Optimal Approaches to Treating Fractures: Faster Healing, Better Results
Key Takeaway
Looking for accurate information on Optimal Approaches to Treating Fractures: Faster Healing, Better Results? Approaches to treating fractures encompass traditional methods like immobilization via casts or surgery, alongside rehabilitation. Innovative options include Low-Intensity Pulsed Ultrasound (LIPUS) therapy, custom 3D-printed casts and implants, and Platelet-Rich Plasma (PRP) therapy. These advanced approaches aim to accelerate healing, minimize pain, and optimize patient outcomes by combining established and cutting-edge techniques.
Introduction and Epidemiology
Fractures represent a significant orthopedic burden characterized by a structural discontinuity in bone integrity resulting from trauma repetitive stress or pathological processes. While historically defined by macroscopic bone disruption a more granular understanding encompasses various classifications including open versus closed simple versus comminuted stable versus unstable and intra-articular versus extra-articular injuries. The etiology is diverse ranging from high-energy mechanisms such as motor vehicle collisions and falls from height to low-energy trauma prevalent in osteoporotic populations stress fractures in athletes and pathological fractures secondary to underlying neoplastic or metabolic disease processes.
Globally fractures contribute substantially to morbidity disability and healthcare expenditure. The incidence of fractures exhibits a classic bimodal distribution varying significantly with age sex and geographical location. The first peak occurs in young males typically associated with high-energy polytrauma requiring complex reconstructive efforts. Pediatric fractures are also common within the younger demographic presenting unique challenges and opportunities related to the physis and the robust remodeling potential of the immature skeleton.
The second peak occurs in the elderly population predominantly affecting females. A substantial and increasing public health concern is the rising prevalence of fragility fractures driven by the global increase in life expectancy and the concomitant rise in osteoporosis. Fractures of the proximal femur distal radius and proximal humerus are hallmark fragility injuries. Hip fractures in particular are associated with high one-year mortality rates approaching twenty to thirty percent and significant long-term functional decline underscoring the necessity for optimal accelerated management strategies.
The evolving understanding of fracture biology and biomechanics coupled with technological advancements in implant design has propelled a paradigm shift in orthopedic traumatology. The historical reliance on prolonged immobilization has been largely supplanted by sophisticated biologically sensitive and functionally oriented operative approaches. Modern fracture management prioritizes the restoration of mechanical alignment while meticulously preserving the local biological environment aiming to achieve faster healing times superior long-term functional outcomes and the mitigation of systemic complications associated with prolonged bed rest.
Surgical Anatomy and Biomechanics
A comprehensive understanding of surgical anatomy and biomechanics is fundamental to optimal fracture management and the selection of appropriate fixation constructs. Bone as a complex anisotropic composite material exhibits distinct mechanical and biological properties depending on its cortical and cancellous components. Cortical bone provides structural rigidity and strength resisting bending and torsional forces while cancellous bone offers excellent energy absorption and serves as a major site for metabolic activity and hematopoiesis.
Vascular Anatomy and Bone Healing
The vascular supply to bone is the critical determinant of healing potential and originates from both periosteal and medullary sources. The periosteal blood supply derived from the surrounding muscle capillary network provides approximately one-third of the diaphyseal blood flow and is particularly vital for the outer cortical bone. This delicate network is often compromised by the initial high-energy trauma or by extensive surgical dissection. Consequently modern surgical approaches emphasize the preservation of soft tissue attachments to mitigate iatrogenic devascularization. The endosteal blood supply derived from the nutrient medullary artery provides the remaining two-thirds of the diaphyseal flow and is crucial for intramedullary bone healing. While intramedullary reaming disrupts this supply the endosteal circulation exhibits a robust capacity for rapid revascularization.
Biomechanics of Fracture Fixation
The biomechanics of fracture healing dictates the choice of fixation strategy guided fundamentally by Perren's strain theory. Strain is defined as the relative change in gap length divided by the original gap length when subjected to physiological loading. Healing occurs through either primary direct or secondary indirect bone healing pathways depending on the mechanical environment.
