Orthopedic Shoulder And Review | Dr Hutaif Shoulder & E -...
Comprehensive 100-Question Exam
00:00
Start Quiz
Question 1
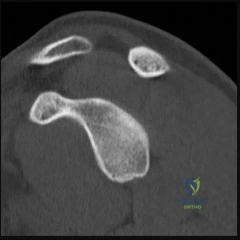
A 65-year-old female sustains a fall on an outstretched hand. Imaging reveals a proximal humerus fracture with the articular segment dislocated from the glenoid, and the lesser tuberosity displaced. According to the Neer classification, what is the primary determinant of a "part"?
Explanation
Question 2
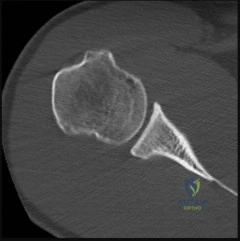
A 22-year-old football player sustains recurrent anterior shoulder dislocations. Preoperative imaging
reveals 25% anterior glenoid bone loss. What is the most appropriate surgical intervention to minimize recurrence?
Explanation
Question 3
A 72-year-old male with severe rotator cuff arthropathy and pseudoparalysis undergoes a reverse total shoulder arthroplasty (RTSA). Biomechanically, how does RTSA restore active forward elevation?
Explanation

Question 4
A 30-year-old elite volleyball player complains of vague posterior shoulder pain and weakness in external rotation. Examination reveals isolated atrophy of the infraspinatus with preserved supraspinatus bulk. Where is the most likely site of nerve compression?
Explanation
Question 5
During diagnostic arthroscopy on a 26-year-old baseball pitcher, the surgeon identifies a SLAP lesion characterized by a bucket-handle tear of the superior labrum with an intact biceps anchor. What type of SLAP tear is this according to Snyder's classification?
Explanation
Question 6
A 45-year-old male presents to the ED after a generalized tonic-clonic seizure. His shoulder is locked in internal rotation and he is unable to externally rotate. Radiographs show a 'lightbulb' sign. Which of the following associated injuries is most frequently seen in this condition?
Explanation
Question 7
A 55-year-old laborer has a massive, irreparable posterosuperior rotator cuff tear. He has an intact subscapularis and a negative hornblower's sign. He struggles primarily with loss of active external rotation and elevation. Which tendon transfer is most historically validated and appropriate for this specific deficit pattern?
Explanation
Question 8
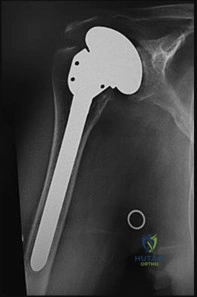
A 28-year-old female presents with a dull ache around her shoulder and medial scapular winging that noticeably worsens when pushing against a wall. Which nerve and muscle are most likely affected?
Explanation
Question 9
A 50-year-old diabetic female presents with global restriction of active and passive shoulder range of motion. She is currently in the 'freezing' phase of adhesive capsulitis. What histologic finding is most characteristic of the glenohumeral capsule in this condition?
Explanation
Question 10
A 19-year-old cyclist falls onto his shoulder. Radiographs demonstrate a midshaft clavicle fracture. Which of the following is considered an absolute indication for immediate open reduction and internal fixation (ORIF)?
Explanation
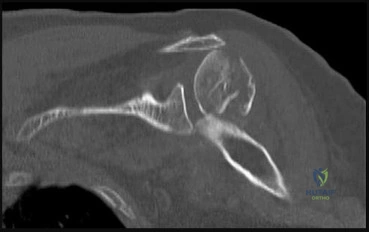
Question 11
A 68-year-old male with end-stage glenohumeral osteoarthritis is being considered for an anatomic Total Shoulder Arthroplasty (TSA). Which of the following is considered an absolute contraindication for an anatomic TSA in this patient?
Explanation
Question 12
A 24-year-old professional baseball pitcher presents with posterior shoulder pain during the late cocking phase of throwing. He exhibits a GIRD (glenohumeral internal rotation deficit) of 25 degrees. What is the primary pathophysiologic mechanism of his shoulder pain?
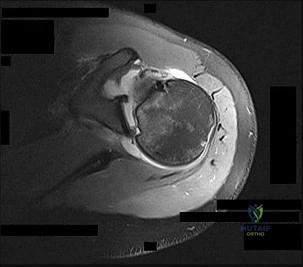
Explanation
Question 13
A 35-year-old male falls directly onto the point of his shoulder. Radiographs show a 150% superior displacement of the distal clavicle relative to the acromion, and the coracoclavicular distance is increased by 50% compared to the normal side. According to the Rockwood classification, what type of injury is this?
