Tarsometatarsal Arthrodesis: An Intraoperative Masterclass for Midfoot Fusion
Key Takeaway
This masterclass guides fellows through tarsometatarsal (TMT) arthrodesis for midfoot arthrosis. We cover essential preoperative planning, patient positioning, and meticulous surgical execution from incision to closure. Detailed anatomical considerations, neurovascular protection, and crucial intraoperative pearls ensure optimal plantigrade foot reduction and stable fusion. Postoperative protocols for rehabilitation and complication management are also discussed.
Tarsometatarsal Arthrodesis: An Intraoperative Masterclass
Alright, fellows, welcome to the operating theater. Today, we're tackling a tarsometatarsal (TMT) arthrodesis, specifically focusing on the first, second, and third TMT joints. This is a crucial procedure for addressing symptomatic midfoot arthrosis, often arising from post-traumatic conditions or systemic inflammatory arthropathies. Our goal is to achieve a stable, plantigrade foot, restoring pain-free function and efficient gait.
Understanding the Foundation: Comprehensive Surgical Anatomy
Before we make any incisions, let's review the critical anatomy of the midfoot. Remember, the foot is a complex structure designed for both rigidity and flexibility.
- Medial Column (Rigid): Comprising the first ray (medial cuneiform and first metatarsal), second ray (intermediate cuneiform and second metatarsal), and third ray (lateral cuneiform and third metatarsal), this column is primarily responsible for rigidity and propulsion during push-off. The first, second, and third TMT joints naturally exhibit minimal motion.
- Lateral Column (Mobile): The fourth and fifth TMT joints, involving the cuboid and fourth/fifth metatarsals, are inherently more mobile, allowing for forefoot accommodation to uneven surfaces. This is why arthrosis in these joints is often managed with motion-preserving procedures, unlike the medial column where fusion is preferred.
Specific Joint Architecture:
* The first TMT joint is surprisingly deep, typically measuring 28 to 30 mm from dorsal to plantar. This depth is critical to remember during joint preparation to ensure complete cartilage removal.
* The second TMT joint is uniquely recessed proximally, like a keystone, between the medial and lateral cuneiforms. This anatomical arrangement contributes significantly to midfoot stability. Identifying this recess is key during dissection.
Neurovascular Structures – Our Primary Concern:
The dorsal aspect of the midfoot is notoriously thin on subcutaneous tissue, making neurovascular structures vulnerable.
* Deep Peroneal Nerve: This nerve runs deep to the extensor hallucis brevis (EHB) tendon, often accompanied by the dorsalis pedis artery, coursing towards the first web space. It provides sensation to the first web space and motor innervation to the EDB. Extreme caution is needed during dissection between the EHL and EHB.
* Dorsalis Pedis Artery: The continuation of the anterior tibial artery, it runs alongside the deep peroneal nerve. Damage can lead to significant bleeding or compromise distal perfusion.
* Dorsal Cutaneous Nerves: These are branches of the superficial peroneal nerve, providing sensation to the dorsum of the foot. They are highly variable and extremely superficial. Aggressive retraction or careless dissection can lead to painful neuromas or persistent sensory deficits.
* Extensor Hallucis Longus (EHL) and Extensor Hallucis Brevis (EHB): These tendons define the interval for our medial incision. The EHL is more medial, the EHB more lateral.
* Extensor Digitorum Brevis (EDB): This muscle belly is encountered during the lateral incision. It often needs to be split longitudinally rather than retracted to avoid excessive tension on superficial nerves.
Osteology & Ligamentous Attachments:
* Identify the medial, intermediate, and lateral cuneiforms.
* Understand the strong interosseous ligaments, particularly the Lisfranc ligament, which connects the medial cuneiform to the base of the second metatarsal. While we are not specifically addressing a Lisfranc injury, understanding this complex provides context for midfoot stability.
Preoperative Planning & Patient Positioning: Setting the Stage for Success
Fellows, meticulous planning is paramount. This isn't just about cutting bone; it's about restoring biomechanics.
