Orthopedic Prometric MCQs - Chapter 3 Part 20
Orthopedic Prometric MCQs - Chapter 3 Part 20
Comprehensive 100-Question Exam
00:00
Start Quiz
Question 1
A 9-year-old girl sustains an injury (Slide) as a result of a fall. What is her risk of avascular necrosis:
Explanation

Question 2
A 9-year-old girl sustains an injury (Slide 1) as a result of a fall. What is the recommended treatment:
Explanation
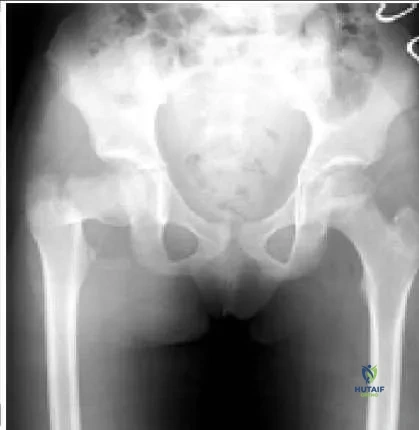 across the fracture site. C losed or open reduction and internal fixation with a compression screw fixation, preferably a hip screw, provide the best control of the fracture. A hip screw provides the best protection against the development of varus. If the fracture is not opened, then aspiration of the hematoma is recommended.
across the fracture site. C losed or open reduction and internal fixation with a compression screw fixation, preferably a hip screw, provide the best control of the fracture. A hip screw provides the best protection against the development of varus. If the fracture is not opened, then aspiration of the hematoma is recommended.
Question 3
A 6-year-old boy presents with a 3-month history of medial midfoot pain. Based on his radiograph (Slide), which of the following is the correct diagnosis:
Explanation
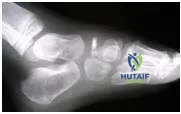 This child has avascular necrosis of the tarsal navicular. This is an idiopathic phenomenon more common in boys of this age than girls. The condition responds to rest and orthotics or cast immobilization. The navicular revascularizes over the ensuing year.
This child has avascular necrosis of the tarsal navicular. This is an idiopathic phenomenon more common in boys of this age than girls. The condition responds to rest and orthotics or cast immobilization. The navicular revascularizes over the ensuing year.
Question 4
Which of the following syndromes has the highest incidence of scoliosis as a percentage of affected patients:
Explanation
Question 5
Acute pain that presents in the lateral arm and shoulder is suggestive of:
Explanation
Question 6
A cervical disk herniation that causes weakness in the wrist extensors will likely produce sensory changes in the:
Explanation
Question 7
In order to diagnose a disk herniation, the preferred test is:
Explanation
Question 8
Initial management of cervical radiculopathy includes all of the following except:
Explanation
Question 9
This patient has a wide-based gait and hyper-reflexia in his lower extremities. His magnetic resonance image is presented. Other physical findings in this patient would likely include:
Explanation
Question 10
A useful test to differentiate cervical radiculopathy from diabetic peripheral neuropathy is:
Explanation
Question 11
With a left-sided anterior cervical spine approach, the structure at increased risk for injury is the:
Explanation
Question 12
With a right-sided anterior cervical spine approach, the structure at increased risk is the:
Explanation
Question 13
The structure most at risk during lateral mass screw placement is the:
Explanation
Question 14
After undergoing an anterior cervical discectomy and fusion through a left- sided neck incision, the patient is noted to have a drooping eyelid and a right pinpoint pupil. This is likely due to:
Explanation
Question 15
After an anterior cervical discectomy and fusion with autogenous iliac crest bone graft, the patient reports numbness in the lateral thigh. This is due to:
Explanation
Question 16
One advantage of posterior laminoforaminotomy in the treatment of cervical radiculopathy is:
Explanation
Question 17
The most frequently involved spinal segment in rheumatoid arthritis is:
Explanation
Question 18
The most useful measurement for predicting neurological deficit in rheumatoid arthritis involvement of the cervical spine is:
Explanation
Question 19
A relative contraindication to cervical laminectomy for the treatment of cervical spondylosis is:
Explanation
Question 20
The major risk factor for nonunion in a type 2 odontoid fracture is:
Explanation
Question 21
A 12-year-old obese boy presents with right hip and knee pain for 3 months. A radiograph is shown
. He is diagnosed with a stable slipped capital femoral epiphysis (SCFE). Which of the following is the most appropriate initial management?

