Pediatric Ankle Pain: Diagnosis Involves the Subtalar Joint
Key Takeaway
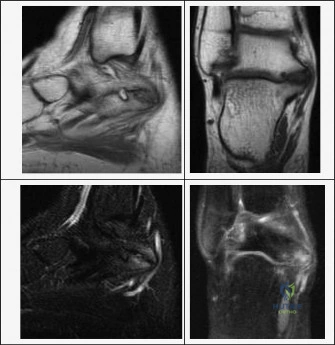
Here are the crucial details you must know about Pediatric Ankle Pain: Diagnosis Involves the Subtalar Joint. Talocalcaneal coalition is a fibrous, cartilaginous, or bony connection between the talus and calcaneus, causing vague, deep medial ankle discomfort. Prevalent in adolescents (12-16 years) due to segmentation failure, it commonly involves of the subtalar joint, leading to limited motion. This condition can present with a lump under the medial malleolus and potentially a valgus hindfoot.
Introduction and Epidemiology
Pediatric ankle pain is a frequent chief complaint in orthopedic clinics, often initially misdiagnosed as recurrent lateral ankle sprains or non-specific mechanical pain. However, a meticulous clinical and radiographic evaluation frequently localizes the pathology not to the talocrural joint, but to the subtalar joint complex. The most prominent and surgically relevant etiology of pediatric subtalar pain is the tarsal coalition—an abnormal fibrous, cartilaginous, or osseous connection between two or more tarsal bones resulting from a failure of mesenchymal segmentation during embryogenesis.
Tarsal coalitions have an estimated prevalence of 1% to 13% in the general population, though many remain asymptomatic. When symptomatic, they typically present during the second decade of life as the cartilaginous anlage begins to ossify, progressively restricting hindfoot motion and increasing mechanical stress on adjacent joints. The two most common types are calcaneonavicular (CN) and talocalcaneal (TC) coalitions, which together account for approximately 90% of all cases. Calcaneonavicular coalitions typically ossify and become symptomatic earlier, between the ages of 8 and 12 years. Talocalcaneal coalitions, which most frequently involve the middle facet of the subtalar joint, ossify later and typically present between the ages of 12 and 16 years.
Bilateral involvement is observed in 50% to 60% of patients. While other conditions such as juvenile idiopathic arthritis, osteochondritis dissecans of the talus, and post-traumatic subtalar fibrosis can generate pediatric subtalar pain, tarsal coalition remains the primary structural and surgically correctable paradigm. Understanding the intricate mechanics of the subtalar joint is paramount for diagnosing these conditions and executing precise surgical interventions that restore hindfoot kinematics and alleviate pain.
Surgical Anatomy and Biomechanics
The subtalar joint, or talocalcaneal joint, is a complex, multi-faceted articulation responsible for the inversion and eversion of the hindfoot, playing a critical role in accommodating uneven terrain and translating tibial rotation into foot pronation and supination.
The joint is anatomically divided into two distinct chambers separated by the sinus tarsi and the tarsal canal. The posterior chamber consists of the large posterior facet of the calcaneus articulating with the posterior facet of the talus. The anterior chamber, often referred to as the talocalcaneonavicular (TCN) joint, includes the anterior and middle facets of the calcaneus, the head of the talus, and the posterior surface of the navicular. The middle facet is supported by the sustentaculum tali, a medial projection of the calcaneus that serves as a critical anatomical landmark during medial surgical approaches.
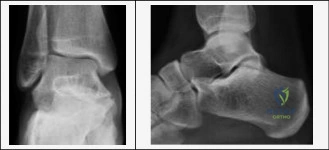
Ligamentous stability of the subtalar joint is provided by the intrinsic ligaments of the sinus tarsi, primarily the interosseous talocalcaneal ligament and the cervical ligament. The interosseous ligament lies in the tarsal canal and acts as the primary restraint to excessive eversion, while the cervical ligament lies more laterally in the sinus tarsi and restricts excessive inversion.
Biomechanically, the subtalar joint functions as a single-axis hinge, often likened to a mitered hinge. The axis of rotation passes from the posterolateral calcaneus to the anteromedial talar neck, angled approximately 42 degrees upward from the transverse plane and 16 degrees medial to the sagittal plane. This unique orientation dictates that motion occurs as a coupled mechanism: inversion is coupled with plantarflexion and internal rotation of the foot (supination), while eversion is coupled with dorsiflexion and external rotation (pronation).
