Crucial Positioning for General Anaesthesia in Pediatric Orthopaedics

Key Takeaway
Learn more about Crucial Positioning for General Anaesthesia in Pediatric Orthopaedics and how to manage it. Epiphysiodesis is a pediatric orthopedic procedure that destroys the physis to equalize leg length discrepancies, primarily targeting growth plates around the knee. Indications include true LLD of 2–5 cm or greater than 7 cm. Preoperative planning involves determining LLD at maturity. Proper **positioning general anaesthesia** is crucial for surgical success and patient safety, mitigating risks like neurovascular injury and infection.
Comprehensive Introduction and Patho-Epidemiology
The intersection of pediatric orthopaedic surgery and general anaesthesia presents a unique crucible of clinical challenges, demanding an exhaustive understanding of both physiological immaturity and precise spatial geometry. While the primary objective of any orthopaedic intervention—be it epiphysiodesis for limb length discrepancy, reduction of developmental dysplasia of the hip (DDH), or pinning of a slipped capital femoral epiphysis (SCFE)—is mechanical and biological restoration, the foundation of a successful outcome is invariably laid before the first incision. Crucial positioning for general anaesthesia is not merely a matter of surgical access; it is a critical determinant of intraoperative stability, fluoroscopic visibility, and the prevention of catastrophic iatrogenic complications such as nerve palsies, compartment syndrome, and avascular necrosis (AVN).

Pediatric patients possess distinct anatomical and physiological characteristics that profoundly influence positioning strategies. Their increased body surface area-to-mass ratio predisposes them to rapid intraoperative hypothermia, necessitating the strategic placement of forced-air warming blankets that must not impede the surgical field or fluoroscopic arcs. Furthermore, the ligamentous laxity inherent in the pediatric population, while advantageous for certain closed reductions, increases the vulnerability of major articulations to subluxation and subsequent neurovascular traction injuries during prolonged positioning.

The patho-epidemiology of the conditions necessitating these interventions further dictates positioning parameters. For instance, in the management of limb length discrepancies (LLD), which affect approximately 1 in 1,000 children to a degree requiring surgical intervention, epiphysiodesis involves the deliberate destruction of the physis to allow equalisation of limb lengths. Precise positioning is mandatory to ensure orthogonal fluoroscopic views of the physis, preventing asymmetric physeal ablation that would result in progressive angular deformity. Similarly, in DDH and SCFE, the positioning directly impacts the delicate vascular supply to the proximal femur, where improper abduction or internal rotation can precipitate irreversible ischemic necrosis.
Detailed Surgical Anatomy and Biomechanics
Physeal Anatomy and Growth Mechanics
A rigorous comprehension of physeal anatomy is paramount when planning an epiphysiodesis or guided growth procedure. The physis is a highly organized cartilaginous structure divided into distinct histological zones: the resting zone, the proliferative zone, the hypertrophic zone (further subdivided into maturation, degeneration, and provisional calcification), and the primary spongiosa. Epiphysiodesis aims to mechanically disrupt the proliferative and hypertrophic zones, thereby arresting longitudinal growth. Biomechanically, the distal femoral and proximal tibial physes contribute approximately 65% of the total longitudinal growth of the lower extremity. Positioning on the operating table must allow for unhindered anterior-posterior (AP) and lateral fluoroscopy to verify that surgical instruments (drills, curettes, or guided growth plates) are perfectly centralized within these critical zones.

Proximal Femoral Vascularity and Hip Biomechanics
In procedures addressing DDH, Perthes disease, and SCFE, the vascular anatomy of the proximal femur is the primary limiting factor in patient positioning. The femoral head is supplied predominantly by the profound branch of the medial circumflex femoral artery (MFCA), which traverses the posterosuperior aspect of the femoral neck. In DDH, placing the hip in extreme abduction (the historical "frog-leg" position) forces the cartilaginous femoral head against the acetabular rim, mechanically compressing the retinacular vessels and leading to AVN. Biomechanically safe positioning—often termed the "human position"—maintains the hip in approximately 90 to 100 degrees of flexion and limits abduction to a safe zone of 40 to 50 degrees.

