Orthopedic Prometric MCQs - Chapter 3 Part 48
Orthopedic Prometric MCQs - Chapter 3 Part 48
Comprehensive 100-Question Exam
00:00
Start Quiz
Question 1
Histology of chronic Achilles tendinosis DOES NOT reveal which of the following:
Explanation
Question 2
Initial management of a symptomatic Haglundâ s deformity in a runner consists of:
Explanation
Question 3
Which of the following is not consistent with a complete rupture of the Achilles tendon:
Explanation
Question 4
The primary collagen type found in the knee meniscus is:
Explanation
Question 5
The transverse intermensical ligament is occasionally the only site of attachment for the:
Explanation
Question 6
With regard to the meniscofemoral ligaments, the ligament of Humphrey runs ___ to the posterior cruciate ligament (PC L) and the ligament of Wrisberg runs _____ to the PC L.
Explanation
Question 7
The ligament that has an association with an unstable lateral discoid meniscus is:
Explanation
Question 8
Vascularity of the adult meniscus is limited to the:
Explanation
Question 9
The most important structure that resists anterior tibial translation in the anterior cruciate ligament (AC L)-deficient knee is the:
Explanation
Question 10
Approximately what percentage of middle-aged tennis players are able to return to tennis after rotator cuff surgery:
Explanation
Question 11
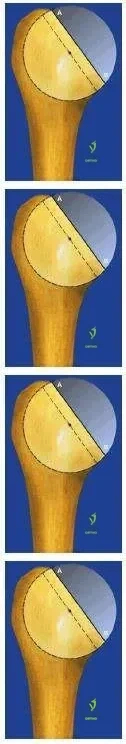
Proximal humeral anatomy is variable. Which of the following measurements most accurately describe the range of diameters of the humeral head (length of line AB):
Explanation

Question 12
Which of the following statements best describes the relationship of humeral head diameter to humeral head thickness:
Explanation
Question 13
Proximal humeral anatomy is variable. Which of the following measurements most accurately describe the range of radius of curvature of the humeral head (length of line AB):
Explanation
Question 14
The proximal humeral articular surface can be described as a portion of a sphere. The center of this sphere has which of the following anatomic relationships to the long axis of the humerus:
Explanation
Question 15
Which of the following pitch types is associated with the development of shoulder pain in baseball pitchers between the ages of 9 and 14 years:
Explanation
Question 16
Which of the following pitch types is associated with the development of elbow pain in baseball pitchers between the ages of 9 and 14 years:
Explanation
Question 17
It is recommended to limit youth baseball pitchers (9 to 14 years of age) to how many pitches per game
Explanation
Question 18
It is recommended to limit youth baseball pitchers (9 to 14 years of age) to how many game situation pitches per baseball season:
Explanation
Question 19
Which of the following statements is true regarding traumatic anterior shoulder instability:
Explanation
Question 20
Which of the following is the most common radiographic finding in patients with lateral epicondylitis:
Explanation
Question 21
A 45-year-old runner presents with chronic posterior heel pain. MRI reveals severe insertional Achilles tendinopathy. The surgeon plans an aggressive debridement of the tendon insertion. If surgical debridement requires excision of greater than 50% of the tendon insertion, which of the following is the most appropriate next step?
Explanation
Question 22
Which of the following physical examination tests is considered the most sensitive for diagnosing an acute Achilles tendon rupture?
Explanation
Question 23
The blood supply to the Achilles tendon is most precarious in its 'watershed' region, predisposing it to tendinosis and rupture. Where is this hypovascular region typically located relative to the calcaneal insertion?
Explanation
Question 24
A 40-year-old man undergoes percutaneous repair of an acute Achilles tendon rupture using a specific jig system. Postoperatively, he complains of numbness along the lateral aspect of his foot. Which nerve was most likely injured during the procedure, and where does it typically cross the lateral border of the Achilles tendon?
