8 Pediatric Cases: Critical Decisions on Exits from the Physis
Key Takeaway
This topic focuses on 8 Pediatric Cases: Critical Decisions on Exits from the Physis, For a 7-year-old girl with a length-stable femur fracture, reduction and flexible nail fixation is the optimal treatment. The most common complication parents should be informed about is pain/irritation at insertion sites. While flexible nails are carefully positioned, understanding the implications of how hardware *exits from the physis* is critical in pediatric orthopedics to prevent potential growth abnormalities.
Detailed Patient Presentation and Mechanism of Injury
The patient is a 7-year-old female who presents to the emergency trauma bay as a transfer from an outside hospital following a high-energy blunt trauma event. The history obtained from the family and emergency medical services indicates that the child was playing tackle football with her older brothers when she sustained a direct, high-velocity impact to her right lower extremity. At the time of the collision, her right leg was reportedly planted while she was struck laterally by a significantly heavier opponent, generating a massive bending moment and axial load across the femoral diaphysis. This specific mechanism of injury is classic for producing transverse or short oblique fractures of the femoral shaft in the pediatric population, as the immature cortical bone is subjected to forces exceeding its ultimate tensile and compressive strength.
Upon initial evaluation at the outside facility, the patient exhibited a notable, gross deformity of the right thigh, accompanied by severe, intractable pain and inability to bear weight. The pre-hospital and outside hospital providers astutely recognized the diaphyseal femur fracture and immediately placed the patient in a Hare traction splint. The application of this traction splint is a critical initial step in the management of pediatric femur fractures; it serves to restore gross longitudinal alignment, dramatically reduce the intense muscle spasms originating from the robust quadriceps and hamstring compartments, and minimize ongoing hemorrhage into the capacious thigh compartments by decreasing the potential volume of the soft tissue envelope. She was subsequently transferred to our Level I pediatric trauma center for definitive orthopedic management.
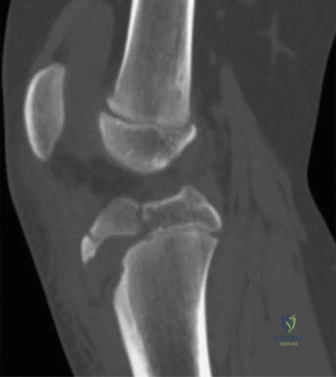
In the context of pediatric sports injuries, tackle football in a 7-year-old female introduces unique biomechanical forces on a rapidly growing skeleton. The pediatric femur is characterized by a thick, highly osteogenic periosteum and a relatively lower modulus of elasticity compared to adult bone. This means the bone can absorb a significant amount of energy and undergo more plastic deformation before catastrophic failure. However, when the energy threshold is surpassed, the resulting fracture often features a robust periosteal hinge that can be leveraged during reduction. The family reports that she is an otherwise healthy, highly active child with no prior medical history, no previous fractures, and no underlying metabolic bone diseases.
During the primary survey upon arrival at our facility, the nursing staff obtained an accurate body weight of 35 kilograms. In the realm of pediatric orthopedic trauma, the patient's age (7 years) and weight (35 kg) are not merely demographic details; they are the absolute, defining parameters that will dictate the entire surgical decision-making algorithm. A weight of 35 kg places her in a very specific biomechanical category where the forces acting across the femur are too substantial for conservative spica casting, yet her proximal femoral anatomy and open physes make adult-type rigid intramedullary nailing highly perilous. Understanding this delicate intersection of patient size, skeletal maturity, and fracture morphology is the hallmark of advanced pediatric orthopedic trauma care.
Comprehensive Clinical Examination Findings
Adhering strictly to Advanced Trauma Life Support (ATLS) protocols, the initial assessment focused on the ABCDEs to rule out life-threatening injuries. Despite the isolated nature of the orthopedic injury, a 35 kg child possesses a relatively small total circulating blood volume (approximately 70-80 mL/kg, yielding a total volume of roughly 2.5 to 2.8 liters). A diaphyseal femur fracture can easily sequester 10% to 20% of this volume within the thigh musculature. Fortunately, the patient remained hemodynamically stable throughout the evaluation, with a heart rate appropriate for her pain level, normotensive blood pressure, and excellent peripheral perfusion. Secondary survey revealed no abdominal tenderness, no chest wall crepitus, and a completely normal Glasgow Coma Scale score.
