9 Pediatrics Cases: Essential Insights on Rotation of the Foot
Key Takeaway
Looking for accurate information on 9 Pediatrics Cases: Essential Insights on Rotation of the Foot? Tibial tubercle fractures are more common in adolescents with Osgood–Schlatter disease, an overuse injury. A significant risk with this fracture is anterior compartment syndrome, potentially involving the recurrent anterior tibial artery. These injuries often occur during sports activities requiring sudden, forceful knee extension or impacts, which can sometimes involve quick acceleration combined with rotation of the foot.
Detailed Patient Presentation and Mechanism of Injury
We are presenting the highly instructive case of a 14-year-old adolescent male who was urgently transferred to our Level I trauma center from an outside emergency department. The patient presented with acute, severe right knee pain and an absolute inability to bear weight following a traumatic event sustained while playing basketball. According to the history obtained from the patient and his parents, the injury occurred when he aggressively planted his foot and forcefully contracted his quadriceps to initiate a jump for a rebound, experiencing an immediate, audible "pop" accompanied by a sudden giving-way of the right lower extremity. This classic mechanism of injury—an explosive, eccentric contraction of the quadriceps muscle complex against a fixed, planted tibia—places an extraordinary tensile load across the extensor mechanism, specifically targeting the weakest link in the adolescent knee: the maturing apophysis of the tibial tubercle.
To fully appreciate the pathophysiology of this injury, one must understand the unique developmental anatomy of the proximal tibia in the adolescent population. The tibial tubercle develops from a secondary ossification center that initially forms as fibrocartilage before undergoing endochondral ossification. During the critical developmental window between 13 and 15 years of age in males, the physis of the tibial tubercle is in a transitional state, gradually closing from proximal to distal. This transitional phase renders the apophysis highly vulnerable to tensile failure. The structural integrity of the tubercle relies heavily on the perichondrium and the surrounding periosteal sleeve. When the force generated by the quadriceps exceeds the tensile strength of the maturing physeal cartilage, catastrophic failure occurs, resulting in an avulsion fracture of the tibial tubercle.
Crucially, upon further detailed history-taking, the patient reported a prolonged, six-month prodromal history of localized anterior knee pain, swelling, and tenderness directly over the tibial tubercle, which was classically exacerbated by running and jumping sports. This clinical picture is the hallmark of Osgood-Schlatter disease, a chronic traction apophysitis. Osgood-Schlatter disease is widely considered a significant predisposing risk factor for acute tibial tubercle avulsion fractures. The repetitive microtrauma and chronic inflammation associated with this condition disrupt the normal architecture of the secondary ossification center, replacing organized columnar cartilage with disorganized, mechanically inferior fibrovascular tissue. This chronic weakening dramatically lowers the threshold for acute failure when the apophysis is subsequently subjected to a sudden, massive eccentric load.
The transfer records from the outside hospital indicated that the patient had been initially evaluated, splinted, and imaged before being sent to our facility due to the lack of an available operating room and the complex nature of the injury. The recognition of the severity of this injury by the outside facility was appropriate, as tibial tubercle avulsion fractures are not merely osseous injuries; they are profound disruptions of the extensor mechanism that carry a substantial risk for devastating soft tissue and neurovascular complications. The immediate goal upon his arrival at our trauma bay was to rapidly assess the integrity of the soft tissue envelope, definitively rule out impending compartment syndrome, and formulate a comprehensive operative plan for anatomic restoration of the extensor mechanism.
Comprehensive Clinical Examination Findings
Upon arrival at our emergency department, the patient was resting in a long leg splint, appearing visibly uncomfortable but hemodynamically stable. Removal of the splint revealed a grossly swollen right knee with a pronounced effusion and a visible structural deformity over the anterior aspect of the proximal tibia. The patella was clinically high-riding (patella alta), and a distinct, palpable step-off and soft tissue defect could be appreciated immediately distal to the inferior pole of the patella, corresponding to the avulsed tibial tubercle fragment. The overlying skin was tense and ecchymotic, but importantly, there was no frank tenting of the skin or impending necrosis, which can sometimes occur if a large, sharp osseous fragment is severely displaced and entrapped within the subcutaneous tissues.
