Pediatric Trigger Thumb: An Intraoperative Masterclass on A1 Pulley Release
Key Takeaway
This masterclass details open A1 pulley release for pediatric trigger thumb, guiding fellows through comprehensive anatomy, meticulous preoperative planning, and granular intraoperative execution. Learn critical neurovascular protection, precise incision techniques, and how to confirm complete release. We cover extensive pearls, pitfalls, and postoperative care for optimal outcomes.
Welcome, colleagues and fellows, to the operating theater. Today, we are addressing a common yet frequently misunderstood condition in pediatric orthopaedics: the pediatric trigger thumb. While historically termed "congenital" trigger thumb, longitudinal studies have demonstrated that it is rarely detected at birth, typically presenting in late infancy through age five. Our goal today is a precise, definitive, and complete open release of the first annular (A1) pulley, restoring full, pain-free kinematic motion to the thumb interphalangeal (IP) joint while meticulously preserving the critical surrounding neurovascular and biomechanical structures.
Comprehensive Introduction and Patho-Epidemiology
Pediatric trigger thumb represents a distinct clinical entity from its adult counterpart, characterized by a mechanical impingement within the flexor tendon sheath rather than a primary inflammatory tenosynovitis. The hallmark of this condition is a localized, pathological tightness of the A1 pulley of the thumb, coupled with a palpable, localized enlargement—often referred to as Notta’s node—within the substance of the flexor pollicis longus (FPL) tendon. This spatial mismatch prevents the normal, smooth gliding excursion of the FPL tendon through the fibro-osseous sheath, thereby restricting full active and passive interphalangeal joint motion. Unlike adult trigger digits, the classic dynamic "triggering" phenomenon, where the digit locks and then suddenly releases with a painful snap, is a rare presentation in the pediatric population. Instead, we typically observe a painless, fixed flexion contracture of the thumb IP joint. In a much smaller, atypical subset of cases, the nodule might lie distal to the A1 pulley, presenting as a fixed extension deformity with an inability to actively flex the IP joint.
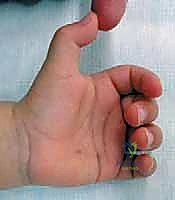
The precise pathogenesis of pediatric trigger thumb remains an area of ongoing academic debate. While adult trigger digits frequently demonstrate an inflammatory component with tenosynovial proliferation, histological analyses of biopsies obtained during pediatric cases have consistently failed to show significant signs of acute or chronic inflammation. Instead, the pathology reveals a fibrocartilaginous metaplasia of the pulley itself, accompanied by reactive thickening and collagen degeneration within the FPL tendon node. Genetic predispositions have been proposed due to a higher incidence in monozygotic twins and certain familial clusters, yet a definitive Mendelian inheritance pattern remains elusive. Traumatic etiologies, such as repetitive grasping or thumb sucking, have also been postulated, but these lack robust biomechanical or epidemiological validation. The current consensus leans toward an acquired mismatch in the growth rates between the FPL tendon and its surrounding retinacular sheath during early childhood development.
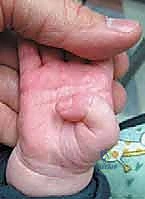
When evaluating a pediatric patient with a flexed thumb, it is critically important to differentiate pediatric trigger thumb from a spectrum of other congenital and acquired conditions that can mimic its clinical presentation. Misdiagnosis can lead to inappropriate surgical interventions and profound functional deficits. The most critical differential is the Congenital Clasped Thumb, a complex deformity where the metacarpophalangeal (MCP) joint is fixed in flexion due to extensor mechanism hypoplasia, while the IP joint typically maintains a full, supple passive range of motion. Cerebral Palsy presenting with a "thumb-in-palm" deformity involves spasticity and increased tone in the intrinsic adductor and flexor musculature, leading to a fundamentally different biomechanical pattern that requires a comprehensive neurological assessment. Furthermore, one must rule out Arthrogryposis Multiplex Congenita, a non-progressive condition characterized by multiple rigid joint contractures present at birth, and Thumb Hypoplasia, which encompasses a broad spectrum of congenital longitudinal deficiencies of the radial ray.
