Orthopedic Prometric MCQs - Chapter 3 Part 16
Orthopedic Prometric MCQs - Chapter 3 Part 16
Comprehensive 100-Question Exam
00:00
Start Quiz
Question 1
The best way to diagnose dysplasia epiphysealis hemimelica, in addition to history and physical, is:
Explanation
Question 2
Which of the following commonly used statements regarding the pelvis in patients with bladder exstrophy is true:
Explanation
Question 3
A 1-year-old child requires evaluation of limb length inequality. The surgeon notices a disproportional increase in length, as well as width, of the ipsilateral upper and lower extremity. No other physical abnormalities are evident. Recommended treatment includes which of the following:
Explanation
Question 4
Which of the following statements describes the growth plate biomechanics of the distal femur:
Explanation
Question 5
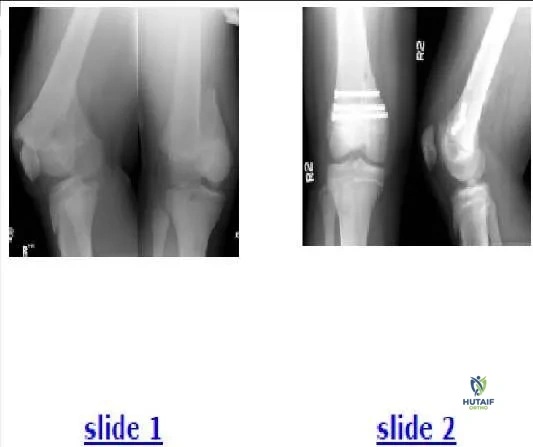
A 200-lb 13-year-old boy sustained a fracture while playing football. His radiographs are presented (Slide 1). Which of the following treatments should be attempted first:

