Pediatric Pain & Swelling: 16 Cases Solved & Diagnoses Revealed
Key Takeaway
Here are the crucial details you must know about Pediatric Pain & Swelling: 16 Cases Solved & Diagnoses Revealed. For an adolescent experiencing acute knee pain and swelling after an injury, particularly with an effusion and a challenging physical exam, an MRI is the next best diagnostic step. It accurately identifies soft tissue injuries, such as an ACL rupture or patellar dislocation, which are common causes of these acute knee symptoms in this age group.
The diagnostic evaluation of pediatric musculoskeletal pain and swelling represents one of the most challenging paradigms in orthopedic surgery. Over the past academic quarter, our department reviewed a consecutive series of 16 complex pediatric cases presenting with non-specific extremity pain and swelling. These cases ranged from occult trauma (toddler's fractures, subtle physeal injuries) and infectious etiologies (acute hematogenous osteomyelitis, septic arthritis) to rheumatologic conditions (juvenile idiopathic arthritis). However, the most critical diagnostic dilemmas occurred when benign presentations masked malignant pathology.
For this Grand Rounds presentation, we will perform an exhaustive, deep-dive analysis into Index Case #4 from this series. This case exemplifies the treacherous overlap between sports-related trauma and primary malignant bone tumors. The delayed diagnosis of pediatric bone sarcomas remains a significant clinical challenge, often initially misattributed to "growing pains" or minor athletic trauma. This case study will dissect the clinical, radiographic, and surgical management of a high-grade pediatric osteosarcoma of the distal femur, highlighting the multidisciplinary approach required for limb salvage and oncologic survival.
Patient Presentation and History
Mechanism of Injury and Initial Timeline
The patient is an 11-year-old male who initially presented to an urgent care facility with a chief complaint of right distal thigh and knee pain. The onset of symptoms was insidious but acutely exacerbated following a minor twisting injury sustained while playing competitive youth soccer. Initially diagnosed with a presumed medial collateral ligament sprain, the patient was prescribed a brief period of rest, ice, compression, and elevation, alongside non-steroidal anti-inflammatory drugs.
Despite compliance with conservative management, the pain progressively worsened over a six-week period. The patient developed a distinct nocturnal pain pattern, frequently awakening from sleep, which was unresponsive to over-the-counter analgesia. Furthermore, the parents noted a progressive, asymmetric swelling localized to the distal third of the right femur, accompanied by an antalgic gait.
Demographic Profile and Systemic Review
The patient has no significant past medical history and no known drug allergies. Immunizations are up to date. A review of systems reveals a recent history of unexplained fatigue and a documented unintentional weight loss of approximately three kilograms over the preceding two months. There is no history of fevers, chills, or night sweats, which initially lowered the clinical suspicion for an acute infectious process such as acute hematogenous osteomyelitis.
Family history is negative for childhood malignancies, neurofibromatosis, retinoblastoma, or Li-Fraumeni syndrome. The patient's physiological maturity corresponds to Tanner Stage II, indicating significant remaining skeletal growth potential, a critical factor that will heavily influence subsequent surgical reconstructive decision-making.
Clinical Examination Findings
Inspection and Soft Tissue Assessment
Upon presentation to our orthopedic oncology clinic, visual inspection revealed a gross asymmetry of the right lower extremity compared to the contralateral side. There was a prominent, fusiform swelling over the distal anteromedial aspect of the right thigh. The overlying skin exhibited mild erythema and prominent superficial venous engorgement, indicative of increased regional vascularity often associated with rapidly growing neoplasms or severe inflammatory processes. There were no sinus tracts, ulcerations, or prior surgical scars.
Palpation and Provocative Testing
Palpation elicited moderate to severe tenderness directly over the medial femoral condyle and the distal femoral metaphysis. A firm, fixed, and deeply seated soft tissue mass was palpable, extending proximally from the adductor tubercle. The mass measured approximately 8 centimeters in longitudinal length and was inseparable from the underlying osseous structures.
Range of motion testing of the right knee demonstrated a clinically significant effusion. Active and passive flexion was restricted to 90 degrees secondary to mass effect and pain, while extension lacked 5 degrees. Ligamentous examination (Lachman, anterior/posterior drawer, varus/valgus stress) was stable, effectively ruling out isolated intra-articular ligamentous disruption.
