Surgical Stabilization of Nonplantigrade Midfoot Charcot Arthropathy: An Intraoperative Masterclass
Key Takeaway
This masterclass guides fellows through surgical stabilization of nonplantigrade midfoot Charcot arthropathy. We'll meticulously cover comprehensive anatomy, detailed preoperative planning, and granular intraoperative execution, including Achilles lengthening, wedge osteotomy, and precise internal fixation. Expect extensive pearls on avoiding pitfalls, managing complications, and optimizing postoperative rehabilitation for superior patient outcomes.
Comprehensive Introduction and Patho-Epidemiology
The Scope of the Pathology
Welcome to the operating theater. Today, we are undertaking a complex, demanding, yet profoundly impactful surgical endeavor: the stabilization and reconstruction of nonplantigrade midfoot Charcot arthropathy. This pathology represents one of the most formidable challenges in orthopedic foot and ankle surgery. We are not merely executing an osteosynthesis or an arthrodesis; we are attempting to restore structural integrity to a profoundly compromised biomechanical envelope. Our ultimate objective is the prevention of devastating ulceration, the eradication of osteomyelitis risk, the salvage of the lower extremity, and the restoration of a functional, plantigrade foot for our diabetic patients.

Charcot foot arthropathy is an aggressive, destructive, and non-infectious inflammatory process that primarily targets the osseous and ligamentous architectures of the foot and ankle. It manifests predominantly in patients afflicted with long-standing diabetes mellitus and profound peripheral neuropathy (PN). The pathogenesis is a multifactorial cascade resulting in the catastrophic loss of normal pedal architecture. As the medial and lateral columns collapse, weight-bearing forces are abnormally transferred through less durable plantar soft tissues, particularly at the apex of the midfoot deformity. This aberrant biomechanical loading sets the stage for inevitable soft tissue failure, deep ulceration, contiguous osteomyelitis, systemic sepsis, and, if left unchecked, major lower extremity amputation.
Pathogenesis: Neurotraumatic and Neurovascular Paradigms
To effectively reconstruct the Charcot foot, the surgeon must first understand the underlying mechanisms driving the destruction. The etiology is classically bifurcated into two primary theories, though contemporary understanding acknowledges a synergistic combination of both.
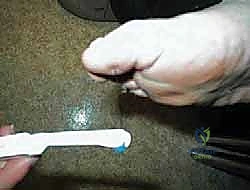
The Neurotraumatic Theory posits that patients with advanced peripheral neuropathy suffer a critical loss of protective sensation. This is clinically quantifiable by an inability to detect a 10-gram Semmes-Weinstein monofilament. Without nociceptive feedback, these patients sustain repetitive microtrauma and mechanical stress fractures during normal ambulation. Because they experience no pain, they continue to bear weight on the compromised extremity, driving a cycle of progressive fracture, joint dislocation, and a hyperemic response that mimics an aggressive hypertrophic nonunion.
The Neurovascular Theory introduces the role of autonomic neuropathy. A vasomotor dysfunction leads to the loss of sympathetic tone in the lower extremity vasculature, resulting in high-flow arteriovenous shunting. This chronic hyperemia washes out bone mineral density, causing localized osteopenia. The weakened, osteopenic bone is subsequently highly susceptible to fracture and collapse under normal physiological loads.
Furthermore, we must account for the accompanying motor neuropathies. Motor neuropathy preferentially affects the intrinsic muscles of the foot and the smaller anterior compartment muscles of the leg. This creates a profound dynamic imbalance—typically an overpowering of the Achilles tendon (equinus contracture)—which pathologically increases forefoot and midfoot pressures during the terminal stance phase of gait, directly contributing to midfoot breakdown. Histochemically, the acute Charcot event is driven by a massive localized inflammatory cascade. Pro-inflammatory cytokines, particularly TNF-alpha and Interleukin-1, upregulate the RANKL pathway, leading to aggressive osteoclastic bone resorption. Intraoperatively, this manifests as a destructive, hypervascular gray tissue that grossly resembles the acute pannus seen in rheumatoid arthritis.