For SCFE, the biomechanical instability of the capital femoral epiphysis dictates that the patient must be transferred and positioned with extreme care. The use of a fracture table with traction is generally contraindicated for unstable SCFE, as longitudinal traction and forced internal rotation can stretch the already compromised retinacular vessels, inducing ischemia. Instead, positioning the patient supine on a completely radiolucent flat table allows for in situ fixation without applying deleterious deforming forces to the vulnerable physis.
Exhaustive Indications and Contraindications
The decision to proceed with pediatric orthopaedic interventions under general anaesthesia requires a meticulous risk-benefit analysis, heavily weighted by the patient's skeletal maturity and the specific pathology. The following table delineates the core indications and contraindications for the primary procedures, with a specific focus on positioning constraints.
| Surgical Procedure | Primary Indications | Absolute Contraindications | Positioning / Anaesthesia Constraints |
|---|---|---|---|
| Epiphysiodesis | Projected LLD > 2.0 cm at skeletal maturity; Constitutional tall stature (rare). | Skeletal maturity; LLD < 1.5 cm; Active physeal infection. | Requires fully radiolucent table; Contraindicated if severe flexion contracture prevents orthogonal AP imaging. |
| DDH: Closed Reduction | Dislocated hip in child 6-18 months; Failure of Pavlik harness. | Teratologic dislocation; Severe neuromuscular dysplasia; Age > 18-24 months. | Extreme abduction > 60° strictly prohibited (AVN risk); Requires perineal post for spica casting. |
| DDH: Open Reduction | Failure of closed reduction; Age > 18 months; Interposed soft tissue (pulvinar, inverted limbus). | Active systemic infection; Uncontrolled coagulopathy. | Supine with ipsilateral bump; Must allow free draping of the entire lower extremity for intraoperative manipulation. |
| SCFE: In Situ Pinning | Confirmed SCFE (stable or unstable) to prevent further slippage. | Severe degenerative joint disease (requires salvage); Active infection. | Fracture table traction contraindicated in unstable slips; Flat radiolucent table mandatory. |
| CTEV (Clubfoot) Correction | Rigid equinovarus deformity; Failure of serial Ponseti casting (requires TAL). | Non-rigid, positional clubfoot (responds to stretching). | Prone or lateral positioning for extensive posteromedial release; Supine for percutaneous TAL. |
| Guided Growth (eight-Plate) | Coronal/sagittal plane angular deformities in a growing child. | Closed physes; Physiologic bowing (resolves spontaneously). | Supine; Requires unobstructed C-arm access for perfect AP and lateral physeal visualization. |


Pre-Operative Planning, Templating, and Patient Positioning
The Art of Pre-Operative Templating
Pre-operative planning in pediatric orthopaedics is a highly quantitative discipline. For epiphysiodesis, determining the exact timing of the surgical intervention is paramount. The surgeon must utilize validated predictive models, such as the Green-Anderson Growth Remaining charts, the Moseley straight-line graph, or the Paley Multiplier method. These tools synthesize the child's chronological age, skeletal age (assessed via Greulich and Pyle atlas of the left hand and wrist), and current LLD to predict the discrepancy at maturity. Over-correction or under-correction stems directly from errors in this pre-operative calculation phase.
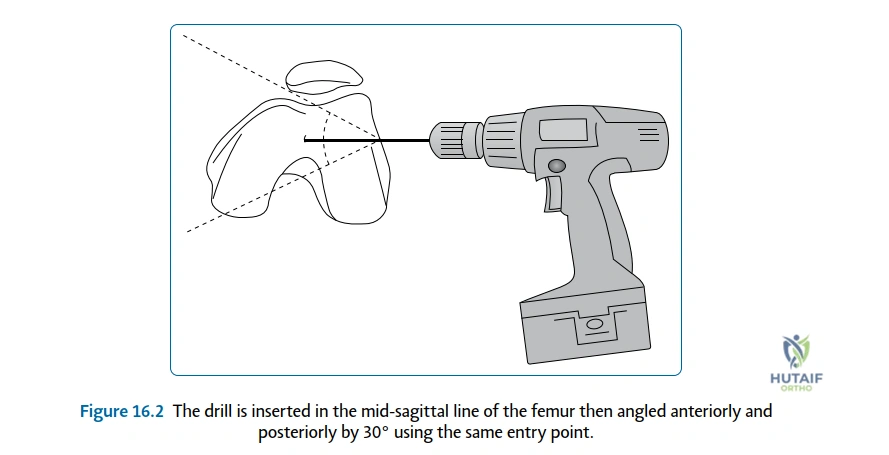
For DDH and pelvic osteotomies (e.g., Salter, Pemberton, or Dega), pre-operative templating involves calculating the acetabular index and the center-edge angle of Wiberg on a standardized AP pelvis radiograph. The surgeon must template the exact angle and depth of the osteotomy to ensure adequate anterior and lateral coverage of the femoral head without causing iatrogenic impingement.

