Orthopedic Prometric MCQs - Chapter 3 Part 28
Orthopedic Prometric MCQs - Chapter 3 Part 28
Comprehensive 100-Question Exam
00:00
Start Quiz
Question 1
A patient with a fracture dislocation of the spine has a sensory level at the xiphoid process. Which of the following nerve root levels indicates this finding:
Explanation
Question 2
A patient with a fracture dislocation of the spine has a sensory level at the umbilicus. Which of the following nerve root levels indicates this finding:
Explanation
Question 3
Which of the following statements regarding the presentation of thoracic disk herniations is false:
Explanation
Question 4
Which of the following statements regarding the treatment of thoracic disk herniations is true:
Explanation
Question 5
Which of the following is the only accepted pharmacological agent for the acute treatment of a spinal cord injury:
Explanation
Question 6
A 45-year-old man has neck pain following a motor vehicle accident. His neurologic examination is normal. His plain radiographs are shown (Slide). The most likely diagnosis is:
Explanation
Question 7
A 35-year-old man has neck pain following a motor vehicle accident. His axial computed tomography scan is shown (Slide). The most likely diagnosis is:
Explanation
Question 8
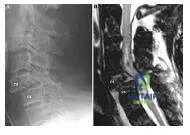
A 40-year-old woman has severe neck pain following a motor vehicle accident. Her plain lateral radiograph of the spine is shown (Slide). A sagittal magnetic resonance scan is shown (Slide). The most likely diagnosis is:
Explanation
Question 9
A 40-year-old woman has severe neck pain following a motor vehicle accident. Her plain lateral radiograph of the spine is shown (Slide). A sagittal magnetic resonance is shown (Slide). The most appropriate treatment would be:
Explanation
Question 10
In which of the following nerve roots is compression neuropathy common in cervical spondylosis:
Explanation
Question 11
Which of the following sensory areas is affected by compression of the C 6 nerve root:
Explanation
Question 12
Which of the following sensory areas is affected by compression of the C 7 nerve root:
Explanation
Question 13
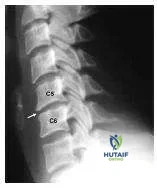
A patient comes into your office with neck and arm pain. The patientâ s plain radiograph is shown (Slide). Which of the following signs is most likely to be found on physical examination:
Explanation
 C5 Base of neck to shoulder and upper arm C6 Lateral forearm into the radial side of the hand C7 Posterolateral forearm into the middle finger of the hand C8 Ulnar side of the forearm and hand
C5 Base of neck to shoulder and upper arm C6 Lateral forearm into the radial side of the hand C7 Posterolateral forearm into the middle finger of the hand C8 Ulnar side of the forearm and hand
Question 14
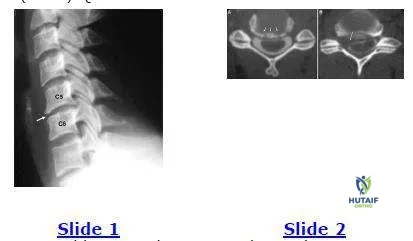
A 45-year-old woman has pain in her right upper extremity and neck. The plain film is is presented (Slide 1) as well as an axial post myelogram CT images (Slide 2, A & B). Her pain has not responded to nonsteroidal anti- inflammatory drugs or physical therapy. Which of the following is the most appropriate treatment:
Explanation
Question 15
Plain radiographs of the lumbosacral spine are useful for:
Explanation
Question 16
Computerized tomography scans are efficacious for detecting which of the following conditions:
Explanation
Question 17
A 35-year-old construction worker has left leg pain and difficulty walking. His examination is normal except for decreased sensation to the lateral border of the left foot, the inability to walk on the toes of the left foot, and a positive stretch test producing left heel and lateral foot pain. A magnetic resonance image shows a large posterolateral herniated nucleus pulposus on the left side at L5-S1. The gait abnormality is most likely due to:
Explanation
Question 18
Which of the following types of neural dysfunction is present with a cervical fracture-dislocation, resulting in a Brown-Sequard neurological injury:
Explanation
Question 19
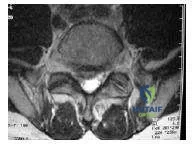
The axial computed tomography scan depicts a patient with spinal stenosis (Slide). The primary source of neural compression is impingement on the traversing nerve root by the:
Explanation
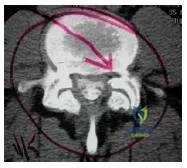
Question 20
The type of disk herniation shown (Slide) at the L5-S1 level is most likely to cause:
Explanation

Question 21
A 32-year-old male sustains a stab wound to the back.
Neurological examination reveals right-sided paralysis and loss of vibration sense, along with left-sided loss of pain and temperature sensation below the T8 level. Which of the following best describes this syndrome?