Clinical Presentation and the Critical Differential Diagnosis
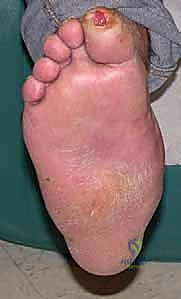
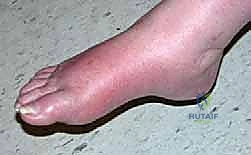
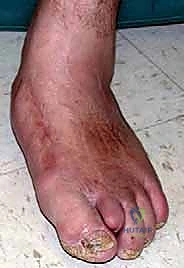
Patients presenting with acute Charcot arthropathy classically exhibit a grossly edematous, erythematous, and calorific foot. While classical literature often describes this as occurring "without a history of trauma," meticulous history-taking reveals that over half of these patients recall a specific, albeit trivial, mechanical event. They are typically in their fifth or sixth decade of life, possess a high body mass index, and suffer from poorly controlled diabetes.
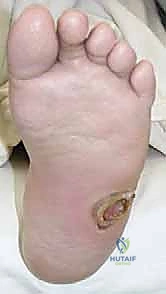
The absolute most critical differential diagnosis to establish upon presentation is distinguishing acute Charcot arthropathy from a deep diabetic foot abscess or acute osteomyelitis. Misdiagnosing an infection as Charcot can lead to catastrophic sepsis, while misdiagnosing Charcot as infection often leads to unnecessary surgical debridements that further destabilize the foot.
Clinical acumen is paramount here. Patients harboring a deep infection typically exhibit systemic signs of illness: malaise, sudden unexplained spikes in blood glucose levels, or a sudden increase in insulin requirements. They frequently have an identifiable portal of entry, such as an ingrown toenail, a web-space fissure, or a plantar puncture. Crucially, the erythema and edema associated with a deep infection will not significantly dissipate with strictly enforced limb elevation.
Conversely, the acute Charcot patient is generally systemically well. Their glycemic control remains at their baseline, and there is an absence of purulent drainage or an open wound (in the early stages). The hallmark clinical test is the elevation test: when the Charcot limb is elevated above the level of the heart for 10 to 15 minutes, the profound erythema and rubor will significantly lessen or resolve entirely, confirming its vasomotor and inflammatory—rather than infectious—etiology. Furthermore, surgeons must remember that diabetic patients are frequently immunocompromised hosts; a normal serum white blood cell (WBC) count does not reliably exclude a deep infection.
Eichenholtz Staging System
Weight-bearing biplanar radiographs remain the cornerstone of initial evaluation and staging. The Eichenholtz classification, while historical, remains a highly functional framework for guiding treatment:
* Stage I (Developmental/Acute): Characterized by acute inflammation. Radiographs may initially appear radiographically normal or show subtle periarticular fragmentation, subluxation, and debris formation. The foot is clinically hot, red, and swollen.
* Stage II (Coalescence): The acute inflammatory phase subsides. Radiographs demonstrate the absorption of fine osseous debris, the fusion of larger fragments, and early sclerosis. This is the stage where the classic structural deformities (e.g., rocker-bottom foot) become rigidly apparent.
* Stage III (Consolidation/Reconstruction): The destructive process is completely "burned out." The foot assumes its final, often severely deformed, architecture with dense hypertrophic reactive bone formation, rounding of bone ends, and rigid ankylosis.
Detailed Surgical Anatomy and Biomechanics
Osteology and Columnar Biomechanics of the Midfoot
To successfully reconstruct the Charcot midfoot, the surgeon must possess an intimate understanding of its complex, interlocking osteology. The midfoot acts as the crucial transitional zone between the mobile forefoot and the rigid hindfoot. It is conceptually divided into three biomechanical columns:
1. The Medial Column: Comprising the talus, navicular, medial cuneiform, and first metatarsal. This is the primary load-bearing column during the propulsive phase of gait. In Charcot arthropathy, failure often occurs at the talonavicular or naviculocuneiform joints, leading to dorsal subluxation of the midfoot and a profound loss of the medial longitudinal arch.
2. The Middle Column: Comprising the intermediate and lateral cuneiforms and the second and third metatarsals. The base of the second metatarsal is recessed proximally into the cuneiforms, acting as the "keystone" of the Lisfranc complex.
3. The Lateral Column: Comprising the calcaneus, cuboid, and the fourth and fifth metatarsals. This column is inherently more mobile to accommodate uneven terrain. Charcot collapse here often results in cuboid subluxation, turning the cuboid into a prominent plantar weight-bearing bony prominence that is highly susceptible to ulceration.
