Elbow Arthroscopy for Degenerative Joint Disease: An Intraoperative Masterclass
Key Takeaway
This masterclass guides fellows through arthroscopic débridement for elbow degenerative joint disease. We'll cover essential anatomy, meticulous patient positioning, and a granular, real-time surgical execution from initial incision to hardware application. Extensive pearls, pitfalls, and postoperative protocols ensure comprehensive learning for managing elbow osteoarthritis with arthroscopy.
Comprehensive Introduction and Patho-Epidemiology
Primary degenerative arthritis of the elbow is a relatively uncommon but profoundly debilitating clinical entity that presents unique challenges to the orthopedic surgeon. Unlike the weight-bearing joints of the lower extremity, where osteoarthritis is ubiquitous and largely driven by axial loading and senility, primary osteoarthritis of the elbow is distinctly mechanical and demographic-specific. It predominantly afflicts middle-aged male laborers, elite weightlifters, overhead throwing athletes, and individuals who rely on their upper extremities for mobility, such as manual wheelchair users or those dependent on crutches. In these populations, the elbow is subjected to repetitive microtrauma, supraphysiologic axial loads, and sheer forces that exceed the intrinsic reparative capacity of the articular cartilage.
The pathogenesis of this condition is best understood as a relentless, self-perpetuating "vicious cycle" of mechanical impingement and biologic degradation. The cascade typically initiates with focal cartilage loss and fragmentation, secondary to repetitive sheer stress. This fragmentation liberates chondral and osteochondral debris into the joint space, which are nourished by synovial fluid and progressively enlarge to form intra-articular loose bodies. Concurrently, the joint responds to altered biomechanics and capsular traction by forming robust, hypertrophic osteophytes. These reactive bony prominences characteristically develop at the joint margins—most notably at the tips of the coronoid and olecranon processes, as well as within the depths of the coronoid, radial, and olecranon fossae.
As these osteophytes hypertrophy and loose bodies proliferate, they precipitate the third phase of the cycle: severe joint contracture. The bony excrescences physically block terminal extension and flexion, creating a mechanical impingement. The anterior and posterior joint capsules, subjected to chronic irritation and recurrent micro-hemorrhage from this impingement, undergo fibrotic thickening and contracture. This triad of cartilage loss, osteophyte formation, and capsular contracture manifests clinically as a progressive, painful loss of motion. Patients typically present with pain localized to the extremes of their arc of motion—a hallmark sign of bony impingement. Crucially, pain in the mid-arc of motion is frequently absent, a clinical pearl that helps differentiate primary osteoarthritis from inflammatory arthropathies (like rheumatoid arthritis) where pan-articular synovitis causes pain throughout the entire range of motion.
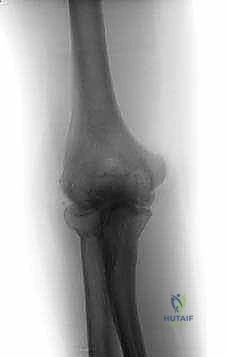
A comprehensive clinical evaluation must also prioritize the assessment of the ulnar nerve. It is exceedingly common for these patients to present with concurrent ulnar neuropathy, manifesting as paresthesias in the ring and small fingers, intrinsic muscle weakness, or diminished grip strength. The ulnar nerve is rendered vulnerable by the underlying pathology; a contracted medial capsule, medial osteophytosis, and overall joint deformity can decrease the volume of the cubital tunnel, leading to traction or compression neuropathy. Documenting these findings preoperatively is absolutely critical, as it dictates the necessity for concurrent open ulnar nerve decompression or transposition during the arthroscopic intervention. Standard anteroposterior and lateral radiographs are usually sufficient to confirm the diagnosis, revealing classic signs: joint space preservation in the early stages, progressing to subchondral sclerosis, hypertrophic osteophytosis, and radiopaque loose bodies.
Detailed Surgical Anatomy and Biomechanics
A profound, three-dimensional understanding of elbow anatomy is the bedrock of safe and effective arthroscopic intervention. The elbow is an unforgiving, highly congruent, and compact joint surrounded by critical neurovascular structures that are separated from the arthroscopic instruments by mere millimeters. The osseous architecture comprises three distinct articulations: the humeroulnar joint (a highly constrained hinge joint dictating flexion and extension), the humeroradial joint, and the proximal radioulnar joint (which together facilitate pronation and supination). In the degenerative elbow, the critical biomechanical failure occurs at the extremes of the humeroulnar arc. Anteriorly, the hypertrophic coronoid process impacts prematurely against a narrowed, osteophyte-filled coronoid fossa, mechanically blocking flexion. Posteriorly, a prominent olecranon tip wedges into an overgrown olecranon fossa, obliterating terminal extension. Arthroscopic osteocapsular arthroplasty aims to directly address these specific points of bony impingement.
