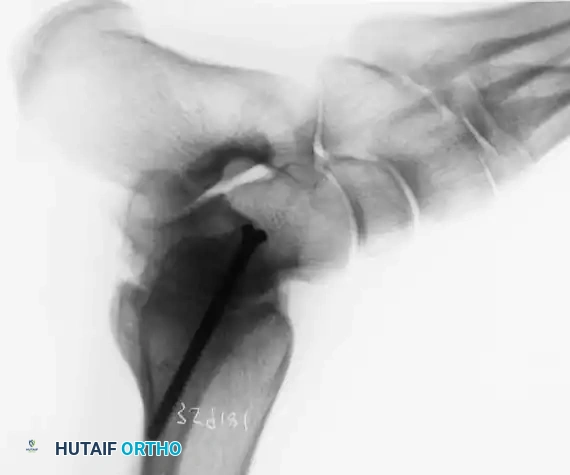
Revision First Metatarsophalangeal Joint Arthrodesis: An Intraoperative Masterclass
Key Takeaway
Join us in the OR for an immersive masterclass on revision first MTPJ arthrodesis. We meticulously cover patient selection, comprehensive surgical anatomy, precise intraoperative techniques for various failure patterns, including bone grafting, and detailed postoperative care. Learn critical pearls and pitfalls to ensure successful outcomes in these challenging cases, restoring a stable, pain-free medial column.
Fellows, welcome to the operating theater. Today, we're tackling a challenging, yet incredibly rewarding procedure: Revision First Metatarsophalangeal Joint (MTPJ) Arthrodesis. This isn't just about fusing a joint; it's about restoring function, alleviating chronic pain, and correcting complex deformities that have often plagued our patients for years following previous failed surgeries. Our goal is to create a painless, solid medial column, appropriate in length, that provides a stable medial arch and a plantigrade foot, preventing painful load transfer to the lesser rays.
Defining the Challenge: Why Revision?
Revision first MTPJ arthrodesis is indicated for persistent pain or significant deformity after a trial of conservative management has failed. This can stem from several scenarios:
- Failed Hallux Valgus Surgery: This might present as recurrent valgus deformity, avascular necrosis (AVN) of the metatarsal head, or accelerated degeneration of the first MTPJ leading to pain and stiffness.
- Excisional Arthroplasty (e.g., Keller-Brandes): Often results in recurrent valgus, a "cock-up" deformity, or a flail toe. These cases frequently involve significant bone loss.

FIG 1 • A failed Keller’s resection arthroplasty.
* Prosthetic Arthroplasty (e.g., Silastic implant): Can lead to an aggressive foreign body reaction, causing substantial bone loss on one or both sides of the joint, depending on the implant type.
* Nonunion or Malunion of Primary First MTPJ Arthrodesis:
* Nonunion: Persistent pain and instability at the fusion site.
* Malunion: A fusion that is either too straight (leading to a painful callus under the proximal phalanx condyles) or too dorsiflexed (causing a painful callus on the dorsum of the IP joint).
Comprehensive Surgical Anatomy: Navigating Disrupted Terrain
In revision surgery, we must always anticipate severely disrupted normal anatomy. Previous incisions, scar tissue, and bone resections can significantly alter tissue planes and obscure vital structures.
Osteology and Joint Mechanics:
The first MTPJ is a critical component of the foot's medial column, essential for propulsion during gait. Its proper alignment and stability are paramount. We must assess the integrity of the first metatarsal length, the viability of the metatarsal head (especially for AVN), and the bone stock of the proximal phalanx. The relationship between the IP joint, MTPJ, and first Tarsometatarsal (TMT) joint must be thoroughly evaluated. Degeneration of the first TMT or IP joints can be a relative contraindication, as fusion of the MTPJ may transfer stress to these adjacent joints.
Neurovascular Structures:
The dorsal aspect of the foot, where we operate, is rich in delicate neurovascular structures.
* Dorsal Cutaneous Nerve (Medial Dorsal Cutaneous Nerve): A branch of the superficial peroneal nerve, this nerve runs along the dorsomedial aspect of the foot, often crossing our incision path. Injury can lead to painful neuromas or troublesome paresthesias.