Detailed Surgical Anatomy and Biomechanics
Precision in hand surgery is inexorably linked to an intimate, three-dimensional understanding of regional anatomy. The flexor pollicis longus (FPL) tendon is the sole flexor of the thumb interphalangeal joint, originating from the volar aspect of the radius and inserting onto the base of the distal phalanx. As it traverses the volar aspect of the thumb, it is constrained within a complex fibro-osseous sheath, anchored to the underlying phalanges and volar plates by a highly specialized series of retinacular pulleys. These pulleys are biomechanically imperative for maintaining the tendon closely apposed to the center of rotation of the MCP and IP joints, thereby preventing bowstringing, preserving mechanical efficiency, and maximizing tendon excursion during active flexion.

The retinacular system of the thumb is uniquely configured compared to the triphalangeal digits. The primary structures include the A1, oblique, and A2 pulleys. The A1 pulley, our primary surgical target, is the most proximal of the annular pulleys. It is a robust, transversely oriented fibrous band located at the level of the volar plate of the MCP joint, clinically correlating with the palmar digital crease. Critically, biomechanical studies have definitively shown that isolated division of the A1 pulley does not cause clinically significant bowstringing or loss of flexion power of the FPL tendon. Conversely, the oblique pulley, located immediately distal to the A1 pulley and coursing from proximal-ulnar to distal-radial over the proximal phalanx, is the essential biomechanical constraint against bowstringing. Identifying and meticulously protecting the oblique pulley during an A1 release is paramount; iatrogenic injury to this structure will result in profound biomechanical failure, decreased IP flexion strength, and a functionally compromised digit.
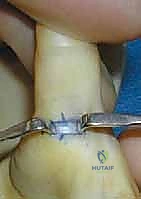
Navigating the volar aspect of the thumb requires an acute awareness of the neurovascular relationships, specifically the digital nerves, which represent the most significant structures at risk during this procedure. The digital nerves to the thumb lie in treacherous proximity to the FPL tendon sheath. The radial digital nerve is particularly vulnerable; its anatomical course frequently takes it obliquely across the proximal aspect of the flexor sheath, crossing from ulnar to radial just proximal to the A1 pulley. It is often located in a more superficial plane than anticipated. The ulnar digital nerve runs a more predictable, longitudinal course parallel to the tendon sheath, typically resting immediately alongside the ulnar border of the A1 pulley. The surgical interval we exploit is a narrow subcutaneous plane directly overlying the flexor sheath, bounded on either side by these delicate neurovascular bundles.
Exhaustive Indications and Contraindications
The decision to proceed with surgical intervention for a pediatric trigger thumb must be guided by a thorough understanding of the condition's natural history and a careful assessment of the individual patient's functional deficit. While historical literature suggested immediate surgical release upon diagnosis, contemporary longitudinal studies have illuminated a significant rate of spontaneous resolution. Observation alone can yield spontaneous improvement in 24% to 63% of cases; however, this resolution often requires a protracted period, averaging 48 months, and rarely results in a truly normal IP joint with physiological hyperextension. Therefore, surgical release is indicated when the deformity is rigid, bilateral, severely limits prehensile function, or fails to resolve after an appropriate period of watchful waiting (typically up to age 2 or 3).
Prolonged delay in surgical intervention is not without consequence. Chronic, unyielding flexion contractures of the IP joint can lead to secondary adaptive changes, most notably a compensatory hyperextension laxity at the MCP joint. This occurs as the child attempts to clear the flexed thumb from the palm during grasp and pinch activities. If left untreated into later childhood, the capsular contracture at the IP joint may become permanent, and the MCP joint instability may require concurrent surgical stabilization. Therefore, the optimal surgical window is generally considered to be between 12 and 36 months of age, balancing the potential for spontaneous resolution against the risks of secondary joint deformity.
Contraindications to surgical release are relatively few but absolute when present. Active local or systemic infection precludes elective surgery. A misdiagnosis, particularly confusing a trigger thumb with a spastic thumb-in-palm deformity secondary to cerebral palsy, is a critical contraindication to an isolated A1 pulley release, as this will fail to address the underlying muscular spasticity and may paradoxically worsen the deformity. Furthermore, patients with severe medical comorbidities precluding safe general anesthesia should be managed non-operatively until their medical status is optimized.
