Pediatric Anterior Knee Pain: Solve the Puzzle with Case Insights
Key Takeaway
Looking for accurate information on Pediatric Anterior Knee Pain: Solve the Puzzle with Case Insights? For anterior knee pain, the initial step is to assess flexibility and strength, focusing on deficits in core strength, single leg balance, and overall flexibility. Physical therapy is then appropriate, concentrating on proximal stretching and strengthening, particularly of the core and hip muscles. This approach effectively addresses the body's inability to stabilize and absorb load, often preceding the need for further imaging.
Patient Presentation and History
A 14-year-old male athlete presents to the orthopedic trauma bay following an acute injury sustained during a competitive basketball tournament. The patient reports a sudden, severe onset of anterior knee pain in the dominant right lower extremity. The mechanism of injury involved a forceful eccentric contraction of the quadriceps muscle during a rapid deceleration and landing from a jump. The patient felt an immediate "pop" and was subsequently unable to bear weight or actively extend the knee.
A detailed review of the patient's history reveals a six-month prodrome of insidious, intermittent anterior knee pain localized to the tibial tubercle, which had been previously diagnosed as Osgood-Schlatter disease. He had been managing this chronic condition with conservative measures, including ice, non-steroidal anti-inflammatory drugs, and physical therapy, without cessation of athletic activities.
The patient is otherwise healthy, with a body mass index in the 85th percentile for his age, representing a robust, muscular build typical of high-level adolescent athletes. There is no prior history of systemic illness, metabolic bone disease, or connective tissue disorders. No previous surgical interventions have been performed on either lower extremity. The presentation of acute-on-chronic anterior knee pain in a peripubertal athlete with an eccentric loading mechanism raises a high index of suspicion for a catastrophic failure of the extensor mechanism.
Clinical Examination Findings
Inspection and Soft Tissue Assessment
Upon initial inspection in the trauma bay, the right lower extremity exhibits profound swelling localized to the anterior aspect of the proximal tibia. There is a distinct loss of the normal peripatellar topographical anatomy, with the patella appearing superiorly migrated within the trochlear groove, indicative of patella alta. Significant ecchymosis is beginning to develop over the anterior tibial crest.
Palpation and Range of Motion
Palpation reveals exquisite, localized tenderness directly over the tibial tubercle. A palpable defect or "step-off" is appreciated just distal to the inferior pole of the patella, corresponding to the disrupted extensor mechanism.
Range of motion testing is severely limited by pain and mechanical discontinuity. The patient exhibits a profound extensor lag; he is entirely unable to perform a straight leg raise or actively extend the knee against gravity. Passive range of motion demonstrates unrestricted flexion, though this exacerbates the anterior tibial pain.
Neurological and Vascular Assessment
A meticulous neurovascular examination is paramount in this clinical scenario. The anterior tibial recurrent artery is anatomically tethered near the proximal tibia and is highly susceptible to laceration or avulsion during violent displacement of the tibial tubercle. Consequently, there is a well-documented risk of acute anterior compartment syndrome secondary to arterial hemorrhage.
Palpation of the anterior, lateral, deep posterior, and superficial posterior compartments reveals tense, non-compressible soft tissue envelopes, particularly in the anterior compartment. The patient reports pain out of proportion to the apparent injury with passive plantar flexion of the hallux and ankle. Dorsalis pedis and posterior tibial pulses remain palpable and symmetric to the contralateral extremity, but capillary refill is brisk, and two-point discrimination in the first web space (deep peroneal nerve distribution) is diminished. These findings necessitate immediate compartment pressure monitoring.
Imaging and Diagnostics
Standard Radiographic Evaluation
Initial diagnostic imaging includes standard anteroposterior and lateral radiographs of the affected knee.

The lateral radiograph is the most diagnostic, revealing a displaced avulsion fracture of the tibial tubercle. The fracture line propagates proximally through the secondary ossification center of the tibial apophysis and extends intra-articularly into the proximal tibial epiphysis. The avulsed fragment is displaced anteriorly and proximally by the unopposed pull of the quadriceps musculature.