Explanation
Question 22
An 8-year-old boy presents with a painless limp and restricted hip internal rotation. Radiographs demonstrate fragmentation of the capital femoral epiphysis with 60% involvement of the lateral pillar. According to the Herring Lateral Pillar Classification, which group does this represent?
Explanation
Question 23
A 4-week-old female infant is diagnosed with a dislocated but reducible left hip. Treatment with a Pavlik harness is initiated. Which of the following is an absolute contraindication to the continued use of a Pavlik harness?
Explanation
Question 24
A 4-year-old girl is evaluated for severe bowing of the left leg. Radiographs reveal varus deformity at the proximal tibia with a metaphyseal-diaphyseal angle (Drennan's angle) of 18 degrees. What is the most appropriate treatment?
Explanation
Question 25
A 6-year-old boy sustains a completely displaced, extension-type supracondylar humerus fracture. After closed reduction and percutaneous pinning with two lateral pins, you notice the anterior interosseous nerve (AIN) is non-functional. What is the most common physical finding of AIN palsy?
Explanation
Question 26
A 7-year-old boy presents with an established nonunion of a lateral condyle fracture of the humerus
that occurred 3 years ago. Which of the following nerve palsies is he at greatest risk of developing?

Explanation
Question 27
When treating an idiopathic clubfoot using the Ponseti method, what is the correct sequence of deformity correction?
Explanation
Question 28
A 12-year-old boy presents with recurrent ankle sprains and rigid flatfeet. A lateral radiograph of the foot reveals an "anteater nose" sign. Which of the following coalitions is most likely present?
Explanation
Question 29
A 3-year-old boy sustains an isolated midshaft femur fracture
. He is hemodynamically stable and has no other injuries. What is the preferred definitive treatment?

Explanation
Question 30
A 13-year-old girl sustains an ankle injury. Radiographs show a Salter-Harris III fracture of the anterolateral distal tibial epiphysis. What ligament is responsible for the avulsion of this bony fragment?
Explanation
Question 31
In a 6-year-old child with spastic quadriplegic cerebral palsy, routine hip surveillance radiographs show a Reimers migration index of 45%. Which of the following is the most appropriate management?
Explanation
Question 32
An 18-month-old child presents with a painless limp and is found to have an untreated developmental dysplasia of the hip (DDH) on the right side. Which of the following is the most appropriate treatment?
Explanation
Question 33
Which of the following pediatric physis injuries has the highest risk of premature physeal closure and subsequent growth arrest?
Explanation
Question 34
A 2-year-old boy presents with anterolateral bowing of the tibia and a radiographic pseudarthrosis
. This condition is most strongly associated with which of the following systemic disorders?
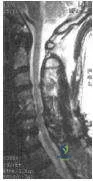
Explanation
Question 35
A 5-year-old boy presents with right hip pain, a limp, and a temperature of 38.8°C. He refuses to bear weight. His WBC is 13,000/mm³ and ESR is 45 mm/hr. According to the Kocher criteria, what is the probability that this child has septic arthritis rather than transient synovitis?
Explanation
Question 36
A 10-year-old boy presents after a high-energy fall. Radiographs demonstrate a displaced transcervical femoral neck fracture.
According to the Delbet classification, what is the approximate risk of avascular necrosis (AVN) for this fracture pattern?

Explanation
Question 37
A 6-year-old boy presents with medial midfoot pain and a limp for 2 months. Radiographs reveal sclerosis and flattening of the navicular bone. What is the most appropriate initial management?
Explanation
Question 38
Which of the following conditions is the strongest indication for prophylactic pinning of the contralateral asymptomatic hip in a patient presenting with a unilateral slipped capital femoral epiphysis (SCFE)?
Explanation
Question 39
When correcting an idiopathic clubfoot deformity using the Ponseti method, what is the proper sequence of deformity correction?
Explanation
Question 40
A 5-year-old boy sustains a completely displaced supracondylar humerus fracture. On examination, the hand is pink and well-perfused but the radial pulse is absent. What is the next best step in management?
Explanation
Question 41
A 4-year-old child presents with an elbow injury. Radiographs reveal a displaced lateral condyle fracture.
If this fracture goes on to nonunion, which of the following long-term complications is most likely to develop?

Explanation
Question 42
An infant with developmental dysplasia of the hip (DDH) is being treated with a Pavlik harness. During a follow-up visit, the infant is unable to actively extend the knee on the treated side. Which of the following harness adjustments was most likely flawed?
Explanation
Question 43
A 13-year-old girl sustains an ankle injury.
Radiographs reveal an avulsion fracture of the anterolateral distal tibial epiphysis. What is the typical pathomechanics of this fracture?

Explanation
Question 44
In Legg-Calve-Perthes disease, the Herring Lateral Pillar classification is most useful for predicting outcome. In a Group C classification, what percentage of the lateral pillar height is maintained?
Explanation
Question 45
A 2-year-old child presents with bilateral genu varum. A standing AP radiograph is obtained. Which radiographic parameter most strongly predicts the progression of infantile Blount disease rather than physiologic bowing?
Explanation
Question 46
A 10-year-old active boy complains of posterior heel pain that worsens with soccer practice. Examination reveals point tenderness at the insertion of the Achilles tendon on the calcaneal apophysis. Radiographs are unremarkable. What is the most appropriate initial treatment?
Explanation
Question 47
A 6-year-old child presents with a Bado Type I Monteggia fracture-dislocation. After closed reduction and casting, follow-up radiographs show re-dislocation of the radial head. What is the most common cause of failure to maintain radial head reduction in this scenario?
Explanation
Question 48
Osteogenesis imperfecta (OI) is primarily caused by mutations affecting which of the following structural proteins?
Explanation
Question 49
An infant with achondroplasia presents with hypotonia, sleep apnea, and hyperreflexia. Which of the following is the most likely underlying etiology?
Explanation
Question 50
A 14-year-old boy presents with a painful, rigid flatfoot and a history of recurrent ankle sprains.
Radiographs demonstrate a "C-sign" on the lateral view. Which of the following is the most likely diagnosis?