The neurovascular anatomy dictates our portal placement and limits the extent of our capsular releases. The ulnar nerve represents the most significant hazard during posterior and posteromedial instrumentation. It courses posterior to the medial epicondyle within the cubital tunnel, lying directly superficial to the medial collateral ligament (MCL) and the posteromedial joint capsule. During a posteromedial capsulectomy or when resecting medial osteophytes, the surgeon is working perilously close to the nerve. Furthermore, the ulnar nerve is prone to anterior subluxation in a subset of the population; failure to identify a hypermobile nerve preoperatively can lead to catastrophic iatrogenic transection during portal establishment or shaver utilization.
Anteriorly, the radial and median nerves are at risk. The radial nerve courses anterior to the lateral epicondyle, traversing the anterior compartment before dividing into the superficial sensory branch and the deep posterior interosseous nerve (PIN) at the level of the radiocapitellar joint. The anterolateral portal must be meticulously placed to avoid these structures, typically utilizing a "soft spot" just anterior and proximal to the radiocapitellar articulation. The median nerve and the brachial artery lie centrally over the anterior joint capsule, separated from the joint space only by the brachialis muscle. While standard portals do not routinely endanger the median nerve, aggressive anterior capsulectomy or the inadvertent plunging of a burr or shaver through the anterior capsule can result in devastating neurovascular injury.
To navigate this complex anatomy safely, we rely on specific muscular intervals and precise portal trajectories. The direct posterior portal traverses the triceps tendon, providing a safe and expansive view of the olecranon fossa. Anterior portals are designed to pass through internervous and intermuscular planes where possible, or to safely displace muscles without penetrating their main bellies. The fundamental principle of elbow arthroscopy is that the joint capsule is the definitive barrier protecting the neurovascular structures; therefore, maintaining capsular integrity until a formal, controlled release is performed is paramount.
Exhaustive Indications and Contraindications
The decision to proceed with arthroscopic osteocapsular debridement must be predicated on a thorough failure of non-operative modalities and a clear alignment of patient expectations with surgical realities. Operative intervention is never the first line of treatment. Patients must have exhausted a comprehensive regimen of conservative care, including activity modification (avoiding heavy lifting, repetitive impact, and terminal loading), optimized regimens of nonsteroidal anti-inflammatory drugs (NSAIDs), and potentially intra-articular corticosteroid injections to manage acute inflammatory flares. When these measures fail to provide durable relief, and the patient experiences unacceptable limitations in their activities of daily living or vocation, surgical intervention becomes warranted.
The primary indication for arthroscopic debridement is functionally limiting pain, specifically mechanical pain occurring at the extremes of motion (terminal flexion or extension) due to bony impingement. Secondary indications include mechanical symptoms such as catching, locking, or painful crepitus caused by intra-articular loose bodies. Loss of motion itself is a relative indication; while arthroscopic release can significantly improve the arc of motion, patients must be counseled that the primary goal is pain relief, and a completely "normal" range of motion is rarely achieved in a severely degenerative joint. The presence of concurrent, symptomatic ulnar neuropathy that has failed conservative management is a strong indication for a combined procedure, typically involving an open ulnar nerve decompression or transposition prior to the arthroscopic portion of the case.
Contraindications must be strictly respected to avoid exacerbating the patient's condition or precipitating catastrophic complications. Absolute contraindications include active local or systemic infection, and severe distortion of the normal bony architecture (such as that seen in severe post-traumatic deformity or advanced inflammatory arthropathy with profound joint subluxation), which precludes safe arthroscopic navigation. In these scenarios, open procedures or total elbow arthroplasty may be more appropriate.
