Arthroscopic Distal Clavicle Resection: An Intraoperative Masterclass for AC Joint Pathology
Key Takeaway
This masterclass provides an immersive, step-by-step guide to arthroscopic distal clavicle resection. Fellows will learn critical surgical anatomy, meticulous patient positioning, and granular intraoperative execution for both indirect and direct approaches. We'll cover instrument use, rationale, and crucial pearls to ensure successful outcomes for symptomatic acromioclavicular joint pathology, emphasizing complication avoidance and precise technique.
Comprehensive Introduction and Patho-Epidemiology
Arthroscopic distal clavicle resection has evolved into a cornerstone procedure for the management of recalcitrant acromioclavicular (AC) joint pathology. Historically managed via the open Mumford procedure, the advent of advanced arthroscopic techniques has allowed orthopedic surgeons to achieve equivalent, if not superior, clinical outcomes while minimizing morbidity to the critical deltotrapezial fascial envelope. This intraoperative masterclass delineates the nuanced execution of this procedure, emphasizing that success relies not merely on bone resection, but on the precise restoration of functional kinematics while preserving the vital static and dynamic stabilizers of the shoulder girdle.
A profound understanding of the underlying patho-epidemiology is the prerequisite for any surgical intervention. Symptomatic AC joint pathology predominantly manifests in three distinct clinical entities: primary osteoarthritis, post-traumatic arthritis, and distal clavicular osteolysis. Primary osteoarthritis is virtually ubiquitous in the aging population; autopsy and radiographic studies demonstrate that degenerative changes in the fibrocartilaginous intra-articular disc begin as early as the second decade of life, with frank articular degeneration commonly established by the fourth decade. However, radiographic evidence of degeneration correlates poorly with clinical symptoms, necessitating rigorous clinical correlation.
Post-traumatic arthritis frequently arises secondary to Type I or Type II AC joint sprains. Epidemiological data indicates that between 8% and 42% of patients sustaining these seemingly innocuous injuries will subsequently develop chronic, debilitating symptoms due to altered joint mechanics and subsequent articular wear. Distal clavicular osteolysis, conversely, is a stress-induced microtraumatic condition classically observed in weightlifters and overhead athletes. The repetitive high-compressive loads placed across the AC joint during exercises such as the bench press or overhead press induce subchondral microfractures. When the rate of repetitive microtrauma exceeds the osteoblastic reparative capacity, it culminates in hypervascularity, bone resorption, and profound localized pain. Recognizing these distinct etiologies is critical, as the inflammatory cascade and resultant anatomic alterations dictate both our preoperative planning and intraoperative approach.
Detailed Surgical Anatomy and Biomechanics
The acromioclavicular articulation is a diarthrodial joint formed by the medial articular facet of the acromion and the distal articular surface of the clavicle. Despite its diminutive size—averaging merely 9 by 19 millimeters—it functions as the critical strut suspending the upper extremity from the axial skeleton. The sagittal orientation of the joint line exhibits profound anatomic variability, ranging from a nearly vertical alignment to a medial angulation of up to 50 degrees. This inclination is a critical intraoperative landmark; failure to recognize and accommodate a highly angled joint line frequently results in an incomplete, asymmetric resection, leaving a residual posterior or superior bony impingement that guarantees persistent postoperative pain.
The stability of the AC joint relies on a sophisticated interplay of capsular ligaments, extracapsular ligaments, and fascial attachments. The capsular ligaments (superior, inferior, anterior, and posterior) are the primary restraints to anteroposterior translation. Among these, the superior AC ligament is the most robust, heavily reinforced by the aponeurotic fascial attachments of the overlying deltoid and trapezius muscles. Preservation of this superior capsular complex during arthroscopic resection is paramount to preventing iatrogenic anteroposterior instability.
The extracapsular coracoclavicular (CC) ligaments—comprising the conoid and trapezoid—serve as the primary restraints to superior displacement of the clavicle under large physiologic loads. The trapezoid ligament originates on the coracoid and inserts anterolaterally on the undersurface of the clavicle, approximately 1.1 to 1.3 centimeters medial to the distal articular surface. The conoid ligament inserts more posteromedially, approximately 2.5 centimeters from the distal end. This anatomic relationship dictates our surgical limits: resection of the distal clavicle must strictly not exceed 10 millimeters to avoid compromising the trapezoid ligament insertion, which would precipitate iatrogenic vertical instability of the clavicular strut.