1. Patient History and Physical Examination:
* We've already confirmed persistent, localized dorsal midfoot pain, exacerbated by motion, despite an adequate course of conservative management (NSAIDs, activity modification, stiff-soled shoes, orthotics, physiotherapy for equinus).
* Remember the Silfverskiöld test for equinus: Correct the hindfoot to neutral subtalar position, check dorsiflexion with the knee extended, then flexed 30 degrees. If dorsiflexion improves with knee flexion, it's an isolated gastrocnemius equinus, which we must address.
* Inspect for localized swelling and osteophytic formation over the TMT joints – a common finding due to the thin subcutaneous tissue.
* Rule out other pathologies: stress fractures, gout, ganglions, neuromas.
2. Imaging Studies:
* Weight-bearing radiographs (AP, lateral, oblique): These are our workhorses. We've scrutinized them for the extent of arthrosis, relative lengths of metatarsal heads, and foot alignment (talar-first metatarsal angle for cavus/planus). Ensure a true lateral with talar dome overlap.
* CT scan/MRI: Seldom needed unless we suspect a subtle Lisfranc injury or other complex pathology not evident on plain films.
* Fluoroscopically guided injection: If diagnostic uncertainty remains, a targeted injection into the suspected TMT joint is invaluable – both diagnostic and potentially therapeutic.
3. Operative Plan Templating:
* Based on the radiographs, we've templated our screw lengths and sizes. We're aiming for 3.5mm cortical screws for the first TMT and 3.0mm cannulated screws for the second and third TMTs, with the potential for washers on the cuneiforms due to softer bone. Compression staples will augment fixation.
* We've assessed for concomitant equinus and are prepared for a percutaneous Achilles tendon lengthening (TAL) or gastrocnemius slide if indicated. This is critical for preventing recurrence of deformity and reducing stress on the fusion site.
4. Patient Positioning:
* Supine on a radiolucent table: This allows unrestricted fluoroscopy access.
* Padded wedge under the ipsilateral hip: This corrects for external rotation of the limb, ensuring the foot is truly perpendicular to the floor, which is essential for accurate AP fluoroscopic views and proper anatomical alignment during surgery.
* Arm across the chest, ulnar nerve padded: Protect all pressure points.
* Tourniquet application: We'll apply a tourniquet to the thigh for this case. Why the thigh? Because we may harvest autograft from the proximal tibia, and a thigh tourniquet provides a bloodless field for both the foot and the donor site. If no autograft is planned, a calf tourniquet can suffice.
* Exsanguination: Use an Esmarch bandage to exsanguinate the limb thoroughly before inflating the tourniquet to 250-300 mmHg, or 100 mmHg above systolic pressure. This provides a clear, bloodless field, crucial for identifying delicate neurovascular structures.
Step-by-Step Intraoperative Execution: The Surgeon's Viewpoint
Alright, fellows, let's get scrubbed in. We've got our patient positioned, tourniquet inflated, and the field prepped and draped.
1. Incisions and Initial Exposure
We're going to use two well-spaced longitudinal incisions to maximize our skin bridge and minimize the risk of wound complications.
-
Medial Incision (First and Medial Second TMT Joints):
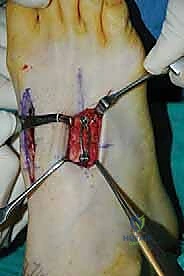
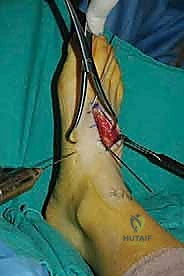
- "Fellows, let's make our first incision. It's a 4-cm longitudinal incision, centered over the lateral third of the first TMT joint. This incision runs roughly between the extensor hallucis longus (EHL) and the extensor hallucis brevis (EHB) tendons. Visualize that interval."