Explanation
Question 22
A patient with a suspected spinal fracture is found to have sensory loss up to the level of the nipples. Which dermatomal nerve root level corresponds to this finding?
Explanation
Question 23
During the evaluation of a patient with a spinal cord injury, the examiner notes that the patient has intact proprioception and vibration sense, but complete loss of motor function, pain, and temperature sensation below the level of the lesion. What is the most likely diagnosis?
Explanation
Question 24
Which of the following surgical approaches is strictly contraindicated for the excision of a central calcified thoracic disc herniation?
Explanation
Question 25
A 25-year-old male is brought to the emergency department after a high-speed motor vehicle accident. He has a T2 fracture-dislocation. His blood pressure is 80/50 mmHg and heart rate is 50 bpm. His extremities are warm and pink. What is the primary cause of his hemodynamic instability?
Explanation
Question 26
A 45-year-old female presents with a seatbelt-type flexion-distraction injury (Chance fracture) of the L1 vertebra.
Which of the following associated injuries must be meticulously ruled out?

Explanation
Question 27
According to the Thoracolumbar Injury Classification and Severity (TLICS) score, which of the following patients has an absolute indication for surgical intervention?
Explanation
Question 28
A patient with a T4 level complete spinal cord injury suddenly develops a severe pounding headache, diaphoresis above the level of injury, and a blood pressure of 210/110 mmHg. What is the most appropriate initial management?
Explanation
Question 29
A spinal cord injury patient presents with perianal sensation, voluntary anal sphincter contraction, and intact great toe flexion, despite otherwise complete motor and sensory loss below T10. This clinical scenario indicates:
Explanation
Question 30
The bulbocavernosus reflex is mediated by which of the following nerve roots?
Explanation
Question 31
Thoracic disc herniations most commonly occur at which of the following vertebral levels?
Explanation
Question 32
A 65-year-old male with long-standing cervical spondylosis sustains a hyperextension injury to his neck. Examination shows marked bilateral weakness in his upper extremities, particularly the hands, with relative sparing of motor function in his lower extremities. What is the most likely diagnosis?
Explanation
Question 33
A patient with a suspected spinal injury demonstrates a sensory level exactly at the umbilicus.
Which dermatome correlates to this landmark?
Explanation
Question 34
A patient is brought to the emergency department after a motor vehicle collision. Neurological examination reveals loss of motor function, pain, and temperature sensation below the T6 level, but proprioception and vibratory sense are intact. Which of the following spinal cord syndromes is the most likely diagnosis?
Explanation
Question 35
A 28-year-old male sustains a thoracic spine injury.
Radiographs reveal a bony Chance fracture. Which of the following mechanisms of injury is most classically associated with this fracture pattern?

Explanation
Question 36
In a patient presenting with a traumatic spinal cord injury, the physical examination demonstrates a sensory level isolated to the nipple line. Which of the following dermatomal nerve root levels corresponds directly to this finding?
Explanation
Question 37
A 65-year-old male with a history of severe cervical spondylosis falls forward, striking his chin. He presents with severe weakness in his upper extremities but is able to move his lower extremities against gravity. What is the pathophysiological mechanism responsible for this specific neurological pattern?
Explanation
Question 38
A 40-year-old female presents with severe myelopathy and imaging confirms a large, central, calcified disc herniation at the T8-T9 level. Which of the following surgical approaches is explicitly contraindicated due to a high risk of iatrogenic neurological deterioration?
Explanation
Question 39
A 22-year-old male sustains a severe spinal cord injury. On examination, he has flaccid paralysis, absent reflexes below the level of injury, and absent perianal sensation. The bulbocavernosus reflex is absent. This clinical picture most accurately represents:
Explanation
Question 40
Which of the following vital sign patterns correctly distinguishes neurogenic shock from hypovolemic shock in a polytrauma patient?
Explanation
Question 41
A trauma patient presents with a cervical spine injury.
Imaging reveals bilateral fractures through the pars interarticularis of C2. Which of the following is the primary mechanism resulting in this specific injury?

Explanation
Question 42
Which of the following associated injuries has the highest incidence in patients diagnosed with a bony Chance fracture of the thoracolumbar junction?
Explanation
Question 43
A patient presents with a traumatic cervical spine injury.
A Type II odontoid fracture is identified. Which of the following factors contributes most significantly to the high nonunion rate of this specific fracture type?

