Pediatric Distal Radius Salter-Harris Type II Fracture: Diagnosis & Management Case Study
Key Takeaway
A pediatric Salter-Harris Type II distal radius fracture involves the distal radius metaphysis extending through the physis, often from a FOOSH injury. Diagnosis includes clinical examination for "dinner fork" deformity and localized tenderness, confirmed by PA, lateral, and oblique X-rays revealing the metaphyseal and physeal components, often with a "Thurston Holland fragment."
Patient Presentation and History
A 10-year-old right-hand dominant male presented to the orthopedic emergency department following a high-energy traumatic event sustained during a competitive soccer match. The mechanism of injury involved a direct, high-velocity impact to the left upper extremity followed by a fall onto an outstretched hand as the patient attempted to break his fall and brace against the turf. The patient reported immediate, severe pain, functional impotence of the affected limb, and gross deformity of the left wrist. There was no reported direct head trauma, loss of consciousness, or axial loading to the cervical spine.
His past medical history is unremarkable, with no known drug allergies, prior surgical interventions, or previous fractures. He is pre-pubertal, corresponding to Tanner Stage I, with no diagnosed skeletal dysplasias, metabolic bone conditions, or connective tissue disorders. The patient's parents report that he is a highly active, multi-sport athlete, participating in year-round competitive soccer and basketball, which establishes a high baseline functional demand.
Biomechanics of Pediatric Physeal Injuries
The mechanism of a fall onto an outstretched hand generates complex multi-planar forces across the radiocarpal joint and distal forearm. In the pediatric population, the biomechanical properties of the skeletal system differ significantly from adults. The ligaments and joint capsules are biomechanically stronger than the cartilaginous physis (growth plate). Consequently, energy that would typically result in a ligamentous sprain or carpal bone fracture in an adult is transferred directly to the structurally vulnerable physis in a child.
During wrist hyperextension, the strong volar radiocarpal ligaments become taut, creating a tension band effect that transmits a sheer force across the distal radius. The physis typically fails through the zone of provisional calcification and the zone of hypertrophy, as these layers lack the abundant collagen matrix found in the resting and proliferating zones. As the shear force propagates, it exits through the metaphysis on the compression side (dorsal aspect), resulting in the classic Salter-Harris Type II fracture pattern. The thick, robust pediatric periosteum often remains intact on the compression (dorsal) side, acting as a periosteal hinge, while tearing completely on the tension (volar) side. This periosteal hinge plays a critical role in both the displacement pattern and the subsequent reduction maneuvers.
Clinical Examination Findings
Upon initial assessment in the trauma bay, the patient was in acute distress, guarding the left upper extremity. Initial trauma primary survey (Airway, Breathing, Circulation, Disability, Exposure) was intact and unremarkable. Focus was directed to the isolated left upper extremity injury.
Inspection and Soft Tissue Assessment
Gross deformity of the distal forearm and wrist was immediately evident. The presentation was consistent with an apex volar angulation and dorsal displacement of the distal fracture fragment, clinically manifesting as the classic "dinner fork" deformity. Significant, tense swelling was observed circumferentially around the radiocarpal joint extending into the distal third of the forearm.
Careful evaluation of the soft tissue envelope revealed no open wounds, abrasions, or lacerations, classifying this as a closed injury. There was no skin tenting or blanching over the dorsal bony prominence that would necessitate emergent, un-imaged reduction to prevent skin necrosis. While the swelling was substantial, the forearm compartments were soft and compressible proximally. There were no signs of impending acute compartment syndrome, such as pain out of proportion to the injury or pain with passive stretch of the digits, though the high-energy nature of the injury required vigilant serial monitoring.
Palpation and Range of Motion
Palpation was conducted with extreme care to minimize patient discomfort. Diffuse, exquisite tenderness was elicited circumferentially over the distal radius, localizing maximally to the distal radial metaphysis and the anatomic location of the physis. Palpation of the distal ulna revealed minimal tenderness, suggesting that the injury was primarily isolated to the radius, without a concomitant ulnar shaft or distal ulnar physeal fracture.
The ulnar styloid was non-tender, and the distal radioulnar joint space did not exhibit palpable widening or gross instability, although full assessment was limited by acute pain. No crepitus was intentionally elicited, as gentle manipulation was deferred pending radiographic confirmation of the fracture pattern. All active and passive radiocarpal range of motion arcs (flexion, extension, radial deviation, ulnar deviation) as well as forearm rotation (pronation, supination) were severely limited secondary to pain, mechanical block from the deformity, and involuntary muscle guarding.
