Orthopedic Prometric MCQs - Chapter 3 Part 35
Orthopedic Prometric MCQs - Chapter 3 Part 35
Comprehensive 100-Question Exam
00:00
Start Quiz
Question 1
Advantages of minimally invasive lumbar interbody fusion over traditional open interbody fusion include:
Explanation
Question 2
Which of the following instruments are of value to a surgeon when performing minimally invasive lumbar fusions:
Explanation
Question 3
Which of the following statements is true regarding minimally invasive posterior lumbar interbody fusion:
Explanation
Question 4
Which of the following is not a described technique of minimally invasive anterior lumbar interbody fusion:
Explanation
Question 5
Which of the following statements is false regarding minimally invasive transperitoneal anterior lumbar interbody fusion:
Explanation
Question 6
All of the following are elements of the lateral mass of cervical spinal segments except:
Explanation
Question 7
To avoid vertebral artery injury during cervical lateral mass screw placement, it is best to:
Explanation
Question 8
Which of the following is/are potential complications associated with posterior cervical decompression and placement of lateral mass screws:
Explanation
Question 9
Which of the following statements is true regarding the C 2 lateral mass:
Explanation
Question 10
The technique for C1-C 2 lateral mass fixation may involve:
Explanation
Question 11
Which of the following conditions is not associated with cervical fractures:
Explanation
Question 12
Which of the following pathogens is not typically implicated in diskitis:
Explanation
Question 13
Which imaging modality is usually the least sensitive in diagnosing discitis:
Explanation
Question 14
Potts disease is most commonly treated by:
Explanation
Question 15
Which of the following is characteristic of patients with Klippel-Feil syndrome:
Explanation
Question 16
A burst fracture results in failure of the:
Explanation
Question 17
What type of fracture is presented in the radiograph (Slide):
Explanation
Question 18
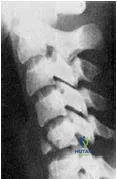
What type of fracture is presented in the radiograph (Slide):
Explanation
 Clearly seen in this radiograph is a fracture along the anterior/inferior vertebral body, which is a characteristic of a teardrop fracture.
Clearly seen in this radiograph is a fracture along the anterior/inferior vertebral body, which is a characteristic of a teardrop fracture.
Question 19
Which of the following may be used as treatment options for bilateral facet dislocations:
Explanation
Question 20
Which of the following fracture types is the most stable fracture:
Explanation
Question 21
Which of the following strictly defines the boundaries of Kambin's working triangle utilized in transforaminal endoscopic and minimally invasive spine procedures?
Explanation
Question 22
A key theoretical advantage of the paramedian Wiltse approach used in minimally invasive lumbar fusion, as opposed to the traditional midline open approach, is the preservation of which of the following structures?
Explanation
Question 23
A 55-year-old female undergoes a minimally invasive lateral lumbar interbody fusion (LLIF) at L4-L5. Postoperatively, she demonstrates weakness in hip flexion and knee extension, along with anterior thigh numbness. Which of the following structures was most likely injured during the retractor docking phase?
Explanation
Question 24
Cortical bone trajectory (CBT) pedicle screws are increasingly used in minimally invasive lumbar fusions. Which of the following best describes the starting point and trajectory of a CBT screw compared to a traditional pedicle screw?
Explanation
Question 25
Which of the following statements is true regarding radiation exposure to the surgical team during minimally invasive (MIS) lumbar fusions compared to traditional open procedures?
Explanation
Question 26
A 62-year-old male presents with neurogenic claudication and L5-S1 isthmic spondylolisthesis. Why is a standard lateral lumbar interbody fusion (LLIF) approach generally contraindicated at this specific level?
Explanation
Question 27
During a single-level minimally invasive transforaminal lumbar interbody fusion (MIS TLIF) using a non-expandable tubular retractor, a small incidental durotomy occurs. The surgeon assesses the tear to be 2 mm. What is the most appropriate management strategy?
Explanation
Question 28
When comparing minimally invasive transforaminal lumbar interbody fusion (MIS TLIF) to anterior lumbar interbody fusion (ALIF), which of the following is a recognized limitation of the MIS TLIF approach?
Explanation
Question 29
Review the provided imaging.
In managing a patient with symptomatic L4-L5 degenerative spondylolisthesis, which of the following is a proven advantage of utilizing a minimally invasive transforaminal lumbar interbody fusion (MIS TLIF) over an open approach?
Explanation
Question 30
Based on the intraoperative fluoroscopy image,
when placing percutaneous pedicle screws, what is the most common direction of cortical breach that risks injury to the exiting nerve root?

