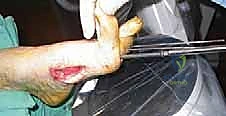
Alright, fellows, welcome to the operating theater. Today, we're tackling a challenging case: a Charcot midfoot deformity requiring an axial screw arthrodesis. This isn't just about putting screws in; it's about understanding the unique pathophysiology of Charcot neuroarthropathy, meticulous planning, and precise execution to salvage a limb in a patient with compromised sensation and bone quality.
Understanding Charcot Neuroarthropathy: The Foundation
Before we even consider making an incision, we must internalize the nature of Charcot foot. This is a progressive, destructive arthropathy occurring in patients with peripheral neuropathy, most commonly diabetes. The loss of protective sensation, coupled with repetitive microtrauma, leads to bony dissolution, fragmentation, and severe deformity, often progressing to a "rocker-bottom" foot.
Pathogenesis and Clinical Presentation
The underlying problem is multifaceted:
* Neuropathy: Glycosylation and diminished blood supply to peripheral nerves cause progressive loss of sensation, motor innervation, and autonomic function. Longer nerves are more severely affected, leading to the classic "stocking and glove" sensory deficit.
* Motor Imbalance: Loss of motor function results in intrinsic muscle imbalance, often causing an equinus contracture of the ankle and Achilles. This significantly increases forefoot and midfoot pressures during gait, exacerbating the deformity. Intrinsic foot muscle imbalance also contributes to clawing of the hallux and lesser digits.
* Autonomic Dysfunction: This leads to drying and cracking of the skin, compromising the integumentary barrier against pathogens. Furthermore, loss of vasomotor control can cause edema and stasis, further complicating wound healing and increasing infection risk.
* Bone Dissolution: Repetitive microtrauma in insensate joints, combined with a neurally stimulated vasomotor response increasing blood flow, leads to accelerated bony dissolution. This process is typically painless, meaning patients may present late with massive swelling, gross deformity, ulceration, and even infection.
Eichenholz Staging and Prognostic Factors
We classify Charcot neuroarthropathy using Eichenholz stages:
* Stage I (Inflammatory): The foot is hyperemic, swollen, and hot. Radiographs show bony dissolution and fragmentation. Differentiating this from infection can be challenging due to similar physical signs.
* Stage II (Coalescence): Swelling, edema, and warmth decrease.
* Stage III (Consolidation): Bony consolidation occurs, often with significant residual deformity. Patients presenting in this stage typically have a stable deformity, potentially amenable to bracing.
Prognosis is significantly influenced by:
1. Presence of Infection: A critical determinant for limb salvage.
2. Adequate Blood Flow: To the level of the digits.
3. Chronic Venous Stasis: With associated poor integument.
4. Control of Medical Comorbidities: Especially diabetes. Immunocompromised patients (e.g., transplant, dialysis) have a much worse prognosis.
Surgical Indications
While most non-infected Charcot arthropathy can be managed non-operatively with total-contact casting or custom orthotics, surgery is reserved for specific situations:
* Gross instability on physical examination.
* Acute fracture-dislocation from trauma.
* Progressive or unbraceable deformities.
* Recurrent ulcerations despite multiple attempts at accommodative bracing.
* Deformity at the level of the midfoot is poorly tolerated and leads to significantly increased plantar pressures, which, combined with loss of sensation and impaired integumentary function, frequently results in ulceration and deep infection.
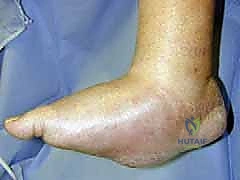
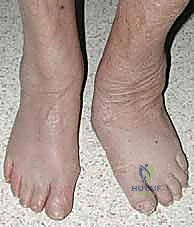
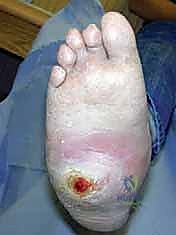
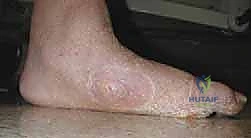
Figure: Clinical deformity with midfoot fracture-dislocation and plantar ulceration.