When a tarsal coalition restricts this coupled motion, the normal biomechanical chain is disrupted. The energy usually absorbed by subtalar motion is transferred to the talocrural (ankle) joint and the transverse tarsal (Chopart) joint. Over time, this abnormal stress distribution leads to adaptive changes, including the classic "talar beak" (a traction osteophyte at the dorsal talar neck) and eventual degenerative arthrosis of the surrounding joints. The peroneal musculature often undergoes spastic contracture in an attempt to splint the painful, rigid subtalar joint, leading to the classic clinical presentation of a peroneal spastic flatfoot.
Indications and Contraindications
The management of pediatric subtalar pain secondary to tarsal coalition depends on the patient's age, the type and extent of the coalition, the presence of secondary degenerative changes, and the response to conservative management. Non-operative management, consisting of short-leg casting, custom orthotics (UCBL), and physical therapy, is the first-line treatment. Surgical intervention is indicated when non-operative measures fail to relieve pain and restore function.
| Parameter | Operative Indications | Non Operative Indications | Contraindications to Resection |
|---|---|---|---|
| Clinical Status | Persistent pain > 3-6 months despite conservative care; recurrent peroneal spasticity. | Incidental finding; asymptomatic patient; first-time presentation of pain. | Active local or systemic infection; severe peripheral neuropathy. |
| Coalition Size | TC coalition involving < 50% of the posterior facet; localized CN coalition. | Small, fibrous coalitions responsive to immobilization. | TC coalition > 50% of posterior facet area (requires arthrodesis instead). |
| Joint Health | Absence of advanced degenerative changes in the subtalar or Chopart joints. | Mild pain with no radiographic arthrosis. | Advanced arthrosis of the posterior facet or transverse tarsal joint. |
| Foot Alignment | Mild to moderate valgus that is correctable or well-tolerated. | Pain-free rigid flatfoot. | Severe, rigid valgus deformity (requires corrective osteotomy or fusion). |
| Patient Age | Skeletally immature or young adult with preserved joint cartilage. | Very young patients where ossification has not yet occurred. | Advanced age with globally stiff, arthritic hindfoot. |

Pre Operative Planning and Patient Positioning
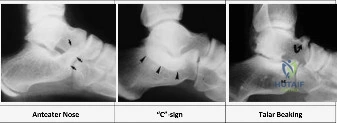
Thorough preoperative planning relies heavily on advanced imaging. While weight-bearing orthogonal radiographs of the foot and ankle are the starting point, they are often insufficient for complete surgical planning. Radiographic signs such as the "C-sign" (continuity of the talar dome and sustentaculum tali) and the "anteater nose sign" (elongation of the anterior process of the calcaneus) suggest TC and CN coalitions, respectively.
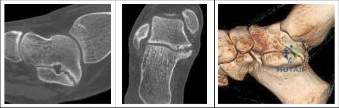
Computed Tomography (CT) is the gold standard for mapping the exact three-dimensional anatomy of the coalition. For TC coalitions, coronal CT slices perpendicular to the posterior facet are critical for calculating the percentage of joint surface involved. A coalition involving more than 50% of the posterior facet surface area is generally considered a contraindication to simple resection, as the remaining joint will likely be unstable and degenerate rapidly; these cases are better served by subtalar arthrodesis. Magnetic Resonance Imaging (MRI) is reserved for cases where a fibrous or cartilaginous coalition is suspected but not clearly visible on CT, or to evaluate the integrity of the surrounding cartilage and tendons.
Patient positioning is dictated by the specific approach required for the coalition type:
Positioning for Calcaneonavicular Coalition
For a CN coalition, the patient is placed supine on the operating table. A large bump is placed under the ipsilateral hip to internally rotate the leg, bringing the lateral aspect of the foot into a direct superior orientation. A well-padded thigh tourniquet is applied. The limb is prepped and draped in the standard sterile fashion.
Positioning for Talocalcaneal Coalition
For a TC coalition (which typically involves the middle facet), a medial approach is required. The patient is placed supine, and the hip is allowed to externally rotate into a "frog-leg" position, exposing the medial aspect of the hindfoot. A thigh tourniquet is utilized. A radiolucent table is mandatory for both procedures to allow for unencumbered intraoperative fluoroscopy.
Detailed Surgical Approach and Technique
The surgical objective in tarsal coalition resection is the complete excision of the abnormal bar, restoration of hindfoot motion, and the interposition of tissue to prevent recurrence.
Calcaneonavicular Coalition Resection Technique
The CN coalition is approached laterally.
- Incision and Dissection: An Ollier-type incision is made over the sinus tarsi, extending obliquely from the inferior tip of the lateral malleolus toward the base of the fourth metatarsal. Subcutaneous tissues are bluntly dissected, taking care to identify and protect the intermediate dorsal cutaneous nerve superiorly and the sural nerve inferiorly.