Explanation
Question 14
A 32-year-old competitive weightlifter feels a 'pop' and sudden pain in his anterior shoulder while performing a heavy bench press. Examination reveals loss of the anterior axillary fold and weakness in internal rotation. Which part of the pectoralis major is most commonly injured in this specific scenario?
Explanation
Question 15
A 17-year-old rugby player sustains a severe lateral blow to his shoulder and presents with shortness of breath, dysphagia, and a prominent soft tissue depression at the medial end of his clavicle. What is the most appropriate next step in management?
Explanation
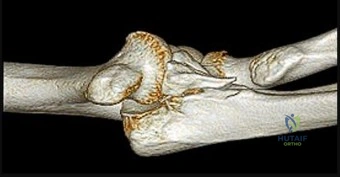
Question 16
A 29-year-old recreational tennis player presents with vague, poorly localized shoulder pain and paresthesias over the lateral deltoid. MRI reveals isolated denervation atrophy of the teres minor. Which vascular structure is most likely compressed along with the involved nerve in this syndrome?
Explanation
Question 17
A 13-year-old elite baseball pitcher complains of insidious onset, activity-related pain in his throwing shoulder. Radiographs reveal widening of the proximal humeral physis. What is the recommended initial management?
Explanation
Question 18
A 55-year-old male sustains an anterior shoulder dislocation. Post-reduction, he has numbness over the lateral aspect of his shoulder and inability to actively abduct his arm. An EMG performed at 3 weeks shows fibrillation potentials in the deltoid. What is the most appropriate management?
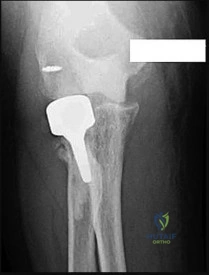
Explanation
Question 19
During an anatomic dissection of the shoulder, you isolate the coracoclavicular (CC) ligaments. Which of the following correctly describes the anatomical relationship and primary biomechanical function of these ligaments?
Explanation
Question 20
A 40-year-old male presents with severe, acute-onset right shoulder pain that lasted for two weeks, awakened him from sleep, and has now transitioned into profound weakness of shoulder abduction and external rotation. He reports a recent viral respiratory illness. MRI of the shoulder is unremarkable. What is the most likely diagnosis?
Explanation
Question 21
An 18-year-old male is injured during a rugby tackle. He presents to the trauma bay with a hoarse voice, mild stridor, and left shoulder pain. Examination reveals a visible depression at the medial aspect of the left clavicle. What is the most appropriate next step in the management of this patient?
Explanation

Question 22
Which of the following radiographic parameters is the most reliable predictor of humeral head ischemia following a complex proximal humerus fracture, according to the Hertel criteria?
Explanation
Question 23
A 28-year-old competitive weightlifter feels a sudden "pop" in his anterior axilla while performing a heavy bench press. Examination reveals loss of the anterior axillary fold and weakness in internal rotation and adduction. Which of the following describes the most common anatomic location of this injury?
Explanation

Question 24
A 26-year-old professional baseball pitcher presents with vague posterior shoulder pain and numbness over the lateral deltoid. MRI reveals isolated atrophy of the teres minor. Compression of the involved nerve is most likely occurring in a space bounded medially by which of the following structures?
Explanation
Question 25
A 31-year-old male volleyball player presents with insidious onset of right shoulder weakness. Physical exam reveals notable atrophy of the infraspinatus fossa but normal bulk of the supraspinatus. External rotation strength is significantly decreased, while abduction strength is preserved. What is the most likely etiology of this patient's condition?
Explanation