The Pathoanatomy of the Rocker-Bottom Deformity
The hallmark of midfoot Charcot is the "rocker-bottom" deformity. This occurs when the ligamentous constraints of the midfoot—specifically the plantar fascia, the spring ligament (plantar calcaneonavicular ligament), and the Lisfranc ligament complex—fail under the stress of neurotraumatic loading. As the arch collapses, the midfoot joints dislocate, typically with the forefoot abducting and dorsiflexing relative to the hindfoot. The apex of this collapse frequently becomes the cuboid or the medial cuneiform, which are driven plantarly to become the new, pathological weight-bearing surface.
Neurovascular Topography and Surgical Danger Zones
Meticulous dissection is required to navigate the neurovascular structures surrounding the midfoot, particularly given the compromised vascular status of the diabetic patient.
- Dorsal Approach Anatomy: The dorsalis pedis artery, a direct continuation of the anterior tibial artery, courses over the dorsal aspect of the navicular and middle cuneiform, typically residing between the extensor hallucis longus (EHL) and extensor digitorum longus (EDL) tendons. It is accompanied by the deep peroneal nerve, which provides critical motor innervation to the extensor digitorum brevis and sensory innervation to the first web space. The superficial peroneal nerve arborizes extensively across the subcutaneous tissues of the dorsal foot and is at high risk during initial skin incisions.
- Medial Approach Anatomy: The saphenous nerve and the greater saphenous vein course anterior to the medial malleolus and along the medial column. These must be identified and protected during medial utility incisions to prevent painful neuromas and venous congestion.
- Plantar Anatomy: While rarely approached directly due to the risk of painful scarring, the plantar aspect houses the posterior tibial neurovascular bundle, which bifurcates into the medial and lateral plantar arteries and nerves deep to the abductor hallucis muscle. During extensive plantarflexion osteotomies or plantar plating, great care must be taken not to tether or injure these structures.
Exhaustive Indications and Contraindications
Patient Selection and the Treatment Algorithm
The decision to proceed with surgical reconstruction in a Charcot patient is highly nuanced. Not every Charcot foot requires surgical intervention. The primary goal is a stable, plantigrade foot that is free of ulceration and capable of being shod in commercially available therapeutic footwear.
Patients who present with a clinically plantigrade foot, maintain a colinear lateral talar–first metatarsal axis (Meary's angle roughly 0 degrees) on weight-bearing radiographs, and possess no significant plantar bony prominences are excellent candidates for non-operative management.
Non-operative management is the gold standard for acute (Eichenholtz Stage I) Charcot. This typically involves immediate offloading utilizing a total-contact cast (TCC). The TCC is changed every 7 to 14 days to accommodate rapidly decreasing limb edema. Once clinical stability is achieved and limb volume plateaus (often taking 3 to 6 months), the patient is transitioned to a Charcot Restraint Orthotic Walker (CROW) or a pneumatic fracture boot, and ultimately into custom therapeutic footwear with rigid rocker-bottom soles and custom accommodative orthoses.
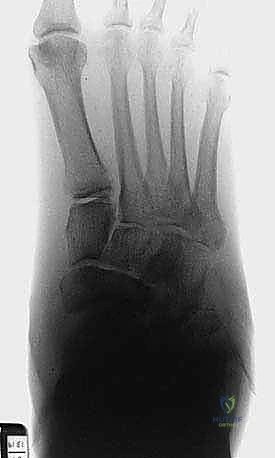
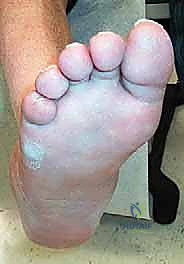
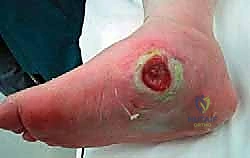
However, surgical correction is absolutely indicated for patients who fail conservative management. This includes patients who present with severe, nonplantigrade deformities that cannot be accommodated in custom footwear, or patients who develop recurrent, recalcitrant plantar ulcerations despite strict compliance with offloading and orthotics.
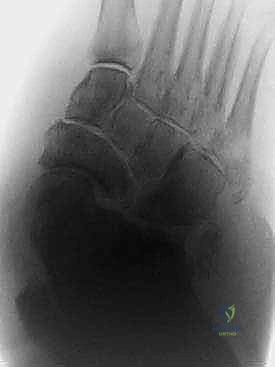
Stratifying the Surgical Host
Once surgery is indicated, the surgeon must rigidly categorize the patient into either a "good surgical host" or a "poor surgical host." This categorization dictates the entirely of the surgical approach and fixation strategy.