- Muscle Elevation: The extensor digitorum brevis (EDB) muscle belly is identified. Its proximal origin on the lateral calcaneus is sharply elevated and reflected distally. A tagging suture is placed in the proximal EDB to facilitate later interposition.
- Exposure of the Coalition: Elevation of the EDB exposes the anterior process of the calcaneus and the lateral aspect of the navicular. The coalition will appear as a bony, cartilaginous, or fibrous bridge connecting these two structures. The calcaneocuboid joint lies immediately inferior and must be identified and protected.
- Resection: Using a combination of osteotomes, rongeurs, and a high-speed burr, a rectangular block of the coalition is resected. The resection must be generous. Proximally, the resection extends to the normal anterior calcaneal wall. Distally, it extends to the normal navicular surface. Medially, the resection must reach the talar head. A common error is incomplete medial resection.
- Confirmation: Intraoperative fluoroscopy is used to confirm complete removal. The surgeon should be able to pass an instrument freely between the calcaneus and navicular, and hindfoot motion should be noticeably improved.
- Interposition: To prevent recurrence, the previously tagged EDB muscle belly is mobilized, drawn into the resection defect, and secured to the medial soft tissues or through a drill hole in the cuboid using absorbable suture. Alternatively, free fat grafting can be utilized.
Talocalcaneal Coalition Resection Technique
The TC coalition, typically located at the middle facet, requires a meticulous medial approach due to the proximity of the tarsal tunnel structures.
- Incision: A longitudinal medial incision is made, starting just distal and posterior to the medial malleolus and extending anteriorly toward the navicular tuberosity, paralleling the course of the posterior tibial tendon (PTT).
- Deep Dissection and Retraction: The flexor retinaculum is divided. The PTT is identified and retracted superiorly. The flexor digitorum longus (FDL) tendon is identified and retracted inferiorly. This internervous/intertendinous plane exposes the sustentaculum tali. The neurovascular bundle (posterior tibial artery and tibial nerve) lies posterior and inferior to the FDL and must be meticulously protected throughout the case.
- Identification of the Coalition: The flexor hallucis longus (FHL) tendon runs directly beneath the sustentaculum tali. The coalition is typically found just superior to the sustentaculum. The periosteum over the sustentaculum is elevated to expose the bony bridge between the talus and calcaneus.
- Resection: Excision begins at the anterior aspect of the coalition, near the posterior margin of the anterior facet, and proceeds posteriorly. A 1/4-inch osteotome or a high-speed burr is used. The resection must follow the upward slope of the posterior facet to avoid violating the normal joint cartilage.
- Restoration of Motion: Resection continues until normal articular cartilage of the posterior facet is visualized and the fibrous tissue of the tarsal canal is reached laterally. The surgeon should manually invert and evert the heel; a sudden "release" and restoration of motion indicate complete resection.
- Interposition: Bone wax is applied to the raw cancellous bone surfaces. A free fat graft, typically harvested from the gluteal fold or the local subcutaneous tissue, is packed into the defect. Alternatively, a split portion of the FHL tendon can be interposed.
Subtalar Arthrodesis Technique
In cases where a TC coalition involves greater than 50% of the posterior facet, or if severe degenerative changes are present, resection will lead to painful instability. In these instances, a subtalar arthrodesis is indicated.
- Approach: A lateral approach via the sinus tarsi is utilized.
- Joint Preparation: The posterior, middle, and anterior facets are denuded of all remaining cartilage down to bleeding subchondral bone using curettes and burrs. The coalition itself is taken down to allow for realignment of the hindfoot.
- Reduction and Fixation: The hindfoot is positioned in approximately 5 degrees of valgus. Fixation is typically achieved with one or two large-diameter (6.5mm or 7.3mm) cannulated screws placed from the posterior non-weight-bearing surface of the calcaneus, directed anteriorly and superiorly into the talar body and neck.
Complications and Management
Surgical management of tarsal coalitions, while generally successful, carries a specific set of potential complications. Meticulous surgical technique and appropriate patient selection are the primary defense against these adverse outcomes.