Local examination of the right lower extremity, performed after carefully loosening the traction splint straps to inspect the soft tissue envelope, revealed a tense, swollen right thigh with significant anterolateral ecchymosis. There were no open wounds, abrasions, or degloving injuries (Morel-Lavallée lesions) to suggest an open fracture or severe soft tissue compromise. While acute compartment syndrome of the thigh is an exceedingly rare clinical entity due to the large volume and compliance of the fascial compartments, the high-energy nature of the football tackle necessitated a rigorous assessment of compartment compressibility. The thigh compartments were firm but compressible, and the patient's pain, while severe, was proportional to the fracture and not indicative of the out-of-proportion ischemic pain seen in compartment syndrome.
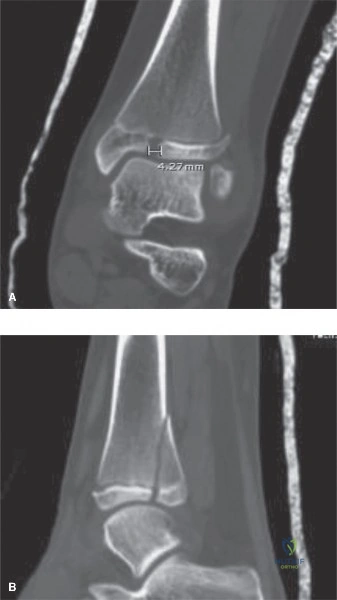
A meticulous neurovascular examination of the distal extremity was performed and documented. The dorsalis pedis and posterior tibial arteries were palpable and symmetric to the contralateral uninjured limb, with brisk capillary refill in the toes of less than two seconds. Motor function was assessed within the limits of pain; the patient was able to actively dorsiflex the ankle (extensor hallucis longus and tibialis anterior, deep peroneal nerve), plantarflex the ankle (gastrocnemius-soleus complex, tibial nerve), and demonstrate intact intrinsic foot musculature. Sensory examination confirmed intact light touch sensation across the sural, superficial peroneal, deep peroneal, saphenous, and tibial nerve distributions. This intact neurovascular status is crucial, as vascular injury, though rare, can occur with severe displacement of femur fractures, particularly in the distal third near the adductor hiatus.
Furthermore, a comprehensive musculoskeletal examination of the adjacent joints and the contralateral extremity was executed. The ipsilateral knee and hip joints were carefully palpated for effusions, ligamentous laxity, or localized tenderness. In high-energy pediatric femur fractures, one must maintain a high index of suspicion for concomitant injuries, such as an ipsilateral femoral neck fracture or a ligamentous disruption of the knee, which can be easily masked by the dramatic presentation of the shaft fracture. The pelvis was stable to AP and lateral compression. The uninjured extremities demonstrated full, painless active and passive range of motion. Finally, although the history of a football tackle provided a clear mechanism, the orthopedic surgeon must always maintain a vigilant mindset regarding non-accidental trauma (NAT); however, the fracture pattern, patient age, and consistent history provided by multiple witnesses made NAT highly unlikely in this specific scenario.
Advanced Imaging and Diagnostics
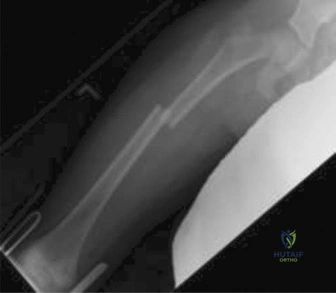
The radiographic evaluation of a pediatric femur fracture must be systematic and comprehensive, ensuring that the entire bone, as well as the joints above and below, are adequately visualized. The initial radiographs obtained at the outside hospital (Figure 10-10) demonstrated a displaced, transverse to short-oblique fracture of the middle third of the right femoral diaphysis. There was significant overriding of the fracture fragments, indicative of the powerful deforming forces exerted by the thigh musculature. The proximal fragment was held in flexion, abduction, and external rotation by the unopposed pull of the iliopsoas, gluteus medius, and short external rotators, respectively. The distal fragment was drawn proximally and into varus by the adductors and the hamstring/quadriceps complex.