- The Good Surgical Host: These patients present with a rigid, nonplantigrade deformity but importantly have an intact soft tissue envelope. They have no open wounds over the apex of the deformity, no history of deep osteomyelitis in the surgical field, adequate vascular perfusion (palpable pulses, biphasic Doppler signals, or an Ankle-Brachial Index > 0.8), and reasonable bone stock as assessed radiographically. These patients are ideal candidates for single-stage internal fixation utilizing superconstruct principles.
- The Poor Surgical Host: These patients present with active or recently healed deep ulcerations, a history of contiguous osteomyelitis, severely compromised soft tissue envelopes, profound osteopenia, or significant medical comorbidities (e.g., end-stage renal disease). Internal fixation in this cohort carries an unacceptably high risk of catastrophic hardware infection and failure. These patients are definitively managed with external fixation, typically utilizing a multi-plane circular ring fixator (Ilizarov or Taylor Spatial Frame) to achieve stability and gradual deformity correction without introducing massive foreign bodies into a compromised bed.
| Indication for Surgery | Contraindication for Surgery (Internal Fixation) |
|---|---|
| Nonplantigrade foot unbraceable in custom orthotics | Active, deep soft tissue infection or osteomyelitis |
| Recurrent plantar ulceration despite strict TCC compliance | Severe peripheral arterial disease (ABI < 0.5, un-revascularizable) |
| Severe instability threatening imminent skin breakdown | Profound medical instability (e.g., recent myocardial infarction) |
| Disabling pain in a Stage III consolidated deformity | Non-ambulatory patient (wheelchair bound baseline) |
| Good host with adequate bone stock for internal fixation | Active, non-compliant patient with severe psychiatric illness |
Pre-Operative Planning, Templating, and Patient Positioning
Advanced Imaging and Superconstruct Templating
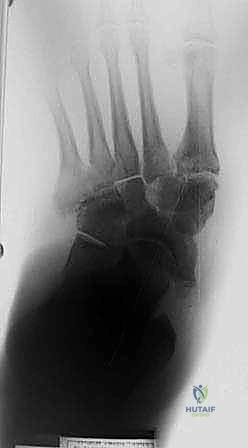
Preoperative planning is the most critical phase of Charcot reconstruction. Standard weight-bearing anteroposterior, lateral, and oblique radiographs are mandatory to assess the apex of the deformity, typically measuring Meary's angle, the calcaneal pitch, and the cuboid height.

Advanced imaging is highly recommended. A computed tomography (CT) scan with 3D reconstructions provides unparalleled visualization of the complex midfoot subluxations, areas of bony fragmentation, and the exact location of hypertrophic bone that will require resection. Magnetic Resonance Imaging (MRI) is utilized selectively, primarily when there is a high clinical suspicion of underlying osteomyelitis contiguous to a chronic ulceration.
Templating involves mapping out the planned osteotomies and hardware placement. Modern Charcot reconstruction relies heavily on the "Superconstruct" principles pioneered by Sammarco. These principles dictate that:
1. Fusion must extend beyond the zone of injury to include normal, healthy bone proximally and distally.
2. Bone resection should be utilized to shorten the limb and reduce tension on the compromised soft tissue envelope, rather than attempting to stretch contracted soft tissues to fit the bone.
3. The strongest possible hardware devices must be utilized, acknowledging that neuropathic bone will subject the hardware to immense, prolonged stress.
4. Hardware should be positioned to maximize its mechanical advantage (e.g., utilizing intramedullary beaming or plantar tension-band plating).
Operating Room Setup and Patient Positioning
For a standard midfoot reconstruction in a good surgical host, general endotracheal anesthesia is preferred to provide complete muscle relaxation, aiding in the reduction of severe deformities. Regional anesthesia (popliteal block) can be used as an adjunct for postoperative pain control, though its utility is debated in patients with profound baseline neuropathy.
The patient is positioned supine on a radiolucent operating table. Meticulous attention must be paid to padding all bony prominences (heels, sacrum, elbows) to prevent iatrogenic neuropathic ulcerations during the prolonged case. A bump is frequently placed under the ipsilateral hip to internally rotate the limb, bringing the medial column of the foot into a neutral, easily accessible position.
A proximal thigh tourniquet is applied to ensure a pristine, bloodless surgical field, which is critical for identifying delicate neurovascular structures and assessing the adequacy of bony debridement. The fluoroscopic C-arm is positioned on the contralateral side of the table, draped sterilely, and tested prior to incision to ensure unimpeded AP, lateral, and oblique views of the entire foot and ankle complex.
