Unmasking Axillary Nerve Palsy in Complex Elbow Trauma: A Case of Missed Shoulder Injury
Key Takeaway
Axillary nerve palsy observed in complex elbow dislocation cases is a critical red flag for co-occurring, often missed, shoulder injuries like surgical neck fractures or glenohumeral dislocations. Thorough neurological assessment of deltoid strength and lateral shoulder sensation is paramount to guide targeted imaging and ensure comprehensive, timely treatment.
Patient Presentation and History
A 58-year-old male, employed as a professional carpenter, presented to the Emergency Department following a high-energy fall from a height of approximately 2.5 meters. The mechanism of injury involved a direct axial load onto an outstretched right upper extremity. Based on the patient's account and the resultant injury pattern, the biomechanical vector likely involved a combination of axial loading, supination, and valgus stress applied to a partially flexed elbow, followed by a secondary direct impact to the lateral aspect of the right shoulder as his torso struck the ground.
His initial chief complaint was dominated by severe, intractable pain and gross deformity of the right elbow. He reported generalized right shoulder pain, which he subjectively quantified as secondary in severity to the elbow trauma. This phenomenon of a "distracting injury" is a well-documented pitfall in trauma evaluation, often leading to delayed diagnosis of concurrent ipsilateral pathology.
A comprehensive review of his past medical history revealed essential hypertension and Type 2 Diabetes Mellitus, both well-controlled on oral pharmacological regimens (Hemoglobin A1c of 6.8% recorded three months prior). Optimization of his glycemic control is a critical factor in mitigating postoperative surgical site infection and ensuring adequate osseous union. He is a non-smoker and reports occasional ethanol consumption. He has no known drug allergies. Crucially, the patient denied any pre-existing cervical radiculopathy, peripheral neuropathy, or baseline motor/sensory deficits in the bilateral upper extremities. Given his occupation, baseline functional demand on the right upper extremity was exceptionally high, requiring repetitive overhead activity, heavy lifting, and precise pronation/supination arcs under load.
Initial assessment in the trauma bay demonstrated a hemodynamically stable patient with a Glasgow Coma Scale of 15. Emergency Medical Services had applied a provisional long-arm splint to the right upper extremity. The primary and secondary surveys of the Advanced Trauma Life Support protocol revealed no occult thoracic, abdominal, or pelvic injuries. The initial orthopedic evaluation was heavily biased toward the overt elbow deformity, with a cursory examination of the shoulder noting diffuse tenderness but lacking gross architectural distortion. The acute pain crisis precluded a highly granular neurological assessment during the initial triage phase, necessitating a more rigorous secondary evaluation following appropriate analgesia.
Clinical Examination Findings
Following initial resuscitation, administration of intravenous multimodal analgesia, and removal of the provisional splint, a systematic and detailed examination of the right upper extremity was executed.
Inspection of the Upper Extremity
Evaluation of the elbow revealed gross posterolateral deformity, consistent with a major joint dislocation. Significant soft tissue swelling was present, obliterating the normal anatomical landmarks of the olecranon, medial epicondyle, and lateral epicondyle. Ecchymosis was evolving, extending distally into the proximal forearm and proximally into the distal brachium. The soft tissue envelope, while compromised by profound edema (Tscherne Grade II closed soft tissue injury), remained intact with no evidence of open traumatic wounds.
Inspection of the shoulder girdle revealed moderate, diffuse swelling over the deltoid region and lateral proximal humerus. There was no obvious step-off at the acromioclavicular joint and no gross anterior fullness suggestive of an unreduced anterior glenohumeral dislocation. However, critical observation revealed a subtle but distinct flattening of the lateral deltoid contour compared to the contralateral uninjured shoulder, raising immediate suspicion for either a spontaneously reduced dislocation or significant underlying skeletal/neurological pathology.
Palpation and Osseous Landmarks
Palpation of the elbow elicited exquisite point tenderness over the radial head and the lateral collateral ligament complex origin at the lateral epicondyle. Tenderness was also noted over the medial epicondyle and the anterior joint capsule. Palpable crepitus was evident with any inadvertent micro-motion of the joint, highly suggestive of intra-articular osseous fragmentation.
