Arthroscopic AC Joint Reduction and Coracoclavicular Stabilization: A TightRope Masterclass
Key Takeaway
This masterclass guides fellows through arthroscopic AC joint reduction with TightRope fixation. We cover precise patient positioning, detailed anatomy, and meticulous intraoperative execution, from portal placement to hardware application. Learn critical pearls, potential pitfalls, and comprehensive postoperative care for optimal patient outcomes in acute, high-grade AC separations. Focus is on Rockwood Type III and VI injuries in active patients seeking functional restoration.
Comprehensive Introduction and Patho-Epidemiology
Acromioclavicular (AC) joint separations represent a significantly debilitating subset of shoulder trauma, predominantly affecting the young, active, and athletic populations. These injuries are typically the direct result of a high-energy blow to the lateral aspect of the shoulder with the arm in an adducted position. This specific mechanism is frequently encountered in contact sports such as rugby, hockey, and American football, as well as in high-velocity trauma scenarios like equestrian accidents and cycling crashes. The force of the impact drives the acromion inferiorly and medially, while the clavicle remains relatively stabilized by the robust sternocleidomastoid and trapezius muscle complexes. This opposing vector of forces leads to a sequential, catastrophic failure of the AC joint capsule, the acromioclavicular ligaments, and ultimately, the thick coracoclavicular (CC) ligaments, contingent upon the exact magnitude and vector of the applied energy.
The pathophysiological consequences of high-grade AC joint disruptions extend far beyond mere cosmetic deformity or localized pain. The loss of the crucial suspensory mechanism provided by the CC ligaments results in a functional dissociation of the superior shoulder suspensory complex (SSSC). This dissociation precipitates profoundly altered scapulothoracic kinematics, universally manifesting as scapular dyskinesia. The scapula loses its superior tether to the clavicle, leading to an abnormal inferior translation, anterior tilt, and internal rotation of the scapula relative to the thorax. Consequently, patients frequently experience profound weakness in overhead activities, chronic periscapular pain due to muscular fatigue and spasm, and a significantly elevated risk of secondary impingement syndromes and rotator cuff pathology over time as the subacromial space is dynamically compromised.
Historically, the management of these complex injuries has been a subject of intense orthopedic debate, characterized by an evolution from conservative neglect to extensive, morbid open reconstructions. Traditional non-anatomic procedures, such as the Weaver-Dunn operation, involved the transfer of the coracoacromial (CA) ligament to the distal clavicle following distal clavicle excision. While foundational in the history of shoulder surgery, these techniques often failed to restore the native biomechanics of the SSSC, leading to unacceptable rates of recurrent instability, construct elongation, and residual pain. The modern paradigm has shifted decisively toward anatomic reconstruction utilizing suspensory cortical button fixation, such as the TightRope system. This arthroscopically assisted approach allows for the precise, anatomic recreation of the conoid and trapezoid ligament vectors, offering superior biomechanical strength, minimizing soft tissue morbidity, and facilitating a more rapid and reliable return to pre-injury activity levels.
The Rockwood Classification System
The cornerstone of clinical decision-making and surgical planning in AC joint trauma remains the Rockwood classification system, which categorizes injuries based on the degree of ligamentous disruption and the resultant direction and magnitude of clavicular displacement. Type I injuries involve a mild sprain of the AC ligaments without macroscopic tearing, presenting with localized tenderness and a radiographically normal joint. Type II injuries denote a complete disruption of the AC ligaments with a concomitant sprain of the CC ligaments, resulting in slight widening of the AC joint but no significant superior translation of the distal clavicle. These low-grade injuries are universally managed non-operatively with a brief period of immobilization followed by progressive, scapula-focused rehabilitation.
High-grade injuries, encompassing Types III through VI, represent a complete structural failure of both the AC and CC ligament complexes. Type III injuries are characterized by 25% to 100% superior displacement of the distal clavicle relative to the acromion. The management of Type III injuries remains highly nuanced and controversial; while many patients tolerate the deformity well with conservative care, surgical intervention is increasingly favored in elite overhead athletes, heavy manual laborers, and those who fail an exhaustive initial trial of non-operative management. Type IV injuries involve posterior displacement of the distal clavicle into or through the trapezius muscle fascia. This posterior displacement is often palpable clinically and is exquisitely painful, as the clavicle dynamically impinges upon the muscular architecture of the posterior shoulder girdle.
