Pediatric Cases: Optimal Closure of the Distal Femur
Key Takeaway
In this comprehensive guide, we discuss everything you need to know about Pediatric Cases: Optimal Closure of the Distal Femur. For a 7-year-old with a length-stable femur fracture, reduction and flexible nail fixation is the optimal treatment, offering better patient outcomes than a spica cast. The most common complication parents should know is pain or irritation at nail insertion sites. This approach considers the child's ongoing growth and avoids risks associated with treatments that could prematurely affect the closure of the distal growth plates.
Welcome to this week’s Orthopedic Grand Rounds. Today, we will dissect a highly representative and complex pediatric trauma scenario. While the management of pediatric femoral shaft fractures has evolved significantly over the past three decades, the nuances of surgical decision-making, biomechanical construct selection, and meticulous surgical execution remain paramount. Specifically, we will focus on the principles of Elastic Stable Intramedullary Nailing (ESIN) and the critical, often underappreciated aspect of the procedure: the optimal management and closure of the distal femoral entry sites to prevent long-term morbidity.
Detailed Patient Presentation and Mechanism of Injury
History of Present Illness
A 7-year-old female is transferred to our Level I Pediatric Trauma Center following a high-energy mechanism of injury. The patient was playing tackle football with her older brothers when she was tackled directly on the right thigh while her foot was firmly planted, resulting in a rotational and bending moment across the femoral diaphysis. She immediately collapsed, unable to bear weight, and reported excruciating pain in the right lower extremity.
Emergency Medical Services (EMS) arrived on the scene to find the patient in significant distress with an obvious gross deformity of the right thigh, characterized by shortening, external rotation, and significant soft tissue swelling. A Hare traction splint was applied in the field to restore length, provide preliminary stabilization, and minimize ongoing soft tissue injury and hemorrhage. She was initially evaluated at an outside community hospital where she was hemodynamically stabilized before being transferred to our facility for definitive orthopedic management.
Patient Demographics and Physiological Profile
Upon arrival at our trauma bay, the family provides a comprehensive history. The patient is an otherwise healthy, highly active child described as a "tomboy." She has no significant past medical history, no prior fractures, no known metabolic bone diseases, and takes no daily medications.
A critical piece of data obtained during the nursing intake is her weight: she weighs exactly 35 kg (approximately 77 lbs). In pediatric orthopedics, particularly in the management of long bone fractures, chronologic age and physiological weight are the two most critical variables dictating the treatment algorithm. At 7 years of age and 35 kg, she sits at a crucial inflection point in the treatment paradigm, bridging the gap between conservative casting and rigid adult-type fixation.
Comprehensive Clinical Examination Findings
Primary Survey and Trauma Evaluation
Despite the isolated appearance of the injury, a rigorous Advanced Trauma Life Support (ATLS) protocol is initiated. Pediatric patients possess a remarkable ability to maintain cardiovascular compensation despite significant volume loss, often crashing precipitously once their physiological reserve is exhausted.
- Airway/Breathing: Intact, protecting her airway, saturating 99% on room air.
- Circulation: Tachycardic at 115 bpm (expected secondary to pain and hypovolemia from the fracture hematoma), but normotensive. Capillary refill is brisk globally.
- Disability: Glasgow Coma Scale (GCS) is 15.
- Exposure: Full exposure reveals no other signs of trauma, ecchymosis, or abrasions on the torso or upper extremities. Abdominal examination is benign with no tenderness or guarding, ruling out concurrent solid organ injury.
Focused Orthopedic Examination
The right lower extremity remains in the pre-hospital traction splint.
- Inspection: There is evident swelling over the right mid-thigh with a developing ecchymotic patch over the lateral aspect. The skin is intact with no evidence of open fracture or impending skin necrosis.
- Palpation: Exquisite tenderness is localized to the mid-diaphysis of the right femur. The compartments of the thigh and leg are soft and compressible. While compartment syndrome of the thigh is exceedingly rare due to the large volume of the fascial compartments, it remains a critical consideration in high-energy pediatric trauma.
