SLAP Tears: Your Guide to Diagnosis & Treatment in Elbow Cases
Key Takeaway
This topic focuses on SLAP Tears: Your Guide to Diagnosis & Treatment in Elbow Cases, After failed conservative management for shoulder SLAP tears, an MR arthrogram classifies the injury using Snyder criteria. For instance, Type II tears often require labrum repair in younger, unstable patients, or biceps tenodesis for older individuals. Such precise treatment decisions are crucial for optimal recovery in complex orthopaedic conditions, including specific elbow cases slap.
Introduction to the Kinetic Chain Breakdown
In the realm of sports medicine and orthopedic trauma, the presentation of medial elbow pain in the overhead athlete is a ubiquitous diagnostic challenge. While the immediate clinical suspicion often gravitates toward the Ulnar Collateral Ligament (UCL) or flexor-pronator mass, a sophisticated orthopedic evaluation must account for the concept of regional interdependence. The title of this Grand Rounds presentation highlights a classic, yet frequently mismanaged, clinical scenario: the superior labrum anterior and posterior (SLAP) tear presenting masquerading as, or contributing directly to, elbow pathology.
When an overhead athlete sustains a SLAP lesion, the resulting microinstability and pain during the late cocking and acceleration phases of throwing fundamentally alter glenohumeral kinematics. To compensate for the inability to achieve maximal external rotation without pain, the athlete invariably alters their mechanics—often "dropping the elbow" or opening the trunk prematurely. This biomechanical compensation exponentially increases the valgus torque transmitted across the medial elbow, leading to secondary UCL strain, medial epicondylitis, or valgus extension overload. Therefore, treating the elbow without diagnosing the primary shoulder pathology will result in inevitable clinical failure. This comprehensive case study delineates the exhaustive diagnostic and surgical management of a complex SLAP tear driving secondary elbow symptoms in an elite overhead athlete.
Patient Presentation and History
Demographics and Chief Complaint
The patient is a 21-year-old right-hand-dominant male collegiate baseball pitcher presenting to the orthopedic clinic with a primary chief complaint of insidious onset right medial elbow pain and a precipitous drop in throwing velocity. The patient reports that his fastball velocity has decreased from 92 mph to 84 mph over the course of the current competitive season. He describes a sensation of a "dead arm" and notes that while the elbow pain is his primary limiting factor, he also experiences deep, vague anterior shoulder pain during the late cocking phase of his pitching delivery.
History of Present Illness
The patient denies any acute traumatic event, pop, or sudden tearing sensation in either the shoulder or the elbow. The symptoms began approximately three months prior, initially manifesting as delayed onset muscle soreness following high pitch-count outings. Over the ensuing weeks, the pain localized to the medial aspect of the elbow, specifically during the acceleration phase of throwing. He reports that rest and non-steroidal anti-inflammatory drugs (NSAIDs) provide temporary relief, but the symptoms recur immediately upon returning to the mound.
A detailed review of his throwing history reveals a recent transition from a starting rotation to a relief role, which altered his warm-up routine and recovery periods. He denies any radicular symptoms, numbness, or tingling in the ulnar nerve distribution. He has undergone six weeks of conservative management directed solely at the elbow, including physical therapy focusing on flexor-pronator strengthening and modalities, with no clinical improvement.
Biomechanical Throwing History
A meticulous biomechanical history is paramount. The patient’s pitching coach noted a recent, unintentional alteration in his mechanics. Video analysis demonstrates a decreased maximum shoulder external rotation during the late cocking phase and a lowered arm abduction angle at foot strike. This "dropped elbow" posture is a classic compensatory mechanism for deep shoulder pain. By lowering the arm slot, the athlete decreases the torsional "peel-back" forces on the superior labrum but inadvertently increases the valgus stress on the medial elbow. This history strongly suggests that the elbow pain is a secondary manifestation of a primary proximal kinetic chain deficit.
Clinical Examination Findings
Inspection and Scapular Assessment
Physical examination begins with the patient undressed to the waist to allow for bilateral comparison. Inspection reveals significant asymmetry in shoulder girdle musculature. There is noticeable hypertrophy of the right dominant shoulder, but closer inspection reveals mild atrophy of the infraspinatus fossa, raising suspicion for suprascapular nerve involvement or chronic disuse secondary to pain.
Assessment of scapular kinematics reveals a Type III scapular dyskinesis. At rest, the right shoulder demonstrates an inferior, protracted posture. During active elevation, there is early scapular elevation and lack of appropriate upward rotation and posterior tilt, consistent with the SICK scapula syndrome (Scapular malposition, Inferior medial border prominence, Coracoid pain and malposition, and dysKinesis of scapular movement).