Neurovascular considerations, while less immediate than in deeper shoulder procedures, remain critical. The suprascapular nerve traverses the suprascapular notch and spinoglenoid notch, remaining deep to the operative field, but can be compromised by excessive traction or aggressive fluid extravasation. Superficially, the cephalic vein courses through the deltopectoral groove; precise placement of the anterior working portals is essential to avoid inadvertent laceration. Furthermore, branches of the thoracoacromial artery supply the AC joint capsule and must be meticulously managed with radiofrequency ablation to maintain a hemostatic visual field during the resection.
Exhaustive Indications and Contraindications
The decision to proceed with an arthroscopic distal clavicle resection must be predicated on a rigorous diagnostic algorithm. The hallmark presentation is insidious onset pain localized meticulously to the anterior and superior aspect of the shoulder, exacerbated by cross-body adduction and extreme internal rotation. Physical examination must isolate the AC joint; direct palpation yielding highly localized tenderness is the most sensitive physical finding. The cross-arm adduction test and the Paxinos test (applying anterior pressure to the acromion while pushing the mid-clavicle superiorly) are highly provocative.
However, because impingement syndrome, superior labral (SLAP) tears, and rotator cuff pathology frequently coexist with or mimic AC joint pain, a diagnostic fluoroscopically or ultrasound-guided intra-articular injection of local anesthetic is the definitive gold standard. Complete, albeit temporary, eradication of the patient's specific symptoms following the injection confirms the AC joint as the primary pain generator and is highly prognostic of surgical success.
Below is a comprehensive matrix of indications and contraindications for arthroscopic distal clavicle resection:
| Category | Specific Criteria | Clinical Rationale / Impact |
|---|---|---|
| Primary Indications | Failure of conservative management (3-6 months) | Exhaustion of NSAIDs, physical therapy, and activity modification is required before surgical intervention. |
| Primary Indications | Symptomatic primary osteoarthritis | Confirmed by localized pain, positive provocative testing, and radiographic evidence correlating with symptoms. |
| Primary Indications | Post-traumatic arthritis (Type I/II injuries) | Chronic pain secondary to altered joint kinematics following low-grade sprains. |
| Primary Indications | Distal clavicular osteolysis | Repetitive stress pathology, particularly in weightlifters, unresponsive to rest. |
| Absolute Contraindications | Active localized or systemic infection | High risk of septic arthritis and systemic dissemination. |
| Absolute Contraindications | High-grade AC joint instability (Type III-VI) | Resection alone will exacerbate instability; requires formal CC ligament reconstruction. |
| Relative Contraindications | Massive, irreparable rotator cuff tears | Altered glenohumeral kinematics may lead to anterosuperior escape; altering the coracoacromial arch/AC joint may worsen pseudoparalysis. |
| Relative Contraindications | Severe cervical radiculopathy | Cervical spine pathology must be addressed or ruled out as the primary pain generator prior to shoulder surgery. |
Pre-Operative Planning, Templating, and Patient Positioning
Preoperative imaging is indispensable for surgical mapping. Standard anteroposterior, scapular Y, and axillary lateral radiographs are obtained to evaluate the overall glenohumeral architecture. However, the Zanca view is non-negotiable for AC joint evaluation. By tilting the x-ray beam 10 to 15 degrees cephalad, the Zanca view removes the superimposition of the scapular spine, providing an unobstructed, orthogonal projection of the AC articulation.
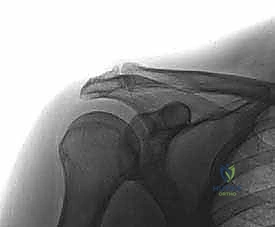
This view allows the surgeon to meticulously assess joint space narrowing, subchondral sclerosis, cystic changes, and the presence of inferior osteophytes that may be contributing to concomitant subacromial impingement. While magnetic resonance imaging (MRI) is highly sensitive, its specificity for symptomatic AC pathology is notoriously poor due to the high prevalence of asymptomatic degeneration. The critical MRI finding to identify is reactive bone marrow edema within the distal clavicle or medial acromion on T2-weighted fluid-sensitive sequences.
