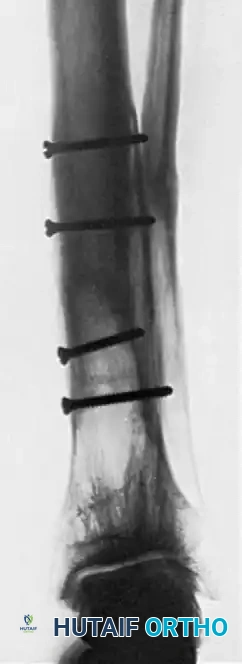
Comprehensive Introduction and Patho-Epidemiology
The management of recalcitrant nonunions, particularly those complicated by severe biological compromise or catastrophic mechanical instability, remains one of the most formidable challenges in the field of reconstructive orthopedic surgery. Among these, congenital pseudarthrosis of the tibia (CPT) and osteoporotic periarticular nonunions present unique patho-epidemiological profiles that frequently defy standard osteosynthesis techniques. In 1941, recognizing the inherent biological and mechanical deficiencies that doomed conventional plating and grafting methods, H.B. Boyd devised the dual onlay graft operation. This ingenious surgical strategy was born out of necessity, designed to address the hamartomatous periosteum and dysplastic bone characteristic of CPT, which inherently lacks both the osteogenic potential and the structural integrity required for normal fracture consolidation.
The pathophysiology of these complex nonunions dictates the necessity of the dual onlay technique. In CPT, frequently associated with neurofibromatosis type 1 (NF1), the local environment is characterized by a thick, fibrous, hamartomatous tissue that effectively strangles the local vascular supply and actively inhibits osteogenesis. Similarly, in the geriatric population, osteoporotic nonunions—particularly those in the metaphyseal-diaphyseal junction—are defined by cortices that are paper-thin and structurally incompetent. In these atrophic or oligotrophic environments, standard metallic implants such as locked plates or intramedullary nails often fail to achieve adequate purchase, leading to screw pull-out, implant failure, and persistence of the nonunion. The dual onlay graft bypasses these local deficiencies by importing massive structural autograft or allograft that serves simultaneously as a rigid biological plate and an osteoconductive scaffold.
While the advent of modern locked plating technology, advanced intramedullary nailing systems, and circular external fixation (such as the Ilizarov method and the Taylor Spatial Frame) has undeniably reduced the frequency of this procedure, the dual onlay graft remains an indispensable salvage technique in the armamentarium of the reconstructive orthopedic surgeon. Contemporary epidemiology indicates a rising incidence of complex, multi-operated nonunions, often accompanied by significant bone loss and compromised soft tissue envelopes. In these tertiary referral scenarios, where the biological reservoir of the host bone has been exhausted by multiple prior surgical interventions, the dual onlay graft provides a definitive, albeit technically demanding, solution.
Furthermore, the dual onlay technique is not merely of historical interest but represents a foundational concept in orthopedic biomechanics and biological osteosynthesis. By utilizing two cortical onlay grafts placed diametrically opposite each other on the host bone, bridging the nonunion site, the construct grips the host bone fragments like a vise. Any intervening space at the bone ends is meticulously packed with cancellous bone chips to provide immediate osteogenic and osteoconductive properties. Understanding the patho-epidemiology of these recalcitrant nonunions is critical for the modern surgeon to recognize when standard modalities have reached their limits and when the massive structural and biological augmentation of the dual onlay graft is decisively indicated.
Detailed Surgical Anatomy and Biomechanics
A profound understanding of both the surgical anatomy of the donor and recipient sites, as well as the intricate biomechanics of the dual onlay construct, is paramount for the successful execution of this procedure. Anatomically, the donor site is most frequently the anterior medial aspect of the contralateral tibial diaphysis. This region provides a massive, thick cortical strut that can be harvested with relative safety, provided the surgeon meticulously avoids creating stress risers at the corners of the osteotomy. The blood supply to the diaphyseal cortex is primarily endosteal (centrifugal flow); however, once harvested as a free, non-vascularized autograft, the strut relies entirely on the surrounding soft tissue envelope of the recipient site for revascularization and eventual incorporation.