Explanation
Question 6
An 8-year-old boy was injured by a lawnmower. The resulting proximal tibial injury presented in the radiograph (Slide) is classified as a:
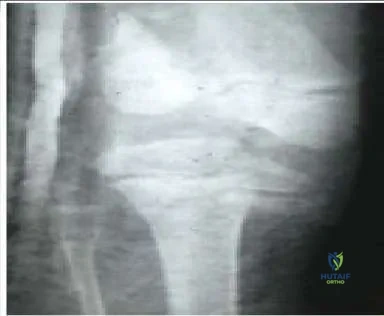
Explanation
Question 7
A 12-year-old boy twisted his knee while riding a bicycle. Based on his radiographs (Slide), which of the following is the most appropriate diagnosis:
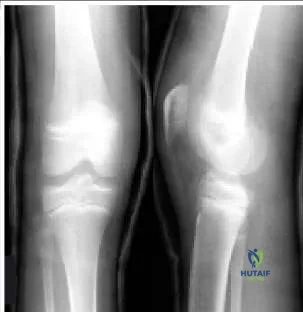
Explanation
Question 8
What is the most common cause of intoeing in children with bilateral cerebral palsy:
Explanation
Question 9
Risk factors for superior mesenteric artery syndrome after adolescent idiopathic scoliosis surgery include all of the following except:
Explanation
Question 10
An 8-year-old girl fractures her right femur when starting a sprint. Based on her radiograph (Slide), which of the following is the most likely diagnosis:
Explanation
Question 11
An 8-year old girl with fibrous dysplasia fractures her femur (Slide). Which of the following procedures is the best treatment option:
Explanation
Question 12
The patient presented in the radiograph (Slide) has a slight, painless limp. Which of the following is the most likely diagnosis:
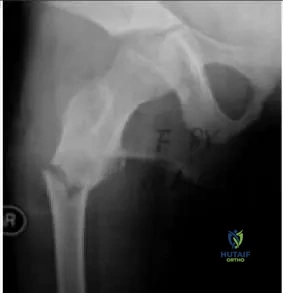
Explanation
Question 13
A 14-year-old boy sustains an avulsion of the tibial tubercle while playing basketball. The fracture extends vertically into the joint, crossing the proximal tibial articular surface. He is at greatest risk for which of the following complications:
Explanation
Question 14
An infant presents with idiopathic scoliosis. Which of the following factors indicates observation as the treatment of choice:
Explanation
Question 15
Which of the following factors predicts a lesser degree of impairment of pulmonary function in patients with adolescent idiopathic scoliosis:
Explanation
Question 16
All except which of the following neurologic/muscular disorders can present undiagnosed in a patient with scoliosis:
Explanation
Question 17
All except which of the following structural disorders often causes scoliosis and presents undiagnosed in patients:
Explanation
Question 18
Which of the following levels of evidence should be assigned to a prospective, randomized therapeutic study with 80% follow-up:
Explanation
Question 19
A prospective comparative study should be assigned which level of evidence:
Explanation
Question 20
A case-control study should be assigned which level of evidence:
Explanation
Question 21
A 3-year-old boy presents with short-limbed dwarfism, frontal bossing, and midface hypoplasia. Radiographs show narrowing of the interpedicular distances in the lumbar spine. Which of the following gene mutations is most likely responsible for this condition?
Explanation
Question 22
A 10-year-old child presents with a waddling gait, joint pain, and short stature. Radiographs show delayed, irregular ossification of multiple epiphyses and a "double-layered" patella laterally. A mutation in which of the following is most commonly implicated?
Explanation
Question 23
A newborn is evaluated for multiple congenital joint dislocations involving the knees, hips, and elbows. Physical examination reveals spatulate thumbs, a depressed nasal bridge, and a prominent forehead. What is the most critical initial imaging study to obtain in this patient?
Explanation
Question 24
A newborn infant is noted to have short limbs, rigid clubfeet, cystic swelling of the ear pinnae (cauliflower ears), and proximally placed, abducted thumbs (hitchhiker thumbs). This condition is caused by a defect in which of the following?
Explanation
Question 25
A 2-year-old child presents with an asymptomatic, painless mass over the mid-clavicle. There is no history of trauma. Radiographs reveal a defect in the middle third of the right clavicle with smooth, rounded bone ends. What is the most appropriate management?
Explanation
Question 26
A 4-year-old boy presents with progressive, asymmetric limb overgrowth, plantar cerebriform connective tissue nevi, and epidermal nevi. A mutation in which of the following genes is classically associated with this syndrome?
Explanation
Question 27
A 6-year-old child presents with severe disproportionate short-trunk dwarfism, corneal clouding, and normal intelligence. Radiographs show universal platyspondyly and hypoplasia of the odontoid. The patient is deficient in which of the following enzymes?
Explanation
Question 28
A 5-year-old boy has short-trunk dwarfism, coxa vara, and myopia. Radiographs reveal delayed ossification of the femoral heads and platyspondyly. Which of the following genetic mutations is responsible for this condition?
Explanation
Question 29
A 3-year-old child with multiple café-au-lait spots and axillary freckling presents with anterolateral bowing of the tibia. Radiographs show medullary canal narrowing and early pseudarthrosis. Which of the following is true regarding surgical management?
Explanation
Question 30
A 10-year-old girl is noted to have a large head with delayed closure of the fontanelles, dental anomalies, and the ability to appose her shoulders anteriorly. Radiographs reveal hypoplastic clavicles. Which of the following genes is affected in this autosomal dominant condition?
Explanation
Question 31
A newborn is diagnosed with osteogenesis imperfecta. According to the Sillence classification, which type is characterized by normal or near-normal stature and blue sclerae throughout life, making it the most common and mildest form?
Explanation
Question 32
A newborn presents with a deep constriction ring around the left lower leg and a distal clubfoot deformity. The toes exhibit acrosyndactyly. Which of the following is the most appropriate management for the deep constriction ring if it is causing distal vascular compromise?
Explanation
Question 33
A 1-year-old girl is evaluated for a short right leg. Examination reveals an absent 5th ray, anteromedial bowing of the tibia, and a dimple over the anterior shin. Radiographs confirm complete absence of the fibula. Which of the following knee ligament anomalies is most commonly associated?
Explanation
Question 34
A 5-year-old girl presents with an enlarged left lower extremity, varicose veins, and a port-wine stain extending from her thigh to her foot. No significant arteriovenous fistulas are noted. Which of the following is the most appropriate initial management for her projected 4 cm leg length discrepancy?
Explanation
Question 35
A newborn has multiple rigid joint contractures, featureless limbs lacking normal skin creases, and internal rotation of the shoulders. Sensation is intact, and intellect appears normal. Muscle biopsy is likely to show which of the following?
Explanation
Question 36
A child is born with a severely shortened right thigh held in flexion, abduction, and external rotation. Radiographs show absence of the proximal femur. According to the Aitken classification, a Type C Proximal Focal Femoral Deficiency (PFFD) is characterized by which of the following?
Explanation
Question 37
A 2-year-old boy presents with short stature, frontal bossing, and rhizomelic shortening of the limbs. Genetic testing reveals a mutation in the FGFR3 gene. Which of the following is true regarding the pathophysiology and inheritance of this condition?
Explanation
Question 38
A newborn presents with micromelic shortening, severe rigid clubfeet, "hitchhiker" thumbs, and cauliflower ears. What is the most likely underlying genetic defect?
Explanation
Question 39
A 7-year-old girl is evaluated for a broad forehead, delayed tooth eruption, and the ability to appose her shoulders anteriorly. Radiographs show hypoplastic clavicles. What is the primary molecular defect associated with this syndrome?
Explanation
Question 40
A 1-year-old child presents with a shortened right lower extremity. Radiographs reveal a severe proximal focal femoral deficiency (Aitken Class D) with absent hip joint.
Which of the following conditions is most frequently associated with this specific congenital anomaly?