* Terminal Branch of the Deep Peroneal Nerve: Located in the first web space, this nerve supplies sensation to the adjacent sides of the first and second toes and innervates the extensor digitorum brevis. It is vulnerable during deep dissection in the first web space.
* Extensor Hallucis Longus (EHL) Tendon: This prominent tendon lies just lateral to our ideal incision line. It must be carefully retracted, usually laterally, to expose the joint. Excessive or prolonged retraction can cause tendonitis or even rupture.
* Dorsalis Pedis Artery and its Branches: While typically deeper, smaller dorsal metatarsal arteries and their branches can be encountered and must be protected or meticulously ligated if necessary.
Muscular Intervals and Soft Tissues:
Previous surgery often creates dense scar tissue, obliterating normal fascial planes. We must be prepared to raise full-thickness flaps off the metatarsus and proximal phalanx with extreme care. This meticulous technique minimizes damage to the already compromised soft tissue envelope and protects the underlying neurovascular structures.
Surgical Warning: Always assume altered anatomy in revision cases. Identify and protect the dorsal cutaneous nerve and the terminal branch of the deep peroneal nerve. Handle all tissues gently to preserve vascularity, especially in scarred fields.
Preoperative Planning: Laying the Foundation for Success
Successful revision arthrodesis hinges on meticulous preoperative planning.
Patient History and Physical Findings:
A thorough history is paramount. Document any history of cigarette smoking, as this significantly increases the risk of nonunion. Assess peripheral circulation and sensation thoroughly. Note the age and exact site of previous surgical scars to plan the safest approach, ideally incorporating existing incisions.
Imaging and Diagnostic Studies:
* Weight-Bearing AP and Lateral Radiographs: These are essential. We need to assess the extent of bone loss from the proximal phalanx and metatarsal head. An oblique radiograph can often provide additional detail regarding bone stock. Pay close attention to the alignment of the first TMTJ and IP joint, as well as any existing lesser toe deformities.
* Templating: Use preoperative radiographs to template potential graft sizes and hardware. This helps anticipate the need for bone graft and select the appropriate plate length.
* MRI: If avascular necrosis (AVN) of the metatarsal head is suspected, an MRI can be invaluable, provided the patient has no metallic implants.
* Infection Rule-Out: If infection is suspected, it must be definitively ruled out preoperatively. Obtain a differential white cell count, C-reactive protein (CRP) level, and erythrocyte sedimentation rate (ESR). An isotope bone scan can be helpful, but remember it can be "hot" for both nonunion and infection, so clinical correlation and laboratory values are crucial.
* Rheumatology/Anesthetic Consultation: Arrange these as needed, especially for patients with systemic conditions or complex medical histories.
Addressing Coexisting Forefoot Pathology:
This is a critical step. Any lesser toe deformities must be addressed before setting the final hallux position. Correcting these first allows us to set the hallux at the correct valgus angle relative to its neighbors, preventing painful transfer lesions. Common procedures include:
* Proximal interphalangeal joint (PIP) arthrodesis for clawed or hammered toes.
* MTPJ capsulotomy.
* Extensor digitorum longus (EDL) lengthening.
* Plantar condylectomy.
* Weil's osteotomies for metatarsalgia.
Surgical Warning: When performing Weil's osteotomies for transfer metatarsalgia, never perform a Weil's osteotomy of the second metatarsal head in isolation. An osteotomy of the third metatarsal head must accompany it to prevent transfer metatarsalgia to the third metatarsal head.
Bone Graft Planning:
The extent of bone loss dictates the need for bone graft. We prefer to harvest autogenous iliac crest bone graft from the ipsilateral crest to limit postoperative disability to one side only. This will be prepared and draped as a separate field.
Patient Positioning and Setup: The OR Environment
Fellows, let's discuss our setup.
1. Patient Position: The patient is positioned supine on the operating table.
2. Table Configuration: The heels are placed at the very end of the operating table. The end of the table is then dropped 20 to 30 degrees, allowing the surgeon to sit comfortably at the end of the table, optimizing ergonomics and visualization.
