Orthopedic Prometric MCQs - Chapter 3 Part 39

Orthopedic Prometric MCQs - Chapter 3 Part 39
Comprehensive 100-Question Exam
00:00
Start Quiz
Question 1
Following two previous shoulder stabilization procedures for recurrent dislocations, a 45-year-old man complains of pain and limited motion. Examination reveals increased passive external rotation and an inability to lift the back of the hand away from his back. Which of the following muscles is injured:
Explanation
Question 2
Which of the following is not a cause of failure following arthroscopic subacromial decompression:
Explanation
Question 3
Which of the following structures is involved in the â essential lesionâ of a stiff shoulder:
Explanation
Question 4
A 35-year-old businessman sustains a type III acromioclavicular (AC ) separation of his dominant shoulder. Preferred treatment should be:
Explanation
Question 5
Which of the following muscles is most responsible for deceleration of the arm during pitching:
Explanation
Question 6
Which of the following conditions most often accompanies a dislocation of the longhead of the biceps tendon?
Explanation
Question 7
Which of the following combinations correctly describes the contributions of the acromioclavicular ligaments and coracoclavicular ligaments in stabilizing the acromioclavicular joint:
Explanation
Question 8
Which of the following statements is true concerning the bands of the anterior cruciate ligament:
Explanation
Question 9
Which of the following statements is true concerning the bands of the posterior cruciate ligament:
Explanation
Question 10
The most sensitive test for posterior cruciate ligament injury is the:
Explanation
Question 11
A 30-year-old male avid runner presents with a 2-week history of right lateral knee pain. He denies any history of trauma, swelling, or mechanical symptoms. The pain only occurs with running and is relieved by cessation of activity. Physical examination does not demonstrate any effusion, and there is no pathologic laxity of the collateral or cruciate ligaments. There is tenderness to palpation along the lateral aspect of the knee that is most severe over the lateral epicondyle, particularly with the knee flexed to 30°. The next most appropriate course of action is:
Explanation
Question 12
This radiograph shows a diaphysis of a 21-year-old female collegiate soccer player. She reports pain in the midshaft of her tibia for 7 months. She has been previously treated with cessation of soccer, 8 weeks in a short leg cast, and 3 months of treatment with an ultrasonic bone stimulator. Recommended treatment at this time should include:
Explanation
 healing. Since this patient has failed nonoperative treatment, insertion of a reamed intramedullary nail would offer her the best chance of healing and earlier return to activity.
healing. Since this patient has failed nonoperative treatment, insertion of a reamed intramedullary nail would offer her the best chance of healing and earlier return to activity.
Question 13
A "stinger" (transient weakness of the upper extremity commonly seen after a blow to the head and shoulder in football) most commonly affects the:
Explanation
Question 14
A 16-year-old male high school football player was making a tackle when he felt sudden pain in his right long finger. He has swelling and tenderness along the volar aspect of the injured digit. He is unable to actively flex the distal interphalangeal joint of the injured digit. Radiographs are negative for fracture. Recommended treatment should include:
Explanation
Question 15
C atastrophic cervical spine injuries occurring during contact sports are most commonly a result of:
Explanation
Question 16
A collegiate level sprinter sustains an acute nondisplaced fracture at the proximal metaphyseal-diaphyseal junction of the fifth metatarsal. Appropriate treatment for early return to play includes:
Explanation
Question 17
This is the radiograph of a right hand dominant 15-year-old baseball player who felt a pop when swinging a bat. There is pain in the upper portion of the first rib. Recommended treatment should consist of:
Explanation
Question 18
A 10-year-old female gymnast twists her knee on her dismount from the balance beam. She hears a pop and has immediate swelling. She is unable to continue with activity. Physical examination reveals a positive Lachman test and positive pivot shift. She has no joint line tenderness. Radiographs are normal. After an initial period of ice and range of motion exercises, recommended treatment should include:
Explanation
Question 19
The most common location of osteochondritis dissecans in the knee is the:
Explanation
Question 20
A 15-year-old female volleyball player twisted her knee while planting her foot. She states she felt her knee give out. She had immediate swelling and was unable to continue participation. She denies hearing a pop. Physical examination reveals a large effusion with a range of motion from full extension to 80° flexion. She has marked tenderness along the medial retinaculum of her knee. She has no joint line tenderness. There is no pathologic laxity involving the collateral or cruciate ligaments. The most likely diagnosis is:
Explanation
Question 21
A 55-year-old man presents with anterior shoulder pain and increased passive external rotation after a heavy fall. Examination reveals a positive belly-press test and an inability to maintain internal rotation against resistance. Which structure is most likely injured?
