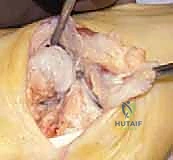
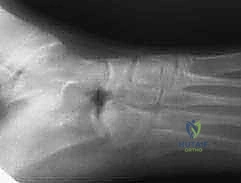
Minimally Invasive Gradual Realignment and Arthrodesis for Charcot Foot Deformity: An Intraoperative Masterclass

Key Takeaway
This masterclass details a two-stage minimally invasive approach for Charcot foot deformity. We'll cover comprehensive preoperative planning, precise patient positioning, and granular intraoperative execution of gradual realignment with external fixation, followed by percutaneous arthrodesis. Emphasis is placed on neurovascular protection, meticulous technique, and managing potential pitfalls to achieve stable, plantigrade foot reconstruction and prevent amputation.
Welcome, fellows, to the operating theater. Today, we're tackling one of the most challenging conditions in orthopaedic surgery: Charcot neuroarthropathy. We'll be performing a two-stage minimally invasive gradual correction of a midfoot Charcot deformity, a technique pioneered by Dr. Paley, utilizing external fixation followed by percutaneous arthrodesis. This approach offers significant advantages over traditional open methods, particularly for severe, unstable deformities.
Understanding Charcot Neuroarthropathy and Our Surgical Philosophy
Charcot neuroarthropathy is a progressive, destructive process affecting joints, often in the foot and ankle, secondary to underlying neuropathy. This can be from diabetes, syphilis, or other conditions. The loss of protective sensation, coupled with repetitive microtrauma and an inflammatory response, leads to bone resorption, ligamentous laxity, joint subluxation, dislocation, and ultimately, severe osseous malalignment.
Our primary goal in chronic Charcot neuroarthropathy is to restore anatomical alignment, impart stability, prevent devastating complications like ulceration, infection, and amputation, preserve limb length, and ultimately, allow the patient to be ambulatory.
The Challenge of Acute Deformity Correction
Traditionally, acute realignment procedures – involving extensive osteotomies, débridement, arthrodesis, and open reduction with internal fixation – have been attempted. However, in these extremely deformed feet, acute realignment is often challenging and fraught with complications. Large open incisions can lead to significant soft tissue compromise, neurovascular injury, poor wound healing, and incomplete deformity reduction, often resulting in foot shortening. Moreover, maintaining non–weight-bearing status for months in this patient population is notoriously difficult due to muscle atrophy, obesity, and diminished proprioception, which can lead to osteopenia and increased stress on the contralateral limb.
This is where our two-stage gradual correction method shines. It allows for precise, controlled realignment of dislocated or subluxated Charcot joints, minimizing soft tissue trauma and reducing the risk of acute neurovascular compromise. For an unstable or incompletely coalesced Charcot foot, gradual distraction with external fixation is the preferred method. Even in cases with radiographic appearance of coalescence, many Charcot deformities can undergo distraction without formal osteotomy, leveraging the underlying bone fragility and ligamentous laxity.
Comprehensive Surgical Anatomy: Navigating the Charcot Foot
Before we make any incision, let's review the critical anatomy of the midfoot and hindfoot, focusing on neurovascular structures and osseous landmarks relevant to our fixation strategy.
Osteology and Joint Relationships
- Hindfoot: Calcaneus, talus. We'll be fixing to the calcaneus and talar neck. The subtalar joint is often spared and we aim to preserve it.
- Midfoot: Navicular, cuboid, and three cuneiforms. These articulate with the talus and calcaneus proximally and the metatarsals distally. The primary sites of Charcot collapse are often at the talonavicular, calcaneocuboid, and cuneonavicular joints, or the tarsometatarsal (Lisfranc) joints.
- Forefoot: Metatarsals and phalanges. We will be spanning from the metatarsals into the hindfoot.