- Neurovascular Status: The dorsalis pedis and posterior tibial pulses are palpable and symmetric with the contralateral limb. Motor function of the deep peroneal, superficial peroneal, and tibial nerves is intact (the patient can actively dorsiflex, plantarflex, and wiggle her toes). Sensation is intact to light touch in all dermatomal distributions distal to the injury.
- Adjacent Joints: The ipsilateral hip, knee, and ankle exhibit no effusions, swelling, or tenderness. A thorough examination of the joints above and below the injury is mandatory to rule out ipsilateral femoral neck fractures or distal femoral physeal injuries.
Advanced Imaging and Diagnostics
Radiographic Evaluation
Upon completion of the secondary survey, portable radiographs are obtained in the trauma bay to assess the fracture pattern and the adequacy of the applied traction.
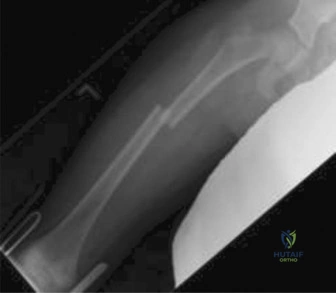
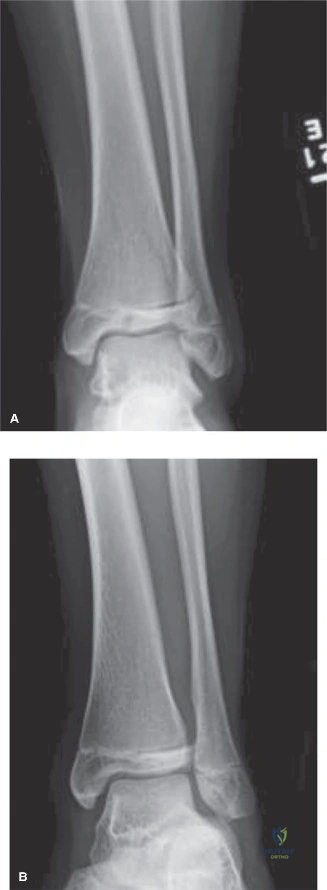
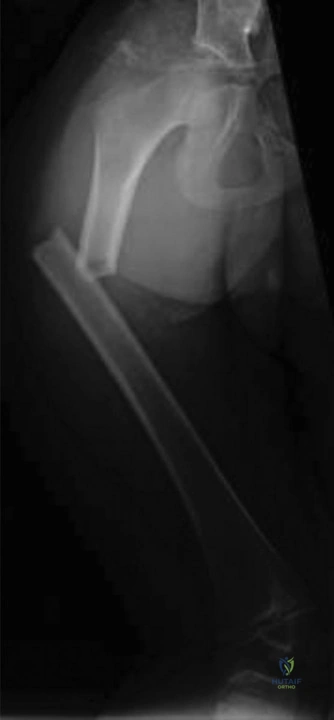
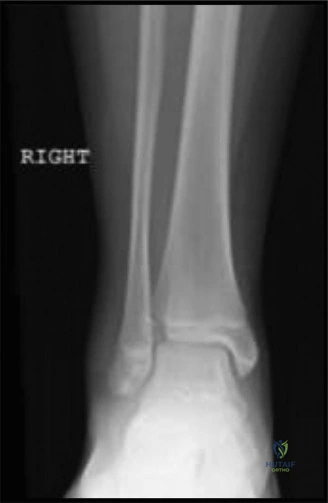
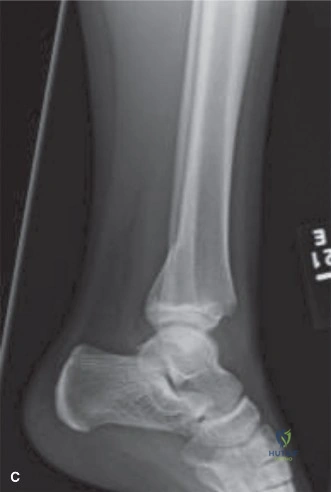
The initial anteroposterior (AP) and lateral radiographs of the right femur demonstrate a complete, displaced, length-stable transverse fracture of the middle third of the femoral diaphysis. There is minimal comminution. The traction splint has effectively restored length, though there remains slight apex-lateral and apex-anterior angulation.