Explanation
Question 41
A 4-year-old child presents with an enlarged left lower extremity, cutaneous port-wine stains, and prominent varicose veins. There is a 3 cm leg length discrepancy (left longer than right). What is the most appropriate initial management for the limb length inequality?
Explanation
Question 42
An infant is born with shortening of the leg, an anteromedial bow of the tibia, absent lateral rays of the foot, and a severe equinovalgus foot deformity. What is the most likely diagnosis?
Explanation
Question 43
A 3-year-old child with anterolateral bowing of the tibia develops a fracture that fails to heal despite casting.
Which of the following systemic conditions is most strongly associated with this bony pathology?

Explanation
Question 44
A 12-year-old boy presents with multiple painless bony bumps around his knees and ankles. Radiographs demonstrate multiple osteochondromas. Which gene mutation is responsible, and what is its normal cellular function?
Explanation
Question 45
A neonate sustains a clavicle fracture during birth. Sclerae are distinctly blue, and radiographs show osteopenia but no severe long bone bowing. By age 2, the child has had minimal fractures and is ambulatory. This presentation best fits which Sillence type of Osteogenesis Imperfecta?
Explanation
Question 46
A 6-year-old boy presents with short stature, normal intelligence, knock-knees, and a short trunk. Radiographs reveal platyspondyly with central anterior beaking of the vertebral bodies. He is at greatest risk for which of the following potentially life-threatening orthopedic complications?
Explanation
Question 47
A child with short-trunk dwarfism, a barrel chest, and coxa vara is diagnosed with Spondyloepiphyseal dysplasia congenita (SEDC). Which of the following genetic defects is characteristic of this disorder?
Explanation
Question 48
A 9-year-old child presents with a waddling gait and bilateral knee pain. Radiographs reveal delayed, irregular ossification of the femoral heads and other epiphyses, but the spine appears completely normal.
Which of the following is true regarding this condition?

Explanation
Question 49
A 3-year-old girl is evaluated for asymmetric overgrowth of her right leg. She has a history of an abdominal wall defect at birth, neonatal hypoglycemia, and macroglossia. She should be routinely screened with ultrasound for which of the following?
Explanation
Question 50
A 5-year-old boy presents with progressive, disproportionate overgrowth of the right lower extremity, macrodactyly, and cerebriform connective tissue nevi on his foot. The mutation associated with this syndrome is most likely located in which gene?
Explanation
Question 51
A 4-year-old child presents with short-limb dwarfism but was of normal length at birth. Radiographs show small, irregular epiphyses and fragmented metaphyses. The face and head are normal. Genetic testing shows a defect in the COMP gene. What is the diagnosis?
Explanation
Question 52
An infant is born with ring-like constrictions on multiple digits of both hands, and a severe clubfoot on the right side.
Which of the following is true regarding this syndrome?