Comprehensive Surgical Anatomy for Midfoot Arthrodesis
Fellows, a thorough understanding of the midfoot anatomy is paramount to avoid iatrogenic injury and achieve a stable construct. We're primarily focusing on the tarsometatarsal (TMT) joints, intercuneiform joints, and potentially extending to the naviculocuneiform joints.
Osteology and Joint Relationships
The midfoot is a complex array of bones:
* Medial Column: Navicular, medial cuneiform, first metatarsal.
* Middle Column: Intermediate cuneiform, lateral cuneiform, second and third metatarsals.
* Lateral Column: Cuboid, fourth and fifth metatarsals.
Charcot fracture-dislocation can occur through any of these joints, often with extensive bony dissolution and fragmentation. The goal of this technique is to bridge these areas of dissolution, obtaining fixation in more normal bone proximally and distally.
Neurovascular Structures: A Constant Vigilance
The dorsal aspect of the foot, where we'll be making our approaches, harbors critical neurovascular structures.
* Dorsalis Pedis Artery: This is a direct continuation of the anterior tibial artery, running distally from the ankle joint, typically between the extensor hallucis longus (EHL) and extensor digitorum longus (EDL) tendons. It's crucial for foot perfusion, especially in diabetic patients.
* Deep Peroneal Nerve: Accompanies the dorsalis pedis artery, providing sensation to the first web space and motor innervation to the extensor digitorum brevis.
* Superficial Peroneal Nerve: Divides into medial and intermediate dorsal cutaneous nerves, providing sensation to the dorsum of the foot. These branches are highly variable and extremely susceptible to injury during dorsal approaches.
* Dorsal Venous Arch: Superficial veins that can be a source of significant bleeding if not carefully managed.
Muscular Intervals and Tendon Management
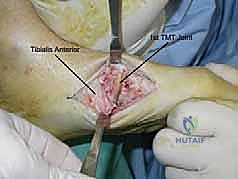
- Tibialis Anterior: Inserts primarily on the medial cuneiform and base of the first metatarsal. Its insertion may be involved in the deformity. If detached, it must be reattached to maintain foot balance.
- Tibialis Posterior: Inserts on the navicular tuberosity, cuneiforms, and bases of the second to fourth metatarsals. Also critical for arch support.
- Extensor Tendons (EHL, EDL): These will be retracted to expose the dorsal midfoot. Care must be taken to avoid excessive traction.
Surgical Warning: In Charcot patients, bone quality is often poor and soft tissues are friable. Meticulous, gentle dissection is paramount to protect neurovascular structures and minimize soft tissue damage, which could lead to wound complications.
Preoperative Planning: The Blueprint for Success
Fellows, the success of this complex reconstruction begins long before we scrub in. Preoperative planning is absolutely critical in Charcot cases.
Infection and Vascular Workup
- Infection Status: Active infection or osteomyelitis is a contraindication for this technique, as the hardware is typically permanent and difficult to remove without significant bony destruction. We must establish the absence of infection.
- Radiographs: Provide initial staging but are unreliable for distinguishing infection from Charcot.
- MRI: Useful, but caution is needed. Bone destruction and edema can be present without infection. Gadolinium enhancement, fluid collections (abscess), or air are stronger indicators of infection.
- CT Scan: Excellent for bony detail and surgical planning. Air on CT is diagnostic of deep infection, often communicating with an ulcer.
- Nuclear Imaging: A three-phase technetium bone scan combined with a labeled white blood cell scan is particularly useful to differentiate sterile Charcot from soft tissue infection or osteomyelitis.
- Vascular Status: Arterial insufficiency is a relative contraindication. We perform rigorous noninvasive vascular testing. If significant insufficiency is present, a staged arterial reconstruction by a vascular surgeon is necessary before our procedure.
Medical Optimization and Timing of Surgery
- Medical Comorbidities: Close involvement of an astute internist or endocrinologist is vital for optimizing diabetes control and managing other medical conditions.
