Unraveling 10 Pediatric Cases: Surgical Reduction and Internal Fixation
Key Takeaway
Your ultimate guide to Unraveling 10 Pediatric Cases: Surgical Reduction and Internal Fixation starts here. A Tillaux fracture is an adolescent transitional ankle fracture of the distal tibial epiphysis, where the AITFL attaches, classified as Salter-Harris III because the fracture exits the physis into the epiphysis. For displaced fractures, **surgical reduction and internal** fixation is often required to ensure proper alignment, stability, and growth plate integrity, preventing long-term complications.
Patient Presentation and History
Mechanism of Injury and Prehospital Course
The management of pediatric orthopedic trauma requires a profound understanding of the unique biomechanical properties of the immature skeleton, the presence of open physes, and the substantial remodeling potential inherent in children. This Grand Rounds presentation synthesizes the surgical principles applied to ten complex pediatric fracture patterns, anchored by an index presentation of a high-energy pediatric polytrauma.
The index patient is an 8-year-old male who presented to the Level I Pediatric Trauma Center following a high-speed motor vehicle collision. The patient was a restrained rear-seat passenger in a vehicle that sustained a lateral T-bone impact at approximately sixty miles per hour. Extrication by emergency medical services required twenty minutes. Prehospital reports indicated an initial Glasgow Coma Scale of fourteen, with localized pain and obvious deformities in the right upper extremity and right lower extremity.
Prehospital interventions included the application of a rigid cervical collar, supplemental oxygen via a non-rebreather mask, and the establishment of a single large-bore peripheral intravenous line. The right upper extremity was temporarily stabilized with a cardboard splint, and a pediatric traction splint was applied to the right lower extremity to manage a suspected femoral shaft fracture. The patient received intravenous fentanyl for analgesia during transport. There was no reported loss of consciousness, and the patient had no significant past medical history, no known drug allergies, and no prior surgical interventions.
Emergency Department Resuscitation
Upon arrival at the trauma bay, the patient was evaluated according to the Advanced Trauma Life Support protocols modified for pediatric patients. The primary survey revealed a patent airway, symmetric bilateral breath sounds, and hemodynamic stability with a heart rate of 115 beats per minute and a blood pressure of 105/65 mmHg. The focused assessment with sonography for trauma examination was negative for free intraperitoneal or pericardial fluid.
The secondary survey isolated the injuries to the musculoskeletal system. The patient exhibited a classic "floating elbow" presentation on the right side, characterized by a severely displaced supracondylar humerus fracture combined with an ipsilateral displaced diaphyseal forearm fracture. Additionally, there was a closed, length-unstable fracture of the right femoral shaft. The constellation of these injuries represents a significant transfer of kinetic energy, necessitating meticulous evaluation to rule out evolving compartment syndrome and subtle physeal injuries that could compromise future growth. The lack of medical comorbidities allowed the surgical team to focus entirely on the acute resuscitation and orthopedic stabilization of the patient.
Clinical Examination Findings
Primary Survey and Systemic Evaluation
The clinical examination of a pediatric polytrauma patient must be systematic, prioritizing life-threatening injuries before addressing limb-threatening conditions. Following the clearance of the cervical spine, chest, and abdomen by the general trauma surgery service, the orthopedic team commenced a detailed musculoskeletal evaluation. The patient was cooperative but in significant distress. The skin was intact globally, with no evidence of open fractures, lacerations, or high-pressure injection injuries.
Orthopedic Inspection and Palpation
Inspection of the right upper extremity revealed gross deformity at the elbow with significant soft tissue swelling, ecchymosis over the antecubital fossa, and the classic "puckering" sign (dimpling of the anterior skin), which is highly indicative of the proximal fracture fragment penetrating the brachialis muscle and tethering the subcutaneous tissue. This clinical sign is a harbinger of potential neurovascular entrapment and necessitates urgent reduction. The ipsilateral forearm demonstrated an apex-volar clinical deformity consistent with a both-bone forearm fracture.
Inspection of the right lower extremity revealed shortening, external rotation, and significant thigh swelling. The pediatric traction splint had partially restored length, but the thigh compartments were tense. Palpation elicited severe localized tenderness over the distal humerus, the midshaft of the radius and ulna, and the mid-diaphysis of the femur. Crepitus was noted, though intentional elicitation of crepitus was avoided to prevent further soft tissue trauma and neurovascular compromise. Range of motion testing was deferred due to the obvious instability and the risk of exacerbating the injuries.
