Mastering Lateral Ankle Ligament Repair: A Modified Brostrom Intraoperative Guide
Key Takeaway
This masterclass guides fellows through Modified Brostrom and Brostrom-Evans lateral ankle ligament repair. We cover comprehensive anatomy, meticulous preoperative planning, precise patient positioning, and a granular step-by-step intraoperative execution from incision to closure. Detailed pearls, pitfalls, and postoperative management ensure optimal outcomes for chronic ankle instability, emphasizing technique and rationale as if you are scrubbed in alongside me.
Introduction and Epidemiology
Lateral ankle injuries represent one of the most frequently encountered musculoskeletal pathologies in both athletic and general populations. Epidemiological data indicate an incidence rate as high as 7 per 1000 person-years in the general population, with a significantly higher prevalence among individuals participating in cutting and pivoting sports. Despite the high frequency of these injuries, the initial management remains predominantly non-operative. However, clinical outcomes demonstrate that 10% to 20% of acute lateral ankle sprains progress to chronic lateral ankle instability (CAI).


Chronic ankle instability manifests through a spectrum of clinical presentations, broadly categorized into functional instability and mechanical instability. Functional instability is characterized by the subjective sensation of the ankle "giving way" during dynamic activities, often driven by impaired proprioception, neuromuscular deficits, and perceived weakness. Mechanical instability refers to objective, demonstrable laxity of the lateral ligamentous complex, permitting joint motion beyond normal physiologic limits. Accurately distinguishing between functional and mechanical instability—or identifying their concurrent presence—is paramount for formulating evidence-based surgical treatment recommendations.
Pathogenesis of Lateral Ankle Instability
The classic mechanism of injury involves a sudden inversion force applied to the ankle while it is in a plantarflexed position. In plantarflexion, the narrower posterior portion of the talar dome rotates into the ankle mortise, inherently decreasing the bony stability of the tibiotalar joint and placing maximum tension on the lateral capsuloligamentous structures. The anterior talofibular ligament (ATFL) is the first structure to reach its ultimate tensile failure point. If the deforming force continues, the calcaneofibular ligament (CFL) is subsequently injured.


Ligamentous disruptions most commonly occur as midsubstance tears or as avulsions from their fibular or talar attachments. In the chronically sprained ankle, the ATFL often heals in an elongated state or becomes ill-defined, manifesting intraoperatively as a thickened, redundant capsular expansion rather than a distinct ligamentous band.
Natural History and Progression
While the majority of patients achieve satisfactory outcomes with functional rehabilitation, a subset remains at elevated risk for recurrent lateral ankle sprains. Failure to fully rehabilitate the neuromuscular control and proprioceptive pathways following an initial injury significantly increases this risk. The natural history of untreated chronic mechanical instability is characterized by repetitive microtrauma to the articular cartilage, leading to progressive loss of function, altered joint kinematics, and ultimately, the development of asymmetric osteoarthritic changes within the medial tibiotalar joint.


Surgical Anatomy and Biomechanics
A comprehensive understanding of the lateral ankle anatomy is essential for executing anatomic reconstructions like the modified Broström-Gould procedure. The lateral ankle ligament complex consists of three primary structures: the anterior talofibular ligament (ATFL), the calcaneofibular ligament (CFL), and the posterior talofibular ligament (PTFL).
Lateral Ankle Ligament Complex
The ATFL originates from the anterior margin of the distal fibula, approximately 10 mm proximal to the tip, and courses anteromedially to insert on the lateral aspect of the talar neck. It is an intracapsular but extrasynovial structure. Biomechanically, the ATFL limits anterior translation of the talus within the mortise when the ankle is in a neutral position. It becomes the primary restraint to inversion stress when the ankle is plantarflexed.


The CFL originates from the anterior aspect of the distal tip of the fibula and courses posteroinferiorly to insert on a small tubercle on the lateral wall of the calcaneus. The CFL is a robust, cord-like structure measuring approximately 4 to 6 mm in diameter and 13 mm in length. It is directed posteriorly at an angle of 10 to 45 degrees relative to the longitudinal axis of the fibula. The CFL functions as the primary restraint to inversion when the ankle is in a neutral or dorsiflexed position. It is intimately associated with the peroneal tendons, lying directly deep to them.


The PTFL is the strongest of the lateral ligaments and originates from the medial surface of the lateral malleolus, inserting onto the posterior tubercle of the talus. It is rarely injured except in severe ankle dislocations and plays a minimal role in isolated lateral ankle instability.
Dynamic Stabilizers and Retinacular Structures
The osseous anatomy plays a crucial role in ankle stability. The anterior margin of the talar dome is significantly wider than the posterior margin. During dorsiflexion, the wider anterior talus wedges into the distal tibiofibular mortise, providing inherent osseous stability. Conversely, during plantarflexion, the narrower posterior talus occupies the mortise, rendering the joint highly reliant on ligamentous restraints and more susceptible to inversion injuries.