Type V injuries represent a severe, high-energy progression of Type III, with greater than 100% (often up to 300%) superior displacement of the clavicle, accompanied by extensive, violent stripping of the deltotrapezial fascia from the distal half of the clavicle. This profound soft tissue disruption renders the SSSC grossly unstable and necessitates meticulous surgical repair of both the bony and fascial anatomy. Type VI injuries are exceedingly rare and involve inferior displacement of the distal clavicle into a subacromial or subcoracoid position, typically resulting from severe hyperabduction trauma combined with axial loading. Types IV, V, and VI are considered absolute indications for surgical reduction and stabilization due to the severe biomechanical derangement, intractable pain, and near certainty of long-term functional impairment if left unreduced.
Detailed Surgical Anatomy and Biomechanics
A profound, three-dimensional understanding of the surgical anatomy is the absolute prerequisite for executing an arthroscopic AC joint stabilization safely and effectively. The acromioclavicular joint itself is a diarthrodial articulation formed by the medial facet of the acromion and the distal end of the clavicle. The joint surfaces are inherently incongruent and are interposed by a fibrocartilaginous intra-articular disc, which undergoes rapid, physiological degeneration beginning as early as the second decade of life. The joint capsule is reinforced by the superior, inferior, anterior, and posterior AC ligaments. Biomechanical studies have unequivocally demonstrated that the superior AC ligament is the thickest and most robust, serving as the primary restraint to anterior-posterior horizontal translation of the distal clavicle. Consequently, meticulous repair or formal plication of the superior capsule and fascial sleeve during the open portion of the procedure is critical for restoring horizontal stability and preventing late-onset dynamic instability.
The coracoclavicular (CC) ligaments—the conoid and the trapezoid—are the primary static stabilizers of the SSSC, providing critical resistance against superior and anterior-posterior displacement of the clavicle relative to the scapula. The conoid ligament is the more medial and posterior of the two, originating from the posteromedial aspect of the coracoid process base and inserting onto the conoid tubercle of the clavicle, located approximately 45 millimeters medial to the distal clavicular articular surface. It is functionally a thick, triangular band that acts as the primary restraint to superior translation of the clavicle. The trapezoid ligament originates from the anterolateral aspect of the coracoid base and inserts onto the trapezoid line, extending laterally and anteriorly from the conoid tubercle, approximately 30 millimeters from the distal end of the clavicle. The trapezoid is broader and flatter, serving primarily to resist axial compression and posterior translation of the clavicle toward the acromion.
The dynamic stabilizers of the AC joint comprise the muscular and fascial attachments of the anterior deltoid and the trapezius muscles. The trapezius inserts onto the superior and posterior aspects of the distal clavicle and acromion, while the deltoid originates from the anterior and lateral borders. The confluence of their dense fascial investments over the superior aspect of the AC joint forms the deltotrapezial fascia. In high-grade separations, particularly Rockwood Type V, this fascial sleeve is violently stripped from the clavicle, exacerbating the superior migration of the bone. Failure to recognize and meticulously repair this fascial disruption during surgery will inevitably compromise the dynamic stability of the construct, placing excessive, unmitigated stress on the implanted suspensory hardware and significantly increasing the risk of mechanical failure or button pull-through.
Critical Neurovascular Proximity
The surgical approach to the coracoid process is fraught with potential neurovascular hazards, demanding exact spatial awareness from the operating surgeon. The suprascapular nerve, originating from the upper trunk of the brachial plexus, traverses the suprascapular notch, which is located immediately medial to the base of the coracoid process. The nerve is tethered beneath the transverse scapular ligament. Errant medial placement of the drill guide or over-penetration of the drill bit during coracoid tunnel preparation poses a catastrophic risk of direct injury to the suprascapular nerve. Such an iatrogenic injury leads to irreversible denervation of the supraspinatus and infraspinatus musculature, resulting in devastating functional loss of shoulder abduction and external rotation.
Furthermore, the major neurovascular bundle of the upper extremity—comprising the cords of the brachial plexus and the axillary artery and vein—lies in dangerously close proximity to the medial and inferior aspects of the coracoid process. These critical structures are situated deep to the pectoralis minor tendon, which inserts onto the medial border of the coracoid. During the arthroscopic skeletonization of the coracoid base, the surgeon must maintain a strict lateral and inferior working zone. Any instrument plunging medially or blindly sweeping inferior to the coracoid risks devastating vascular injury or plexus avulsion. The safe zone for drilling is strictly localized to the central, posterior aspect of the coracoid base, maintaining a trajectory that is precisely perpendicular to the superior surface of the coracoid to ensure maximum bone bridge integrity while avoiding medial structures.