Relative contraindications require nuanced clinical judgment. A history of prior ulnar nerve transposition is a significant relative contraindication to standard arthroscopic portal placement, as the altered anatomical course of the nerve makes it highly susceptible to injury. In such cases, the nerve must be formally explored and protected via a small open incision before any medial arthroscopic work is undertaken. Similarly, extensive prior open elbow surgery or severe extra-articular soft tissue contractures may limit the efficacy and safety of an arthroscopic approach.
| Category | Indications | Contraindications (Absolute & Relative) |
|---|---|---|
| Clinical Presentation | - Disabling pain at extremes of motion - Mechanical locking/catching - Failure of >6 months conservative care - Symptomatic loose bodies |
- Pain throughout entire arc of motion (suggests inflammatory/pan-articular disease) - Active local or systemic infection (Absolute) |
| Anatomic/Structural | - Radiographic evidence of impingement (osteophytes) - Capsular contracture limiting functional ROM - Concurrent ulnar neuropathy requiring release |
- Severe architectural distortion (post-traumatic) (Absolute) - Profound joint instability/subluxation (Absolute) |
| Surgical History | - Virgin elbow joint - Previous simple arthroscopy |
- Prior ulnar nerve transposition (Relative - requires open exploration) - Extensive prior open trauma surgery (Relative) |
Pre-Operative Planning, Templating, and Patient Positioning
Meticulous preoperative planning is the cornerstone of a successful arthroscopic osteocapsular arthroplasty. While standard plain radiographs are mandatory, advanced imaging is frequently utilized in our practice. A non-contrast Computed Tomography (CT) scan, ideally with three-dimensional surface rendering, is invaluable for complex cases. It allows the surgeon to precisely map the size, location, and morphology of osteophytes within the coronoid and olecranon fossae, and to identify occult loose bodies that may be obscured by overlying bone on plain films. This mental templating allows the surgeon to anticipate the exact volume of bone resection required to restore the fossae and eliminate impingement, streamlining the intraoperative workflow.
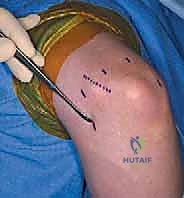
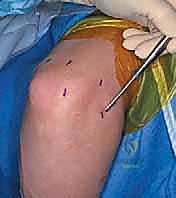
In the preoperative holding area, a final, rigorous physical examination is conducted, with an exclusive focus on neurovascular mapping. The ulnar nerve is palpated along its course in the cubital tunnel, and any tendency for subluxation over the medial epicondyle during dynamic flexion and extension is noted. The precise anatomical course of the ulnar nerve, the medial and lateral epicondyles, the radial head, and the tip of the olecranon are marked on the skin with a sterile surgical marker. This step is critical because once the joint is distended with fluid during the procedure, these vital bony landmarks become obscured by soft tissue swelling, making blind portal placement hazardous.
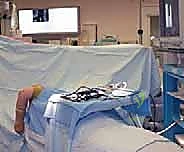
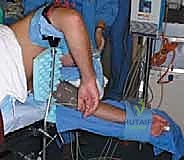
Patient positioning is a critical variable that significantly impacts surgical ergonomics and patient safety. We strongly advocate for the lateral decubitus position. The patient is placed under general endotracheal anesthesia and positioned laterally on a beanbag with all bony prominences meticulously padded. The operative arm is brought over a padded arm holder (such as a dedicated elbow positioner) attached to the side of the operating table. This setup allows the elbow to rest at approximately 90 degrees of flexion with the forearm hanging freely, permitting an unhindered, 360-degree manipulation of the joint.
Crucially, the arm holder must be positioned so that the elbow is elevated slightly higher than the level of the right atrium. This elevation utilizes gravity to assist with fluid egress, thereby minimizing extravasation into the soft tissues of the arm and forearm—a critical factor in preventing iatrogenic compartment syndrome. A nonsterile pneumatic tourniquet is applied high on the brachium but is generally not inflated unless visualization becomes compromised by bleeding, as routine inflation can tether the neurovascular structures and increase the risk of ischemic injury. Finally, the C-arm fluoroscopy unit is brought into the field from the anterior aspect of the patient, positioned to allow seamless acquisition of true anteroposterior and lateral views without requiring the surgeon to break scrub or reposition the patient.
Step-by-Step Surgical Approach and Fixation Technique
The surgical execution demands a systematic, compartmentalized approach, beginning with joint distention to maximize the capsular volume and displace neurovascular structures away from the portal trajectories. We identify the "soft spot"—the anconeus triangle bordered by the lateral epicondyle, the radial head, and the olecranon tip. An 18-gauge spinal needle is introduced here, directed towards the center of the joint. A palpable "pop" confirms capsular penetration. We then instill 20 to 30 mL of sterile saline. This distention is paramount; it acts as a fluid wedge, pushing the radial nerve anteriorly and the ulnar nerve medially, dramatically increasing the safety margin for subsequent portal establishment.
