Orthopedic Prometric Exam Preparation MCQs - Part 1
Comprehensive 100-Question Exam
00:00
Start Quiz
Question 1
Which of the following is the proper sequence (or order) of the classes of macromolecules in articular cartilage in regard to the percentage of dry weight of the components (highest to lowest):
Explanation
Question 2
Which of the following articular cartilage collagens form cross-banded fibrils:
Explanation
Question 3
Which of the following molecules binds with type II collagen and may aid in the stabilization of the type II collagen network in articular cartilage:
Explanation
Question 4
A high collagen concentration and a low proteoglycan concentration is found in which of the following zones of articular cartilage:
Explanation
Question 5
A high concentration of fibronectin and water is found in which of the following articular cartilage zones:
Explanation
Question 6
Which of the following zones of the articular cartilage most likely seals the cartilage off from the immune system:
Explanation
Question 7
Which of the following statements is true concerning the transitional zone of articular cartilage:
Explanation
Question 8
The chondrocytes in which of the following articular cartilage zones have the lowest metabolic activity:
Explanation
Question 9
Which of the following molecules causes the expression of matrix metalloproteinases that can degrade the articular cartilage extracellular matrix:
Explanation
Question 10
Which of the following resist tensile and shear deformation forces in articular cartilage:
Explanation
Question 11
Which of the following resist articular cartilage compression and fluid flow:
Explanation
Question 12
Which of the following stimulates aggrecan core protein and glycosaminoglycan synthesis:
Explanation
Question 13
Which of the following are characteristic of osteoarthritis:
Explanation
Question 14
Which of the following chemical changes occur in the first phase (earliest) of osteoarthritis:
Explanation
Question 15
Which of the following is characteristic of the second stage of osteoarthritis:
Explanation
Question 16
Which of the following is characteristic of the second stage of osteoarthritis:
Explanation
Question 17
Which of the following is characteristic of the second stage of osteoarthritis:
Explanation
Question 18
Which of the following is characteristic of the third and final stage of osteoarthritis:
Explanation
Question 19
Three years ago, a patient underwent successful resection of a third web space neuroma. She now presents with identical symptoms in the same location. She requests surgery because all attempts at conservative care have failed. Recommended treatment includes:
Explanation
Question 20
A 72-year-old woman presents for treatment of a painful hallux valgus deformity. On examination of the foot, crepitus is present to range of motion of the hallux. Pain upon compression of the joint is also present. The hallux valgus angle is 45° and the intermetatarsal angle is 20°. The recommended surgical procedure is:
Explanation
Question 21
Resection of the tibial sesamoid may result in which deformity of the hallux:
Explanation
Question 22
Arthrodesis of the ankle in a 34-year-old woman should be performed with the ankle positioned in:
Explanation
Question 23
A 27-year-old male athlete presents with a 2-month history of pain along the posteromedial ankle. Swelling is present posteriomedially. The pain is exacerbated with resisted plantarflexion and inversion of the foot. This condition is likely to be associated with:
Explanation
Question 24
A 23-year-old collegiate athlete presents for evaluation of recurrent ankle pain associated with ankle sprains. Upon examination, pain is present along the lateral ankle, an anterior drawer test is negative, and marked instability is apparent with inversion stress of the ankle. Stress radiographs are normal. The most likely cause of the patientâ s symptoms is:
Explanation
Question 25
A 46-year-old nurse presents for treatment of pain in the heel. The pain has been present for 6 months and increases upon rising from bed and after sedentary periods. The pain is focal and reproduced with pressure over the proximal medial heel. The initial treatment most likely to be associated with relief of symptoms is:
Explanation
Question 26
A 72-year-old man presents for evaluation and treatment of pain and limited motion in his arthritic ankle and subtalar joint. The foot is plantigrade with respect to the leg. Radiographs demonstrate ankle arthritis, an absent joint space, no malalignment of the tibiotalar joint, and a normal subtalar joint. The most reliable surgical procedure consistent with maintaining increased activity and patient function is:
