olecranon, combined with the negative ligamentous and neurological findings, heavily points toward isolated VEO secondary to posteromedial impingement.
Advanced Imaging and Diagnostics (X-ray, CT, MRI, Templating)
Standard Radiographic Evaluation
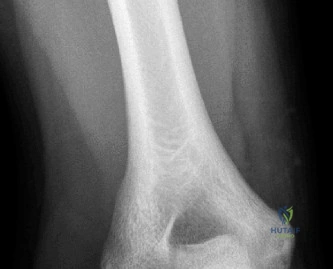
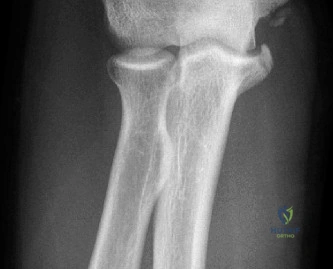
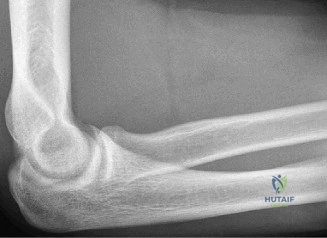
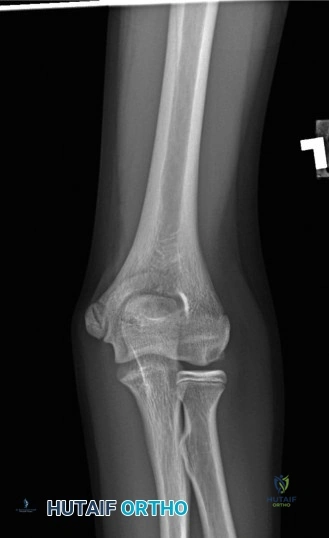
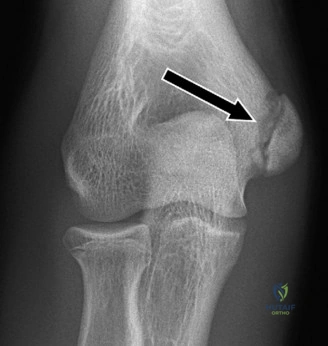
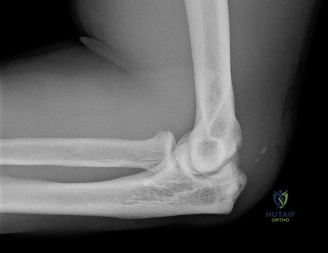
Standard radiographic evaluation of the thrower's elbow must include true anteroposterior (AP), lateral, oblique, and axial (cubital tunnel) views. In this patient, the AP view may appear relatively unremarkable, though subtle hypertrophy of the medial epicondyle or radiocapitellar sclerosis may be noted. The true lateral radiograph is highly informative, often demonstrating the presence of a posterior olecranon osteophyte.
However, the most critical view for diagnosing VEO is the internal rotation oblique view, or a specialized axial view of the olecranon fossa. In our patient's radiographs, we observe a distinct, hypertrophic osteophyte on the posteromedial aspect of the olecranon process. There are also faint radiopacities within the posterior compartment, highly suggestive of intra-articular loose bodies resulting from the fragmentation of these osteophytes.
