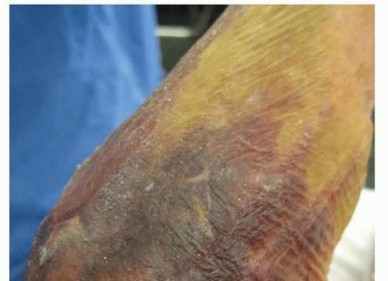
Ulnohumeral (Outerbridge-Kashiwagi) Arthroplasty: An Intraoperative Masterclass
Key Takeaway
This masterclass provides a comprehensive, intraoperative guide to Ulnohumeral (Outerbridge-Kashiwagi) Arthroplasty for primary elbow osteoarthritis. We'll meticulously cover surgical anatomy, patient positioning, step-by-step execution including osteophyte removal and foraminectomy, critical pearls, potential pitfalls, and essential postoperative management. Fellows will gain a granular understanding of this technique to restore elbow function and alleviate pain.
Introduction and Epidemiology
Primary osteoarthritis of the elbow is a relatively uncommon but disabling disorder that affects mostly middle-aged men who use the upper extremity in a repetitive fashion. Typically, patients are heavy manual workers or athletes. Osteoarthritis affects the elbow less frequently than other major joints.
Early stages of arthritis of the elbow may be characterized primarily by pain at the extremes of motion, with some loss of terminal extension and flexion. Some patients present with pain carrying an object with the arm in extension. More advanced stages may present with pain and crepitus throughout the range of motion, stiffness, or locking. Rotation of the forearm may be spared, depending on radiocapitellar involvement.
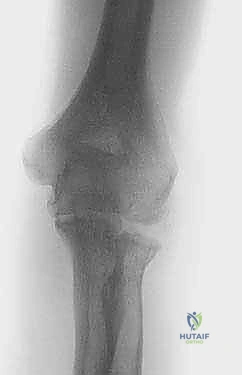
Radiographs show osteophyte formation on the coronoid and olecranon but relatively preserved joint space at the early stages. More advanced stages may be associated with significant joint space narrowing.
Multiple operative techniques have been described for treatment of primary osteoarthritis of the elbow: débridement arthroplasty, interposition arthroplasty, the Outerbridge-Kashiwagi procedure, arthroscopic débridement, and total elbow replacement.
Ulnohumeral (Outerbridge-Kashiwagi) arthroplasty was first described in 1978 and became popular a few years later. It is based on a posterior approach to the elbow, removal of any olecranon spur and bony overgrowth of the olecranon fossa, trephination of the fossa to expose the anterior capsule, and excision of the coronoid osteophyte.
Recent advancements allow the procedure to be performed with arthroscopic fenestration of the olecranon fossa, débridement, and removal of loose bodies.
Symptomatic osteoarthritis of the elbow has been found to affect about 2% of the general population and represents only 1% to 2% of all patients diagnosed with degenerative arthritis. It has a predilection for males, with a ratio of 4:1 or 5:1. It is most commonly seen in middle-aged and older patients. The majority of patients experience symptoms in their dominant extremity.
The exact etiology of primary degenerative elbow arthritis is still unknown. It is generally attributed to overuse. About 60% of patients report employment or hobbies/sports requiring repetitive use of the limb. The few younger patients who present likely have a predisposing condition such as osteochondritis dissecans.
There are characteristic pathologic changes that occur within the elbow joint: osteophyte formation on the olecranon, olecranon fossa, coronoid, and coronoid fossa. In early stages, the joint space is relatively well preserved. The periarticular bone is typically sclerotic, reflecting the chronic, repetitive axial loading and shear forces transmitted across the joint.

Unlike weight-bearing joints such as the hip or knee, where cartilage degradation is the primary inciting event, primary osteoarthritis of the elbow is primarily a disease of capsular contracture and osteophytic impingement. The central articular cartilage of the ulnohumeral joint often remains remarkably intact until the very late stages of the disease process. The peripheral osteophytes effectively block terminal flexion and extension, leading to secondary capsular contracture. As the osteophytes fracture or fragment, intra-articular loose bodies develop, contributing to mechanical locking and accelerated third-body wear.