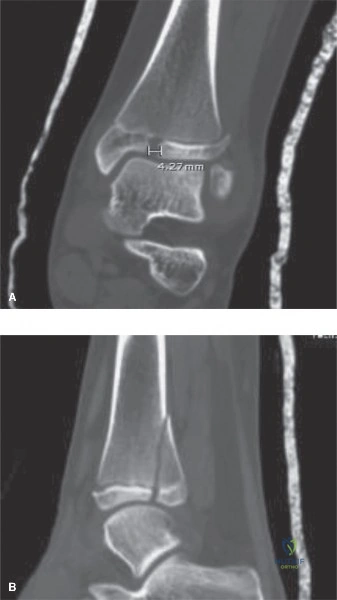
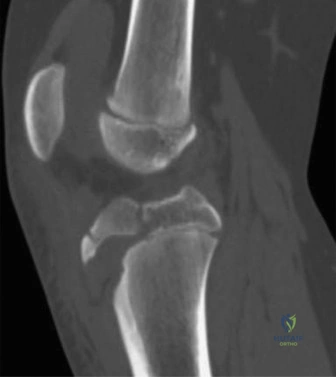
Crucially, dedicated AP and lateral views of the right hip and right knee are obtained. The femoral neck is intact, with no evidence of a basicervical or transcervical fracture—a classic "missed injury" in the setting of high-energy femoral shaft fractures. The distal femoral physis is open and symmetric, with no widening or displacement to suggest a concurrent Salter-Harris injury.
Pre-Operative Templating and Planning
For a diaphyseal femur fracture in a pediatric patient, advanced imaging such as Computed Tomography (CT) or Magnetic Resonance Imaging (MRI) is rarely indicated unless there is suspicion of a pathological lesion, intra-articular extension, or severe soft tissue degloving (Morel-Lavallée lesion).
Instead, the diagnostic focus shifts to meticulous radiographic templating. The narrowest portion of the medullary canal (the isthmus) is measured on both the AP and lateral projections. The fundamental rule for Elastic Stable Intramedullary Nailing (ESIN) dictates that the combined diameter of the two selected nails should fill approximately 80% of the narrowest diameter of the medullary canal. Therefore, the formula used is:
(Narrowest Canal Diameter in mm) × 0.4 = Optimal Single Nail Diameter.
In this patient, the isthmus measures 10 mm. Thus, two 4.0 mm titanium elastic nails will be selected to provide optimal biomechanical stability.
Exhaustive Differential Diagnosis
When evaluating a pediatric femur fracture, the surgeon must consider not only the fracture pattern but the etiology and potential concurrent injuries. Below is a comprehensive differential diagnosis matrix.
| Differential Diagnosis | Clinical Presentation & Mechanism | Radiographic Findings | Management Implications |
|---|---|---|---|
| Traumatic Diaphyseal Femur Fracture | High-energy trauma (MVA, sports). Severe pain, deformity, inability to bear weight. | Transverse, oblique, or spiral fracture of the shaft. Normal bone morphology. | Age/weight-dependent (Spica, FIN, or rigid IM nail). |
| Non-Accidental Trauma (NAT) | Inconsistent history, delayed presentation, age < 3 years (especially non-ambulatory infants). | Spiral fractures in non-ambulatory children, multiple fractures in various healing stages. | Mandatory CPS reporting, skeletal survey, ophthalmology consult. |
| Pathological Fracture (e.g., UBC, ABC, Osteosarcoma) | Low-energy mechanism or spontaneous fracture. Prodromal pain preceding the injury. | Lytic lesion, cortical thinning, periosteal reaction, or "fallen leaf" sign. | Biopsy, curettage/bone grafting, or oncologic referral. Avoid immediate nailing if malignant. |
| Distal Femoral Physeal Fracture (Salter-Harris) | Direct blow to the knee or varus/valgus stress. Localized swelling at the knee. | Widened physis, metaphyseal Thurston-Holland fragment (SH II). | Anatomic reduction, smooth K-wire or screw fixation avoiding physis. |
In our patient, the history of a high-energy tackle in an active 7-year-old perfectly aligns with a traumatic diaphyseal fracture. The radiographs confirm normal bone density and morphology, ruling out a pathological etiology. Her age and the witnessed mechanism effectively rule out NAT.
