Pediatric Femur Fracture: Closed Reduction & Spica Casting Masterclass

Key Takeaway
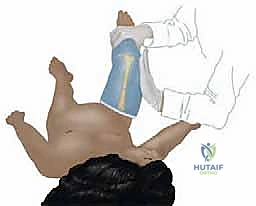
Welcome to the OR, fellows. Today, we're tackling pediatric femur fractures with closed reduction and spica casting. This masterclass covers critical anatomy, meticulous preoperative planning, and a step-by-step intraoperative execution. We'll delve into precise patient positioning, reduction maneuvers, and casting techniques for both traditional and walking spicas, emphasizing crucial pearls to avoid complications and ensure optimal outcomes for our young patients.
Alright fellows, gather 'round. Let's scrub in. Today, we're performing a closed reduction and spica casting for a pediatric femoral shaft fracture. This is a fundamental skill in pediatric orthopaedics, and mastering it requires a deep understanding of pediatric anatomy, meticulous technique, and a keen eye for potential pitfalls. While the incidence is relatively low—around 20 per 100,000 children annually, comprising about 2% of all pediatric fractures—the impact on the child and family is significant.
Initial Assessment and Differential Diagnosis
Before we even consider the OR, remember the initial presentation. When a young child presents with a femoral shaft fracture, especially if they're non-ambulatory, our first thought must always be child abuse. This is a critical differential. We also consider conditions like osteogenesis imperfecta, particularly in children with a history of multiple fractures, which can often be mistaken for abuse.
During the initial physical exam, which is often done in the emergency department, we are meticulously palpating the entire lower extremity, feeling for bony deformity and, crucially, checking compartments for tension. A tense compartment is an absolute red flag for developing compartment syndrome. We must also confirm the integrity of the neurovascular status:
* Vascular: Palpate femoral, popliteal, dorsalis pedis, and posterior tibial pulses. If diminished, a Doppler assessment is mandatory.
* Neurological: Assess sensation to light touch along the entire lower extremity. Motor examination can be challenging due to pain, but attempt ankle dorsiflexion and plantarflexion. Diminished strength can indicate nerve damage or compartment syndrome. Similarly, reflexes – patellar and Achilles – are tested, though guarding can make this difficult.
We're also looking for open wounds, bruising, and obvious deformity. An isolated femur fracture typically presents with a swollen thigh, minor abrasions, and often noticeable shortening. High-energy trauma may present with concomitant soft tissue injuries or injuries to other organ systems, which will significantly influence our management. Remember to always include the joints above and below the fracture site on initial radiographs to avoid missing associated injuries, especially around the knee.
Comprehensive Surgical Anatomy
Let's quickly review the unique anatomy of the pediatric femur, which dictates our approach.
The femur, like all long bones, develops from a limb bud around 4 weeks gestation, with the femoral shaft serving as the primary ossification center. The proximal ossification center appears by 6 months, and the distal femoral ossification center at 7 months. This evolving bone structure is crucial; initially, the bone is weaker woven bone, gradually replaced by stronger lamellar bone throughout childhood. This explains why low-energy injuries can cause fractures in toddlers, while older children require significantly more force.
The vascular supply to the femur is robust, coming from both endosteal and periosteal circulations. The profunda femoris artery is a key player, giving rise to four perforating arteries that enter the femur posteromedially. While the endosteal circulation is the primary supply in an intact bone, during fracture healing, the periosteal circulation takes over a more dominant role. This abundant blood supply contributes to the excellent healing potential we see in pediatric femur fractures.
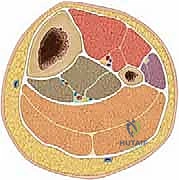
The femoral shaft flares distally, forming the supracondylar area, which is important to recognize for distal fracture patterns. While not directly relevant to the spica cast application itself, understanding the surrounding musculature and neurovascular bundles is paramount to avoid iatrogenic injury during reduction maneuvers or cast application. The femoral nerve and artery lie anteriorly, while the sciatic nerve is posterior. The popliteal fossa, where we'll apply extra padding, houses the popliteal artery and tibial nerve, making excessive knee flexion in a cast a significant risk for neurovascular compromise.
Preoperative Planning: The Blueprint for Success
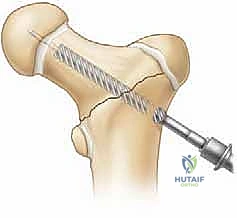
Our patient today is a 4-year-old with an oblique diaphyseal femur fracture, sustained from a low-energy fall. This fits perfectly within our indications for closed reduction and spica casting.