Surgical Anatomy and Biomechanics
The elbow joint consists of three separate articulations: the ulnohumeral, the radiocapitellar, and the proximal radioulnar joints. The elbow has two main functions: to position the hand in space and to stabilize the upper extremity for motor activities and power.
The normal range of elbow flexion-extension is 0 to 150 degrees, whereas normal forearm pronation-supination is 80 degrees of each. A 100-degree flexion-extension arc of motion (30 to 130 degrees) is required for normal activities of daily living. Functional forearm rotation is quoted as 100 degrees (50 degrees pronation and 50 degrees supination).

Osseous Architecture
The condyles articulate at the elbow joint, as the trochlea medially and the capitellum laterally. The articular surface is tilted about 30 degrees anterior to the axis of the humeral shaft and aligns in approximately 6 degrees of valgus. The coronoid fossa and the olecranon fossa, just proximal to the articular surface, accommodate the coronoid process and olecranon process of the ulna in the extremes of flexion and extension, respectively.
The olecranon and coronoid process coalesce to form the greater sigmoid notch, the main articulating portion of the proximal ulna. It is often not completely covered with articular cartilage centrally; this devoid area is known as the bare area or the non-articular transverse ridge. Surgeons must not mistake this normal anatomic variant for a chondral defect during joint inspection.

The Olecranon Fossa and Septum
The central aspect of the distal humerus contains a thin diaphanous bone separating the anterior coronoid fossa from the posterior olecranon fossa. In a small percentage of the normal population, this septum is naturally patent (the supratrochlear foramen). In the Outerbridge-Kashiwagi procedure, this septum is intentionally fenestrated. The structural integrity of the distal humerus relies heavily on the medial and lateral columns (the supracondylar ridges). Preservation of these columns during the trephination process is paramount to prevent iatrogenic supracondylar fractures.

Soft Tissue and Neurovascular Structures
The ulnar nerve is the most critical neurovascular structure at risk during posterior approaches to the elbow. It courses posterior to the medial epicondyle within the cubital tunnel, roofed by Osborne's ligament and the flexor carpi ulnaris aponeurosis. Any posterior approach requires careful identification, mobilization, and protection of the ulnar nerve.
The collateral ligaments provide critical stability. The medial ulnar collateral ligament (MUCL), specifically its anterior bundle, is the primary restraint to valgus stress. The lateral ulnar collateral ligament (LUCL) is the primary restraint to varus and posterolateral rotatory instability. The Outerbridge-Kashiwagi procedure is designed to be an extra-ligamentous procedure, meticulously avoiding disruption of the collateral ligament origins on the medial and lateral epicondyles.

Indications and Contraindications
Patient selection is the primary determinant of success in ulnohumeral arthroplasty. The ideal candidate is a high-demand patient (e.g., laborer, weightlifter, throwing athlete) with pain localized to the extremes of flexion and extension, preserved mid-arc motion, and radiographic evidence of impingement but preserved ulnohumeral joint space.
Patients presenting with pain throughout the entire arc of motion typically have advanced cartilaginous wear and are poor candidates for joint-preserving procedures. In these cases, total elbow arthroplasty or interposition arthroplasty may be required, though these procedures carry significant lifting restrictions that are often unacceptable to the typical demographic presenting with primary elbow osteoarthritis.
Operative vs Non Operative Management
| Modality | Indications | Clinical Presentation | Expected Outcomes |
|---|---|---|---|
| Non-Operative Management | Mild to moderate OA, patient unwilling to undergo surgery | Intermittent pain, mild loss of terminal extension | Temporary relief; does not alter disease progression. Relies on NSAIDs, bracing, and intra-articular corticosteroid/hyaluronic acid injections. |
| Outerbridge-Kashiwagi Arthroplasty | Primary OA with terminal impingement pain, failed conservative therapy | Pain at extremes of ROM, preserved mid-arc, locking/catching from loose bodies | Significant pain relief at extremes of motion, improvement in ROM (average 15-20 degrees), return to heavy labor. |
| Total Elbow Arthroplasty | Advanced OA, inflammatory arthritis, low-demand patient | Severe pain throughout ROM, bone-on-bone articulation, severe instability | Excellent pain relief, but permanent 5-10 lb lifting restriction. Contraindicated in laborers. |
| Interposition Arthroplasty | Advanced OA in a young, high-demand patient | Severe pain, failed O-K procedure, bone-on-bone articulation | Unpredictable outcomes, potential for instability, requires prolonged rehabilitation. |