Primary healing characterized by direct osteonal remodeling via cutting cones without intermediate callus formation requires absolute stability. Absolute stability dictates an interfragmentary strain of less than two percent. This is typically achieved through anatomical reduction and interfragmentary compression utilizing lag screws or dynamic compression plates. This approach is mandatory for simple intra-articular fractures where anatomical restoration of the joint surface is required to prevent post-traumatic osteoarthritis.
Secondary healing involves the formation of a robust external bridging callus and occurs under conditions of relative stability. Relative stability tolerates and indeed requires micro-motion generating an interfragmentary strain between two and ten percent. This mechanical environment stimulates chondrogenesis and subsequent endochondral ossification. Relative stability is the goal for complex comminuted diaphyseal fractures where anatomical reduction of every fragment would require excessive soft tissue stripping. Intramedullary nailing and bridging plate osteosynthesis are the quintessential techniques for achieving relative stability.
Implant Biomechanics
Implants function as either load-sharing or load-bearing devices. Intramedullary nails act as load-sharing devices positioned in the biomechanical central axis of the bone minimizing the bending moment and providing excellent resistance to bending and torsional forces. Plates applied to the tension band surface of a fractured bone convert tensile forces into compressive forces at the fracture site optimizing the mechanical environment for healing. Wolffs Law underscores the dynamic nature of this process wherein bone adapts its trabecular and cortical structure in response to applied mechanical stresses highlighting the importance of controlled progressive loading during the postoperative phase.
Indications and Contraindications
The decision algorithm for operative versus non-operative management of fractures requires a nuanced assessment of patient-specific physiological factors local soft tissue envelopes and the mechanical characteristics of the fracture pattern. The primary objective is to restore function while minimizing the risk of iatrogenic complications.
Operative Indications
Operative intervention is definitively indicated in scenarios where non-operative management predictably leads to unacceptable functional outcomes or systemic morbidity. Open fractures necessitate emergent operative debridement and stabilization to mitigate infection risk. Polytrauma patients benefit from Early Total Care or Damage Control Orthopedics depending on their physiological stability to facilitate early mobilization and reduce the incidence of acute respiratory distress syndrome. Intra-articular fractures with step-off or gap displacement require operative anatomical reduction to minimize the risk of early-onset osteoarthritis. Furthermore fractures exhibiting inherent mechanical instability such as displaced femoral neck fractures or highly comminuted diaphyseal fractures failing closed reduction mandate surgical fixation.
Contraindications
Absolute contraindications to immediate definitive internal fixation include severe physiological instability active local infection at the operative site and critically compromised soft tissue envelopes such as severe fracture blisters or extensive degloving injuries. In these scenarios temporizing stabilization with external fixation is often employed. Relative contraindications include severe medical comorbidities precluding anesthesia non-ambulatory baseline status where the surgical risk outweighs functional benefit and severe osteopenia where implant purchase is highly likely to fail.
| Management Strategy | Primary Indications | Primary Contraindications |
|---|---|---|
| Operative Fixation | Open fractures polytrauma intra-articular displacement unstable fracture patterns failure of conservative management pathological fractures | Active local infection severe physiological instability hemodynamic shock inadequate soft tissue coverage terminal illness with short life expectancy |
| Non Operative Management | Stable non-displaced fractures pediatric buckle fractures high surgical risk patients non-ambulatory baseline isolated low-energy upper extremity fractures | Open fractures neurovascular compromise unstable intra-articular fractures polytrauma requiring early mobilization |
| External Fixation | Damage control in polytrauma severe soft tissue compromise open fractures with massive contamination periarticular fractures awaiting swelling resolution | Definitive management of simple diaphyseal fractures non-compliant patients definitive intra-articular reconstruction |
Pre Operative Planning and Patient Positioning
Meticulous preoperative planning is the cornerstone of successful orthopedic trauma surgery. The execution of a surgical plan begins long before the incision is made relying on comprehensive imaging templating and physiological optimization.