Question 26
Which of the following best describes the biomechanical alterations achieved by a Grammont-style reverse total shoulder arthroplasty compared to native shoulder anatomy?
Explanation
Question 27
In patients who undergo reverse total shoulder arthroplasty, scapular notching is a well-recognized radiographic phenomenon. Which surgical modification during the procedure most effectively reduces the incidence of inferior scapular notching?
Explanation

Question 28
A 62-year-old male with primary glenohumeral osteoarthritis is scheduled for a total shoulder arthroplasty. Preoperative CT scan demonstrates a biconcave glenoid with 20 degrees of retroversion and posterior subluxation of the humeral head. According to the Walch classification, what type of glenoid morphology is this?
Explanation
Question 29
During an anatomic coracoclavicular (CC) ligament reconstruction for a chronic type V acromioclavicular joint dislocation, the surgeon plans to drill the clavicle to recreate the conoid and trapezoid ligaments. Which of the following accurately describes the anatomic relationship of these ligaments?
Explanation
Question 30
The Latarjet procedure involves transfer of the coracoid process to the anterior glenoid neck. During the approach, the subscapularis muscle is often split longitudinally. Which nerve is at greatest risk of iatrogenic injury if this split is extended too far medially?
Explanation
Question 31
A 55-year-old male presents with a massive, irreparable tear of the subscapularis tendon following a failed repair. He complains of debilitating anterior pain, has a positive belly-press test, and increased passive external rotation. Which tendon transfer is most appropriate to restore anterior shoulder function?
Explanation
Question 32
A 48-year-old manual laborer has a massive, retracted, and fatty-infiltrated tear of the supraspinatus and infraspinatus. He lacks active external rotation and has a positive external rotation lag sign, but has intact subscapularis function and no significant glenohumeral arthritis. Which tendon transfer is most indicated for this patient?
Explanation
Question 33
A 25-year-old male is brought to the trauma bay after a high-speed motorcycle collision. His left upper extremity is pulseless, pale, and flail. Chest radiograph shows significant lateral displacement of the left scapula relative to the spine and a displaced clavicle fracture. What is the most critical next step in management?
Explanation

Question 34
A 13-year-old elite baseball pitcher presents with right shoulder pain when throwing. Radiographs demonstrate widening of the proximal humeral physis on the affected side compared to the contralateral side. What is the recommended initial management?
Explanation
Question 35
A 65-year-old female sustains an anterior shoulder dislocation. After successful closed reduction in the emergency department, post-reduction radiographs reveal a concentric glenohumeral joint but a displaced greater tuberosity fracture with 7 mm of superior displacement. What is the most appropriate management?
Explanation
Question 36
A 50-year-old female with poorly controlled type II diabetes presents with severe, progressive stiffness and pain in her right shoulder, consistent with the "freezing" stage of adhesive capsulitis. Which of the following histologic findings is most characteristic of the glenohumeral joint capsule in this condition?
Explanation
Question 37
A 40-year-old male presents to the ER after a generalized seizure. He holds his right arm firmly in internal rotation and adduction. Radiographs confirm a posterior glenohumeral dislocation. After closed reduction, a CT scan shows a reverse Hill-Sachs lesion involving 25% of the humeral head articular surface. Which of the following is the most appropriate surgical treatment?
Explanation