- Timing:
- Acute Trauma (without significant swelling/inflammation): If recognized early, reduction and fusion can proceed within 1-2 weeks.
- Inflammatory Phase (Stage I): We prefer to cast the patient for 6-8 weeks to allow edema to resolve and perform the reconstruction in a staged manner. Rushing surgery in an acute inflammatory phase significantly increases complication rates.
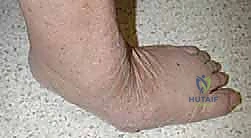
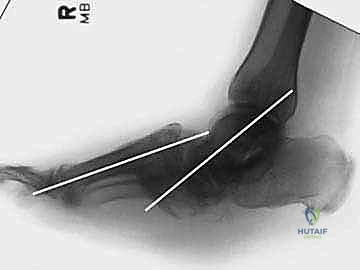
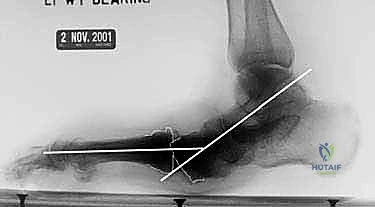
Figure: Preoperative clinical radiographs showing dislocation at the tarsometatarsal joint.
Imaging for Surgical Planning
- Weight-bearing Radiographs: AP, lateral, and oblique views of the foot and ankle are essential to stage the deformity, assess alignment, and identify areas of bony destruction.
- CT Scan: Invaluable for understanding the 3D bony architecture, the extent of fragmentation, and planning bone resection. It helps us anticipate the amount of bone we'll need to remove to achieve a plantigrade foot without excessive soft tissue tension.
Templating and Hardware Selection
- Screw Selection: We'll be using large-bore cannulated screws. For the medial column (1st TMT joint), we typically plan for 6.5mm or 8.0mm screws. For the lesser metatarsals (2nd-5th TMT joints), 4.5mm or 5.0mm screws are usually appropriate. We need a variety of lengths.
- Guidewires: Ensure we have multiple lengths and types.
- Ancillary Fixation: Consider temporary K-wires, external fixators, or even intramedullary devices for severe instability.
Patient Positioning and Pre-Incision Maneuvers
Alright team, let's get our patient positioned.
Positioning
- Supine Position: The patient is positioned supine on the operating table.
- Hip Bump: A small bump is placed under the ipsilateral hip. This internally rotates the limb slightly, allowing the toes to face perpendicular to the operating table, which provides better access to the medial and dorsal aspects of the foot and optimizes fluoroscopic views.
- Pneumatic Tourniquet: A pneumatic tourniquet is applied to the proximal thigh. We will inflate this after our initial soft tissue release to ensure a bloodless field, which is crucial for precise dissection and identifying subtle anatomical landmarks in a foot with often distorted anatomy.
- Prep and Drape: The entire limb is prepped and draped from above the knee to the toes, allowing for full range of motion of the ankle and foot during the procedure.
Tendo-Achilles Lengthening (TAL) or Gastroc-Soleus Recession
- Crucial First Step: Before inflating the tourniquet, we must address the often-present equinus contracture. A three-step percutaneous tendo-Achilles lengthening (TAL) or an open gastroc-soleus recession is performed.
- Goal: To achieve at least 15 degrees of ankle dorsiflexion. This is non-negotiable. If we don't correct the equinus, the forces across the midfoot will remain excessive post-fusion, leading to recurrent deformity, nonunion, or hardware failure.
- Technique (Percutaneous TAL):
- First Cut: With the ankle maximally dorsiflexed, make a small stab incision (e.g., #15 blade) on the medial side of the Achilles tendon, approximately 4-5 cm proximal to its insertion, cutting two-thirds of the tendon.
- Second Cut: With the ankle maximally plantarflexed, make another stab incision on the lateral side of the Achilles, approximately 2-3 cm distal to the first cut, cutting two-thirds of the tendon.