3. Iliac Crest Graft Setup: If bone graft is required, a sandbag is placed under the ipsilateral buttock to facilitate access to the iliac crest.
4. Tourniquet: A thigh tourniquet is applied.
5. Prophylaxis: Prophylactic intravenous antibiotics are administered at the induction of anesthesia.
6. Exsanguination: The limb is exsanguinated prior to tourniquet inflation.
7. Preparation and Draping: The iliac crest (if harvested) and the entire leg are meticulously prepared and draped in a routine sterile manner, ensuring a wide sterile field.
8. Fluoroscopy: The C-arm should be positioned and draped for easy intraoperative access, allowing for AP, lateral, and oblique views of the forefoot to confirm alignment and hardware placement.
Step-by-Step Intraoperative Execution: The Surgeon's Viewpoint
Alright, fellows, let's begin. We've completed our preoperative checks and the patient is positioned.
I. Surgical Approach and Exposure
-
Incision: I will make a dorsal, slightly curved incision, ideally incorporating any previous dorsal scars. This incision is meticulously placed just medial to the extensor hallucis longus (EHL) tendon and lateral to the dorsal cutaneous nerve. It extends from the middle of the shaft of the first metatarsal distally to the interphalangeal (IP) joint.
> Surgical Warning: Always identify and protect the dorsal cutaneous nerve. Dissect carefully through the subcutaneous tissue to avoid inadvertent injury. -
Soft Tissue Dissection: We'll now raise full-thickness flaps off the metatarsus and proximal phalanx. This is a critical step in revision surgery due to dense scarring. Use a fine scalpel and careful blunt dissection.
> Surgical Warning: Handle the tissues with utmost care. Self-retaining retractors should be positioned under low tension for only short periods to prevent skin necrosis or nerve compression, especially if the hallux is held in forced plantarflexion. Avoid excessive retraction with bone levers. -
EHL Tendon Retraction: The EHL tendon is identified and gently retracted laterally to expose the joint capsule.
-
Capsulotomy and Joint Exposure: A capsulotomy is made in the same plane as our skin incision, exposing the MTPJ. Any previous metalwork or implants are now identified and meticulously removed.
-
Synovectomy and Debridement: A thorough synovectomy is performed, and any avascular bone or necrotic tissue is sharply excised until healthy, bleeding bone is encountered.
-
Soft Tissue Release: The medial and lateral soft tissues around the joint are released. This is crucial to allow maximum plantarflexion of the proximal phalanx, which will provide optimal exposure of both surfaces to be arthrodesed and facilitate proper positioning later.
II. Preparation of the Distal First Metatarsal and Proximal Phalanx
The technique for joint preparation varies significantly based on the nature of the previous failure and the extent of bone loss.
A. Revision of Nonunion, Failed Hallux Valgus Surgery, or Failed Excision Arthroplasty (with minimal resection of the proximal phalanx):
In these cases, where bone graft is generally not required, we aim for a ball-and-socket preparation to maximize cancellous contact.
1. Osteophyte Excision: First, any remaining osteophytes around the joint are carefully excised with an osteotome or rongeur.
2. Proximal Phalanx Reaming: We will size the proximal phalanx to determine the correct convex reamer. A 1.6-mm guidewire is then passed centrally through the proximal phalanx. Over this guidewire, the articular surface of the proximal phalanx is reamed with the appropriate convex reamer.
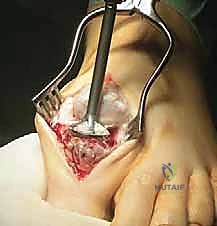
TECH FIG 1 • A . Reaming the articular surface of the proximal phalanx.
3. Metatarsal Head Reaming: A size-matched concave reamer is then used to prepare the metatarsal head in a similar manner, ensuring a congruent fit with the reamed phalanx.
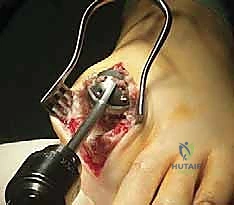
TECH FIG 1 • B. Reaming the articular surface of the metatarsal head.