Absolute and Relative Contraindications
Absolute contraindications for the Outerbridge-Kashiwagi procedure include active intra-articular or periarticular infection, advanced joint space destruction (bone-on-bone arthritis), and gross multidirectional instability.
Relative contraindications include inflammatory arthropathies (e.g., rheumatoid arthritis), as the disease process affects the entire articular surface rather than just the periphery. Severe preoperative ulnar neuropathy may require a concomitant ulnar nerve transposition. Prior surgical procedures that have compromised the medial or lateral columns represent a relative contraindication due to the increased risk of iatrogenic fracture during fossa fenestration.
Pre Operative Planning and Patient Positioning
Thorough preoperative planning begins with high-quality orthogonal radiographs of the elbow. Anteroposterior (AP) and lateral views will demonstrate the extent of anterior and posterior osteophyte formation, the presence of loose bodies, and the preservation of the central joint space.

Advanced Imaging Modalities
A non-contrast Computed Tomography (CT) scan with three-dimensional (3D) reconstructions is highly recommended. The CT scan allows for precise mapping of osteophytes, accurate measurement of the medial and lateral column widths, and identification of occult loose bodies hidden within the fossae. The thickness of the olecranon fossa septum can be measured to determine the appropriate depth of trephination.

Patient Positioning and Anesthesia
The procedure is typically performed under general anesthesia, often supplemented with a regional block (e.g., supraclavicular or infraclavicular nerve block) for postoperative pain control.
Positioning can be either lateral decubitus or prone, depending on surgeon preference.
1. Lateral Decubitus: The patient is placed in the lateral position with the operative arm supported over a padded post (e.g., a Montreal bar). The forearm hangs freely, allowing the elbow to be flexed to 90 degrees or fully extended during the procedure. This position provides excellent access to the posterior compartment and facilitates intraoperative fluoroscopy.
2. Prone: The patient lies prone with the arm abducted 90 degrees and the elbow flexed over a padded arm board.
A sterile tourniquet is applied high on the brachium to ensure a bloodless surgical field. The arm is prepped and draped in standard sterile fashion, ensuring the entire upper extremity from the axilla to the fingertips is accessible.

Detailed Surgical Approach and Technique
The Outerbridge-Kashiwagi procedure requires meticulous soft tissue handling, precise bone resection, and thorough dynamic testing. The following details the open technique, though the principles remain identical for the arthroscopic equivalent.
Incision and Superficial Dissection
A straight posterior midline incision is made, beginning approximately 5 cm proximal to the tip of the olecranon and extending 3 to 4 cm distally along the ulnar crest. The incision is curved slightly radially around the tip of the olecranon to prevent a painful scar directly over the bony prominence.
Full-thickness fasciocutaneous flaps are elevated medially and laterally. The medial flap must be elevated with caution to avoid injury to the ulnar nerve.

Ulnar Nerve Management
The ulnar nerve is identified proximal to the cubital tunnel and traced distally. The cubital tunnel retinaculum (Osborne's ligament) is released. The nerve is neurolysed and protected throughout the procedure. If the patient has preoperative symptoms of cubital tunnel syndrome or if the nerve subluxates anteriorly during flexion after release, a formal anterior transposition (subcutaneous or submuscular) should be performed at the conclusion of the arthroplasty.
Deep Dissection and Triceps Management
Access to the posterior humerus can be achieved via a triceps-splitting or a triceps-sparing (paratricipital) approach.
* Triceps-Splitting: A longitudinal incision is made through the midline of the triceps tendon and muscle belly. The medial and lateral halves of the triceps are elevated off the posterior humerus subperiosteally.
* Triceps-Sparing: The medial and lateral borders of the triceps are identified, and the entire extensor mechanism is mobilized and retracted medially or laterally to access the posterior humerus.
The posterior capsule is typically thickened and contracted. A posterior capsulectomy is performed to expose the olecranon fossa and the tip of the olecranon.