The functional assessment of the extensor mechanism was unequivocally compromised. The patient was completely unable to perform a straight leg raise or actively extend the knee against gravity, confirming a full-thickness functional disruption of the extensor apparatus. While this is an expected finding in a displaced tibial tubercle avulsion, it is a critical clinical data point that mandates surgical intervention. Passive range of motion was severely limited by pain and apprehension, and any attempt to flex the knee exacerbated the tension on the anterior soft tissues. The collateral ligaments and cruciate ligaments appeared grossly stable, though a comprehensive ligamentous examination is notoriously difficult in the acute setting of a massive hemarthrosis and severe pain.
The most critical aspect of the physical examination in this specific clinical scenario is the meticulous and repeated assessment of the neurovascular status, with a hyper-focus on the compartments of the lower leg. The patient was currently neurovascularly intact, demonstrating strong, symmetric dorsalis pedalis and posterior tibial pulses, normal capillary refill, and intact sensation in the deep peroneal, superficial peroneal, tibial, and sural nerve distributions. He had full active dorsiflexion and plantarflexion of the toes. However, the soft tissues over the anterior compartment were noticeably firm. This is the paramount clinical trap in tibial tubercle fractures: the insidious development of acute anterior compartment syndrome.
The anatomical basis for this severe complication lies in the vascular supply to the proximal tibia. The recurrent anterior tibial artery branches from the anterior tibial artery just after it passes through the interosseous membrane, coursing superiorly and laterally over the anterior tibia to supply the proximal tibiofibular joint and the anterolateral capsule of the knee. In the setting of a displaced tibial tubercle fracture, this artery or its branches are highly susceptible to tearing. Because the robust fascial boundaries of the anterior compartment often remain intact despite the fracture, arterial bleeding rapidly accumulates within the confined space of the anterior compartment. We admitted the patient directly to the orthopedic floor, elevated the limb, and instituted strict, serial neurovascular checks every two hours, recognizing that anterior compartment syndrome can develop rapidly and requires emergent surgical decompression to prevent irreversible ischemic necrosis of the extensor hallucis longus and tibialis anterior muscles.
Advanced Imaging and Diagnostics
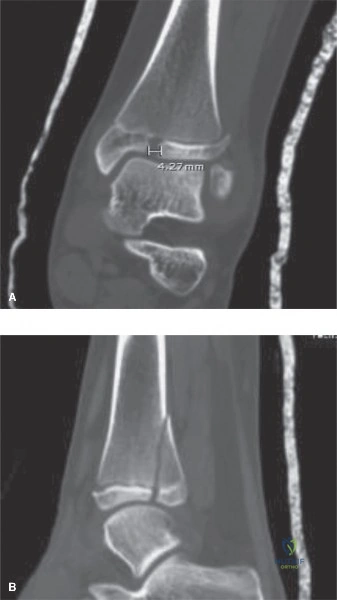
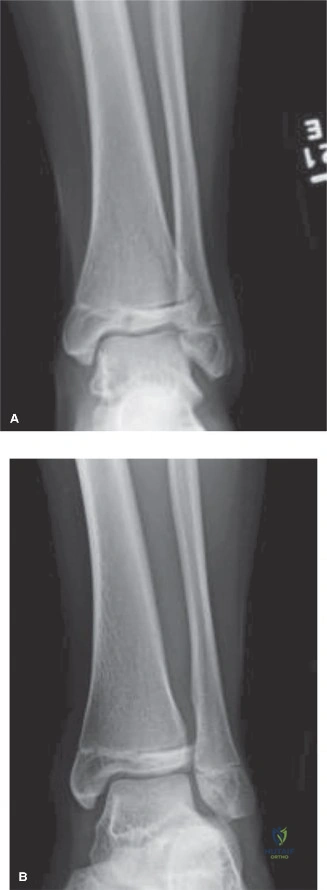
Standard orthogonal plain radiographs of the right knee (anteroposterior and lateral views) were the first step in the diagnostic algorithm. The lateral radiograph is particularly illustrative in these injuries, clearly demonstrating the avulsed osseous fragment of the tibial tubercle migrated proximally due to the unopposed pull of the quadriceps tendon. The Insall-Salvati ratio, measured on the lateral film with the knee flexed to 30 degrees, was greater than 1.2, confirming the presence of patella alta secondary to the distal detachment of the patellar tendon footprint. The AP radiograph was useful for assessing any medial or lateral translation of the fragment and for ruling out associated plateau fractures, though the tubercle itself is often obscured by the complex overlapping anatomy of the proximal tibia on this view.