Complex Surgical Decision Making and Classifications
The Pediatric Femur Fracture Algorithm
The treatment of pediatric femoral shaft fractures is heavily dictated by the American Academy of Orthopaedic Surgeons (AAOS) Clinical Practice Guidelines, which stratify treatment based on chronological age, physiological weight, and fracture pattern.
- 0 to 6 Months: Pavlik harness or simple splinting. Remodeling potential is immense.
- 6 Months to 5 Years: Early spica casting. If the fracture is highly unstable or the child is approaching 5 years and is exceptionally large, flexible intramedullary nailing may be considered.
- 5 to 11 Years (The "FIN" Window): Flexible Intramedullary Nailing (FIN) is the gold standard for length-stable fractures in children weighing less than 50 kg (ideally < 40 kg).
- > 11 Years or > 50 kg: Lateral entry rigid trochanteric intramedullary nail or submuscular bridge plating.
Analyzing the Options for Our Patient
Our patient is 7 years old and weighs 35 kg with a length-stable transverse fracture. Let us critically evaluate the proposed treatment modalities:
- Reduction and Immediate Spica Cast: While historically the standard of care for all ages, spica casting in a 35 kg 7-year-old is fraught with complications. The psychosocial burden on the family is immense. Furthermore, maintaining a 35 kg child in a spica cast risks loss of reduction, skin breakdown, and prolonged joint stiffness.
- Traction followed by Delayed Spica Casting: This antiquated approach requires prolonged hospitalization (often 2-3 weeks), significantly increasing healthcare costs and psychological trauma to the child, without yielding superior functional outcomes compared to operative intervention.
- External Fixation: External fixation is an excellent tool for damage control orthopedics, severe open fractures, or highly comminuted fractures where length cannot be maintained. However, for a closed, length-stable fracture, it carries unacceptably high rates of pin tract infections, loss of motion, and refracture upon frame removal.
- Lateral Trochanteric Intramedullary Nail: Rigid nailing is reserved for older adolescents (> 9-11 years) or those over 50 kg. In a 7-year-old, the greater trochanteric apophysis and the piriformis fossa remain largely cartilaginous. Violating these structures with a rigid nail carries a devastating risk of iatrogenic avascular necrosis (AVN) of the femoral head and premature physeal arrest leading to severe coxa valga.
- Flexible Intramedullary Nails (FIN): This is the definitive treatment of choice. FIN provides a load-sharing, biologically friendly construct that allows for early mobilization, rapid bridging callus formation, and minimal hospital stay, perfectly suited for a 35 kg 7-year-old.

Step-by-Step Surgical Technique and Intervention
Biomechanical Principles of ESIN
Elastic Stable Intramedullary Nailing relies on the principle of symmetric, three-point fixation. Two pre-bent titanium or stainless-steel nails are inserted retrogradely from the distal femoral metaphysis. As they advance through the isthmus, the inherent elasticity of the metal creates a continuous outward radial force against the endosteum. When two nails of identical diameter are used, their opposing forces neutralize varus/valgus and apex-anterior/posterior bending moments, while allowing micromotion at the fracture site to stimulate robust secondary bone healing.