Question 38
Which of the following radiographic or demographic characteristics is most strongly associated with an increased risk of nonunion in conservatively managed midshaft clavicle fractures?
Explanation
Question 39
A 72-year-old female presents with chronic, intractable right shoulder pain and pseudoparalysis. Radiographs reveal an acromiohumeral distance (AHD) of 3 mm and acetabularization of the coracoacromial arch, but no significant glenohumeral arthritis. According to the Hamada classification, what grade is her rotator cuff arthropathy?
Explanation
Question 40
In a 65-year-old sedentary patient undergoing arthroscopic rotator cuff repair, a severely frayed and subluxated long head of the biceps tendon is noted. The surgeon decides to perform a biceps tenotomy rather than a tenodesis. Compared to tenodesis, which of the following is the most likely outcome of tenotomy?
Explanation
Question 41
A 28-year-old competitive weightlifter feels a pop in his anterior axilla while performing a heavy bench press. Examination reveals ecchymosis and loss of the anterior axillary fold. MRI confirms a complete rupture of the pectoralis major tendon at its insertion. In surgical repair, what is the normal anatomical relationship of the pectoralis major insertion footprint?
Explanation
Question 42
A 25-year-old motorcyclist presents after a high-speed collision. He has a flail upper extremity, massive swelling over the shoulder and chest wall, and absent radial and ulnar pulses. An AP radiograph shows severe lateral displacement of the scapula relative to the spinous processes. What is the most critical immediate step in the management of this condition?
Explanation
Question 43
A 22-year-old collegiate baseball pitcher complains of posterior shoulder pain during the late cocking phase of throwing. Physical examination reveals a glenohumeral internal rotation deficit (GIRD) of 25 degrees compared to the contralateral side. Which of the following best describes the pathophysiology of his internal impingement?
Explanation
Question 44
A 31-year-old elite volleyball player presents with insidious onset of right shoulder weakness. Physical examination reveals profound atrophy isolated to the infraspinatus fossa, with normal bulk of the supraspinatus. External rotation strength is significantly decreased, while abduction strength is preserved. What is the most likely anatomical location of the nerve compression?
Explanation
Question 45
A 17-year-old high school football player is tackled with a lateral compressive force to his left shoulder. He complains of left shoulder pain, dysphagia, and a choking sensation. Physical examination reveals a palpable depression at the medial end of the left clavicle. What is the most appropriate next step in management?
Explanation
Question 46
A 35-year-old male sustains a direct blow to the shoulder and presents with anterior shoulder pain. Imaging reveals a fracture of the coracoid process base extending into the superior glenoid. According to the Ogawa classification, which type of fracture is this, and what is the typical management?
Explanation
Question 47
An 68-year-old male with primary osteoarthritis of the shoulder is planned for an anatomic total shoulder arthroplasty. A preoperative CT scan reveals a biconcave glenoid with severe posterior wear and a retroversion of 20 degrees.
According to the Walch classification, what type of glenoid is this?

Explanation
Question 48
A 72-year-old female presents with pain and crepitus 3 years after a reverse total shoulder arthroplasty for cuff tear arthropathy. Radiographs demonstrate a radiolucent area on the scapular neck extending beyond the inferior screw of the glenoid baseplate.
According to the Sirveaux classification of scapular notching, what grade is this?

