Detailed Patient Presentation and Mechanism of Injury
The case before us involves a highly concerning and rapidly evolving clinical scenario in a 5-year-old male who was transferred to our tertiary care pediatric orthopedic trauma center from an outside community hospital. The patient’s history of present illness began the previous evening when he developed acute, unprovoked pain localized to his left groin, with radiation into the left testicle and the anterior aspect of his left hip. By the morning of presentation, the patient exhibited a pronounced antalgic gait that rapidly deteriorated into an absolute refusal to bear weight on the affected extremity. This rapid progression from localized pain to complete functional impairment is a hallmark of acute intra-articular pathology in the pediatric population and demands immediate, systematic evaluation to prevent catastrophic joint destruction.
Upon initial presentation to the outside emergency department, the patient was noted to be febrile with a core temperature of 102.5°F (39.2°C). Initial laboratory investigations revealed a leukocytosis with a white blood cell (WBC) count of 15,000/µL. Given the prominent testicular pain, the initial clinical team appropriately prioritized ruling out testicular torsion, obtaining a scrotal ultrasound which confirmed normal testicular blood flow. However, a concurrent ultrasound of the left hip demonstrated a significant unilateral joint effusion. Notably, the contralateral hip was not evaluated sonographically, which is a common oversight in community settings. The patient was subsequently transferred to our facility for definitive orthopedic management under the presumptive diagnosis of an acute pediatric hip effusion of unknown etiology.
The mechanism of injury in such cases is rarely traumatic; rather, it is typically hematogenous seeding of the synovium. In the pediatric population, the highly vascularized synovial membrane is particularly susceptible to bacterial inoculation during transient bacteremia. The referred pain pattern observed in this child—radiating to the groin and testicle—is a classic anatomical manifestation mediated by the obturator nerve. The obturator nerve provides sensory innervation to both the hip joint capsule and the medial thigh, often confounding the initial clinical picture and leading inexperienced clinicians down the path of urological or general surgical workups. Recognizing this referred pain pattern is critical for the orthopedic surgeon to rapidly redirect the diagnostic focus back to the hip joint.
Understanding the temporal sequence of these symptoms is paramount. The progression from mild discomfort to severe pain and refusal to bear weight over a 12-to-18-hour window strongly suggests a rapidly expanding intra-articular process, most notably a pyogenic infection. The accumulation of purulent fluid within the constrained space of the hip capsule leads to exponential increases in intra-articular pressure. This not only causes severe pain but also threatens the vascular supply to the developing femoral head, potentially resulting in avascular necrosis (AVN) or irreversible chondrolysis if surgical decompression is delayed.
Comprehensive Clinical Examination Findings
Upon arrival at our facility, a meticulous and comprehensive physical examination was performed. The patient appeared acutely ill and somewhat toxic, lying supine on the examination table and actively resisting any attempts to move the left lower extremity. His temperature upon arrival was 38.6°C. Observation of the resting posture of the limb is a critical component of the pediatric hip examination. Interestingly, this patient was holding his left leg in a position of full extension and external rotation.
This specific resting posture is highly atypical for a classic septic hip presentation and warrants deep biomechanical consideration. In the setting of an acute intra-articular effusion, a patient will instinctively position the joint to maximize capsular volume, thereby minimizing intra-articular pressure and pain. For the hip joint, the position of maximum capsular capacity is classically described as flexion, abduction, and external rotation (the FABER position). The fact that this child is holding the leg in extension rather than flexion presents a clinical conundrum. It may indicate an early stage of effusion where maximum capsular distension has not yet been reached, profound psoas spasm overriding the typical capsular resting position, or potentially an extra-articular pathology such as a psoas abscess or osteomyelitis of the proximal femur that is irritating the joint capsule without fully distending it.
Despite the atypical resting position, the patient exhibited extreme irritability with any passive movement of the hip. The "log-roll" test, which involves gentle internal and external rotation of the extended leg, elicited severe pain and guarding. This test is highly sensitive for intra-articular hip pathology because it moves the femoral head within the acetabulum without significantly engaging the extra-articular musculature. The presence of severe pain with microscopic capsular sheer forces strongly corroborates the presence of an acute inflammatory or infectious capsulitis.
Furthermore, palpation of the groin and proximal thigh revealed diffuse tenderness, though localized point tenderness over the femoral metaphysis was difficult to ascertain due to the child's distress. The patient's absolute refusal to bear weight is a critical clinical indicator. In a young child, the transition from a limp to non-weight-bearing status correlates strongly with the severity of the inflammatory response and the volume of the effusion. The combination of a toxic appearance, fever, and extreme pain with micro-motion necessitates an aggressive diagnostic approach, regardless of the slightly atypical resting posture of the limb.