Imaging and Digital Templating
Standard orthogonal radiographs are mandatory for initial assessment. For complex periarticular fractures computed tomography is essential to delineate the three-dimensional fracture morphology identify impacted articular segments and plan screw trajectories. Digital templating utilizing calibrated radiographs allows the surgeon to anticipate implant size length and optimal anatomical placement. Templating also facilitates the anticipation of necessary adjunctive equipment such as bone graft substitutes specific reduction clamps or specialized retractors.
Patient Optimization and Timing
The timing of surgical intervention is dictated by the patients physiological status and the local soft tissue envelope. In the polytraumatized patient the concepts of Damage Control Orthopedics versus Early Total Care must be carefully applied. Patients exhibiting signs of the lethal triad coagulopathy hypothermia and acidosis should undergo rapid physiological stabilization and temporizing external fixation. Definitive fixation is delayed until physiological parameters normalize. For isolated closed fractures definitive fixation should ideally be performed once the initial soft tissue swelling has subsided indicated by the presence of skin wrinkling to minimize the risk of wound dehiscence and deep infection.
Positioning and Fluoroscopy
Patient positioning must facilitate optimal surgical exposure unobstructed fluoroscopic access and the application of traction if required. Radiolucent tables are standard for diaphyseal fractures allowing unhindered anterior-posterior and lateral fluoroscopic imaging. Traction tables are frequently utilized for femoral intramedullary nailing to maintain length and alignment during the procedure. The positioning of the C-arm must be planned to avoid interference with the surgical team while providing orthogonal views of the entire bone segment and adjacent joints. Meticulous padding of all bony prominences is mandatory to prevent perioperative neuropraxia.
Detailed Surgical Approach and Technique
The execution of surgical fracture fixation demands a rigorous adherence to anatomical principles soft tissue respect and precise biomechanical construct application. The chosen surgical approach must exploit internervous and intermuscular planes to access the osseous structures while minimizing denervation and devascularization.
Soft Tissue Management and Internervous Planes
The principle of atraumatic soft tissue handling cannot be overstated. Incisions should be planned to respect angiosomes and avoid crossing previous surgical scars at acute angles. Deep dissection must utilize established internervous planes. For example the anterolateral approach to the humerus exploits the plane between the brachialis innervated by the musculocutaneous nerve and the brachioradialis innervated by the radial nerve. The posterior approach to the humerus utilizes the interval between the lateral and long heads of the triceps. In the lower extremity the standard anterolateral approach to the tibia avoids major neurovascular structures by remaining anterior to the anterior tibial artery and deep peroneal nerve while the medial approach utilizes the subcutaneous border requiring minimal muscle elevation.
Reduction Techniques
Reduction maneuvers aim to restore length alignment and rotation. Direct reduction involves exposing the fracture site and utilizing instruments such as pointed reduction forceps or bone tenaculums to manipulate fragments directly. This technique is necessary for absolute stability constructs in simple fracture patterns. Indirect reduction techniques are paramount when aiming for relative stability in comminuted fractures. Indirect methods utilize traction femoral distractors Schanz pins functioning as joysticks or the implant itself to align the major osseous segments without disturbing the fracture hematoma or stripping the periosteum of the comminuted fragments.
Fixation Strategies and Plate Osteosynthesis
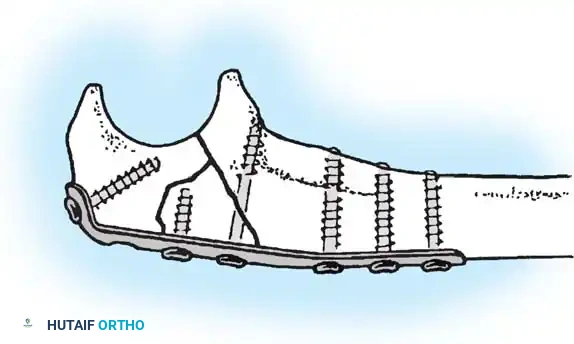
The application of plates must adhere to specific biomechanical functions based on the fracture pattern.
Neutralization plating is utilized to protect a primary lag screw from bending and torsional forces. The lag screw provides interfragmentary compression and the plate neutralizes physiological loads.
Compression plating utilizes dynamic compression principles via eccentrically drilled screws to generate axial compression across a transverse or short oblique fracture.
