Arthroscopic Management of Elbow Valgus Extension Overload: A Masterclass
Key Takeaway
This masterclass guides fellows through arthroscopic treatment of valgus extension overload. We cover detailed anatomy, prone positioning, and meticulous intraoperative steps for posteromedial olecranon spur excision. Emphasizing ulnar nerve protection and UCL assessment, we discuss portal placement, instrument use, and postoperative care, preparing you for complex elbow cases and managing potential complications.
Introduction and Epidemiology
Valgus extension overload (VEO) of the elbow represents a complex constellation of pathologies predominantly observed in the overhead-throwing athlete. The repetitive, high-velocity kinematics of the overhead throwing motion—most notably in baseball pitchers, javelin throwers, and tennis players—impart massive valgus torque across the elbow joint during the late cocking and early acceleration phases of the throwing cycle. This repetitive stress cascade is characterized by medial compartment distraction, lateral compartment compression, and posterior compartment impingement.
The pathogenesis of VEO is intrinsically linked to the attenuation of the medial stabilizing structures. As the ulnar collateral ligament (UCL) experiences microtrauma and subsequent plastic deformation from incomplete recovery cycles, the highly constrained osseous anatomy of the posterior elbow joint is subjected to abnormal kinematics. This subtle valgus instability allows the olecranon to deviate medially and impinge abnormally within the posteromedial olecranon fossa during the deceleration and follow-through phases of throwing, which involve rapid elbow extension.




Chronic posteromedial impingement inevitably leads to chondral lesions, reactive osteophyte formation on the posteromedial aspect of the olecranon, and the generation of intra-articular loose bodies. Patients typically present with a history of progressive posterior or posteromedial elbow pain, mechanical symptoms such as catching or locking, and a measurable loss of terminal elbow extension. In the competitive pitcher, this structural and mechanical deficit manifests clinically as a precipitous decrease in throwing velocity and a loss of control, with pain peaking during the acceleration and deceleration phases of the throw.
Surgical Anatomy and Biomechanics
Osseous Articulations and Ligamentous Restraints
The elbow is a highly congruent, constrained hinge joint dependent on both osseous architecture and capsuloligamentous integrity for stability. The bony articulation of the ulnohumeral joint provides primary stability to varus and valgus forces at extremes of motion—specifically at angles of less than 20 degrees and greater than 120 degrees of flexion. However, soft tissues are the chief stabilizers between 20 and 120 degrees, which is the precise arc of motion where the majority of athletic activity and peak throwing torques occur.
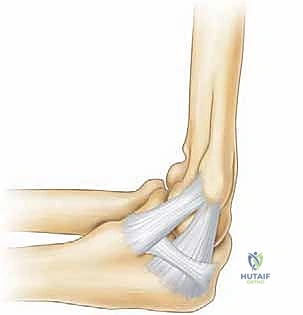
The ulnar collateral ligament (UCL) complex is the primary restraint to valgus stress. It is anatomically composed of three distinct segments the anterior band, the posterior band, and the transverse ligament (Cooper's ligament). The anterior band is the most critical biomechanical structure and is further subdivided into the anterior and posterior bundles, which perform reciprocal functions throughout the arc of flexion. The anterior bundle is taut in extension, while the posterior bundle becomes taut in deeper flexion.


UCL insufficiency can be remarkably subtle. In vitro ligament-sectioning studies have demonstrated that cutting the anterior band of the UCL results in only a 3-degree difference in valgus opening. Yet, in the context of the overhead athlete, this microscopic laxity is sufficient to alter the contact mechanics of the olecranon within its fossa.
Pathomechanics of Valgus Extension Overload
When the UCL fails to adequately resist the valgus torque of throwing, the resultant medial joint opening forces the olecranon tip to wedge against the medial wall of the olecranon fossa. This repetitive abutment shears the articular cartilage and stimulates the formation of a posteromedial osteophyte.