- Third Cut: With the ankle maximally dorsiflexed again, make a final stab incision on the medial side, approximately 2-3 cm distal to the second cut, cutting two-thirds of the tendon.
- Feel the Release: Gently dorsiflex the ankle. You should feel a palpable "give" as the tendon lengthens. Confirm at least 15 degrees of passive dorsiflexion.
Intraoperative Execution: The Axial Screw Technique
Now, fellows, let's get scrubbed in. We'll proceed systematically, column by column, ensuring meticulous reduction and stable fixation.
Approach: Strategic Incisions for Exposure
We typically employ a two- or three-incision approach to adequately expose the deformity, reduce it, and prepare the arthrodesis bed.
-
Medial Approach (for Medial Column):
- Incision: Make a longitudinal incision, approximately 6-8 cm, centered over the medial column, extending from the navicular-cuneiform joint to the base of the first metatarsal.
- Deep Dissection: Carefully identify and protect the saphenous vein and nerve, which lie subcutaneously. Deepen the incision through subcutaneous tissue.
- Tibialis Anterior Management: The insertion of the tibialis anterior tendon on the medial cuneiform and first metatarsal base is often involved in the deformity. If it's attached to fragmented or dislocated bone, we will release it. Use a nonabsorbable suture (e.g., 2-0 Fiberwire) placed in a locking fashion through the tendon, tagging it for later reattachment. Perform a subperiosteal dissection to expose the medial cuneiform, navicular, and first metatarsal base.
- Exposure: Use small Hohmann retractors or similar instruments to maintain exposure.
-
Dorsal Approach (for Middle Column):
- Incision: Make a second longitudinal incision, approximately 6-8 cm, centered between the second and third metatarsal bases. This provides access to the intermediate and lateral cuneiforms, and the bases of the second and third metatarsals.
- Skin Bridge:
> Surgical Warning: Maintain an adequate skin bridge (at least 2-3 cm) between the dorsal incisions to prevent wound necrosis or dorsal skin slough, a devastating complication in these patients. - Deep Dissection: Carefully dissect through the subcutaneous tissue. Identify and protect the branches of the superficial peroneal nerve and the dorsal venous arch. Retract the extensor tendons (EHL, EDL) gently.
- Neurovascular Protection:
> Surgical Warning: Be acutely aware of the dorsalis pedis artery and deep peroneal nerve, which run in this general vicinity. Use blunt dissection and careful retraction to avoid injury. A small, curved Metzenbaum scissors or blunt probe can help identify these structures. - Exposure: Perform a subperiosteal dissection to expose the middle column joints.
-
Lateral Dorsal Approach (for Lateral Column, if necessary):
- Incision: If the lateral column (cuboid-4th/5th TMT joints) is significantly involved, a third longitudinal incision, approximately 5-7 cm, is made dorsally at the level of the fourth and fifth tarsometatarsal joints.
- Skin Bridge: Again, ensure an adequate skin bridge with the central dorsal incision.
- Deep Dissection: Similar careful dissection, protecting superficial peroneal nerve branches.
- Exposure: Subperiosteal dissection to expose the lateral column joints.
Resection of Deformity and Joint Preparation
Now, with our exposures achieved, we move to the crucial step of deformity correction and joint preparation. Our goal is to create broad, bleeding bone surfaces for fusion and achieve a plantigrade foot without excessive tension on the dorsal soft tissues.
- Deformity Assessment: Visually inspect the extent of bony dissolution, fragmentation, and dislocation. Often, the metatarsals are dorsally dislocated relative to the tarsals.
- Bone Resection:
- Initial Resection: Using an oscillating saw (e.g., sagittal saw with a small, narrow blade), perform bone resection at the level of the deformity. For the medial column, resect bone medially; for the middle and lateral columns, resect dorsally.
- Proximal and Distal Fragments: Remove bone from both the proximal and distal fragments involved in the fracture-dislocation.
- Debridement: Use a curved curette, pituitary rongeur, or osteotome to meticulously remove all necrotic, sclerotic, and fragmented bone from the fusion sites. We want healthy, bleeding cancellous bone.