Buttress plating is employed in metaphyseal or periarticular fractures to resist shear forces preventing axial deformity. The plate must be applied to the cortex subjected to compressive forces.
Bridge plating is the standard for comminuted diaphyseal fractures. The plate spans the zone of comminution anchored only to the proximal and distal main fragments. This technique provides relative stability preserving the vascularity of the intermediate fragments and promoting robust secondary callus formation.
Minimally Invasive Plate Osteosynthesis
Minimally Invasive Plate Osteosynthesis represents a critical advancement in fracture management. By utilizing small proximal and distal incisions a plate is slid submuscularly or subcutaneously across the fracture zone. This technique relies entirely on indirect reduction and fluoroscopic guidance. Minimally Invasive Plate Osteosynthesis minimizes iatrogenic disruption of the periosteal blood supply and preserves the osteogenic fracture hematoma resulting in lower rates of nonunion and infection compared to traditional extensive open approaches.
Intramedullary Nailing Techniques
Intramedullary nailing is the gold standard for most diaphyseal fractures of the femur and tibia. The technique involves establishing a precise entry point passing a guide wire across the reduced fracture and sequentially reaming the medullary canal. Reaming generates autologous bone graft and allows for the insertion of a larger diameter nail increasing the biomechanical strength of the construct. The nail is subsequently locked proximally and distally with interlocking screws to control rotation and axial length. Meticulous attention to the entry point is critical as eccentric starting points can lead to iatrogenic malalignment or iatrogenic fracture propagation.
Complications and Management
Despite meticulous surgical technique and advanced implants fracture management is associated with a spectrum of biological and mechanical complications. Early recognition and aggressive management are essential to salvage the limb and optimize functional outcomes.
Biological Complications
Nonunion is defined as the cessation of fracture healing prior to complete consolidation typically diagnosed when no radiographic progression is observed over three consecutive months after a minimum of six to nine months post-injury. Hypertrophic nonunion characterized by abundant callus formation without bridging indicates adequate biology but inadequate mechanical stability. Management requires revising the fixation to a more rigid construct. Atrophic nonunion characterized by a lack of callus indicates biological failure often secondary to devascularization or infection. Management necessitates debridement decortication autologous bone grafting and revision of fixation.
Infection following internal fixation is a devastating complication. Acute postoperative infections require prompt aggressive surgical debridement implant retention if the construct remains stable and culture-directed intravenous antibiotic therapy. Chronic infections associated with nonunion or implant loosening mandate complete implant removal radical debridement of all necrotic bone and soft tissue placement of local antibiotic delivery systems such as antibiotic-impregnated cement spacers and stabilization with an external fixator until the infection is eradicated.
Mechanical Complications
Implant failure including plate breakage screw pull-out or nail fracture occurs when the mechanical loads placed on the construct exceed its fatigue life prior to bone consolidation. This is frequently a sequela of delayed union or nonunion where the implant is subjected to prolonged cyclical loading. Management requires revision surgery addressing the underlying biological or mechanical deficiency often involving larger implants bone grafting and altered weight-bearing protocols.
| Complication | Estimated Incidence | Primary Etiology | Salvage Strategy and Management |
|---|---|---|---|
| Aseptic Nonunion | 5 to 10 percent | Inadequate stability excessive soft tissue stripping smoking metabolic deficiencies | Hypertrophic requires increased stability atrophic requires biological stimulation bone graft and revision fixation |
| Deep Surgical Site Infection | 1 to 5 percent higher in open fractures | Contamination poor soft tissue envelope compromised host immunity | Aggressive serial debridement targeted systemic antibiotics implant removal if loose or unhealed |
| Malunion | 5 to 15 percent | Inadequate initial reduction loss of fixation premature weight bearing | Corrective osteotomy revision fixation if symptomatic or causing adjacent joint arthrosis |
| Implant Failure | 2 to 5 percent | Fatigue failure secondary to nonunion poor implant selection technical error | Revision osteosynthesis bone grafting addressing underlying biological failure |
| Post Traumatic Osteoarthritis | Variable highly dependent on joint | Intra-articular step-off cartilage necrosis altered joint biomechanics | Conservative management initially intra-articular injections arthrodesis or arthroplasty for end-stage disease |
Post Operative Rehabilitation Protocols
The surgical intervention represents only the first phase of fracture management. A structured biologically informed postoperative rehabilitation protocol is critical to achieving faster healing and better functional results. Rehabilitation must balance the mechanical protection of the fixation construct with the physiological benefits of early mobilization.