The recipient site anatomy, whether it be the tibia, femur, or humerus, is inevitably distorted by previous trauma, prior surgical incisions, and the pathological process of the nonunion itself. The surgeon must carefully navigate altered fascial planes and neurovascular bundles that may be encased in dense scar tissue. The critical anatomical consideration at the recipient site is the preservation of the periosteal blood supply to the remaining viable host bone fragments, while simultaneously identifying and excising the avascular, sclerotic bone ends back to bleeding, healthy tissue—the so-called "paprika sign." The soft tissue envelope must be thoroughly evaluated, as the addition of two bulky cortical struts will significantly increase the cross-sectional volume of the limb, potentially compromising skin closure and placing underlying neurovascular structures at risk of compression.
Biomechanically, the superiority of the dual onlay graft lies in its unparalleled vise-like compression and its exceptional load-sharing capabilities. When screws are inserted through the first cortical graft, through the osteoporotic host bone, and into the second cortical graft, the host bone is subjected to massive compressive forces. The dense cortical grafts act as massive, rigid washers, effectively preventing the screw heads and threads from pulling through the mechanically incompetent host bone. This compression not only stabilizes the nonunion site but also minimizes micromotion, creating a favorable mechanical environment for osteogenesis.
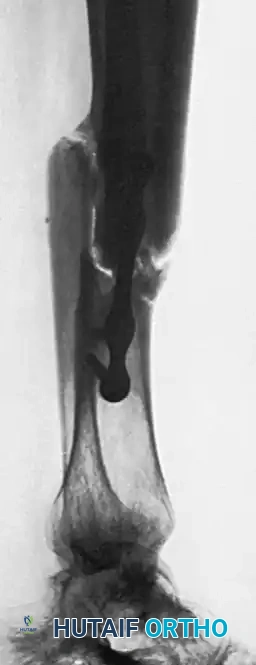
Furthermore, the placement of two cortical struts on opposite sides of the mechanical axis significantly increases the area moment of inertia of the construct. According to biomechanical principles, the resistance to bending forces is proportional to the distance of the implant from the neutral axis. By placing the rigid cortical grafts at the extreme periphery of the host bone, the construct provides exceptional resistance to both bending and torsional forces. The construct effectively bypasses the mechanically incompetent nonunion site, transferring physiological loads through the rigid cortical grafts until creeping substitution and bony consolidation occur. This load-sharing phenomenon is critical; unlike rigid metallic plates that can cause stress shielding, the biological nature of the grafts ensures that as they incorporate and remodel according to Wolff's Law, physiological stresses are gradually transferred back to the healing host bone.
Exhaustive Indications and Contraindications
The decision to proceed with a dual onlay graft must be based on a rigorous evaluation of the patient's biological capacity, the mechanical demands of the affected extremity, and the failure of prior interventions. This is a massive, physiologically demanding procedure that is reserved for specific, highly complex clinical scenarios where standard osteosynthesis is doomed to fail.
Primary Indications
Historically, the primary indication for the dual onlay graft has been congenital pseudarthrosis of the tibia (CPT). In CPT, the local biological environment is profoundly dysplastic, and the bone lacks the intrinsic capacity to heal. The dual onlay graft provides massive structural support and introduces healthy, biologically active bone to a biologically inert and mechanically unstable segment. While modern approaches often utilize the Ilizarov method or vascularized fibular grafts for CPT, the dual onlay technique remains a highly effective option, particularly in cases where microsurgical expertise is unavailable or where previous vascularized grafts have failed.

A second major indication is the treatment of osteoporotic nonunions in the elderly, particularly those involving the shafts of long bones where the host cortex is paper-thin. In these scenarios, standard cortical or cancellous screws will inevitably strip and fail to achieve purchase in the osteoporotic fragments. However, by utilizing the dual onlay technique, the screws achieve excellent, rigid purchase in the dense cortical bone of the dual autografts or allografts, effectively sandwiching and compressing the weak host bone between them. This is especially valuable in short juxta-articular nonunions where a short metaphyseal fragment is difficult to control with standard intramedullary or extramedullary devices.
Absolute and Relative Contraindications
The absolute contraindications to the dual onlay graft are primarily biological. The presence of active, deep infection at the nonunion site is an absolute contraindication. Placing massive, avascular cortical grafts into an infected bed is a recipe for catastrophic failure, inevitably leading to graft sequestration, chronic osteomyelitis, and potential limb loss. Any suspicion of infection must be rigorously evaluated with preoperative inflammatory markers, advanced imaging, and intraoperative tissue cultures. If infection is confirmed, a staged approach involving radical debridement, antibiotic spacer placement, and subsequent reconstruction is mandatory.