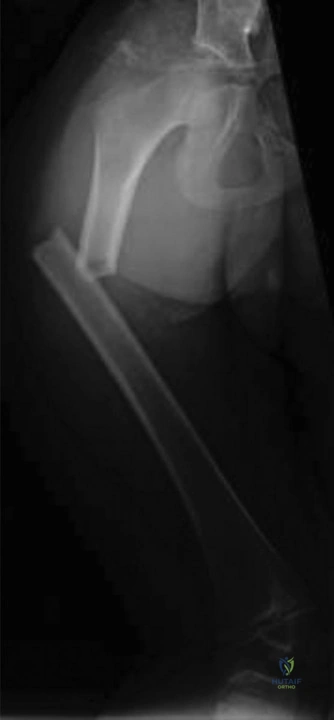
Upon arrival at our trauma center, portable radiographs were obtained with the patient remaining in the traction splint (Figure 10-11). These in-traction films are exceptionally valuable for several reasons. First, they allow the surgeon to assess the "personality" of the fracture once the gross overriding has been reduced. In this case, the traction films confirmed that the fracture was length-stable; meaning, once pulled out to length, the cortical ends could be opposed without a massive comminuted segment that would lead to telescoping. Second, these films help rule out any subtle, non-displaced extensions of the fracture line into the proximal or distal metaphysis that might have been obscured by the initial deformity. The alignment in traction showed excellent restoration of length and a significant improvement in the angular deformity.
In the context of isolated, closed, diaphyseal femur fractures in pediatric patients, advanced cross-sectional imaging such as Computed Tomography (CT) or Magnetic Resonance Imaging (MRI) is rarely indicated. The standard anteroposterior (AP) and lateral radiographs of the femur, supplemented by dedicated AP pelvis and AP/lateral knee views, provide all the necessary information for surgical planning. CT scans involve a significant dose of ionizing radiation and are generally reserved for highly complex, intra-articular fractures, severe comminution where external fixation is planned, or when there is a high suspicion of a pathological fracture that requires detailed assessment of the bony architecture. In this healthy 7-year-old, the radiographic appearance was classically traumatic, with healthy-appearing cortical bone and no evidence of lytic lesions, periosteal reaction, or abnormal medullary expansion.
Pre-operative templating is a critical phase of the diagnostic workup, particularly when planning for flexible intramedullary nailing. The surgeon must carefully measure the narrowest diameter of the femoral medullary canal, known as the isthmus, on both the AP and lateral radiographic views. The fundamental biomechanical principle of titanium elastic nails (TENs) dictates that the combined diameter of the two chosen nails should fill approximately 80% of the narrowest portion of the canal. Therefore, the formula used is: (Canal Diameter at Isthmus × 0.4) = Individual Nail Diameter. For example, if the isthmus measures 9 millimeters, the ideal nail size would be 3.5 mm or 4.0 mm. Templating also involves assessing the canal diameter at the planned entry points in the distal metaphysis to ensure that the bone can accommodate the insertion of the nails without iatrogenic fracturing.
Exhaustive Differential Diagnosis
When evaluating a pediatric patient with a deformed, painful thigh following trauma, the primary diagnosis of a diaphyseal femur fracture is usually clinically obvious and radiographically straightforward. However, the orthopedic surgeon must approach every case with a broad differential diagnosis to avoid missing concomitant injuries, underlying pathological conditions, or alternative fracture patterns that dictate vastly different treatment algorithms. The differential diagnosis must encompass not only traumatic etiologies but also congenital, metabolic, and neoplastic conditions that can predispose the pediatric femur to failure under loads that would normally be well-tolerated.
