Irreparable Rotator Cuff Tears: What Are Your Treatment Options?
Key Takeaway
We review everything you need to understand about Irreparable Rotator Cuff Tears: What Are Your Treatment Options?. Massive, immobile rotator cuff tears, often presenting as an **irreparable rotator cuff** injury due to retraction and immobility, can be surgically repaired using specialized techniques. An anterior or posterior interval slide decreases tension and improves mobilization, allowing the supraspinatus to be reattached to the greater tuberosity. This is often followed by marginal convergence to facilitate final repair.
Comprehensive Introduction and Patho-Epidemiology
The management of massive and potentially irreparable rotator cuff tears remains one of the most formidable challenges in contemporary orthopedic shoulder surgery. A massive rotator cuff tear is classically defined by Cofield as a tear with an anteroposterior dimension greater than 5 centimeters, or by Gerber as a tear involving two or more complete tendon footprints. However, the designation of a tear as "irreparable" is a distinct clinical and intraoperative determination. An irreparable tear is one in which the torn tendon edges cannot be mobilized and securely fixed to their anatomical footprint on the greater tuberosity, even after maximal surgical releases and mobilization techniques. The distinction between massive and irreparable is critical; many massive tears can be rendered reparable through advanced arthroscopic techniques, while some smaller, chronically retracted tears with severe muscle degeneration may prove truly irreparable.
The classic clinical presentation of a patient with a massive, potentially irreparable rotator cuff tear is exemplified by a patient in their late sixth or seventh decade of life—such as a 70-year-old right-hand-dominant woman—presenting with profound shoulder pain, severe nocturnal pain, and progressive weakness. These patients often exhibit pseudoparalysis, defined as the inability to actively elevate the arm above 90 degrees (often limited to 30 or 40 degrees of active flexion and abduction) in the setting of full passive range of motion, absent neurological deficit, and without end-stage glenohumeral osteoarthritis. Clinical examination frequently reveals profound atrophy of the supraspinatus and infraspinatus fossae, positive impingement signs (Neer, Hawkins), a positive drop arm test, and a positive external rotation lag sign indicating severe posterosuperior cuff dysfunction.
The pathophysiology of irreparable rotator cuff tears is driven by chronic biomechanical failure leading to secondary biological degradation. Once a tendon detaches from its insertion, the muscle-tendon unit undergoes progressive retraction, muscle atrophy, and fatty infiltration. The Goutallier classification (evaluated on sagittal MRI or CT) and the Thomazeau classification (for muscle atrophy) are critical prognosticators. Tears associated with Goutallier grade 3 or 4 fatty infiltration (where fat equals or exceeds muscle tissue) and severe retraction to the glenoid rim (Patte Stage 3) are historically considered irreparable. However, in cases where an MRI reveals a massive tear retracted to the glenoid but with only minimal atrophy and minimal fatty infiltration, the surgeon must approach the case with the intent to repair, utilizing advanced mobilization techniques before declaring the tear irreparable.
Understanding the epidemiology and natural history of these lesions is paramount for surgical decision-making. The prevalence of rotator cuff tears increases linearly with age, with massive tears comprising up to 20% of all rotator cuff tears and up to 80% of recurrent tears. If left untreated, massive tears predictably progress. The disruption of the glenohumeral force couples leads to superior migration of the humeral head, articulation of the humerus with the acromion, and eventual development of rotator cuff tear arthropathy (Hamada classification). Therefore, the orthopedic surgeon must carefully weigh the patient's physiological age, functional demands, symptom severity, and anatomical patho-morphology when navigating the complex algorithm of treatment options.
Detailed Surgical Anatomy and Biomechanics
A profound comprehension of shoulder biomechanics and the intricate anatomy of the rotator cuff is mandatory for addressing massive tears. The rotator cuff functions not merely as a collection of individual muscles, but as a highly coordinated, dynamic stabilizing envelope. According to Burkhart’s principles, the rotator cuff operates through crucial "force couples" in both the coronal and transverse planes. In the coronal plane, the inferiorly directed vector of the inferior rotator cuff (infraspinatus, teres minor, and subscapularis) counterbalances the superiorly directed vector of the deltoid. In the transverse plane, the anterior subscapularis balances the posterior infraspinatus and teres minor. Disruption of these force couples, particularly the transverse couple in massive posterosuperior tears, results in the uncoupling of glenohumeral kinematics, leading to superior humeral head escape and the clinical manifestation of pseudoparalysis.