Severe soft tissue compromise represents another critical contraindication. Two bulky cortical grafts materially crowd the soft tissues. If the soft tissue envelope is heavily scarred, irradiated, or otherwise inadequate to achieve a tension-free closure over the massive construct, the procedure is contraindicated unless it is combined with a vascularized soft tissue flap (e.g., a free latissimus dorsi or anterolateral thigh flap). Inadequate host bone stock for graft harvest is a relative contraindication; if the patient's contralateral tibia is osteoporotic or previously traumatized, massive structural allografts may be utilized, though they lack the osteogenic potential and favorable incorporation profile of fresh autografts.
Summary Table of Indications and Contraindications
| Category | Specific Clinical Scenario | Rationale / Surgical Consideration |
|---|---|---|
| Primary Indication | Congenital Pseudarthrosis of the Tibia (CPT) | Provides massive mechanical bridging and biological stimulation to a dysplastic, hamartomatous environment. |
| Primary Indication | Osteoporotic Diaphyseal Nonunions | Bypasses weak host bone; screws achieve rigid purchase in the dense cortical grafts rather than the paper-thin host cortices. |
| Primary Indication | Short Juxta-Articular Nonunions | Grasps the short, osteoporotic metaphyseal fragment securely between the grafts, allowing for stable compression. |
| Absolute Contraindication | Active Deep Osteomyelitis | Avascular cortical struts will act as a massive sequestrum, perpetuating infection and leading to catastrophic failure. |
| Absolute Contraindication | Inadequate Soft Tissue Envelope | Bulky grafts will cause excessive skin tension, leading to wound breakdown, graft exposure, and subsequent infection. |
| Relative Contraindication | Poor Donor Bone Stock | Inability to harvest robust autograft (e.g., severe systemic osteoporosis); necessitates the use of structural allograft. |
Pre-Operative Planning, Templating, and Patient Positioning
Meticulous, exhaustive preoperative planning is the cornerstone of success in the dual onlay graft technique. The surgeon must approach this procedure with a definitive, step-by-step blueprint, as intraoperative improvisation in the face of massive structural grafting and compromised soft tissues frequently leads to disastrous outcomes.
Imaging and Digital Templating
The initial phase of planning requires comprehensive imaging. Standard orthogonal radiographs of the entire affected bone, including the joints above and below, are mandatory to assess the overall mechanical axis, limb length discrepancy, and the macroscopic architecture of the nonunion. However, radiographs alone are insufficient. A fine-cut Computed Tomography (CT) scan with metal artifact reduction software (if retained hardware is present) is critical. The CT scan allows the surgeon to accurately assess the volume of bone loss, the geometry of the host fragments, and the true density of the remaining cortical bone.
Digital templating is then utilized to calculate the exact required dimensions of the cortical grafts. The grafts must be long enough to span the nonunion site and allow for the insertion of at least two, and preferably three or four, fully threaded screws into the healthy host bone both proximal and distal to the defect. The width of the graft must be sufficient to accommodate the chosen screw diameter (typically 3.5mm or 4.5mm) without risking iatrogenic splitting of the strut during drilling and tapping. Furthermore, the surgeon must calculate the required volume of cancellous bone graft needed to pack the intervening defect, ensuring adequate biological stimulation.
Soft Tissue Assessment and Logistics
A rigorous clinical assessment of the soft tissue envelope is non-negotiable. The surgeon must evaluate the pliability of the skin, the presence of previous surgical scars, and the overall vascularity of the limb. The addition of two massive cortical struts will significantly increase the cross-sectional area of the extremity. The surgeon must anticipate whether primary closure will be possible or if prophylactic fasciotomies, local rotational flaps, or free tissue transfer will be required. Consultation with a plastic and reconstructive surgeon is highly recommended in cases of severe soft tissue compromise.
Logistically, the dual onlay graft is best performed using a two-team approach to minimize tourniquet time, reduce overall operative duration, and mitigate the physiological insult to the patient. One highly experienced surgical team is dedicated to the exposure, debridement, and preparation of the recipient site, while a second team simultaneously harvests and prepares the massive cortical strut and cancellous bone from the donor site.
Patient Positioning
Patient positioning must facilitate simultaneous access to both the donor and recipient sites. The patient is typically positioned supine on a radiolucent operating table. If the contralateral tibia is chosen as the donor site, a bump is placed under the ipsilateral hip to internally rotate the donor leg, bringing the anterior medial face of the tibia into a prime surgical position. Sterile tourniquets are applied to both extremities. The entire lower half of the patient, from the umbilicus to the toes bilaterally, is prepped and draped into the sterile field to allow for unrestricted manipulation of the limbs and the use of intraoperative fluoroscopy.