Neurological and Vascular Assessment
A rigorous neurovascular examination is the cornerstone of pediatric fracture evaluation, particularly in the setting of a supracondylar humerus fracture. Vascular assessment of the right upper extremity revealed a palpable but diminished radial pulse compared to the contralateral side. Capillary refill was brisk at less than two seconds, and the hand was warm and pink, indicating a "pink, pulseless" hand scenario or a perfused hand with a diminished pulse due to vasospasm or partial brachial artery kinking.
Neurological evaluation in the pediatric patient requires specific, age-appropriate motor and sensory testing. The anterior interosseous nerve was assessed by asking the patient to form an "OK" sign; the patient demonstrated an inability to flex the interphalangeal joint of the thumb and the distal interphalangeal joint of the index finger, indicating an anterior interosseous nerve neuropraxia, the most common neurological deficit associated with extension-type supracondylar humerus fractures. Radial nerve function (wrist extension, thumb extension) and ulnar nerve function (finger abduction, cross-finger test) were intact.
In the lower extremity, dorsalis pedis and posterior tibial pulses were bounding. Sensation in the deep peroneal, superficial peroneal, tibial, and sural nerve distributions was intact. However, the tense swelling in the right thigh and the ipsilateral forearm raised the clinical suspicion for impending compartment syndrome. Baseline compartment pressure measurements were not immediately taken, but the threshold for intervention was set exceptionally low, dictating the need for urgent surgical stabilization to reduce the fractures and decompress the soft tissue envelopes indirectly.
Imaging and Diagnostics
Standard Radiographic Protocols
Radiographic evaluation of the pediatric skeleton requires adherence to the "Rule of Twos": two orthogonal views (anteroposterior and lateral), two joints (inclusion of the joint above and below the injury), two limbs (comparison views of the uninjured contralateral extremity when physeal anatomy is ambiguous), and two occasions (repeat radiographs if initial films are negative but clinical suspicion remains high).
For the index patient, anteroposterior and lateral radiographs of the right humerus, elbow, forearm, and femur were obtained. The elbow radiographs revealed a Gartland Type III extension-type supracondylar humerus fracture. The anterior humeral line passed completely anterior to the capitellum on the true lateral view, and Baumann's angle was significantly altered on the anteroposterior view, indicating coronal plane malalignment. The forearm radiographs demonstrated completely displaced, overriding fractures of the midshaft radius and ulna. The femur radiographs showed a transverse, length-unstable fracture of the middle third of the femoral diaphysis with three centimeters of overriding shortening.
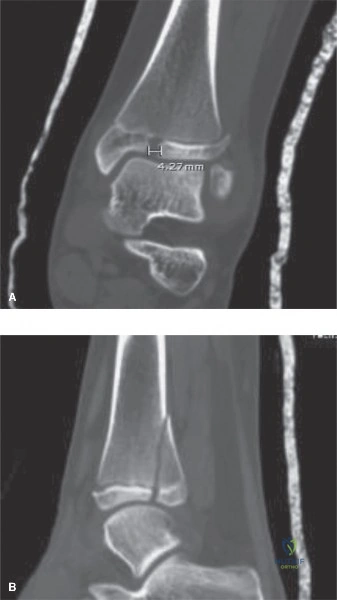
Advanced Imaging Indications
While standard radiography is sufficient for the majority of pediatric diaphyseal and metaphyseal fractures, advanced imaging modalities are critical for evaluating complex intra-articular fractures, transitional fractures of the distal tibia (such as Tillaux or triplane fractures), and injuries involving the cartilaginous epiphysis.
In cases where a lateral condyle fracture is suspected but displacement is ambiguous, an internal oblique radiograph or a magnetic resonance imaging scan may be indicated to assess the integrity of the cartilaginous hinge. If the cartilaginous hinge is intact, the fracture may be treated with closed reduction and percutaneous pinning or cast immobilization. If the hinge is disrupted, open reduction is mandatory to prevent nonunion, cubitus valgus deformity, and tardy ulnar nerve palsy. Computed tomography with three-dimensional reconstruction is invaluable for preoperative planning in complex physeal fractures, allowing the surgeon to visualize the exact plane of the fracture lines and plan lag screw trajectories that minimize physeal violation.