Neurovascular Structures: Our Guiding Principles for Safety
- Medial Side: The posterior tibial neurovascular bundle (posterior tibial artery, posterior tibial nerve, and venae comitantes) runs posterior to the medial malleolus and then divides into medial and lateral plantar nerves and arteries. When placing wires or pins in the calcaneus or medial midfoot, we must be acutely aware of this bundle. The saphenous nerve and great saphenous vein run anterior to the medial malleolus and ascend along the medial aspect of the leg.
- Lateral Side: The sural nerve runs along the lateral aspect of the foot and ankle. Wires and pins in the lateral calcaneus or cuboid region must respect this structure. The superficial peroneal nerve (also known as the musculocutaneous nerve) runs anterolaterally in the leg and divides into intermediate and medial dorsal cutaneous nerves, supplying sensation to the dorsum of the foot. Pins in the distal tibia and forefoot dorsum require careful consideration of its branches.
- Dorsal Side: The dorsalis pedis artery is a continuation of the anterior tibial artery, running on the dorsum of the foot. It's often palpable and provides a critical blood supply to the forefoot. The deep peroneal nerve accompanies it.
- Plantar Side: The medial and lateral plantar nerves and arteries are crucial for sensation and blood supply to the plantar aspect of the foot. Our percutaneous screw insertion technique for arthrodesis will involve a plantar approach, demanding extreme caution to avoid these structures.
Muscular Intervals
- Achilles Tendon: The largest tendon in the body, formed by the gastrocnemius and soleus, inserting into the calcaneus. Our percutaneous Z-lengthening will address the equinus deformity often seen in Charcot feet.
- Tibialis Anterior: Inserts into the medial cuneiform and first metatarsal base.
- Peroneus Brevis/Longus: Insert into the fifth metatarsal base and first metatarsal/medial cuneiform, respectively.
- Understanding these muscle-tendon units is crucial for assessing and correcting the dynamic forces contributing to the deformity.
Preoperative Planning and Patient Positioning: Setting the Stage for Success
Fellows, meticulous preoperative planning is paramount. This isn't just about identifying the deformity; it's about understanding its multiplanar nature and planning every wire, pin, and screw trajectory.
Imaging and Templating
We start with standard weight-bearing AP, lateral, and oblique radiographs of the foot and ankle, along with a full-length tibia film.
* AP Radiograph: Evaluate midfoot adduction/abduction, talar-first metatarsal angle (Meary's angle).
* Lateral Radiograph: Assess the rocker-bottom deformity, equinus, and forefoot dorsiflexion/plantarflexion. Meary's angle on the lateral view helps quantify the sagittal plane collapse. Calcaneal pitch angle is also critical.
* CT Scans: Often invaluable for assessing bone quality, fragmentation, and joint congruity, especially in complex cases.
* Fluoroscopy: Intraoperatively, we'll rely heavily on fluoroscopy. Ensure the C-arm is draped and positioned for easy orthogonal (AP and lateral) views of the entire foot and distal tibia without repositioning the patient.
Patient Positioning and OR Setup
- Position: The patient is positioned supine on the operating table.
- Leg Prep: The affected limb is prepped and draped from the mid-thigh to the toes, allowing full access to the foot, ankle, and distal tibia.
- Bolster: A small bump or roll is placed under the ipsilateral hip to internally rotate the limb slightly, ensuring the foot is in a neutral position relative to the table and allowing for true AP views.
- Tourniquet: A high thigh tourniquet is applied, but not inflated initially. We may inflate it for the Achilles lengthening or if significant bleeding is encountered, but generally, we prefer to work without it to assess perfusion.
- Fluoroscopy: The C-arm is brought in from the contralateral side of the table, allowing for easy AP and lateral views. Ensure the image intensifier is positioned to capture both the distal tibia and the entire foot.
- Table Attachments: We'll need a stable setup for the external fixator. Ensure all necessary clamps and posts are readily available.
External Fixation Planning: The Taylor Spatial Frame (TSF)
The Taylor Spatial Frame is central to our gradual correction.