Indications for Closed Reduction and Casting (Children < 6 years):
* Isolated femoral shaft fracture.
* Shortening less than 2 cm (though some argue spica casting can be effective regardless of initial shortening, we aim for less than 2 cm post-reduction).
* No massive thigh swelling or associated injuries precluding cast treatment.
* Low-energy mechanism, especially for a walking spica.
Contraindications:
* Significant open fractures.
* Massive thigh swelling increasing compartment syndrome risk.
* Associated injuries requiring alternative management (e.g., head trauma requiring supine positioning).
* Unstable polytrauma patients.
Let's review the imaging. We have high-quality AP and lateral radiographs of the femur, extending to include the hip and knee joints.
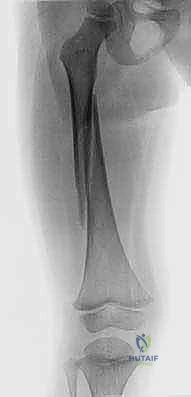
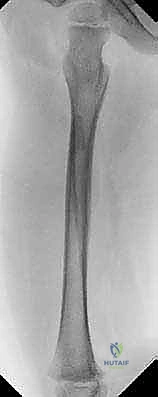
FIG 1 • AP and lateral radiographs of an oblique diaphyseal femur fracture in a child 4 years and 2 months of age.
Notice the oblique diaphyseal pattern. This is a common presentation. We've assessed the degree of shortening and angulation. For our 4-year-old, we're aiming for a traditional spica cast today, given the fracture pattern and our institutional preference for this age group, though a walking spica could be considered for a very stable, low-energy injury in a toddler.
Fluoroscopy Setup:
The C-arm will be positioned to allow for immediate AP and lateral views of the fracture site without repositioning the patient. This usually means a diagonal setup or having the C-arm ready to swing in for both planes. Ensure your fluoroscopy technician understands the critical views needed for real-time assessment during reduction.
Patient Positioning and Anesthesia
Our patient has been brought into the operating room. We'll be doing this under general anesthesia to ensure complete muscle relaxation and patient comfort, which is paramount for an effective reduction.
- Initial Supine Positioning: The child is initially placed supine on the operating table. We ensure proper padding of all pressure points.
- Anesthesia Induction: Once anesthesia is induced and the child is relaxed, we'll perform a final, gentle neurovascular check.
- Preparation for Casting: We'll apply stockinette to the injured leg, extending from the groin to beyond the toes, and to the torso.
- Transfer to Spica Table (Post-Initial Cast): The traditional method involves applying the initial cast on the injured extremity first, then transferring to the spica table. However, many centers, including ours, now prefer to perform the reduction and apply the bulk of the cast on the spica table for better control and stability. For today, we'll proceed with the latter approach.
Step-by-Step Intraoperative Execution: The Traditional Spica Cast
Alright fellows, let's get started.
1. Preparing the Injured Extremity
- Padding: We begin by applying generous soft roll padding. Pay particular attention to the bony prominences: the malleoli, tibial crest, fibular head, patella, and especially the popliteal fossa.
- Surgical Warning:
> CRITICAL PEARL: Excessive padding in the popliteal fossa is a must. However, once this padding is in place, we must be extremely careful not to hyperflex the knee, as this can create a tourniquet effect and lead to vascular compromise or compartment syndrome.
- Surgical Warning:
- Stockinette: Ensure the stockinette is smooth, without wrinkles, and extends well beyond the planned cast edges. We use a Gore-Tex liner at some institutions under the stockinette to prevent skin irritation, especially diaper rash and superficial infections, which is a common issue with prolonged casting.
2. Application of the Long-Leg Cylinder Cast (Initial Phase)
- We'll start with a long-leg cylinder cast on the injured side. For a traditional spica, our goal is 90 degrees of knee flexion and 90 degrees of ankle flexion.
- Casting Material: We'll use a combination of fiberglass and plaster. Fiberglass provides strength and durability, while plaster allows for better molding.
- Application: Apply the cast material smoothly, ensuring even tension. Mold it well around the contours of the leg.
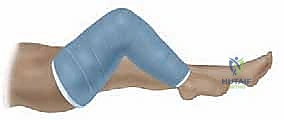
*TECH FIG 1 • A. Cylinder cast with 90 degrees of knee flexion for traditional spica casting.*
* **Surgical Warning:**
> **PITFALL:** Recent reports highlight the risk of compartment syndrome in the leg after spica casting, particularly with aggressive knee flexion. While 90/90 was traditional, we are now trending towards slightly less hip and knee flexion and often *not including the foot* for the injured leg to mitigate this risk. For today, we'll aim for 90 degrees of knee flexion but will monitor closely.