Concurrently, the radial head is driven into the capitellum, leading to lateral compartment chondromalacia or osteochondritis dissecans (OCD) lesions. The natural history of untreated VEO includes progressive posteromedial olecranon osteophytosis, secondary ulnar nerve irritation (ulnar neuritis) due to the proximity of the osteophyte to the cubital tunnel, progressive loss of extension, and eventual posterior compartment osteoarthritis.


Indications and Contraindications
The management of VEO dictates a careful algorithmic approach, differentiating between isolated posterior impingement, primary UCL failure, and combined pathology.
| Indication Category | Specific Clinical Scenarios |
|---|---|
| Non-Operative Management | First-line treatment for all non-mechanical VEO; Mild to moderate pain without loose bodies; Asymptomatic osteophytes discovered incidentally; Early-stage UCL attenuation without frank rupture. |
| Operative Management (Arthroscopic) | Failure of 3-6 months of directed conservative therapy; Presence of mechanical symptoms (locking, catching) due to loose bodies; Symptomatic posteromedial osteophytes causing extension block and pain; Chondral flap lesions in the posterior compartment. |
| Operative Management (Combined) | VEO accompanied by frank, symptomatic UCL rupture (requires concurrent UCL reconstruction); Severe ulnar neuritis (requires concurrent ulnar nerve transposition/decompression). |
Diagnostic Evaluation
Arthroscopic debridement is contraindicated in patients with asymptomatic osteophytes or those whose primary symptom is medial elbow pain secondary to gross UCL instability without posterior mechanical symptoms. Resecting an osteophyte in the presence of an incompetent UCL without reconstructing the ligament will exacerbate valgus instability, as the osteophyte often acts as a secondary, albeit pathologic, bony restraint to valgus stress.


Pre Operative Planning and Patient Positioning
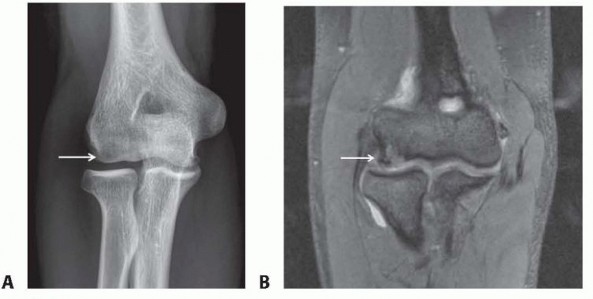
Preoperative imaging is paramount. Standard anteroposterior, lateral, and oblique radiographs of the elbow are required. The lateral view is particularly useful for identifying the posteromedial osteophyte and any loose bodies within the olecranon fossa. An axial view of the olecranon can further delineate posteromedial osseous overgrowth. Magnetic Resonance Imaging (MRI), preferably an MR Arthrogram (MRA), is highly recommended to evaluate the structural integrity of the UCL, assess the articular cartilage of the radiocapitellar joint, and map the exact location of posterior loose bodies.
Patient Positioning Options
Elbow arthroscopy for VEO can be performed in the lateral decubitus, prone, or supine suspended positions. The lateral decubitus position is highly favored in academic centers for its excellent access to the posterior compartment and airway security.
The patient is placed in the lateral decubitus position with the operative arm draped over a well-padded bolster or held in a specialized arm holder. The elbow must be allowed to flex to at least 90 degrees and extend fully. A non-sterile tourniquet is applied high on the brachium. Bony landmarks, including the medial epicondyle, lateral epicondyle, olecranon tip, and radial head, are meticulously outlined. The course of the ulnar nerve is palpated and marked to ensure its protection during portal placement and capsular distension.