General Anaesthesia and Crucial Positioning Protocols
Once the patient is induced under general anaesthesia, the critical phase of positioning commences. The standard operating table is often insufficient for pediatric orthopaedics; a fully radiolucent cantilever table (e.g., Jackson table or OSI flat top) is mandatory.
- Airway and Neurovascular Protection: The pediatric airway is secured, and the head is placed on a specialized gel doughnut to prevent occipital alopecia and pressure necrosis. The arms are typically tucked securely at the patient's sides using draw sheets, ensuring the elbows are padded and the forearms are in a neutral position to prevent ulnar nerve compression at the cubital tunnel and brachial plexus traction.
- The "Free-Floating" Lower Extremity: For procedures like epiphysiodesis, SCFE pinning, and DDH open reductions, the operative extremity must be prepped and draped completely free. A sterile tourniquet is often applied as high as possible on the proximal thigh.
- Fluoroscopic Triangulation: Before the surgical prep, the C-arm must be brought into the field to confirm that orthogonal AP and lateral views can be obtained without moving the patient's core. The C-arm should arc around the table, not the patient.

For SCFE positioning, the patient is placed supine on a flat radiolucent table. A bump is placed under the ipsilateral sacrum to elevate the affected hip, correcting for the external rotation deformity inherent to the slip and bringing the femoral neck parallel to the floor. This subtle positioning maneuver is crucial for accurate percutaneous guidewire placement.

Step-by-Step Surgical Approach and Fixation Technique
Epiphysiodesis: Permanent Physeal Arrest
Epiphysiodesis involves the deliberate, irreversible destruction of the physis to allow equalisation of limb lengths. The modern gold standard is the percutaneous technique under fluoroscopic guidance, which minimizes soft tissue dissection and accelerates recovery.
- Incision and Approach: Small 1 cm incisions are made over the medial and lateral aspects of the target physis (distal femur or proximal tibia/fibula).
- Fluoroscopic Localization: Keith needles are inserted percutaneously to identify the exact center of the physis on both AP and lateral views.
- Physeal Ablation: A cannulated drill (typically 4.5 mm or 5.0 mm depending on patient size) is passed over the guidewires, traversing the physis from medial to lateral and vice versa.
- Curettage: Angled curettes are introduced through the drill holes. The surgeon systematically destroys the cartilaginous physis in a sweeping motion, ensuring at least 7-8% of the cross-sectional area of the physis is ablated to guarantee the formation of a solid osseous bar.
- Closure: The wounds are thoroughly irrigated to remove cartilaginous debris, which could cause ectopic ossification, and closed in layers.

Guided Growth: Temporary Hemiepiphysiodesis
For angular deformities (genu varum or genu valgum), temporary hemiepiphysiodesis utilizes the tension-band principle.
1. Positioning: Supine, radiolucent table.
2. Implantation: A non-locking two-hole plate (eight-Plate) is centered exactly over the physis on the convex side of the deformity.
3. Fixation: Cannulated screws are placed into the epiphysis and metaphysis. As the child grows, the plate acts as a tether, gradually correcting the angular deformity. Once correction is achieved, the hardware is removed to allow resumption of normal growth.

Developmental Dysplasia of the Hip: Open Reduction and Pelvic Osteotomy
When closed reduction fails or the child is over 18 months of age, open reduction is indicated.
1. Approach: An anterior Smith-Petersen approach is utilized, exploiting the internervous plane between the sartorius (femoral nerve) and tensor fasciae latae (superior gluteal nerve).
2. Intra-articular Obstacles: The iliopsoas tendon is released at the pelvic brim. The joint capsule is opened via a T-shaped arthrotomy. The ligamentum teres is excised, and the fibrofatty pulvinar is cleared from the acetabular fossa. The transverse acetabular ligament is incised to allow seating of the femoral head.
3. Pelvic Osteotomy (Salter): If there is significant acetabular dysplasia (acetabular index > 25 degrees in a toddler), an innominate osteotomy is performed. A Gigli saw is passed through the greater sciatic notch to the anterior inferior iliac spine. The osteotomy is opened anteriorly and laterally, and a triangular structural bone graft (harvested from the iliac crest) is impacted into the defect. Fixation is achieved with two threaded Kirschner wires.


Slipped Capital Femoral Epiphysis (SCFE): In Situ Pinning
- Guidewire Placement: With the patient supine on a flat table, an anterior approach is used. A guidewire is advanced from the anterior aspect of the proximal femur, aiming for the center of the epiphysis on both AP and lateral fluoroscopic views.
- Screw Fixation: A single, large-diameter (6.5 mm or 7.3 mm) partially threaded cannulated screw is advanced over the wire. The threads must cross the physis and engage the epiphysis completely, but the surgeon must maintain a minimum distance of 5 mm from the subchondral bone to prevent joint penetration.
- Approach to the Contralateral Hip: Prophylactic pinning of the contralateral hip is heavily debated but highly recommended in patients with endocrinopathies or those under 10 years of age, given the high risk of sequential bilateral slips.