* Software: We utilize the Internet-based software (www.spatialframe.com) for planning. This requires precise input of mounting parameters.
* Reference Ring: We'll choose either the distal tibial ring or the forefoot ring as our reference. For foot deformities, a distal reference ring is typically chosen.
* Deformity Input: Based on our preoperative radiographs and intraoperative fluoroscopic images, we'll input the specific deformity magnitude and axis into the software.
* Correction Schedule: The software then generates a daily schedule of strut adjustments for the patient, dictating the rate and duration of correction. This allows us to control the speed of realignment, typically aiming for 1-2 mm of distraction per day, adjusted based on patient tolerance and soft tissue response.
Stage 1: External Fixation Application and Gradual Realignment
Alright, fellows, let's scrub in. This is where we lay the foundation for correction. Our first stage focuses on achieving a neutral hindfoot position and applying the Taylor Spatial Frame for gradual forefoot realignment.
Step-by-Step Intraoperative Execution (Stage 1)
1. Achilles Tendon Lengthening
- Objective: Correct the often-present equinus deformity and achieve a neutral hindfoot position, which is critical for successful forefoot alignment.
- Technique: We perform a percutaneous Z-lengthening of the Achilles tendon.
- Incision: Identify the Achilles tendon. Make a 1-2 cm transverse incision on the medial side of the tendon, approximately 3-4 cm proximal to its insertion on the calcaneus. Use a small blade (e.g., #15) to incise approximately two-thirds of the tendon thickness.
- Second Incision: Distally, make another 1-2 cm transverse incision on the lateral side of the tendon, approximately 2 cm proximal to its insertion. Again, incise approximately two-thirds of the tendon thickness.
- Lengthening: With the incisions made, gently dorsiflex the ankle. You should feel the tendon fibers separate and lengthen. Aim for at least neutral dorsiflexion, ideally 5-10 degrees of dorsiflexion without excessive force. Confirm the hindfoot can be manually held in a neutral position.
- Closure: Close the small skin incisions with absorbable sutures.
2. Distal Tibial Fixation Block Application
- Objective: Create a stable proximal anchor for our external fixator.
- Ring Placement: We'll start by applying a full external fixation ring to the distal tibia. This ring should be positioned approximately 2-3 cm proximal to the ankle joint line to allow for soft tissue clearance and avoid joint impingement.
- Wire/Pin Insertion:
- U-plate to Tibia: We'll use a U-plate fixed to the tibia for initial stability. First, insert a 1.8-mm lateromedial smooth wire through the tibia, ensuring it's orthogonal to the long axis of the tibia. This is typically done about 5-7 cm proximal to the ankle joint.
- Surgical Warning:
> CRITICAL PEARL: When inserting lateromedial wires in the distal tibia, be mindful of the superficial peroneal nerve anterolaterally and the saphenous nerve and great saphenous vein medially. Make small stab incisions and use a drill sleeve to protect soft tissues.
- Surgical Warning:
- Additional Fixation: Supplement this with two or three additional points of fixation. These can be a combination of smooth wires (1.8mm) or half-pins (e.g., 5.0mm). We prefer a delta configuration of half-pins for maximum stability in the distal tibia.
- Technique for Half-Pins: Make a small stab incision, use a blunt trocar to dissect down to the bone, insert a drill guide, and then drill the pilot hole. Advance the half-pin under constant fluoroscopic guidance, ensuring it engages both cortices.
- Second Distal Tibial Ring: For additional stability, especially in larger patients or those with poor bone quality, we often add a second distal tibial ring, creating a robust distal tibial fixation block. This second ring is connected to the first with threaded rods.
- U-plate to Tibia: We'll use a U-plate fixed to the tibia for initial stability. First, insert a 1.8-mm lateromedial smooth wire through the tibia, ensuring it's orthogonal to the long axis of the tibia. This is typically done about 5-7 cm proximal to the ankle joint.