| Variable | Surgical Indications | Surgical Contraindications |
|---|---|---|
| Clinical Presentation | Fixed, rigid IP flexion contracture > 30 degrees | Supple, passively correctable IP joint (consider observation) |
| Duration/Timing | Failure to spontaneously resolve by age 2-3 years | Presentation in early infancy (< 12 months) without functional deficit |
| Secondary Changes | Development of compensatory MCP hyperextension | Active local skin infection or paronychia |
| Functional Impact | Significant impairment of pinch, grasp, or fine motor skills | Misdiagnosis (e.g., Cerebral Palsy, Arthrogryposis, Clasped Thumb) |
| Patient Factors | Bilateral rigid presentation | Severe cardiopulmonary instability precluding general anesthesia |
Pre-Operative Planning, Templating, and Patient Positioning
Operative success in pediatric hand surgery begins long before the scalpel touches the skin. While extensive radiographic imaging is rarely necessary for a classic pediatric trigger thumb, a meticulous clinical assessment and thoughtful preoperative preparation are absolutely essential. The physical examination must confirm the diagnosis by palpating the characteristic Notta's node within the FPL tendon, typically located at the level of the palmar digital crease. The surgeon must rigorously assess the passive range of motion of the IP joint, noting whether the thumb is locked in flexion or extension, and carefully evaluate the MCP joint for any compensatory hyperextension laxity.
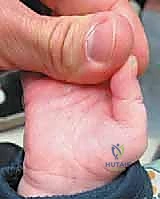
Family counseling is a paramount component of the preoperative phase. Parents are often highly anxious regarding surgery on their young child. The surgeon must clearly articulate the natural history of the condition, explaining that while spontaneous improvement is possible, it is unpredictable and often incomplete. The discussion should highlight the high success rate (approaching 99% in experienced hands) and the low complication profile of a surgical release, framing it as a definitive and highly effective intervention. The controversy surrounding the optimal timing of surgery should be discussed transparently, acknowledging the rationale for early intervention to prevent permanent capsular contractures and secondary joint deformities.
Anesthetic considerations in the pediatric population require specialized expertise. Because of the microscopic proximity of the digital nerves to the flexor sheath and the absolute necessity for a perfectly still surgical field, local anesthesia alone is entirely insufficient and unsafe for a pediatric patient. General anesthesia, typically utilizing a laryngeal mask airway (LMA) or endotracheal intubation, administered by a fellowship-trained pediatric anesthesiologist, is mandatory. While the surgical procedure itself is brief, often lasting less than 15 minutes, patient cooperation and absolute immobility are non-negotiable prerequisites for avoiding catastrophic neurovascular injury.
Operating room setup must be ergonomic and optimized for microsurgical precision. The patient is positioned supine on the operating table. The affected upper extremity is extended and secured onto a specialized, radiolucent hand table. A pediatric-sized pneumatic tourniquet is placed high on the brachium over soft cast padding. The entire limb distal to the tourniquet is meticulously prepared with a standard antiseptic solution (such as chlorhexidine gluconate) and draped in a sterile fashion. The limb is then exsanguinated using an Esmarch bandage, and the tourniquet is inflated to a pressure typically calculated at 100 mm Hg above the patient's systolic blood pressure (usually around 150-200 mm Hg in toddlers) to ensure a perfectly bloodless surgical field.
Step-by-Step Surgical Approach and Fixation Technique
With the patient optimally positioned, anesthetized, and the tourniquet inflated, we commence the surgical approach. The assistant is instructed to hold the thumb in a perfectly vertical position, applying gentle traction. This maneuver is critical; it correctly orients the flexor sheath and prevents the surgeon from making an incision too far radial, a common pitfall given the natural pronation of the thumb relative to the plane of the palm. We plan a small, transverse incision, typically 7 to 10 millimeters in length, placed directly within or immediately parallel to the palmar digital crease of the thumb. This specific orientation minimizes postoperative scar contracture and yields an optimal cosmetic outcome.
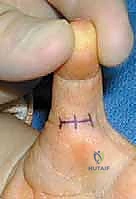
Using a #15 scalpel blade, a careful, superficial incision is made exclusively through the epidermis and dermis. The surgeon must acutely remember that the radial digital nerve frequently crosses the surgical field just deep to the dermis in this region. Once the skin is incised, we transition immediately to blunt dissection. Utilizing a fine curved iris scissor or a small, delicate hemostat, the subcutaneous tissues are gently spread longitudinally, parallel to the anticipated course of the neurovascular bundles. Sharp dissection in the subcutaneous plane is strictly avoided to prevent iatrogenic nerve transection. The use of surgical loupe magnification (minimum 2.5x to 3.5x) is mandatory during this phase to reliably differentiate the glistening white, transversely oriented fibers of the A1 pulley from the softer, longitudinally oriented peripheral nerve tissue.