B. Revision of Malunion of Primary Arthrodesis:
These cases are revised because the hallux is either excessively dorsiflexed or plantarflexed.
1. Closing Wedge Osteotomy: A simple closing wedge osteotomy is performed with flat cuts, with the apex of the wedge at the original arthrodesis site. This allows us to correct the sagittal plane deformity without significantly shortening the ray. We use an oscillating saw for precise cuts.
C. Complex Revision Cases (Significant Bone Stock Deficit):
When the first ray is short and defunctioned due to substantial bone loss, a graft is essential.
- Revision for Failed Excision Arthroplasty (Large Resection of Proximal Phalanx):
- Metatarsal Resection: Using an oscillating saw, bone from the distal first metatarsal is resected back to healthy, vascular cancellous bone. To ensure proper alignment, a flat surface is placed against the sole of the foot, and the osteotomy is performed in the coronal plane and in the sagittal plane, at 90 degrees to this flat surface.
- Proximal Phalanx Resection: Bone from the proximal phalanx is similarly resected back to vascular cancellous bone, perpendicular to its long axis.
- Gap Measurement: The hallux is held in an estimated best functional position. The gap between the flat surfaces of the proximal phalanx and metatarsal head is carefully measured.
- Tricortical Iliac Crest Graft Harvest: A precisely sized tricortical iliac crest bone graft is harvested from the ipsilateral crest in a standard fashion. We aim for a graft that will restore appropriate length and alignment.
- Trough Creation and Graft Insertion: A trough is cut out of the dorsum of each bone (metatarsal and phalanx) to accept the tricortical graft. The appropriately sized tricortical graft is then inserted into this trough, bridging the defect. The remaining defect around the graft is then packed with additional cancellous graft harvested from the iliac crest.
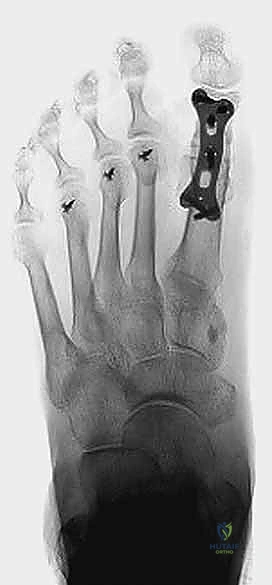
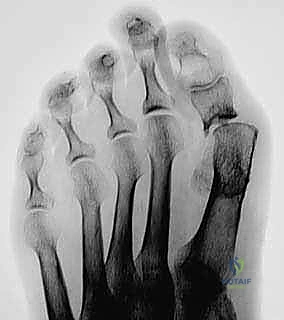
FIG 2 • A. AP radiograph following revision arthrodesis with tricortical iliac crest graft for failed excision arthroplasty.
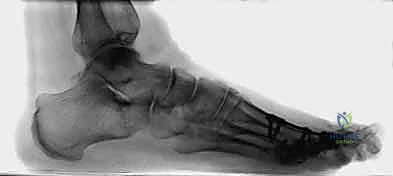
FIG 2 • B . Lateral radiograph following revision arthrodesis with tricortical iliac.
-
Revision for Avascular Necrosis (AVN) Following Hallux Valgus Surgery:
- The distal first metatarsal and proximal phalanx are prepared as previously described, excising all necrotic bone. The goal is to create healthy, bleeding surfaces.
- A trough is created in the metatarsal head and phalanx, and a tricortical inlay graft is used to replace the avascular segment and bridge the fusion site.
-
Revision of Failed Prosthetic Arthroplasty (e.g., Silastic):
- Curettage: Following removal of the implant, the defect in both the metatarsal and phalanx is vigorously curettaged until normal, healthy bone is reached. This typically leaves a considerable "champagne-glass" shaped defect in each bone.
- Temporary K-wire Alignment: A retrograde 1.6-mm K-wire is passed through the proximal phalanx, retrieved distally, and then driven into the remaining metatarsal shaft. This K-wire acts as a central alignment guide.