The anatomical concept of the "rotator cable" and "rotator crescent" is equally essential when evaluating reparability. The rotator cable is a thick bundle of fibers running perpendicular to the supraspinatus and infraspinatus tendons, spanning from the coracohumeral ligament anteriorly to the inferior margin of the infraspinatus posteriorly. It acts much like the suspension cable of a bridge, stress-shielding the thinner, avascular rotator crescent that inserts onto the greater tuberosity. In massive tears, the integrity of the rotator cable attachments is often lost. Restoring the biomechanical function of the shoulder does not always require complete anatomical footprint coverage; rather, restoring the continuity of the rotator cable and re-establishing the transverse force couple can yield excellent clinical outcomes, a concept that forms the basis of partial repair and marginal convergence techniques.
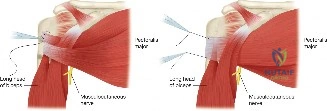
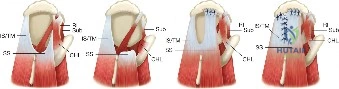
The surgical anatomy of the rotator interval and the posterior interval is of paramount importance when attempting to mobilize a retracted tear. The rotator interval is a triangular anatomic space bordered by the anterior margin of the supraspinatus, the superior margin of the subscapularis, and the base of the coracoid process. It contains the coracohumeral ligament (CHL) and the superior glenohumeral ligament (SGHL). The CHL is a robust structure that originates on the base of the coracoid and envelops the supraspinatus and subscapularis. In chronic retracted tears, the CHL becomes contracted and acts as a primary tether preventing lateral excursion of the supraspinatus. Releasing this structure is the cornerstone of the anterior interval slide.
Posteriorly, the interval between the supraspinatus and infraspinatus can also become scarred and tethered. The posterior interval slide involves separating these two distinct muscle bellies to allow independent lateral excursion. However, this maneuver carries a significant neurovascular risk. The suprascapular nerve courses through the suprascapular notch, supplies the supraspinatus, and then wraps around the spinoglenoid notch to innervate the infraspinatus. The nerve lies approximately 1.5 to 2.0 centimeters medial to the glenoid rim. Aggressive dissection or deep capsular releases in the posterior interval can inadvertently injure the suprascapular nerve, leading to catastrophic denervation of the remaining posterior cuff. Thus, meticulous, superficial dissection is required when executing a posterior interval slide.
Exhaustive Indications and Contraindications
The decision-making algorithm for massive, potentially irreparable rotator cuff tears is highly nuanced. The surgeon must synthesize patient-specific variables (age, activity level, medical comorbidities) with patho-anatomical variables (tear size, retraction, fatty infiltration, presence of arthritis, and dynamic shoulder function). Treatment options range from arthroscopic debridement to complex tendon transfers and arthroplasty. Proper patient selection is the single most critical determinant of surgical success.
Treatment Options and Patient Selection Algorithm
- Arthroscopic Debridement and Biceps Tenotomy/Tenodesis: Indicated for elderly, low-demand patients with profound pain but preserved active elevation (no pseudoparalysis). It addresses pain generators (the long head of the biceps and bursitis) without the morbidity of a prolonged repair rehabilitation. Contraindicated in young, high-demand patients or those with pseudoparalysis.
- Partial Repair: Indicated when the tear cannot be fully mobilized to the footprint, but the anterior and posterior leaves can be repaired to restore the transverse force couple. Ideal for patients with intact subscapularis and teres minor.
- Superior Capsule Reconstruction (SCR): Indicated for younger or highly active patients (<65 years) with an irreparable supraspinatus/infraspinatus tear, intact or repairable subscapularis, functional deltoid, and minimal to no glenohumeral arthritis (Hamada 1 or 2). Contraindicated in the setting of severe arthritis, deltoid dysfunction, or advanced pseudoparalysis that does not correct with local anesthetic injection.