Exhaustive Indications and Contraindications
The decision to proceed with operative intervention for an AC joint separation requires a highly nuanced synthesis of the injury grade, chronicity, patient demographics, occupational demands, and athletic aspirations. While the surgical indications for low-grade (Types I-II) and extreme high-grade injuries (Types IV-VI) are well-established and universally agreed upon, the management of intermediate Type III injuries remains highly individualized. The advent of arthroscopic, minimally invasive techniques utilizing suspensory fixation has subtly lowered the threshold for surgical intervention in borderline cases, given the significantly reduced morbidity, superior cosmesis, and improved biomechanical restoration compared to traditional open reconstructions.
Acute injuries—strictly defined in the literature as those presenting within 3 to 4 weeks of the initial trauma—are the ideal candidates for isolated suspensory fixation, such as the TightRope system. In the acute setting, the native, ruptured CC ligaments retain their intrinsic healing potential. The primary surgical objective is to anatomically reduce the joint and hold it rigidly in place, acting as an internal splint that allows the native ligaments to heal in an isometric, anatomic position. Conversely, chronic injuries (presenting after 4 to 6 weeks) exhibit established ligamentous scarring, retraction, and a complete loss of biological healing capacity. In these chronic scenarios, isolated suspensory fixation is biomechanically insufficient and carries an unacceptably high failure rate. Chronic separations mandate a biological augmentation, typically involving a free tendon allograft or autograft (such as a semitendinosus tendon) woven through the clavicle and around the coracoid to biologically reconstruct the CC ligaments, supplemented by a suspensory button for immediate mechanical stability during the graft incorporation phase.
Patient-specific factors are paramount in the complex decision-making matrix. Elite overhead athletes (e.g., baseball pitchers, tennis players, volleyball attackers) and heavy manual laborers who perform repetitive lifting above shoulder level require absolute, flawless restoration of SSSC kinematics. In these high-demand populations, even a technically "mild" Rockwood Type III injury can result in career-ending scapular dyskinesia, dynamic impingement, and fatigue-induced pain. Therefore, early surgical intervention is strongly recommended. Conversely, an elderly, low-demand patient with a Type III or even a Type IV injury may achieve entirely acceptable functional outcomes with non-operative management, avoiding the inherent risks of general anesthesia, hardware complications, and surgical site infections.
| Variable | Indications for Surgery | Contraindications for Surgery |
|---|---|---|
| Injury Grade | Rockwood Types IV, V, VI; Select symptomatic Type III | Rockwood Types I, II; Asymptomatic or low-demand Type III |
| Chronicity | Acute (< 4 weeks) for isolated TightRope suspensory fixation | Chronic (> 6 weeks) without planned biological graft augmentation |
| Patient Profile | Elite athletes, heavy manual laborers, overhead workers | Sedentary lifestyle, low functional demands, non-compliant patients |
| Local Tissue | Intact skin envelope, absence of local infection | Active local/systemic infection, severe skin abrasions/burns over the AC joint |
| Bone Quality | Normal bone mineral density and cortical thickness | Severe osteoporosis or lytic lesions (high risk of button pull-through or fracture) |
| Systemic Factors | Medically optimized for elective general anesthesia | Severe cardiopulmonary comorbidities, uncontrolled diabetes, active smoking |
Pre-Operative Planning, Templating, and Patient Positioning
Meticulous preoperative planning is the absolute foundation of a flawless intraoperative execution and optimal patient outcomes. The clinical evaluation must be exhaustive, not only confirming the AC joint diagnosis but also rigorously ruling out concomitant shoulder pathology, which occurs in up to 15-20% of high-energy AC separations. Provocative testing is essential. The AC joint compression (shear) test, performed by stabilizing the scapula and compressing the clavicle posteriorly, will elicit sharp, localized pain. The cross-arm adduction test reliably compresses the AC joint, though the clinician must carefully differentiate anterior AC pain from posterior capsular tightness or subacromial impingement. Crucially, a comprehensive neurovascular examination of the affected extremity is mandatory, specifically assessing the function of the brachial plexus, as high-energy Type V and VI injuries can cause traction neuropraxias that must be documented prior to any surgical intervention.