Explanation
Question 25
A 55-year-old male presents with non-insertional Achilles tendinopathy. He is prescribed an eccentric training program (Alfredson protocol). Which of the following best describes the physiologic rationale for this specific physical therapy regimen?
Explanation
Question 26
A 32-year-old active patient with an acute Achilles tendon rupture is discussing nonoperative versus operative management. Based on modern high-level evidence utilizing early functional rehabilitation protocols, which of the following is true regarding clinical outcomes?
Explanation
Question 27
A 48-year-old patient presents with chronic Achilles tendinosis. Histological evaluation of the diseased tendon would most likely demonstrate which of the following findings when compared to a healthy, normal tendon?
Explanation
Question 28
A patient with severe insertional Achilles tendinopathy is scheduled for debridement and FHL transfer. If the surgeon harvests the FHL at the level of the midfoot, they must identify the Master Knot of Henry. Which of the following accurately describes this anatomic landmark?
Explanation
Question 29
A 35-year-old weekend warrior sustains an acute injury resulting in severe posterior heel pain.
To confirm an Achilles tendon rupture, the O'Brien needle test is performed. A needle is inserted 10 cm proximal to the calcaneal insertion. What is the expected movement of the needle hub during passive dorsiflexion of the foot if the tendon is completely ruptured distal to the needle?
Explanation
Question 30
Which of the following classes of antibiotics is a well-established risk factor for spontaneous Achilles tendon rupture, especially when used concurrently with oral corticosteroids?
Explanation
Question 31
A 60-year-old male presents with a neglected Achilles tendon rupture that occurred 3 months ago. MRI demonstrates a 6 cm gap between the tendon ends. What is the most appropriate surgical management for a defect of this size?
Explanation
Question 32
A 55-year-old active man presents with chronic insertional Achilles tendinopathy refractory to 6 months of conservative care. Intraoperatively, extensive calcific tendinosis is noted, and thorough debridement requires excision of 60% of the tendon insertion. What is the most appropriate next step in management?
Explanation
Question 33
Which of the following best describes the histologic findings characteristically seen in chronic non-insertional Achilles tendinosis?
Explanation
Question 34
Recent randomized controlled trials comparing operative repair versus non-operative management with early functional rehabilitation for acute Achilles tendon ruptures most consistently demonstrate which of the following?
Explanation
Question 35
During a percutaneous or minimally invasive repair of an acute Achilles tendon rupture, the sural nerve is most at risk of iatrogenic injury at which location relative to the tendon insertion?
Explanation
Question 36
A 60-year-old patient sustains an Achilles tendon rupture while taking levofloxacin for pneumonia. What is the proposed mechanism by which fluoroquinolones increase the risk of tendon rupture?
Explanation
Question 37
A 42-year-old recreational basketball player complains of chronic pain 4 cm proximal to the Achilles tendon insertion. This specific "watershed" zone is predisposed to tendinopathy primarily due to poor blood supply originating from which vessel?
Explanation
Question 38
A 28-year-old female runner presents with posterior heel pain and a palpable bony prominence lateral to the Achilles insertion. She has failed 3 weeks of rest. What is the most appropriate next step in the conservative management of her suspected Haglund's syndrome?
Explanation
Question 39
A 45-year-old man presents with sudden posterior ankle pain after lunging for a tennis ball. Clinical examination reveals a positive Thompson test. A lateral radiograph is obtained.
Which radiographic sign on a lateral ankle X-ray is most indicative of an acute Achilles tendon rupture?
Explanation
Question 40
The Alfredson protocol is considered a first-line treatment for non-insertional Achilles tendinopathy. Which of the following biomechanical principles is the primary focus of this rehabilitation protocol?
Explanation
Question 41
A 10-year-old boy who plays competitive soccer presents with bilateral posterior heel pain that worsens after practice. Examination reveals point tenderness over the calcaneal apophysis but no swelling or erythema. The Achilles tendon is intact. What is the most appropriate initial management?