Step-by-Step Surgical Approach and Fixation Technique
The execution of the dual onlay graft is technically demanding, requiring precise carpentry and meticulous handling of both the host bone and the massive structural grafts. The procedure must follow a rigorous, sequential protocol to ensure biomechanical stability and biological viability.
Exposure and Radical Debridement
The recipient site is exposed through an extensile approach that respects the local angiosomes and incorporates previous surgical incisions where possible. Once the nonunion is identified, a radical, aggressive debridement is mandatory. The surgeon must excise all intervening fibrous tissue, necrotic cartilage, and avascular, sclerotic bone. The debridement continues until healthy, bleeding cortical and cancellous bone is encountered—the definitive "paprika sign."
Following the resection of the nonunion, the medullary canals of both the proximal and distal host fragments must be opened and reamed using drill bits, curettes, or flexible reamers. This step is critical to restore endosteal blood flow and to allow for the ingress of osteoprogenitor cells and vascular buds into the nonunion site.
Preparation of the Host Bed
The preparation of the host bed dictates the mechanical stability of the final construct. Using a sharp, broad osteotome or an oscillating saw under continuous saline irrigation, the surgeon prepares flat beds for the grafts on two diametrically opposite sides of the host fragments.

It is a critical technical point that the surgeon must not countersink the beds deeply or expose the medullary canal excessively during this step. Removing too much host bone will further weaken the already compromised fragments. The goal is to remove just enough cortical convexity to create a perfectly flat, planar surface. This allows the rigid, unyielding cortical grafts to be applied absolutely flush against the host bone without bending, rocking, or leaving gaps that would compromise the vise-like compression.
Graft Harvesting and Preparation
While the primary surgeon prepares the recipient bed, the secondary team harvests the graft. The anterior medial face of the donor tibia is exposed subperiosteally. Using an oscillating saw, a massive, full-thickness cortical graft is harvested. To prevent catastrophic donor site fracture, the corners of the harvest site must be pre-drilled to create rounded edges, eliminating stress risers. Copious amounts of cancellous bone are simultaneously harvested from the proximal tibial metaphysis (Gerdy's tubercle).
Once the massive cortical strut is transferred to the back table, it is meticulously prepared. Using a fine oscillating saw, the cancellous surface of the deep aspect of the graft is carefully removed and preserved. The cortical graft is then divided transversely (if harvested with sufficient length) or split longitudinally to form two identical, robust cortical struts.
Application and Provisional Fixation
The two prepared cortical grafts are placed on the opposite, flattened sides of the host fragments, bridging the nonunion defect. The entire construct—Graft 1, Host Bone, Graft 2—is compressed together using large, self-retaining bone-holding forceps, such as Verbrugge or Lewin clamps.

At this stage, the surgeon must utilize intraoperative fluoroscopy to verify the mechanical axis, rotation, and overall limb length. Minor adjustments are made by manipulating the clamps. The grafts must overlap the healthy host bone sufficiently to allow for multi-cortical screw fixation.
Definitive Fixation: The Alternating Screw Technique
Fixing two unyielding cortical grafts to a mobile, multi-fragmentary nonunion requires a highly specific, sequential technique to maintain compression and alignment. The grafts are fixed using the alternating screw technique:
- Provisional Short Screws: The surgeon drills and taps through the first graft and only the near cortex of the host bone. Short, temporary cortical screws are inserted to fix this first graft to both the proximal and distal host fragments. This stabilizes the first graft and the host bone as a single, unified block.
- Definitive Long Screws: Attention is turned to the second graft. The surgeon drills through the second graft, through both cortices of the intervening host fragments, and directly into the first graft. Fully threaded cortical screws (typically 3.5mm or 4.5mm) are inserted. These screws must be perfectly measured to pass through all four cortices (Graft 2 $/rightarrow$ Host Near Cortex $/rightarrow$ Host Far Cortex $/rightarrow$ Graft 1).
- Screw Exchange: Once the second graft is securely fastened with definitive long screws, the short temporary screws are removed from the first graft. These holes are then over-drilled through the host bone and into the second graft, tapped, and filled with definitive long screws that traverse the entire construct.
This technique ensures that the dense cortical grafts act as the primary structural anchors, effectively compressing the weak host bone between them.
Cancellous Bone Grafting and Closure
The rigid cortical grafts provide immediate structural stability but are biologically slow to incorporate. Rapid biological stimulation is provided by the addition of cancellous bone.