Explanation
Question 27
A 37-year-old construction worker presents for evaluation and treatment of a painful stiff foot. He has noticed the stiffness for approximately 12 years, and particularly feels the stiffness when he is working on uneven ground surfaces. Upon clinical and radiographic examination, he is noted to have a calcaneonavicular coalition without any peritalar arthritis. Your recommended treatment is:
Explanation
Question 28
A 28-year-old male runner presents for treatment of a painful lesion under the first metatarsal head (located more toward the medial aspect of the metatarsophalangeal joint). The lesion is associated with painful callosity to palpation, normal hallux function, and a normal position of the first metatarsal. Attempts to relieve the pressure with orthoses and shoe modifications have not been successful. The ideal treatment is:
Explanation
Question 29
A 29-year-old football player twisted his foot 1 year ago, and he recalls pain and swelling of the midfoot at the time of the injury. No definitive treatment was provided at that time. Although he returned to athletic activity, he has experienced constant pain and occasional swelling. The pain is present upon passive pronation and abduction of the midfoot, and radiographs demonstrate that there is a 2.5-mm gap between the base of the first and second metatarsal and medial and middle cuneiform. Initial management should include:
Explanation
Question 30
A 44-year-old man has a 2-year history of pain in his hallux. The pain is accompanied by limited range of motion, pain on passive dorsiflexion of the hallux, and difficulty with athletic activities. Radiographs demonstrate that the plantar two-thirds of the joint is normal, with osteophytes of the dorsal surface of the joint. He has been unsuccessful with shoe wear modifications, and he requests surgery. The ideal procedure for him would be:
Explanation
Question 31
A 32-year-old woman with a history of diabetes presents with a 1-month history of painless swelling in the foot. The foot is swollen, warm, and erythema is present in the midfoot. She has no fever and her blood sugars are normal. Radiographs demonstrate the presence of fracture and dislocation of the tarsometatarsal joint. There are no new periosteal bone formations, and complete dorsal dislocation of the metatarsals on the cuneiforms is noted. The ideal treatment is:
Explanation
Question 32
A 54-year-old woman presents with a 1-year history of medial foot and ankle pain. She does not recall an episode of trauma, and she has had no change in her daily living activities. Her foot is changing shape; it is flatter than the opposite foot. On clinical examination she has a unilateral flatfoot deformity, an inability to perform a single heel rise, and weak inversion strength. The subtalar joint is flexible. Following an initial period of support of the foot, surgery is recommended. The ideal procedure is:
Explanation
Question 33
The anatomic structure responsible for the development of an interdigital neuroma is:
Explanation
Question 34
A 14-year-old boy with a painful flatfoot deformity presents for evaluation and treatment. He has had pain of the midfoot associated with thickening, callosity, and shoe wear. Shoe wear modifications, orthoses, and restriction of activity have not been successful. On examination, he has a very flexible flatfoot deformity. The hindfoot and midfoot are passively correctable, the subtalar and transverse tarsal joints are mobile, and callosity is present over the talar head. The recommended treatment is:
Explanation
Question 35
A 23-year-old woman with juvenile rheumatoid arthritis presents for treatment of painful forefoot deformity. Painful hallux valgus is present and is associated with dislocation of the lesser metatarsophalangeal joints. The recommended surgical treatment is:
Explanation
Question 36
The most common complication following triple arthrodesis in the adult patient is:
Explanation
Question 37
A pantalar arthrodesis is described as a:
Explanation
Question 38
A 23-year-old woman with a bilateral leg and foot deformity presents for evaluation. She has weakness in the foot and ankle, giving way of the ankle, and difficulty with exercise activities. She mentions that both her brother and uncle have similar problems and deformities with their limbs. On examination, she has a cavovarus foot deformity and muscle weakness. The most likely combination of muscle loss is:
Explanation
Question 39
A 63-year-old woman presents for evaluation and treatment of a painful bunion deformity. She has a moderate hallux valgus deformity. Pain and crepitus are present with range of motion of the hallux metatarsophalangeal joint. The hallux valgus deformity measures 25° and the intermetatarsal angle is 14°. The recommended surgical procedure is:
Explanation
Question 40
The nerve commonly associated with painful heel syndrome is the:
Explanation
Question 41
A 63-year-old woman with diabetes has had an ulcer under the plantar aspect of the foot for 3 months. The ulcer extends from the inferior aspect of the heel pad toward the midfoot. Nonoperative measures have failed to heal the ulcer. The amputation that is most likely to be successful is a:
Explanation
Question 42
A 56-year-old man has a painful flatfoot deformity. Attempts at orthotic support and bracing of the foot have not been successful. On examination, the forefoot is abducted, the heel is fixed in valgus, and the subtalar joint is rigid. The operation that is most likely to correct the foot deformity is:
Explanation
Question 43
A 54-year-old woman with a 10-year history of diabetes presents for treatment of a non-healing ulcer that has been present under the plantar aspect of her second metatarsal for 9 months. The ulcer is 1.5 cm in diameter, is associated with mild serous drainage, and has shown no radiographic changes. She has normal circulation to the forefoot. The recommended treatment is:
Explanation
Question 44
A patient presents for treatment in your emergency department following an injury that he sustained 4 hours earlier. His foot was run over by a piece of heavy industrial equipment. On examination, he has pain in the foot, a displaced fracture of the second metatarsal, a 3-cm area of severe contusion over the forefoot, and numbness of the dorsal surface of the foot. The next examination that you recommend is:
Explanation
Question 45
A 63-year-old woman presents for treatment of pain and a burning/tingling sensation along the medial aspect of the foot and hallux. She underwent a tarsal tunnel release 12 months ago, but she has not experienced much symptomatic relief. Upon clinical examination, she has a positive percussion test (Tinel sign) along the course of the distal tibial nerve and pain upon pressure of the tarsal canal. There are no other pertinent clinical findings and a magnetic resonance image does not reveal any pathologic lesion. The next course of treatment is:
Explanation
Question 46
For 3 years, a 23-year-old female gymnast has experienced recurrent ankle sprains associated with a sense of instability of the hindfoot. Upon examination, a positive anterior drawer test is present and stress radiographs are taken. She has attempted rehabilitation numerous times. She is unable to compete with her current symptoms. The recommended treatment is:
Explanation
Question 47
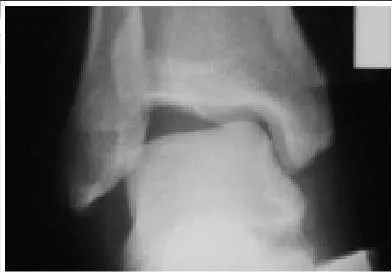
A 31-year-old recreational soccer player presents for evaluation of chronic ankle pain during physical activity. He reports a severe inversion ankle sprain that occurred 1 year ago and notes that he was treated with cast immobilization. Upon examination, he does not demonstrate laxity of the ankle ligaments and pain is present along the anterior medial ankle. A radiograph is presented. The recommended treatment is:
Explanation
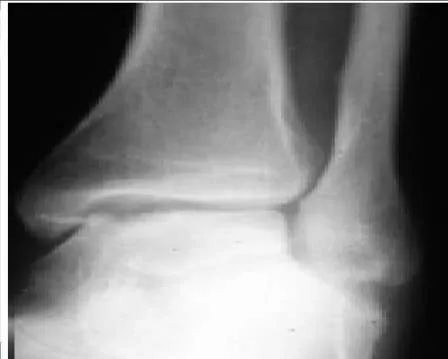 This patient has an osteochondral defect of the talus. According to most classification systems, the grade of the defect is not severe. Retrograde drilling of the defect through the sinus tarsi is possible for a posteromedial lesion of the talus for which the cartilage surface is intact. An autogenous osteochondral bone graft is indicated for a severe lesion with bone loss or following failure of previous attempts at arthroscopic drilling. The ideal procedure is arthroscopic debridement and drilling of the subchondral bone.
This patient has an osteochondral defect of the talus. According to most classification systems, the grade of the defect is not severe. Retrograde drilling of the defect through the sinus tarsi is possible for a posteromedial lesion of the talus for which the cartilage surface is intact. An autogenous osteochondral bone graft is indicated for a severe lesion with bone loss or following failure of previous attempts at arthroscopic drilling. The ideal procedure is arthroscopic debridement and drilling of the subchondral bone.