- Valgus Mold: As the cast material sets, we apply a valgus mold at the fracture site. This is crucial to prevent varus deformity, which is a common malunion pattern in femur fractures due to muscle forces. We are essentially counteracting the adductor pull.
TECH FIG 1 • (continued) B. Valgus molding technique to prevent varus deformity in early postcasting period.
3. Transfer to the Spica Table and Reduction
- Once the initial cylinder cast is stable enough, we carefully transfer the patient to the spica table. The spica table allows for controlled suspension and traction, which is essential for achieving and maintaining reduction.
- Manual Traction: The weight of the legs is supported with manual traction, usually applied by an assistant holding the foot or distal cast. This provides longitudinal traction to overcome muscle spasm and restore length.
- Surgical Warning:
> CRITICAL PITFALL: Avoid excessive traction. While traction is necessary, too much can increase the risk of compartment syndrome and skin sloughing, especially in the groin and perineal areas. It's a delicate balance.
- Surgical Warning:
- Hip Positioning: Now, we position the injured hip precisely. For a traditional spica, we aim for:
- 90 degrees of hip flexion.
- 30 degrees of abduction.
- 15 degrees of external rotation.
- Rationale: This specific position helps to align the proximal and distal fragments by relaxing the powerful hip flexors and abductors, and by counteracting the typical external rotation tendency of the distal fragment.

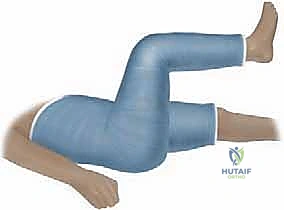
*TECH FIG 1 • (continued) C,D. Traditional spica casting with 90 degrees of hip flexion, 30 degrees of abduction, and 15 degrees of external rotation.*
- Reduction Under Fluoroscopy: With the hip in the correct position and gentle manual traction applied, we now use fluoroscopy to confirm our reduction. We obtain AP and lateral views.
- Maneuver: If further reduction is needed, we apply direct pressure over the fracture site while maintaining traction and the desired hip position. The valgus mold should be maintained. We're looking for acceptable alignment: less than 15 degrees of angulation in any plane and less than 2 cm of shortening. Rotational alignment is assessed clinically by comparing the patellar and foot positions.
4. Application of the Pelvic Band and Contralateral Leg
- Once satisfactory alignment is confirmed with fluoroscopy, we apply the remainder of the spica cast. This involves incorporating the torso and the uninjured leg into the cast.
- Pelvic Band: Apply the cast material around the torso, extending from the nipple line down to the mid-thigh on the uninjured side. This wide pelvic band is essential for immobilizing the hip.
- Contralateral Leg: The uninjured leg is typically included in the cast, usually with the hip in slight flexion and abduction, and the knee in slight flexion (around 20-30 degrees) to provide a stable base.
- Reinforcement: Ensure adequate layers of casting material, especially around the hip and perineal area, as these are high-stress zones.
5. Final Checks
- Radiographs: Obtain new AP and lateral radiographs of the injured femur in the cast to ensure acceptable anatomic alignment has been maintained. This is your final intraoperative check.
- Neurovascular Status: Perform a careful neurovascular check of both lower extremities. Ensure pulses are palpable and sensation is intact.
- Cast Edges: Smooth all cast edges to prevent skin irritation. Ensure there are no tight spots or areas of excessive pressure. Check for any signs of skin blanching.
Step-by-Step Intraoperative Execution: The Walking Spica Cast
Now, let's discuss the walking spica, which is gaining popularity for low-energy femur fractures in toddlers. The concept is to allow for some weight-bearing and mobility, decreasing the burden of care on the family.
1. Preparing the Injured Extremity
- Similar to the traditional spica, apply generous padding, particularly to bony prominences and the supramalleolar area.
- Foot Uncovered: A key difference here is that the foot remains uncovered, with the cast stopping in the supramalleolar area. Protect this area with extra padding.
2. Application of the Cylinder Cast (Walking Spica)
- The cylinder cast on the injured side is applied with about 50 degrees of knee flexion. This is less flexion than the traditional spica, allowing for more functional positioning.

*TECH FIG 2 • A. Cylinder cast with 50 degrees of knee flexion and 45 degrees of hip flexion for walking spica cast.*
- Apply the valgus mold at the fracture site as before.
3. Transfer to Spica Table and Reduction (Walking Spica)
- Transfer the patient to the spica table.
- Hip Positioning: For a walking spica, the hip is flexed to 45 degrees, remains abducted to 30 degrees, and externally rotated 15 degrees. This position is more functional for ambulation while still providing stability.