- Impaction Grafting: The champagne-glass defects are then meticulously impaction grafted with cancellous bone to create concave surfaces that will accept a ball-shaped graft.
- Trough Creation: A trough is carefully cut out of the dorsum of each bone, using the underlying K-wire as an alignment guide. The dimensions of this trough are measured, and the K-wire is then temporarily removed.
- Ball-shaped Cancellous Graft: A ball-shaped cancellous graft of sufficient size to fill the impaction-grafted defect is prepared. The hallux is again held in an estimated best position, and the graft is inserted.
III. Positioning of the Hallux: The Functional Arc
This is arguably the most critical step, fellows. The final position of the arthrodesed first MTPJ must allow for appropriate heel rise during the late stance phase of gait and comfortable weight-bearing.
- Initial Assessment: If a graft has been used, it is positioned in the arthrodesis site. The alignment of the hallux is then meticulously reassessed.
- Functional Position Check:
- Place a flat surface against the sole of the foot.
- Bring the ankle to 90 degrees.
- In this position, with the IP joint in full extension, the tip of the hallux should lie approximately 1 cm from the flat surface.
- When the IP joint is flexed to 45 to 60 degrees, its tip should comfortably come into contact with the plantar surface. This precise positioning enables the foot to rock at the MTPJ on heel rise without impingement.
- Ensure a gap of 3 to 5 mm is maintained between the hallux and the second toe.
- The rotation of the hallux should be neutral, so that the arc of rotation of the IP joint is at 90 degrees to the weight-bearing surface.
- Graft Trimming and Temporary Fixation: The interposition graft is carefully trimmed as required to achieve this precise functional position. Once satisfied, the entire construct is held securely with temporary K-wires. These K-wires are crucial for maintaining alignment while we apply definitive fixation.
IV. Fixation of the Arthrodesis: Achieving Stability
Now that we have the optimal position, we proceed with definitive fixation. We prefer a low-profile precontoured titanium plate for its stability and ability to accommodate various bone stock scenarios.
-
Plate Selection: We use a dorsal titanium precontoured plate (e.g., HALLU-S Plate; Newdeal). These plates are available in three side-specific sizes (small, medium, and large).
- In revision arthrodesis, the large size is usually required for men, medium for women, and small if no interposition graft is used.
- If the hallux length has not been fully restored, the plate may need to be slightly straightened to accommodate the longer construct. Conversely, the dorsum of the MTP joint may require "feathering down" with an oscillating saw to ensure a flush fit of the plate.
-
Fixation Without Interposition Graft (e.g., reamed surfaces, simple malunion correction):
- An oblique 2.7-mm compression screw of appropriate length is inserted from distal-medial to proximal-lateral across the MTPJ. This provides initial interfragmentary compression.
- The dorsal titanium precontoured plate is then carefully positioned and secured with a temporary K-wire.
- Six to seven 2.7-mm diameter self-tapping screws are then inserted through the plate, ensuring bicortical purchase where possible, to achieve strong, stable fixation.
-
Fixation With Interposition Graft:
- It may be necessary to reposition the temporary K-wire fixation to allow for optimal positioning of a trial plate.
- Once the plate is perfectly contoured and positioned, it is secured to the dorsal aspect of the joint with a temporary K-wire.
- The plate is then fixed with six to seven 2.7-mm diameter self-tapping screws.
- Crucially, the interposition graft is secured to the plate with one screw to prevent rotation or displacement.
-
Addressing Poor Bone Quality:
- If the bone quality is poor and initial screw purchase is insufficient, we have 3-mm diameter rescue screws available to provide enhanced fixation.
-
Final Assessment: After all hardware is secured, we perform a final fluoroscopic check in AP, lateral, and oblique views to confirm hardware position, joint alignment, and graft incorporation. We also visually inspect the foot for any signs of impingement or malrotation.
V. Closure and Dressing
- Wound Irrigation: The wound is thoroughly irrigated with sterile saline.
- Drain Placement: A small suction drain may be placed, especially in cases with significant dead space or if extensive bone grafting was performed, to prevent hematoma formation.