- Tendon Transfers (Latissimus Dorsi or Lower Trapezius): Indicated for young, high-demand patients with irreparable posterosuperior tears, severe external rotation weakness (positive hornblower's sign), and no arthritis. The lower trapezius transfer is increasingly preferred due to its in-phase biomechanical vector compared to the out-of-phase latissimus dorsi.
- Reverse Total Shoulder Arthroplasty (RTSA): The gold standard for elderly patients (>65-70 years) with irreparable tears and pseudoparalysis, regardless of the presence of glenohumeral arthritis (cuff tear arthropathy). RTSA medializes the center of rotation and distalizes the humerus, tensioning the deltoid to restore active elevation.

| Treatment Option | Primary Indications | Absolute Contraindications | Relative Contraindications |
|---|---|---|---|
| Debridement / Biceps Tenotomy | Elderly, low demand, primary symptom is pain, preserved ROM. | Young, high demand, pseudoparalysis. | Moderate to severe weakness. |
| Partial Repair / Marginal Convergence | Massive tear, reparable anterior/posterior margins, intact force couples. | Complete loss of teres minor and subscapularis. | Severe Goutallier Grade 4 fatty infiltration. |
| Superior Capsule Reconstruction (SCR) | Age < 65, intact subscapularis, intact deltoid, Hamada 1-2. | Deltoid deficiency, severe glenohumeral arthritis (Hamada 4-5). | Irreparable subscapularis, fixed pseudoparalysis. |
| Tendon Transfer (Latissimus / Lower Trap) | Young, active, isolated loss of external rotation, no arthritis. | Glenohumeral arthritis, deltoid deficiency, unable to comply with rehab. | Elderly patients, generalized myopathy. |
| Reverse Total Shoulder Arthroplasty (RTSA) | Age > 65, pseudoparalysis, cuff tear arthropathy (Hamada 3-5). | Active infection, non-functioning deltoid (axillary nerve palsy). | Age < 55 (due to implant longevity concerns), intact functioning cuff. |
Pre-Operative Planning, Templating, and Patient Positioning
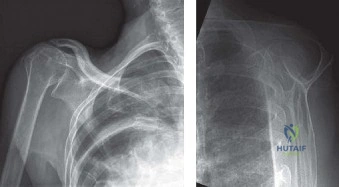
Thorough pre-operative planning begins with a comprehensive radiographic evaluation. A standard shoulder series must include a true anteroposterior (Grashey) view, a scapular Y view, and an axillary lateral view. The Grashey view is critical for assessing the acromiohumeral interval (AHI). A normal AHI is 7-14 mm; an AHI of less than 7 mm indicates superior humeral migration and suggests a massive, chronic tear. An AHI of less than 5 mm is highly predictive of an irreparable tear and early cuff tear arthropathy. The axillary view is evaluated for static subluxation and glenoid wear patterns.
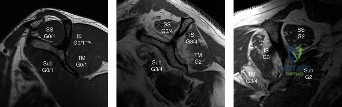
Magnetic Resonance Imaging (MRI) is the gold standard for soft tissue evaluation. Sagittal T1-weighted images are scrutinized to grade fatty infiltration of the supraspinatus, infraspinatus, and subscapularis muscle bellies using the Goutallier classification. Coronal T2-weighted images are used to assess the degree of medial tendon retraction (Patte classification). In cases where a patient presents with pseudoparalysis but has minimal fatty infiltration on MRI, the surgeon must plan for a primary repair utilizing advanced mobilization techniques, rather than immediately defaulting to arthroplasty or tendon transfer.
Patient positioning is a matter of surgeon preference, but both the beach chair and lateral decubitus positions offer distinct advantages. The beach chair position allows for anatomical orientation, ease of converting to an open procedure or arthroplasty if necessary, and excellent visualization of the anterior and superior compartments. It is particularly advantageous if an RTSA is the backup plan. The lateral decubitus position, utilizing longitudinal and lateral traction, opens the subacromial space significantly, providing superior visualization of the glenoid and facilitating complex suturing and graft passage required for techniques like SCR or lower trapezius transfer.