Explanation
Question 22
In a patient diagnosed with idiopathic adhesive capsulitis, contracture of which of the following specific structures is primarily responsible for the severe restriction of external rotation when the arm is adducted at the side?
Explanation
Question 23
During shoulder arthroscopy for a suspected SLAP lesion, the surgeon notes peeling back of the superior labrum when the arm is placed in abduction and external rotation. This "peel-back" mechanism is most commonly associated with which type of SLAP tear?
Explanation
Question 24
In the context of severe proximal humerus fractures, which of the following vessels provides the dominant blood supply to the humeral head, thereby placing it at high risk of avascular necrosis if disrupted?
Explanation
Question 25
A 25-year-old cyclist falls directly onto his shoulder point. Radiographs reveal a 150% superior displacement of the distal clavicle relative to the acromion, with marked widening of the coracoclavicular space. What is the most appropriate classification and typical initial management recommendation?
Explanation
Question 26
A 19-year-old football player sustains a direct compressive blow to the medial clavicle. He presents with shortness of breath, dysphagia, and a palpable defect at the medial clavicle. Which imaging modality is considered the gold standard for accurately evaluating this injury?
Explanation
Question 27
A 32-year-old elite volleyball player presents with isolated weakness in external rotation of the shoulder. Examination reveals atrophy of the infraspinatus fossa, but supraspinatus strength and bulk are perfectly normal. Where is the most likely site of nerve entrapment?
Explanation
Question 28
A 28-year-old pitcher complains of poorly localized posterolateral shoulder pain and paresthesias. Angiography reveals dynamic occlusion of the posterior circumflex humeral artery with the arm in extreme abduction and external rotation. Which nerve is most likely concurrently compressed in this specific anatomical syndrome?
Explanation
Question 29
A 22-year-old rugby player with recurrent anterior shoulder instability is found to have 25% anterior glenoid bone loss. An open Latarjet procedure is planned. During the surgical approach to the anterior glenoid, which muscle's tendon is classically split horizontally?
Explanation
Question 30
A professional baseball pitcher demonstrates a 25-degree loss of internal rotation in his throwing shoulder compared to his contralateral shoulder, but his total arc of motion (internal + external rotation) remains completely symmetric. What is the most appropriate initial management?
Explanation
Question 31
A 45-year-old man feels a sudden pop in his anterior elbow while lifting heavy machinery. He exhibits profound weakness in forearm supination and a positive Hook test. If the surgeon utilizes a single-incision anterior approach for distal biceps repair, which nerve is at greatest risk of iatrogenic injury from lateral retraction?
Explanation
Question 32
A 50-year-old woman presents with numbness in her ring and small fingers. Examination reveals a positive Froment sign when asked to pinch a piece of paper. Which of the following muscles is actively compensating to cause the typical interphalangeal flexion seen in a positive Froment sign?
Explanation
Question 33
Which of the following specific combinations of injuries definitively constitutes the "terrible triad" of the elbow?
Explanation
Question 34
A 35-year-old man complains of his elbow "clicking" and giving way when pushing himself up from a chair. Examination reveals a positive lateral pivot-shift test of the elbow. Which ligament is primarily incompetent in this condition?
Explanation
Question 35
A 42-year-old carpenter presents with chronic medial elbow pain that drastically worsens with resisted wrist flexion and forearm pronation. If non-operative management fails and surgical debridement is required, which tendinous structure is the primary anatomical site of pathology?
Explanation
Question 36
A 22-year-old professional baseball pitcher presents with posterior shoulder pain during the late cocking phase of throwing. Examination reveals a 20-degree loss of internal rotation compared to the contralateral side. What is the most likely pathophysiology of his condition?
Explanation
Question 37
A 30-year-old weightlifter presents with vague posterior shoulder pain and paresthesias over the lateral deltoid. MRI demonstrates isolated fatty infiltration and atrophy of the teres minor muscle. The affected nerve is compressed in a space defined by which of the following boundaries?
Explanation
Question 38
A 32-year-old man presents with anterior shoulder pain and a sensation of giving way after a traumatic dislocation. MRI arthrogram reveals a J-sign with extravasation of contrast into the axillary pouch. Which of the following best describes this lesion?
Explanation
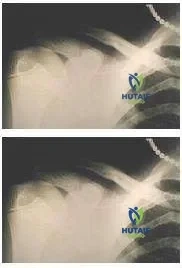
Question 39
A 25-year-old overhead athlete presents with deep shoulder pain and a positive O'Brien test. An MRI is obtained.