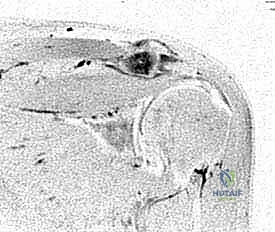
This edema represents active inflammation and microtrabecular stress, correlating strongly with the patient's acute pain presentation and confirming the necessity of resection.
Patient positioning is a critical determinant of intraoperative success. While the lateral decubitus position is utilized by some surgeons, the beach-chair position is overwhelmingly preferred for isolated or concomitant AC joint procedures. The beach-chair orientation places the AC joint in its physiologic, upright anatomical position, which intuitively aids the surgeon's spatial awareness during resection. Furthermore, it allows for gravity to assist in distracting the arm, opening the subacromial space, and provides unparalleled flexibility to convert to an open approach should unexpected pathology or complications arise.
The patient is positioned with the head meticulously secured in a specialized headrest, ensuring the cervical spine is neutral to prevent brachial plexus traction injuries. A small bump is placed under the medial border of the ipsilateral scapula to protract the shoulder girdle, allowing the glenohumeral joint to fall posteriorly and expanding the anterior working space. The operative arm is draped free and placed in an articulated, sterile pneumatic arm holder. This allows the assistant to dynamically manipulate the arm into varying degrees of flexion, internal rotation, and cross-body adduction throughout the procedure, which is essential for assessing the dynamic clearance of the resected AC joint.
Step-by-Step Surgical Approach and Fixation Technique
The execution of an arthroscopic distal clavicle resection demands a meticulous, systematic approach. The indirect (subacromial) approach is generally preferred over the direct superior approach, as it allows for simultaneous evaluation and treatment of the glenohumeral joint and subacromial space, which frequently harbor concomitant pathology.
Diagnostic Arthroscopy and Subacromial Preparation
The procedure commences with a standard diagnostic glenohumeral arthroscopy. A standard posterior viewing portal is established approximately 1.5 centimeters inferior and 1.5 centimeters medial to the posterolateral corner of the acromion. A comprehensive evaluation of the articular cartilage, labrum, biceps anchor, and the articular surface of the rotator cuff is performed. Once intra-articular pathology is addressed or ruled out, the arthroscope is redirected blindly, but carefully, beneath the posterior edge of the acromion into the subacromial space.
A standard lateral working portal is established under direct intra-articular visualization, typically 2 to 3 centimeters lateral to the lateral edge of the acromion, aligned with the posterior aspect of the AC joint. Using a 4.0mm or 5.5mm aggressive resector (shaver) and a radiofrequency ablation wand, a thorough subacromial bursectomy is performed.
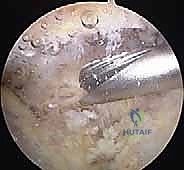
The surgeon must clear the subdeltoid bursa until the undersurface of the acromion, the coracoacromial (CA) ligament, and the inferior capsule of the AC joint are starkly visible. Hemostasis must be absolute; the hypervascular nature of the inflamed bursa can rapidly obscure the visual field. If an impinging acromial spur is present, an acromioplasty is performed prior to addressing the clavicle to establish a flat, clear working ceiling.
Joint Identification and Capsular Management
Identifying the exact joint line from the subacromial space can be deceptive due to inferior osteophytes and capsular hypertrophy. To definitively establish the joint orientation, an 18-gauge spinal needle is introduced percutaneously from the superior aspect of the shoulder, directly through the AC joint capsule.
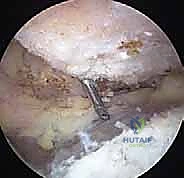
This needle serves as an unassailable topographic landmark, delineating the exact sagittal inclination of the joint. Once the joint line is confirmed, the radiofrequency wand is utilized to meticulously resect the inferior capsule of the AC joint and ablate any inferior osteophytes.