Radiographic evaluation must extend far beyond standard trauma shoulder series. The standard anteroposterior (AP) view of the shoulder is often overpenetrated, rendering the AC joint radiolucent and difficult to assess accurately. The Zanca view is the undisputed gold standard for evaluating AC joint pathology. By tilting the X-ray beam 10 to 15 degrees cephalad, the AC joint is projected clear of the dense bone of the scapular spine, allowing for precise measurement of the coracoclavicular distance and identification of subtle distal clavicle fractures or intra-articular loose bodies that could complicate reduction.
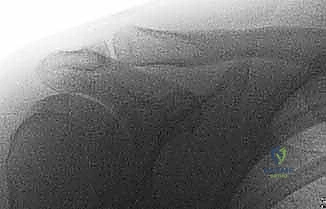
Bilateral Zanca views are highly recommended to compare the injured CC distance to the patient's native, contralateral anatomy, as baseline CC distances vary significantly among individuals. An axillary view is also mandatory to evaluate for posterior displacement of the clavicle (diagnostic of a Type IV injury) and to definitively rule out a subtle glenohumeral dislocation or coracoid base fracture. Advanced imaging, such as Magnetic Resonance Imaging (MRI), is not strictly necessary for acute, isolated AC separations but becomes invaluable if concomitant rotator cuff tears, superior labral anterior-posterior (SLAP) lesions, or subtle coracoid fractures are suspected based on the mechanism of injury or clinical examination.
Operating Room Setup and Patient Positioning
The patient is positioned in the beach-chair configuration, which provides unparalleled, three-dimensional access to the superior and anterior aspects of the shoulder girdle, facilitating both the arthroscopic and open phases of the procedure seamlessly. The torso is elevated to 60 to 70 degrees, with the hips and knees slightly flexed to prevent sciatic nerve traction and venous pooling. The head is meticulously secured in a neutral cervical spine position using a dedicated head positioner, ensuring that the endotracheal tube is secure and the contralateral eye and ear are protected from pressure necrosis.
The operative arm is prepped and draped free, allowing for dynamic manipulation during the reduction phase of the procedure. A mechanical arm holder can be utilized to maintain the arm in 30 to 45 degrees of forward flexion and slight internal rotation, which relaxes the anterior deltoid and facilitates arthroscopic access to the subcoracoid space. The C-arm fluoroscopy unit must be positioned on the contralateral side of the table, entering perpendicular to the patient to allow for unobstructed intraoperative Zanca views. Prior to making any incisions, the surgeon must confirm that the C-arm can easily swing into position to visualize the clavicle and coracoid without compromising the sterile field.
Step-by-Step Surgical Approach and Fixation Technique
The surgical procedure begins with a comprehensive diagnostic glenohumeral arthroscopy. Utilizing a standard posterior viewing portal, the surgeon systematically evaluates the joint for concomitant pathology. High-energy AC joint separations are frequently associated with SLAP tears, partial articular-sided rotator cuff tears, and intra-articular loose bodies. Any identified intra-articular pathology should be addressed appropriately before proceeding to the extra-articular AC joint stabilization. Once the glenohumeral joint is cleared, the arthroscope is directed anteriorly, and an anterosuperior portal is established via an outside-in technique using a spinal needle. This portal is positioned just lateral to the coracoid process, passing through the rotator interval, to serve as the primary viewing portal for the subcoracoid space.
The critical phase of coracoid preparation begins by establishing an anterolateral working portal. Using a radiofrequency ablation wand and an arthroscopic shaver, the surgeon meticulously clears the soft tissue overlying the base of the coracoid process. The coracoacromial (CA) ligament is identified, and its medial border is traced to the coracoid base. The surgeon must skeletonize the superior, medial, and lateral aspects of the coracoid base, creating a clear "safe zone" for subsequent drilling.

Extreme caution is exercised during medial dissection to avoid the neurovascular bundle and the suprascapular nerve. The inferior surface of the coracoid base is then cleared to allow for flat, flush seating of the inferior suspensory button. This step is paramount; soft tissue interposition beneath the inferior button will lead to postoperative creep, loss of reduction, and potential clinical failure.