Explanation
Question 42
Unlike many flexor tendons in the hand and wrist, the Achilles tendon lacks a true synovial sheath. Instead, it is enveloped by a layer of loose connective tissue. What is the primary function of this structure?
Explanation
Question 43
A patient presents with chronic insertional Achilles pain. The examiner passively dorsiflexes the ankle with the knee extended, noting 0 degrees of dorsiflexion. When the knee is flexed to 90 degrees, ankle dorsiflexion increases to 15 degrees. What does this physical examination finding indicate?
Explanation
Question 44
A 35-year-old male presents with bilateral, painless, nodular swelling of the Achilles tendons. He has a strong family history of premature coronary artery disease. A core biopsy of the mass would most likely reveal which of the following?
Explanation
Question 45
A 50-year-old patient presents with a neglected Achilles tendon rupture sustained 4 months ago. MRI reveals a defect of 7 cm between the retracted tendon ends. Which of the following is the most appropriate surgical reconstruction option?
Explanation
Question 46
When performing an FHL tendon transfer for a massive Achilles tendon defect, harvesting the FHL requires careful dissection to avoid injury to which closely associated structure at the level of the master knot of Henry?
Explanation
Question 47
Which of the following anatomic and pathologic triads correctly defines Haglund's syndrome?
Explanation
Question 48
Following surgical repair of an acute Achilles tendon rupture, what is the primary advantage of initiating an early functional rehabilitation protocol compared to traditional prolonged cast immobilization?
Explanation
Question 49
A 45-year-old male undergoes percutaneous repair of an acute Achilles tendon rupture. Postoperatively, he complains of numbness and tingling along the lateral border of his foot. Which of the following nerves was most likely injured during the procedure?
Explanation
Question 50
A 55-year-old patient with chronic insertional Achilles tendinosis undergoes surgical debridement. During the procedure, the surgeon notes that 60% of the tendon must be excised to remove all degenerative tissue. What is the most appropriate next step in management?
Explanation
Question 51
Non-insertional Achilles tendinopathy typically occurs in a poorly vascularized 'watershed' region. This region is located approximately how far proximal to the calcaneal insertion?
Explanation
Question 52
A 35-year-old male runner presents with acute posterior heel pain and weakness following a sudden push-off mechanism. The clinical examination finding shown in the image is expected to be positive. Which of the following is true regarding conservative management of this condition?
Explanation
Question 53
During physical examination for equinus contracture, a patient demonstrates 0 degrees of ankle dorsiflexion with the knee extended, and 15 degrees of dorsiflexion with the knee flexed to 90 degrees. What is the most appropriate surgical intervention if conservative measures fail?
Explanation
Question 54
A 40-year-old female undergoes an endoscopic plantar fascia release for recalcitrant plantar fasciitis. Six months postoperatively, she complains of new-onset lateral midfoot pain. What is the most likely cause of her current symptoms?
Explanation
Question 55
A 25-year-old skier sustains an acute dorsiflexion and eversion injury to the ankle, resulting in posterolateral ankle pain and a snapping sensation behind the lateral malleolus. Disruption of which of the following structures is most likely responsible for these symptoms?
Explanation
Question 56
A 55-year-old woman presents with a painful, flexible flatfoot deformity. Examination reveals inability to perform a single-leg heel raise, and the 'too many toes' sign is positive. The subtalar joint remains mobile. Which of the following is the most appropriate surgical treatment?
Explanation
Question 57
Which of the following nerves is classically entrapped between the deep fascia of the abductor hallucis muscle and the medial aspect of the quadratus plantae, causing chronic heel pain?
Explanation
Question 58
A 22-year-old professional ballet dancer complains of posterior ankle pain when assuming the 'en pointe' position. Physical examination reveals tenderness posteromedially and triggering of the great toe during active range of motion. What is the most likely diagnosis?
Explanation
Question 59
A 10-year-old boy presents with posterior heel pain that worsens after playing soccer. Examination reveals point tenderness over the calcaneal apophysis and a negative squeeze test of the calcaneal body. Radiographs show sclerosis of the apophysis. What is the recommended initial management?