- Sequential Resection and Reduction: This is a dynamic process, fellows. Resect bone slowly and incrementally. After each pass of the saw or rongeur, attempt to manually reduce the deformity.
> Surgical Warning: Adequate bone resection is necessary to prevent excessive tension on the dorsal soft tissue envelope and vascular structures once the foot is reduced. However, it is equally important not to resect too much bone, as this can lead to a gap that prevents adequate bony apposition, jeopardizing fusion. We need a balanced reduction. - Achieving Reduction: Apply gentle longitudinal traction and direct pressure to reduce the midfoot. Temporary K-wires can be used to hold the reduction once achieved. The foot should be plantigrade, meaning the plantar aspect of the foot rests flat on the table without any bony prominences.
- Cartilage Removal: Ensure all articular cartilage is removed from the surfaces to be fused to promote bony union.
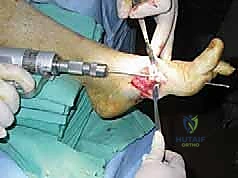
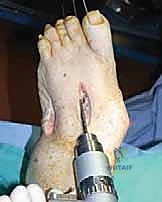
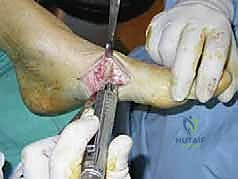
Figure: Bone resection at the level of deformity to allow reduction.
Axial Screw Placement: The Core Technique
This technique uses long, axial cannulated screws to bridge the areas of dissolution and achieve fixation in healthier bone proximally and distally.
- Medial Column First (First Metatarsal): We typically start with the medial column as it's critical for stability.
- Guidewire Placement:
- Entry Point: Identify the head of the first metatarsal. The entry point for the guidewire will be on the dorsal aspect of the first metatarsal head, slightly off-center to allow for screw purchase.
- Trajectory: Under constant fluoroscopic guidance (AP, lateral, and oblique views), carefully advance a 1.6mm or 2.0mm guidewire. The trajectory should be axial, crossing the first metatarsophalangeal (MTP) joint, traversing the first metatarsal shaft, crossing the TMT joint, and engaging into the medial cuneiform, navicular, and ideally, into the talus or even the calcaneus. The goal is to bridge the area of dissolution and achieve bicortical purchase in healthy bone proximally.
> Surgical Warning: Pay close attention to the guidewire tip. It must remain within the bone and not penetrate the plantar cortex, which could lead to plantar ulceration postoperatively. Lateral fluoroscopy is crucial to confirm the depth and trajectory. - Confirmation: Confirm optimal position in all fluoroscopic views. The guidewire should be well-seated, providing initial stability.
- Drilling:
- Sequential Drilling: Once the guidewire is perfectly positioned, use a cannulated drill bit over the guidewire. Start with a smaller drill (e.g., 2.5mm or 3.5mm) and then sequentially increase to the planned screw diameter.
- Irrigation: Drill under constant irrigation to prevent thermal necrosis of the bone, especially important in compromised Charcot bone.
- Final Drill: For the medial column, we typically drill to 5.5mm in preparation for a 6.5mm or 8.0mm cannulated screw.
- Screw Length Measurement: Use the guidewire depth gauge to accurately measure the required screw length.
- Screw Insertion: Insert a fully threaded or partially threaded cannulated screw over the guidewire. Advance the screw slowly and gently, ensuring good purchase. The screw should provide compression across the fusion site.
- Guidewire Placement:
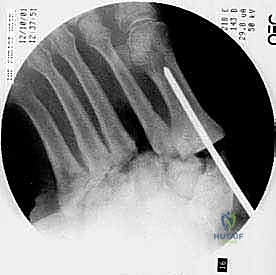
Figure: Guidewire placement for axial screw across the first metatarsal and medial cuneiform.
- Lesser Metatarsals (Second and Third Metatarsals - Middle Column):
- Guidewire Placement:
- Entry Point: Similar to the first metatarsal, place guidewires on the dorsal aspect of the second and third metatarsal heads.