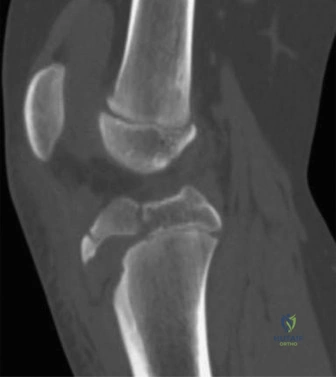
Given the complexity of the fracture pattern and the need for precise preoperative planning, a computed tomography (CT) scan with multiplanar reconstructions had been appropriately obtained at the outside hospital. The CT scan is invaluable for fully characterizing the three-dimensional anatomy of the fracture. In this specific case, the axial and sagittal CT cuts meticulously delineated the extent of the fracture line. It allowed us to accurately measure the size of the avulsed fragment, assess the degree of comminution, and, most importantly, determine if the fracture line extended proximally into the articular surface of the knee joint. Intra-articular extension dramatically alters the surgical approach, as anatomic reduction of the joint surface becomes a primary objective to prevent premature post-traumatic osteoarthritis.
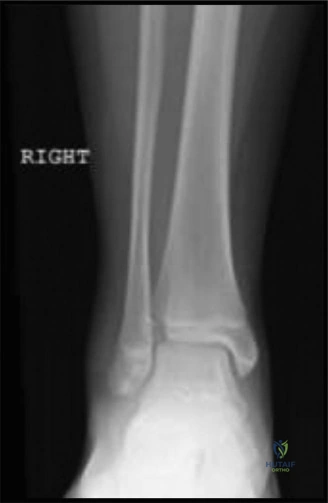
While Magnetic Resonance Imaging (MRI) is not routinely indicated in the acute management of isolated tibial tubercle avulsion fractures, it can be a highly useful adjunct if there is high clinical suspicion for concomitant soft tissue injuries. In complex, high-energy variants, MRI can identify associated meniscal tears, particularly entrapment of the anterior horn of the lateral meniscus within the fracture gap, which is a known block to anatomic reduction. Furthermore, MRI can definitively evaluate the integrity of the patellar tendon itself, ensuring that the injury is purely an osseous avulsion rather than a combined osseous and tendinous rupture. In our patient, the CT and plain films provided sufficient osseous detail to proceed with surgical planning without the need for an acute MRI.
Preoperative templating was performed using the digital imaging software to determine the optimal trajectory and length of the fixation hardware. We planned for the use of 4.0 mm or 4.5 mm partially threaded cannulated cancellous screws. The templating process involved measuring the depth of the proximal tibia at the level of the tubercle to ensure the screws would achieve adequate purchase in the posterior tibial cortex without plunging into the popliteal fossa, thereby avoiding iatrogenic injury to the neurovascular bundle. We also evaluated the status of the proximal tibial physis; given the patient's age of 14, the physis was nearing the end of its growth potential, which influenced our decision regarding the placement of hardware across the growth plate.
Exhaustive Differential Diagnosis
When evaluating an adolescent patient presenting with acute anterior knee pain, swelling, and an inability to extend the knee, the differential diagnosis must encompass the entire spectrum of extensor mechanism disruptions, as well as acute exacerbations of chronic overuse syndromes. While the clinical presentation of a displaced tibial tubercle avulsion is often dramatic and radiographically obvious, subtle or non-displaced variants require a high index of suspicion and careful differentiation from other pathologies. The primary entities to consider include patellar sleeve fractures, acute ruptures of the patellar tendon, Osgood-Schlatter disease, and Sinding-Larsen-Johansson syndrome.
Patellar sleeve fractures are a distinct pediatric injury characterized by an avulsion of a large sleeve of unossified cartilage from the inferior pole of the patella, often accompanied by a tiny, radiographically subtle fleck of bone. Clinically, these patients present similarly with a loss of active extension and patella alta. However, the pathology lies at the proximal origin of the patellar tendon rather than its distal insertion. Missing a patellar sleeve fracture is a significant pitfall, as the cartilaginous nature of the avulsed fragment can lead to gross underestimation of the injury severity on plain radiographs, potentially resulting in inappropriate conservative management and catastrophic elongation of the extensor mechanism.
Osgood-Schlatter disease and Sinding-Larsen-Johansson syndrome are chronic traction apophysitides that must be differentiated from acute traumatic avulsions. Osgood-Schlatter affects the tibial tubercle, while Sinding-Larsen-Johansson affects the inferior pole of the patella. Both present with localized pain, swelling, and tenderness exacerbated by activity. However, unlike acute avulsion fractures, these chronic conditions do not typically present with an acute loss of the extensor mechanism or a sudden, dramatic "giving way" episode. Radiographically, they demonstrate fragmentation and sclerosis of the apophysis, but not the gross displacement seen in acute fractures. It is critical to recognize, as in our patient's case, that a history of Osgood-Schlatter disease serves as a major risk factor for an acute avulsion event.