Patient Positioning and Preparation
The patient is brought to the operating room and placed under general anesthesia. She is positioned supine on a radiolucent flat Jackson table. A bump is placed under the ipsilateral hip to correct external rotation. The entire right lower extremity is prepped and draped free to allow for unencumbered manipulation and traction. Fluoroscopy (C-arm) is brought in from the contralateral side to ensure orthogonal views of the entire femur can be obtained effortlessly.
Nail Preparation and Contouring
Based on our preoperative templating, two 4.0 mm titanium elastic nails are selected. The nails must be contoured prior to insertion. A smooth, continuous bow is created in the distal two-thirds of each nail. The apex of the bow should be designed to rest exactly at the level of the fracture site. The maximum height of the curve should be approximately three times the diameter of the medullary canal. This precise contouring is what generates the internal three-point fixation.
The Critical Distal Femoral Entry Points
The success of the procedure—and the prevention of postoperative complications—hinges on the meticulous creation of the entry portals in the distal femur.
- Incision and Dissection: Two 2-3 cm longitudinal incisions are made over the medial and lateral aspects of the distal femur, approximately 2.5 to 3.0 cm proximal to the distal femoral physis. On the lateral side, the iliotibial (IT) band is split longitudinally. On the medial side, the vastus medialis is carefully elevated off the intermuscular septum.
- Protecting the Physis: Under direct fluoroscopic guidance, the starting points are localized. It is absolutely critical to stay strictly proximal to the perichondrial ring and the distal femoral physis to prevent iatrogenic growth arrest.
- Cortical Opening: An awl or drill is used to open the cortex. The instrument is initially directed perpendicularly to gain purchase, then angled 45 degrees proximally to create an oblique track that facilitates smooth nail passage.
Fracture Reduction and Nail Advancement
The lateral nail is introduced first and advanced to the level of the fracture. The medial nail is then introduced and advanced to the same level.
Closed reduction is achieved using manual longitudinal traction and manipulation. Once the fracture is reduced, the nails are driven across the fracture site in an alternating fashion to prevent the construct from displacing the fracture into varus or valgus.
The nails are advanced into the proximal metaphysis. The lateral nail is directed toward the femoral neck (stopping short of the capital femoral physis), and the medial nail is directed toward the greater trochanter. The divergent proximal placement maximizes rotational stability.
Optimal Closure of the Distal Femur
This brings us to the titular focus of this case: the optimal closure and management of the distal femur. The most common complication of FIN is irritation at the insertion site, leading to painful bursa formation, knee stiffness, and the need for premature hardware removal.
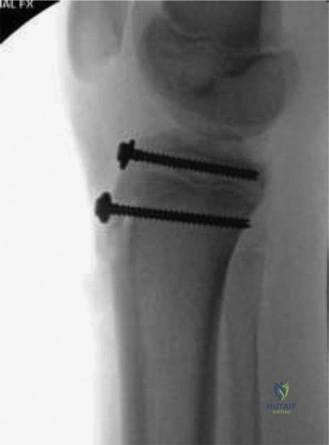
- Cutting the Nails: The nails must not be left too long or too short. They are backed out slightly, cut, and then tapped back in so that approximately 1.0 to 1.5 cm of the nail remains outside the cortex. This allows for future removal while minimizing soft tissue prominence.
- Managing the Soft Tissues: The ends of the nails must sit flush against the metaphyseal flare. They must be buried deep to the deep fascia. On the lateral side, the IT band must be meticulously repaired over the nail end. If the nail protrudes through the IT band, it will cause a painful snapping syndrome with every knee flexion cycle.
- Layered Closure: The vastus medialis and lateral fascia are closed with heavy absorbable sutures. Subcutaneous tissues are reapproximated, and the skin is closed with a running subcuticular stitch. Steri-strips and a sterile dressing are applied.
Strict Post-Operative Protocol and Rehabilitation Stages
Immediate Post-Operative Phase (Weeks 0-2)
The biological advantage of ESIN is the avoidance of rigid immobilization. The patient is placed in a simple knee immobilizer or a soft bulky dressing for comfort.