Range of Motion and Glenohumeral Internal Rotation Deficit
Range of motion testing is critical in the overhead athlete. Forward flexion is symmetric at 170 degrees. However, assessment of rotation at 90 degrees of abduction reveals a profound Glenohumeral Internal Rotation Deficit (GIRD). The right shoulder demonstrates 125 degrees of external rotation and only 25 degrees of internal rotation, compared to the contralateral non-dominant shoulder which exhibits 100 degrees of external rotation and 60 degrees of internal rotation.
While the total arc of motion (150 degrees) is relatively preserved, the 35-degree loss of internal rotation significantly exceeds the accepted physiologic adaptation of 15-20 degrees. This pathologic GIRD is indicative of posterior capsular contracture, which shifts the glenohumeral center of rotation posterosuperiorly during the throwing motion, exacerbating the peel-back forces on the biceps-labral complex.
Special Tests for the Superior Labrum
A comprehensive battery of provocative tests is performed to isolate the superior labrum.
1. O'Brien Active Compression Test: Elicits deep shoulder pain when the arm is flexed to 90 degrees, adducted 10 degrees, and maximally internally rotated (thumb down) against resistance. The pain is significantly relieved when the arm is externally rotated (thumb up).
2. Crank Test: Positive for catching and pain when an axial load is applied to the humerus at 160 degrees of elevation with internal and external rotation.
3. Biceps Load Test II: The patient is placed supine, arm abducted to 120 degrees and maximally externally rotated. Resisted elbow flexion reproduces deep shoulder pain, highly specific for a SLAP lesion.
4. Dynamic Labral Shear Test: Moving the arm from a flexed position to an abducted and externally rotated position while maintaining a posterior shear force reproduces a painful click, confirming superior labral instability.
Concomitant Elbow Assessment
Given the chief complaint, a rigorous elbow examination is mandatory. Inspection reveals a normal carrying angle with no effusion. Palpation over the medial epicondyle and the sublime tubercle (insertion of the anterior bundle of the UCL) elicits mild tenderness.
1. Valgus Stress Test: Performed at 30 degrees of elbow flexion to unlock the olecranon from the fossa. There is a firm endpoint with no significant laxity compared to the contralateral side, though mild pain is noted.
2. Moving Valgus Stress Test: The elbow is rapidly extended from full flexion while maintaining a valgus torque. The patient reports mild apprehension and pain between 120 and 70 degrees, though less severe than his shoulder pain during provocative testing.
3. Tinel's Sign: Negative over the cubital tunnel.
4. Radiocapitellar Compression: Negative, ruling out lateral compartment pathology.
The clinical picture strongly points to a primary symptomatic SLAP tear with secondary, non-structural medial elbow stress.
Imaging and Diagnostics
Radiographic Evaluation
Standard orthogonal radiographs of both the shoulder and the elbow are obtained.
For the shoulder, an anteroposterior (AP) view in internal and external rotation, a true AP (Grashey view), an axillary lateral, and a Stryker notch view are evaluated. The radiographs demonstrate no acute osseous abnormalities, no evidence of Hill-Sachs or bony Bankart lesions, and a normal acromiohumeral interval. The Stryker notch view reveals no evidence of a Bennett lesion (exostosis at the posterior-inferior glenoid margin).
Elbow radiographs, including AP, lateral, and axial views, show no loose bodies, no osteophyte formation at the posteromedial olecranon (which would indicate Valgus Extension Overload), and no calcification within the UCL substance.
Magnetic Resonance Arthrography
The gold standard for diagnosing superior labral pathology is Magnetic Resonance Arthrography (MRA). The intra-articular administration of gadolinium distends the joint capsule, allowing for excellent visualization of labral tears, capsular volume, and the biceps anchor.
The MRA of the right shoulder is obtained in standard planes as well as the Abduction External Rotation (ABER) position. The axial and coronal oblique T1-weighted fat-suppressed images demonstrate contrast extending laterally between the superior labrum and the glenoid cartilage. Crucially, the contrast tracks posterior to the biceps anchor, indicating a posterior extension of the labral tear.
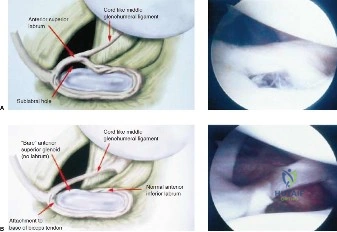
The ABER sequence is particularly valuable as it simulates the late cocking phase of throwing. In this position, the MRA clearly demonstrates the "peel-back" phenomenon, with the superior labrum lifting off the glenoid rim under the tension of the biceps tendon. There is also evidence of thickening of the posterior band of the inferior glenohumeral ligament (IGHL), corroborating the clinical finding of GIRD.