Advanced Cross-Sectional Imaging
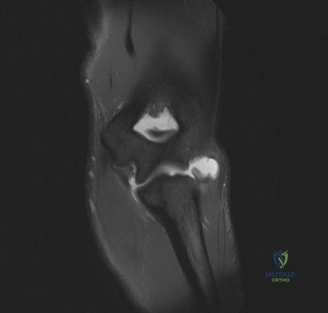
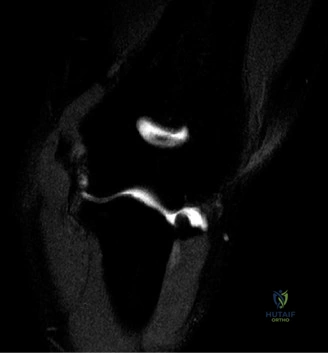
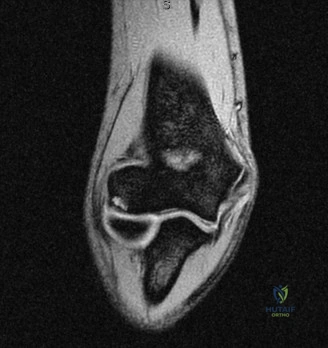
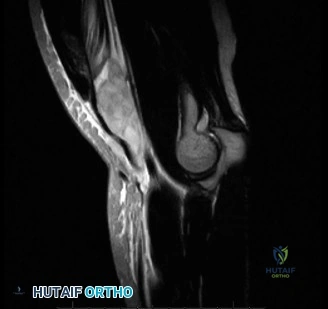
While plain films confirm the presence of osseous reactive changes, Magnetic Resonance Imaging (MRI) is indispensable for evaluating the articular cartilage, the integrity of the UCL, and the presence of occult loose bodies. A high-resolution MRI, preferably an MR Arthrogram (MRA) if subtle UCL pathology is suspected, provides a comprehensive map of the elbow's soft tissue envelope.
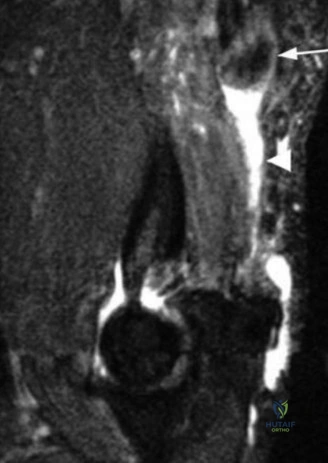
In this case, the MRI demonstrates focal chondromalacia and subchondral edema at the posteromedial olecranon tip and the corresponding medial wall of the olecranon fossa—the classic "kissing lesion" of VEO. Crucially, the anterior bundle of the UCL appears continuous and intact, with no evidence of high-grade partial tearing, T-sign (contrast leakage beneath the distal insertion), or severe attenuation. The flexor-pronator mass and the ECRB origin are pristine.
Computed Tomography and Surgical Templating
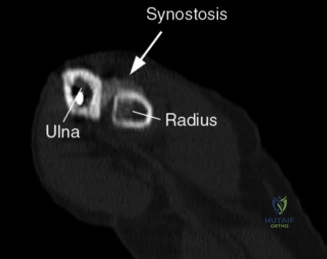
For definitive surgical planning, particularly when addressing complex osseous impingement, a non-contrast Computed Tomography (CT) scan with 3D reconstructions is often utilized. The CT scan allows the orthopedic surgeon to precisely quantify the size and exact location of the posteromedial osteophyte.
Surgical templating is critical here. The surgeon must calculate exactly how many millimeters of bone need to be resected to alleviate the impingement without violating the native olecranon anatomy. Resecting too much bone—specifically, violating the medial cortex of the olecranon—can inadvertently increase strain on the UCL, leading to iatrogenic valgus instability. The CT scan provides the exact topographical map required to execute a precise, conservative arthroscopic resection.
Exhaustive Differential Diagnosis
Evaluating the Thrower's Elbow
The differential diagnosis for elbow pain in a 16-year-old overhead athlete is broad and requires a systematic approach to differentiate between medial tension, lateral compression, and posterior shear pathologies. While the clinical picture strongly supports Valgus Extension Overload, we must rigorously exclude other entities that could co-exist or mimic this presentation.