Regardless of the position, meticulous preparation and draping are required. The arm must be freely mobile to assess tension during repair. A standard posterior viewing portal is established, followed by an anterior portal through the rotator interval, and a lateral portal for subacromial work. A thorough diagnostic arthroscopy is the first and most critical step, as the true reparability of the tear can only be determined by grasping the tendon edges and assessing their excursion toward the greater tuberosity.
Step-by-Step Surgical Approach and Fixation Technique
When encountering a massive, immobile rotator cuff tear intraoperatively, the surgeon must employ a systematic, stepwise approach to mobilization. The vignette of a massive U-shaped or longitudinal tear retracted to the glenoid, yet possessing minimal fatty infiltration, is the classic indication for extensive interval slides and marginal convergence. The goal is to convert an immobile, seemingly irreparable tear into a reparable construct without placing undue tension on the healing tendon-to-bone interface.
Step 1: Comprehensive Releases
The initial step involves extensive intra-articular and bursal-sided releases. All subacromial adhesions and bursal tissue must be meticulously resected to free the superior surface of the cuff. Intra-articularly, a capsular release is performed just superior to the glenoid labrum. If the tendon remains immobile, the surgeon proceeds to specific interval slides.
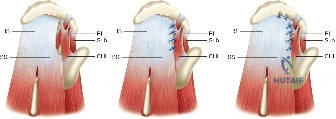
Step 2: The Anterior Interval Slide
The anterior interval slide is the most critical maneuver for mobilizing a retracted supraspinatus. The supraspinatus is often tethered anteriorly by a thickened, contracted coracohumeral ligament (CHL).
1. The rotator interval is identified between the anterior edge of the supraspinatus and the superior edge of the subscapularis.
2. Using an arthroscopic electrocautery or tissue liberator, the interval tissue is incised from lateral to medial, heading toward the base of the coracoid process.
3. The CHL is completely transected. This release separates the anterior supraspinatus from its tethering structures, frequently providing 1 to 2 centimeters of lateral excursion.
Step 3: The Posterior Interval Slide
If the tear remains U-shaped and under high tension, a posterior interval slide may be necessary.
1. The interval between the supraspinatus and infraspinatus is identified.
2. A controlled incision is made separating the two muscle-tendon units.
3. Crucial Technical Pearl: This incision must not extend further medial than the glenoid rim to avoid iatrogenic injury to the suprascapular nerve as it courses through the spinoglenoid notch.
4. This slide allows the supraspinatus and infraspinatus to be mobilized independently, significantly reducing tension on the posterior leaf.
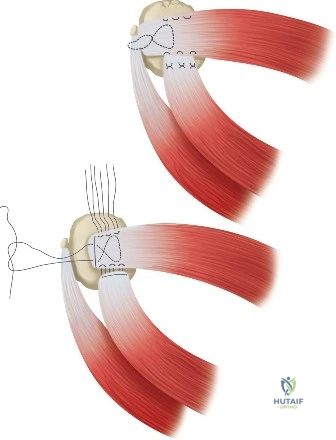
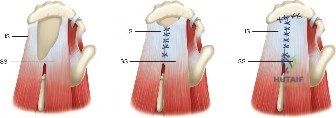
Step 4: Marginal Convergence
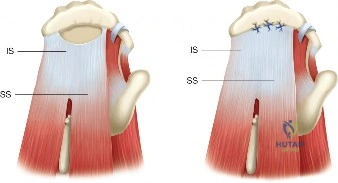
Once the tendons are mobilized, they often cannot reach the lateral footprint in their entirety. Marginal convergence is employed to close the longitudinal split of the U-shaped tear, effectively converting it into a smaller, crescent-shaped tear.
1. Side-to-side sutures (often utilizing a "shoelace" or Krackow-type configuration arthroscopically) are passed between the anterior and posterior leaves of the tear.