Palpation of the shoulder demonstrated diffuse, severe tenderness over the greater tuberosity and the surgical neck of the humerus. Deep palpation along the bicipital groove and the anterior joint line was poorly tolerated. No gross crepitus was elicited during gentle palpation of the shoulder, though muscle guarding was significant.
Range of Motion Assessment
Elbow range of motion was severely restricted and mechanically blocked. The passive flexion-extension arc was estimated at a mere 30 to 70 degrees. Any attempt to extend the elbow beyond 30 degrees resulted in a palpable and visible subluxation event, indicating profound posterolateral rotatory instability. Forearm pronation and supination were completely restricted by pain and mechanical impingement, likely secondary to a radial head fracture.
Shoulder range of motion was similarly compromised. Active abduction was limited to approximately 30 degrees and was achieved almost entirely through compensatory scapulothoracic substitution rather than true glenohumeral articulation. Active forward elevation and external rotation were severely diminished. Passive range of motion was limited by pain, preventing accurate assessment of capsular compliance.
Neurological and Vascular Assessment
A meticulous neurological examination was the critical diagnostic maneuver that unmasked the full extent of the patient's injury complex. Given the high-energy axial load, a thorough evaluation of the brachial plexus and peripheral nerves was mandatory.
- Median Nerve: Sensory distribution intact over the volar aspect of the thumb, index, middle, and radial half of the ring finger. Motor function intact for thumb opposition (abductor pollicis brevis) and flexion of the distal phalanx of the index finger (flexor digitorum profundus).
- Ulnar Nerve: Sensory distribution intact over the little finger and ulnar half of the ring finger. Motor function intact for finger abduction (dorsal interossei) and adduction (palmar interossei).
- Radial Nerve: Sensory distribution intact over the dorsal first web space. Motor function intact for wrist extension (extensor carpi radialis longus/brevis) and thumb extension (extensor pollicis longus).
- Musculocutaneous Nerve: Sensory distribution intact over the lateral antebrachial cutaneous nerve territory. Motor function intact for biceps brachii contraction.
- Axillary Nerve: This assessment revealed profound deficits.
- Motor: Markedly diminished active contraction of the deltoid muscle. The patient was unable to actively abduct the arm against gravity past 30 degrees (Medical Research Council Grade 2/5). Palpation of the anterior, middle, and posterior heads of the deltoid during attempted abduction revealed minimal to no fibrillations. Teres minor function, assessed via resisted external rotation with the arm adducted to the side, was also significantly weakened (MRC Grade 2/5).
- Sensory: Distinct anesthesia and hypoesthesia were mapped over the lateral aspect of the shoulder, precisely corresponding to the superior lateral brachial cutaneous nerve distribution (the classic "regimental badge" area).
Vascular assessment demonstrated palpable and symmetric radial and ulnar pulses. Capillary refill was brisk (less than 2 seconds) in all digits. The compartments of the forearm and arm were soft and compressible, with no clinical indicators of impending acute compartment syndrome.
Imaging and Diagnostics
Standard trauma radiographic series were obtained for both the right elbow and the right shoulder to delineate the osseous architecture and guide definitive surgical planning.
Radiographic Evaluation of the Elbow
Initial anteroposterior and lateral radiographs of the right elbow confirmed a complex fracture-dislocation. The ulna was dislocated posteriorly relative to the distal humerus. A displaced, comminuted fracture of the radial head was evident, alongside a visible fracture fragment anterior to the distal humerus, consistent with a coronoid process fracture. This constellation of findings is pathognomonic for the "Terrible Triad" of the elbow.
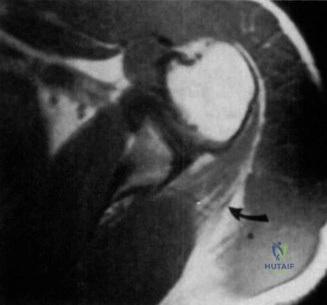
To further characterize the fracture morphology, a non-contrast Computed Tomography scan of the elbow with 3D reconstructions was obtained. The CT scan provided critical details:
* Radial Head: A Mason Type III comminuted fracture involving the entire articular surface, with significant displacement and intra-articular step-off rendering it unamenable to stable internal fixation.