The peroneal tendons (peroneus longus and brevis) serve as the primary dynamic stabilizers of the lateral ankle, actively resisting inversion forces. The inferior extensor retinaculum (IER) is a specialized, Y-shaped thickening of the crural fascia. Its stem originates from the sinus tarsi and the lateral calcaneus. The mobilization and advancement of the IER (the Gould modification) over the repaired ATFL and CFL constructs provide a critical secondary restraint, limiting inversion and significantly augmenting the strength of the traditional Broström repair.


Indications and Contraindications
Patient selection is the cornerstone of successful surgical intervention for lateral ankle instability. Patients typically present with a history of recurrent sprains elicited by minimal provocation, chronic lateral-sided pain, and a subjective feeling of apprehension during uneven ground ambulation.
Patient History and Physical Examination
A meticulous history should ascertain the duration of symptoms, the specific mechanisms triggering instability, the frequency of functional bracing requirements, and the outcomes of previous non-operative treatments (e.g., dedicated physical therapy focusing on peroneal strengthening and proprioception). If lateral ankle pain persists continuously between acute episodes of instability, the clinician must maintain a high index of suspicion for concomitant intra-articular pathology, such as osteochondral lesions of the talus (OCDs), anterior impingement, or peroneal tendon tears.


Physical examination must include palpation of the ATFL, CFL, syndesmosis, medial and lateral malleoli, peroneal tendons, base of the fifth metatarsal, and the anterior process of the calcaneus. The anterior drawer test evaluates ATFL integrity; a positive test is characterized by increased anterior talar translation with a soft or absent bony end point compared to the contralateral limb. The talar tilt test evaluates the CFL by applying an inversion force to the hindfoot with the ankle in neutral dorsiflexion.



| Clinical Scenario | Operative Indications | Non-Operative Indications |
|---|---|---|
| Primary Diagnosis | Chronic mechanical instability failing >3-6 months of targeted physical therapy. | Acute first-time lateral ankle sprain; functional instability without mechanical laxity. |
| Concomitant Pathology | Symptomatic osteochondral lesions of the talus (OCD); peroneal tendon tears; symptomatic os subfibulare. | Mild impingement symptoms responding to corticosteroid injections. |
| Patient Factors | High-demand athletes requiring return to pivoting sports; structural hindfoot varus (requires concurrent bony correction). | Sedentary lifestyle; poor surgical candidates; uncontrolled diabetes or severe peripheral vascular disease. |
| Contraindications | Active local infection; Charcot neuroarthropathy; severe uncorrected malalignment (relative contraindication for isolated soft tissue repair). | N/A |


Pre Operative Planning and Patient Positioning
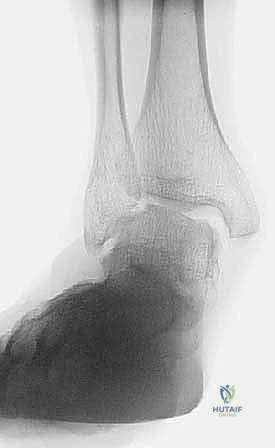
Thorough preoperative planning requires a comprehensive radiographic evaluation. Standard weight-bearing radiographs of the ankle (anteroposterior, lateral, and mortise views) are mandatory to assess for joint space narrowing, loose bodies, os subfibulare, and osseous alignment. Hindfoot alignment views (e.g., Saltzman view) are critical to rule out a cavovarus foot deformity, which, if left uncorrected, will lead to premature failure of the lateral ligament reconstruction.
Imaging Modalities
Stress radiography (anterior drawer and talar tilt views) can quantify mechanical laxity, though its clinical utility is debated due to variability in applied force and patient guarding. Magnetic Resonance Imaging (MRI) without contrast is highly recommended to evaluate the integrity of the ATFL and CFL, and more importantly, to identify concomitant soft tissue or chondral pathology. Up to 90% of patients with chronic lateral ankle instability exhibit associated intra-articular lesions, including OCDs, anterolateral impingement lesions, or loose bodies.



Operating Room Setup
The patient is placed in the supine position on a standard radiolucent operating table. A well-padded bump is placed under the ipsilateral hip to internally rotate the operative extremity, allowing the lateral malleolus to sit directly superiorly. A non-sterile thigh tourniquet or sterile calf tourniquet is applied to provide a bloodless surgical field. The entire lower extremity is prepped and draped in standard sterile fashion. Prophylactic intravenous antibiotics are administered prior to tourniquet inflation.