Question 48
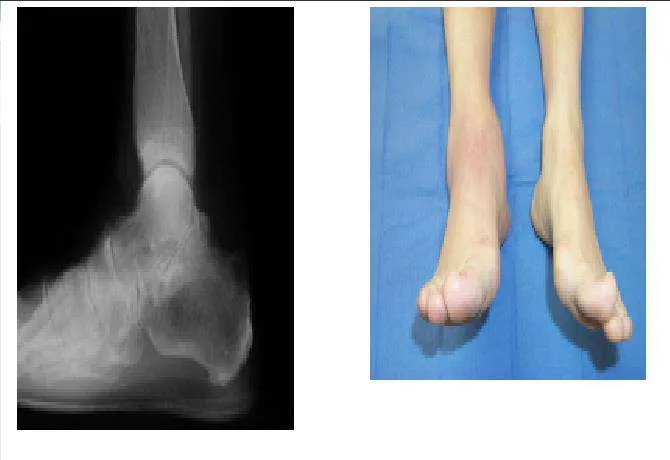
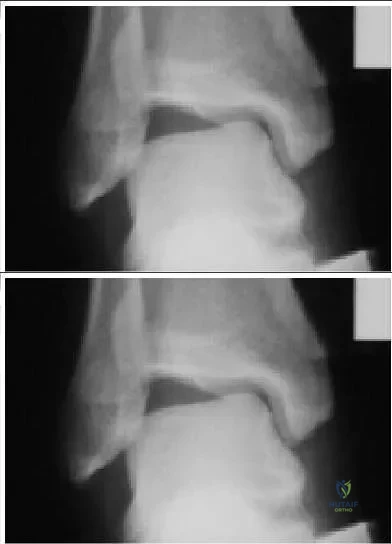
A 43-year-old woman has had a 2-year history of ankle pain. Her ankle pain is associated with swelling, decreased activities, and limited range of motion. Upon examination, diffuse warmth and swelling of the ankle are noted. Radiographs and a clinical picture are presented. The most likely diagnosis is:

Explanation
Question 49
A 25-year-old football player sustained an injury to his ankle 2 months ago. He has ankle pain upon dorsiflexion and external rotation. A radiograph demonstrates widening of the tibiofibular syndesmosis and a 3-mm space between the medial talus and the medial malleolus. The recommended treatment is:
Explanation
Question 50
A patient presents for surgical treatment of a third web space neuroma. She inquires as to the potential for complications from the procedure. You inform her that the recurrence rate following excision is approximately:
Explanation
Question 51
What is the primary function of aggrecan in the extracellular matrix of articular cartilage?
Explanation
Question 52
Which of the following bundles of the anterior cruciate ligament (ACL) is the primary restraint to anterior tibial translation when the knee is in 90 degrees of flexion?
Explanation
Question 53
A 13-year-old obese male presents with progressive left groin and knee pain. On physical examination, as his left hip is passively flexed, it obligatorily deviates into external rotation. What is the most likely diagnosis?
Explanation
Question 54
In the setting of a traumatic anterior pelvic ring injury (APC-III), where is the anatomically correct placement of a circumferential pelvic binder to effectively reduce pelvic volume?
Explanation
Question 55
Which of the following total hip arthroplasty (THA) bearing surface combinations demonstrates the lowest volumetric wear rate in laboratory simulator studies?
Explanation
Question 56
Primary bone healing occurs without the formation of a visible fracture callus. Which of the following fixation constructs is designed to achieve primary bone healing?
Explanation
Question 57
What is the most common neurological deficit associated with a severely displaced extension-type supracondylar humerus fracture in a pediatric patient?
Explanation
Question 58
The primary blood supply to the adult femoral head is derived predominantly from which of the following vessels?
Explanation
Question 59
During a total knee arthroplasty (TKA), internal rotation of the femoral component relative to the epicondylar axis will most likely result in which of the following complications?
Explanation
Question 60
A 25-year-old male sustains a humeral shaft fracture at the junction of the middle and distal thirds (Holstein-Lewis fracture).
Which nerve is most acutely at risk in this specific fracture pattern?

Explanation
Question 61
Which of the following ligaments is primarily responsible for stabilizing the base of the second metatarsal to the medial cuneiform, and is critically evaluated in midfoot trauma?
Explanation
Question 62
In the context of flexor tendon injuries of the hand, what anatomical landmarks define 'Zone II'?
Explanation
Question 63
A 16-year-old male presents with knee pain. Radiographs show an aggressive, bone-forming distal femoral metaphyseal lesion with periosteal reaction (Codman's triangle). Which is the most common site of metastasis for this suspected malignancy?
Explanation
Question 64
Which of the following muscles is innervated by the posterior interosseous nerve (PIN)?
Explanation
Question 65
A 35-year-old construction worker falls from a height and sustains a comminuted, displaced intra-articular calcaneus fracture.
If utilizing an extensile lateral approach for ORIF, the sural nerve is most at risk in which part of the incision?

Explanation
Question 66
Which of the following describes the typical mechanism of injury for a Hangman's fracture (traumatic spondylolisthesis of the axis)?
Explanation
Question 67
Which of the following cytokines is considered the major stimulator of osteoclast differentiation, activation, and bone resorption?
Explanation
Question 68
Perren's strain theory postulates specific mechanical environments for different types of bone healing. According to this theory, primary bone healing occurs without callus formation when the interfragmentary strain is maintained at:
Explanation
Question 69
A 25-year-old male presents with a displaced, vertically oriented femoral neck fracture (Pauwels type III). What is the most biomechanically stable fixation construct to resist the high shear forces inherent in this fracture pattern?
Explanation
Question 70
A 13-year-old obese male presents with a 2-month history of groin pain and an obligatory external rotation of the thigh during passive hip flexion. Following fixation of the affected hip, which of the following is the most robust indication for prophylactic pinning of the contralateral hip?