Explanation
Question 53
A 2-year-old child presents with a shortened lower extremity, anteromedial bowing of the tibia, and an absent lateral ray of the foot. What is the most common associated anomaly of the knee in this condition?
Explanation
Question 54
A newborn is evaluated for a markedly shortened thigh and flexed, abducted, and externally rotated hip. Radiographs reveal absence of the proximal femur but a normal acetabulum. Which of the following conditions is most likely to be present ipsilaterally?
Explanation
Question 55
A mother brings her 3-month-old infant to the clinic because of a painless lump over the right collarbone. There is no history of birth trauma. Radiographs show a distinct lucency in the middle third of the right clavicle with smooth, rounded bone ends. What is the most appropriate management?
Explanation
Question 56
A 7-year-old boy presents with delayed tooth eruption, frontal bossing, and the ability to approximate his shoulders in the midline anteriorly. A mutation in which of the following genes is responsible for this condition?
Explanation
Question 57
A 4-year-old child with achondroplasia presents with progressively declining motor milestones, hyperreflexia, and sleep apnea. What is the most critical next step in evaluation?
Explanation
Question 58
A 5-year-old child presents with disproportionate short stature, a waddling gait, and ligamentous laxity. The facial features are completely normal. Radiographs reveal delayed ossification of the epiphyses and irregular metaphyses. A mutation in which gene is most likely responsible?
Explanation
Question 59
A 12-year-old boy presents with bilateral knee pain and a waddling gait. Radiographs show delayed, irregular ossification of the epiphyses and a "double-layer" patella on the lateral view. Which of the following best describes this condition?
Explanation
Question 60
A 6-year-old child with severe short-trunk dwarfism, a barrel chest, and cleft palate is diagnosed with spondyloepiphyseal dysplasia congenita. Which of the following orthopedic complications requires meticulous monitoring in this patient?
Explanation
Question 61
A neonate presents with short-limbed dwarfism, rigid clubfeet, swelling of the pinnae ("cauliflower ears"), and abducted thumbs. What is the most common spinal deformity associated with this condition?
Explanation
Question 62
A neonate is born with internally rotated shoulders, extended elbows, flexed wrists, dislocated hips, and rigid equinovarus foot deformities bilaterally. Sensation and intelligence are normal. Muscle biopsy would most likely show:
Explanation
Question 63
A newborn presents with bilateral knee dislocations, bilateral hip dislocations, and clubfeet. The face exhibits a depressed nasal bridge and prominent forehead. What critical radiographic evaluation must be performed before any manipulative casting or surgery?
Explanation
Question 64
A newborn has an amputation of the right hand at the wrist and a deep, circumferential constriction band around the left lower leg. The left foot is swollen and cyanotic. What is the appropriate management for the left leg?
Explanation
Question 65
A neonate presents with a markedly shortened lower leg, varus foot positioning, and an absent hallux. Radiographs reveal complete absence of the tibia but an intact fibula (Jones Type 1a). Which of the following inheritance patterns is associated with this condition when part of Werner syndrome?
Explanation
Question 66
A 4-year-old child with multiple café-au-lait spots and axillary freckling presents with progressive anterolateral bowing of the tibia. Radiographs show a narrowing of the tibial diaphysis with a cystic lesion. Which of the following treatments has the highest success rate if a pseudarthrosis develops?
Explanation
Question 67
Which of the following statements regarding the pelvic anatomy in patients with classic bladder exstrophy is correct?

Explanation
Question 68
A 12-year-old boy presents with recurrent ankle sprains and a painful, rigid flatfoot.
CT confirms a calcaneonavicular coalition. What is the most common radiographic sign of this condition seen on a lateral plain film?