Below is a comprehensive comparison of the primary differential diagnoses considered in this clinical scenario:
| Pathology | Primary Location of Pain | Key Clinical Findings | Imaging Hallmarks |
|---|---|---|---|
| Valgus Extension Overload (VEO) | Posteromedial | Pain with terminal extension, locking/catching, normal valgus stress. | Posteromedial olecranon osteophytes, loose bodies, kissing lesions. |
| UCL Insufficiency / Tear | Medial | Pain during late cocking/acceleration, positive moving valgus stress test. | Edema/discontinuity of anterior band of UCL, T-sign on MRA. |
| Medial Epicondylitis | Medial | Pain with resisted wrist flexion and forearm pronation. | Thickening/edema of flexor-pronator mass origin. |
| Osteochondritis Dissecans (OCD) | Lateral | Insidious lateral pain, mechanical symptoms, loss of extension. | Radiolucent lesion of capitellum, subchondral bone fragmentation. |
| Lateral Epicondylitis (ECRB) | Lateral | Pain with resisted wrist extension and supination. | Tendinosis/tearing at the ECRB origin on lateral epicondyle. |
The Role of Extensor Carpi Radialis Brevis in Elbow Pain
Addressing the title of our clinical case, we must discuss the Extensor Carpi Radialis Brevis (ECRB) and its relation to elbow pain. Lateral epicondylitis, often termed "tennis elbow," is primarily a tendinopathy of the ECRB origin. While less common in young baseball pitchers compared to medial or posterior pathologies, it remains a critical differential for lateral-sided elbow pain.
Pathology of the ECRB presents with pain localized to the lateral epicondyle, exacerbated by gripping and resisted wrist extension. The pathophysiology involves angiofibroblastic hyperplasia and microtearing of the ECRB tendon due to repetitive eccentric overload. In our current patient, the complete absence of lateral pain, negative resisted wrist extension testing, and normal lateral compartment imaging effectively rule out ECRB pathology. However, understanding the ECRB's mechanics is vital for a complete orthopedic evaluation of the elbow.
Differentiating Olecranon Stress Fractures
Another critical differential in the adolescent throwing athlete is an olecranon stress fracture. Like VEO, this presents with posterior elbow pain exacerbated by throwing. However, the pain is typically located more centrally over the olecranon rather than posteromedially.
Stress fractures result from the immense triceps traction forces during the deceleration phase, combined with the posterior shear forces. Clinically, these patients will have profound tenderness directly over the olecranon physis or the central olecranon body. Radiographs and MRI will show a transverse sclerotic line or marrow edema across the olecranon. Differentiating this from VEO is crucial, as an olecranon stress fracture often requires prolonged cessation of throwing and occasionally internal fixation, whereas VEO is treated with osteophyte excision.

Complex Surgical Decision Making and Classifications
Indications for Operative Intervention
The initial management for Valgus Extension Overload is strictly non-operative. This includes a period of active rest (cessation of throwing), mechanical analysis of the pitching motion to correct flaws that exacerbate valgus stress, targeted physical therapy focusing on periscapular and core strengthening, and NSAIDs.
Operative intervention is indicated only when a patient fails a rigorous 3-to-6-month trial of conservative management, or if they present with acute mechanical symptoms such as frank locking or catching caused by intra-articular loose bodies. In our 16-year-old patient, the presence of progressive pain, loss of terminal extension, radiographic evidence of a hypertrophic osteophyte, and suspected loose bodies after 6 months of symptoms provides a clear, evidence-based indication for surgical intervention.
Preoperative Planning and the "Danger Zone"
The surgical management of VEO involves arthroscopic debridement and posteromedial osteophyte excision. However, the decision-making process is fraught with biomechanical peril. The surgeon must navigate the delicate balance between relieving impingement and maintaining medial column stability.
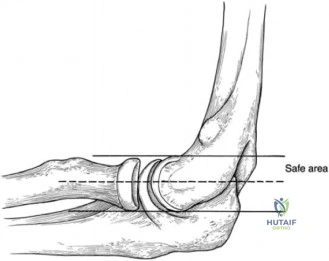
The posteromedial olecranon serves as a secondary bony stabilizer to valgus stress. If the surgeon resects too much of the olecranon—specifically violating the native medial cortex—the primary restraint (the UCL) is subjected to exponentially higher tensile forces. This over-resection pushes the elbow into the "danger zone," frequently resulting in iatrogenic valgus instability that subsequently requires a Tommy John surgery (UCL reconstruction). Preoperative templating dictates that resection should be limited strictly to the reactive osteophyte, typically no more than 2 to 3 millimeters of bone.