The surgeon must meticulously pack the entire defect between the host fragments with the cancellous bone harvested from the proximal tibia, combined with the cancellous scrapings from the grafts. If the defect is voluminous, additional autogenous iliac crest bone graft (ICBG) or allograft cancellous chips mixed with bone marrow aspirate concentrate (BMAC) should be utilized.
Prior to closure, the tourniquet is deflated, and meticulous hemostasis is achieved. Because the limb volume has been significantly increased, the deep fascia is left open to prevent compartment syndrome. The subcutaneous tissue and skin are closed carefully over closed-suction drains. If the skin closure is excessively tight, the surgeon must not hesitate to perform prophylactic fasciotomies or utilize a local soft tissue flap to ensure a tension-free envelope over the avascular grafts.
Complications, Incidence Rates, and Salvage Management
The dual onlay graft is a massive physiological undertaking, and the complication profile reflects the severity of the underlying pathology and the magnitude of the surgical intervention. Surgeons must be acutely aware of these risks and possess the reconstructive armamentarium to manage catastrophic failures.
Soft Tissue Necrosis and Deep Infection
The most immediate and threatening complication is soft tissue necrosis. The addition of two massive cortical struts significantly expands the volume of the limb. Excessive tension on the skin closure inevitably leads to marginal ischemia, wound breakdown, and subsequent exposure of the avascular bone grafts. The incidence of delayed wound healing or superficial necrosis in these complex cases can approach 15-20%. If the wound breaks down, the avascular grafts are rapidly colonized by skin flora, leading to deep infection.
Deep infection in the presence of massive cortical autografts is a devastating complication. Because the grafts are avascular, systemic antibiotics cannot penetrate the bone, and the grafts act as massive sequestra. Management requires aggressive, radical debridement, which usually necessitates the complete removal of the dual grafts. This leaves the patient with a massive segmental bone defect. Salvage management typically involves the placement of an antibiotic-impregnated cement spacer (the Masquelet technique) or the application of a circular external fixator (Ilizarov) for bone transport once the infection is eradicated.
Graft Fracture and Donor Site Morbidity
During the postoperative period, the massive cortical grafts undergo incorporation via a process known as creeping substitution. In this process, osteoclasts resorb the dead graft bone while osteoblasts simultaneously lay down new host bone. During the height of this remodeling phase (typically between 3 to 6 months postoperatively), the graft actually becomes temporarily weaker and highly porous before it becomes stronger. Premature weight-bearing during this vulnerable window can lead to catastrophic fracture of the grafts. If a graft fracture occurs but alignment is maintained, prolonged immobilization may suffice. However, displaced fractures require revision open reduction and internal fixation, often necessitating the addition of a supplementary locking plate and further cancellous bone grafting.
Donor site morbidity is another significant concern. Harvesting a massive structural strut from the anterior medial tibia creates a large cortical defect. Complications include tibial plateau fractures (if the harvest extends too proximally), diaphyseal stress fractures (if the corners of the harvest site are not properly rounded), and massive hematoma formation. Prophylactic restriction of activities for the donor leg is absolutely required, and patients must be counseled on the risk of donor site pain and potential fracture.
Summary Table of Complications and Salvage Strategies
| Complication | Estimated Incidence | Pathophysiology | Salvage Management Strategy |
|---|---|---|---|
| Soft Tissue Necrosis | 15% - 20% | Excessive tension over bulky grafts leading to skin ischemia and wound breakdown. | Early aggressive debridement; local rotational flap or free tissue transfer (e.g., ALT flap). |
| Deep Infection | 5% - 10% | Bacterial colonization of avascular grafts, forming a massive sequestrum. | Complete hardware and graft removal; aggressive debridement; temporary antibiotic spacer (Masquelet). |
| Graft Fracture | 10% - 15% | Mechanical failure during the structurally vulnerable phase of creeping substitution. | Revision ORIF with supplementary locked plating; additional cancellous bone grafting; prolonged NWB. |
| Donor Site Fracture | 2% - 5% | Stress risers at the corners of the tibial harvest site leading to diaphyseal fracture. | Standard osteosynthesis of the donor tibia (IM nailing or locked plating); prolonged immobilization. |
| Persistent Nonunion | 10% - 20% | Failure of biological incorporation due to poor vascularity or inadequate mechanical stability. | Revision with circular external fixation (Ilizarov); vascularized fibular grafting. |
Phased Post-Operative Rehabilitation Protocols
The postoperative management of a patient who has undergone a dual onlay graft is characterized by extreme patience and rigorous adherence to a phased rehabilitation protocol. The mechanical integrity of the construct relies entirely on the slow, biological process of creeping substitution. The surgeon must resist the temptation to accelerate rehabilitation, as premature loading will inevitably lead to graft failure.