Anterior Compartment Debridement and Release
We begin in the anterior compartment, addressing the pathology responsible for flexion deficits. The anterolateral portal is established first, serving as our primary viewing portal. A small stab incision is made just anterior to the radiocapitellar joint. Utilizing a blunt hemostat, meticulous dissection is carried down to the distended capsule to avoid the radial nerve branches. A blunt trocar and cannula are then introduced into the joint. We utilize a 4.0-mm, 30-degree arthroscope. Upon entry, a diagnostic sweep is performed, assessing the radiocapitellar and ulnohumeral articulations, identifying chondral damage, synovitis, and loose bodies.
The anteromedial working portal is then established using a rigorous "inside-out" technique to protect the median nerve and brachial artery. The arthroscope is advanced to the medial aspect of the joint. A blunt Wissinger rod or switching stick is introduced through the anterolateral cannula, passing across the joint under direct visualization, and directed towards the anteromedial capsule, just anterior to the medial epicondyle. The rod is pushed firmly to tent the skin. A stab incision is made over the tented skin, and the rod is advanced out. A cannula is then retrograded over the rod into the joint. This ensures the portal trajectory originates from within the safe confines of the joint space, pushing vital structures away rather than blindly piercing towards them.

With the anterior portals established, the debridement commences. We utilize a 4.0-mm aggressive shaver to perform a subtotal anterior synovectomy, clearing the view of the coronoid process and fossa. Loose bodies are meticulously localized and extracted using arthroscopic graspers. The core of the anterior procedure is the osteocapsular arthroplasty. Using a 4.0-mm round motorized burr, the hypertrophic osteophytes on the tip of the coronoid process are systematically resected until the normal anatomic contour is restored. Next, the coronoid and radial fossae are addressed. The burr is used to excavate the reactive bone filling these fossae, deepening them to accommodate the coronoid and radial head during terminal flexion. If a severe anterior capsular contracture is present, an anterior capsulectomy is performed. Using an arthroscopic punch or radiofrequency wand, the capsule is released from lateral to medial. Extreme vigilance is required here; once the capsule is breached, the fibers of the brachialis muscle are exposed, and the median nerve and brachial artery lie immediately anterior to this muscle belly.
Posterior Compartment Debridement and Release
Following completion of the anterior work, attention is shifted to the posterior compartment to address extension deficits. The direct posterior portal is established approximately 3 cm proximal to the olecranon tip, passing directly through the triceps tendon. A posterolateral portal is also established at the lateral margin of the triceps. The arthroscope is introduced, revealing the olecranon fossa and the tip of the olecranon process.
The posterior pathology is often characterized by a massive olecranon tip osteophyte and a fossa filled with fibrotic tissue, loose bodies, and reactive bone. A shaver is used to clear the soft tissue from the olecranon fossa. The burr is then introduced to resect the olecranon tip osteophyte. The resection must be aggressive enough to allow the olecranon to seat deeply into the fossa during terminal extension, but conservative enough to preserve the insertion of the triceps tendon and avoid destabilizing the ulnohumeral joint. The olecranon fossa itself is then burred out, removing peripheral osteophytes and deepening the recess.
The most perilous portion of the posterior procedure is the clearance of the posteromedial gutter. This recess frequently harbors occult loose bodies and osteophytes that impinge on the medial column. However, the ulnar nerve lies immediately adjacent to the posteromedial capsule. When working in this area, the shaver blade must always face laterally, away from the capsule, and suction should be minimized to avoid drawing the capsule (and potentially the nerve) into the cutting window. If a posteromedial capsular release is deemed necessary to improve flexion, it must be performed with exquisite care, often utilizing a hand-held punch rather than motorized instruments, maintaining constant awareness of the ulnar nerve's proximity.
Complications, Incidence Rates, and Salvage Management
Despite the minimally invasive nature of arthroscopy, the elbow's unforgiving anatomy means that complications, when they occur, can be devastating. The surgeon must be acutely aware of the potential pitfalls and possess the knowledge to execute salvage strategies. Neurologic injury is the most feared complication, with an overall incidence ranging from 1% to 10% in the literature, though permanent severe injuries are rare (<1%). The ulnar nerve is most frequently compromised, usually due to direct trauma during posteromedial portal placement, thermal injury from radiofrequency devices, or traction injury from prolonged positioning. The radial nerve is at risk during anterolateral portal establishment, and the median nerve during anterior capsulectomy. Prevention is paramount: strict adherence to anatomical landmarks, joint distention prior to portal entry, the use of blunt trocars, and the "inside-out" technique for medial portals are non-negotiable standards of care.