Measurement of the Insall-Salvati ratio on the lateral radiograph yields a value of 1.4, confirming the clinical suspicion of patella alta secondary to the distal detachment of the patellar tendon. There is also evidence of chronic apophysitis, characterized by fragmentation and sclerosis of the tubercle, consistent with the patient's history of Osgood-Schlatter disease.
Advanced Imaging Indications
Given the intra-articular extension of the fracture line and the need for precise preoperative templating, a non-contrast computed tomography scan with three-dimensional reconstructions is indicated.
The computed tomography scan provides superior delineation of the fracture morphology. Axial and sagittal reconstructions precisely quantify the degree of intra-articular step-off, which measures 4 millimeters, and confirm the presence of a comminuted, purely cartilaginous hinge at the posterior aspect of the fracture. Furthermore, the imaging allows for the evaluation of the anterior horns of the medial and lateral menisci, which can frequently become entrapped within the intra-articular fracture gap, preventing closed reduction.
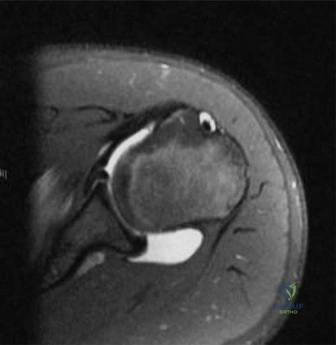
Magnetic resonance imaging is generally reserved for cases where concomitant ligamentous injury is suspected or to evaluate the integrity of the patellar tendon in the setting of a purely cartilaginous patellar sleeve fracture. In this specific presentation, the osseous avulsion is clearly delineated on computed tomography, making magnetic resonance imaging unnecessary for acute surgical decision-making.
Differential Diagnosis
The presentation of acute anterior knee pain and extensor mechanism failure in a pediatric or adolescent patient requires a systematic differentiation of several distinct pathologies.
| Condition | Clinical Presentation | Radiographic Findings | Management Strategy |
|---|---|---|---|
| Tibial Tubercle Avulsion Fracture | Acute pain, inability to extend knee, palpable gap at tubercle, often jumping mechanism in adolescent males. | Displaced fracture of the tibial apophysis, +/- intra-articular extension. Patella alta. | Operative fixation (screws/tension band) for displaced or intra-articular fractures. Cast for non-displaced. |
| Patellar Sleeve Fracture | Acute pain, extensive effusion, palpable gap at inferior pole of patella. Typically younger children (8-12 years). | Small osseous fleck at inferior patella, significant patella alta. MRI shows extensive cartilaginous avulsion. | Urgent operative repair (transosseous sutures) to restore extensor mechanism and prevent patellar duplication. |
| Osgood Schlatter Disease | Chronic, insidious anterior knee pain. Pain with kneeling or running. No acute extensor lag. | Fragmentation and sclerosis of the tibial tubercle. No acute fracture line or significant displacement. | Non-operative. Activity modification, NSAIDs, physical therapy focusing on quadriceps flexibility. |
| Patellar Tendon Rupture | Acute pain, palpable gap mid-substance or at insertion. Rare in adolescents without systemic disease or steroid use. | Patella alta. No acute fracture of the patella or tibial tubercle. MRI confirms tendon discontinuity. | Operative primary repair with suture anchors or transosseous tunnels. |
| Sinding Larsen Johansson Syndrome | Chronic pain at the inferior pole of the patella. Overuse injury. | Calcification or fragmentation at the proximal attachment of the patellar tendon. | Non-operative. Rest, physical therapy, counterforce bracing. |
Surgical Decision Making and Classification
The Ogden Classification System
Surgical decision-making for tibial tubercle avulsion fractures is heavily guided by the Ogden modification of the Watson-Jones classification system. This system categorizes fractures based on the anatomical location of the fracture line and the degree of displacement:
- Type I: Fracture through the secondary ossification center of the tibial tubercle.
- Type II: Fracture propagates proximally to the junction of the primary and secondary ossification centers.
- Type III: Fracture extends proximally through the primary ossification center into the knee joint (intra-articular).
- Type IV: Fracture extends posteriorly through the proximal tibial physis.
- Type V: Periosteal avulsion of the extensor mechanism from the secondary ossification center.