Explanation
Question 71
In the context of anterior cruciate ligament (ACL) reconstruction, which of the following graft choices possesses the highest initial ultimate tensile load?
Explanation
Question 72
When counseling a 40-year-old highly active patient regarding total hip arthroplasty (THA), which of the following bearing surface combinations should be noted as having the lowest linear and volumetric wear rates?
Explanation
Question 73
A 45-year-old male presents with bilateral lower extremity radicular pain, progressive leg weakness, and recent onset of bowel incontinence. MRI confirms a massive central L4-L5 disc herniation compressing the cauda equina. To maximize the probability of full sphincter function recovery, surgical decompression should ideally be performed within what timeframe from symptom onset?
Explanation
Question 74
During the surgical repair of a zone II flexor tendon laceration, preservation of the flexor sheath pulleys is critical. Which two pulleys are the most biomechanically important to prevent flexor tendon bowstringing?
Explanation
Question 75
A 28-year-old male presents with midfoot swelling after a fall from a horse. The AP foot radiograph demonstrates a small bony avulsion fragment in the first intermetatarsal space (the "fleck sign"). This fragment represents an avulsion of a ligament that classically originates from the:
Explanation
Question 76
Which of the following is the most frequent primary site of involvement for classic high-grade intramedullary osteosarcoma in the pediatric population?
Explanation
Question 77
A 4-year-old child presents with hip pain and a limp. According to the original Kocher criteria used to differentiate septic arthritis from transient synovitis, which of the following is NOT one of the four classic predictive variables?
Explanation
Question 78
A 40-year-old male sustains an anteroposterior compression (APC-III) pelvic ring injury. Upon arrival, he is hypotensive and tachycardic. Despite the immediate application of a pelvic binder and administration of 2 units of packed red blood cells, he remains hemodynamically unstable. What is the most appropriate next step in management?
Explanation
Question 79
A 65-year-old female presents with a dorsally displaced distal radius fracture. She is treated with open reduction and internal fixation utilizing a volar locking plate. What is the most common complication associated with this specific surgical approach and implant placement distal to the watershed line?
Explanation
Question 80
A 13-year-old obese male presents with left thigh pain and a limp for 3 weeks. An AP pelvis radiograph is evaluated.
On physical examination, what is the most likely finding when the affected hip is passively flexed?
Explanation
Question 81
A 55-year-old male presents with a painless, enlarging mass in the proximal humerus. Biopsy reveals a malignant cartilage-forming tumor with permeation of the host bone trabeculae. What is the most appropriate initial treatment for a conventional grade II chondrosarcoma?
Explanation
Question 82
During the process of secondary bone healing following a diaphyseal fracture, which of the following signaling molecules is most directly responsible for stimulating the differentiation of multipotent mesenchymal stem cells into osteoblasts?
Explanation
Question 83
A 68-year-old male presents with deteriorating handwriting, dropping objects, frequent falls, and hyperreflexia in both lower extremities. What is the most sensitive physical examination maneuver for detecting early upper motor neuron dysfunction in this patient's suspected condition?
Explanation
Question 84
A 22-year-old soccer player undergoes an anterior cruciate ligament reconstruction using a bone-patellar tendon-bone (BTB) autograft.
Six months postoperatively, she complains of persistent anterior knee pain when descending stairs. What is the most likely cause of her pain?

Explanation
Question 85
A 70-year-old female sustains a posterior dislocation of her total hip arthroplasty 4 weeks post-surgery. Her index surgical approach was posterior. To minimize the risk of recurrent posterior dislocation during a planned revision, which component position adjustment is most appropriate?
Explanation
Question 86
A 35-year-old male is brought to the trauma bay after an industrial crush injury. He has an open-book pelvic ring disruption (APC-III) and remains hemodynamically unstable despite a massive transfusion protocol. What is the most appropriate next step in management?
Explanation
Question 87
A 24-year-old male falls on an outstretched hand and sustains a fracture of the scaphoid proximal pole.
Which of the following anatomic factors most significantly increases the risk of avascular necrosis and nonunion in this specific fracture pattern?

Explanation
Question 88
A 30-year-old equestrian rider gets her foot caught in the stirrup, causing a severe hyperplantarflexion midfoot injury. Radiographs reveal pathological widening of the space between the medial and middle cuneiforms. The injured Lisfranc ligament primarily connects which two bony structures?
Explanation
None
Detailed Chapters & Topics
Dive deeper into specialized chapters regarding orthopedic-prometric-exam-preparation-mcqs-part-1