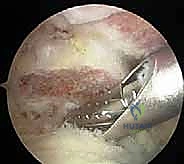
Crucially, the surgeon must exercise extreme caution to preserve the superior and posterior capsular ligaments. The radiofrequency wand should only strip the inferior and anterior-inferior soft tissues to expose the distal 10 millimeters of the clavicle. Aggressive superior capsular release is the primary genesis of postoperative anteroposterior instability.
The Bony Resection
With the distal clavicle exposed, a 5.5-millimeter barrel burr is introduced through the lateral portal. The resection begins on the acromial side of the joint to remove any medial acromial osteophytes and create working space, a process known as coplaning.
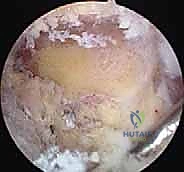
Attention is then turned to the distal clavicle. The burr is used to decorticate the articular surface, progressing from anterior to posterior.
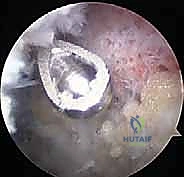
The surgeon must maintain a strict awareness of the burr's orientation relative to the previously identified joint inclination. A common technical error is creating a "V-shaped" resection, where the anterior clavicle is adequately resected, but a prominent posterior or superior ridge of bone is left intact due to the convex shape of the clavicle and the trajectory of the lateral portal.
To prevent this, an anterior portal is frequently established just lateral to the coracoid process. By alternating the viewing and working portals (viewing from the lateral portal while burring from the anterior portal, and vice versa), the surgeon achieves orthogonal perspectives of the resection bed.
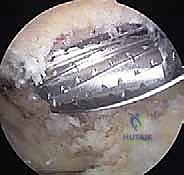
The goal is to resect a uniform 7 to 10 millimeters of distal clavicle. The 5.5-millimeter burr itself serves as an excellent intraoperative caliper. If the burr can be passed freely between the resected distal clavicle and the acromion in all planes—anterior to posterior, and superior to inferior—the resection is generally adequate.
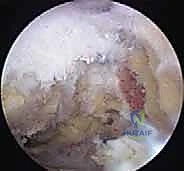
During the resection, the surgeon must dynamically assess the joint gap. The assistant should release the arm from traction and bring it into cross-body adduction.

While visualizing from the lateral or posterior portal, the surgeon observes the resected gap during this provocative maneuver. If the distal clavicle impinges against the acromion during adduction, further resection is mandatory.
The final resection bed should be flat, bleeding subchondral bone, completely devoid of any superior or posterior cortical ridges. The superior capsule should be seen draping intact over the newly created void, ensuring sustained anteroposterior stability.
Complications, Incidence Rates, and Salvage Management
While arthroscopic distal clavicle resection is highly successful, it is not immune to complications. The most frequent cause of failure is technical error during the bony resection. A profound understanding of these complications is essential for both prevention and salvage management.
| Complication | Estimated Incidence | Etiology and Clinical Presentation | Salvage / Management Strategy |
|---|---|---|---|
| Incomplete Resection | 5% - 10% | Failure to resect the posterior/superior cortex due to poor visualization or failure to recognize joint inclination. Presents as persistent localized pain. | Revision arthroscopic resection. Utilization of alternating anterior/posterior portals to ensure complete superior and posterior bone removal. |
| Over-resection / Instability | 2% - 5% | Resection exceeding 10-15mm, compromising the trapezoid ligament, or aggressive superior capsular takedown. Presents as dynamic AP or superior instability and pain. | Conservative management initially. If refractory, requires open or arthroscopic coracoclavicular (CC) ligament reconstruction using allograft or synthetic suspensory fixation. |
| Heterotopic Ossification | 3% - 8% | Bone formation in the resection gap, often due to inadequate irrigation of bone debris or aggressive soft tissue stripping. | Prophylactic NSAIDs (e.g., Indomethacin) in high-risk patients. If symptomatic, delayed arthroscopic excision after the bone scan indicates metabolic maturity (usually >12 months). |
| Infection (Septic Arthritis) | < 1% | Contamination of portals or intra-articular space. Presents with severe pain, erythema, and elevated inflammatory markers. | Emergent arthroscopic irrigation and debridement, targeted intravenous antibiotic therapy based on intraoperative cultures. |
| Neurovascular Injury | < 0.5% | Cephalic vein laceration during anterior portal placement, or suprascapular nerve injury from extreme fluid extravasation. | Vein injuries require open ligation or repair. Nerve injuries are typically neuropraxias that resolve with observation; rarely require decompression. |
The surgeon must maintain a high index of suspicion for incomplete resection in patients presenting with persistent pain at 3 to 6 months postoperatively. Zanca views and potentially a computed tomography (CT) scan with 3D reconstructions are invaluable for identifying residual posterior bony impingement, which is the most common culprit requiring revision surgery.