Neurological and Vascular Integrity
A meticulous neurovascular examination was performed due to the proximity of the mass to the popliteal fossa and the adductor hiatus. The dorsalis pedis and posterior tibial pulses were palpable and symmetric bilaterally (2+). Capillary refill was brisk (under two seconds) in all digits. Motor function of the extensor hallucis longus, tibialis anterior, and gastrocnemius-soleus complex was intact (Grade 5/5). Sensation to light touch and pinprick was preserved across the sural, saphenous, superficial peroneal, and deep peroneal nerve distributions. However, the theoretical risk of neurovascular encasement or compression necessitated urgent advanced imaging.
Imaging and Diagnostics
Plain Radiography Evaluation
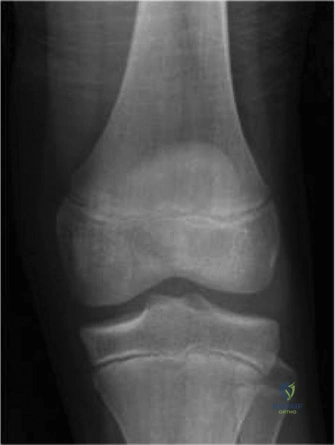
Standard orthogonal radiographs (anteroposterior and lateral views) of the right femur and knee were obtained. The radiographic findings were stark and immediately concerning for a primary malignant bone tumor.
The images revealed a highly aggressive, permeative osteolytic and osteoblastic lesion centered within the intramedullary cavity of the distal femoral metaphysis. The lesion extended through the anterior and medial cortices, demonstrating frank cortical destruction. A florid, aggressive periosteal reaction was evident, characterized by a classic "sunburst" appearance and the presence of a Codman triangle at the proximal margin of the periosteal elevation. These radiographic features represent the rapid, disorganized intramembranous ossification occurring as the tumor outpaces the periosteum's ability to lay down mature bone. Furthermore, a distinct, mineralized soft tissue mass was visible extending anteriorly into the vastus intermedius.
Advanced Cross Sectional Imaging
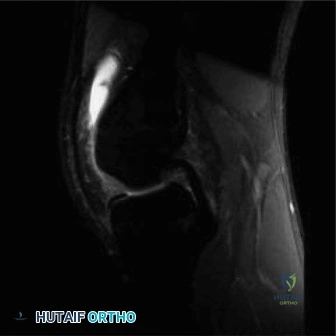
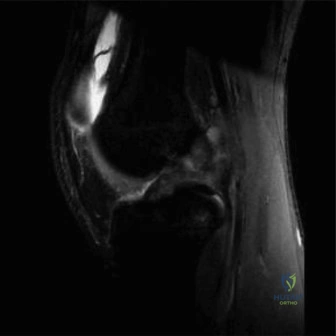
Following the plain radiographs, an urgent Magnetic Resonance Imaging study of the entire right femur with and without intravenous gadolinium contrast was executed to delineate the exact anatomical extent of the lesion.

The MRI protocols included T1-weighted, T2-weighted fat-suppressed (STIR), and T1 post-contrast sequences. The T1-weighted coronal sequences were critical for mapping the intramedullary extent of the tumor, which replaced the normal high-signal fatty marrow with intermediate-signal tumor tissue. The tumor measured 11.5 centimeters in craniocaudal dimension. Crucially, the MRI confirmed that the distal extent of the tumor abutted, but did not frankly cross, the open distal femoral physis.
Axial T2-weighted sequences demonstrated a large, heterogeneous, hyperintense extraosseous soft tissue component. The neurovascular bundle (popliteal artery and vein) was displaced posteriorly but maintained a visible fat plane, indicating it was not directly encased by the tumor—a vital finding for potential limb salvage. Whole-bone imaging confirmed the absence of intramedullary "skip" metastases.
Concurrently, a high-resolution Computed Tomography scan of the chest was obtained to evaluate for pulmonary metastases, which are the most common site of systemic dissemination in osteosarcoma. The CT chest was negative for pulmonary nodules. A Technetium-99m whole-body bone scan showed intense radiotracer uptake localized solely to the right distal femur, ruling out synchronous skeletal lesions.
Pathological Tissue Sampling
With a presumptive diagnosis of a primary bone sarcoma, a core needle biopsy was carefully planned. The biopsy tract was placed meticulously in the anterior compartment, directly in line with the planned future surgical incision for definitive resection. This ensures that the entire biopsy tract can be excised en bloc during the definitive surgery, preventing local tumor seeding.