Infection, while rare in arthroscopy (incidence <0.5%), can present as superficial portal site cellulitis or deep septic arthritis. A unique complication to elbow arthroscopy is prolonged portal site leakage, driven by the high intra-articular pressures generated during the procedure and the relatively thin subcutaneous tissue envelope. This leakage usually resolves with compressive dressings and brief immobilization, but persistent drainage warrants evaluation for deep infection. Fluid extravasation leading to compartment syndrome of the forearm or arm is a catastrophic, albeit rare, complication. It is mitigated by utilizing gravity (elevating the arm), keeping pump pressures as low as possible (typically 30-40 mmHg), using outflow cannulas, and minimizing the duration of the procedure.
Heterotopic ossification (HO) and postoperative stiffness are significant biological complications. The trauma of the burr and the release of the capsule can stimulate reactive bone formation, which can severely compromise the newly acquired range of motion. The incidence of clinically significant HO varies, but high-risk patients (those with prior trauma or severe hypertrophic osteoarthritis) may benefit from prophylaxis. Salvage management for recurrent stiffness or HO typically involves a period of aggressive static progressive splinting; if this fails, a secondary, open arthrolysis and excision of heterotopic bone may be required once the bone has fully matured (typically 6-12 months postoperatively).
| Complication | Estimated Incidence | Prevention Strategy | Salvage / Management |
|---|---|---|---|
| Neurologic Injury (Ulnar/Radial/Median) | 1% - 10% (Transient) <1% (Permanent) |
Blunt trocars, joint distention, inside-out medial portal, avoid suction near capsule. | Immediate neurology consult, EMG at 6 weeks if no recovery. Open exploration if transection suspected. |
| Fluid Extravasation / Compartment Syndrome | <1% | Low pump pressure (30-40 mmHg), elevate arm, limit surgical time, use outflow. | Immediate cessation of procedure, fasciotomy if compartment pressures are elevated and sustained. |
| Heterotopic Ossification (HO) | 3% - 5% | Meticulous bone dust clearance, gentle tissue handling. | Prophylactic Indomethacin or localized radiation in high-risk patients. Late open excision. |
| Recurrent Stiffness | 10% - 15% | Aggressive early rehab, adequate intraoperative bony resection. | Static progressive splinting, manipulation under anesthesia (rarely effective), revision arthrolysis. |
Phased Post-Operative Rehabilitation Protocols
The success of an arthroscopic osteocapsular arthroplasty is intrinsically linked to the quality and immediacy of the postoperative rehabilitation. The surgical procedure merely "unlocks" the joint; it is the physical therapy that maintains the motion and prevents the recurrence of capsular contracture. The rehabilitation protocol must be aggressive yet carefully phased to respect soft tissue healing and manage postoperative inflammation.
The Immediate Post-Operative Phase (Days 0-7) prioritizes edema control and the immediate initiation of motion. Unlike many orthopedic procedures where a period of immobilization is favored, the elbow requires immediate mobilization to prevent fibrinous adhesions from organizing into mature scar tissue. Patients are typically placed in a bulky, compressive soft dressing without rigid splinting in flexion. Active and active-assisted range of motion (ROM) exercises for flexion, extension, pronation, and supination are initiated on postoperative day one. Cryotherapy and elevation are employed aggressively to manage hemarthrosis and swelling. To combat the tendency for the anterior capsule to re-contract, patients are often fitted with a custom anterior extension splint to be worn exclusively at night, holding the elbow in maximum tolerable extension while they sleep.
The Intermediate Phase (Weeks 1-4) focuses on pushing the limits of the newly acquired arc of motion. Supervised physical therapy sessions become more rigorous, incorporating gentle, sustained capsular stretching and joint mobilization techniques. If the patient exhibits a lag in achieving their intraoperative ROM, static progressive splinting (such as turnbuckle splints) may be introduced during the day for 30-to-60-minute intervals. Strengthening exercises are initiated cautiously, beginning with submaximal isometrics for the biceps, triceps, and forearm musculature, ensuring that these exercises do not provoke a significant inflammatory flare that could paradoxically increase stiffness.
The Late Phase (Weeks 4-12 and beyond) represents the transition to functional restoration. Aggressive strengthening is incorporated, utilizing isotonic and eventually isokinetic modalities