What is the most appropriate management for an isolated Type II SLAP tear in a young, high-level throwing athlete who has failed nonoperative treatment?

Explanation
Question 40
In the Latarjet procedure for anterior shoulder instability, the transferred coracoid process provides stability through a 'sling effect'. Which of the following structures is responsible for this dynamic sling effect?
Explanation
Question 41
A 35-year-old volleyball player has persistent shoulder weakness. MRI reveals a paralabral cyst at the spinoglenoid notch compressing a nerve. Which of the following clinical findings is expected?
Explanation
Question 42
A 50-year-old construction worker presents with weakness in internal rotation and a positive belly-press test following a lifting injury 8 months ago. MRI shows a massive, retracted, irreparable tear of the subscapularis with severe fatty infiltration. Which tendon transfer is most appropriate?
Explanation
Question 43
A 60-year-old man complains of profound weakness in shoulder elevation and external rotation. Imaging reveals an irreparable massive tear of the supraspinatus and infraspinatus with an intact subscapularis. There is no significant glenohumeral arthritis. Which of the following tendon transfers is best indicated?
Explanation
Question 44
According to the Rockwood classification of acromioclavicular (AC) joint injuries, what defines a Type V injury?
Explanation
Question 45
During anterior portal placement in shoulder arthroscopy, the musculocutaneous nerve is at risk if instruments are directed too far medially and inferiorly. The safe zone is determined by the nerve's entry into the conjoined tendon, which is typically located how far distal to the tip of the coracoid process?
Explanation
Question 46
A 28-year-old bodybuilder feels a sudden pop in his anterior chest while performing a bench press. Examination reveals loss of the anterior axillary fold and weakness in shoulder adduction and internal rotation. What is the most common anatomical site of this rupture?
Explanation
Question 47
In the pathogenesis of primary adhesive capsulitis, synovial inflammation progresses to capsular fibrosis. Which of the following cytokines is considered the primary driver of this fibrotic process?
Explanation
Question 48
During arthroscopic evaluation of a stiff shoulder, a key anatomic structure is targeted for release.
Which structure forms the roof of the rotator interval and is typically contracted in adhesive capsulitis, limiting external rotation in adduction?

Explanation
Question 49
A 45-year-old man experiences a seizure and subsequently presents with his shoulder locked in internal rotation. Radiographs demonstrate a 'lightbulb' sign on the AP view. What is the most likely associated osseous defect?
Explanation
Question 50
A 13-year-old baseball pitcher presents with vague proximal arm pain during throwing. Radiographs reveal widening and lateral fragmentation of the proximal humeral physis. What is the most appropriate initial management?
Explanation
Question 51
Which of the following physical examination tests is most specific for diagnosing a tear involving the upper border of the subscapularis tendon?
Explanation
Question 52
A 21-year-old gymnast presents with painless winging of the scapula after a neck injury. Examination shows the vertebral border of the scapula translated laterally and superiorly. Which nerve is most likely injured?
Explanation
Question 53
A 35-year-old male presents with acute, severe, unrelenting unilateral shoulder pain lasting several weeks, followed by patchy weakness in his periscapular muscles. MRI of the shoulder is unremarkable. What is the most likely diagnosis?
Explanation
Question 54
In the evaluation of recurrent anterior glenohumeral instability, critical glenoid bone loss often dictates the need for a bony augmentation procedure (e.g., Latarjet) rather than an isolated soft-tissue Bankart repair. The universally accepted threshold for 'critical' bone loss is greater than:
Explanation
Question 55
The long head of the biceps tendon is stabilized at the entrance to the bicipital groove by the biceps reflection pulley. Which of the following capsuloligamentous structures are the primary components of this pulley system?
Explanation
Question 56
A 45-year-old manual laborer presents with persistent anterior shoulder pain. MRI confirms a Type II SLAP lesion. What is the most appropriate surgical management for this patient considering his age and occupation?
Explanation
Question 57
A 22-year-old collegiate baseball pitcher reports posterior shoulder pain during the late cocking phase of throwing. The 'internal impingement' test is positive. What is the primary pathophysiological mechanism of this condition?
Explanation
Question 58
A patient undergoes a Latarjet procedure for recurrent anterior shoulder instability. Postoperatively, he presents with profound weakness in elbow flexion and forearm supination, along with numbness over the lateral aspect of the forearm. Which structure was most likely injured during the procedure?
Explanation
Question 59
A 23-year-old rugby player has recurrent anterior shoulder dislocations. Advanced imaging reveals 12% anterior glenoid bone loss and a Hill-Sachs lesion that is determined to be 'off-track'. What is the most appropriate surgical intervention?