Histopathological evaluation of the core biopsy specimens revealed highly pleomorphic, spindle-shaped cells producing disorganized, lace-like osteoid matrix. Frequent atypical mitotic figures and areas of coagulative necrosis were present. Immunohistochemistry was positive for SATB2 and negative for cytokeratins and CD45. These findings definitively confirmed the diagnosis of high-grade conventional (osteoblastic) osteosarcoma.
Differential Diagnosis
The presentation of localized bone pain, swelling, and a destructive osseous lesion in a pediatric patient necessitates a broad but highly specific differential diagnosis. Distinguishing between malignant neoplasms, benign aggressive tumors, and infectious processes is paramount for appropriate clinical routing.
Comparative Pathologies
| Pathology | Clinical Hallmark | Radiographic Features | Histological Characteristics |
|---|---|---|---|
| Osteosarcoma | Night pain, palpable mass, metaphyseal location. | Permeative destruction, sunburst periosteal reaction, Codman triangle, soft tissue extension. | Malignant spindle cells producing disorganized, lace-like osteoid matrix. |
| Ewing Sarcoma | Systemic symptoms (fever, weight loss), diaphyseal location. | "Onion-skin" (lamellated) periosteal reaction, large soft tissue mass out of proportion to bone destruction. | Small round blue cells, CD99 positive, EWSR1 gene translocation (t(11;22)). |
| Acute Hematogenous Osteomyelitis | Acute onset, high fever, elevated inflammatory markers (CRP, ESR), extreme tenderness. | Early normal X-rays; later shows focal osteopenia, periosteal elevation, Brodie's abscess. | Acute inflammatory infiltrate, neutrophils, necrotic bone (sequestrum), positive bacterial cultures. |
| Aneurysmal Bone Cyst | Rapid swelling, often preceded by minor trauma, occasionally pathological fracture. | Eccentric, expansile, lytic metaphyseal lesion with a thin cortical shell ("soap bubble"). | Blood-filled cystic spaces separated by fibrous septa containing multinucleated giant cells. |
| Langerhans Cell Histiocytosis | Solitary or multiple bone lesions, variable pain, skull/pelvis/femur common. | Punched-out lytic lesions, "hole-within-a-hole" appearance, variable periosteal reaction. | Clonal proliferation of Langerhans cells, eosinophils, positive for CD1a and S100. |
Surgical Decision Making and Classification
Oncologic Staging Systems
The patient's tumor was classified according to the Enneking Surgical Staging System for benign and malignant bone tumors. Given the high-grade histological nature of the osteosarcoma (Grade G2), its extension through the cortex into the extraosseous soft tissues (Anatomic Setting T2), and the absence of regional or distant metastases (Metastasis M0), the tumor was staged as Enneking Stage IIB.
According to the Musculoskeletal Tumor Society and current National Comprehensive Cancer Network guidelines, the standard of care for Stage IIB osteosarcoma involves a multimodal approach: neoadjuvant (preoperative) chemotherapy, followed by definitive local control (surgical resection), and subsequent adjuvant (postoperative) chemotherapy. The patient underwent a standard MAP regimen (High-dose Methotrexate, Doxorubicin, and Cisplatin) for 10 weeks. Post-chemotherapy restaging MRI demonstrated a 20% reduction in the soft tissue mass volume and increased peripheral calcification, suggesting a favorable chemotherapeutic response.
Limb Salvage Criteria
The decision between limb-sparing surgery and amputation (e.g., transfemoral amputation or rotationplasty) is complex, particularly in a growing child. The absolute contraindications to limb salvage include major neurovascular bundle encasement that cannot be reconstructed, massive soft tissue involvement precluding adequate muscle coverage, and poor expected functional outcome compared to a prosthesis.
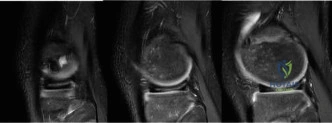
In this case, the restaging MRI confirmed that the popliteal vessels and sciatic nerve remained free of tumor involvement. Furthermore, sufficient quadriceps musculature could be preserved to ensure functional knee extension. Therefore, the decision was made to proceed with limb salvage via a wide en bloc resection of the distal femur.