Explanation
Question 31
During the placement of percutaneous pedicle screws for a minimally invasive fusion, the surgeon inadvertently advances the Jamshidi guidewire too far anteriorly. Which of the following complications is most likely to occur as a direct result of an anterior vertebral body breach at the L4 level?
Explanation
Question 32
The use of recombinant human bone morphogenetic protein-2 (rhBMP-2) in minimally invasive transforaminal lumbar interbody fusion (MIS TLIF) has been associated with which of the following specific postoperative complications?
Explanation
Question 33
Which of the following is the most appropriate indication for utilizing an interlaminar endoscopic approach rather than a transforaminal endoscopic approach for a lumbar discectomy?
Explanation
Question 34
During a lateral lumbar interbody fusion (LLIF) at L4-L5, which of the following intraoperative neuromonitoring modalities is most critical to prevent lumbar plexus injury during dilation and retractor placement?
Explanation
Question 35
During a percutaneous transforaminal endoscopic discectomy or MIS approach, the surgeon accesses the disc space via Kambin's triangle. Which of the following structures forms the medial (posterior) boundary of this working zone?
Explanation
Question 36
The Wiltse paraspinal approach is frequently utilized in minimally invasive lumbar surgeries to minimize muscle morbidity. This approach utilizes an internervous and intermuscular plane between which of the following muscle groups?
Explanation
Question 37
When establishing the operative corridor for a minimally invasive transforaminal lumbar interbody fusion (MIS TLIF) using a tubular retractor system, what is the primary initial bony docking point?

Explanation
Question 38
Cortical bone trajectory (CBT) screws have gained popularity in minimally invasive lumbar fusions. Which of the following best describes the entry point and trajectory of a CBT pedicle screw compared to a traditional pedicle screw?
Explanation
Question 39
A surgeon is performing a lateral lumbar interbody fusion (LLIF/XLIF). At which of the following operative levels is the patient at the highest risk for postoperative lumbar plexus injury or severe psoas weakness?
Explanation
Question 40
A 55-year-old patient undergoes an uncomplicated L4-L5 MIS TLIF for right-sided radiculopathy. Postoperatively, the patient develops severe new-onset left-sided (contralateral) radicular leg pain. What is the most likely intraoperative cause of this complication?
Explanation
Question 41
Oblique lumbar interbody fusion (OLIF) was developed as an alternative to the transpsoas lateral approach (LLIF). What is the primary anatomical advantage of OLIF over LLIF?
Explanation
Question 42
Histological studies comparing multifidus muscle integrity after open versus minimally invasive lumbar fusion demonstrate significantly less muscle atrophy in the MIS group. What is the primary mechanism of multifidus injury prevented by the MIS tubular approach?
Explanation
Question 43
Recombinant human bone morphogenetic protein-2 (rhBMP-2) is frequently used off-label as a bone graft extender in MIS TLIF procedures. Which of the following is a recognized complication specifically associated with its use in the posterior lumbar spine?
Explanation
Question 44
The image demonstrates interbody cage subsidence. Which of the following technical errors most significantly increases the risk of cage subsidence following an MIS TLIF?