Explanation
Question 49
A 65-year-old female falls on her outstretched hand and sustains a displaced proximal humerus fracture. Which of the following radiographic findings (Hertel criteria) is considered the strongest predictor for the development of avascular necrosis (AVN) of the humeral head?
Explanation
Question 50
A 29-year-old male competitive tennis player complains of vague posterior shoulder pain and numbness over the lateral deltoid after overhead activities. MRI of the shoulder reveals isolated fatty atrophy of the teres minor muscle. Which of the following structures are most likely being compressed?
Explanation
Question 51
A 13-year-old male baseball pitcher complains of right shoulder pain during throwing. Radiographs demonstrate widening and lateral fragmentation of the proximal humeral physis. What is the most appropriate initial treatment?
Explanation
Question 52
A 55-year-old heavy laborer presents with a massive, retracted, and irreparable posterosuperior rotator cuff tear. He has significant weakness in external rotation and elevation. A latissimus dorsi tendon transfer is planned. Which of the following is an absolute contraindication to this procedure?
Explanation
Question 53
An orthopedic surgeon is performing an anatomic coracoclavicular (CC) ligament reconstruction for a chronic Type V AC joint separation. To accurately recreate the biomechanics, the surgeon must understand the anatomy of the native CC ligaments. Which of the following best describes the normal anatomical attachment of the CC ligaments on the clavicle?
Explanation
Question 54
A 24-year-old male weightlifter presents with an aching pain over his right AC joint, exacerbated by dips and bench presses. Cross-body adduction test is positive. Radiographs reveal subchondral cysts and osteopenia of the distal clavicle. Which of the following is the most definitive surgical treatment if 6 months of conservative management fails?
Explanation
Question 55
Reverse total shoulder arthroplasty (RTSA) alters the biomechanics of the shoulder joint to compensate for a deficient rotator cuff. Which of the following best describes the biomechanical changes achieved by RTSA?
Explanation
Question 56
A 21-year-old male undergoes diagnostic arthroscopy for recurrent anterior shoulder instability. The surgeon visualizes an anterior labral tear. The labrum is displaced medially and inferiorly on the glenoid neck, but the anterior scapular periosteum remains intact, forming a sleeve. What is the eponym for this specific lesion?
Explanation
Question 57
A 34-year-old female presents with paresthesias and pain in the medial aspect of her right forearm and hand, particularly with overhead activities. On examination, the Adson test is positive. Plain radiographs show large bilateral cervical ribs. Electromyography reveals decreased conduction velocity in the ulnar nerve distribution. Which of the following anatomical triangles is most commonly implicated in this form of Thoracic Outlet Syndrome?
Explanation
Question 58
In the management of proximal biceps tendon pathology, a surgeon elects to perform an open subpectoral biceps tenodesis instead of an arthroscopic suprapectoral tenodesis. What is the primary theoretical advantage of a subpectoral tenodesis?
Explanation
Question 59
A 70-year-old male with a massive, chronic rotator cuff tear presents with worsening shoulder pain. An AP radiograph reveals an acromiohumeral interval of 3 mm, acetabularization of the acromion, and significant narrowing of the true glenohumeral joint space.
According to the Hamada classification of rotator cuff tear arthropathy, what is the correct grade for these radiographic findings?
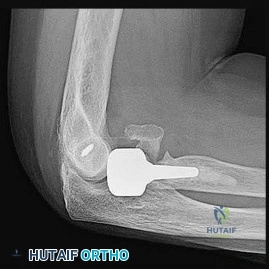
Explanation
Question 60
A 45-year-old female is 6 months post-ORIF for a proximal humerus fracture. She complains of severe shoulder stiffness. Radiographs show a healed fracture with implants in good position, and no intra-articular screw penetration. She has failed conservative management and is scheduled for an arthroscopic capsular release. Which nerve must be most carefully protected when releasing the inferior capsule (closest to the 6 o'clock position)?
Explanation
Question 61
A 25-year-old male sustains a neck injury during a wrestling match. Exam shows drooping of the right shoulder, inability to actively abduct the shoulder above 90 degrees, and the medial border of the scapula is translated laterally. Which of the following physical exam findings is most characteristic of this specific nerve injury?
Explanation
Question 62
A 32-year-old male presents with vague posterior shoulder pain and numbness over the lateral deltoid after a blunt trauma to the posterior shoulder. An MRI reveals isolated atrophy of the teres minor muscle. Entrapment of the neurovascular bundle in the quadrilateral space is suspected. Which of the following structures forms the superior border of this space?
Explanation
Question 63
In reverse total shoulder arthroplasty (RTSA), moving the center of rotation medially and distally compared to the native glenohumeral joint achieves which of the following biomechanical advantages?

Explanation
Question 64
What is the most common radiographic complication specific to the Grammont-style reverse total shoulder arthroplasty, and how is it biomechanically prevented?
Explanation
Question 65
A 28-year-old competitive weightlifter feels a 'pop' in his anterior axilla while performing a heavy bench press. Examination reveals bruising over the anterior chest wall and a palpable defect in the anterior axillary fold. If surgical repair is planned, which portion of the pectoralis major is most commonly ruptured and in what anatomical relationship does it insert?
Explanation
Question 66
A 24-year-old elite volleyball player complains of vague posterior shoulder pain and progressive weakness. On exam, she has full active forward elevation and normal internal rotation, but significant isolated weakness in external rotation. An MRI is obtained. What is the most likely pathological finding and its anatomical location?
Explanation
Question 67
A 21-year-old collegiate baseball pitcher presents with posterior shoulder pain during the late cocking phase of throwing. He has a 25-degree loss of internal rotation compared to his contralateral arm. Pathology in internal impingement syndrome typically involves contact between which two structures?
Explanation
Question 68
In the patient described above with glenohumeral internal rotation deficit (GIRD), what is the primary pathoanatomic cause, and what is the initial recommended treatment?
Explanation
Question 69
A 52-year-old female with type 1 diabetes presents with severe, progressive shoulder stiffness over the last 6 months. She is currently in the 'frozen' phase of adhesive capsulitis. Which of the following anatomical structures is classically the primary site of fibroblastic proliferation and contracture in this condition?
Explanation
Question 70
A 45-year-old female presents to the emergency department with acute, excruciating right shoulder pain of 2 days duration. She has no history of trauma. Radiographs reveal a cloudy, poorly defined, 'toothpaste-like' radiopacity adjacent to the greater tuberosity. Which phase of calcific tendinitis is she most likely experiencing, and what is the underlying pathophysiology of the pain?