Phased Post-Operative Rehabilitation Protocols
The postoperative rehabilitation following an isolated arthroscopic distal clavicle resection is generally accelerated compared to procedures involving soft tissue repair, but it must be phased appropriately to respect the localized inflammatory response and prevent capsular adhesions.
Phase I: Immediate Postoperative Phase (Weeks 0-2)
The primary goals are pain control, reduction of inflammation, and protection of the healing soft tissue envelope. The patient is placed in a standard shoulder sling for comfort, but strict immobilization is discouraged to prevent adhesive capsulitis. Patients are instructed to remove the sling 3 to 4 times daily for passive and active-assisted range of motion (ROM) exercises, including pendulum exercises, forward elevation, and external rotation as tolerated. Cross-body adduction and heavy lifting are strictly prohibited to avoid compressing the inflamed resection site.
Phase II: Intermediate Range of Motion (Weeks 2-4)
The sling is formally discontinued. The focus shifts to achieving full, symmetric active and passive ROM. Scapular mobilization and stabilization exercises (e.g., scapular retractions, shrugs) are initiated to ensure proper scapulothoracic kinematics, which reduces compensatory stress on the AC joint. Isotonic strengthening of the rotator cuff and deltoid begins with light resistance bands, keeping the arm below 90 degrees of elevation.
Phase III: Advanced Strengthening (Weeks 4-8)
Once full, painless ROM is achieved, the patient progresses to heavier isotonic and functional strengthening. Exercises mimicking activities of daily living and occupational demands are integrated. Cross-body adduction stretching is gently introduced to ensure the resected gap is accommodating physiologic translation without impingement.
Phase IV: Return to Sport/Heavy Labor (Weeks 8-12)
For athletes, particularly weightlifters and overhead throwers, sport-specific plyometrics and heavy resistance training (e.g., bench press, overhead press) are gradually reintroduced. The patient must demonstrate symmetric strength, dynamic stability, and zero pain at the AC joint during maximum loading before full, unrestricted clearance is granted.
Summary of Landmark Literature and Clinical Guidelines
The evolution of distal clavicle resection is deeply rooted in landmark orthopedic literature. The foundational open technique, described by Mumford in 1941, established the principle that excision of the distal clavicle reliably eliminates AC joint pain. However, the open approach necessitated detachment of the deltotrapezial fascia, leading to prolonged recovery and potential weakness.
The transition to arthroscopic techniques was pioneered by surgeons such as Gartsman and Flatow in the 1990s. Gartsman's seminal studies demonstrated that the arthroscopic subacromial approach yielded equivalent pain relief to the open Mumford procedure but with significantly faster return to work and sport, primarily due to the preservation of the deltotrapezial envelope.
Biomechanical studies, notably those by Flatow and colleagues, were instrumental in defining the safe limits of resection. Their cadaveric models proved that resections exceeding 10 to 15 millimeters exponentially increased strain on the coracoclavicular ligaments, fundamentally altering the kinematics of the shoulder girdle and predisposing the patient to iatrogenic instability. This established the modern clinical guideline: the goal is a minimal, complete resection (typically 7-10mm) that eliminates bony contact during dynamic movement while meticulously preserving the superior capsule and the extracapsular ligamentous insertions.
Contemporary meta-analyses continue to support arthroscopic resection as the gold standard for refractory AC joint pathology, citing high patient satisfaction rates, low complication profiles, and the distinct advantage of simultaneously addressing the frequently co-occurring subacromial and glenohumeral pathologies. Mastery of this procedure, as detailed in this text, empowers the orthopedic surgeon to reliably restore function and eliminate pain in this challenging patient population.