- "Carefully deepen your dissection through the subcutaneous tissue. Remember, the dorsal cutaneous nerves are extremely superficial here. Use a sharp scalpel initially, then switch to blunt dissection with Metzenbaum scissors or a small hemostat. We want to avoid any aggressive retraction on the skin edges."
- "Now, identify the EHL tendon medially and the EHB tendon laterally. We're working in this interval. As we deepen, be vigilant for the deep peroneal nerve and the dorsalis pedis artery. They lie just deep to the medial aspect of the EHB tendon, coursing towards the first web space. Gently retract these structures medially with a small Hohmann or a blunt army-navy retractor. Never use sharp retractors here."
- "Once we've identified and protected these vital structures, we can identify the capsule of the first TMT joint. You can often feel the joint line by gently mobilizing the first metatarsal. Incise the capsule transversely, in line with the joint. This minimizes periosteal stripping, which can compromise blood supply to the fusion site."
- "Now, carefully dissect proximally between the first and second metatarsal bases to expose the medial aspect of the second TMT joint. Remember, the second TMT joint is recessed more proximally relative to the first."
-
Lateral Incision (Lateral Second and Third TMT Joints):
- "Next, let's make our second incision. This is another 4-cm longitudinal incision, centered directly over the third TMT joint."
- "Again, deepen carefully through the subcutaneous tissue, being mindful of the dorsal cutaneous nerves. These are even more prevalent laterally. Blunt dissection is your friend here."
- "You'll encounter the extensor digitorum brevis (EDB) muscle belly. Typically, we cannot simply retract the EDB plantar without causing undue tension on the neurovascular structures or the muscle itself. Therefore, we will split the EDB longitudinally, directly in line with our skin incision. This provides excellent exposure without excessive soft tissue trauma."
- "Once the EDB is split, identify the capsule of the third TMT joint. Again, split the periosteum and capsule in line with the joint to avoid excessive stripping."
- "Through this incision, we can also expose the lateral aspect of the second TMT joint and the space between the second and third metatarsal bases."
2. Joint Preparation for Arthrodesis
This is a critical step, fellows. Inadequate joint preparation is a primary cause of nonunion. We need to create a robust, bleeding bone-on-bone interface.
-
First TMT Joint Preparation:
- "Let's start with the first TMT joint. We need to denude all joint surfaces of cartilage. Use a combination of instruments: an AO elevator to peel off superficial cartilage, a quarter-inch osteotome for more stubborn areas, straight and curved curettes to reach into concave surfaces, and a rongeur for bulk debridement."
- "CRITICAL POINT: Remember the depth of the first TMT joint – 28 to 30 mm. It is absolutely imperative to remove cartilage all the way down to the plantar aspect of the joint. Failure to do so will leave a cartilaginous hinge, preventing complete compression and often leading to persistent dorsiflexion of the first ray and nonunion. Use your curved curettes to ensure you've reached the very plantar-most recess."
- "Once all cartilage is removed, we want to optimize surface area and blood flow. Use a 2.0-mm drill bit to create multiple perforations, or 'fish-scaling,' across the entire arthrodesis surfaces of both the medial cuneiform and the first metatarsal base. This promotes vascular ingrowth and enhances the biological environment for fusion."
- "A lamina spreader can be helpful here to distract the joint slightly, giving you better visualization for thorough debridement and drilling."
-
Second and Third TMT Joint Preparation:
- "Now, we'll prepare the second and third TMT joints in a similar meticulous fashion. Denude all cartilage from the articulating surfaces of the second metatarsal base, the intermediate cuneiform, the third metatarsal base, and the lateral cuneiform."
- "Again, use your AO elevator, osteotomes, curettes, and rongeurs. Pay particular attention to the recessed nature of the second TMT joint. Ensure complete cartilage removal from its proximal and lateral aspects."
- "Once denuded, perform the same 'fish-scaling' technique with the 2.0-mm drill bit to create perforations across all fusion surfaces, maximizing bone-to-bone contact and promoting blood supply."