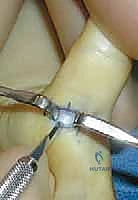
As the blunt dissection proceeds, the radial and ulnar digital nerves are gently swept aside, though they do not necessarily require formal skeletonization. Small Sen retractor or delicate Ragnell retractors are placed proximally and distally to expose the entire volar surface of the A1 pulley. The surgeon must clearly identify the proximal and distal extents of the A1 pulley. The proximal edge is typically located just distal to the palpable Notta's node. Once the A1 pulley is fully visualized, a fine scalpel (such as a #67 Beaver blade) or tenotomy scissors are used to sharply incise the pulley longitudinally along its exact midline.
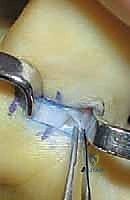
The release must be absolute and complete. As the A1 pulley is divided, the underlying FPL tendon and its associated nodule will visibly "pop" through the created defect. It is a common error to perform an incomplete release, leaving a few distal fibers intact, which inevitably leads to recurrent triggering. However, as the dissection proceeds distally, the surgeon must exercise extreme caution to identify and preserve the oblique pulley. The oblique pulley fibers angle distally and radially; violating this structure will result in FPL bowstringing.

Following the complete longitudinal division of the A1 pulley, the adequacy of the release must be dynamically verified. The surgeon passively extends and flexes the IP joint through its maximum range of motion. The Notta's node should be observed gliding smoothly and unimpeded through the released area, without any residual catching, snapping, or impingement. If any resistance is encountered, the proximal and distal margins of the release must be re-inspected and further divided as necessary.
Once a complete release is confirmed and the tendon glides freely, the surgical site is thoroughly irrigated with sterile saline. The tourniquet is deflated, and meticulous hemostasis is achieved using bipolar electrocautery, ensuring no thermal injury occurs to the adjacent digital nerves. The skin is then meticulously approximated. In the pediatric population, we utilize absorbable sutures, such as 5-0 chromic gut or fast-absorbing plain gut, placed in an interrupted or simple continuous fashion. This eliminates the need for a traumatic and anxiety-inducing suture removal in the clinic.
Complications, Incidence Rates, and Salvage Management
While the open release of a pediatric trigger thumb is generally considered a highly successful procedure with a low overall complication rate, the potential complications are significant and can result in profound, lifelong functional impairment. The most devastating complication is iatrogenic injury to the digital nerves. The radial digital nerve is at the highest risk due to its oblique and relatively superficial course across the proximal aspect of the flexor sheath. The incidence of nerve injury is reported to be less than 1% in the hands of experienced pediatric hand surgeons but rises sharply with inadequate exposure, poor lighting, lack of magnification, or aberrant anatomy.
If a digital nerve transection is recognized intraoperatively, immediate primary microsurgical epineurial repair using 8-0 or 9-0 nylon suture is mandatory. If the injury is discovered postoperatively, presenting as a dense sensory deficit or a painful neuroma along the lateral aspect of the thumb, prompt re-exploration and microsurgical reconstruction (potentially requiring a nerve autograft if a gap exists) are indicated. Recurrence of triggering or persistence of the IP flexion contracture is almost exclusively the result of a technical error: specifically, an incomplete release of the A1 pulley, usually failing to divide the most proximal or distal fibers. Management requires a secondary surgical exploration to complete the release.
Iatrogenic bowstringing of the FPL tendon is a severe biomechanical complication resulting from the inadvertent division of the oblique pulley. This manifests clinically as a loss of active IP joint flexion power, a visible prominence of the tendon in the volar thumb during attempted flexion, and a decrease in overall grip and pinch strength. Salvage management for established bowstringing is complex and typically requires a formal pulley reconstruction using a tendon graft (such as palmaris longus or a slip of the flexor digitorum superficialis) routed circumferentially around the proximal phalanx, a procedure that carries its own morbidity and prolonged rehabilitation.