Advanced Imaging and Diagnostics
The diagnostic workup for a suspected pediatric septic hip must be executed with precision and urgency, balancing the need for accurate information against the risk of delaying definitive surgical intervention. The initial diagnostic step, beyond the physical examination, involves a targeted laboratory workup. While the outside hospital obtained a WBC count, the standard of care dictates a more comprehensive inflammatory panel. Our immediate next step was to obtain an Erythrocyte Sedimentation Rate (ESR) and a C-Reactive Protein (CRP), alongside a repeat Complete Blood Count (CBC) with a manual differential, and blood cultures.
The kinetics of these inflammatory markers are crucial for clinical interpretation. CRP is an acute-phase reactant synthesized by the liver that elevates rapidly—within 6 to 8 hours of the onset of a bacterial infection. It is an independent, highly sensitive predictor of septic arthritis. Conversely, the ESR rises more slowly, typically peaking at 24 to 48 hours post-infection, and falls slowly as the infection resolves. In our patient, the updated labs returned a WBC of 12.8 x 10^9/L, an ESR of 20 mm/h, and a CRP of 3.0 mg/dL. The elevated CRP (>2.0 mg/dL) in the face of a relatively normal ESR is a classic presentation of an acute, early-onset septic process where the ESR has not yet had time to peak.
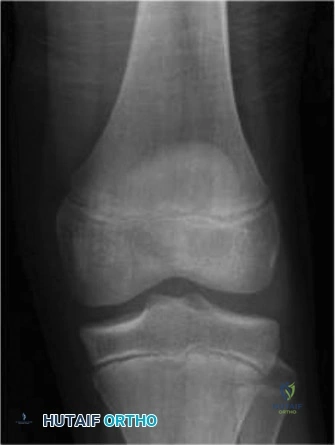
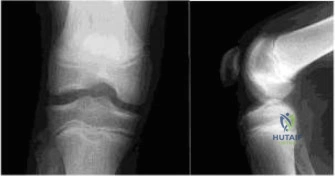
Imaging plays a supportive but vital role. Standard anteroposterior (AP) and frog-leg lateral radiographs of the pelvis are mandatory. While radiographs cannot diagnose a septic hip, they are essential to rule out other pathologies such as trauma, tumors, or Legg-Calvé-Perthes disease. In the setting of a septic hip, plain films may demonstrate subtle widening of the medial joint space (Waldenström sign) or obscuration of the periarticular fat planes due to edema, though these findings are often absent early in the disease course.
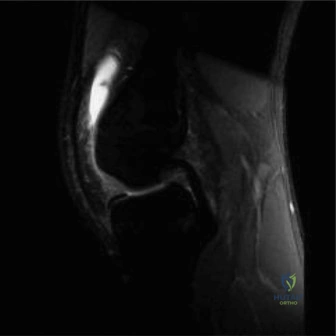
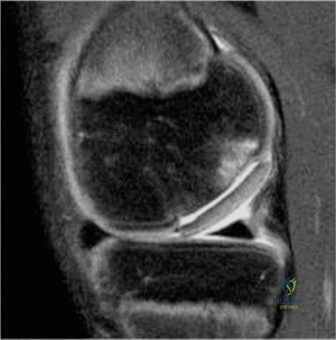
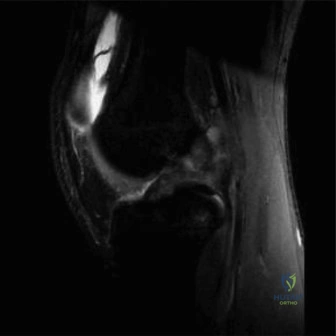
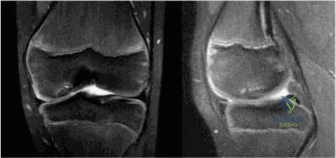
Advanced imaging modalities, specifically Magnetic Resonance Imaging (MRI) and Computed Tomography (CT), must be utilized judiciously. An MRI is highly sensitive for detecting joint effusions, synovial enhancement, and concurrent osteomyelitis. However, obtaining an MRI in a 5-year-old typically requires deep sedation or general anesthesia, which can significantly delay definitive surgical treatment. In a patient with high clinical suspicion for septic arthritis based on Kocher criteria, delaying an arthrotomy to obtain an MRI is contraindicated. MRI should be reserved for cases with an ambiguous clinical picture, failure to improve after initial surgical decompression, or when concurrent pelvic osteomyelitis or a psoas abscess is strongly suspected.