Explanation
Question 51
Congenital pseudarthrosis of the tibia (CPT) is most strongly associated with which of the following systemic conditions?
Explanation
Question 52
A 13-year-old obese boy presents with 3 weeks of vague left knee pain and a limp. Examination reveals an obligate external rotation of the hip during active flexion.
What is the most devastating potential complication of the underlying condition?

Explanation
Question 53
In a 7-year-old boy diagnosed with Legg-Calve-Perthes disease, which of the following radiographic findings is considered a 'head at risk' sign according to Catterall?
Explanation
Question 54
According to the Ponseti method for the treatment of idiopathic congenital talipes equinovarus (clubfoot), what is the correct sequence of deformity correction?
Explanation
Question 55
A 6-month-old girl is diagnosed with developmental dysplasia of the hip (DDH) and has failed a proper 3-week trial of a Pavlik harness, with the hip remaining dislocated. What is the most appropriate next step in management?
Explanation
Question 56
A 14-year-old boy sustains an ankle injury. Radiographs demonstrate a Salter-Harris III fracture of the anterolateral distal tibia.
Which ligament's avulsion force is responsible for this specific fracture pattern?

Explanation
Question 57
A 6-year-old girl sustains a severely displaced extension-type supracondylar humerus fracture. On presentation, her hand is well-perfused and pink, but the radial pulse is absent. What is the most appropriate initial management?
Explanation
Question 58
A 5-year-old boy sustains a lateral condyle fracture of the humerus.
If left untreated, leading to nonunion and progressive deformity, what late neurological complication is he at highest risk of developing?

Explanation
Question 59
A 7-year-old child with spastic quadriplegic cerebral palsy is undergoing routine hip surveillance.
What radiographic measurement is most critical for monitoring lateral hip subluxation in this patient?

Explanation
Question 60
A 3-year-old boy presents with a temperature of 38.8 C, refusal to bear weight on his right leg, an ESR of 55 mm/hr, and a serum WBC of 14,000/mm3 with suspected hip pathology. According to Kocher criteria, what is the statistical probability of septic arthritis?
Explanation
Question 61
A 2-year-old girl presents with bilateral genu varum. Radiographs reveal a metaphyseal-diaphyseal angle (Drennan's angle) of 18 degrees. What is the most likely diagnosis?
Explanation
Question 62
A 14-year-old boy presents with frequent ankle sprains and a rigid, painful flatfoot. Radiographs reveal a 'C sign' on the lateral view of the ankle. What is the most likely underlying diagnosis?
Explanation
Question 63
In which of the following patients presenting with a unilateral slipped capital femoral epiphysis (SCFE) is prophylactic pinning of the contralateral hip most strongly indicated?
Explanation
Question 64
A 13-year-old boy presents with vague anterior knee pain. Radiographs demonstrate an osteochondritis dissecans (OCD) lesion. What is the most common anatomic location for this lesion in the knee?
Explanation
Question 65
An 11-year-old gymnast sustains an elbow dislocation that is reduced in the emergency department. Subsequent radiographs show a medial epicondyle fracture. Which of the following is an absolute indication for operative fixation?
Explanation
Question 66
A 3-year-old boy weighing 14 kg sustains an isolated, closed, spiral midshaft femur fracture after a ground-level fall. Which of the following is the most appropriate definitive treatment?
Explanation
Question 67
Proximal focal femoral deficiency (PFFD) in a newborn is most frequently associated with which of the following concurrent congenital anomalies?
Explanation
Question 68
A 13-year-old girl sustains a twisting injury to her ankle. A CT scan confirms a classic triplane fracture. In which planes do the fracture lines of a typical triplane fracture occur?
Explanation
Question 69
A 2-year-old boy with anterolateral bowing of the tibia develops a spontaneous fracture. This condition (congenital pseudoarthrosis of the tibia) is most strongly associated with which of the following genetic disorders?
Explanation
Question 70
A 12-year-old elite baseball pitcher presents with insidious onset of proximal shoulder pain while throwing. Radiographs show widening and irregularity of the proximal humeral physis. What is the most appropriate initial treatment?
Explanation
Question 71
A 6-year-old girl is noted by her parents to have a painless, clunking sensation in her lateral knee with active flexion and extension. MRI confirms a complete, asymptomatic discoid lateral meniscus. What is the recommended management?
Explanation
Question 72
A 7-year-old boy is diagnosed with Legg-Calvé-Perthes disease. Which of the following describes the most critical prognostic factors for long-term hip deformity?
Explanation
None