2. As these sutures are tied sequentially from medial to lateral, the free margin of the tendon is drawn laterally toward the greater tuberosity.
3. This technique relies on the principle of margin convergence, which exponentially decreases the strain at the lateral margin of the tear, allowing the newly formed crescent edge to be repaired to the bone using standard suture anchor techniques (single or double-row) without catastrophic tension.
Alternative Techniques for the Truly Irreparable Tear
If, after all releases, the tear cannot be approximated to the footprint, the surgeon must pivot.
* Superior Capsule Reconstruction (SCR): A thick dermal allograft or fascia lata autograft is secured medially to the superior glenoid and laterally to the greater tuberosity footprint. This graft acts as a static restraint, depressing the humeral head and restoring the fulcrum for the deltoid to act upon.
* Subacromial Balloon Spacer: A biodegradable balloon is deployed into the subacromial space and inflated with saline. It temporarily depresses the humeral head, allowing for rehabilitation of the deltoid and remaining cuff. It degrades over 6-12 months.
* Tendon Transfers: For profound external rotation weakness, the lower trapezius can be harvested, augmented with an Achilles tendon allograft, and routed under the deltoid to insert on the infraspinatus footprint.
Complications, Incidence Rates, and Salvage Management
The surgical management of massive and irreparable rotator cuff tears is fraught with potential complications. The most common complication following any attempt at repairing a massive tear is structural failure or re-tear. Despite advanced techniques like interval slides and marginal convergence, re-tear rates for massive tears range from 20% to as high as 90% in some series. However, it is well-documented that clinical success and pain relief can be maintained even in the presence of an asymptomatic structural re-tear, provided the force couples have been partially restored.
Other significant complications include postoperative stiffness (adhesive capsulitis), infection, and neurovascular injury. Iatrogenic injury to the suprascapular nerve during posterior releases or anchor placement at the superior glenoid (during SCR) can lead to devastating, irreversible atrophy of the remaining cuff musculature. Furthermore, hardware complications, such as anchor pullout from osteoporotic tuberosity bone, remain a constant threat in the elderly population.
| Complication | Estimated Incidence | Risk Factors | Prevention / Management |
|---|---|---|---|
| Structural Re-tear | 20% - 90% | Age > 65, Goutallier 3-4, high tension repair, smoking. | Maximize releases, double-row constructs, biologic augmentation. Manage non-operatively if asymptomatic. |
| Postoperative Stiffness | 5% - 15% | Prolonged immobilization, diabetes, concomitant capsular procedure. | Early passive ROM, judicious use of intra-articular corticosteroids, arthroscopic capsular release if refractory. |
| Infection (P. acnes / C. acnes) | 1% - 3% | Male gender, prolonged surgical time, open procedures. | Benzoyl peroxide prep, meticulous sterile technique, IV antibiotics. Requires prompt arthroscopic washout and targeted antibiotics. |
| Suprascapular Nerve Injury | < 1% | Aggressive posterior interval slide, medial dissection > 1.5 cm from glenoid. | Stay lateral to the glenoid rim during posterior releases. Observe for spontaneous recovery; EMG at 3 months. |
| Progression to Arthropathy | Variable | Failure of repair, continued superior humeral escape. | Monitor radiographically. Definitive salvage is Reverse Total Shoulder Arthroplasty (RTSA). |
When joint-preserving operations fail and the patient develops progressive, debilitating pain and pseudoparalysis (cuff tear arthropathy), salvage management is required. The Reverse Total Shoulder Arthroplasty (RTSA) is the definitive salvage procedure. By reversing the ball-and-socket geometry, the center of rotation is medialized and distalized. This effectively recruits the deltoid muscle, increasing its moment arm and resting tension, allowing it to act as the primary elevator of the arm in the absence of a functioning rotator cuff.
Phased Post-Operative Rehabilitation Protocols
Rehabilitation following the repair or reconstruction of a massive rotator cuff tear is a delicate balancing act between protecting the tenuous surgical construct and preventing debilitating postoperative stiffness. A slow, phased, and highly supervised physical therapy protocol is mandatory. The rehabilitation timeline is generally more conservative than that of a standard small or medium rotator cuff repair.