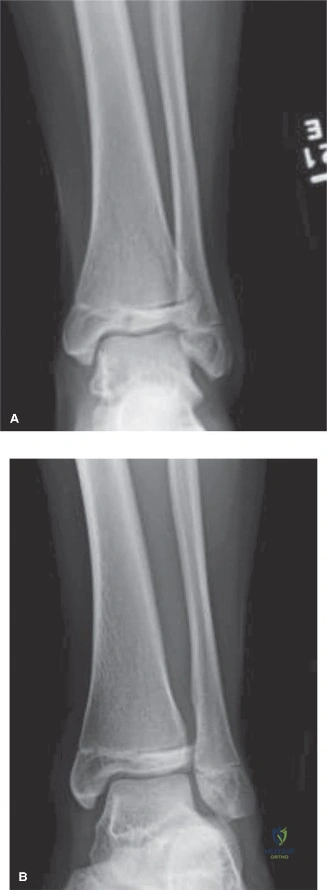
Preoperative Templating
Preoperative templating is a non-negotiable step in the surgical management of pediatric orthopedic trauma, particularly when utilizing elastic stable intramedullary nailing for long bone fractures. For the femoral shaft fracture in our index patient, digital templating was utilized to determine the appropriate diameter of the titanium elastic nails. The rule of thumb dictates that the combined diameter of the two nails should occupy approximately eighty percent of the narrowest portion of the medullary canal.
The isthmus of the pediatric femur was measured on the anteroposterior radiograph, and the appropriate nail size was calculated. For example, if the narrowest canal diameter is 10 millimeters, two 4.0-millimeter nails would be selected. Templating also involves planning the entry points—typically retrograde via the medial and lateral distal femoral metaphysis, ensuring the entry sites are proximal to the distal femoral physis to avoid iatrogenic growth arrest. For the supracondylar humerus fracture, templating involves determining the appropriate Kirschner wire size (typically 1.6 or 2.0 millimeters for an 8-year-old) and planning the pin configuration (divergent lateral pins versus crossed medial and lateral pins) based on the fracture geometry and the size of the medial and lateral columns.
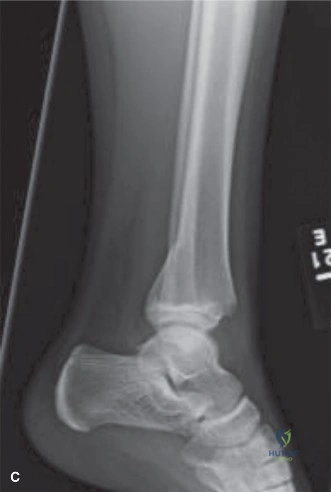
Differential Diagnosis
Diagnostic Considerations in Pediatric Trauma
The differential diagnosis in pediatric orthopedic trauma must account for the unique anatomical features of the growing child, specifically the physes, apophyses, and the thick, osteogenic periosteum. A misdiagnosis can lead to inappropriate treatment, resulting in severe complications such as growth arrest, angular deformity, or joint incongruity. The following table outlines the differential diagnosis for three critical pediatric elbow injuries that often present with similar clinical mechanisms (fall on an outstretched hand) but require vastly different surgical decision-making algorithms.
| Diagnostic Entity | Radiographic Hallmarks | Clinical Implications | Surgical Indications |
|---|---|---|---|
| Supracondylar Humerus Fracture | Disruption of anterior humeral line; altered Baumann's angle; posterior fat pad sign. Fracture line propagates through the olecranon fossa. | High risk of neurovascular compromise (AIN, brachial artery). High risk of cubitus varus malunion if coronal rotation is not corrected. | Gartland Type II (with rotational instability) and all Type III/IV fractures require closed/open reduction and percutaneous pinning. |
| Lateral Condyle Humerus Fracture | Fracture line exits through the metaphysis and the capitellotrochlear groove (Milch I) or apex of the trochlea (Milch II). Thurston-Holland fragment present. | Intra-articular injury. High risk of nonunion due to synovial fluid bathing the fracture and pull of the extensor origin. | Displacement > 2mm requires open reduction and internal fixation to restore articular congruity and prevent tardy ulnar nerve palsy. |
| Transphyseal Separation of Distal Humerus | Radius and ulna maintain normal relationship to each other but are displaced relative to the humerus. Often occurs in infants before capitellar ossification. | Frequently mistaken for an elbow dislocation. High association with non-accidental trauma in infants. | Closed reduction and percutaneous pinning if unstable. Requires arthrogram to confirm reduction due to lack of ossific nuclei. |
Distinguishing between a supracondylar fracture and a lateral condyle fracture is paramount. A lateral condyle fracture is a Salter-Harris Type IV equivalent (or Type II if the fracture exits through the cartilaginous trochlea without violating the joint, though this is rare). It requires anatomic articular reduction. Conversely, a supracondylar fracture is extra-articular; while anatomic reduction is preferred, slight translation is tolerated provided that coronal and sagittal alignment are perfectly restored to prevent the classic gunstock deformity (cubitus varus).