3. Temporary Stabilization: Achieving Plantigrade Alignment
Before we commit to definitive hardware, we must ensure our reduction is perfect and the foot is in a truly plantigrade position. This is where your surgical eye and tactile feedback are critical.
- "First, release any retractors and hold the foot in a reduced position. Now, palpate the forefoot. Gently press on the metatarsal heads. Ensure they are all level and the forefoot is in a plantigrade position, not dorsiflexed or plantarflexed, and without any pronation or supination."
-
"We'll use Kirschner wires (K-wires) and guide pins for temporary stabilization."
-
First TMT Joint Temporary Fixation:
- "Let's make a small stab incision over the medial aspect of the medial cuneiform, just through the skin. Use a small hemostat to dissect down to bone, carefully retracting the tibialis anterior tendon."
- "Now, we'll place our first 0.062 Kirschner wire. Aim it from the dorsal-medial aspect of the medial cuneiform, angling distally and slightly plantar, into the plantar aspect of the first metatarsal base. This K-wire should be placed where one of our final screws will go."
- "Next, place a second 0.062 K-wire. This one goes from the dorsal aspect of the first metatarsal shaft, angling proximally and slightly plantar, into the plantar aspect of the medial cuneiform. These two crossed K-wires will hold the first TMT joint securely in its reduced position."
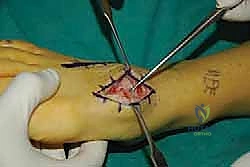
* "Once these are in, check your fluoroscopy. AP, lateral, and oblique views. Confirm good reduction and alignment of the first ray."
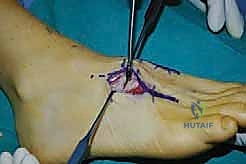
- Second TMT Joint Temporary Fixation:
- "Now, let's stabilize the second metatarsal. We'll use a guide pin from our 3.0-mm cannulated screw set for this. Make a small stab incision dorsally, protecting the tibialis anterior tendon."
- "Reduce the second metatarsal to the intermediate cuneiform and ensure it's aligned with the first metatarsal base. Again, palpate the metatarsal heads to confirm they are level and plantigrade."
- "Aim the guide pin from the base of the second metatarsal, angling proximally and slightly medially, into the intermediate cuneiform. This provides axial compression and alignment."
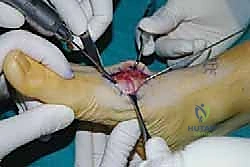
- Third TMT Joint Temporary Fixation:
- "Finally, for the third metatarsal, make a stab incision on the lateral forefoot. Insert another guide pin from the 3.0-mm cannulated screw set."
- "Reduce the third metatarsal to the lateral cuneiform, ensuring it's in a plantigrade position relative to the second metatarsal. Aim the guide pin from the base of the third metatarsal into the lateral cuneiform."
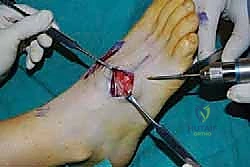
- Final Fluoroscopic Check:
- "Before we proceed to definitive fixation, let's get a full set of intraoperative fluoroscopy images: AP, lateral, and oblique. We need to ensure adequate reduction and opposition of all arthrodesis surfaces, and that our temporary wires are in good position. Look for any gapping or malalignment. Are all metatarsal heads level on the lateral view? Is the alignment restored on the AP?"
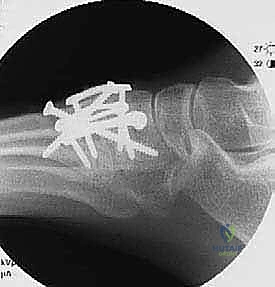
- "Before we proceed to definitive fixation, let's get a full set of intraoperative fluoroscopy images: AP, lateral, and oblique. We need to ensure adequate reduction and opposition of all arthrodesis surfaces, and that our temporary wires are in good position. Look for any gapping or malalignment. Are all metatarsal heads level on the lateral view? Is the alignment restored on the AP?"