Concomitant Pathology Considerations
During the decision-making process, the surgeon must also plan for potential concomitant pathologies. Even if the MRI suggests an intact UCL, the arthroscopic evaluation must include a dynamic assessment of the medial compartment. If subtle UCL laxity is discovered intraoperatively (e.g., opening of the ulnohumeral joint space greater than 1-2 mm under valgus stress), the surgeon must be prepared to alter the plan.
Furthermore, if the patient had exhibited any signs of ulnar neuritis preoperatively, a concurrent in situ ulnar nerve decompression or anterior transposition might be warranted. In our patient, the absence of ulnar nerve symptoms and a clinically stable UCL allows us to focus purely on the posterior compartment arthroscopy and osteophyte excision.
Step-by-Step Surgical Technique and Intervention
Patient Positioning and Setup
The patient is brought to the operating room and placed under general anesthesia. A thorough examination under anesthesia (EUA) is performed to confirm the absence of valgus instability when the muscles are completely relaxed. The patient is then positioned in the lateral decubitus position with the operative arm supported over a bolstered arm holder, allowing the elbow to rest comfortably at 90 degrees of flexion and freely hang for dynamic testing.
A non-sterile tourniquet is applied high on the brachium. The arm is prepped and draped in a standard sterile orthopedic fashion. We utilize a standard 4.0 mm, 30-degree arthroscope. Fluid pressure is kept meticulously low (typically around 30-40 mmHg) to prevent fluid extravasation into the forearm compartments, which could precipitate compartment syndrome.

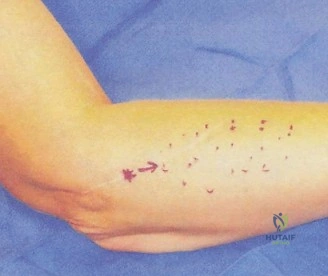
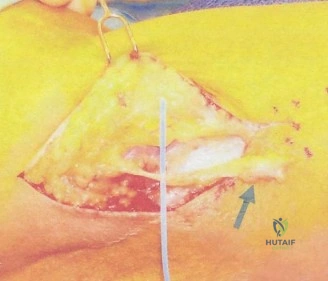
Portal Placement and Diagnostic Arthroscopy
Arthroscopy begins in the anterior compartment. The joint is insufflated with 20-30 cc of normal saline via the soft spot. A proximal anteromedial portal is established first, taking great care to stay anterior to the intermuscular septum to avoid the ulnar nerve. An anterolateral portal is then established under direct visualization.
A comprehensive diagnostic sweep of the anterior compartment is performed, evaluating the radiocapitellar joint, the coronoid, and the anterior capsule. We specifically look for chondral damage on the capitellum, which could indicate lateral compression overload. Once the anterior compartment is cleared and any loose bodies are removed, our attention turns to the posterior compartment, which is the primary site of pathology in VEO.
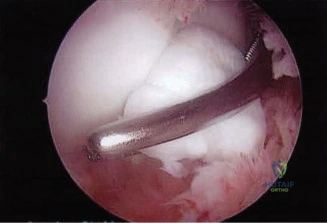
Posteromedial Osteophyte Excision
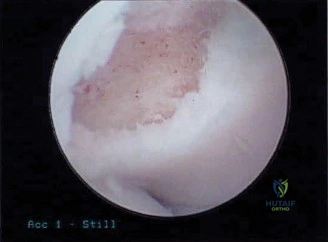
Posterior access is gained via a direct posterior portal (trans-tricipital) and a posterolateral portal. Upon entering the posterior compartment, a localized synovectomy is performed using a mechanical shaver to improve visualization. The posteromedial osteophyte is immediately identified, often accompanied by a "kissing lesion" of chondromalacia on the corresponding olecranon fossa.