* Coronoid Process: A Regan-Morrey Type II (O'Driscoll Anteromedial Facet Subtype 1) fracture involving approximately 30% of the coronoid height. The fragment was displaced proximally and anteriorly, attached to the anterior capsule.
* Distal Humerus: No evidence of capitellar or trochlear shear fractures.
Radiographic Evaluation of the Shoulder
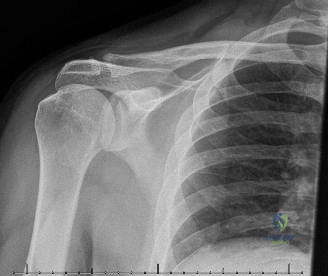
Given the clinical findings of axillary nerve palsy and lateral shoulder contour flattening, a complete trauma series of the shoulder (True AP, Scapular Y, and Axillary lateral views) was mandatory.

The radiographs revealed a displaced, two-part proximal humerus fracture involving the surgical neck (Neer Classification). The humeral shaft was medially translated and apex anteriorly angulated relative to the humeral head. The greater and lesser tuberosities appeared intact on initial plain films. There was no evidence of glenohumeral dislocation on the axillary view, suggesting that the axillary nerve palsy was likely secondary to a traction neurapraxia at the moment of impact, or direct impingement/stretch across the sharp medial osseous spike of the displaced humeral shaft fracture.
A dedicated CT scan of the proximal humerus was also acquired for preoperative templating. This confirmed the Neer two-part surgical neck fracture and ruled out occult tuberosity extensions or articular head splitting components. The medial calcar region demonstrated significant comminution, indicating inherent medial instability that would dictate the choice of fixation construct.
Advanced Neurodiagnostic Considerations
While Electromyography and Nerve Conduction Studies are highly sensitive for evaluating peripheral nerve injuries, they are generally not indicated in the acute trauma setting (less than 3 weeks post-injury) due to the delayed onset of Wallerian degeneration and denervation potentials (fibrillations and positive sharp waves). The diagnosis of axillary nerve palsy in this acute phase was entirely clinical. Baseline EMG/NCS may be considered at 4 to 6 weeks post-injury if there is no clinical evidence of spontaneous neurological recovery.
Differential Diagnosis
The presentation of concomitant severe elbow trauma and shoulder dysfunction with neurological deficits requires a broad differential to ensure no subtle pathology is overlooked. The primary diagnostic challenge lies in differentiating the etiology of the axillary nerve palsy and understanding the exact pattern of the multi-level upper extremity trauma.
| Differential Diagnosis | Clinical Presentation Characteristics | Radiographic/Imaging Findings | Rationale for Inclusion or Exclusion |
|---|---|---|---|
| Terrible Triad of Elbow + Proximal Humerus Fracture with Axillary Neuropathy | Severe elbow pain, instability, blocked ROM. Flattened shoulder contour, "regimental badge" anesthesia, profound deltoid weakness. | Elbow: Posterior dislocation, radial head comminution, coronoid fracture. Shoulder: Displaced surgical neck fracture. | Primary Diagnosis. Perfectly aligns with the mechanism of injury, physical exam findings (specifically the isolated axillary nerve deficit), and all advanced imaging modalities. |
| Transolecranon Fracture-Dislocation + Anterior Shoulder Dislocation (Spontaneously Reduced) | Massive elbow swelling, palpable defect over olecranon. Shoulder pain, apprehension, potential axillary nerve palsy. | Elbow: Comminuted olecranon fracture with anterior dislocation of radius/ulna. Shoulder: Hill-Sachs lesion, bony Bankart. | Excluded. Radiographs show posterior elbow dislocation with radial head/coronoid involvement, not a transolecranon variant. No Hill-Sachs or Bankart lesions seen on shoulder CT to suggest a reduced dislocation. |
| Monteggia Variant + Brachial Plexus Injury (Posterior Cord) | Proximal forearm deformity, radial head palpable anteriorly/laterally. Widespread weakness in radial and axillary nerve distributions. | Elbow/Forearm: Proximal ulnar shaft fracture with radial head dislocation. Shoulder: Normal osseous anatomy. | Excluded. Ulnar shaft is intact. Radial nerve function (wrist/finger extension) is completely normal, ruling out a higher posterior cord brachial plexus lesion. The nerve injury is isolated to the axillary branch. |
Surgical Decision Making and Classification
The management of this complex, multi-level upper extremity injury necessitates operative intervention. Non-operative management is absolutely contraindicated given the profound instability of the elbow (Terrible Triad) and the significantly displaced, unstable nature of the proximal humerus fracture, particularly in a high-demand 58-year-old carpenter.