Surgical Decision Making and Classification
Principles of Pediatric Fracture Management
Surgical decision-making in pediatric orthopedics is governed by the patient's age, the bone involved, the proximity of the fracture to the physis, and the plane of the deformity. The remodeling potential of a pediatric bone is greatest in the plane of adjacent joint motion (sagittal plane), near rapidly growing physes (e.g., distal radius, proximal humerus), and in younger patients. However, rotational deformities and intra-articular step-offs do not remodel and require precise surgical correction.
The decision to proceed with operative intervention versus non-operative management hinges on whether the fracture can be maintained in an acceptable alignment using closed methods. In the context of our polytrauma index case, the presence of a floating elbow and an ipsilateral femur fracture dictated an absolute indication for surgical stabilization of all fractures to facilitate nursing care, allow for early mobilization, and reduce the risk of systemic complications such as acute respiratory distress syndrome or fat embolism syndrome.
Analysis of Ten Critical Pediatric Fracture Patterns
To fully unravel the complexities of pediatric surgical reduction and internal fixation, we must analyze the ten foundational cases that define this subspecialty. The surgical decision matrix for each pattern is distinct.
Case One Supracondylar Humerus Fractures
Classified by the Gartland system. Type I (non-displaced) is treated with long-arm casting. Type II (hinged intact posterior cortex) and Type III (completely displaced) require closed reduction and percutaneous pinning. Type IV fractures exhibit multidirectional instability due to complete periosteal circumferential disruption and often require open reduction if closed methods fail. The standard fixation utilizes two or three divergent lateral-entry Kirschner wires to avoid iatrogenic injury to the ulnar nerve, which is highly vulnerable with medial pin placement.
Case Two Lateral Condyle Fractures
Classified by the Milch system based on the fracture line's exit point. The critical decision-making factor is displacement. Fractures displaced greater than 2 millimeters require open reduction and internal fixation, typically utilizing a lateral approach (Kocher interval between the anconeus and extensor carpi ulnaris) and fixation with two divergent Kirschner wires or cannulated screws. Failure to achieve anatomic reduction leads to nonunion and progressive cubitus valgus.
Case Three Both Bone Forearm Fractures
While many pediatric forearm fractures are treated with closed reduction and casting, surgical intervention is indicated for open fractures, irreducible fractures, loss of reduction in a cast, or in the setting of a floating elbow. The standard of care for diaphyseal fractures is elastic stable intramedullary nailing. The nails are inserted retrogradely into the radius (via the distal lateral metaphysis, avoiding the superficial radial nerve) and antegradely or retrogradely into the ulna. The nails must be pre-bent to restore the radial bow, which is critical for restoring pronation and supination.
Case Four Radial Neck Fractures
Classified by the Judet system based on the angle of angulation. Angulation greater than 30 degrees in children over ten years old, or greater than 45 degrees in younger children, requires reduction. The preferred surgical technique is the Metaizeau technique, which involves retrograde insertion of a pre-bent titanium elastic nail from the distal radius. The nail is advanced to the proximal radius, and rotation of the nail is used to reduce the radial head anatomically without opening the fracture site, thereby preserving the tenuous blood supply to the radial head and minimizing the risk of avascular necrosis.
Case Five Femoral Shaft Fractures
Treatment is highly age-dependent. Infants (0-6 months) are treated with a Pavlik harness. Children 6 months to 5 years are typically treated with immediate spica casting. For children aged 5 to 11 years (or weighing less than 50 kilograms), elastic stable intramedullary nailing is the gold standard. For adolescents over 11 years or weighing more than 50 kilograms, rigid lateral-entry trochanteric intramedullary nailing or submuscular plating is indicated. ESIN utilizes two C-shaped titanium nails inserted retrogradely to provide three-point fixation and rotational stability.