Step-by-Step Surgical Approach and Fixation Technique
Incision Planning and Soft Tissue Management
The surgical approach is dictated by the apex of the deformity. For a classic medial column collapse, a robust medial utility incision is utilized. This incision begins just distal to the medial malleolus, coursing longitudinally along the medial aspect of the talonavicular and naviculocuneiform joints, and extending to the diaphysis of the first metatarsal.
It is absolutely imperative to raise full-thickness fasciocutaneous flaps. The surgeon must dissect straight down to the osseous structures without undermining the subcutaneous tissues. Undermining in a diabetic patient destroys the fragile subdermal vascular plexus, guaranteeing catastrophic marginal skin necrosis and subsequent deep infection. The saphenous vein and nerve are carefully identified, mobilized dorsally or plantarly, and protected throughout the procedure.

For lateral column involvement, a secondary longitudinal incision is made over the lateral aspect of the cuboid and the base of the fourth and fifth metatarsals, taking care to protect the sural nerve and the peroneal tendons.
Joint Preparation and Deformity Correction
Once the osseous structures are exposed, the extent of the hypertrophic Charcot bone becomes apparent. A combination of osteotomes, rongeurs, and a high-speed burr is used to aggressively resect the pathological bone.
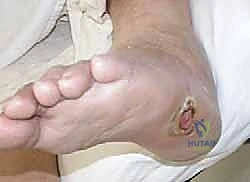
The goal is not merely to debride the joints, but to perform a biplanar, closing-wedge osteotomy at the apex of the deformity. This osteotomy serves two critical functions: it shortens the medial column to relieve tension on the medial soft tissues, and it allows for the plantarflexion of the first ray, effectively recreating the medial longitudinal arch.
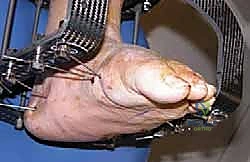
All articular cartilage must be meticulously removed down to bleeding subchondral bone. The subchondral plates are then aggressively "fish-scaled" or drilled with a 2.0mm bit to promote robust angiogenesis and osteogenesis across the planned fusion mass.
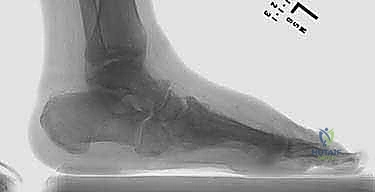
Executing the Superconstruct Fixation
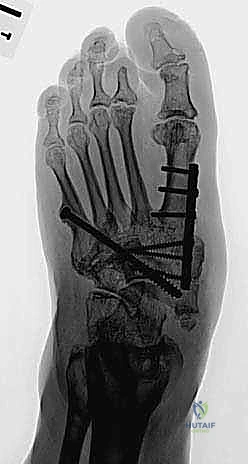
Once the deformity is reduced and provisionally held with heavy Kirschner wires, definitive fixation is applied. The current gold standard involves intramedullary "beaming" combined with robust plating.
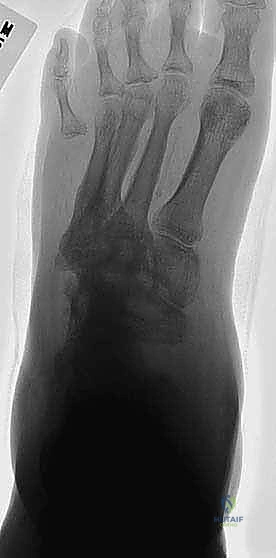
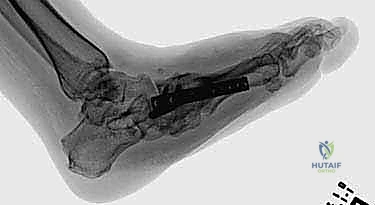
Intramedullary Beaming: A large-diameter (typically 6.5mm to 8.0mm), solid, fully threaded intramedullary screw is introduced through the head of the first metatarsal. It is driven proximally, crossing the cuneiforms and the navicular, and anchored deeply into the dense bone of the talar body. This "beam" acts as an internal load-sharing device, providing immense resistance to bending moments across the medial column. A similar, smaller beam (e.g., 4.5mm) can be utilized in the lateral column, driven from the base of the fourth or fifth metatarsal into the calcaneus.