Classification Systems Guiding Treatment
- Elbow - Radial Head (Mason Classification): Type III (comminuted, displaced, mechanically blocking motion). Given the severe comminution involving the entire head and neck junction, attempted Open Reduction and Internal Fixation is associated with high rates of failure, non-union, and early post-traumatic arthrosis. Radial head arthroplasty is the gold standard for this specific morphology in the setting of a terrible triad to restore the lateral column strut.
- Elbow - Coronoid (Regan-Morrey / O'Driscoll): Regan-Morrey Type II / O'Driscoll Anteromedial Facet. The coronoid is the primary stabilizer against posterior subluxation. Even small fragments in a terrible triad must be stabilized. The fragment is attached to the anterior capsule; thus, capsuloligamentous repair via a lasso technique or direct screw fixation is mandated to restore anterior stability.
- Shoulder - Proximal Humerus (Neer Classification): Two-part surgical neck fracture. The medial calcar comminution represents a loss of the medial hinge. Non-operative treatment would likely result in progressive varus collapse, malunion, and severe functional limitation.
- Nerve Injury (Seddon Classification): The axillary nerve palsy is clinically presumed to be a neurapraxia or, at worst, axonotmesis, secondary to traction or contusion during the initial trauma and subsequent fracture displacement. Neurotmesis (complete transection) is exceedingly rare with closed proximal humerus fractures unless associated with a massive, high-energy penetrating injury. The strategy is to carefully protect the nerve during surgery, reduce the fracture to remove ongoing tension, and observe for spontaneous recovery.
Staging and Sequence of Fixation
A critical preoperative decision involves the sequence of surgical fixation. Addressing two major, unstable joints in the same extremity requires careful logistical planning.
The consensus in this scenario is to stabilize the proximal humerus first.
* Rationale: Securing the proximal humerus establishes a stable proximal lever arm. If the elbow is addressed first, the manipulation required to reduce and fix the elbow, assess its stability through a full arc of motion, and apply stress testing could exacerbate the displacement of the proximal humerus fracture, potentially causing further iatrogenic injury to the already compromised axillary nerve. Furthermore, a stable shoulder allows for easier positioning and manipulation of the arm during the subsequent elbow reconstruction.
Surgical Technique and Intervention
The patient was brought to the operating room and placed under general endotracheal anesthesia. A supplementary interscalene regional nerve block was avoided to allow for immediate postoperative neurological assessment of the axillary nerve and to monitor for any evolving compartment syndrome, though a supraclavicular block could be considered for postoperative analgesia once baseline function is documented.
Patient Positioning
The patient was positioned in a modified beach chair position (approximately 45 degrees of elevation) on a radiolucent operating table. This position allows excellent access to the anterior shoulder for the deltopectoral approach and permits the arm to be draped free, enabling unrestricted access to the elbow for the subsequent lateral and medial approaches. A sterile tourniquet was placed high on the brachium but not inflated during the shoulder phase.
Phase 1: Proximal Humerus Open Reduction and Internal Fixation
- Approach: A standard deltopectoral approach was utilized. The skin incision was made from the tip of the coracoid process extending distally along the deltopectoral groove.
- Dissection: The cephalic vein was identified and retracted laterally with the deltoid to preserve its primary venous drainage. The clavipectoral fascia was incised. The conjoined tendon was identified and retracted medially.
- Nerve Protection: Deep dissection proceeded with extreme caution. The axillary nerve was palpated and visually identified at the inferior border of the subscapularis as it entered the quadrangular space. It appeared contiguous but hyperemic, consistent with a traction injury. No transection was observed. The nerve was carefully protected throughout the procedure.