Explanation
Question 60
A patient with a chronic Achilles tendon rupture presents with a palpable gap of 6 cm. What is the most appropriate reconstructive option?
Explanation
Question 61
A 60-year-old male is diagnosed with an acute Achilles tendon rupture. He has a history of a recent respiratory infection treated with an antibiotic. Which class of antibiotics is most strongly associated with an increased risk of Achilles tendon rupture?
Explanation
Question 62
In the surgical management of Haglund's syndrome, a Zadek osteotomy is sometimes performed. What is the primary anatomical alteration achieved by this procedure?
Explanation
Question 63
When performing a minimally invasive or percutaneous Achilles tendon repair, the sural nerve is at greatest risk of iatrogenic injury. At what approximate distance proximal to the calcaneal insertion does the sural nerve typically cross the lateral border of the Achilles tendon?
Explanation
Question 64
Which of the following biologic factors is most highly upregulated in the pathophysiology of chronic non-insertional Achilles tendinopathy, contributing directly to neovascularization?
Explanation
Question 65
A 40-year-old recreational athlete sustains an acute Achilles tendon rupture. Compared to traditional surgical repair, non-operative management utilizing early functional bracing and mobilization protocols has been shown to result in:
Explanation
Question 66
A 55-year-old male undergoes surgical debridement for severe insertional Achilles tendinopathy. After removing the calcific tendon portions and the Haglund's exostosis, 60% of the Achilles tendon insertion has been detached. What is the most appropriate next step in reconstruction?
Explanation
Question 67
During harvest of the flexor hallucis longus (FHL) through a posterior single-incision approach for Achilles augmentation, which neurovascular structure is at greatest risk if dissection strays immediately medial to the FHL muscle belly?
Explanation
Question 68
A 62-year-old patient presents with a neglected Achilles tendon rupture from 4 months ago. Intraoperatively, after debridement of the necrotic ends, there is a 7 cm gap with the ankle in neutral. Which reconstructive option is most appropriate for a defect of this size?
Explanation
Question 69
A 32-year-old runner has chronic posterior heel pain due to Haglund's deformity. If conservative measures fail, what is the biomechanical rationale for performing a Zadek (dorsal closing wedge) osteotomy of the calcaneus?
Explanation
Question 70
A patient with recalcitrant hindfoot pain is noted to have a lack of passive ankle dorsiflexion with the knee extended, but achieves 15 degrees of passive dorsiflexion with the knee flexed. Which surgical procedure targets the isolated pathology identified by this test?
Explanation
Question 71
A 19-year-old professional ballet dancer presents with posterior ankle pain exacerbated by the "en pointe" position. Nonoperative management has failed.
Surgical excision of the symptomatic Os trigonum is planned. This bony structure is located immediately lateral to which tendon?
Explanation
Question 72
The Achilles tendon is most vulnerable to rupture and non-insertional tendinopathy in its relative "watershed" area of decreased vascularity. This hypovascular zone is typically located:
Explanation
Question 73
A 65-year-old patient on chronic systemic corticosteroids is prescribed a broad-spectrum antibiotic for a respiratory infection and subsequently suffers bilateral acute Achilles tendon ruptures. Which class of antibiotics is most strongly associated with this complication?
Explanation
Question 74
A 72-year-old diabetic female falls and complains of severe posterior heel pain. Radiographs reveal a displaced avulsion fracture of the posterior calcaneal tuberosity involving the Achilles tendon insertion. The overlying skin is severely blanched. What is the most appropriate management?
Explanation
Question 75
Following an acute open Achilles tendon repair, utilizing an accelerated functional rehabilitation protocol (early weight-bearing and controlled range of motion) rather than traditional prolonged cast immobilization has been shown to:
Explanation
Question 76
When clinically evaluating a patient with a suspected acute Achilles tendon rupture, the Thompson test is considered highly reliable. A positive Thompson test is defined by:
Explanation
None