Phase I: Maximum Protection (Weeks 0 to 6)
The primary goal in Phase I is the protection of the repair. The patient is placed in an abduction sling (often at 15 to 30 degrees of abduction to reduce tension on the supraspinatus). Absolute avoidance of active shoulder motion is strictly enforced. Therapy consists solely of passive range of motion (PROM) exercises, typically limited to 90 degrees of forward flexion and 20 degrees of external rotation to prevent stress on the anchors. Pendulum exercises and scapular retractions are initiated to maintain scapulothoracic mobility.
Phase II: Moderate Protection and Active-Assisted Motion (Weeks 6 to 12)
At 6 weeks, provided there is clinical evidence of early healing and minimal pain, the sling is gradually weaned. Active-assisted range of motion (AAROM) is introduced utilizing pulleys, cane exercises, and wall walks. The goal is to restore full passive and active-assisted motion by week 10 to 12. Submaximal isometric exercises for the deltoid and intact rotator cuff muscles may begin late in this phase. For patients who underwent tendon transfers (e.g., lower trapezius), specific biofeedback and neuromuscular re-education are critical during this phase to train the transferred muscle to fire in its new, out-of-phase biomechanical role.
Phase III: Strengthening and Return to Function (Weeks 12 to 24+)
Active range of motion (AROM) against gravity is permitted only after 12 weeks. Isotonic strengthening begins with light resistance bands and progresses to free weights, focusing heavily on the periscapular stabilizers, deltoid, and remaining rotator cuff force couples. Patients are counseled that maximal medical improvement following a massive cuff repair or reconstruction may take up to 12 to 18 months. Return to heavy lifting or strenuous overhead activities is generally discouraged to protect the longevity of the repair.
Summary of Landmark Literature and Clinical Guidelines
The evolution of treatment for massive and irreparable rotator cuff tears is deeply rooted in several landmark biomechanical and clinical studies. Mastery of this literature is essential for the academic orthopedic surgeon.
Burkhart’s seminal work in the early 1990s revolutionized our understanding of rotator cuff biomechanics. He introduced the concepts of the "suspensory force couples," the "rotator cable," and the biomechanical rationale for partial repair. Burkhart demonstrated that restoring the transverse force couple (subscapularis and infraspinatus) could restore stable glenohumeral kinematics even if the superior supraspinatus footprint remained uncovered. This laid the foundation for the marginal convergence technique, which mathematically reduces strain on the tear margin.
Gerber’s extensive research on massive tears defined the parameters of tendon retraction and muscle degeneration. Gerber popularized the latissimus dorsi tendon transfer for irreparable posterosuperior tears, demonstrating significant improvements in active external rotation and forward flexion in appropriately selected young patients without arthritis. More recently, Elhassan has pioneered the use of the lower trapezius transfer, arguing that its force vector is more anatomical and "in-phase" with the native infraspinatus compared to the latissimus dorsi.
In the realm of joint preservation, Mihata’s introduction of the Superior Capsule Reconstruction (SCR) in 2012 provided a novel biomechanical solution for the irreparable tear. By reconstructing the superior capsule, Mihata demonstrated a restoration of the superior restraint to the humeral head, preventing superior escape and improving deltoid efficiency. While early clinical results were highly promising, mid-to-long-term data has shown variable graft healing rates, emphasizing the need for strict patient selection.
Finally, the work of Grammont, and later Sirveaux and Boileau, established the Reverse Total Shoulder Arthroplasty as the ultimate solution for cuff tear arthropathy and pseudoparalysis. The Grammont principles of medializing and distalizing the center of rotation remain the bedrock of modern RTSA design, reliably restoring function to elderly patients with truly irreparable pathology.
Through a combination of rigorous clinical evaluation, advanced arthroscopic mobilization techniques such as interval slides, and a deep understanding of salvage options, the orthopedic surgeon can successfully navigate the formidable challenge of the massive and potentially irreparable rotator cuff tear.