- Fracture Reduction: The fracture site was exposed. The hematoma was evacuated. The biceps tendon was identified and utilized as a landmark for rotation. Traction, abduction, and gentle manipulation were used to reduce the apex-anterior and medially translated shaft to the humeral head.
- Fixation: A Proximal Humerus Interlocking System (PHILOS) plate was selected. Given the medial calcar comminution, ensuring adequate medial support was paramount. The plate was positioned lateral to the bicipital groove and distal to the greater tuberosity to avoid subacromial impingement. Multiple locking screws were placed into the humeral head, including critical calcar screws directed inferomedially to support the medial hinge and prevent varus collapse. Cortical screws were utilized in the distal shaft.
- Closure: Fluoroscopy confirmed anatomical reduction and extra-articular screw placement. The deltopectoral interval was copiously irrigated and closed in layers over a closed suction drain.
Phase 2: Elbow Terrible Triad Reconstruction
Following shoulder stabilization, the arm was brought across the chest for the elbow reconstruction. The sterile tourniquet was inflated to 250 mmHg.
- Lateral Approach (Kocher): An incision was made from the lateral epicondyle extending distally towards the ulnar crest. The interval between the anconeus and extensor carpi ulnaris was developed.
- Radial Head Excision and Arthroplasty: The lateral collateral ligament complex was found to be completely avulsed from its humeral origin. The highly comminuted radial head fragments were meticulously excised, ensuring no intra-articular debris remained. The radial neck was prepared with a planar. A modular radial head prosthesis was trialed. Sizing was critical to avoid overstuffing the radiocapitellar joint, which can lead to capitellar wear and restricted motion. The definitive uncemented radial head stem and articular head were impacted into place.
- Coronoid Fixation: Through the lateral exposure, the anterior capsule and the attached coronoid fragment were visualized. Given the fragment size (Type II), a "lasso" suture technique was employed. Heavy non-absorbable sutures (#2 FiberWire) were passed through the anterior capsule and around the coronoid fragment. Two drill holes were made from the posterior aspect of the proximal ulna exiting at the base of the coronoid fracture bed. The sutures were passed through these tunnels and tied over the posterior ulnar cortex, securely reducing the coronoid fragment and tensioning the anterior capsule.
- Lateral Ulnar Collateral Ligament (LUCL) Repair: The avulsed LUCL was identified. The isometric point on the lateral epicondyle was cleared of soft tissue. Two suture anchors loaded with high-strength suture were placed into the lateral epicondyle. The sutures were passed through the LUCL utilizing a Krackow locking stitch.
- Joint Assessment: The elbow was reduced. The LUCL sutures were tied with the elbow in 90 degrees of flexion and full pronation to appropriately tension the lateral structures.
- Stability Testing: Intraoperative fluoroscopy and clinical examination demonstrated a concentric reduction. The elbow was stable through a full arc of flexion and extension, and in both pronation and supination. No medial approach was deemed necessary as the lateral and anterior reconstructions restored profound stability.
- Closure: The lateral wound was irrigated and closed in layers. A well-padded posterior splint was applied with the elbow at 90 degrees of flexion and neutral rotation.
Post Operative Protocol and Rehabilitation
The postoperative rehabilitation for a combined proximal humerus fracture and a terrible triad of the elbow is highly complex, requiring a delicate balance between protecting the osseous/ligamentous repairs and preventing devastating joint stiffness. The presence of an axillary nerve palsy further complicates the protocol.
Phase I: Maximum Protection (Weeks 0-2)
- Immobilization: The patient is maintained in a posterior elbow splint at 90 degrees of flexion and neutral rotation for the first 7-10 days to allow the soft tissue envelope to calm and the LUCL repair to begin initial healing. The shoulder is supported in a standard sling.
- Shoulder: Pendulum exercises are initiated immediately to prevent adhesive capsulitis. Passive forward elevation and external rotation are strictly limited to 90 degrees and 30 degrees, respectively, to protect the tuberosities and the plate construct. Active abduction is contraindicated, not only due to the fracture but also due to the axillary nerve palsy.