3. Hindfoot Fixation
- Objective: Secure the hindfoot in the corrected, neutral position achieved after Achilles lengthening.
- U-plate to Calcaneus: With the hindfoot manually held in a neutral position, we'll fix a second U-plate to the calcaneus.
- Wire Insertion: Insert two crossing 1.8-mm smooth wires through the calcaneus. These wires should capture the body of the calcaneus, providing strong purchase.
- Surgical Warning:
> CRITICAL PITFALL: Be extremely cautious of the posterior tibial neurovascular bundle medially and the sural nerve laterally when placing calcaneal wires. Always make a small stab incision, spread with a hemostat, and use a drill sleeve to protect soft tissues. Fluoroscopic guidance is essential to ensure wires stay within the bone envelope.
- Surgical Warning:
- Talar Neck Wire: Next, insert a 1.8-mm mediolateral smooth wire through the talar neck. This wire is then fixed to the calcaneal U-plate. This provides a stable connection between the talus and calcaneus, stabilizing the hindfoot.
- Surgical Warning:
> CRITICAL PEARL: The talar neck is a confined space. Ensure the wire trajectory avoids the subtalar joint and the neurovascular structures anteriorly (dorsalis pedis artery, deep peroneal nerve) and posteriorly (posterior tibial neurovascular bundle). Use a small drill bit and gentle technique.
- Surgical Warning:
- Wire Insertion: Insert two crossing 1.8-mm smooth wires through the calcaneus. These wires should capture the body of the calcaneus, providing strong purchase.
4. Forefoot Fixation
- Objective: Create a distal segment for gradual distraction and realignment.
- Full Forefoot Ring: Mount a full external fixation ring to the forefoot.
- Metatarsal Wires: Insert two crossing 1.8-mm smooth wires through the metatarsals, typically spanning the second to fourth metatarsals. These wires provide the primary fixation for the forefoot ring.
- Surgical Warning:
> CRITICAL PITFALL: Avoid performing Gigli saw osteotomy across multiple metatarsals due to the high risk of neurovascular injury. For wire placement, aim for the midshafts of the metatarsals to maximize bone purchase and avoid the neurovascular bundles in the intermetatarsal spaces.
- Surgical Warning:
- Digital Pinning: In cases with significant forefoot splaying or digital deformities, digital wires (1.5 or 1.8 mm) can be inserted through the phalanges and attached to the forefoot ring. This provides additional control for digital alignment.
- Metatarsal Wires: Insert two crossing 1.8-mm smooth wires through the metatarsals, typically spanning the second to fourth metatarsals. These wires provide the primary fixation for the forefoot ring.
5. Stirrup Wire Placement
- Objective: Focus distraction precisely at the Charcot joints, preventing unwanted distraction elsewhere.
- Technique: Insert two 1.8-mm stirrup wires through the osseous segments just proximal and distal to the primary Charcot joints (typically the midfoot).
- Placement: These wires are bent 90 degrees just outside the skin, extending towards and attaching to their respective external fixation rings, but they are not tensioned.
- Rationale: These stirrup wires act as "guide wires" for distraction. By being placed adjacent to the region of distraction and not tensioned, they ensure that the distraction forces applied by the TSF struts are concentrated across the intended Charcot joints, facilitating accurate and precise realignment.

6. Taylor Spatial Frame (TSF) Assembly
- Strut Placement: Once all rings and wires are secured, attach the six TSF struts between the distal tibial fixation block and the forefoot ring. Ensure proper orientation as per the frame design.
- Build-out: In some cases, a build-out (e.g., a two-hole plate) may be required off the distal foot ring to allow for adequate soft tissue clearance, especially in swollen feet.

7. Fluoroscopic Documentation for Computer Planning
- Reference Ring: Confirm which ring (distal tibial or forefoot) will serve as the reference for computer planning. We usually choose a distal reference for foot corrections.