Neurological and Vascular Assessment
A comprehensive neurovascular examination of the distal extremity is paramount in severely displaced pediatric distal radius fractures due to the proximity of the median nerve and radial artery to the volar metaphyseal spike.
Sensation to light touch and two-point discrimination were intact and symmetric across the median, ulnar, and radial nerve distributions of the hand. Motor function was assessed within the limits of patient tolerance. The patient demonstrated intact function of the anterior interosseous nerve (AIN) by performing an "OK" sign (flexion of the interphalangeal joint of the thumb and distal interphalangeal joint of the index finger). Posterior interosseous nerve (PIN) function was confirmed via active extension of the thumb interphalangeal joint and digital metacarpophalangeal joints. Intrinsic ulnar nerve motor function was intact, demonstrated by digit abduction and adduction.
Vascular assessment revealed strong, bounding, and symmetric radial and ulnar pulses bilaterally. Capillary refill was brisk, occurring in under two seconds in all five digits. The digits were warm and well-perfused, with no evidence of pallor, poikilothermia, or paresthesias, confirming an intact vascular supply.
Imaging and Diagnostics
Standard orthopedic trauma radiographic evaluation of the left wrist was obtained, comprising orthogonal posteroanterior, lateral, and oblique projections. Accurate radiographic interpretation requires careful analysis of the fracture geometry, the degree of displacement, and the integrity of adjacent anatomical structures.
Radiographic Analysis
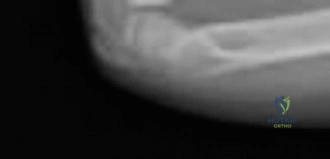
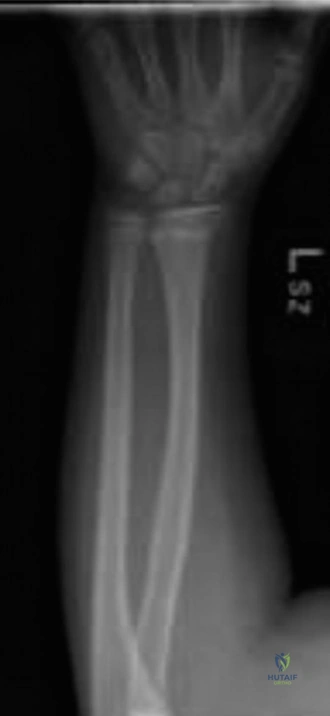
The initial posteroanterior projection demonstrated a transverse fracture line propagating through the distal metaphysis of the radius. The fracture line extended proximally from the radial cortex and exited through the physis on the ulnar side.
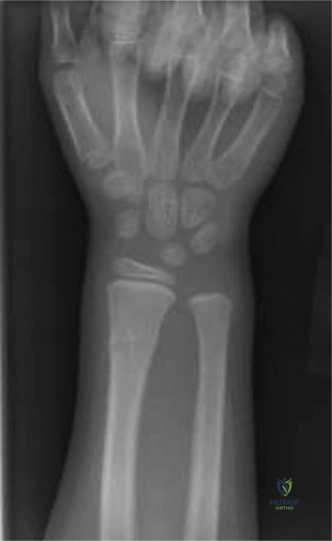
This specific propagation pattern is the hallmark of a Salter-Harris Type II fracture. There was significant dorsal displacement of the distal epiphyseal-metaphyseal fragment relative to the proximal radial shaft. The lateral radiograph provided critical information regarding the sagittal plane deformity.

The lateral view confirmed the Salter-Harris Type II classification, revealing marked dorsal displacement and an apex volar angulation measuring approximately 35 degrees. Furthermore, there was significant overriding of the fracture fragments, with approximately 75% dorsal cortical translation.
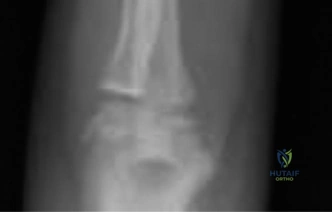
An additional oblique view was obtained to further delineate the metaphyseal component and assess for intra-articular extension or occult carpal pathology.