Detailed Surgical Approach and Technique
Portal Establishment and Diagnostic Arthroscopy
Following the induction of general anesthesia, a thorough Examination Under Anesthesia (EUA) is performed. The moving valgus stress test and milking maneuver are executed to assess for gross UCL insufficiency, which may alter the surgical plan.
The joint is insufflated with 20-30 mL of normal saline through the soft spot (direct lateral portal) to displace neurovascular structures anteriorly. A standard 4.0-mm, 30-degree arthroscope is utilized.
The proximal anteromedial portal is established first, remaining anterior to the medial intermuscular septum to protect the ulnar nerve. Diagnostic arthroscopy of the anterior compartment is performed, evaluating the coronoid, the anterior capsule (looking for undersurface tearing indicative of valgus instability), and the radiocapitellar joint (assessing for lateral compression chondromalacia). An anterolateral portal is established under direct visualization for instrumentation.


Posterior Compartment Debridement and Osteophyte Resection
The core of the VEO procedure occurs in the posterior compartment. The arthroscope is redirected or placed into a posterolateral portal, located approximately 3 cm proximal to the olecranon tip, just lateral to the triceps tendon. A direct posterior portal or accessory posterolateral portal is established for instrumentation.
- Debridement and Loose Body Removal: The olecranon fossa is systematically inspected. Synovitis and scar tissue are debrided using a 4.0-mm oscillating shaver to expose the osseous anatomy. Any loose bodies, which frequently hide in the deep recesses of the fossa or the posteromedial gutter, are extracted.
- Identification of the Osteophyte: The elbow is taken through a dynamic range of motion. The impingement of the posteromedial olecranon osteophyte against the medial wall of the olecranon fossa during terminal extension is directly visualized.
- Osteophyte Resection: A high-speed 4.0-mm arthroscopic burr is introduced. Resection targets the abnormal posteromedial osseous overgrowth. Critical Surgical Pearl: The resection must be limited strictly to the pathologic osteophyte. Biomechanical studies have definitively shown that resecting more than 3 mm of the normal olecranon tip removes critical osseous constraint, exponentially increasing strain on the UCL and precipitating iatrogenic valgus instability. The normal contour of the olecranon must be preserved.
- Ulnar Nerve Protection: During posteromedial resection, the surgeon must remain acutely aware of the medial capsule. Violation of the posteromedial capsule places the ulnar nerve at immediate risk of thermal or mechanical injury from the burr. The burr should always be oriented with the cutting surface facing laterally or distally, away from the medial capsule.
- Dynamic Assessment: Following resection, the elbow is again taken through full extension and valgus stress. The surgeon must confirm that the impingement has been eliminated and that the olecranon tracks smoothly within the fossa without abutting the medial wall.