Finally, pure tendinous ruptures of the patellar or quadriceps tendons, while more common in adults, can occasionally occur in the adolescent population, often in the setting of systemic conditions (e.g., systemic lupus erythematosus, chronic corticosteroid use) or extreme localized trauma. These present with a palpable defect in the tendon itself rather than at the osseous insertion sites. Ultrasonography or MRI is often required to definitively diagnose a mid-substance tendon rupture in the absence of osseous avulsion.
Differential Diagnosis Comparison Table
| Condition | Patient Demographic | Pathoanatomy | Imaging Findings | Clinical Presentation |
|---|---|---|---|---|
| Tibial Tubercle Avulsion | Adolescent males (13-16 yrs), jumping sports | Acute osseous avulsion of the tibial tubercle apophysis | Displaced bony fragment from anterior tibia, patella alta | Acute severe pain, palpable defect at tubercle, inability to actively extend knee |
| Patellar Sleeve Fracture | Children (8-12 yrs) | Cartilaginous avulsion from the inferior pole of the patella | Small bony fleck inferior to patella, patella alta, large cartilaginous gap on MRI | Acute pain, palpable defect at inferior patellar pole, loss of active extension |
| Osgood-Schlatter Disease | Adolescents (10-15 yrs), highly active | Chronic traction apophysitis of the tibial tubercle | Fragmentation, sclerosis, and enlargement of the tibial tubercle | Chronic, activity-related anterior knee pain, prominent tubercle, intact extension |
| Sinding-Larsen-Johansson | Children/Adolescents (10-14 yrs) | Chronic traction apophysitis of the inferior pole of patella | Fragmentation and calcification at the inferior patellar pole | Chronic pain at inferior patella, exacerbated by jumping, intact extension |
Complex Surgical Decision Making and Classifications
The surgical decision-making process for tibial tubercle avulsion fractures is heavily guided by the Ogden classification system, which is a modification of the original Watson-Jones classification. The Ogden system categorizes these injuries based on the anatomic location and proximal extent of the fracture line, which directly dictates the surgical approach and fixation strategy. Type I fractures involve an avulsion of the distal portion of the tubercle, distal to the physis. Type II fractures extend proximally into the physis, bridging the secondary ossification center. Type III fractures are the most severe, extending proximally through the epiphysis and into the articular surface of the knee joint. Each of these types can be further subclassified as 'A' (non-displaced) or 'B' (displaced).

Our patient presented with an Ogden Type III-B fracture. The CT scan clearly demonstrated the fracture line extending proximally through the epiphysis and violating the articular surface of the tibial plateau, with significant anterior and proximal displacement of the fragment. The indications for operative intervention in this scenario are absolute. Non-operative management of a displaced Type III fracture would inevitably lead to a nonunion or malunion of the extensor mechanism, resulting in a profound extensor lag, profound weakness, and early-onset, rapidly progressive patellofemoral and tibiofemoral osteoarthritis due to the articular step-off. The surgical goals are to achieve anatomic reduction of the articular surface, restore the functional length of the extensor mechanism, and provide rigid internal fixation to allow for early mobilization.
A critical, often-debated aspect of the surgical plan for this specific injury is the decision regarding prophylactic anterior compartment fasciotomy. As previously discussed, the recurrent anterior tibial artery is at high risk of injury. The literature is replete with case reports of patients developing devastating anterior compartment syndrome in the immediate postoperative period following fixation of a tibial tubercle fracture. Because the surgical approach requires an anterior incision directly over the compartment, many trauma surgeons, including myself, advocate for a limited, prophylactic release of the anterior compartment fascia at the time of internal fixation. This adds minimal morbidity to the procedure but provides an absolute safeguard against a catastrophic ischemic complication that could result in a permanent foot drop and loss of anterior compartment musculature.