4. Definitive Stabilization: Lag Screws and Compression Staples
Once we are absolutely satisfied with our temporary reduction and alignment, we'll proceed to definitive fixation. The principle here is rigid internal fixation to achieve compression across the fusion sites.
-
First TMT Joint Definitive Stabilization:
- "We'll start with the first TMT joint. Take a 3.5-mm drill sleeve and place it over the more dorsal 0.062 K-wire (the one from the medial cuneiform to the first metatarsal). Use cautery to mark the angulation of this wire on the bone. This helps us maintain the trajectory."
- "Carefully back out the 0.062 K-wire, ensuring the drill sleeve remains fixed in position. Now, using the 3.5-mm drill bit, drill through the near cortex of the medial cuneiform. Then, switch to a 2.5-mm drill bit to create the pilot hole in the far cortex of the first metatarsal. This differential drilling creates a lag effect."
- "Measure your screw length. Countersink the screw head to prevent prominence and soft tissue irritation. Now, insert a 3.5-mm cortical screw in a lag manner. Feel that compression as it bites into the far cortex. That's what we want."
- "Repeat these steps for the second screw, which goes from the first metatarsal to the medial cuneiform. Place a 3.5-mm drill sleeve over the K-wire, mark the trajectory, remove the K-wire, drill with 3.5mm through the near cortex (first metatarsal) and 2.5mm through the far cortex (medial cuneiform), measure, countersink, and insert the 3.5-mm cortical lag screw."
- "Confirm placement and compression with fluoroscopy."
-
Second and Third TMT Joints Definitive Stabilization:
- "Now, let's move to the second metatarsal. We'll use our cannulated system here. Drill over the guide pin with the appropriate cannulated drill bit for our 3.0-mm cannulated screw. Remember to protect the tibialis anterior tendon during this entire process."
- "Once the pilot hole is drilled, measure your screw length. The bone of the cuneiforms can be softer, so be prepared to use a washer under the screw head if needed to prevent pull-through. Insert the 3.0-mm cannulated lag screw, achieving good compression."
- "Repeat this similar technique for the third metatarsal. Drill over the guide pin with the cannulated drill, measure, and insert the 3.0-mm cannulated lag screw from the third metatarsal into the lateral cuneiform."
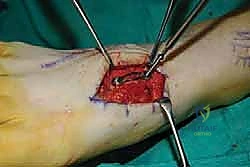
- "To further enhance stability and compression, we will now place compression staples. For the third TMT joint, we'll place a compression staple dorsally, spanning the fusion site."
* "And for the second TMT joint, another compression staple dorsally, spanning the fusion site between the second metatarsal and the intermediate cuneiform. This adds robust, broad-surface compression, particularly helpful in the midfoot."
5. Bone Grafting
Once our definitive fixation is in place and verified, we'll augment the fusion with bone graft.
- "We will apply bone graft to the dorsal surfaces of all arthrodesis sites. This provides osteoconductive scaffold and, if autograft or certain allografts are used, osteoinductive properties."
- "For this case, we're using cancellous allograft mixed with a platelet-rich derivative. This combination promotes both osteoconduction (a scaffold for new bone growth) and osteoinduction (signaling for bone formation)."
- "If autograft were needed, we could harvest it from the calcaneus, proximal or distal tibia, or iliac crest, which is why we had the thigh tourniquet in place."
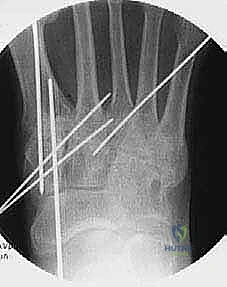
6. Intraoperative Fluoroscopy: Final Verification
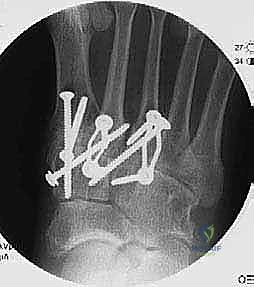
- "Alright, fellows, one last set of comprehensive fluoroscopy images. We need AP, lateral, and oblique views. This is our final check to ensure adequate reduction, excellent opposition of arthrodesis surfaces, and appropriate hardware positioning. Confirm no hardware prominence, no gapping at the fusion sites, and that our plantigrade alignment is perfectly maintained."