Explanation
Question 69
A 13-year-old obese boy presents with thigh pain and obligatory external rotation with hip flexion. He is diagnosed with a slipped capital femoral epiphysis (SCFE). Which of the following is an absolute indication for prophylactic pinning of the contralateral asymptomatic hip?
Explanation
Question 70
A 3-year-old child presents with progressive bilateral genu varum. Radiographs demonstrate changes consistent with Langenskiöld stage III Blount's disease.
The primary pathophysiology of infantile Blount's disease involves which of the following?

Explanation
Question 71
A 6-year-old boy is diagnosed with Legg-Calvé-Perthes disease. Which of the following radiographic findings is recognized as a 'head-at-risk' sign indicating a poorer prognosis and risk for hinge abduction?
Explanation
Question 72
A 2-week-old infant is being evaluated for developmental dysplasia of the hip (DDH). In which of the following clinical scenarios is the use of a Pavlik harness strictly contraindicated?
Explanation
Question 73
A newborn is noted to have a shortened leg, anterior bowing of the tibia, and an absent lateral ray of the foot.
Radiographs confirm fibular hemimelia. Which of the following knee conditions is most commonly associated with this anomaly?

Explanation
Question 74
A 7-year-old boy with spastic diplegic cerebral palsy has progressive hip pain. AP pelvis radiograph demonstrates a migration percentage of 55%. What is the most appropriate definitive management?
Explanation
Question 75
A 12-year-old boy with Duchenne muscular dystrophy has developed a 50-degree scoliotic curve. His forced vital capacity (FVC) is currently 40% of predicted. What is the recommended management?
Explanation
Question 76
A 5-year-old child with blue sclerae, dentinogenesis imperfecta, and multiple prior fractures is started on pamidronate therapy. What is the primary mechanism of action of this medication?
Explanation
Question 77
During the initial phases of the Ponseti method for correcting clubfoot (talipes equinovarus), the foot is externally rotated/abducted. To avoid creating a midfoot breach, counter-pressure must be correctly applied to which specific anatomical structure?
Explanation
Question 78
A 9-year-old girl is diagnosed with Klippel-Feil syndrome based on a short neck, low posterior hairline, and limited cervical range of motion. Screening of which of the following organ systems is mandatory due to a high association with this syndrome?
Explanation
Question 79
A 3-year-old child presents with progressive bowing of the lower extremities, short stature, and a waddling gait.
Laboratory studies show a normal serum calcium, markedly low serum phosphate, elevated alkaline phosphatase, and normal PTH. What is the most likely diagnosis?

Explanation
Question 80
Congenital pseudarthrosis of the tibia (CPT) presents with anterolateral bowing of the tibia and is notoriously difficult to treat. It is most strongly associated with which of the following systemic conditions?
Explanation
Question 81
A 2-month-old boy is brought to the clinic for congenital muscular torticollis. His head is tilted to the right and rotated to the left. A firm mass is palpated in the right sternocleidomastoid muscle. Which of the following screening evaluations is highly recommended?
Explanation
Question 82
A 5-year-old child with achondroplasia presents with newly developed central sleep apnea, hyperreflexia, and clonus.
What is the most likely anatomical etiology of these neurological symptoms?

Explanation
Question 83
A 6-year-old boy sustains a severely displaced extension-type supracondylar humerus fracture. On examination, he has a completely absent radial pulse, but his hand is warm, pink, and has a capillary refill of less than 2 seconds. What is the most appropriate next step in management?
Explanation
Question 84
Sprengel deformity is characterized by a high-riding, dysplastic scapula. It is often associated with an omovertebral bone or fibrous band. The omovertebral connection typically attaches from the cervical spine to which part of the scapula?
Explanation
Question 85
According to the Aitken classification for Proximal Focal Femoral Deficiency (PFFD), Class A is defined by which of the following characteristics?
Explanation
Question 86
A 10-year-old girl has a projected limb length discrepancy of 3.5 cm at skeletal maturity due to overgrowth following a previous femur fracture. What is the most appropriate treatment option?
Explanation
None