Hardware selection is another crucial preoperative decision. The standard of care for displaced tibial tubercle fractures is open reduction and internal fixation (ORIF) using partially threaded cancellous screws. The use of cannulated systems is preferred, as it allows for precise provisional fixation with K-wires before definitive drilling and screw placement. Depending on the size of the fragment, two or three 4.0 mm or 4.5 mm screws are typically utilized. Washers may be employed if the anterior cortex of the avulsed fragment is comminuted or osteopenic, to prevent the screw heads from burying into the bone and losing compression. In cases where the fragment is highly comminuted or the patient is exceptionally large, augmenting the screw fixation with a figure-of-eight tension band wire construct may be necessary to neutralize the massive tensile forces of the quadriceps.
Step-by-Step Surgical Technique and Intervention
The patient was brought to the operating room and placed supine on a radiolucent Jackson table. After the induction of general anesthesia, a thorough examination under anesthesia (EUA) was performed to confirm the complete loss of the extensor mechanism and to assess for any subtle ligamentous laxity that was masked by guarding in the ER. A non-sterile tourniquet was placed high on the right thigh. The operative extremity was meticulously prepped and draped in the standard sterile orthopedic fashion. The limb was exsanguinated using an Esmarch bandage, and the tourniquet was inflated to 250 mmHg to ensure a bloodless surgical field, which is critical for identifying the articular surface and the delicate anatomical structures.
An anterior longitudinal incision was utilized, centered over the tibial tubercle and extending slightly laterally to avoid placing the surgical scar directly over the bony prominence of the tibial crest, which can cause significant discomfort when kneeling postoperatively. The subcutaneous tissues were sharply dissected to expose the deep fascia. A massive fracture hematoma was immediately encountered and evacuated using suction and careful curettage. This exposure revealed the completely avulsed tibial tubercle fragment, which was retracted proximally by the patellar tendon. The periosteal sleeve was found to be extensively torn both medially and laterally.
Because this was an Ogden Type III fracture with intra-articular extension, the joint capsule was carefully opened to inspect the articular surface. We specifically visualized the anterior horn of the lateral meniscus to ensure it was not entrapped within the fracture site. The fracture bed on the proximal tibia was irrigated and meticulously debrided of any interposed periosteum, organizing hematoma, or small, non-viable chondral fragments that would impede an anatomic reduction. The knee was then placed in full extension to completely relax the quadriceps and the extensor mechanism, significantly facilitating the reduction maneuver.
Using a pointed Weber reduction clamp, the avulsed fragment was anatomically reduced to its native footprint on the proximal tibia. The reduction was provisionally held with two parallel 1.6 mm Kirschner wires directed from anterior to posterior. Fluoroscopic imaging in both the AP and lateral planes confirmed an absolutely anatomic reduction of both the tibial tubercle and the intra-articular extension. We then proceeded with definitive fixation using two 4.5 mm partially threaded cannulated cancellous screws with washers. The screws were placed over the K-wires, ensuring they engaged the dense posterior cortex of the tibia for maximum pull-out strength. The K-wires were subsequently removed, and final fluoroscopic images confirmed excellent hardware placement and compression across the fracture site.
Following definitive osseous fixation, we addressed the soft tissues. A crucial step in this procedure was the prophylactic release of the anterior compartment. A small incision was made in the anterior fascial compartment, and using dissecting scissors, the fascia was released longitudinally for a distance of approximately 10 centimeters. This prophylactic fasciotomy effectively eliminates the risk of postoperative compartment syndrome. Finally, the massive medial and lateral periosteal tears were meticulously repaired using heavy, absorbable #1 Vicryl sutures. This periosteal repair is vital for restoring the secondary restraints of the extensor mechanism and promoting rapid biologic healing. The wound was copiously irrigated and closed in layers, utilizing a subcuticular Monocryl stitch for the skin. The patient was placed in a hinged knee brace locked in full extension before the tourniquet was deflated.
Strict Post-Operative Protocol and Rehabilitation Stages
The immediate postoperative phase (Weeks 0-2) is focused entirely on protecting the surgical repair, managing edema, and preventing complications. The patient was admitted for 24 hours of observation, primarily to ensure adequate pain control and to monitor the neurovascular status, despite the prophylactic fasciotomy. The hinged knee brace was locked in absolute full extension (0 degrees) at all times, including during sleep. The patient was instructed to remain strictly non-weight-bearing (NWB) on the operative extremity, utilizing bilateral axillary crutches for all mobility. Cryotherapy and strict limb elevation were heavily emphasized to mitigate postoperative swelling.