The most critical alternative diagnosis to consider is a pathological fracture through a pre-existing benign or malignant bone lesion. In the pediatric population, unicameral bone cysts (UBCs), aneurysmal bone cysts (ABCs), and non-ossifying fibromas (NOFs) are common benign lesions that can weaken the cortical integrity of the femur. Malignant lesions, such as osteosarcoma or Ewing sarcoma, must also be considered, particularly if the patient reports a history of antecedent pain prior to the traumatic event, or if the radiographs demonstrate permeative bone destruction, a wide zone of transition, or an aggressive periosteal reaction (e.g., Codman's triangle or a "sunburst" appearance). In our 7-year-old patient, the radiographs demonstrated pristine, thick cortical bone, rendering a pathological fracture highly improbable.
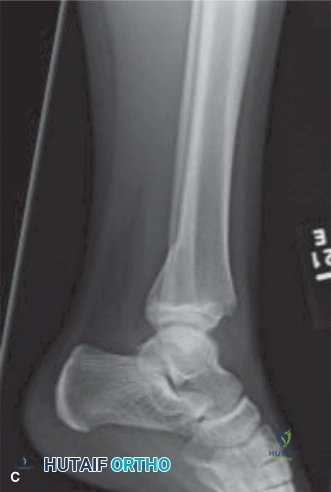
Another crucial differential consideration is an ipsilateral femoral neck fracture or a distal femoral physeal fracture (Salter-Harris injuries). Femoral neck fractures in children are high-energy injuries associated with a devastatingly high rate of avascular necrosis (AVN) of the femoral head due to the tenuous blood supply traversing the femoral neck. These fractures must be aggressively identified and treated, often taking precedence over the shaft fracture. Distal femoral physeal injuries can mimic shaft fractures clinically but occur at the level of the growth plate. These require precise anatomical reduction and fixation (often with smooth K-wires or screws that do not cross the physis in a compression mode) to minimize the risk of premature physeal closure and subsequent limb length discrepancies or angular deformities.
Furthermore, while the history of a tackle football injury in a 7-year-old is highly plausible, the surgeon must always keep Non-Accidental Trauma (NAT) on the differential diagnosis for any pediatric fracture. Femur fractures in children who are not yet of walking age (typically <1 year) are highly suspicious for child abuse. In a 7-year-old, the index of suspicion is lower, but the clinician must remain observant for inconsistencies in the history, delayed presentation to care, or the presence of multiple fractures in various stages of healing.
Diagnostic Comparison Table
| Pathology / Injury | Clinical Presentation | Radiographic Hallmarks | Primary Treatment Modality | Prognostic Concerns |
|---|---|---|---|---|
| Traumatic Diaphyseal Femur Fracture | Acute severe pain, gross deformity, clear high-energy mechanism (e.g., tackle football). | Transverse, oblique, or spiral fracture of the shaft; normal bone density. | Age/weight dependent: Pavlik, Spica, Flexible Nails, or Rigid Nails. | Limb length discrepancy (overgrowth), malunion. |
| Pathological Fracture (Benign Cyst) | Mild antecedent pain, fracture occurs with low-energy or trivial trauma. | Lytic lesion, thin cortices, "fallen leaf" sign in UBCs. | Treat the fracture first (often conservative or flexible nails), then address the cyst. | Recurrence of cyst, delayed union, need for bone grafting. |
| Distal Femoral Physeal Fracture | Swelling localized to the knee, hemarthrosis, pain with knee range of motion. | Fracture line extending through the physis (Salter-Harris classification). | Closed or open reduction, smooth K-wire or screw fixation avoiding physeal compression. | High rate of premature physeal closure, angular deformity. |
| Pediatric Femoral Neck Fracture | Groin pain, shortened and externally rotated limb, high-energy trauma. | Disruption of the femoral neck, Delbet classification. | Urgent open or closed reduction and stable internal fixation (screws/pins). | Avascular necrosis (AVN) of the femoral head, coxa vara. |
Complex Surgical Decision Making and Classifications
The surgical decision-making process for pediatric femur fractures is one of the most highly algorithmic and protocol-driven areas in orthopedic trauma. The treatment of choice is dictated by a complex interplay between the patient's chronological age, physiological weight, fracture pattern (length stable vs. unstable), and associated injuries (polytrauma vs. isolated). The American Academy of Orthopaedic Surgeons (AAOS) Clinical Practice Guidelines provide a robust framework for these decisions. For infants less than 6 months of age, a Pavlik harness or simple splinting is highly effective due to the massive remodeling potential of the infant skeleton. For children between 6 months and 4-5 years of age, early spica casting (with or without a brief period of traction) remains the gold standard, offering excellent outcomes with minimal surgical risk.