- Layered Closure: The wound is meticulously closed in layers: deep capsule, subcutaneous tissue, and skin. We use fine sutures to minimize tension and optimize cosmesis.
- Compression Dressing: A soft, compressive dressing is applied to provide support and reduce swelling.
💡 Pearls and Pitfalls
- Failed Keller-Brandes Procedure: Almost always requires a tricortical iliac crest graft to restore length and provide a stable construct. Do not attempt primary fusion without a graft if significant bone loss is present.
- Avascular Necrosis (AVN): Meticulous debridement of all avascular bone is paramount. A trough and tricortical inlay graft is often the best solution to bridge the defect and promote revascularization.
- Nerve Injury: The dorsal cutaneous nerve and deep peroneal nerve terminal branch are highly vulnerable. Always identify, protect, and avoid excessive retraction. Neuroma formation is a significant complication.
- Inadequate Bone Preparation: Failure to achieve healthy, bleeding cancellous bone surfaces will significantly increase the risk of nonunion. Be aggressive in debridement.
- Malpositioning: The functional position (1 cm tip clearance, 45-60 deg IPJ flexion to ground, 3-5mm interdigital gap, neutral rotation) is non-negotiable. Reassess multiple times with temporary K-wires before definitive fixation. A malunion can be as painful as a nonunion.
- Hardware Impingement: Ensure the plate lies flush. If not, feathering down the dorsal MTP joint or adjusting the plate contour is necessary. Prominent hardware can cause irritation and require removal.
- Nonunion Risk Factors: Counsel patients about smoking cessation. Poor bone quality, large grafts, and infection significantly increase nonunion rates.
- Infection: Active infection is an absolute contraindication. Rule it out thoroughly preoperatively. If suspected intraoperatively, send cultures and consider a staged procedure.
- Vascular Complications: Rare, but aggressive retraction or excessive cautery can compromise dorsal blood supply, especially in scarred fields.
- Time to Union: Be realistic with patients. The entire process of graft incorporation and union can take up to 6 months, particularly with large defects or AVN.
Postoperative Care and Rehabilitation: Guiding Recovery
Fellows, our work isn't done until the patient is walking comfortably. Postoperative care is crucial for successful integration of the arthrodesis.
- Dressing and Shoe: We prefer to use a compressive dressing for the first 1-2 weeks to minimize swelling. The patient is immediately placed into a postoperative stiff-soled shoe or a CAM walker.
- Mobilization and Weight-Bearing: Early mobilization with careful heel weight bearing only is encouraged immediately postoperatively. This means the patient can ambulate, but must avoid forefoot loading. The stiff-soled shoe protects the fusion site. Full weight-bearing is gradually advanced based on radiographic evidence of healing, typically starting around 6-8 weeks and progressing over the next several weeks.
- Range of Motion (ROM) Exercises:
- Early stretching of the tendo Achilles is encouraged to prevent equinus contracture and facilitate heel rise.
- Early range-of-motion exercises of the IP joint of the hallux are encouraged to prevent stiffness in this adjacent joint. This is a key advantage of using a dorsal plate over transarticular K-wires.
- DVT Prophylaxis: Standard deep vein thrombosis (DVT) prophylaxis protocols are followed, which may include chemical prophylaxis (e.g., LMWH) and mechanical prophylaxis (e.g., compression stockings, early ambulation).
- **
REFERENCES
-
Mann RA, Thompson FM. Arthrodesis of the first metatarsophalangeal joint for hallux valgus in rheumatoid arthritis. J Bone Joint Surg Am 1984;66A:687–692.
-
Flavin R, Stephens MM. Arthrodesis of the 1st metatarsal phalangeal joint using a dorsal titanium contoured plate. Foot Ankle Int 2004; 25:783–787.
-
Stephens MM, ed. An Atlas of Foot and Ankle Surgery, ed
-
London: Martin Dunitz, 2001.
-
Machacek F, Easley M, Gruber F, et al. Salvage of the failed Keller resection arthroplasty. J Bone Joint Surg Am 2004;86A:1131–1138.
You Might Also Like