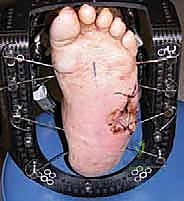
Plating Techniques: To supplement the intramedullary beams, a robust locking plate is applied. Ideally, if soft tissue permits, a plantar plate is utilized to act as a tension band, resisting the plantar-gaping forces of weight-bearing. However, a medial column locking plate is more commonly utilized due to easier surgical access. The plate must span from the talus to the distal diaphysis of the first metatarsal, utilizing multiple locking screws in each segment to prevent pullout in osteopenic bone.
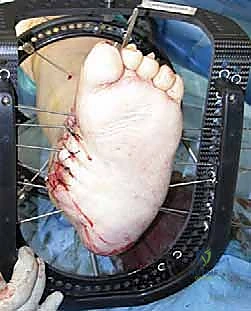
Bone grafting is frequently required to fill voids created by the deformity correction. Autograft (e.g., from the proximal tibia or iliac crest) is the biological gold standard, though cellular allografts and orthobiologics (such as Bone Morphogenetic Protein-2) are increasingly utilized to augment the fusion mass in these compromised hosts.
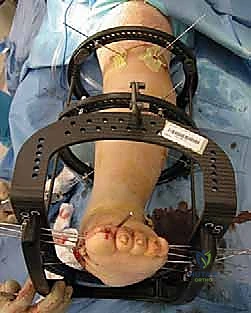
Following rigid fixation, the tourniquet is deflated, and meticulous hemostasis is achieved. A closed suction drain is frequently placed deep to the fascial layer. The soft tissues are closed in a layered, tension-free manner using non-absorbable sutures for the skin, left in place for a minimum of 3 to 4 weeks.
Complications, Incidence Rates, and Salvage Management
Navigating Surgical Pitfalls
Operating on the Charcot foot is fraught with potential complications. The surgeon must counsel the patient extensively preoperatively that the complication rate is exceptionally high, and the ultimate salvage procedure—a major lower extremity amputation—remains a distinct possibility even after a technically flawless reconstruction.
The most dreaded complication is deep surgical site infection (SSI), which occurs in up to 10-15% of cases. Given the diabetic host's impaired immune response and microvascular disease, an SSI rapidly progresses to osteomyelitis and hardware contamination.
Hardware failure is another frequent complication. Neuropathic bone is notoriously slow to heal, and the complete lack of protective sensation means the patient will inadvertently subject the hardware to massive, repetitive loads before solid osseous fusion is achieved. This leads to screw breakage, plate fracture, or hardware pullout, resulting in a loss of correction and recurrent deformity. Nonunion or delayed union is seen in roughly 20-30% of fusions, necessitating prolonged periods of non-weight-bearing.
Salvage Protocols
When complications arise, aggressive and immediate intervention is required. Superficial wound dehiscence can often be managed with local wound care and negative pressure wound therapy. However, deep infections require an immediate return to the operating room for radical irrigation, debridement, and typically, the removal of all internal hardware.
If hardware is removed due to infection or failure in the setting of a nonunion, the limb must be stabilized externally. The application of a multi-plane circular external fixator (Ilizarov frame) allows for rigid stabilization of the osseous segments while providing unrestricted access to the soft tissue envelope for wound care.
| Complication | Estimated Incidence | Salvage Management Strategy |
|---|---|---|
| Superficial Wound Dehiscence | 15 - 25% | Local wound care, strict offloading, Negative Pressure Wound Therapy (NPWT). |
| Deep Surgical Site Infection | 5 - 15% | Urgent surgical I&D, hardware removal, culture-directed IV antibiotics, transition to external fixation. |
| Hardware Failure / Breakage | 10 - 20% | If stable and plantigrade: observe. If unstable/loss of correction: revision ORIF vs. external fixation. |
| Aseptic Nonunion | 20 - 30% | Prolonged immobilization, bone stimulators. Revision surgery with autograft if symptomatic or unstable. |
| Recurrent Plantar Ulceration | 10 - 15% | Re-evaluate biomechanics. Modify custom footwear. Consider exostectomy of recurrent bony prominences. |
| Major Amputation (BKA/AKA) | 5 - 10% | Indicated for overwhelming, unsalvageable sepsis, massive tissue loss, or chronic, painful, non-reconstructable limbs. |
Phased Post-Operative Rehabilitation Protocols
Phase I: Maximum Protection and Osseous Consolidation (Weeks 0-12)
The postoperative rehabilitation following a midfoot Charcot reconstruction is exceptionally prolonged and demands absolute patient compliance. Immediately postoperatively, the patient is placed in a well-padded, short-
Clinical & Radiographic Imaging Archive