Detailed Surgical Approach and Technique
The surgical management of chronic lateral ankle instability typically begins with ankle arthroscopy, followed by the open modified Broström-Gould procedure.
Diagnostic Arthroscopy
Prior to the open ligamentous repair, diagnostic ankle arthroscopy is strongly advocated. Standard anteromedial and anterolateral portals are established. The joint is systematically inspected for synovitis, osteochondral lesions, loose bodies, and anterior tibial osteophytes. Anterolateral gutter synovitis and meniscoid lesions (hypertrophic scar tissue) are common in chronic instability and should be aggressively debrided with a motorized shaver and radiofrequency ablation wand to resolve impingement symptoms. Once intra-articular pathology is addressed, the arthroscopic fluid is evacuated, and the open procedure commences.



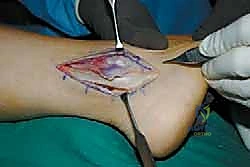
Open Surgical Approach
A 4 to 6 cm curvilinear incision is made just posterior to the anterior border of the distal fibula, extending distally toward the sinus tarsi. This incision allows optimal access to both the ATFL and CFL footprints while minimizing the risk of nerve injury.
Blunt dissection is utilized in the subcutaneous tissues. The surgeon must remain vigilant to identify and protect the intermediate dorsal cutaneous nerve (IDCN), a branch of the superficial peroneal nerve, which often crosses the surgical field anteriorly. Similarly, the sural nerve must be protected posteriorly, particularly during dissection near the peroneal tendon sheath and CFL.



The inferior extensor retinaculum (IER) is identified as a distinct fascial layer superficial to the joint capsule. The IER is sharply incised and carefully mobilized, preserving its integrity for later use in the Gould augmentation.


The anterior ankle capsule is then incised longitudinally along the anterior border of the fibula, leaving a 2 to 3 mm cuff of tissue attached to the bone to facilitate later repair, though modern techniques often utilize suture anchors directly into the fibula, rendering the tissue cuff less critical. The ATFL is inspected; it is frequently attenuated, scarred, or avulsed from the fibula.
To visualize the CFL, the peroneal tendon sheath is identified and retracted posteriorly. The CFL lies deep to the tendons, coursing from the fibular tip to the calcaneus.



Ligament Repair and Augmentation
The anatomic footprints of the ATFL and CFL on the distal fibula are identified and decorticated using a curette, rongeur, or motorized burr to expose bleeding cancellous bone. This step is critical to optimize biological healing of the soft tissue to bone.
Two metallic or biocomposite suture anchors (typically 2.5 mm to 3.5 mm in diameter) are placed into the distal fibula. The proximal anchor is positioned at the ATFL footprint (approximately 10 mm proximal to the distal tip), and the distal anchor is placed at the CFL footprint near the fibular tip.



Using a free needle or suture passing device, the sutures from the proximal anchor are passed through the ATFL and the adjacent anterior capsule using a horizontal mattress or Krackow configuration. The sutures from the distal anchor are passed through the substance of the CFL.
Before tying the knots, the foot is held in strict neutral dorsiflexion and slight eversion. This positioning is critical to restore the appropriate tension to the ligamentous complex. The sutures are tied sequentially, firmly securing the capsuloligamentous tissue to the decorticated fibular bed. An anterior drawer test is performed intraoperatively to confirm the restoration of mechanical stability.



Following the primary Broström repair, the Gould augmentation is performed. The previously mobilized proximal edge of the inferior extensor retinaculum (IER) is advanced superiorly and laterally over the repaired ligaments. It is sutured directly to the periosteum of the distal fibula or secured using the residual tails of the suture anchors. This augmentation limits inversion, reinforces the primary repair, and helps address subtle subtalar instability.



The subcutaneous tissues are closed in layers using absorbable sutures, and the skin is closed with a subcuticular stitch or nylon sutures. A sterile dressing is applied, and the extremity is placed in a well-padded short leg splint in neutral dorsiflexion and slight eversion.


Complications and Management
While the modified Broström-Gould procedure is highly successful, complications can occur and must be managed promptly to ensure optimal patient outcomes.
| Complication | Incidence | Etiology and Management Strategies |
|---|---|---|
| Nerve Injury (IDCN or Sural Nerve) | 3% - 10% | Caused by aggressive retraction or errant suture placement. Presents as numbness, paresthesias, or neuroma. Management includes gabapentinoids, desensitization, or surgical neuroma excision if conservative measures fail. |
| Recurrent Instability | 5% - 10% | Often due to unrecognized fixed hindfoot varus, premature return to sport, or poor tissue quality. Requires comprehensive re-evaluation. Salvage strategies include anatomic tendon reconstruction (e.g., using semitendinosus allograft) and corrective calc |
Clinical & Radiographic Imaging


























































You Might Also Like