- Orthogonal Views: Obtain orthogonal AP and lateral fluoroscopic images of the reference ring. These images are crucial for providing the mounting parameters needed for the TSF computer software.
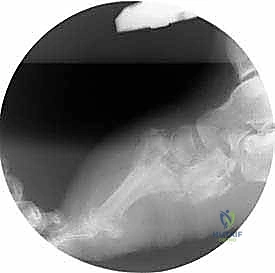
- Final Radiographs: Obtain final AP and lateral radiographs of the foot, including the distal tibia, to document the immediate postoperative alignment and frame construct.
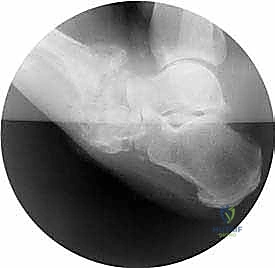
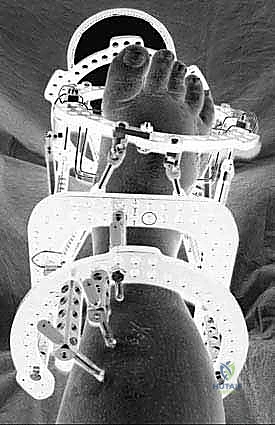
* Notice the midfoot adduction that is still present, which will be corrected gradually.

* Observe the initial plantarflexion of the forefoot. The stirrup wires are visible, strategically placed near the midfoot distraction zone.
* Software Input: The mounting parameters from these images, along with the desired correction, are entered into the TSF computer software to generate the patient's daily strut adjustment schedule.
8. Postoperative Management (Stage 1)
- Initial Care: The patient will be discharged with instructions for daily pin site care and education on performing the strut adjustments as per the computer-generated schedule.
- Follow-up: We schedule weekly or biweekly clinical and radiographic follow-up appointments to monitor correction progress, assess pin sites, and address any potential issues.
- Duration: Gradual distraction for realignment typically takes approximately 1 to 2 months, depending on the severity of the deformity and the rate of correction.
Stage 2: Frame Removal and Minimally Invasive Arthrodesis
Fellows, after 1-2 months of gradual distraction, the foot anatomy should be significantly realigned. We'll now proceed with the second stage: frame removal and definitive minimally invasive arthrodesis. This simultaneous approach allows us to maintain the corrected position while achieving stable internal fixation.
Step-by-Step Intraoperative Execution (Stage 2)
1. Confirm Correction and Pre-position Guidewires
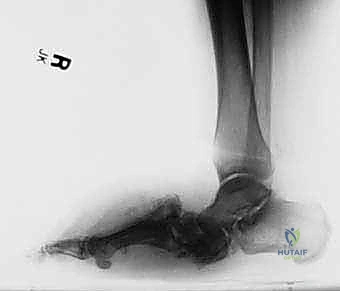
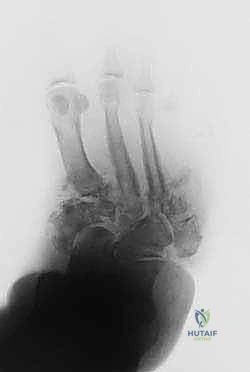
- Fluoroscopic Confirmation: Before any frame removal, obtain repeat AP and lateral fluoroscopic images to confirm that the desired anatomical realignment has been achieved.
- Guidewire Placement (Crucial Step): This is a critical sequence. To maintain the corrected foot position during frame removal, we will insert the guidewires for our intramedullary screws before removing the external fixator.
- Approach: Under fluoroscopic guidance, make small stab incisions (approximately 5mm) on the plantar aspect of the metatarsal heads. You may need to dorsiflex the metatarsophalangeal (MTP) joint to facilitate access and avoid the plantar plate.