Using a 4.0 mm motorized burr, the osteophyte is carefully resected. The resection is meticulously limited to the hypertrophic bone. The surgeon constantly references the native medial cortex of the olecranon, ensuring it is not violated. We dynamically extend the elbow under direct visualization to confirm that the mechanical impingement has been completely eradicated and that full, impingement-free terminal extension is achieved. The joint is thoroughly irrigated to remove all bone debris, and the portals are closed with simple non-absorbable sutures.
Strict Post-Operative Protocol and Rehabilitation Stages
Acute Protection and Mobility Phase (Weeks 0-2)
The immediate post-operative goal is to control inflammation, protect the surgical site, and restore full range of motion. The patient is placed in a soft, bulky compressive dressing. Unlike UCL reconstructions, VEO debridement does not require rigid immobilization.
Active and active-assisted range of motion exercises for the elbow, wrist, and hand begin on post-operative day one. Cryotherapy is utilized aggressively. The primary milestone in this phase is the restoration of full, symmetrical terminal extension, which should now be pain-free following the removal of the bony block. Isometrics for the biceps, triceps, and forearm musculature are initiated to prevent atrophy.
Intermediate Strengthening Phase (Weeks 2-6)
Once full range of motion is achieved and the portal sites are completely healed, the patient transitions to the intermediate phase. This phase focuses on progressive resistance exercises. The "Thrower's Ten" program is initiated, which is a specialized regimen targeting the rotator cuff, periscapular stabilizers, and forearm musculature.
It is imperative to address the entire kinetic chain. Pitching is a whole-body activity, and core or lower extremity deficits often lead to compensatory stress at the elbow. Therefore, aggressive core stabilization, gluteal strengthening, and balance training are integrated into the daily physical therapy routine.
Advanced Return to Throwing Phase (Weeks 6+)
At approximately 6 to 8 weeks post-operatively, assuming the patient has full, painless range of motion, normal strength, and a stable clinical exam, an interval throwing program (ITP) is initiated. The ITP is a highly structured, phased progression of throwing distances and intensities.
The patient begins with flat-ground throwing at 45 feet, gradually progressing to 120 feet over several weeks. Only after successfully completing the flat-ground phase without pain does the patient progress to throwing off the mound. Pitch velocity and breaking balls are introduced in the final stages. A comprehensive biomechanical analysis of the patient's pitching mechanics is performed by a specialized pitching coach and physical therapist to ensure that the mechanical flaws that led to the VEO are corrected prior to returning to competitive play.
High-Yield Clinical Pearls and Pitfalls
Surgical and Diagnostic Pitfalls
The most catastrophic pitfall in the management of Valgus Extension Overload is the over-resection of the posteromedial olecranon. Surgeons must remember that the olecranon is a critical secondary stabilizer against valgus stress. Resecting into the native medial cortex will invariably lead to increased strain on the UCL, resulting in iatrogenic instability and the likely need for subsequent ligamentous reconstruction.
Diagnostically, a major pitfall is failing to recognize concomitant UCL insufficiency. VEO is often the osseous manifestation of chronic medial ligamentous laxity. If a surgeon addresses the posterior osteophyte but ignores a compromised UCL, the patient will continue to experience pain and instability upon returning to throwing. Always perform a dynamic intraoperative assessment of medial joint opening.
High-Yield Clinical Pearls
- The Triad: Always evaluate the throwing elbow for the triad of medial tension, lateral compression, and posterior shear. Pathology in one compartment often implies stress in the others.
- Terminal Extension Pain: Pain specifically at forced terminal extension in a thrower is the hallmark sign of VEO and posterior impingement.
- ECRB Differentiation: While lateral epicondylitis (ECRB tendinopathy) causes lateral pain, it is rare in young pitchers. Always rule out radiocapitellar overload or OCD lesions when a young thrower presents with lateral-sided pain.
- Conservative Resection: When burring the posteromedial osteophyte, "less is more." Remove only the reactive bone necessary to clear the impingement.
By adhering to these rigorous diagnostic and surgical principles, orthopedic surgeons can successfully navigate the complexities of the thrower's elbow, ensuring optimal outcomes and a safe return to elite athletic competition.