Case Six Slipped Capital Femoral Epiphysis
SCFE is a Salter-Harris Type I equivalent injury of the proximal femur. It is classified as stable (patient can bear weight) or unstable (patient cannot bear weight). Unstable SCFE has a high rate of avascular necrosis. The surgical standard is in situ percutaneous pinning utilizing a single partially threaded cannulated screw placed centrally within the epiphysis. The goal is to stabilize the physis and prevent further slippage; routine prophylactic pinning of the contralateral hip is debated but often performed in high-risk demographics.
Case Seven Tibial Eminence Fractures
Often considered the pediatric equivalent of an anterior cruciate ligament tear. Classified by the Meyers-McKeever system. Type I is non-displaced. Type II is hinged anteriorly. Type III is completely displaced. Types II and III require surgical reduction. Arthroscopic reduction and internal fixation utilizing sutures, anchors, or cannulated screws is the preferred method. The meniscus, particularly the anterior horn of the medial meniscus, is frequently incarcerated in the fracture site and must be extracted prior to reduction.
Case Eight Distal Tibial Transitional Fractures
These include the Tillaux fracture (Salter-Harris III of the anterolateral distal tibia) and the Triplane fracture (Salter-Harris IV equivalent occurring in three planes). These occur during the asymmetrical closure of the distal tibial physis (closing central to medial to lateral). Displacement greater than 2 millimeters requires open or arthroscopically assisted reduction and internal fixation to prevent post-traumatic arthritis. Fixation is typically achieved with epiphyseal or metaphyseal parallel cannulated lag screws, ensuring no screws cross the remaining open physis.
Case Nine Medial Epicondyle Fractures
Often associated with elbow dislocations. Absolute indications for surgery include an incarcerated medial epicondyle fragment within the joint space, an open fracture, or ulnar nerve dysfunction. Relative indications include displacement greater than 5 millimeters in a high-level throwing athlete. Surgical fixation involves an open approach, identification and protection of the ulnar nerve, and fixation with a single cannulated screw and washer or Kirschner wires.
Case Ten Monteggia Fracture Dislocations
Defined by the Bado classification as a fracture of the ulna with an associated dislocation of the radial head. The most common pediatric variant is Bado Type I (anterior dislocation of the radial head with an apex-anterior ulnar fracture). The surgical principle dictates that anatomic restoration of ulnar length and alignment will spontaneously reduce the radial head. If closed reduction of the ulna fails to reduce the radial head, surgical fixation of the ulna (via plating or elastic nailing) is required. If the radial head remains dislocated after ulnar fixation, an open reduction of the radiocapitellar joint is mandated to clear interposed annular ligament or capsule.
Surgical Technique and Intervention
Operating Room Setup and Patient Positioning
Returning to our index polytrauma patient, the surgical sequence was carefully orchestrated to minimize anesthesia time and optimize workflow. The patient was positioned supine on a radiolucent operating table. A bump was placed under the right scapula to facilitate access to the posterior aspect of the elbow, and the right upper extremity was prepped and draped free on a radiolucent hand table. The right lower extremity was prepped and draped free to the level of the iliac crest to allow for access to the distal femur and visualization of the entire limb for the elastic stable intramedullary nailing.
Two image intensifiers (C-arms) were utilized simultaneously to prevent the need for continuous repositioning of the equipment between the upper and lower extremities. The surgical team was divided into two groups, working synchronously. The primary orthopedic surgeon addressed the supracondylar humerus and forearm fractures, while the senior orthopedic resident, under direct supervision, addressed the femoral shaft fracture.
Closed Reduction and Percutaneous Pinning
The supracondylar humerus fracture was addressed first due to the risk of neurovascular compromise. The reduction maneuver began with longitudinal traction applied in supination and extension to unlock the fracture fragments. The medial and lateral columns were palpated to ensure the restoration of length. While maintaining traction, the surgeon corrected the coronal plane translation and the rotational deformity. Finally, the elbow was hyperflexed while applying anteriorly directed pressure to the olecranon to reduce the posterior displacement and close the posterior periosteal hinge.
Fluoroscopy was utilized to confirm anatomical reduction in both the anteroposterior and lateral planes. The anterior humeral line was restored to intersect the middle third of the capitellum, and Baumann's angle was measured at 75 degrees, matching the anticipated normal value. Fixation was achieved utilizing three divergent 2.0-millimeter Kirschner wires inserted from the lateral epicondyle. The pins were placed percutaneously, ensuring bicortical purchase in the proximal fragment. The pins were cut outside the skin and bent to prevent migration.

Following the stabilization of the elbow