Because the patient was 11 years old with significant remaining skeletal growth, a standard static endoprosthesis would inevitably lead to a severe limb length discrepancy at skeletal maturity. Consequently, we opted for reconstruction utilizing a non-invasive expandable distal femoral endoprosthesis. This advanced implant contains an internal magnetic driving mechanism that allows for incremental lengthening in the outpatient clinic without the need for repeated surgical interventions, effectively accommodating the child's longitudinal growth.
Surgical Technique and Intervention
Patient Positioning and Initial Approach
The patient was placed supine on a radiolucent operating table. A bump was placed under the ipsilateral hip to prevent external rotation of the limb. A sterile tourniquet was applied to the proximal thigh but not inflated, reserving its use for catastrophic hemorrhage, as tourniquet inflation can theoretically risk tumor embolization. The limb was prepped and draped in a standard sterile fashion, ensuring access from the iliac crest to the toes.
An extensile anteromedial approach to the distal femur was utilized. The skin incision incorporated the previous biopsy tract, utilizing an elliptical incision to excise the tract en bloc with a 1-centimeter margin of healthy skin. The incision extended proximally along the medial border of the rectus femoris and distally across the knee joint, terminating at the medial aspect of the tibial tubercle.
Neurovascular Dissection and Tumor Resection
The initial phase of the deep dissection focused on isolating and protecting the critical neurovascular structures. The superficial femoral artery and vein were identified at the apex of the femoral triangle and traced distally into the adductor canal. The vastus medialis was elevated anteriorly. The adductor magnus tendon was identified and released from the adductor tubercle, allowing access to the popliteal fossa.
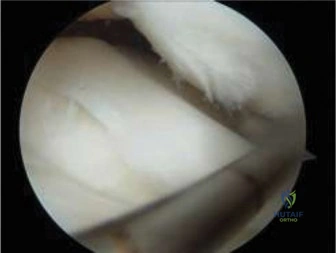
The popliteal artery and vein were meticulously dissected free from the posterior capsule of the knee and the posterior aspect of the tumor pseudocapsule. A layer of healthy muscle (a cuff of vastus intermedius) was left attached to the tumor to ensure wide oncologic margins. The sciatic nerve and its bifurcation into the tibial and common peroneal nerves were visualized and protected.
Once the neurovascular bundle was safely mobilized laterally, attention was turned to the osteotomy. Based on preoperative MRI templating, the proximal femoral osteotomy was planned 3 centimeters proximal to the most proximal extent of the intramedullary marrow abnormality. The femur was circumferentially cleared at this level, and the osteotomy was performed using a cooled oscillating saw. Intramedullary marrow margins were sent for immediate frozen section analysis, which returned negative for tumor cells.
Distally, an intra-articular resection was performed. The cruciate ligaments, collateral ligaments, and menisci were transected. The entire distal femur, encompassing the tumor, the biopsy tract, and the surrounding cuff of normal tissue, was removed en bloc and sent for permanent pathological evaluation and assessment of chemotherapeutic necrosis.
Endoprosthetic Reconstruction Phase
Following copious irrigation of the surgical bed, the reconstruction phase commenced. The proximal femur was sequentially reamed to accommodate the diaphyseal stem of the expandable endoprosthesis. A cemented stem was selected to provide immediate rigid fixation and allow for early weight-bearing. The intramedullary canal was plugged, pulsatile lavage was performed, and polymethylmethacrylate bone cement was injected in a retrograde fashion. The proximal body of the prosthesis was inserted and held in appropriate version (typically 10 to 15 degrees of anteversion) until the cement cured.
Attention was then directed to the proximal tibia. The articular surface was resected using standard total knee arthroplasty cutting jigs. The tibial canal was broached, and a cemented tibial baseplate with a rotating hinge mechanism was implanted. The expandable intercalary segment was then linked to the tibial hinge, completing the structural reconstruction.
Soft tissue reconstruction is paramount to prevent implant infection and ensure functional recovery. The extensor mechanism was realigned. The patellar tendon was secured, and the medial and lateral retinacula were meticulously repaired. A medial gastrocnemius rotational flap was mobilized and transposed anteriorly to provide robust, well-vascularized soft tissue coverage directly over the metallic prosthesis, mitigating the risk of wound breakdown and deep infection. Two deep subfascial closed suction drains were placed, and the skin was closed in layers using absorbable sutures for the deep dermis and surgical staples for the epidermis.