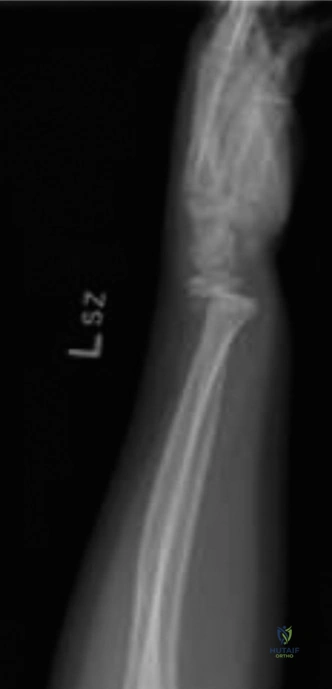
The oblique projection clearly highlighted the "Thurston Holland fragment." This is the pathognomonic triangular metaphyseal fragment that remains attached to the epiphysis on the compression side of the injury. The presence of this fragment confirms that the fracture line has exited through the metaphysis rather than traversing the entire physis (which would be a Salter-Harris Type I) or entering the epiphysis and joint space (Salter-Harris Type III or IV).
The distal radioulnar joint appeared radiographically congruent on all views, with no evidence of an associated ulnar shaft fracture, ulnar styloid avulsion, or widening of the radioulnar interval. The carpal arcs of Gilula were intact, and the growth plate of the distal ulna appeared uninjured.
Advanced Imaging Considerations
In the context of typical, non-comminuted pediatric distal radius physeal fractures, advanced imaging modalities such as Computed Tomography or Magnetic Resonance Imaging are generally not indicated and do not alter acute management. The diagnosis and surgical planning can almost universally be accomplished with high-quality orthogonal plain radiographs.
However, specific indications for advanced imaging in pediatric wrist trauma include:
* Computed Tomography: Indicated when there is high suspicion of intra-articular extension (Salter-Harris Type III or IV injuries) that is not clearly delineated on plain films, significant metaphyseal comminution precluding accurate assessment of the articular surface, or when evaluating complex fracture-dislocations (e.g., suspected Galeazzi equivalent lesions with subtle distal radioulnar joint subluxation). CT with 3D reconstruction is invaluable for preoperative templating in complex intra-articular fractures requiring precise anatomical reduction.
* Magnetic Resonance Imaging: MRI is reserved for cases of suspected occult fractures (e.g., radiographically negative scaphoid fractures with persistent anatomic snuffbox tenderness), evaluation of acute ligamentous injuries (scapholunate or lunotriquetral ligament tears), or assessment of the triangular fibrocartilage complex in the setting of persistent ulnar-sided wrist pain following skeletal healing. MRI is also the gold standard for evaluating suspected physeal bars (premature partial growth arrest) in the delayed post-operative setting.
Differential Diagnosis
When evaluating a pediatric patient with acute wrist trauma and deformity, the differential diagnosis must encompass a spectrum of osseous, physeal, and ligamentous injuries. Accurate differentiation is critical, as management algorithms and prognostic implications vary significantly among these pathologies.
| Diagnosis | Clinical Features | Radiographic Hallmarks | Management Implications |
|---|---|---|---|
| Salter-Harris Type II Distal Radius Fracture | Severe pain, gross deformity (dinner fork), maximal tenderness over the physis. High-energy mechanism. | Fracture through the physis exiting the metaphysis. Presence of a Thurston Holland fragment. Varying degrees of displacement and angulation. | Requires anatomical or near-anatomical reduction. High risk of displacement necessitates close follow-up. Operative intervention (CRPP) indicated for unstable or unacceptably displaced patterns. |
| Pediatric Torus Buckle Fracture | Mild to moderate pain, localized swelling, typically no gross deformity. Low-energy mechanism. | Cortical buckling or bulging, typically at the metaphyseal-diaphyseal junction. No distinct fracture line traversing the entire cortex. | Inherently stable. Managed non-operatively with a removable splint or short arm cast for comfort. Excellent prognosis with virtually zero risk of growth arrest. |
| Complete Distal Radius Metaphyseal Fracture | Severe pain, deformity, crepitus. Swelling proximal to the radiocarpal joint. | Transverse, oblique, or spiral fracture line completely traversing the metaphysis, proximal to the physis. The physis is radiographically intact. | Managed with closed reduction and casting. Higher tolerance for angulation due to profound remodeling potential of the metaphysis compared to the physis. CRPP if highly unstable. |
| Galeazzi Equivalent Lesion | Wrist pain, deformity, prominent distal ulna. Pain with forearm rotation. | Distal radius fracture (often physeal) combined with distal ulnar physeal separation or complete rupture of the distal radioulnar joint ligaments. | Requires precise reduction of both the radius and the DRUJ. Highly unstable. Often necessitates operative fixation of the radius and potentially stabilization of the DRUJ to prevent chronic instability. |
| Salter-Harris Type I Distal Radius Fracture | Tenderness precisely along the physeal line. May lack gross deformity if undisplaced. | Widening of the radiolucent physeal line. No metaphyseal or epiphyseal fracture lines. May appear normal on initial radiographs if spontaneously reduced. | Often managed non-operatively with casting. Diagnosis is sometimes clinical or confirmed retrospectively by periosteal reaction on follow-up imaging. Low risk of growth arrest if undisplaced. |
Surgical Decision Making and Classification
The management of pediatric distal radius fractures is dictated by the patient's age (which correlates with remaining growth and remodeling potential), the fracture classification, the degree of initial displacement, and the inherent stability of the fracture pattern.