Advanced Elbow Imaging
To definitively rule out structural compromise of the elbow that would necessitate concurrent surgical intervention, a non-contrast MRI of the right elbow is acquired. The coronal and axial T2-weighted fat-suppressed sequences demonstrate a continuous, intact anterior bundle of the UCL with no high-grade partial or full-thickness tearing. There is mild periligamentous edema consistent with a grade I sprain. The flexor-pronator mass is intact, and there is no evidence of osteochondral lesions of the capitellum. This confirms the hypothesis that the elbow symptoms are a secondary biomechanical overload phenomenon.
Differential Diagnosis
The presentation of medial elbow pain combined with deep shoulder pain in an overhead athlete requires a broad differential diagnosis. The following table delineates the primary considerations, highlighting the distinguishing clinical and radiographic features.
| Condition | Primary Pathoanatomy | Key Clinical Findings | Imaging Hallmark |
|---|---|---|---|
| Type II SLAP Tear | Detachment of the superior labrum and biceps anchor from the superior glenoid rim. | Deep shoulder pain in late cocking, positive Biceps Load II, GIRD, secondary medial elbow pain. | MRA shows contrast tracking beneath the superior labrum, positive peel-back on ABER sequence. |
| UCL Tear (Anterior Bundle) | Attenuation or rupture of the anterior band of the medial ulnar collateral ligament. | Acute pop or chronic medial elbow pain during acceleration, positive Moving Valgus Stress Test, laxity at 30° flexion. | MRI shows high signal, discontinuity, or T-sign (contrast leakage) at the sublime tubercle insertion. |
| Valgus Extension Overload (VEO) | Impingement of the posteromedial olecranon into the olecranon fossa due to chronic valgus stress. | Posterior elbow pain during deceleration/follow-through, loss of terminal extension, crepitus. | Radiographs show posteromedial olecranon osteophytes; MRI shows chondromalacia/loose bodies. |
| Flexor-Pronator Mass Strain | Microtrauma or tearing of the common flexor tendon origin at the medial epicondyle. | Medial elbow pain worse with resisted wrist flexion and pronation, localized tenderness over epicondyle. | MRI demonstrates hyperintense signal within the flexor-pronator origin without UCL involvement. |
| Internal Impingement | Pathologic contact between the articular surface of the rotator cuff and the posterosuperior glenoid. | Posterior shoulder pain in extreme abduction/external rotation, positive relocation test. | MRA shows undersurface cuff fraying and posterosuperior labral fraying (kissing lesions). |
Surgical Decision Making and Classification
Snyder Classification of Superior Labral Lesions
The surgical decision-making process is heavily reliant on the accurate classification of the SLAP lesion. The original classification by Snyder describes four distinct types:
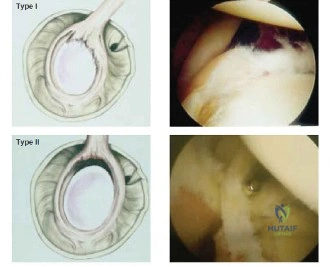
* Type I: Fraying and degeneration of the superior labrum with an intact biceps anchor. Typically treated with arthroscopic debridement.
* Type II: Detachment of the superior labrum and the biceps anchor from the superior glenoid. This is the classic lesion seen in overhead athletes due to the peel-back mechanism. It is further subdivided into anterior, posterior, or combined anterior-posterior detachment.
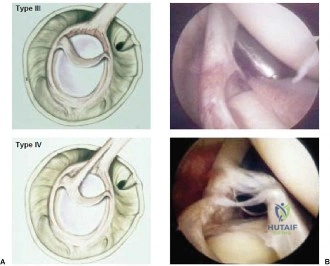
* Type III: A bucket-handle tear of the superior labrum with an intact biceps anchor. Treated with excision of the bucket-handle fragment.
* Type IV: A bucket-handle tear of the superior labrum that extends into the biceps tendon. Treatment depends on the extent of biceps involvement (repair vs. tenodesis).
Subsequent authors have expanded this classification (Types V through X) to include extensions into the anterior labrum (Bankart), the posterior labrum, or the middle glenohumeral ligament. Based on the MRA and clinical exam, our patient presents with a classic Type II SLAP lesion with posterior extension.
Operative Versus Nonoperative Management
The management of Type II SLAP tears in overhead athletes remains one of the most debated topics in sports medicine. Nonoperative management, consisting of a prolonged period of rest, posterior capsular stretching (sleeper stretches, cross-body adduction), and periscapular strengthening, is the mandatory first line of treatment.