Explanation
Question 60
A 28-year-old elite volleyball player presents with isolated weakness in shoulder external rotation. MRI reveals a paralabral cyst causing nerve compression. Where is the cyst most likely located?
Explanation
Question 61
A 35-year-old man presents with poorly localized posterior shoulder pain and numbness over the lateral deltoid. MRI shows isolated atrophy of the teres minor. Which of the following defines the superior border of the anatomical space involved in this syndrome?
Explanation
Question 62
During a physical examination for a suspected rotator cuff tear, the examiner places the patient's palm on their contralateral shoulder and asks the patient to resist an anteriorly directed force applied to the hand. What is this test, and which specific muscle portion does it evaluate?
Explanation
Question 63
A 65-year-old active man presents with severe shoulder pain and stiffness. Radiographs demonstrate advanced glenohumeral osteoarthritis. Physical exam and MRI confirm an intact and fully functional rotator cuff. What is the most appropriate surgical option?
Explanation
Question 64
A 30-year-old bodybuilder feels a sudden 'pop' in his chest while performing a heavy bench press. Examination reveals loss of the anterior axillary fold contour and weakness in internal rotation. Which anatomical structure is most commonly ruptured in this scenario?
Explanation
Question 65
Which of the following is considered the primary pathological change occurring during the 'freezing' stage of idiopathic adhesive capsulitis?
Explanation
Question 66
A 25-year-old cyclist falls directly onto his shoulder. Radiographs show a 100% superior displacement of the distal clavicle relative to the acromion. The coracoclavicular distance is increased by 50% compared to the contralateral side. What is the generally accepted initial management?
Explanation
Question 67
Following an extensive axillary lymph node dissection, a patient presents with medial winging of the scapula, which is accentuated when the patient pushes against a wall. Which muscle and corresponding nerve have been injured?
Explanation
Question 68
An 18-year-old is involved in a high-speed motor vehicle accident and presents with severe chest pain, dyspnea, and dysphagia. Exam reveals a palpable defect at the medial end of the right clavicle. What is the best initial diagnostic imaging and definitive treatment if closed reduction fails?
Explanation
Question 69
A 72-year-old patient presents with a massive, irreparable rotator cuff tear and pseudoparalysis of the shoulder. Radiographs demonstrate an acromiohumeral distance of 2 mm and early 'acetabularization' of the acromion without glenohumeral arthritis. What is the Hamada classification and optimal treatment?
Explanation
Question 70
A 40-year-old man falls on an outstretched hand, sustaining a 'terrible triad' injury of the elbow. Which of the following describes the recommended sequence of surgical reconstruction to restore stability?
Explanation
Question 71
A 21-year-old collegiate baseball pitcher complains of posteromedial elbow pain occurring primarily during the deceleration phase of throwing. Examination reveals a 15-degree flexion contracture and sharp pain with forced terminal extension. What is the most likely diagnosis?
Explanation
Question 72
A 13-year-old baseball pitcher presents with progressive shoulder pain during throwing. Radiographs show widening and sclerosis of the proximal humeral physis compared to the contralateral side. What is the most appropriate initial treatment?
Explanation
Question 73
What is the most common cause of significant, permanent loss of external rotation following an open anterior shoulder stabilization procedure (such as a Putti-Platt or standard open Bankart)?
Explanation
Question 74
A 22-year-old gymnast complains of deep, poorly localized shoulder pain during overhead routines. An MR arthrogram demonstrates a superior labral tear that propagates into the biceps anchor, causing instability of the biceps-labral complex. Based on the Snyder classification, what type of SLAP lesion is this?
Explanation
Question 75
A professional tennis player presents with vague shoulder aching. Physical examination demonstrates 20 degrees of internal rotation and 110 degrees of external rotation in 90 degrees of abduction. Which anatomical structure is primarily contracted, causing this Glenohumeral Internal Rotation Deficit (GIRD)?
Explanation
Question 76
A 55-year-old man presents with severe shoulder pain and restricted external rotation 15 years after an open anterior shoulder stabilization (Putti-Platt procedure). Radiographs reveal severe glenohumeral osteoarthritis. What is the primary pathophysiological mechanism leading to this complication?
Explanation
Question 77
A 45-year-old woman with type 1 diabetes presents with progressive, painful restriction of both active and passive shoulder motion. During the early 'freezing' phase of this condition, histological analysis of the joint capsule would most likely demonstrate:
Explanation
Question 78
A 40-year-old weightlifter presents with acute weakness in internal rotation and a positive bear-hug test after a heavy bench press. MRI confirms an isolated full-thickness tear of the subscapularis tendon. What associated structural pathology is most critical to evaluate and address during surgical repair?