Exhaustive Differential Diagnosis
The differential diagnosis for an acutely irritable hip in a pediatric patient is broad, ranging from benign, self-limiting conditions to true surgical emergencies. The clinician must systematically synthesize the patient's age, history, physical exam, and laboratory findings to stratify risk. The most critical differentiation to make is between septic arthritis and transient synovitis, as the former requires emergent surgical intervention while the latter is managed conservatively.

Transient synovitis is the most common cause of acute hip pain in children aged 3 to 8 years. It is a benign, self-limiting inflammation of the synovial lining, often following a recent viral upper respiratory or gastrointestinal infection. Patients typically present with a limp or refusal to bear weight, but they generally appear well and lack systemic signs of toxicity. Inflammatory markers (ESR, CRP, WBC) are usually normal or only mildly elevated, and the child is typically afebrile.
Osteomyelitis of the proximal femur or pelvis must also be considered. While the clinical presentation can closely mimic septic arthritis—including fever, elevated inflammatory markers, and refusal to bear weight—the pain is often more localized to the metaphysis rather than the joint itself. However, in neonates and young infants, transphyseal blood vessels allow osteomyelitis to easily decompress into the joint space, creating a concomitant septic arthritis. In older children, a sympathetic joint effusion can occur adjacent to an area of osteomyelitis, complicating the clinical picture.
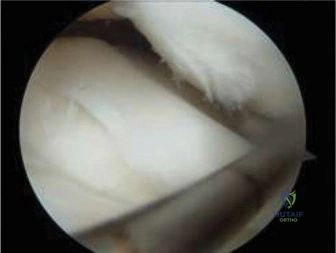
Other differentials include Legg-Calvé-Perthes disease (idiopathic avascular necrosis of the femoral head), which typically presents with a more insidious onset of a painless limp, though acute exacerbations can occur. Lyme arthritis, endemic in certain regions, can present with a large effusion and refusal to bear weight, but patients often lack high fevers and have a more subacute presentation. Juvenile Idiopathic Arthritis (JIA) is another consideration, though it usually involves multiple joints and has a more chronic timeline.
| Clinical Feature | Septic Arthritis | Transient Synovitis | Osteomyelitis (Proximal Femur) | Legg-Calvé-Perthes Disease |
|---|---|---|---|---|
| Onset | Acute, rapid deterioration | Acute to subacute | Subacute to acute | Insidious, chronic |
| Fever | High (>38.5°C) | Absent or low-grade | Moderate to High | Absent |
| Weight Bearing | Absolute refusal | Limp, may refuse | Refusal or severe limp | Antalgic gait, usually bears weight |
| Inflammatory Markers | CRP > 2.0, ESR > 40, WBC > 12k | Normal to mildly elevated | Elevated CRP and ESR | Normal |
| Ultrasound Findings | Complex effusion, capsular distension | Simple effusion | May have sympathetic effusion | Usually normal, possible mild effusion |
| Primary Treatment | Emergent surgical washout | NSAIDs, observation | IV Antibiotics, possible surgery | Containment, observation |
Complex Surgical Decision Making and Classifications
The decision to proceed to the operating room for an acute pediatric hip is guided by a synthesis of clinical prediction algorithms, most notably the Kocher criteria. Originally published in 1999, the Kocher criteria utilize four independent risk factors to differentiate septic arthritis from transient synovitis: history of fever >38.5°C, non-weight-bearing status, ESR >40 mm/h, and WBC >12,000/µL. The probability of septic arthritis increases dramatically with the number of criteria present: 3% for zero criteria, 9% for one, 40% for two, 93% for three, and 99.6% for all four.
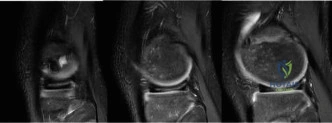
However, modern orthopedic practice has recognized the limitations of the original Kocher criteria, particularly the delayed rise of the ESR. Consequently, modified criteria incorporating the CRP have been widely adopted. A CRP >2.0 mg/dL has been shown to be a strong, independent predictor of septic arthritis. In our patient, we have a fever of 38.6°C, inability to bear weight, a WBC of 12.8, and a CRP of 3.0. Despite the ESR being only 20 (likely due to the acute onset of symptoms), the presence of three strong clinical indicators, combined with the patient's toxic appearance, pushes the probability of septic arthritis well above the threshold for surgical intervention.