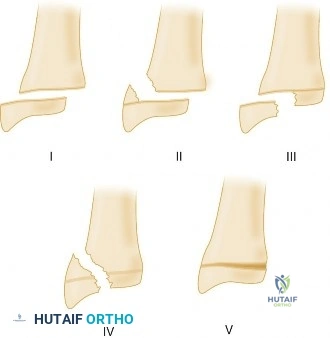
Salter-Harris Classification and Prognosis
The Salter-Harris classification system remains the standard for describing physeal injuries. This case represents a Type II injury, which is the most common physeal fracture, accounting for approximately 75% of all growth plate injuries. The fracture line propagates through the hypertrophic zone of the physis and exits through the metaphysis. Because the generative layers of the physis (the resting and proliferating zones) typically remain attached to the epiphysis and maintain their epiphyseal vascular supply, the prognosis for continued normal growth in Salter-Harris Type II fractures is generally excellent, provided that severe initial trauma to the germinal cells has not occurred and iatrogenic damage is avoided during reduction.
Remodeling Potential and Acceptable Alignment
Pediatric bone possesses a remarkable capacity for remodeling, governed by the Hueter-Volkmann law and Wolff's law. The distal radius is responsible for approximately 75% to 80% of the longitudinal growth of the entire forearm. Consequently, it has the highest remodeling potential of any physis in the upper extremity.
Remodeling is most robust in the sagittal plane (flexion and extension). Deformities in the coronal plane (radial and ulnar deviation) remodel less predictably, and rotational deformities exhibit virtually zero remodeling potential. A widely accepted clinical heuristic is that the distal radius can remodel approximately 1 degree of sagittal angulation per month of remaining growth.
However, the patient's age of 10 years is a critical factor. While he is pre-pubertal, he is approaching the adolescent growth spurt. For a 10-year-old child, acceptable radiographic parameters for non-operative management of a distal radius fracture typically include:
* Less than 20 to 25 degrees of sagittal plane angulation.
* Less than 10 degrees of coronal plane angulation.
* Less than 50% translation.
* Minimal to no rotational malalignment.
Rationale for Operative Intervention
In this specific case, the initial radiographs demonstrated approximately 35 degrees of apex volar angulation and 75% dorsal translation. These parameters significantly exceed the acceptable limits for a 10-year-old patient. While some remodeling would undoubtedly occur, accepting 35 degrees of angulation in a highly active 10-year-old carries a high risk of residual deformity, altered radiocarpal kinematics, and potential limitation in terminal wrist flexion.
Furthermore, fractures presenting with greater than 50% initial translation are notoriously unstable. Even if an anatomical closed reduction is achieved in the emergency department, the risk of secondary displacement within the cast during the first two weeks is unacceptably high, often reported to be between 25% and 40% for severely displaced patterns.
Loss of reduction necessitates a repeated closed reduction maneuver. Multiple reduction attempts significantly increase the shear forces across the vulnerable physis, exponentially increasing the risk of iatrogenic premature physeal closure and subsequent growth arrest. The "one and done" principle is paramount in pediatric physeal trauma: the surgeon should aim for a single, definitive reduction.