Explanation
Question 79
A 22-year-old collegiate baseball pitcher complains of posterior shoulder pain during the late cocking phase of throwing. Examination shows a loss of 25 degrees of internal rotation compared to the contralateral side, and pain is provoked with the shoulder abducted and externally rotated. What is the most likely diagnosis?
Explanation
Question 80
A 24-year-old athlete with recurrent anterior shoulder instability undergoes preoperative evaluation.
Imaging reveals an anterior glenoid bone loss of approximately 30%. Which of the following is the most appropriate definitive management?
Explanation
Question 81
A 28-year-old volleyball player presents with insidious onset of posterior shoulder pain and isolated weakness in external rotation. MRI reveals a paralabral cyst in the spinoglenoid notch. Which muscle is primarily affected by this cyst?
Explanation
Question 82
A 65-year-old man presents with chronic shoulder pain, significant loss of active elevation (pseudoparalysis), and superior migration of the humeral head on radiographs. If an MRI confirms massive, irreducible tears of the supraspinatus and infraspinatus with grade 4 fatty infiltration, what is the best surgical option to restore function?
Explanation
Question 83
A 35-year-old man arrives at the emergency department with a locked shoulder after suffering a grand mal seizure.
He holds his arm in internal rotation and cannot externally rotate. Which of the following osseous lesions is most likely to be present?

Explanation
Question 84
A 55-year-old laborer undergoes a massive, irreparable rotator cuff repair using a latissimus dorsi tendon transfer. For this transfer to be biomechanically effective and successful, which of the following prerequisites MUST be met?
Explanation
Question 85
During a routine shoulder arthroscopy, the surgeon establishes the standard posterior portal approximately 2 cm inferior and 1 cm medial to the posterolateral corner of the acromion. If this portal is placed too inferiorly, which nerve is at greatest risk of injury?
Explanation
Question 86
A 60-year-old female undergoes arthroscopic release for recalcitrant adhesive capsulitis. Which anatomic structure must be released specifically to reliably restore external rotation with the arm at the side?
Explanation
Question 87
A 30-year-old male sustains an acute, high-energy acromioclavicular joint separation. Radiographs demonstrate >100% superior displacement of the clavicle relative to the acromion, with significant posterior displacement into the trapezius fascia. What is the correct classification of this injury?
Explanation
Question 88
A 14-year-old elite baseball pitcher presents with generalized shoulder pain and declining throwing velocity. Radiographs reveal widening and irregularity of the proximal humeral physis. What is the most appropriate initial management?
Explanation
Question 89
During an open anterior shoulder stabilization, a retractor is placed medially over the anterior aspect of the glenoid neck and conjoint tendon. The patient develops postoperative numbness over the lateral forearm and weakness in elbow flexion. Which nerve was most likely injured?
Explanation
Question 90
A 27-year-old male presents to the trauma bay after a severe motor vehicle collision. He complains of chest pain, dysphagia, and shortness of breath. Examination reveals a painful, depressed sternoclavicular joint. What is the most appropriate next step in diagnostic imaging?
Explanation
Question 91
A 32-year-old bodybuilder feels a sudden 'pop' in his anterior chest wall while performing heavy bench presses. He has a loss of the anterior axillary fold and bruising over the medial arm. If operative repair is chosen, what is the anatomic footprint of the ruptured tendon?
Explanation
Question 92
A 65-year-old woman with a massive rotator cuff tear undergoes repair. Six weeks postoperatively, she exhibits profound, isolated weakness of the anterior deltoid and reports a sudden inability to actively elevate her arm after a minor fall, although passive elevation is preserved. An axillary nerve injury is ruled out. What surgical complication most likely occurred?
Explanation
Question 93
In evaluating a patient with scapulothoracic crepitus (snapping scapula syndrome), a palpable mass is felt at the superomedial angle of the scapula. What is the most common benign bone tumor responsible for this presentation?
Explanation
Question 94
A patient is evaluated for Parsonage-Turner syndrome (idiopathic brachial neuritis). Which of the following clinical patterns is the classic hallmark of this condition?
Explanation
Question 95
A 70-year-old woman sustains a 4-part proximal humerus fracture and undergoes a hemiarthroplasty. During the procedure, the tuberosities are reconstructed. What factor is most critical for achieving a good functional outcome regarding active elevation postoperatively?
Explanation
None