Weight Bearing Principles
Weight-bearing protocols are dictated by the fracture pattern the rigidity of the fixation construct and the quality of the host bone. Absolute stability constructs for simple diaphyseal fractures may allow for early partial weight bearing. Conversely complex intra-articular reconstructions or fixation in severely osteoporotic bone often necessitate a period of restricted non-weight bearing to prevent construct failure or articular subsidence. Intramedullary nailing of diaphyseal femur and tibia fractures typically permits immediate weight bearing as tolerated leveraging the load-sharing biomechanics of the nail to stimulate secondary bone healing via dynamic axial compression.
Range of Motion and Functional Recovery
Early initiation of active and active-assisted range of motion is imperative to prevent arthrofibrosis joint contractures and muscle atrophy. For periarticular fractures continuous passive motion machines may be utilized in the immediate postoperative period to facilitate cartilage nutrition and prevent intra-articular adhesions. The rehabilitation protocol must be individualized progressing from isolated joint mobilization to complex proprioceptive and functional kinetic chain exercises as radiographic and clinical healing progress.
Pharmacological and Systemic Adjuncts
Postoperative management must address systemic factors influencing bone healing and patient morbidity. Venous thromboembolism prophylaxis is mandatory following lower extremity trauma and pelvic fractures utilizing low molecular weight heparin or direct oral anticoagulants in accordance with current clinical guidelines. In the fragility fracture population the initiation of secondary fracture prevention protocols is critical. This includes comprehensive osteoporosis evaluation optimization of Vitamin D and calcium levels and the timely initiation of anti-resorptive or anabolic pharmacological therapies. Furthermore smoking cessation must be aggressively counseled as nicotine significantly impairs microvascular perfusion and osteogenesis drastically increasing the risk of delayed union and nonunion.
Summary of Key Literature and Guidelines
Evidence-based practice in orthopedic traumatology relies on a robust foundation of biomechanical research and large-scale clinical trials. Familiarity with landmark literature is essential for the academic orthopedic surgeon.
Foundational Biomechanical Studies
The foundational principles of modern fracture fixation are rooted in the work of Stephan Perren and the Arbeitsgemeinschaft für Osteosynthesefragen. Perrens strain theory remains the definitive biomechanical model explaining the mechanobiology of primary and secondary bone healing. The shift from absolute stability for all fractures to the acceptance of relative stability and biological osteosynthesis for comminuted fractures represents one of the most significant evolutions in the field directly resulting in decreased nonunion rates and improved functional outcomes.
Clinical Trials and Evidence Based Practice
The management of polytrauma patients has been heavily influenced by the literature surrounding Damage Control Orthopedics. Studies by Pape and Scalea demonstrated the mortality benefits of temporizing external fixation in physiologically exhausted patients mitigating the "second hit" phenomenon associated with prolonged early definitive surgery.
In the realm of specific fracture management large multicenter randomized controlled trials have shaped current guidelines. The Study to Prospectively Evaluate Reamed Intramedullary Nails in Patients with Tibial Fractures demonstrated the superiority of reamed over unreamed intramedullary nailing for closed tibial shaft fractures. For femoral neck fractures the Fixation using Alternative Implants for the Treatment of Hip fractures and the Hip Fracture Evaluation with Alternatives of Total Hip Arthroplasty versus Hemiarthroplasty trials have provided critical data guiding the choice between internal fixation hemiarthroplasty and total hip arthroplasty based on patient age displacement and baseline functional demand. Adherence to guidelines published by the Orthopaedic Trauma Association and national orthopedic bodies ensures the delivery of optimal standardized and evidence-based care aiming consistently for faster healing and superior clinical results.