However, in the elite collegiate or professional pitcher who fails a dedicated 3-to-6-month conservative program and exhibits kinetic chain breakdown (manifesting as secondary elbow pain), surgical intervention becomes indicated. The inability to pitch at a competitive velocity without pain dictates the need for anatomic restoration of the biceps-labral complex to restore the stable fulcrum necessary for the throwing motion.
SLAP Repair Versus Biceps Tenodesis
A critical juncture in surgical decision-making is choosing between a primary SLAP repair and a subpectoral biceps tenodesis. Recent literature has shown a trend toward biceps tenodesis in patients over the age of 30, or in non-throwing athletes, due to lower complication rates, reduced postoperative stiffness, and highly predictable pain relief.
However, in the elite pitcher under the age of 25, primary SLAP repair remains the procedure of choice. The long head of the biceps provides essential anterior and superior glenohumeral stability during the extreme ranges of motion required in pitching. A tenodesis alters the length-tension relationship and removes this dynamic stabilizer, which can severely compromise throwing velocity and control. Therefore, the decision is made to proceed with an arthroscopic Type II SLAP repair, coupled with careful evaluation of the posterior capsule.

Surgical Technique and Intervention
Patient Positioning and Anesthesia
The patient is taken to the operating room and placed under general endotracheal anesthesia supplemented with an interscalene regional nerve block for postoperative pain control. The patient is positioned in the lateral decubitus position. While the beach chair position is preferred by some surgeons for shoulder arthroscopy, the lateral decubitus position provides superior access to the superior and posterior labrum and allows for precise control of arm traction.
The right arm is placed in a pneumatic traction sleeve with 10 pounds of longitudinal traction and 5 pounds of lateral traction, maintaining the arm in approximately 45 degrees of abduction and 20 degrees of forward flexion. All bony prominences are meticulously padded, and the peroneal nerve of the down leg is protected.
Portal Placement and Diagnostic Arthroscopy
A standard posterior viewing portal is established 2 cm inferior and 1 cm medial to the posterolateral corner of the acromion. A diagnostic arthroscopy is performed using a 30-degree arthroscope. The articular surfaces of the humeral head and glenoid are inspected, revealing pristine cartilage. The rotator cuff is examined from the articular side, showing no evidence of partial-thickness tearing or internal impingement.
An anterior-inferior working portal is established in the rotator interval, just superior to the subscapularis tendon, using an outside-in spinal needle localization technique to ensure the proper angle of approach to the glenoid. A clear cannula is inserted.
Probing the superior labrum confirms the MRA findings. There is a profound Type II SLAP lesion. When the arm is taken out of traction and placed into the ABER position, the biceps anchor and superior labrum displace medially and posteriorly over the glenoid rim, definitively demonstrating a positive arthroscopic peel-back sign.
Labral Preparation and Anchor Insertion
Preparation of the superior glenoid rim is the most critical step for biological healing. An arthroscopic elevator and a motorized shaver are used to mobilize the superior labrum and debride any interposed fibrous tissue. A curved arthroscopic rasp is then utilized to decorticate the superior glenoid neck, extending down to bleeding subchondral bone to create an optimal healing environment. Care is taken not to violate the articular cartilage.
To achieve the optimal trajectory for anchor placement, an accessory high anterior-superior portal (the Port of Wilmington) is established. This portal is created percutaneously, entering just off the anterolateral tip of the acromion, passing through the muscular portion of the supraspinatus. This trajectory allows for a "deadman's angle" of 45 degrees to the superior glenoid face.
A drill guide is introduced through the percutaneous portal. The first anchor is planned for the posterior aspect of the biceps anchor (approximately the 10:30 position on a right shoulder). The drill is advanced, aiming slightly medial to avoid the articular cartilage, but strictly avoiding deep medial penetration to protect the suprascapular nerve, which courses approximately 1-2 cm medial to the superior glenoid rim. A 2.9 mm biocomposite double-loaded suture anchor is impacted into place.
Suture Management and Knot Tying
Suture management in the tight superior joint space requires meticulous technique to avoid tangling. A penetrator instrument is introduced through the anterior portal, passing through the superior labrum posterior to the biceps tendon. One limb of the suture is retrieved and pulled through the labrum.
A simple suture configuration is chosen over a mattress configuration, as mattress sutures can evert the labrum and create a non-anatomic bumper that may impinge on the humeral head. The knot is tied using a sliding, locking knot (e.g., Weston or SMC knot) backed up by three alternating half-hitches. The knot is carefully positioned away from the articular surface to prevent postoperative chondral abrasion.