Explanation
Question 44
A 35-year-old paraplegic male with a known complete spinal cord injury at T4 suddenly develops severe headache, profuse sweating above the nipple line, and profound hypertension (BP 210/110 mmHg). What is the most appropriate immediate intervention?
Explanation
Question 45
A cervical radiograph of a trauma patient demonstrates anterior translation of C5 over C6 by approximately 25% of the vertebral body width.
What is the most likely diagnosis?

Explanation
Question 46
According to the ASIA (American Spinal Injury Association) Impairment Scale, a patient who has preserved motor function below the neurological level, with more than half of the key muscles demonstrating a muscle grade less than 3, is classified as:
Explanation
Question 47
A 45-year-old male sustains a burst fracture of L1.
According to the Denis three-column theory, which structural failure differentiates a burst fracture from a simple compression fracture?

Explanation
Question 48
Which of the following clinical findings best differentiates a Conus Medullaris syndrome from a Cauda Equina syndrome?
Explanation
Question 49
During a left-sided transthoracic approach for a T10-T11 disc herniation, the surgeon is cautious of a major radiculomedullary artery that supplies the anterior lower two-thirds of the spinal cord. This artery typically arises from the left side between which spinal levels?
Explanation
Question 50
A patient with long-standing Ankylosing Spondylitis sustains a minor ground-level fall and complains of back pain. Which of the following statements regarding spinal fractures in this patient population is most accurate?
Explanation
Question 51
A 55-year-old male presents with clumsiness in his hands and frequent dropping of objects. On examination, he is unable to keep his small finger fully adducted (Wartenberg's sign positive) but his grip strength is intact. He exhibits hyperreflexia in the lower extremities. Which of the following is the most likely diagnosis?
Explanation
Question 52
A penetrating stab wound to the right side of the T8 spinal cord produces a Brown-Sequard syndrome. Which of the following clinical deficits will be observed?
Explanation
Question 53
A Jefferson fracture is defined as a burst fracture of the C1 ring. If the sum of the lateral mass displacement over the C2 articular facets on an open-mouth odontoid radiograph exceeds 7 mm, which critical structure is presumed completely disrupted?
Explanation
Question 54
A patient presents with a spinal cord injury following a severe trauma. Sensation is preserved below the level of injury including the S4-S5 dermatomes, but there is no voluntary motor function in the lower extremities. Anal sphincter tone is absent, but deep anal sensation is present. Which ASIA Impairment Scale (AIS) grade does this represent?
Explanation
Question 55
A 35-year-old male sustains a severe flexion-distraction injury to the T12 vertebra in a motor vehicle collision. Which of the following concurrent injuries is most likely to be present and requires urgent evaluation?
Explanation
Question 56
A patient with a traumatic spinal fracture is noted to have a sensory level localizing to the inguinal ligament. What is the corresponding nerve root level for this dermatome?
Explanation
Question 57
Which of the following is considered an absolute contraindication for a standard posterior laminectomy in the surgical management of a central, calcified thoracic disc herniation?
Explanation
Question 58
A 45-year-old male involved in a high-speed collision presents with paraplegia, loss of pain and temperature sensation in his lower extremities, but preserved vibration and proprioception. Which spinal cord syndrome does this describe?
Explanation
Question 59
Regarding the Thoracolumbar Injury Classification and Severity Score (TLICS), a patient presents with a T11-T12 burst fracture, indeterminate posterior ligamentous complex (PLC) status on MRI, and intact neurologic function. What is the total TLICS score and the recommended management?
Explanation
Question 60
A 28-year-old patient with a complete T4 spinal cord injury sustained 6 weeks ago suddenly develops a pounding headache, facial flushing, profuse sweating above the level of injury, and a blood pressure of 190/110 mmHg. Which of the following is the most appropriate initial management step?
Explanation
Question 61
A patient is diagnosed with spinal shock following severe trauma. Which of the following clinical signs marks the end of the spinal shock phase?