Complications and Management
Arthroscopic management of VEO is generally safe, but complications in the highly constrained and neurovascularly dense elbow joint can be devastating to an overhead athlete's career.
| Complication | Incidence | Etiology and Pathomechanics | Salvage and Management Strategy |
|---|---|---|---|
| Iatrogenic Valgus Instability | 5-10% | Over-resection of the normal olecranon tip (>3mm), removing secondary osseous stabilizers and overloading a previously attenuated UCL. | Immediate cessation of throwing; prolonged bracing. If symptomatic instability persists, formal open UCL reconstruction (Tommy John surgery) is required. |
| Ulnar Nerve Injury | 2-5% | Direct mechanical injury from posteromedial capsular violation with a burr/shaver, or thermal injury. Traction neuropraxia from fluid extravasation. | Intraoperative recognition requires immediate open exploration. Postoperative neuropraxia is observed; if non-resolving or severe, ulnar nerve decompression and anterior transposition are indicated. |
| Portal Site Neuromas | <2% | Injury to the Medial Antebrachial Cutaneous (MABC) nerve during anteromedial portal placement, or the Posterior Antebrachial Cutaneous nerve. | Prevention via meticulous superficial dissection (nick and spread technique). Management includes gabapentinoids, local injections, or surgical excision of the neuroma and burying the stump. |
| Heterotopic Ossification (HO) | 1-3% | Aggressive bony resection, capsular trauma, or inadequate postoperative mobilization. | Prophylaxis with NSAIDs (Indomethacin) in high-risk patients. If mature and limiting ROM, open surgical excision after 6-12 months is required. |
Prevention of Iatrogenic Instability
The most critical error in VEO surgery is the failure to recognize underlying UCL insufficiency prior to osteophyte resection. The posteromedial osteophyte develops as a compensatory mechanism to restrict abnormal valgus opening. If a surgeon aggressively resects this osteophyte in a patient with a compromised UCL, the primary restraint is gone, the secondary osseous restraint is removed, and the patient will experience catastrophic valgus instability upon return to throwing. Preoperative MRA and thorough EUA are non-negotiable steps to prevent this outcome.
Post Operative Rehabilitation Protocols
Rehabilitation following arthroscopic treatment of VEO is phased, biological, and strictly criteria-based rather than purely time-based. The primary goals are the restoration of terminal extension, protection of the medial stabilizing structures, and a graduated return to the extreme kinematics of overhead throwing.
Phased Return to Throwing
Phase 1: Immediate Postoperative Period (Days 0-14)
The elbow is typically placed in a soft compressive dressing. A posterior splint is rarely needed unless concomitant procedures were performed. Cryotherapy and elevation are critical to minimize hemarthrosis. Active and active-assisted range of motion (ROM) exercises for the elbow, wrist, and shoulder are initiated on postoperative day 1. The goal is to achieve full symmetrical ROM by the end of week 2, with particular emphasis on regaining terminal extension, which is often lost preoperatively. Valgus stress is strictly avoided.
Phase 2: Intermediate Phase (Weeks 2-6)
Once full ROM is achieved and incisions are healed, focus shifts to muscular endurance and proprioception. Isotonic strengthening of the forearm flexors and pronators (the dynamic stabilizers of the medial elbow) is initiated. Scapular stabilization and rotator cuff strengthening are integrated, as proximal kinetic chain deficits frequently contribute to distal elbow pathology.
Phase 3: Advanced Strengthening (Weeks 6-10)
Plyometric exercises are introduced. Two-hand plyometrics progress to one-hand plyometrics. Eccentric strengthening of the elbow flexors and extensors is emphasized to prepare the joint for the massive deceleration forces experienced during the follow-through phase of throwing.
Phase 4: Return to Throwing (Weeks 10+)
Clearance for an interval throwing program requires painless, full ROM, normal clinical valgus stability, and isokinetic strength metrics equal to the contralateral extremity. The interval throwing program begins with flat-ground throwing at 45 feet, progressively increasing distance and volume. Pitchers eventually progress to throwing off the mound, initially focusing on fastballs before reintroducing breaking pitches, which place higher torsional loads on the elbow. Full return to competitive pitching typically occurs between 3 to 5 months postoperatively, assuming no concurrent UCL reconstruction was required.
Summary of Key Literature and Guidelines
The academic understanding of Valgus Extension Overload is heavily founded on the seminal biomechanical and clinical studies of the past three decades.
Andrews and colleagues first comprehensively described the clinical entity of VEO, establishing the triad of medial tension, lateral compression, and posterior shear. Their early work defined the necessity of evaluating the entire joint rather than treating the posteromedial osteophyte in isolation.
Subsequent biomechanical studies by Ahmad et al. fundamentally altered the surgical approach to VEO. Using cadaveric models, they demonstrated that the olecranon osteophyte provides significant resistance to valgus torque in the UCL-deficient elbow. Their data proved that resecting the osteophyte without addressing UCL laxity increases strain on the remaining medial structures, leading to the current strict guideline: Resect only the pathologic osteophyte, preserve the normal olecranon anatomy, and concurrent UCL reconstruction is mandatory if frank ligamentous incompetence is present.
Current consensus guidelines dictate that arthroscopic debridement for VEO is highly successful for pain relief and return to sport when indications are strictly followed. However, surgical outcomes are intimately tied to preoperative diagnostic accuracy regarding the status of the UCL and meticulous adherence to conservative osseous resection limits intraoperatively.
You Might Also Like