A second 2.9 mm anchor is placed anterior to the biceps tendon (approximately the 1:30 position) using the same technique. Following the placement of both anchors, the labrum is probed, demonstrating a robust, anatomic restoration of the biceps anchor. The arm is again placed in the ABER position, confirming that the peel-back phenomenon has been completely eliminated.
Given the patient's preoperative GIRD, the posterior capsule is carefully evaluated. While tight, it is determined that aggressive postoperative physical therapy will be sufficient to address the contracture, and a surgical posterior capsular release is deferred to avoid iatrogenic posterior instability. The joint is thoroughly lavaged, the portals are closed with non-absorbable sutures, and the patient is placed in a supportive abduction sling.
Post Operative Protocol and Rehabilitation
The rehabilitation of a throwing athlete following a SLAP repair is arduous, typically requiring 6 to 9 months before a return to competitive pitching. The protocol is divided into four distinct phases, balancing the need to protect the healing labrum with the necessity of preventing glenohumeral stiffness.
Phase One Protection
Weeks 0 to 4:
The primary goal is protection of the surgical repair. The patient remains in the abduction sling continuously, removing it only for hygiene and physical therapy.
* Range of Motion: Passive range of motion (PROM) is initiated immediately but is strictly limited. Forward flexion is limited to 90 degrees for the first two weeks, progressing to 120 degrees by week four. External rotation is strictly limited to neutral (0 degrees) to prevent torsional stress on the biceps anchor.
* Biceps Precautions: Active elbow flexion and supination are strictly prohibited to prevent traction on the superior labrum.
* Scapular Work: Scapular retractions, depressions, and periscapular isometrics are initiated immediately to combat the preoperative scapular dyskinesis.
Phase Two Early Motion
Weeks 5 to 8:
The sling is discontinued. The goal is to gradually restore full, symmetric range of motion.
* Range of Motion: Active-assisted range of motion (AAROM) and active range of motion (AROM) are initiated. External rotation is gradually increased by 10-15 degrees per week. Cross-body adduction stretching and sleeper stretches are heavily emphasized to address the posterior capsular tightness and GIRD.
* Strengthening: Submaximal, pain-free rotator cuff isometrics are begun. Active elbow flexion is permitted, but resisted biceps curls are avoided until week 8.
* Kinetic Chain: Core strengthening and lower extremity kinetic chain integration exercises are initiated.
Phase Three Strengthening
Weeks 9 to 16:
Full ROM should be achieved by week 10. The focus shifts to dynamic stabilization and advanced strengthening.
* Rotator Cuff: Isotonic strengthening of the rotator cuff and periscapular stabilizers (rhomboids, serratus anterior, lower trapezius) using resistance bands and light weights.
* Plyometrics: Two-handed plyometric exercises (e.g., chest passes with a medicine ball) are introduced at week 12, progressing to one-handed plyometrics by week 14.
* Neuromuscular Control: Rhythmic stabilization exercises at various angles of elevation are utilized to restore proprioception.
Phase Four Return to Throwing
Weeks 16 to 24+:
Clearance to begin an interval throwing program requires full, pain-free ROM, normal scapular kinematics, and isokinetic strength testing demonstrating at least 90% strength compared to the contralateral side.
* Interval Throwing Program (ITP): The ITP begins with flat-ground throwing at 45 feet, progressing in distance (up to 120-150 feet) and intensity over several weeks.
* Mound Work: Once flat-ground long toss is tolerated without pain, the pitcher transitions to throwing off the mound, initially focusing on fastballs at 50% effort. Breaking balls, which place different torsional stresses on the arm, are introduced last.
* Elbow Monitoring: Throughout the ITP, the patient's elbow is closely monitored. With the restoration of shoulder stability and mechanics, the secondary valgus overload on the elbow should be entirely resolved.
Clinical Pearls and Pitfalls
Diagnostic Pearls
- The Kinetic Chain Illusion: Never evaluate an elbow in isolation in an overhead athlete. Medial elbow pain is frequently the "victim" of a proximal "culprit." A thorough evaluation of scapular kinematics and glenohumeral rotation is mandatory.
- GIRD Assessment: Accurate measurement of GIRD requires stabilizing the scapula to prevent compensatory scapulothoracic motion. A loss of internal rotation greater than 20 degrees compared to the non-dominant side, or a total arc of motion deficit greater than 5 degrees, is highly pathologic and predictive of SLAP lesions.
- ABER Positioning: Standard MRA can miss subtle peel-back lesions. Always request an ABER