Modifiers "A" (non-displaced) and "B" (displaced) are applied to Types I-III.
Based on the advanced imaging, our patient presents with an Ogden Type IIIB fracture. The fracture line extends intra-articularly, and there is significant proximal and anterior displacement of the osseous fragment.
Indications for Operative Intervention
The indications for surgical intervention in this case are absolute. Non-operative management of an Ogden Type IIIB fracture would result in a catastrophic failure to restore the extensor mechanism, leading to a permanent extensor lag, profound quadriceps atrophy, and severe functional impairment.
Furthermore, the 4-millimeter intra-articular step-off violates the biomechanical principles of joint congruity. Failure to achieve anatomical reduction of the articular surface will inevitably lead to altered contact mechanics, accelerated cartilage wear, and early-onset post-traumatic osteoarthritis.
Finally, the impending risk of acute compartment syndrome necessitates immediate surgical decompression and stabilization. The operative strategy must therefore address three distinct goals: anatomical restoration of the articular surface, rigid biomechanical stabilization of the extensor mechanism, and prophylactic or therapeutic fasciotomy if compartment pressures remain elevated.
Surgical Technique and Intervention
Patient Positioning and Preparation
The patient is positioned supine on a radiolucent operating table. A high-thigh tourniquet is applied but not immediately inflated, allowing for accurate assessment of compartment pressures and vascularity. The entire affected lower extremity is prepped and draped in a standard sterile fashion. A sterile bump is placed under the ipsilateral hip to correct natural external rotation, and a radiolucent triangle is utilized to maintain the knee in approximately 30 degrees of flexion, which relaxes the tension on the extensor mechanism during the approach.
Surgical Approach and Decompression
An anterior longitudinal incision is utilized, centered over the tibial tubercle and extending proximally to the inferior pole of the patella and distally along the tibial crest. Subcutaneous dissection is performed to expose the paratenon, which is longitudinally incised.
Upon entering the fracture hematoma, a substantial volume of clotted blood is evacuated. If preoperative compartment pressures were elevated, a formal single-incision or dual-incision four-compartment fasciotomy is performed prior to fracture fixation. The anterior tibial recurrent artery is meticulously inspected; if actively bleeding or avulsed, it is identified and suture-ligated.
Fracture Preparation and Reduction
The avulsed tibial tubercle fragment is retracted proximally, exposing the fracture bed. The bed is meticulously debrided of all interposed soft tissue, periosteum, and organizing hematoma using a curette and copious pulsatile lavage.
Attention is then directed to the knee joint. A submeniscal arthrotomy is frequently required to visualize the articular extension of the fracture. The anterior horns of the medial and lateral menisci are carefully inspected. In Ogden Type III fractures, the menisci can become incarcerated within the fracture site, blocking anatomical reduction. Any entrapped meniscal tissue is carefully extracted using a nerve hook.
Reduction is achieved by extending the knee to 0 degrees to eliminate quadriceps tension. A pointed reduction forceps (Weber clamp) is applied, with one tine positioned on the proximal aspect of the avulsed fragment and the other on the posterior aspect of the proximal tibia. Gentle, progressive compression is applied until anatomical reduction of both the articular surface and the anterior cortical margin is achieved.
Fixation Construct
Once provisional reduction is confirmed via fluoroscopy in both the anteroposterior and lateral planes, definitive fixation is performed.
For an adolescent nearing skeletal maturity (14 years old), the risk of clinically significant growth arrest (genu recurvatum) from crossing the proximal tibial physis is minimal, as the anterior aspect of the physis is among the first to close. Therefore, rigid compression osteosynthesis is prioritized.
Two 4.5-millimeter partially threaded cannulated cancellous screws are utilized. Guide pins are advanced from anterior to posterior, perpendicular to the fracture plane. The proximal screw is positioned to capture the intra-articular fragment, ensuring it remains subchondral to avoid joint penetration. The distal screw secures the distal aspect of the tubercle.
Overdrilling of the anterior cortex is performed to achieve a lag effect. The screws are advanced over washers to prevent the screw heads from burying into the relatively soft apophyseal bone. Compression is achieved, and anatomical restoration of the articular surface is visually and fluoroscopically confirmed.