- Trajectory: Advance guidewires axially, crossing the MTP joints, traversing the metatarsal shafts, TMT joints, and engaging into the intermediate and lateral cuneiforms, and potentially the cuboid or even calcaneus. Again, the goal is to bridge the dissolution and achieve good proximal fixation.
> Surgical Warning: Be mindful of the dorsal neurovascular structures, especially between the 1st and 2nd metatarsals. Maintain careful retraction.
- Drilling: Drill sequentially over the guidewires. For the lesser metatarsals, we typically drill to 4.5mm in preparation for a 4.5mm or 5.0mm cannulated screw.
- Screw Insertion: Insert appropriate length cannulated screws.
- Guidewire Placement:
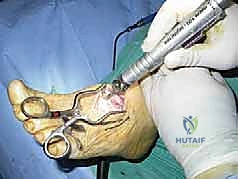
Figure: Guidewire placement for axial screw across the lesser metatarsals.
- Lateral Column (Fourth and Fifth Metatarsals, if involved):
- Guidewire Placement: If the lateral column is unstable or involved in the deformity, place guidewires through the fourth and fifth metatarsal heads, traversing their shafts, the TMT joints, and engaging into the cuboid and potentially the calcaneus.
- Drilling and Screw Insertion: Follow the same principles of sequential drilling and screw insertion using 4.5mm or 5.0mm cannulated screws.
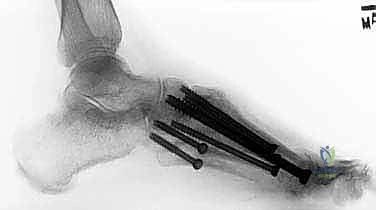
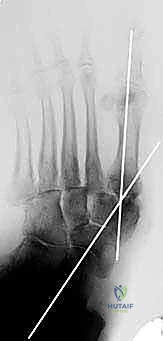
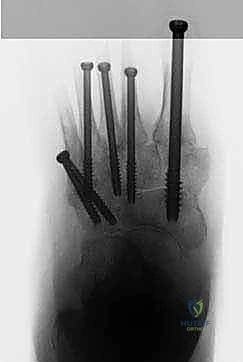
Figure: Intraoperative fluoroscopic image showing guidewires in place for axial screw fixation.
Final Reduction and Confirmation
- Fluoroscopic Confirmation: After all screws are placed, obtain final AP, lateral, and oblique fluoroscopic images. Confirm that the deformity is fully reduced, the foot is plantigrade, and all screws are well-positioned, providing stable fixation without violating joint spaces or exiting the bone.
- Manual Assessment: Palpate the plantar aspect of the foot to ensure no bony prominences remain that could lead to ulceration.
- Bone Grafting (Optional but Recommended): If there are significant bony defects after reduction, consider autogenous bone graft (from the resected bone) or allograft to fill these gaps and enhance fusion.
Closure
- Tendon Reattachment: If the tibialis anterior tendon was released, reattach it securely to the remaining bone (e.g., medial cuneiform or first metatarsal base) using the previously placed locking sutures or bone anchors.
- Layered Closure:
- Close the deep fascial layers with absorbable sutures.
- Carefully approximate the subcutaneous tissues.
- Close the skin with interrupted non-absorbable sutures or staples.
Surgical Warning: Ensure no tension on the skin closures. If significant tension exists, consider a wider skin bridge or alternative fixation methods in the future. Skin edges should be everted.
- Sterile Dressing: Apply a sterile dressing, followed by a well-padded splint or cast.
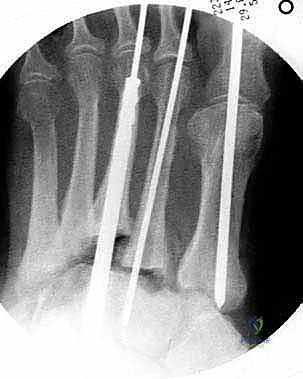
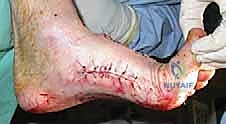
Figure: Postoperative lateral radiograph showing reduced deformity and axial screw fixation.