| Complication | Estimated Incidence | Etiology / Risk Factors | Prevention and Salvage Strategy |
|---|---|---|---|
| Recurrence of Coalition | 10% - 15% | Incomplete initial resection; failure of interposition graft; hematoma ossification. | Prevention: Generous bone resection; secure interposition of EDB or fat graft; early ROM. Salvage: Revision resection vs. subtalar arthrodesis. |
| Sural Nerve Injury | 2% - 5% | Retraction injury or direct laceration during the lateral Ollier approach. | Prevention: Careful blunt dissection in the subcutaneous tissues; minimal retraction tension. Salvage: Neuroma excision and implantation into muscle or bone. |
| Tibial Nerve Injury | < 2% | Iatrogenic injury during medial approach for TC coalition resection. | Prevention: Strict adherence to the plane between PTT and FDL; precise retractor placement. Salvage: Neurolysis; nerve grafting if transected (rare). |
| Continued Pain / Arthrosis | 15% - 20% | Pre-existing degenerative changes; unrecognized secondary coalition; joint instability post-resection. | Prevention: Strict preoperative CT mapping; avoid resection if >50% posterior facet involvement. Salvage: Subtalar or triple arthrodesis. |
| Progression of Flatfoot | 5% - 10% | Loss of medial column support; failure to address severe preoperative valgus. | Prevention: Concomitant medializing calcaneal osteotomy or lateral column lengthening if severe valgus exists. Salvage: Corrective osteotomies or hindfoot fusion. |
Management of Persistent Pain
When a patient presents with persistent pain following a coalition resection, a systematic evaluation is required. A CT scan should be obtained to evaluate for inadequate resection or recurrence of the bony bar. If the resection was adequate, the pain is likely secondary to advanced degenerative arthrosis of the posterior facet or the transverse tarsal joints. In these scenarios, the salvage procedure of choice is a subtalar arthrodesis. If the Chopart joint is also severely arthritic, a triple arthrodesis (subtalar, talonavicular, and calcaneocuboid) may be necessary to provide a stable, plantigrade, and pain-free foot.
Post Operative Rehabilitation Protocols
The postoperative rehabilitation protocol is designed to balance the need for early motion (to prevent recurrent scarring and stiffness) with the need for soft tissue healing.
Phase I: Maximum Protection (Weeks 0-2)
Immediately postoperatively, the patient is placed in a bulky, well-padded short-leg splint in a neutral position. The patient is strictly non-weight-bearing on the operative extremity. Elevation and ice are prioritized to control edema and minimize the risk of wound dehiscence.
Phase II: Early Motion and Progressive Weight Bearing (Weeks 2-6)
At the two-week mark, sutures are removed. If the wound is healing well, the patient is transitioned to a removable controlled ankle motion (CAM) boot.
Crucially, active and active-assisted range of motion (ROM) exercises of the subtalar and ankle joints are initiated immediately. The patient is instructed to perform inversion, eversion, dorsiflexion, and plantarflexion exercises multiple times daily. This early mobilization is the most critical non-surgical step in preventing the recurrence of a fibrous or bony coalition. Weight-bearing is gradually progressed from touch-down to partial weight-bearing over this four-week period, as tolerated by pain.
Phase III: Strengthening and Return to Activity (Weeks 6-12)
By week six, the patient is typically transitioned out of the CAM boot and into supportive athletic footwear, often supplemented with a custom orthotic to support the medial longitudinal arch. Physical therapy focuses on strengthening the peroneal and posterior tibial musculature, improving proprioception, and normalizing the gait pattern. Full weight-bearing is expected. Return to high-impact sports or strenuous physical activity is generally permitted between 3 to 6 months postoperatively, contingent upon the restoration of painless, functional hindfoot motion and adequate radiographic healing of the resection site.
Summary of Key Literature and Guidelines
The academic understanding and surgical management of tarsal coalitions have been shaped by several foundational studies and modern radiographic guidelines.
Cowell's seminal work in the 1970s firmly established the lateral approach and EDB interposition as the gold standard for calcaneonavicular coalitions, demonstrating significantly reduced recurrence rates compared to simple resection. His principles regarding the necessity of a wide, rectangular resection remain the standard of care today.
For talocalcaneal coalitions, Mubarak and colleagues revolutionized the preoperative assessment by emphasizing the necessity of CT scanning. They established the critical threshold of 50% posterior facet involvement; resections performed on coalitions exceeding this size reliably result in postoperative instability, progressive valgus collapse, and severe arthrosis. Their guidelines dictate that extensive TC coalitions are best managed with primary subtalar arthrodesis.
More recently, Wilde et al. contributed significantly to the understanding of the middle facet's role in TC coalitions, detailing the medial approach and the importance of preserving the FHL tendon and the neurovascular bundle. Modern literature also increasingly supports the use of free fat grafts as an alternative to muscle or tendon interposition, citing lower donor site morbidity and excellent anti-osteogenic properties.
Current guidelines from pediatric orthopedic societies recommend an initial trial of non-operative management for all newly diagnosed, non-arthritic tarsal coalitions. However, they strongly advocate for early surgical resection in patients who fail conservative therapy, emphasizing that timely intervention before the onset of secondary degenerative changes yields the most favorable long-term functional outcomes. Integrating advanced CT mapping with precise surgical technique allows the orthopedic surgeon to effectively resolve pediatric subtalar pain and restore the complex biomechanics of the hindfoot.