- Weight Bearing: The construct is load-sharing, not load-bearing. Therefore, the patient is restricted to touch-down weight bearing (TDWB) with the assistance of pediatric crutches or a walker.
- Range of Motion: Active and active-assisted range of motion of the hip and knee is encouraged immediately as tolerated. Early knee flexion prevents quadriceps scarring and stiffness.
- Discharge: Most patients are discharged on postoperative day 1 or 2, once their pain is adequately controlled with oral analgesics and they are cleared by physical therapy.
Intermediate Phase (Weeks 2-6)
The patient returns to the clinic at 2 weeks for a wound check and radiographic evaluation.
- Radiographs: We expect to see maintenance of alignment and the earliest whispers of periosteal reaction.
- Rehabilitation: The knee immobilizer is discontinued entirely. Physical therapy focuses on restoring full knee flexion and hip abductor strength. Weight-bearing remains restricted until the 4-to-6-week mark.
Advanced Phase (Weeks 6-12)
At the 6-week follow-up, radiographs typically demonstrate robust, bridging circumferential callus. This is the hallmark of secondary bone healing promoted by the micromotion of the flexible nails.
- Weight Bearing: Once bridging callus is visualized on three out of four cortices (AP and lateral views), the patient is advanced to full weight-bearing as tolerated.
- Return to Activity: The patient may return to normal daily activities and low-impact play, but contact sports (like tackle football) are strictly prohibited until complete cortical remodeling is achieved, usually around 3 to 4 months.
Hardware Removal
Unlike adult intramedullary nails, flexible nails in growing children are routinely removed. Removal is typically scheduled between 6 and 12 months post-operatively, once the fracture is completely obliterated and remodeled. Delaying removal beyond 12 months increases the risk of the nails becoming encased in cortical bone, making extraction highly morbid.
High-Yield Clinical Pearls and Pitfalls
To conclude this Grand Rounds presentation, I want to leave you with several high-yield technical pearls and potential pitfalls regarding the management of pediatric femur fractures with ESIN.
- The Overgrowth Phenomenon: Pediatric femurs, particularly in children aged 2 to 10, undergo a hyperemic response following a fracture, leading to longitudinal overgrowth. Historically, when treating with spica casts, 1 to 2 cm of overriding was deemed acceptable to account for this. However, with FIN, anatomic length should be restored. The hyperemic overgrowth still occurs, but it is typically less pronounced (average 0.5 to 1.0 cm) and clinically negligible.
- Beware the "Corkscrew" Effect: If the nails cross at the level of the fracture site rather than proximal or distal to it, the construct loses its rotational stability. The fracture can "corkscrew" around the nails, leading to shortening and severe malrotation. Always ensure the maximum bow of the nails is at the fracture, and the crossing points are in the metaphyses.
- Nail Diameter Mismatch: Never use nails of different diameters (e.g., a 3.0 mm medial and a 4.0 mm lateral). The stiffer nail will overpower the weaker nail, inevitably driving the fracture into varus or valgus malalignment.
- Weight Limits are Absolute: Pushing the indications of FIN in a child weighing more than 50 kg (110 lbs) is a recipe for disaster. The biomechanical forces exerted by a heavy child will overwhelm the titanium elasticity, leading to plastic deformation of the nails, loss of reduction, and delayed union. For heavier children, transition to a lateral entry rigid nail or submuscular plating.
- Meticulous Distal Closure: As emphasized by our title, the operation is not over once the fracture is reduced. Take the extra 10 minutes to properly cut, seat, and cover the distal ends of the nails. A prominent lateral nail rubbing against the IT band will result in a miserable patient, an angry family, and a compromised rehabilitation process.
In summary, the 7-year-old, 35 kg patient with a length-stable diaphyseal femur fracture is the quintessential candidate for Elastic Stable Intramedullary Nailing. By adhering to the principles of symmetric three-point fixation, respecting the distal femoral physis, and executing a flawless distal fascial closure, we can ensure rapid healing, early mobilization, and an excellent long-term functional outcome. Thank you for your attention.