- Elbow: At 7-10 days, the splint is transitioned to a hinged elbow orthosis. Active-assisted range of motion is initiated. Crucially, extension is performed with the forearm in pronation to impart inherent stability to the lateral side and protect the LUCL repair. Supination is allowed only in flexion.
- Neurological: Baseline assessment of the axillary nerve is documented. Galvanic electrical stimulation of the deltoid may be considered to maintain muscle bulk during the denervation phase, though clinical evidence for its efficacy is mixed.
Phase II: Moderate Protection and Active Motion (Weeks 2-6)
- Shoulder: Progression to active-assisted range of motion (pulley systems, wand exercises). If the axillary nerve shows signs of recovery (flicker of contraction), gravity-eliminated active motion is initiated.
- Elbow: The hinged brace is gradually opened to allow full extension. Active and active-assisted motion in all planes is encouraged. The brace is typically discontinued around 6 weeks post-operatively.
- Diagnostics: If there is absolutely no clinical evidence of axillary nerve recovery (motor or sensory) by 6 weeks, a baseline Electromyography and Nerve Conduction Study (EMG/NCS) is ordered to quantify the extent of denervation and establish a baseline for future comparison.
Phase III: Strengthening and Functional Restoration (Weeks 6-12)
- Radiographic Review: AP and Lateral radiographs of the shoulder and elbow are obtained at 6 weeks to confirm maintenance of reduction, hardware integrity, and progressive osseous union.
- Shoulder: Isotonic strengthening of the rotator cuff and periscapular stabilizers begins. Deltoid strengthening is incorporated dependent on the status of the axillary nerve.
- Elbow: Progressive strengthening of the biceps, triceps, and forearm musculature. Dynamic splinting (e.g., Turnbuckle splint) may be prescribed if significant flexion or extension contractures are present.
Phase IV: Advanced Strengthening and Return to Work (Months 3-6+)
- The focus shifts to work-hardening programs specifically tailored to the patient's occupation as a carpenter. This includes sustained overhead activity, heavy lifting protocols, and repetitive pronation/supination tasks under resistance.
- If the axillary nerve palsy fails to demonstrate clinical or electromyographic recovery by 3 to 6 months, referral to a peripheral nerve specialist for consideration of nerve exploration, neurolysis, or nerve transfer (e.g., triceps branch to axillary nerve) is mandated.
Clinical Pearls and Pitfalls
- The Pitfall of the Distracting Injury: Severe, visually obvious trauma (like a dislocated elbow) will frequently mask proximal or distal injuries. The trauma mantra "examine the joint above and the joint below" is non-negotiable. A missed proximal humerus fracture or shoulder dislocation in the setting of an elbow injury can lead to catastrophic functional outcomes.
- Anatomy of the Axillary Nerve: The axillary nerve is highly vulnerable as it traverses the quadrangular space and wraps around the surgical neck of the humerus. Any fracture in this region, particularly with medial translation of the shaft, places the nerve at high risk for traction, contusion, or tethering.
- Neurological Examination Nuances: The "regimental badge" sign is highly specific for axillary nerve sensory branch involvement. When assessing deltoid motor function in the acute setting, rely on palpation of the muscle belly during attempted contraction rather than gross limb movement, as scapulothoracic substitution can mimic glenohumeral abduction.
- Surgical Sequencing: In ipsilateral multi-joint trauma, stabilize the most proximal or the most unstable segment first. Establishing a stable proximal humerus provides a foundation for the complex manipulation required during a terrible triad reconstruction.
- Coronoid Management in the Terrible Triad: The coronoid is the keystone of elbow stability. Never ignore a coronoid fracture in the setting of a dislocated elbow and radial head fracture. Even small capsular avulsions (Type I/II) must be secured via suture lasso or anchors to restore the anterior buttress and prevent recurrent posterior rotatory subluxation.
- Radial Head Arthroplasty Sizing: Overstuffing the radiocapitellar joint with a prosthesis that is too large or inserted too proximally will lead to capitellar wear, lateral elbow pain, and severe restriction in flexion and extension. The articular surface of the implant should sit flush with or slightly proximal to the lateral edge of the lesser sigmoid notch of the ulna.