Following coracoid preparation, attention is turned to the superior clavicle. A 3 to 4-centimeter sagittal or transverse incision is made over the distal clavicle, centered approximately 35 millimeters medial to the AC joint line. Dissection is carried down to the deltotrapezial fascia. A meticulous, full-thickness fascial flap is raised, preserving the tissue for robust closure. The superior surface of the clavicle is exposed. Using an arthroscopically assisted specific drill guide, a guide pin is placed through the clavicle and directed toward the central, posterior base of the coracoid. The trajectory must precisely replicate the native vector of the conoid ligament.
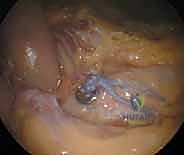
Arthroscopic visualization confirms the guide pin exiting precisely in the center of the inferior coracoid base. Once the optimal trajectory is confirmed, a cannulated drill (typically 4.0mm or 4.5mm, depending on the specific implant system) is passed over the pin, creating the transosseous tunnels through the clavicle and coracoid.
The suspensory implant, such as the TightRope system, is then passed through the tunnels. A passing suture is introduced from superior to inferior through the drilled holes and retrieved arthroscopically out the anterolateral portal. The inferior button is shuttled through the clavicle and the coracoid. Arthroscopic visualization is absolutely critical at this juncture to confirm that the inferior button has deployed horizontally and is seated flush against the cortical bone of the inferior coracoid base, free of any soft tissue interposition.
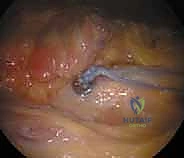
With the inferior button secured, the surgeon manually reduces the AC joint by applying a superiorly directed force to the arm while simultaneously applying an inferiorly directed force to the distal clavicle. Once anatomic reduction is confirmed clinically and fluoroscopically, the superior button is seated against the clavicular cortex, and the construct is tensioned. The knotless tensioning mechanism or alternating half-hitches are secured. Finally, the critical deltotrapezial fascial imbrication is performed using heavy non-absorbable sutures, providing essential dynamic stability to protect the hardware during the early healing phase.
Complications, Incidence Rates, and Salvage Management
Despite advances in arthroscopic techniques and implant biomechanics, surgical stabilization of the AC joint carries a distinct profile of potential complications. The most common complication is a partial loss of radiographic reduction, occurring in 15% to 30% of cases. This phenomenon, often termed "creep," typically occurs within the first 6 to 12 weeks postoperatively. It is usually attributed to suture elongation, minor subsidence of the buttons into the cortical bone, or soft tissue interposition that was not adequately cleared during surgery. Fortunately, mild to moderate loss of reduction (e.g., a few millimeters of superior translation) is rarely clinically significant and does not typically correlate with inferior functional outcomes or pain, provided the dynamic SSSC remains stable.
More catastrophic complications include fractures of the coracoid process or the distal clavicle. Coracoid fractures are particularly devastating and occur in approximately 1% to 3% of cases. They are almost exclusively iatrogenic, resulting from eccentric drilling of the coracoid tunnel, multiple drill passes that weaken the bone bridge, or drilling too anteriorly on the coracoid process where the bone is substantially thinner. Clavicle fractures can similarly occur if the superior button is overtensioned or if the drill hole is placed too close to the anterior or posterior cortex. Management of a coracoid fracture typically requires a complex open revision with internal fixation of the coracoid and a biological reconstruction of the CC ligaments.
Hardware irritation is another frequent postoperative complaint, particularly in thin individuals. The superior button or the prominent suture knots can irritate the overlying skin and subcutaneous tissue, causing localized pain and precluding the wearing of heavy backpacks or shoulder straps. This can often be mitigated by countersinking the superior button into the clavicle or utilizing low-profile, knotless implant systems. If hardware irritation becomes intractable after complete biological healing (typically after 6 to 9 months), the hardware may be electively removed.