During the early rehabilitation phase (Weeks 2-6), the primary goal shifts to preventing arthrofibrosis while continuing to protect the healing bone and periosteum. At the two-week postoperative visit, the surgical incision was inspected, and the sutures were removed. Radiographs were obtained to confirm the maintenance of reduction and hardware integrity. We initiated a highly controlled, progressive passive range of motion (PROM) protocol. The brace was unlocked to allow 0 to 30 degrees of flexion, advancing by 15 degrees each week, strictly under the guidance of a physical therapist. Active quadriceps contraction (e.g., straight leg raises) remained strictly contraindicated to prevent catastrophic pull-out of the hardware. The patient remained non-weight-bearing.
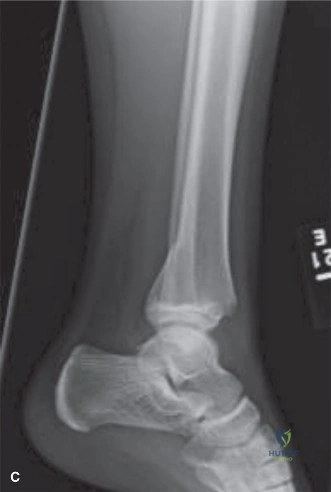
The intermediate phase (Weeks 6-12) marks the transition to active rehabilitation. At the six-week mark, repeat radiographs typically demonstrate early bridging callus and consolidation of the fracture site. Once radiographic healing was confirmed, the patient was allowed to begin progressive partial weight-bearing, advancing to full weight-bearing as tolerated over a two-week period. The brace was unlocked for ambulation. Active range of motion (AROM) exercises were initiated, focusing on regaining terminal extension and full flexion. Closed kinetic chain strengthening exercises, such as mini-squats and leg presses, were gradually introduced. The physical therapist focused heavily on normalizing the patient's gait mechanics and restoring baseline proprioception.
The return to sport phase (Months 3-6) is the final and most demanding stage of rehabilitation. Progression to this phase requires a pain-free, full range of motion, symmetrical quadriceps strength (at least 90% of the contralateral limb), and solid radiographic union. The patient engaged in advanced, sport-specific drills, including plyometrics, cutting maneuvers, and jumping exercises. It is critical to counsel the patient and parents that returning to high-impact sports too early carries a risk of re-injury. Furthermore, we discussed the high likelihood that the prominent screw heads would cause localized irritation when kneeling. Hardware removal is frequently required in these patients, but it is strictly delayed until at least 6 to 9 months postoperatively, ensuring complete, robust remodeling of the avulsion site before the implants are extracted.
High-Yield Clinical Pearls and Pitfalls
Pearl 1: The Osgood-Schlatter Connection. Never evaluate an adolescent knee injury in isolation. A thorough history is paramount. The presence of chronic, preceding anterior knee pain (Osgood-Schlatter disease) is the single greatest risk factor for an acute tibial tubercle avulsion. The chronic apophysitis fundamentally alters the structural integrity of the secondary ossification center, setting the stage for catastrophic failure under eccentric loading. Recognizing this prodrome helps in anticipating the injury pattern and understanding the underlying pathoanatomy.
Pearl 2: The Anterior Compartment Trap. The most devastating pitfall in the management of tibial tubercle fractures is missing an evolving anterior compartment syndrome. The anatomic proximity of the recurrent anterior tibial artery makes it highly susceptible to injury. Always maintain a high index of suspicion. Pain out of proportion to the injury, pain with passive stretch of the great toe (EHL), and a firm anterior compartment are massive red flags. Prophylactic fasciotomy at the time of ORIF is a low-morbidity, high-yield intervention that should be strongly considered in all displaced fractures.
Pearl 3: Meniscal Entrapment in Type III Fractures. When dealing with an Ogden Type III fracture (intra-articular extension), anatomic reduction can sometimes be inexplicably difficult. In these scenarios, the surgeon must immediately suspect entrapment of the anterior horn of the lateral meniscus within the fracture gap. Blind clamping and forceful reduction maneuvers will crush the meniscus. The joint capsule must be opened, the joint inspected, and the meniscus carefully extricated before reduction and fixation are attempted.
Pearl 4: Respect the Periosteal Sleeve. While the osseous fixation with lag screws provides the mechanical strength of the repair, the biologic healing and the ultimate integrity of the extensor mechanism rely heavily on the periosteal sleeve. The medial and lateral periosteal expansions are inevitably torn during a displaced avulsion. Meticulous, watertight repair of these soft tissue envelopes using heavy absorbable sutures is not merely cosmetic; it is a critical step in restoring the secondary restraints of the patella and ensuring a robust, durable recovery.