Phase 1: Immediate Postoperative Period (0 to 6 Weeks)
Immediately following surgery, the affected limb is placed in a well-padded, long-leg cast or a rigid, custom-molded orthosis. The primary goals during this phase are wound healing, edema control, and the prevention of joint contractures in the unimmobilized joints.
Strict non-weight-bearing (NWB) is absolutely enforced. The patient must be educated that the massive grafts are entirely avascular and rely on the delicate ingrowth of capillary buds from the surrounding soft tissues. Any micromotion or mechanical stress can disrupt this fragile neovascularization. Deep vein thrombosis (DVT) prophylaxis is mandatory during this period of strict immobilization.
Phase 2: The Vulnerable Remodeling Phase (6 to 12 Weeks)
At the 6-week mark, the initial cast is typically removed, and the limb is transitioned to a removable functional brace to allow for gentle, passive range of motion of the adjacent joints. Radiographic monitoring is initiated with serial orthogonal radiographs.
During this phase, the process of creeping substitution begins in earnest. Radiographically, the grafts may actually appear more radiolucent or "moth-eaten" as osteoclastic resorption outpaces osteoblastic deposition. The surgeon must recognize that the grafts are mechanically at their weakest during this time. Strict NWB must be maintained. The patient may begin gentle active-assisted range of motion (AAROM) exercises under the strict supervision of a physical therapist, but no torsional or bending forces should be applied to the extremity.
Phase 3: Early Incorporation and Progressive Loading (3 to 6 Months)
Between 3 and 6 months postoperatively, the radiographic appearance of the construct should begin to change. The surgeon looks for the obliteration of the radiolucent lines between the host bone and the grafts, and the appearance of mature trabeculations crossing the nonunion site.
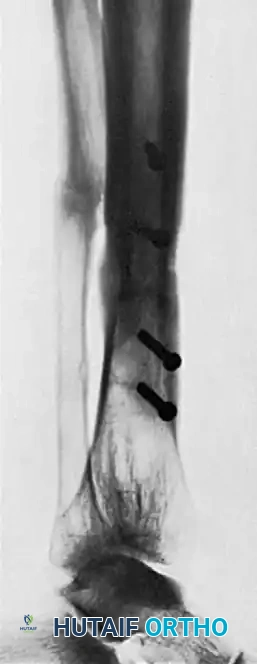
If clear evidence of trabecular bridging is observed on multiple radiographic views, the patient may be advanced to toe-touch weight-bearing (TTWB) and eventually partial weight-bearing (PWB) in a functional orthosis. This progressive mechanical loading stimulates further osteoblastic activity according to Wolff's Law, promoting the remodeling of the woven bone into mature lamellar bone. However, progression must be halted immediately if the patient experiences pain at the nonunion site or if serial radiographs demonstrate any widening of the graft-host interface.
Phase 4: Maturation and Hardware Considerations (6+ Months)
Full, unprotected weight-bearing is typically not permitted until 6 to 12 months postoperatively, and only when the surgeon is completely satisfied that mature, solid bony union has been achieved across the entire construct. The grafts will eventually remodel to resemble the normal diaphyseal cortex of the host bone.
Once massive consolidation has occurred, the surgeon must consider the management of the retained hardware. Because the dual onlay construct is extremely rigid, it can lead to stress shielding of the underlying host bone over the long term. If the patient is young and active, the removal of the transfixing screws may be considered 18 to 24 months postoperatively to allow the bone to regain its normal elastic modulus. However, hardware removal is a major procedure in itself and carries the risk of refracture through the empty screw holes; therefore, it is generally avoided in the elderly or osteoporotic population unless the hardware becomes symptomatic.
Summary of Landmark Literature and Clinical Guidelines
The evolution of the dual onlay graft technique is deeply rooted in the foundational literature of orthopedic surgery. A thorough understanding of these landmark texts provides the modern surgeon with the historical context and the biomechanical rationale necessary to apply this technique effectively.
The seminal paper by H.B. Boyd in 1941 ("Congenital Pseudarthrosis: Treatment by Dual Bone Grafts") remains the definitive text on this procedure. Boyd meticulously detailed the failure of single onlay grafts
Detailed Chapters & Topics
Dive deeper into specialized chapters regarding dual-onlay-graft