Therefore, given the unacceptable initial displacement, the high risk of secondary loss of reduction, and the imperative to avoid multiple manipulations of the physis, the decision was made to proceed with surgical intervention in the form of Closed Reduction and Percutaneous Pinning under general anesthesia. This approach ensures anatomical alignment, provides rigid mechanical stability, prevents secondary displacement, and minimizes the risk of physeal trauma associated with repeated manipulations.
Surgical Technique and Intervention
The patient was taken to the orthopedic operating theater. The surgical objective was to achieve an anatomical or near-anatomical reduction of the physeal fracture and stabilize it with percutaneous K-wires to maintain alignment during the initial phases of osseous healing.
Patient Positioning and Preparation
The patient was placed in the supine position on a standard radiolucent operating table. General endotracheal anesthesia was administered to ensure complete muscle relaxation, which is critical for facilitating reduction without excessive force. A non-sterile pneumatic tourniquet was placed proximally on the left brachium, although it is rarely inflated for closed reduction and percutaneous pinning unless an open reduction becomes necessary.
The left upper extremity was prepped and draped in a standard sterile orthopedic fashion, allowing free access from the elbow to the digits. A sterile mini-C-arm fluoroscopy unit was brought into the field, positioned parallel to the surgical table to allow for seamless orthogonal imaging without compromising the sterile field.
Reduction Maneuvers
The closed reduction maneuver was performed utilizing Charnley's principles of fracture reduction.
1. Exaggeration of the Deformity: The initial step involved gentle hyperextension of the wrist to recreate the dorsal deformity. This maneuver disengages the overriding metaphyseal fragments and unlocks the dorsal periosteal hinge.
2. Traction: Sustained, steady longitudinal traction was applied to the digits (specifically the index and middle fingers) while counter-traction was applied to the proximal forearm by an assistant. This longitudinal traction overcomes the deforming forces of the robust extrinsic flexor and extensor musculature.
3. Translation and Flexion: While maintaining traction, direct volar pressure was applied to the dorsal aspect of the distal epiphyseal fragment using the surgeon's thumb, while simultaneous dorsal pressure was applied to the volar aspect of the proximal radial metaphysis. The wrist was then brought into flexion and slight ulnar deviation to tension the intact dorsal periosteum, which acts as a tension band to lock the reduction in place.
Following the reduction maneuver, the wrist was held in slight flexion and ulnar deviation, and fluoroscopic imaging was obtained to assess the alignment.
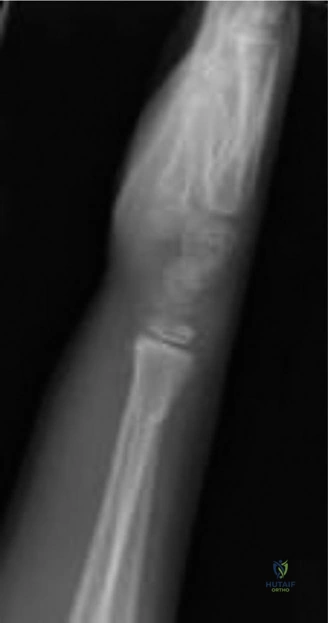
The intra-operative posteroanterior fluoroscopic view demonstrated excellent restoration of the radial length and correction of the coronal plane alignment. The fracture fragments appeared anatomically apposed.

The intra-operative lateral fluoroscopic view confirmed successful reduction of the dorsal displacement and complete correction of the apex volar angulation. The volar cortical continuity was restored, and the dorsal periosteal hinge appeared to be holding the reduction in an anatomical position.
Percutaneous Pinning Construct
Despite the excellent fluoroscopic appearance of the closed reduction, the initial displacement parameters (75% translation) indicated a highly unstable fracture pattern. To prevent secondary loss of reduction, percutaneous pinning was performed.
Smooth 0.062-inch (1.6 mm) Kirschner wires (K-wires) were selected. Smooth wires are preferred over threaded wires in pediatric trauma as they are less likely to cause permanent damage to the physeal chondrocytes during insertion and removal.
A standard crossed-pin configuration was utilized to provide maximum biomechanical stability against both bending and torsional forces.
1. Radial Styloid Pin: The first K-wire was introduced percutaneously starting at the tip of the radial styloid. A small stab incision was made, and blunt dissection with a hemostat was performed down to the bone to protect the superficial sensory branch of the radial nerve. The wire was driven obliquely across the
Clinical & Radiographic Imaging