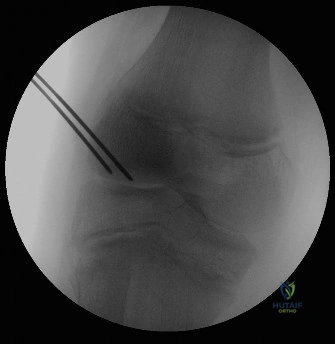
The debate often arises regarding whether to perform a diagnostic hip aspiration prior to formal arthrotomy. In cases where the diagnosis is equivocal (e.g., only one or two Kocher criteria), an ultrasound-guided aspiration can provide definitive synovial fluid analysis. A synovial WBC count >50,000 cells/µL with >90% polymorphonuclear leukocytes (PMNs) is highly diagnostic for bacterial infection. However, in a patient with a high pre-test probability, as in our case, a preoperative aspiration in the emergency department or radiology suite may unnecessarily delay definitive care and subject the child to multiple sedations.
Therefore, the most appropriate surgical decision for this patient is to proceed emergently to the operating room for an open arthrotomy and joint lavage. The pathophysiology of septic arthritis dictates this urgency. Bacterial pathogens, particularly Staphylococcus aureus, release proteolytic enzymes and exotoxins that rapidly degrade articular cartilage. Furthermore, the host's own immune response generates matrix metalloproteinases and inflammatory cytokines that contribute to chondrolysis. Irreversible cartilage damage can occur within 8 to 12 hours of infection onset. Additionally, the increased intra-articular pressure from the purulent effusion can occlude the retinacular vessels supplying the femoral head, leading to devastating avascular necrosis.
Step-by-Step Surgical Technique and Intervention
The surgical management of a pediatric septic hip requires a meticulous and efficient approach to ensure complete joint decompression and thorough eradication of the purulent material. The patient is brought to the operating room and placed in the supine position on a radiolucent table. General endotracheal anesthesia is administered. Prophylactic antibiotics are strictly withheld until intraoperative synovial fluid and tissue cultures are obtained, unless the patient is demonstrating signs of profound hemodynamic instability or sepsis.
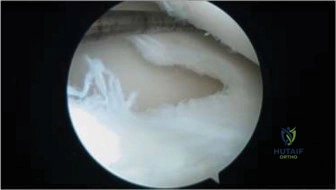
The preferred surgical exposure for a pediatric hip arthrotomy is the anterior approach, originally described by Smith-Petersen. This approach utilizes an internervous and intermuscular plane, minimizing morbidity and allowing direct access to the anterior hip capsule. An oblique incision is made beginning just distal and lateral to the anterior superior iliac spine (ASIS), extending distally toward the lateral aspect of the patella. The superficial fascia is incised, and the interval between the sartorius (innervated by the femoral nerve) and the tensor fasciae latae (innervated by the superior gluteal nerve) is identified and developed.
Deep dissection proceeds by retracting the sartorius medially and the tensor fasciae latae laterally. The rectus femoris is identified, and its direct head is traced proximally to its origin on the anterior inferior iliac spine (AIIS). The rectus is retracted medially, exposing the underlying anterior joint capsule. Care must be taken during this exposure to identify and ligate the ascending branches of the lateral femoral circumflex artery, which reliably cross the operative field in the distal portion of the exposure. Failure to control these vessels can lead to significant postoperative hematoma.
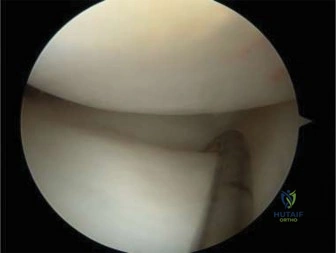
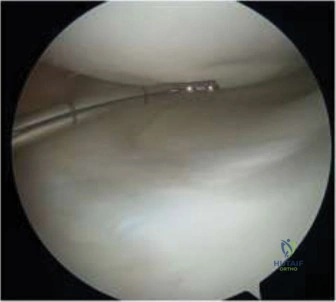
Once the anterior capsule is exposed, a needle is introduced into the joint space to aspirate the effusion. This fluid is immediately sent for cell count, Gram stain, aerobic and anaerobic cultures, and crystal analysis. Following aspiration, a formal capsulotomy is performed. An I-shaped or T-shaped incision is made in the capsule. Upon entering the joint, purulent material, fibrinous exudate, and hypertrophic synovium are typically encountered. The joint is aggressively irrigated with several liters of sterile normal saline. A pediatric feeding tube or a small Frazier suction tip can be gently passed around the femoral neck to ensure that loculated pockets of pus in the posterior and inferior recesses are thoroughly washed out.