However, as children grow older, heavier, and more muscular, the efficacy of spica casting rapidly diminishes. In our patient—a 7-year-old girl weighing 35 kg—spica casting is strongly contraindicated as a primary treatment. A 35 kg child in a spica cast presents a monumental logistical and physical burden for the family regarding hygiene, transportation, and positioning. Furthermore, the sheer muscle mass of a 35 kg 7-year-old can easily overpower the cast, leading to a high risk of loss of reduction, unacceptable shortening, and angular malunion. Traction followed by delayed spica casting (Option 3 in the seed content) is an antiquated approach that forces the child into prolonged hospitalization, increasing the risk of psychological distress, nosocomial infections, and significant financial burden, while offering no superior orthopedic outcome.
Conversely, adult-style rigid intramedullary nailing is equally inappropriate for this patient. The use of a lateral trochanteric entry or piriformis fossa entry rigid nail in a 7-year-old carries unacceptable risks. The vascular supply to the pediatric femoral head is highly vulnerable; a piriformis entry point has historically been associated with devastating rates of iatrogenic avascular necrosis (AVN). Even a lateral trochanteric entry nail, which is indicated for children over 9-11 years of age or weighing more than 49 kg, risks damaging the greater trochanteric apophysis in a 7-year-old. Arrest of this apophysis while the capital femoral physis continues to grow results in a progressive coxa valga deformity and a shortened femoral neck. Therefore, rigid nailing must be strictly avoided in this age and weight bracket.
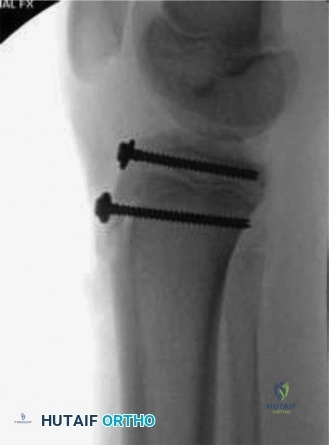
This leaves Flexible Intramedullary Nailing (FIN), also known as Titanium Elastic Nails (TENs), as the absolute treatment of choice. FIN is specifically indicated for children aged 5 to 11 years, weighing less than 49 kg, with length-stable diaphyseal fractures. FIN operates on the biomechanical principle of three-point fixation and symmetric, opposing bending moments. Two pre-bent titanium nails are inserted retrogradely from the distal metaphysis, crossed within the medullary canal, and impacted into the proximal metaphysis. This construct provides excellent rotational and angular stability while allowing for micro-motion at the fracture site, which robustly stimulates secondary bone healing via endochondral ossification. External fixation (Option 5) is reserved strictly for damage control orthopedics in hemodynamically unstable polytrauma, severe open fractures with massive soft tissue loss, or highly comminuted fractures where FIN cannot maintain length.
Step-by-Step Surgical Technique and Intervention
The execution of Flexible Intramedullary Nailing requires meticulous attention to detail, as the success of the procedure relies heavily on precise biomechanical principles rather than rigid metallic strength. The patient is brought to the operating room and placed under general anesthesia. For a 35 kg child, positioning can be achieved on a radiolucent flat table with the limb draped free, allowing an assistant to apply manual traction, or on a small pediatric fracture table. The fracture table allows for sustained, controlled traction and facilitates obtaining orthogonal fluoroscopic views without fighting the patient's weight or moving the limb excessively. The entire right lower extremity from the iliac crest to the toes is prepped and draped in a standard sterile fashion.
Nail selection and contouring constitute the most critical phase of the operation. Based on our pre-operative templating, if the isthmus measures 9 mm, two 3.5 mm titanium nails are selected. The nails must be of identical diameter to ensure that the bending moments they generate within the canal are symmetrical; mismatched nails will cause the construct to deviate toward the stronger nail, resulting in varus or valgus malalignment. The nails are then manually contoured by the surgeon to create a smooth, continuous bow. The apex of this bow must be positioned exactly at the level of the fracture site once inserted. The maximum height of the bow should be approximately three times the diameter of the medullary canal. This contouring ensures that the nails exert continuous outward pressure against the inner cortices, maintaining the three-point fixation.