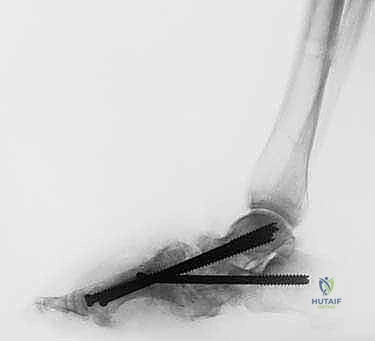
- Medial Column (1st Metatarsal): Insert a 1.8-mm guidewire percutaneously through the plantar skin incision into the head of the first metatarsal. Advance it intramedullary, across the corrected Charcot joint (e.g., first tarsometatarsal joint), through the cuneiform, navicular, and into the talus or calcaneus. Aim for a trajectory that provides maximal bone purchase and crosses the involved midfoot joints.
- Lateral Column (4th or 5th Metatarsal): Similarly, insert a 1.8-mm guidewire into the head of the fourth or fifth metatarsal. Advance it intramedullary, across the corrected Charcot joint, through the cuboid, and into the calcaneus.
- Central Column (2nd Metatarsal): Insert a 1.8-mm guidewire into the head of the second metatarsal, following an intramedullary path into the hindfoot. This screw will provide central stability.
- Surgical Warning:
> CRITICAL PEARL: When inserting guidewires from the plantar aspect, meticulously use a blunt trocar or hemostat to protect the plantar neurovascular bundles. Ensure the guidewire stays central within the metatarsal shaft and does not exit the cortex prematurely. Confirm trajectory with orthogonal fluoroscopic views at every stage of advancement. - Surgical Warning:
> CRITICAL PITFALL: The goal is to span the entire length of the metatarsals to the calcaneus and talus, protecting the adjacent Lisfranc joint from future Charcot events by providing rigid internal stability across it.
- Surgical Warning:
2. Frame Removal and Reprepping
- Removal: Once all guidewires are securely in place, the external fixator is carefully disassembled and removed.
- Reprep: The foot is then thoroughly reprepped and redraped, as the field is now considered "clean"
Additional Intraoperative Imaging & Surgical Steps
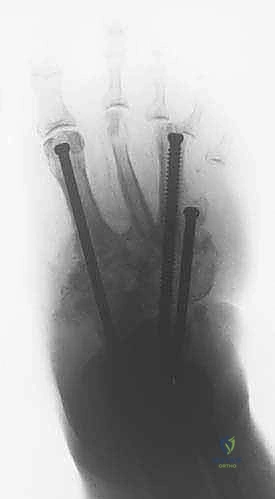

REFERENCES
- Most notably, no deep infection, no screw failure, and no recurrent ulcerations occurred and no amputations were necessary during the past 5 years.
Gradual Charcot foot correction with the TSF plus minimally invasive arthrodesis has constituted a safe and effective treatment.
Our results are promising. The advantages of our method when compared with the resection and plating method reported by Schon 4 or the resection and external fixation method reported by Cooper 1 are preservation of foot length (no bone resection), accurate anatomic realignment of soft
Cooper PS. Application of external fixators for management of Charcot deformities of the foot and ankle. Foot Ankle Clin 2002;7:207–254.
-
Jolly GP, Zgonis T, Polyzois V. External fixation in the management of Charcot neuroarthropathy. Clin Podiatr Med Surg 2003; 20:741–756.
-
Paley D. Principles of Deformity Correction. Rev ed. Berlin: SpringerVerlag, 2005.
-
Schon LC, Easley ME, Weinfeld SB. Charcot neuroarthropathy of the foot and ankle. Clin Orthop Relat Res 1998;349:116–131.
-
Trepman E, Nihal A, Pinzur MS:.Current topics review: Charcot neuroarthropathy of the foot and ankle. Foot Ankle Int 2003;6:46–63.
-
Wang JC, Le AW, Tsukuda RK. A new technique for Charcot’s foot reconstruction. J Am Podiatr Med Assoc 2002;92:429–436.