Tendo-Achilles Lengthening (TAL) and CTEV Correction
In the management of Congenital Talipes Equinovarus (CTEV), the Ponseti method of serial casting corrects the cavus, adductus, and varus components. However, the equinus contracture often persists, necessitating a percutaneous TAL.
1. Positioning: The infant is positioned supine with the hip externally rotated and the knee flexed to 90 degrees.
2. Tenotomy: Under local or brief general anaesthesia, a #11 blade is inserted parallel to the medial border of the Achilles tendon, approximately 1.5 cm proximal to the calcaneal insertion. The blade is rotated 90 degrees, and the tendon is sectioned completely, yielding a palpable "pop" and immediate dorsiflexion of 15 to 20 degrees.
Complications, Incidence Rates, and Salvage Management
Despite rigorous preoperative planning and meticulous surgical execution, complications in pediatric orthopaedics can be profound, often altering the trajectory of a child's skeletal development. The following table highlights critical complications, their incidence rates, and established salvage protocols.
| Complication | Associated Procedure | Incidence Rate | Pathophysiology & Salvage Management |
|---|---|---|---|
| Avascular Necrosis (AVN) | DDH Reduction, SCFE Pinning | 5% - 15% | Patho: Compression of the medial circumflex femoral artery (MFCA) retinacular branches. Salvage: Hinged abduction bracing; Core decompression; Proximal femoral varus derotational osteotomy (VDRO) to contain the head. |
| Incomplete Physeal Arrest | Epiphysiodesis | 2% - 5% | Patho: Insufficient ablation of the physeal plate leading to continued asymmetric growth and angular deformity. Salvage: Repeat epiphysiodesis; Corrective osteotomy (e.g., distal femoral opening wedge) at skeletal maturity. |
| Chondrolysis | SCFE Pinning | 1% - 7% | Patho: Unrecognized intra-articular hardware penetration causing rapid cartilage destruction. Salvage: Immediate hardware removal; Aggressive physical therapy; Arthrodiastasis; Eventual arthrodesis or arthroplasty in adulthood. |
| Sciatic/Femoral Nerve Palsy | Pelvic Osteotomies, DDH | 1% - 3% | Patho: Iatrogenic traction during positioning or direct retractor pressure in the sciatic notch. Salvage: Immediate removal of cast/positioning; AFO bracing for foot drop; Nerve exploration if no recovery by 3-6 months. |
| Re-dislocation | DDH Open/Closed Reduction | 3% - 8% | Patho: Inadequate initial reduction, failure to clear pulvinar, or loss of cast integrity. Salvage: Revision open reduction; Addition of femoral shortening osteotomy or complex pelvic osteotomy. |


Positioning-related complications, particularly peripheral nerve palsies, are entirely preventable. The brachial plexus is exquisitely sensitive to hyperabduction of the arm past 90 degrees, while the common peroneal nerve is vulnerable to compression against the fibular head if the lateral leg is inadequately padded during lateral or supine positioning. Diligence during the initial setup under anaesthesia is the sole prophylactic measure against these iatrogenic injuries.
Phased Post-Operative Rehabilitation Protocols
The post-operative rehabilitation phase in pediatric orthopaedics is highly procedure-specific and relies heavily on the compliance of both the patient and the caregivers.
Spica Cast Management (DDH and Femoral Osteotomies)
Following closed or open reduction of DDH, the child is immobilized in a 1.5 hip spica cast. The critical parameters of the cast include maintaining the "human position" (100 degrees flexion, 40 degrees abduction) while leaving the abdomen free enough to accommodate post-prandial distension.
* Phase I (0-6 weeks): Strict immobilization. Caregivers are educated on hygiene, diapering techniques within the cast, and positioning the child on bean bags to prevent pressure sores.
* Phase II (6-12 weeks): The cast is typically changed under general anaesthesia at 6 weeks to accommodate growth. After 12 weeks, the child is transitioned to an abduction orthosis (e.g., Rhino cruiser) worn full-time, then weaned to nighttime wear until normal acetabular development is confirmed radiographically.

Weight-Bearing Protocols (Epiphysiodesis, SCFE, Guided Growth)
- Epiphysiodesis and Guided Growth: These procedures are remarkably well-tolerated. Patients are typically allowed immediate weight-bearing as tolerated (WBAT) with the assistance of crutches. Return to full athletic activities is permitted once full range of motion and baseline quadriceps strength are restored, usually within 4 to 6 weeks.
- **SCFE
Clinical & Radiographic Imaging Archive