The entry points are established in the distal femoral metaphysis, strictly avoiding the distal femoral physis. Under fluoroscopic guidance, a starting point is identified on both the medial and lateral aspects of the distal femur, approximately 2.5 to 3.0 centimeters proximal to the radiolucent physeal line. Small 2 cm longitudinal incisions are made, and the soft tissues are bluntly dissected down to the bone. An awl or drill is used to breach the cortex. The trajectory of the opening is crucial; it must be angled proximally at approximately 45 degrees to allow smooth passage of the nails into the canal without creating a stress riser that could lead to an iatrogenic supracondylar fracture.
The contoured nails are mounted onto a T-handle chuck and inserted retrogradely. The lateral nail is typically advanced first, followed by the medial nail, bringing both up to the level of the fracture. The fracture is then reduced using longitudinal traction and manipulation. The nails are advanced across the fracture site using a combination of impaction and a "corkscrew" twisting motion to navigate the medullary canal. It is imperative that the nails cross each other proximal or distal to the fracture site, never exactly at the fracture line, to maximize stability. The nails are driven into the proximal metaphysis, with the tips diverging—one anchoring in the greater trochanteric region and the other in the femoral neck region, carefully staying distal to the capital femoral physis. Finally, the distal ends of the nails are cut, leaving approximately 1-2 cm protruding from the cortex to facilitate future removal, but bent slightly away from the IT band and soft tissues to minimize post-operative irritation.
Strict Post-Operative Protocol and Rehabilitation Stages
The immediate post-operative period focuses on pain management, mobilization, and vigilant monitoring for complications. Because FIN utilizes a minimally invasive technique, the surgical trauma to the soft tissue envelope is minimal. However, the fracture itself remains a significant source of pain. Intravenous analgesics are transitioned to oral medications as quickly as tolerated. The neurovascular status of the limb is monitored closely, with particular attention paid to the compartments of the thigh and leg, although the risk of compartment syndrome decreases significantly once the fracture is stabilized and length is restored. Most patients, including our 7-year-old, are comfortable enough to be discharged home on post-operative day 1 or 2.
Unlike rigid intramedullary nailing in adults, which often allows immediate full weight-bearing, the flexible nail construct in a pediatric patient requires a more protected rehabilitation protocol. The construct relies heavily on the intact periosteal hinge and the surrounding muscle envelope for stability. Therefore, the patient is typically made toe-touch weight-bearing (TTWB) or partial weight-bearing (PWB) with the assistance of crutches or a pediatric walker for the first 4 to 6 weeks. Physical therapy is initiated immediately to maintain range of motion in the hip, knee, and ankle, preventing the stiffness that can rapidly develop in pediatric patients. Early knee range of motion is particularly important to prevent adhesions of the quadriceps mechanism over the distal nail insertion sites.

Clinical and radiographic follow-up is rigorously scheduled. The first post-operative visit occurs at 10 to 14 days for wound evaluation and suture removal. Subsequent visits are typically at 4, 8, and 12 weeks. Radiographs are obtained at these intervals to assess the progression of callus formation. Pediatric bone heals rapidly; abundant bridging callus is usually visible by 4 to 6 weeks, at which point the patient can be transitioned to full weight-bearing as tolerated. During these follow-up visits, the surgeon must carefully measure clinical leg lengths. A well-documented phenomenon in pediatric femur fractures, particularly in children aged 2 to 10 years, is post-traumatic overgrowth. The hyperemia associated with fracture healing stimulates the ipsilateral physes, leading to an average overgrowth of 1 to 2 centimeters over the following year.
The final stage of the protocol involves the removal of the titanium elastic nails. Unlike adult implants, which are often left in situ permanently unless symptomatic, FINs are routinely removed. The protruding distal ends of the nails frequently cause soft tissue irritation, bursa formation, or pain with deep knee flexion. Furthermore, leaving implants in a growing skeleton can complicate future orthopedic interventions if