| Complication | Estimated Incidence | Etiology / Risk Factors | Salvage / Management Strategy |
|---|---|---|---|
| Loss of Reduction (Creep) | 15% - 30% | Suture elongation, button subsidence, soft tissue interposition | Usually non-operative; revision only if symptomatic and grossly unstable |
| Coracoid Fracture | 1% - 3% | Eccentric drilling, multiple drill passes, osteoporosis | Open reduction internal fixation (ORIF) of coracoid + biological CC reconstruction |
| Clavicle Fracture | 1% - 2% | Eccentric clavicle tunnel, overtensioning, trauma | ORIF with plate and screws, hardware removal |
| Hardware Irritation | 10% - 20% | Prominent knots, thin soft tissue envelope, superior button prominence | Local padding, modification of activities; elective hardware removal after 6-9 months |
| Infection (Superficial/Deep) | 1% - 4% | Poor soft tissue handling, prolonged operative time | I&D, targeted antibiotics; hardware removal if deep and persistent |
| Adhesive Capsulitis | 5% - 10% | Prolonged immobilization, poor rehabilitation compliance | Aggressive physical therapy, intra-articular corticosteroid injection, rare manipulation |
Phased Post-Operative Rehabilitation Protocols
The postoperative rehabilitation following arthroscopic AC joint stabilization is a delicate balancing act between protecting the healing ligaments and preventing glenohumeral stiffness. The protocol is strictly phased, respecting the biological timeline of ligamentous healing. Phase I (Weeks 0 to 4) focuses entirely on protection. The patient is placed in a dedicated shoulder sling with an abduction pillow to remove the gravitational weight of the arm, which places direct stress on the CC repair. Absolute restrictions are placed on active shoulder elevation, cross-body adduction, and heavy lifting. Passive range of motion (PROM) is initiated early to prevent adhesive capsulitis, but forward flexion is strictly limited to 90 degrees, and external rotation is limited to 30 degrees to prevent excessive strain on the SSSC.
Phase II (Weeks 5 to 8) marks the transition to active-assisted range of motion (AAROM) and active range of motion (AROM). The sling is incrementally discontinued. Patients begin supine AAROM exercises, utilizing a wand or pulleys, gradually progressing to upright AROM as tolerated. Scapular mobilization and periscapular strengthening become the primary focus during this phase. Exercises such as scapular retractions, shrugs, and prone rows are introduced to restore normal scapulothoracic kinematics and address the invariably present scapular dyskinesia. The surgeon must monitor the patient closely during this phase for any clinical signs of loss of reduction or hardware failure.
Phase III (Weeks 9 to 16) initiates formal strengthening. Isotonic and isokinetic exercises for the rotator cuff and deltoid are incorporated. Closed kinetic chain exercises are highly beneficial for promoting dynamic joint stability. Patients are permitted to progress their lifting weight gradually, but heavy overhead lifting and bench pressing are still restricted. Phase IV (Months 4 to 6) is the return-to-play phase. Elite athletes undergo sport-specific functional testing. Clearance for full contact sports (e.g., rugby, football) is typically granted between 5 and 6 months postoperatively, contingent upon the achievement of full, painless ROM, symmetric strength, and radiographic evidence of maintained reduction.
Summary of Landmark Literature and Clinical Guidelines
The evolution of AC joint management is heavily documented in modern orthopedic literature, with several landmark studies shaping current clinical guidelines. Biomechanical studies by Mazzocca et al. have been instrumental in defining the precise anatomical footprints of the conoid and trapezoid ligaments. Their research unequivocally demonstrated that anatomic, dual-bundle reconstructions (or precise single-tunnel suspensory fixations mimicking the conoid vector) exhibit superior load-to-failure strength and reduced anterior-posterior translation compared to non-anatomic procedures like the modified Weaver-Dunn. This biomechanical foundational data drove the industry-wide shift toward suspensory cortical button technologies.
Clinical consensus guidelines, such as those published by the International Society of Arthroscopy, Knee Surgery and Orthopaedic Sports Medicine (ISAKOS), have provided much-needed clarity on the indications for surgery. The ISAKOS consensus strongly supports non-operative management for Rockwood Types I and II, and early operative intervention for Types IV, V, and VI. The management of Type III injuries remains a "gray area," but recent multicenter prospective cohorts suggest that while conservative management yields acceptable results in the general population, surgical stabilization in high-demand laborers and elite overhead athletes significantly reduces the incidence of chronic scapular dyskinesia and secondary rotator cuff pathology.
Furthermore, comparative outcome studies evaluating open versus arthroscopic techniques have consistently shown that arthroscopic-assisted suspensory fixation results in lower visual analog scale (VAS) pain scores in the early postoperative period, superior cosmetic outcomes, and equivalent long-term functional scores (such as the Constant-Murley and ASES scores) compared to open reconstructions. However, the literature also cautions that the arthroscopic approach has a steep learning curve, particularly regarding coracoid skeletonization and precise tunnel drilling, emphasizing the need for rigorous surgical training and meticulous preoperative templating to minimize the risk of catastrophic complications like coracoid fracture or neurovascular injury.