Posterior Debridement
Once the olecranon fossa is exposed, the hypertrophic osteophytes on the tip and medial/lateral borders of the olecranon are identified. Using a high-speed burr or an osteotome, the olecranon tip is resected. Care must be taken not to resect more than 10-15% of the olecranon to avoid compromising the insertion of the triceps tendon or inducing ulnohumeral instability.
Loose bodies within the posterior compartment are extracted. The osteophytes lining the periphery of the olecranon fossa are debrided until the normal anatomic contours of the fossa are restored.

Trephination of the Olecranon Fossa
This is the hallmark of the Outerbridge-Kashiwagi procedure. The goal is to create a fenestration through the distal humerus to access the anterior compartment.
A high-speed burr or a specialized trephine is used to penetrate the thin osseous septum separating the olecranon and coronoid fossae. The fenestration is gradually widened to a diameter of approximately 12 to 15 mm.
Crucial Step: The surgeon must maintain at least 1 cm of intact cortical bone on both the medial and lateral columns. Over-resection of the columns significantly increases the risk of postoperative supracondylar humerus fractures. The fenestration should be perfectly circular or slightly oval to minimize stress risers.

Anterior Debridement via Fenestration
Once the fenestration is complete, the anterior capsule is visualized. If the capsule is contracted, it can be carefully released using a scalpel or arthroscopic punch passed through the defect.
The elbow is flexed, which brings the coronoid process into view through the fenestration. Using a burr or pituitary rongeurs, the osteophytes on the tip of the coronoid are excised. Anterior loose bodies are irrigated and extracted through the posterior fenestration. This "push-pull" technique allows comprehensive clearance of the anterior joint without requiring a separate anterior surgical approach.

Dynamic Testing and Closure
After debridement, the elbow is taken through a full range of motion. The surgeon assesses for any residual bony impingement or soft tissue tethering. Impingement should be relieved at both terminal flexion and extension.
The surgical site is thoroughly irrigated to remove all bone debris, which could act as a nidus for heterotopic ossification. The triceps split is repaired with heavy non-absorbable sutures. The tourniquet is deflated, and meticulous hemostasis is achieved. The subcutaneous tissues and skin are closed in layers. A sterile compressive dressing and a posterior splint in extension are applied.
Complications and Management
While generally safe and effective, ulnohumeral arthroplasty carries specific risks inherent to elbow surgery and the specific biomechanical alterations created by the fenestration.