Explanation
Question 45
Minimally invasive spine surgery heavily relies on intraoperative fluoroscopy, increasing radiation exposure to the surgeon. According to the inverse square law, stepping back 1 meter from the C-arm during exposure reduces the radiation dose by approximately what factor compared to standing 0.5 meters away?
Explanation
Question 46
During a single-level MIS TLIF using a 22 mm tubular retractor, an incidental durotomy occurs with visible cerebrospinal fluid leak. Primary suture repair is technically impossible due to limited visualization. What is the most appropriate next step in management?
Explanation
Question 47
Computer-assisted navigation with intraoperative CT (O-arm) is increasingly used for percutaneous pedicle screw placement in MISS. What intraoperative maneuver is most likely to cause a "registration error" resulting in inaccurate screw navigation?
Explanation
Question 48
For a patient with an L5-S1 isthmic spondylolisthesis and significant loss of segmental lordosis, an Anterior Lumbar Interbody Fusion (ALIF) may be preferred over an MIS TLIF. What is the primary biomechanical advantage of ALIF at this specific level?
Explanation
Question 49
A patient presents with pseudoarthrosis one year after an L4-L5 MIS TLIF. Given the constraints of minimally invasive approaches, what is the most common technical etiology for pseudarthrosis in this specific procedure?
Explanation
Question 50
During the placement of percutaneous pedicle screws, a Kirschner wire (K-wire) is impacted into the pedicle. What is the most devastating complication associated with poor K-wire control during this step?
Explanation
Question 51
Biomechanical studies comparing Cortical Bone Trajectory (CBT) screws to traditional pedicle screws demonstrate which of the following characteristics?
Explanation
Question 52
Which of the following clinical scenarios represents a relative contraindication to a minimally invasive transforaminal lumbar interbody fusion (MIS TLIF)?
Explanation
Question 53
When counseling a patient on the long-term outcomes of minimally invasive vs open lumbar fusion, what does current literature indicate regarding the incidence of symptomatic adjacent segment disease (ASD) at 5 years?
Explanation
Question 54
A surgeon plans a unilateral MIS TLIF with unilateral percutaneous pedicle screw fixation for a patient with a paracentral disc herniation. Compared to a bilateral pedicle screw construct, the unilateral construct is significantly weaker in resisting which force?
Explanation
Question 55
Compared to traditional open transforaminal lumbar interbody fusion (TLIF), minimally invasive (MIS) TLIF is most consistently associated with which of the following?
Explanation
Question 56
During a minimally invasive TLIF using a tubular retractor system, the initial docking site for the first dilator is typically the:
Explanation
Question 57
Which of the following approaches utilizes the interval between the multifidus and longissimus muscles?
Explanation
Question 58
Which of the following is a recognized absolute contraindication for a transpsoas extreme lateral interbody fusion (XLIF)?
Explanation
Question 59
During a lateral transpsoas interbody fusion at L4-L5, the patient develops immediate postoperative ipsilateral hip flexion weakness and anterior thigh numbness. What is the most likely cause?
Explanation
Question 60
In cortical bone trajectory (CBT) pedicle screws used for minimally invasive fusions, the screw trajectory is typically described as:
Explanation
Question 61
A key mechanism by which minimally invasive lateral lumbar interbody fusion (LLIF) achieves indirect decompression of the neural foramina is through:
Explanation
Question 62
Review the clinical image.
When performing a percutaneous transforaminal endoscopic discectomy, instruments are passed through Kambin's triangle. Which of the following defines the medial border of Kambin's triangle?

Explanation
Question 63
The use of continuous free-running electromyography (EMG) is considered standard of care in the transpsoas lateral lumbar approach to avoid injury to which structure?
Explanation
Question 64
Compared to traditional open TLIF, studies evaluating muscle parameters post-MIS TLIF consistently demonstrate:
Explanation
Question 65
A major disadvantage of the minimally invasive posterior lumbar interbody fusion (MIS PLIF) approach compared to MIS TLIF is:
Explanation
Question 66
During a minimally invasive unilateral TLIF with bilateral decompression (over-the-top technique), the surgeon undercuts the spinous process to decompress the contralateral side. Which structure must be preserved to prevent iatrogenic instability?
Explanation
Question 67
Review the radiograph of a MIS stabilization construct.
To ensure proper placement of percutaneous pedicle screws, a true anteroposterior (AP) fluoroscopic image is essential. What confirms a true AP view of a lumbar vertebra?