7. Wound Closure
With fixation confirmed, we'll proceed with meticulous wound closure.
- "First, let's deflate the tourniquet. Apply direct pressure to the wounds to achieve hemostasis. Any bleeders should be meticulously coagulated."
- "We'll reapproximate the capsule over the TMT joints with an absorbable suture, typically 2-0 or 3-0 Vicryl. This helps to reinforce the fusion and provides a layer of soft tissue coverage."
- "Next, reapproximate the subcutaneous tissue with interrupted, buried absorbable sutures (e.g., 3-0 Vicryl). This eliminates dead space and takes tension off the skin."
- "Given the potential for swelling in the foot, we will insert a small drain to prevent postoperative hematoma formation, particularly if there was significant soft tissue dissection or bleeding."
- "Finally, close the skin with horizontal or vertical mattress nylon sutures. The key here is minimal tension. Remember the thin subcutaneous tissue. Aggressive skin retraction or tension during closure can lead to wound dehiscence or necrosis. We want everted skin edges for optimal healing."
- "Apply a sterile dressing and a well-padded splint to protect the foot."
💡 Pearls and Pitfalls: Navigating Challenges
Fellows, every surgery has its potential pitfalls. Knowing them and how to avoid or manage them is the mark of a master surgeon.
Failure to resect plantar aspect of the first TMT joint:
* Pitfall: This is a cardinal sin. Leaving a cartilaginous hinge on the plantar aspect of the joint prevents true compression and leads to persistent dorsiflexion of the first ray. This often results in a painful nonunion and a functionally poor outcome.
* Pearl: Always use curved curettes and an osteotome to meticulously debride the entire joint surface, especially the plantar aspect. Visualize the depth (28-30mm) and ensure you feel bone-on-bone contact from dorsal to plantar. Fluoroscopy can sometimes help confirm the extent of debridement.Prominent first, second, or third metatarsal heads:
* Pitfall: This indicates malreduction in the sagittal plane – typically dorsiflexion of the metatarsal. This can lead to transfer metatarsalgia, painful callosities, and gait abnormalities.
* Pearl: During temporary stabilization, always palpate the metatarsal heads to ensure they are level and plantigrade. Use fluoroscopy (true lateral view) to confirm. If a metatarsal head is prominent, adjust your reduction and K-wire placement before definitive fixation.Failure to hold the metatarsals in a plantigrade position before definitive stabilization:
* Pitfall: Similar to the above, this results in malunion and functional impairment. The entire forefoot must be aligned correctly relative to the hindfoot.
* Pearl: This is why temporary K-wire fixation is so critical. Take your time. Release tension, manipulate the foot, palpate, and use fluoroscopy until you are absolutely certain of the plantigrade position. Don't rush this step.Nonunion:
* Pitfall: The ultimate failure of arthrodesis, leading to persistent pain and requiring revision surgery.
* Pearl: Prevent nonunion by ensuring:
* Thorough joint preparation: Meticulous cartilage removal and robust subchondral drilling for bleeding bone.
* Rigid internal fixation: Adequate number and type of screws/staples providing compression.
* Appropriate bone graft: To enhance biological healing.
* Optimal patient factors: Managing comorbidities like diabetes or smoking preoperatively.
* Salvage: If nonunion occurs, revision typically involves re-debridement of the nonunion site, often with decortication, fresh bone grafting (autograft preferred), and potentially more robust or different fixation constructs (e.g., plates).Inadequate joint preparation or inadequate fixation:
* Pitfall: Direct causes of nonunion and/or loss of reduction.