Explanation
Question 71
A 13-year-old male baseball pitcher presents with generalized shoulder pain that occurs when throwing. Radiographs demonstrate widening and sclerosis of the proximal humeral physis. What is the most appropriate initial management for this condition?
Explanation
Question 72
A 35-year-old cyclist falls directly onto his shoulder and sustains a distal clavicle fracture. Radiographs show a fracture line medial to the coracoclavicular (CC) ligaments, with the proximal fragment displaced superiorly. The CC ligaments remain attached to the distal fragment. Which Neer classification type is this, and what is the expected nonunion rate if treated non-operatively?
Explanation
Question 73
A 19-year-old rugby player sustains a lateral compression injury to his shoulder. He presents to the ER with shortness of breath, a hoarse voice, and severe pain at the medial end of the clavicle. A CT scan confirms a posterior sternoclavicular joint dislocation. What is the most appropriate next step in management?
Explanation
Question 74
A 65-year-old male with a massive rotator cuff tear undergoes arthroscopic rotator cuff repair. A degenerative, symptomatic long head of the biceps tendon is noted, and the surgeon decides to perform a biceps tenotomy instead of a tenodesis. Compared to tenodesis, which of the following is true regarding biceps tenotomy?
Explanation
Question 75
A 55-year-old laborer complains of deep shoulder pain and clicking. MRI reveals an isolated Type II SLAP lesion. He has failed 6 months of conservative management. Based on recent literature, what is the most reliable surgical intervention for this patient to achieve pain relief and return to work?
Explanation
Question 76
Which of the following radiographic parameters is an accepted indication for operative fixation of an extra-articular scapular body or neck fracture?
Explanation
Question 77
A 40-year-old male presents with acute, unrelenting pain in his right shoulder that awoke him from sleep 2 weeks ago. The pain lasted for 10 days and has now subsided, but he has noticed profound weakness in raising his arm and a developing hollow appearance over his shoulder blade. He had a viral respiratory infection 3 weeks prior. What is the most appropriate diagnostic test to confirm the suspected diagnosis?
Explanation
Question 78
A 28-year-old female complains of a painful grating sensation and audible snapping at the superomedial border of her scapula with active shoulder movement. Radiographs reveal a bony prominence on the superomedial aspect of the anterior scapula. What is the eponymous name for this bony variant?
Explanation
Question 79
A 22-year-old football player sustains a direct blow to the point of his shoulder. Radiographs demonstrate an acromioclavicular (AC) joint injury. The clavicle is displaced posteriorly into or through the trapezius fascia, with normal coracoclavicular distance on the AP view but obvious posterior displacement on the axillary lateral view. Which Rockwood classification type is this?
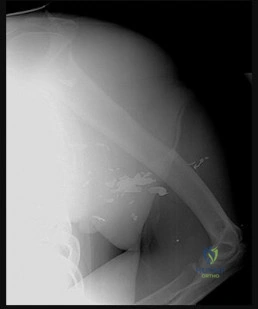
Explanation
Question 80
An isolated fracture of the coracoid process is most commonly treated non-operatively. However, surgical fixation may be indicated in the presence of an associated fracture of the acromion or distal clavicle. This combination disrupts a critical anatomical ring that provides stability to the upper extremity. What is this structural concept called?
Explanation
Question 81
A 42-year-old male presents to the emergency department locked in internal rotation after a severe seizure. Anteroposterior radiographs show a 'lightbulb' appearance of the humeral head. A CT scan reveals a reverse Hill-Sachs lesion involving 35% of the articular surface. Which of the following is the most appropriate surgical management?
Explanation
None
Detailed Chapters & Topics
Dive deeper into specialized chapters regarding orthopedic-mcqs-online-shoulder-and-elbow-017