After meticulous lavage, the joint is inspected. The cartilage of the femoral head should be evaluated for softening or erosions. A partial synovectomy may be performed to remove necrotic tissue, and a sample of the synovium is sent for pathologic evaluation and culture. The capsulotomy is intentionally left open to prevent the re-accumulation of fluid and subsequent elevation of intra-articular pressure. A closed suction drain is placed deep within the joint space and brought out through a separate stab incision. The fascial layers, subcutaneous tissue, and skin are then closed meticulously.
Strict Post-Operative Protocol and Rehabilitation Stages
The postoperative management of a pediatric septic hip is as critical as the surgical intervention itself. Immediately following the procedure, the patient is started on empiric intravenous antibiotics. The choice of antibiotics must cover the most common pediatric pathogens, primarily Staphylococcus aureus (including Methicillin-resistant strains depending on local antibiograms), Streptococcus pyogenes (Group A Strep), and Kingella kingae. A typical empiric regimen might include a first-generation cephalosporin (e.g., Cefazolin) or Clindamycin, combined with coverage for Kingella if the child is under 4 years of age.
The patient is admitted to the pediatric ward for close monitoring. The intra-articular drain is typically left in place for 48 to 72 hours, or until the output becomes minimal and serous. Inflammatory markers, specifically the CRP, are monitored daily. The CRP is an excellent biomarker for tracking the response to treatment; a rapidly falling CRP indicates adequate source control and effective antibiotic therapy. The ESR will also be monitored, but its delayed normalization means it is less useful for acute day-to-day decision making.
Weight-bearing is strictly restricted in the immediate postoperative period. The patient may be placed in a spica cast or a foam abduction pillow to maintain the hip in a stable, decompressed position and to prevent subluxation, particularly if there was extensive capsular distension or ligamentous laxity noted intraoperatively. Once the clinical symptoms improve, the fever resolves, and the CRP demonstrates a significant downward trend, physical therapy is initiated. Early, gentle passive and active-assisted range of motion exercises are crucial to prevent capsular contractures and to stimulate cartilage nutrition via synovial fluid diffusion.
Transitioning from intravenous to oral antibiotics is a major milestone in the rehabilitation phase. This transition is typically considered when the patient is afebrile for 48 hours, demonstrating significant clinical improvement, and the CRP has normalized or is rapidly approaching baseline. The total duration of antibiotic therapy is usually 3 to 4 weeks, guided by the specific organism identified and the clinical response. Outpatient follow-up requires serial radiographs at 6 weeks, 3 months, and 6 months to monitor for late complications such as avascular necrosis, physeal arrest, or progressive joint space narrowing.
High-Yield Clinical Pearls and Pitfalls
When managing a suspected pediatric septic hip, the orthopedic surgeon must navigate a minefield of potential diagnostic and therapeutic pitfalls. One of the highest-yield clinical pearls is to never underestimate the value of the C-Reactive Protein. While the classic Kocher criteria rely on the ESR, the CRP is far more sensitive in the acute setting. If a child presents with a toxic appearance, refusal to bear weight, and an elevated CRP, the index of suspicion for a septic joint must remain extremely high, even if the ESR is normal.
A significant pitfall is delaying definitive surgical management to obtain an MRI. In a patient who meets multiple Kocher criteria and has an ultrasound-confirmed effusion, the diagnosis of septic arthritis is highly probable. The time required to coordinate an MRI with pediatric anesthesia can result in hours of continued cartilage degradation and ischemic insult to the femoral head. In these clear-cut scenarios, the operating room is the appropriate diagnostic and therapeutic destination. MRI should be strictly reserved for atypical presentations or when evaluating for concurrent osteomyelitis after the joint has been decompressed.
Another critical pearl relates to the physical examination. While the FABER position is the classic resting posture for a distended hip capsule, variations exist. As seen in this case, a patient holding the leg in extension and external rotation does not rule out a septic hip. The key physical finding is not the static posture, but rather the extreme irritability and pain elicited by micro-motion, such as the log-roll test.
Finally, surgeons must be vigilant regarding the possibility of concomitant infections. A septic hip in a neonate or young infant is frequently associated with proximal femoral osteomyelitis due to transphyseal vessels. In older children, Staphylococcus aureus bacteremia can seed multiple sites. Therefore, a thorough secondary survey and a low threshold for investigating other areas of bone or joint pain are essential. Complete eradication of the infection requires not only thorough surgical lavage but also precise, culture-directed antimicrobial therapy and rigorous postoperative surveillance.
Detailed Chapters & Topics
Dive deeper into specialized chapters regarding 14-pediatrics-cases