TECH FIG 2 • A. Cylinder cast with 50 degrees of knee flexion and 45 degrees of hip flexion for walking spica cast. B. Walking spica casting position with 30 degrees of abduction and 15 degrees of external rotation.
* Perform reduction under fluoroscopy, aiming for the same acceptable alignment parameters.
4. Application of the Pelvic Band and Reinforcement (Walking Spica)
- Abdominal Compression Prevention: Before applying the pelvic band, place multiple layers of folded stockinette on the abdomen. This creates space and prevents abdominal compression once the cast is applied. These layers are removed after the pelvic band is placed and has started to set.
- Wide Pelvic Band: Apply a wide pelvic band to immobilize the hip.
- Anterior Hip Reinforcement: This is crucial for a walking spica. Place seven or eight layers of folded fiberglass anteriorly in the inter-hip crease on the injured side. This significantly decreases the risk of the cast breaking during ambulation.
TECH FIG 2 • (continued) C. Wide pelvic band and anterior reinforcement for additional support in a final walking spica cast.
* The contralateral leg is typically not included in a walking spica, allowing for independent movement.
5. Final Checks (Walking Spica)
- Obtain post-reduction, post-casting radiographs.
- Perform thorough neurovascular checks.
- Smooth all cast edges.
💡 Pearls and Pitfalls
General Contraindications for Spica Casting:
* Shortening > 2 cm (controversial): While some suggest spica can be effective, significant initial shortening makes achieving and maintaining reduction difficult.
* Massive thigh swelling: This dramatically increases the risk of compartment syndrome.
* Associated injuries: Any injury precluding cast treatment or requiring alternative positioning.Walking Spica Pearls:
* Effective for low-energy, isolated femur fractures: Ideal for toddlers.
* Functional: Toddlers can often pull-to-stand and begin walking in 2 to 3 weeks, reducing family burden.
* Reinforcement is key: Don't skimp on anterior hip reinforcement.Reasons for Cast Change / Intervention:
* Excessive angulation (> 15 degrees): This is a clear indication for revision.
* Shortening (> 2 cm): Especially before callus formation.
* Excessive soiling of the cast: Can lead to skin breakdown and infection.Other Complications to Watch For:
* Need for valgus wedge adjustment: If angulation is less than 15 degrees but still not ideal, a wedge can correct it in the clinic.
* Skin irritation, diaper rash, superficial infections: Preventable with good hygiene, Gore-Tex liners, and proper cast care education.
* Compartment Syndrome: This is arguably the most dreaded complication. It can be associated with excessive traction during application or, as noted, with aggressive knee flexion in a short-leg cast used for traction during a 90/90 spica.
* Salvage: Immediate cast bivalving and removal, followed by emergent fasciotomy if symptoms persist. Always maintain a high index of suspicion.
* Loss of Reduction: Studies show standard spica casting is successful without cast change or wedging about 86% of the time. The remaining 14% require intervention.
Postoperative Care
Our job isn't done once the cast is on. Postoperative care is critical for a successful outcome and managing the significant burden placed on the family.
Family Counseling
Immediately after reduction and casting, we counsel the family extensively. This includes:
* Cast Care: How to keep the cast clean and dry, especially around the perineum.
* Monitoring for Complications: Emphasize signs of neurovascular compromise (pain out of proportion, pallor, paresthesia, pulselessness, paralysis), skin irritation, or cast issues (cracking, foul odor).
* Travel Difficulties: Spica casts make transportation challenging.
* Loss of Time at Work: Often, a parent needs to take significant time off.
* Potential for Wedging: We proactively inform them that cast wedging may be necessary at about 10 to 14 days after injury to correct minor alignment issues. This manages expectations and often avoids unnecessary trips back to the operating room.
Follow-up Schedule and Radiographic Assessment
- First Follow-up (1 week post-injury): The family returns. We obtain true AP and lateral radiographs of the injured femur in the cast.
- Second Follow-up (2 weeks post-injury): Another set of AP and lateral radiographs.
- Assessment: At these visits, we meticulously assess for any loss of reduction, specifically looking for:
- Angulation: If angulation is unsatisfactory (e.g., greater than 15 degrees in any plane), or if there's a progressive deformity, we will wedge the cast in the clinic. This involves cutting the cast, inserting a wedge (often made of plaster or wood), and reinforcing it, followed by repeat radiographs to confirm correction. This maneuver frequently avoids a return to the operating room.
- Shortening: If shortening of more than 2 cm is noted before callus formation, we have options:
- Cast change.
- Application of skeletal traction.
- External fixation.