If there is significant comminution or a purely tendinous avulsion component (Type V variant), supplemental fixation with suture anchors placed into the proximal tibial metaphysis or a tension band wire construct may be required to neutralize the massive tensile forces of the quadriceps. Following fixation, the knee is ranged through a full arc of motion to confirm construct stability and the absence of impingement.
Post Operative Protocol and Rehabilitation
Phase One Early Immobilization
Immediately postoperatively, the knee is immobilized in full extension using a hinged knee brace locked at 0 degrees or a cylinder cast. The patient is made strictly non-weight-bearing on the operative extremity for the first two weeks to protect the soft tissue envelope and the initial stages of osseous healing.
Suture removal is performed at 14 days postoperatively. If the surgical wound is well-healed, the patient may transition to touch-down weight-bearing with bilateral axillary crutches, maintaining the brace locked in extension.
Phase Two Range of Motion Progression
At four weeks postoperatively, radiographic evaluation is performed to confirm the maintenance of reduction and assess for early callus formation. If stable, the rehabilitation protocol advances to Phase Two.
The hinged knee brace is unlocked to allow passive and active-assisted range of motion from 0 to 30 degrees. This arc is progressively increased by 15 to 30 degrees each week, guided by patient tolerance and radiographic progression. Active quadriceps contraction (straight leg raises) is initiated, but eccentric loading and open-chain kinetic exercises are strictly avoided to prevent catastrophic pull-out of the hardware. Weight-bearing is gradually advanced to partial weight-bearing.
Phase Three Strengthening and Return to Sport
By eight to twelve weeks postoperatively, assuming clinical and radiographic evidence of union, the patient is transitioned to full weight-bearing. The brace is discontinued.
Physical therapy focuses on closed-chain kinetic exercises, proprioceptive training, and aggressive restoration of quadriceps and hamstring strength. Return to competitive sports, particularly those involving explosive jumping and deceleration (e.g., basketball), is typically delayed until six to nine months postoperatively. Clearance is contingent upon the patient achieving at least 90% strength symmetry compared to the contralateral extremity on isokinetic testing, full pain-free range of motion, and complete radiographic consolidation of the fracture.
Clinical Pearls and Pitfalls
Pearls for the Orthopedic Surgeon
- Vascular Vigilance: Always maintain a high index of suspicion for anterior compartment syndrome. The avulsion of the tibial tubercle frequently tears the anterior tibial recurrent artery. Serial compartment examinations are mandatory, and a low threshold for fasciotomy should be maintained.
- Meniscal Entrapment: In Ogden Type III fractures, failure to achieve closed reduction is almost pathognomonic for meniscal entrapment. Do not forcefully compress the fracture without visualizing the joint line, as this can result in iatrogenic meniscal laceration.
- Hardware Selection: Utilize partially threaded screws with washers. The apophyseal bone in adolescents is highly cancellous and relatively soft; screw heads without washers will easily plunge through the near cortex, resulting in a loss of compression and construct failure.
- Address the Periosteum: The medial and lateral periosteal sleeves are often torn and retracted. Meticulous repair of these retinacular structures with heavy absorbable suture significantly augments the mechanical stability of the osseous fixation.
Pitfalls to Avoid
- Misdiagnosing a Sleeve Fracture: In younger patients (8-12 years), a seemingly minor osseous fleck on radiographs may represent a massive cartilaginous patellar sleeve fracture. Relying solely on radiographs without assessing the clinical extensor lag or obtaining an MRI can lead to a missed diagnosis and severe disability.
- Over-compression of Comminution: Applying excessive lag compression to a highly comminuted tubercle can cause the fragment to fragment further or shorten, altering the biomechanics of the patellofemoral joint. In comminuted cases, position screws or a tension band construct may be superior to pure lag technique.
- Ignoring the Physis in Younger Children: While the physis is less of a concern in a 14-year-old, placing large, threaded screws across the proximal tibial physis in an 11-year-old will inevitably cause a premature asymmetric physeal arrest, leading to a progressive genu recurvatum deformity. In younger patients, smooth Kirschner wires or suture anchors that do not cross the physis must be utilized.