* Pearl: See nonunion pearls above. Never compromise on these fundamental surgical principles.Lack of bone graft:
* Pitfall: While some fusions can heal without graft, it significantly improves the chances of successful fusion, especially in challenging cases or revision settings.
* Pearl: Always use some form of bone graft (autograft, allograft, or bone graft substitute) to augment the fusion site.Wound complication (dehiscence, infection, necrosis):
* Pitfall: Common on the dorsum of the foot due to thin soft tissue. Can lead to delayed healing, infection, and hardware exposure.
* Pearl:
* Poor soft tissue handling: Be gentle. Use skin hooks or blunt retractors. Avoid aggressive skin retraction; retract deeper tissues.
* Excessive skin retraction: This stretches and devitalizes the skin. Use well-spaced incisions and careful deep dissection.
* Poor incision placement: Incisions should be longitudinal and well-spaced, avoiding areas of high tension or crossing neurovascular structures.
* Hematoma: Meticulous hemostasis and judicious use of drains.
* Closure: Close with minimal tension.
* Salvage: Minor dehiscence may heal with local wound care. Significant dehiscence or necrosis may require debridement, negative pressure wound therapy, or even local or free flap coverage. Deep infection requires aggressive debridement, IV antibiotics, and potentially hardware removal.Neuroma of the superficial or deep peroneal nerve:
* Pitfall: Persistent, debilitating pain from nerve entrapment or injury.
* Pearl: Meticulous identification and protection of all dorsal cutaneous nerves, the deep peroneal nerve, and the dorsalis pedis artery. Blunt dissection is key. Avoid electrocautery directly on or near nerves.
Postoperative Care and Complication Management
Our job doesn't end when the patient leaves the OR, fellows. Meticulous postoperative care is crucial for successful fusion.
1. Immediate Postoperative Period (0-2 weeks):
* Immobilization: The foot will be placed in a well-padded short leg splint or a non-weight-bearing cast immediately post-op. This protects the fusion sites.
* Elevation: Strict elevation of the limb above heart level is mandatory for the first 5-7 days to minimize swelling and promote wound healing.
* Weight-Bearing: Strictly non-weight-bearing on the
REFERENCES
References
- A Well-Molded Below-Knee Posterior Splint Is Applied With Toes Exposed.
-
Analgesic control is optimal with a local or regional anesthetic in addition to oral narcotics.
-
The patient is mobilized on a knee scooter, non–weightbearing.
-
Progressive weight bearing is permitted between 6 and 12 weeks in a removable boot.
-
The patient is weaned out of the removable boot into standard shoes at 12 weeks.
OUTCOMES
- Relatively little is published on outcomes of midfoot arthrodesis.
-
With appropriate surgical indications, surgical technique, and patient compliance, patient satisfaction rates exceed 90%.
-
Hansen ST. Functional Reconstruction of the Foot and Ankle. Philadelphia: Lippincott Williams & Wilkins, 2000:332–334.
-
Johnson JE, Johnson KA. Dowel arthrodesis for degenerative arthrodesis of the tarsometatarsal (Lisfranc) joints. Foot Ankle 1986;5:243–253.
-
Komenda GA, Myerson MS, Biddinger KR. Results of arthrodesis of the tarsometatarsal joints after traumatic injury. J Bone Joint Surg Am 1996;78A:1665–1676.
-
Mann RA, Prieskorn D, Sobel M. Mid-tarsal arthrodesis for primary degenerative osteoarthrosis or osteoarthrosis after trauma. J Bone Joint Surg Am 1996;78A:1376–1385.
-
Sangeorzan BJ, Veith R, Hansen ST. Fusion of Lisfranc’s joint for salvage of tarsometatarsal injuries. Foot Ankle 1990;10: 193–200.
-
Vertullo CJ, Easley ME, Nunley JA. The transverse dorsal approach to the Lisfranc joint. Foot Ankle Int 2002;23:420–426.

You Might Also Like