Pearls and Pitfalls: Navigating the Minefield
Fellows, these are complex cases, and things can go wrong. Anticipation and preparation are key.
Pearls
- Achilles Lengthening is Non-Negotiable: Correcting equinus is paramount for long-term success. Don't skip it.
- Adequate Resection, Not Excessive: The sweet spot is enough bone removal to achieve a plantigrade foot without tension, but not so much that you create a large gap or lose bony apposition.
- Fluoroscopy is Your Best Friend: Use it constantly for guidewire placement, drill depth, and screw position. Don't guess.
- Protect Neurovascular Structures: Always be mindful of the dorsalis pedis artery, deep peroneal nerve, and superficial peroneal nerve branches. Gentle retraction and blunt dissection are critical.
- Skin Bridges: Maintain adequate skin bridges between dorsal incisions to prevent devastating wound complications.
- Plantigrade Foot: The ultimate intraoperative goal is a stable, plantigrade foot without any bony prominences. Palpate the plantar aspect rigorously.
- Bone Grafting: Consider for large defects to enhance fusion rates, especially in poor bone quality.
- Bridging Dissolution: The axial screw technique's strength lies in bridging the areas of poor bone quality and dissolution, securing fixation in healthier bone proximally and distally.
Pitfalls and Salvage Strategies
- Infection/Osteomyelitis:
- Intraoperative Suspicion: If you encounter purulence or necrotic bone not identified preoperatively, send cultures immediately. Debride all infected tissue.
- Salvage: Do not place permanent hardware if active infection is confirmed. Consider temporary external fixation, delayed definitive fusion after a course of IV antibiotics, or even amputation in severe cases.
- Postoperative Infection: Aggressive debridement, IV antibiotics, and potentially hardware removal. If fusion is stable, sometimes hardware can be removed later.
- Neurovascular Injury:
- Prevention: Meticulous dissection, careful retraction, and constant awareness.
- Recognition: Intraoperative bleeding (arterial/venous), nerve transection (visualized), or nerve stretch (postoperative numbness/weakness).
- Salvage: Direct repair of nerve lacerations (if recognized), vascular repair/ligation depending on the vessel and collateral flow.
- Inadequate Reduction / Persistent Deformity:
- Cause: Insufficient bone resection, persistent soft tissue contracture, or unaddressed equinus.
- Salvage: Re-evaluate bone resection. Perform further bony debridement. Check Achilles lengthening. Apply more aggressive reduction maneuvers (e.g., external fixator for temporary distraction/compression). If screws are already placed, they may need to be removed, reduction re-established, and new screws placed.
- Screw Malposition / Plantar Prominence:
- Cause: Incorrect guidewire placement, leading to screw exiting the plantar cortex or violating a joint.
- Salvage: Remove the screw. Re-insert a new guidewire with corrected trajectory under fluoroscopic guidance. If bone quality is severely compromised by the previous hole, consider a different screw trajectory or a larger diameter screw to gain purchase.
- Screw Breakage / Nonunion:
- Risk Factors:
Additional Intraoperative Imaging & Surgical Steps
REFERENCES
-
Alvarez RG, Barbour TM, Perkins TD. Tibiocalcaneal arthrodesis for nonbraceable neuropathic ankle deformity. Foot Ankle Int 1994;15:354–359.
-
Bono JV, Roger DJ, Jacobs RL. Surgical arthrodesis of the neuropathic foot: a salvage procedure. Clin Orthop Relat Res 1993;296:14–20.
-
Campbell JT. Intra-articular neuropathic fracture of the calcaneal body treated by open reduction and subtalar arthrodesis. Foot Ankle Int 2001;22:440–444.

Detailed Chapters & Topics
Dive deeper into specialized chapters regarding axial-screw-technique-for-midfoot-arthrodesis-in-charcot-foot-deformities