Explanation
Question 62
In a patient presenting with an acute traumatic spinal cord injury, which of the following MRI findings of the spinal cord is associated with the poorest prognosis for neurologic recovery?
Explanation
Question 63
What is the most common anatomical location for a symptomatic thoracic disc herniation?
Explanation
Question 64
A patient with a gunshot wound to the abdomen develops paraplegia. Imaging shows a bullet lodged in the T10 vertebral body with an associated incomplete neurologic deficit. CT scan shows bone fragments in the spinal canal. Which of the following is an absolute indication for surgical decompression and removal of the bullet in this scenario?
Explanation
Question 65
A patient sustains a complete spinal cord injury after a fall. Neurological examination reveals a sensory level at the nipple line. Which of the following nerve root levels indicates this finding?
Explanation
Question 66
A trauma patient presents with a complete spinal cord injury. Pinprick and light touch sensation are absent below the inguinal ligament. Which nerve root level does this specific landmark represent?
Explanation
Question 67
A patient with a T4 complete spinal cord injury suddenly develops a severe, pounding headache, profound diaphoresis above the level of injury, and severe hypertension. What is the most common precipitating cause of this condition?
Explanation
Question 68
An elderly patient with pre-existing cervical spondylosis presents after a hyperextension injury to the neck. Examination shows bilateral motor weakness that is much more pronounced in the upper extremities than the lower extremities. What is the most likely diagnosis?
Explanation
Question 69
A 25-year-old man sustains a stab wound to the right side of his thoracic spine. He presents with loss of motor function and proprioception in his right leg, and loss of pain and temperature sensation in his left leg. This clinical picture is most consistent with:
Explanation
Question 70
In the ASIA Impairment Scale, how is a patient classified if they have preserved motor function below the neurological level of injury, and more than half of the key muscle functions below that level have a muscle grade less than 3?
Explanation
Question 71
A patient presents with progressive myelopathy due to a large, calcified central thoracic disc herniation at T8-T9. Which of the following surgical approaches is generally CONTRAINDICATED due to the high risk of iatrogenic spinal cord injury?
Explanation
Question 72
According to the Denis three-column theory of spinal stability, a typical burst fracture of the thoracolumbar spine is characterized by failure of which columns?
Explanation
Question 73
Which of the following physical examination findings is the most reliable clinical indicator that a patient has emerged from the phase of spinal shock?
Explanation
Question 74
Which of the following incomplete spinal cord injury syndromes carries the worst prognosis for functional motor recovery?
Explanation
Question 75
A patient sustains a high-energy pelvic ring injury with a sacral fracture extending through the sacral foramina. According to the Denis classification of sacral fractures, which zone is involved and what is its associated feature?
Explanation
Question 76
A 12-year-old restrained passenger in a motor vehicle collision presents with a lap-belt injury. Radiographs show a fracture extending horizontally through the spinous process, pedicles, and vertebral body of L2. What associated injury must be specifically ruled out?
Explanation
Question 77
A 35-year-old sustains a Type II odontoid fracture with a reverse obliquity fracture line (sloping from anterior-inferior to posterior-superior). Which fixation method is contraindicated?
Explanation
Question 78
Which of the following is an established indication for emergent surgical decompression following a gunshot wound to the spine?
Explanation
Question 79
A 30-year-old presents with a unilateral jumped facet at C5-C6 following a hyperflexion-rotation injury. He is neurologically intact. Pre-reduction MRI demonstrates a large, uncontained C5-C6 disc herniation compressing the cord. What is the most appropriate management?
Explanation
Question 80
A 75-year-old woman presents with severe mid-back pain after a minor fall.
Radiographs show an anterior wedge compression fracture of T11 with 20% loss of height. Neurological examination is normal. What is the most appropriate initial management?

Explanation
Question 81
A 55-year-old diabetic male presents with worsening back pain, fever, and new-onset lower extremity weakness. Laboratory tests show elevated CRP and ESR. MRI with contrast reveals a rim-enhancing fluid collection in the dorsal epidural space. What is the most likely causative organism?
Explanation
Question 82
A patient arrives at the trauma bay after a high-speed motorcycle crash. He has flaccid paralysis below T2. His blood pressure is 80/50 mmHg, and his heart rate is 55 bpm. His extremities are warm and well-perfused. What is the primary pathophysiological mechanism for his hemodynamic state?
Explanation
Question 83
A lateral lumbar radiograph of a 14-year-old gymnast
shows forward slippage of L5 on S1 by 60%. According to the Meyerding classification, what grade of spondylolisthesis does this represent?

Explanation
Question 84
A 40-year-old man sustains an axial load injury to his head resulting in a Jefferson fracture. Open-mouth odontoid radiographs reveal lateral displacement of the lateral masses of C1 relative to C2. According to the Rule of Spence, what total combined overhang of the lateral masses strongly suggests incompetence of the transverse atlantal ligament?
Explanation
None