Post Operative Protocol and Rehabilitation
Immediate Postoperative Management
The patient was transferred to the Pediatric Intensive Care Unit for overnight monitoring, given the extensive nature of the resection and the potential for fluid shifts and blood loss. Intravenous prophylactic antibiotics (Cefazolin) were administered for 24 hours postoperatively. The limb was placed in a hinged knee brace locked in full extension to protect the extensor mechanism repair and the gastrocnemius flap.
Pain management was achieved via a multimodal approach, utilizing a continuous peripheral nerve block (adductor canal catheter), scheduled acetaminophen, and intravenous opioids for breakthrough pain. Deep vein thrombosis prophylaxis consisted of mechanical sequential compression devices and pharmacological anticoagulation (enoxaparin) initiated on postoperative day one.
Long Term Functional Rehabilitation
Physical therapy commenced on postoperative day one. The patient was allowed touch-down weight-bearing on the operative extremity with the use of a walker. The hinged knee brace remained locked in extension during ambulation for the first six weeks. Passive range of motion exercises were initiated at week two, gradually increasing flexion by 10 degrees per week, with strict avoidance of active terminal knee extension to protect the patellar tendon repair.
Adjuvant chemotherapy resumed approximately three weeks postoperatively, once the surgical incision demonstrated primary healing without signs of dehiscence or infection. The interaction between cytotoxic chemotherapy and wound healing requires vigilant monitoring, as chemotherapeutic agents significantly impair fibroblast proliferation and collagen synthesis.
At the three-month postoperative mark, the patient transitioned to weight-bearing as tolerated and began active strengthening of the quadriceps and hamstring complexes. Routine follow-up includes plain radiographs every three months to monitor for aseptic loosening or implant failure, and CT chest imaging to monitor for pulmonary recurrence. The non-invasive lengthening of the endoprosthesis will commence once the contralateral leg outgrows the operative leg by 10 millimeters, utilizing the external magnetic field generator in the outpatient clinic.
Clinical Pearls and Pitfalls
Diagnostic Traps
- The "Sports Injury" Fallacy: The most common pitfall in pediatric orthopedic oncology is attributing persistent pain and swelling to a minor traumatic event. Malignant tumors weaken the bone, making it susceptible to micro-fractures during normal activity. Any pediatric patient presenting with bone pain that awakens them from sleep, or pain that persists beyond the expected healing time for a sprain (typically 2-4 weeks), demands plain radiographic evaluation.
- Inadequate Biopsy Placement: A poorly planned biopsy can convert a limb-salvage candidate into an amputee. The biopsy tract must be considered contaminated with tumor cells. It must be placed longitudinally, within the planned surgical incision, and avoid traversing multiple fascial compartments or contaminating major neurovascular bundles. When in doubt, the surgeon who will perform the definitive resection should perform the biopsy.
- Misinterpreting Inflammatory Markers: High-grade sarcomas, particularly Ewing sarcoma, can present with systemic symptoms, elevated C-reactive protein, and elevated erythrocyte sedimentation rate, perfectly mimicking acute hematogenous osteomyelitis. A high index of suspicion must be maintained if the radiographic appearance is atypical for simple infection.
Surgical Nuances
- Margin Assessment: In orthopedic oncology, the margin is defined by the tissue surrounding the tumor, not the tumor itself. A "wide" margin requires a continuous cuff of normal, healthy tissue (muscle, fat, or normal bone) entirely enveloping the tumor pseudocapsule. Breaching the pseudocapsule during dissection exponentially increases the risk of local recurrence.
- Soft Tissue Coverage: The use of massive metallic endoprostheses in the distal femur often leaves the implant covered only by a thin layer of subcutaneous tissue and skin, particularly anteriorly. The routine use of a prophylactic medial gastrocnemius flap provides a robust, vascularized barrier that significantly reduces the incidence of catastrophic deep periprosthetic joint infections and wound necrosis.
- Growth Preservation Planning: Utilizing expandable prostheses requires meticulous preoperative planning regarding the expected remaining growth of the contralateral limb. The surgeon must ensure that the selected implant has sufficient expansion capacity (often up to 50-80 millimeters) to maintain limb length equality until skeletal maturity is reached.