Complications and Management
Despite our best efforts, complications can arise.
- Nonunion: Rare in pediatric femur fractures due to their excellent healing potential. If it occurs, it often points to an underlying issue (e.g., severe soft tissue injury, infection). Management would involve surgical intervention, often with bone grafting.
- Delayed Union: Healing takes longer than expected. Often managed conservatively with continued immobilization, but close monitoring is required.
- Malunion:
- Angular Deformity: Most common. Minor angulation can be corrected with cast wedging. Significant malunion might require osteotomy once the fracture has healed, especially if it's projected to cause functional issues or progressive deformity.
- Rotational Deformity: More difficult to assess and correct non-operatively. Significant rotational malunion (often >15-20 degrees) may require a derotational osteotomy after healing.
- Leg-Length Discrepancy:
- Shortening: If shortening of more than 2 cm persists after callus has formed, we might consider osteoclasis and lengthening techniques at a pace of 1 mm per day, though this is a significant undertaking.
- Overgrowth: Pediatric femurs, especially after fracture, can exhibit compensatory overgrowth, sometimes leading to a longer ipsilateral leg. This is usually self-limiting and rarely requires intervention.
- Compartment Syndrome: As discussed, this is an orthopaedic emergency. Vigilance for the 5 Ps (pain, pallor, paresthesia, pulselessness, paralysis) is paramount. Immediate cast removal (bivalving) and emergent fasciotomy are required if diagnosed.
- Neurovascular Injury: Direct trauma or iatrogenic injury during reduction or casting. Careful initial assessment and post-casting checks are essential. If identified, urgent consultation with a vascular surgeon is needed.
Remember, fellows, managing pediatric femur fractures with closed reduction and spica casting is a blend of art and science. It requires precision, patience, and a deep respect for the unique physiology of the growing child. By following these principles, we can ensure the best possible outcomes for our young patients.
REFERENCES
-
At union, acceptable angulation and shortening varies by age (Table 1).
-
Beaty JH. Femoral-shaft fractures in children and adolescents. J Am Acad Orthop Surg 1995;3:207–217.
-
Bridgman S, Wilson R. Epidemiology of femoral fractures in children in the West Midlands region of England 1991 to
-
J Bone Joint Surg Br 2004;86B:1152–1157.
-
Cassinelli EH, Young B, Vogt M, et al. Spica cast application in the emergency room for select pediatric femur fractures. J Orthop Trauma 2005;19:709–716.
-
Epps HR, Molenaar E, O’Connor DP. Immediate single-leg spica cast for pediatric femoral diaphysis fractures. J Pediatr Orthop 2006;26: 491–496.
-
Hinton RY, Lincoln A, Crockett MM, et al. Fractures of the femoral shaft in children: incidence, mechanisms, and sociodemographic risk factors. J Bone Joint Surg Am 1999;81A:500–509.
-
Illgen R II, Rodgers WB, Hresko MT, et al. Femur fractures in children: treatment with early sitting spica casting. J Pediatr Orthop 1998;18: 481–487.
-
Landin LA. Epidemiology of children’s fractures. J Pediatr Orthop 1997;6:79–83.
-
Large TM, Frick SL. Compartment syndrome of the leg after treatment of a femoral fracture with an early sitting spica cast: a report of two cases. J Bone Joint Surg Am 2003;85A:2207–2210.
-
Mubarak SJ, Frick S, Sink E, et al. Volkmann contracture and compartment syndromes after femur fractures in children treated with 90/90 spica casts. J Pediatr Orthop 2006;26:567–572.
-
Rewers A, Hedegaard H, Lezotte D, et al. Childhood femur fractures, associated injuries, and sociodemographic risk factors: a populationbased study. Pediatrics 2005;115:e543–552.
OUTCOMES
- Typically the spica cast is worn for 4 to 8 weeks, depending on the extent of the injury.
-
Infant fractures heal in 3 to 4 weeks.
-
Toddler fractures heal in 6 weeks.
-
On removal of the cast, children are encouraged to stand up and walk as soon as they are comfortable.
Table 1 Acceptable Angulation of the Femur VarusAnteriorAge Valgus Posterior Shortening Birth to 30 degrees 30 degrees 15 mm 2 years 2 to 5 years 15 degrees 20 degrees 20 mm 6 to 10 years 10 degrees 15 degrees 15 mm 11 years to 5 degrees 10 degrees 10 mm maturity Rockwood CA, Wilkins KE, Beaty JH, et al., eds. Rockwood and Wilkins’ fractures in children, ed
- Philadelphia: Lippincott Williams & Wilkins, 2001.
You Might Also Like