| Complication | Estimated Incidence | Etiology / Risk Factors | Salvage / Management Strategy |
|---|---|---|---|
| Digital Nerve Injury | < 1.0% | Sharp blind dissection, lack of loupes, anomalous radial nerve course | Immediate microsurgical epineurial repair; late neuroma excision and grafting |
| Incomplete Release / Recurrence | 1.0% - 3.0% | Failure to divide extreme proximal or distal A1 fibers | Re-exploration and complete division of the residual retinacular band |
| FPL Bowstringing | < 0.5% | Iatrogenic transection of the oblique pulley | Complex pulley reconstruction utilizing autologous tendon grafting |
| Superficial Surgical Site Infection | 1.0% - 2.0% | Poor hygiene post-op, maceration of dressings | Oral antibiotics, local wound care; rarely requires operative debridement |
| Incisional Scar Contracture | Rare | Longitudinal incision crossing the palmar digital crease | Z-plasty or local tissue rearrangement (prevented by transverse incision) |
Phased Post-Operative Rehabilitation Protocols
The immediate postoperative management following an A1 pulley release is designed to protect the surgical wound while simultaneously encouraging early, active mobilization to prevent tendon adhesions. Upon completion of the skin closure, a sterile, non-adherent dressing (such as Xeroform or Adaptic) is applied directly to the incision. This is followed by a soft, bulky, compressive dressing utilizing sterile gauze and a cohesive bandage (e.g., Coban). Rigid immobilization with a splint or cast is explicitly contraindicated, as it promotes stiffness, restricts necessary tendon excursion, and provides no biomechanical advantage following an isolated pulley release.
During the first two weeks postoperatively, the primary goals are wound healing and pain control. Parents are instructed to keep the bulky dressing clean, dry, and intact. The child is actively encouraged to use the hand for light, age-appropriate play and daily activities. The natural curiosity and activity level of toddlers usually ensure adequate spontaneous mobilization of the thumb, negating the need for formal physical therapy in the vast majority of cases. Acetaminophen and ibuprofen are typically sufficient for postoperative analgesia.
The patient is evaluated in the outpatient clinic at approximately two weeks post-surgery. At this juncture, the bulky dressing is removed. Because absorbable sutures are utilized, formal suture removal is avoided, significantly reducing the child's anxiety. The surgeon assesses the wound for complete epithelialization and evaluates the active and passive range of motion of the IP joint. The parents are instructed on gentle scar massage techniques using a bland emollient to soften the incisional scar and prevent tethering of the underlying subcutaneous tissues.
Long-term follow-up is generally minimal. A final assessment at six to twelve weeks postoperatively is recommended to ensure full restoration of IP joint motion, complete resolution of any preoperative compensatory MCP hyperextension, and normal integration of the thumb into the child's prehensile patterns. In the exceedingly rare event of persistent stiffness or significant scar contracture, a referral to a specialized pediatric occupational hand therapist may be initiated for targeted stretching and custom static-progressive splinting, though this is almost never required following an uncomplicated, well-executed surgery.
Summary of Landmark Literature and Clinical Guidelines
The contemporary management of pediatric trigger thumb is heavily informed by several landmark epidemiological and clinical studies that have refined our understanding of the condition's natural history. Historically, the seminal work by Dinham and Meggitt in 1974 established the baseline understanding that a subset of these deformities could resolve without intervention, though they advocated for relatively early surgery if the condition persisted past the first year of life. This paradigm shifted significantly with the publication of more robust, long-term observational cohorts.
A pivotal study by Baek et al. (2008) in the Journal of Bone and Joint Surgery fundamentally altered the treatment algorithm. By prospectively observing a large cohort of pediatric patients with trigger thumbs, they documented a spontaneous resolution rate exceeding 60% when observed over a period of up to 48 months. This data provided the evidence-based foundation for the modern practice of a prolonged period of watchful waiting, typically delaying surgical intervention until the child is at least two to three years of age, provided no severe secondary joint contractures are developing.
Current clinical guidelines synthesized from the American Society for Surgery of the Hand (ASSH) and the Pediatric Orthopaedic Society of North America (POSNA) reflect a balanced, evidence-based approach. The consensus dictates that initial management should consist of observation and parental reassurance. Splinting and passive stretching exercises have been investigated but generally demonstrate poor compliance and lack robust evidence of efficacy over observation alone. Surgical intervention—specifically, the open release of the A1 pulley detailed in this masterclass—remains the gold standard for cases that are rigid, bilateral, or fail to resolve after an appropriate observation period, offering a definitive cure with an exceptionally high safety profile when executed with rigorous microsurgical technique.