Complication Profile and Salvage Strategies
| Complication | Incidence | Etiology/Pathoanatomy | Management and Salvage Strategy |
|---|---|---|---|
| Ulnar Neuropathy | 5% - 10% | Traction injury during retraction, postoperative hematoma, or perineural fibrosis. | Postoperative observation if mild. If severe or progressive, requires formal surgical decompression and anterior transposition. |
| Heterotopic Ossification (HO) | 3% - 8% | Bone debris left in the soft tissues, aggressive dissection, or inherent patient predisposition. | Prophylaxis is key (Indomethacin or single-dose radiation). Established, symptomatic HO requires delayed surgical excision once the bone is fully mature (typically 6 months post-op). |
| Supracondylar Fracture | < 2% | Over-resection of the medial or lateral columns during trephination, creating a stress riser. | Requires immediate open reduction and internal fixation (ORIF) with dual orthogonal or parallel plating. |
| Persistent Stiffness/Pain | 10% - 15% | Inadequate resection of osteophytes, failure to release capsular contracture, or progression of central joint OA. | Aggressive physical therapy. If failed, consider arthroscopic debridement or conversion to total elbow/interposition arthroplasty. |
| Triceps Weakness | 2% - 5% | Inadequate repair of the triceps split or over-resection of the olecranon tip. | Graduated strengthening. Rarely requires surgical revision unless there is a complete avulsion. |
Prevention of Heterotopic Ossification
Given the extensive bony resection and burring involved, meticulous irrigation is mandatory. Many surgeons routinely prescribe a course of non-steroidal anti-inflammatory drugs (NSAIDs), such as Indomethacin 75 mg sustained-release daily for 3 to 6 weeks, as prophylaxis against heterotopic ossification. In high-risk patients (e.g., those with a history of HO or traumatic brain injury), a single dose of localized radiation therapy (700 cGy) administered within 24 to 48 hours postoperatively is highly effective.
Post Operative Rehabilitation Protocols
The success of the Outerbridge-Kashiwagi procedure relies heavily on the postoperative rehabilitation protocol. The primary goal is to maintain the range of motion achieved in the operating room while preventing capsular scarring.
Phase 1: Immediate Postoperative Period (Days 0-14)
- Immobilization: The patient is placed in a bulky compressive dressing and a removable posterior splint. The elbow is typically splinted in near-full extension, as extension is the most difficult motion to regain.
- Motion: Active and active-assisted range of motion (A/AAROM) exercises are initiated within 24 to 48 hours postoperatively. The patient removes the splint multiple times a day to perform flexion, extension, pronation, and supination exercises.
- Edema Control: Cryotherapy and elevation are strictly enforced to minimize swelling, which can mechanically block motion and increase pain.
Phase 2: Intermediate Phase (Weeks 2-6)
- Splinting: The daytime splint is discontinued. Static progressive night splinting may be utilized if the patient is losing terminal extension or flexion.
- Strengthening: Gentle isometric exercises are introduced. Isotonic strengthening of the biceps, triceps, and forearm musculature begins around week 4, provided the triceps repair (if a splitting approach was used) is healing adequately.
Phase 3: Advanced Rehabilitation (Weeks 6-12)
- Return to Activity: Progressive resistance exercises are advanced. Patients can typically return to light duty work by week 6 and heavy manual labor or weightlifting by weeks 10 to 12, depending on their recovery of strength and absence of pain.
- Expectations: Patients must be counseled that maximal improvement in range of motion and pain relief may take up to 6 months to achieve.
Summary of Key Literature and Guidelines
The foundational literature for this procedure stems from Outerbridge and Kashiwagi's original 1978 publication, which demonstrated the efficacy of a posterior approach for debriding anterior and posterior osteophytes via a transcortical fenestration.
In the 1990s, Bernard Morrey popularized the term "ulnohumeral arthroplasty" and published extensive series demonstrating durable outcomes. Morrey's data indicated that approximately 75% to 80% of patients achieved significant pain relief, with an average increase in the flexion-extension arc of 20 to 30 degrees. The most reliable improvement is seen in the alleviation of terminal impingement pain.
More recently, the advent of elbow arthroscopy has shifted the paradigm. Arthroscopic ulnohumeral arthroplasty (the arthroscopic O-K procedure) has been shown in multiple comparative studies to yield equivalent improvements in range of motion and pain scores compared to the open technique. The arthroscopic approach offers the advantages of smaller incisions, less soft tissue trauma, and potentially faster early rehabilitation. However, arthroscopic fenestration of the olecranon fossa is technically demanding, carries a steeper learning curve, and places anterior neurovascular structures (such as the brachial artery and median nerve) at risk if capsular penetration occurs during anterior burring.
Current academic consensus suggests that both open and arthroscopic ulnohumeral arthroplasties are highly effective, joint-preserving options for the young, active patient with primary elbow osteoarthritis. The choice of technique should be dictated by the surgeon's experience, the size and location of the osteophytes, and the presence of concomitant pathology requiring intervention.
Clinical & Radiographic Imaging
















You Might Also Like