Explanation
Question 68
When performing an anterior lumbar interbody fusion (ALIF) at L4-L5, the surgeon encounters massive venous bleeding from a large vessel situated directly anterior to the L4-L5 disc space. Which vessel is most likely injured?
Explanation
Question 69
Retrograde ejaculation is a known complication of anterior lumbar interbody fusion (ALIF). This is caused by injury to the:
Explanation
Question 70
In a patient undergoing MIS TLIF for a degenerative spondylolisthesis, which of the following is an advantage of placing a banana-shaped interbody cage anteriorly in the disc space?
Explanation
Question 71
Compared to an open Transforaminal Lumbar Interbody Fusion (TLIF), a minimally invasive (MIS) TLIF is characteristically associated with which of the following?
Explanation
Question 72
When performing a minimally invasive posterior lumbar approach using tubular retractors via a paramedian incision, the surgeon typically utilizes the natural intermuscular plane (Wiltse plane) located between the:
Explanation
Question 73
A major established disadvantage of minimally invasive spine surgery (MISS) techniques when compared to traditional open posterior techniques is:
Explanation
Question 74
During the placement of a percutaneous pedicle screw for an MIS TLIF, what is the ideal starting point for the Jamshidi needle on the true anteroposterior (AP) fluoroscopic view before advancing into the pedicle?
Explanation
Question 75
Which of the following neural structures is at the greatest risk of iatrogenic injury during the annulotomy and disc preparation phase of a minimally invasive transforaminal lumbar interbody fusion (MIS TLIF)?
Explanation
Question 76
What is the most common clinically significant complication uniquely associated with the placement of percutaneous pedicle screws compared to open pedicle screw placement?
Explanation
Question 77
When performing an "over-the-top" bilateral decompression for central canal stenosis through a unilateral minimally invasive tubular approach, which critical stabilizing structure is intentionally preserved?
Explanation
Question 78
Regarding the learning curve for minimally invasive lumbar fusion (MIS TLIF), literature demonstrates that during a surgeon's early experience, there is a statistically higher incidence of which of the following complications?
Explanation
Question 79
In Cortical Bone Trajectory (CBT) screw fixation, often utilized in minimally invasive lumbar surgeries, the pedicle screw path is fundamentally directed:
Explanation
Question 80
A 60-year-old male undergoes a minimally invasive extreme lateral interbody fusion (XLIF) at L4-L5. Postoperatively, he presents with profound weakness in hip flexion and knee extension, along with anterior thigh numbness. Which structure was most likely injured?
Explanation
Question 81
Which of the following is considered an absolute or strong relative contraindication for a minimally invasive direct lateral transpsoas lumbar interbody fusion (LLIF/XLIF)?
Explanation
Question 82
A surgeon uses fluoroscopy to place percutaneous screws
. Which strategy is most effective at reducing radiation exposure specifically to the surgeon's hands?

Explanation
Question 83
During a minimally invasive tubular decompression, an incidental durotomy occurs
. What is the most appropriate initial management step?

Explanation
Question 84
Compared to the traditional open posterior lumbar interbody fusion (PLIF), the minimally invasive (MIS) PLIF or TLIF approach is primarily associated with:
Explanation
Question 85
During an endoscopic transforaminal lumbar discectomy, accessing the L5-S1 disc space is often technically limited or prevented by which anatomical structure?
Explanation
Question 86
In an MIS TLIF, endplate preparation can be challenging due to the limited visual corridor. Inadequate endplate preparation is most strongly associated with which postoperative complication?
Explanation
Question 87
When comparing long-term follow-up (e.g., 2 to 5 years) between patients who underwent MIS TLIF versus Open TLIF, the literature generally shows equivalence in:
Explanation
Question 88
The use of expandable interbody cages in MIS TLIF has gained popularity. A theoretical biomechanical advantage of an expandable cage over a static cage inserted through a small tubular retractor is:
Explanation
Question 89
What is the primary indication for the utilization of continuous intraoperative neuromonitoring (EMG) during a minimally invasive direct lateral interbody fusion (XLIF)?
Explanation
Question 90
A 45-year-old morbidly obese patient requires an L4-L5 fusion for a mobile grade 1 spondylolisthesis. A primary advantage of selecting an MIS tubular approach over a standard open approach in this specific patient population is:
Explanation
None
