Pediatric OCD: When to Consider Drilling for the Femoral
Key Takeaway
This article provides essential research regarding Pediatric OCD: When to Consider Drilling for the Femoral. Osteochondritis Dissecans (OCD) of the femoral condyle, often affecting young athletes, involves a lesion of bone and cartilage. Diagnosis includes plain films and MRI. While stable lesions in pediatric patients often heal with protected weight-bearing and bracing, surgical interventions like arthroscopic **drilling for the femoral** lesion, either antegrade or retrograde, may be performed for unstable or non-healing OCD cases.
Comprehensive Introduction and Patho-Epidemiology
Definition and Historical Context
Osteochondritis dissecans (OCD) is an idiopathic, focal, subchondral osseous abnormality that can lead to the instability and eventual detachment of the overlying articular cartilage. When this condition manifests in patients with open physes, it is classified as juvenile osteochondritis dissecans (JOCD). Historically described by Franz König in 1887, the term "osteochondritis" implies an inflammatory etiology; however, modern histological analysis has consistently demonstrated a lack of inflammatory cells, suggesting that the condition is more accurately a manifestation of subchondral osteonecrosis, microtrauma, or localized ischemia. The distinction between JOCD and adult OCD is paramount, as the presence of an open physis confers a significantly higher potential for spontaneous healing with conservative management. Nevertheless, when conservative measures fail, the orthopedic surgeon must be prepared to intervene surgically to prevent long-term joint degeneration.
Pathogenesis and Etiology
The exact etiology of JOCD remains a subject of considerable debate within the orthopedic community, though it is generally accepted to be multifactorial. The prevailing theories encompass repetitive microtrauma, localized vascular insufficiency, genetic predisposition, and anomalous ossification. Repetitive microtrauma is currently the most widely supported theory, particularly given the high incidence of JOCD in pediatric athletes engaged in high-impact, repetitive sports. The repetitive impaction and sheer forces across the joint lead to subchondral stress fractures. If the biological repair mechanisms are outpaced by ongoing mechanical stress, localized ischemia and subsequent subchondral necrosis occur. This necrotic bone fails to support the overlying hyaline cartilage, leading to softening, fibrillation, and eventual separation of the osteochondral fragment. Vascular theories suggest that the watershed areas of the distal femoral epiphysis are particularly susceptible to ischemic events, which may be exacerbated by transient thrombotic events or anatomical vascular variants.
Epidemiology and Demographics
JOCD most frequently affects the knee, accounting for approximately 75% of all pediatric OCD lesions, followed by the capitellum and the talus. Within the knee, the classic location is the lateral aspect of the medial femoral condyle, which harbors approximately 70% to 80% of these lesions. The lateral femoral condyle accounts for 15% to 20%, while the patella and trochlea are involved in less than 5% of cases. The incidence of JOCD is estimated to be between 15 and 30 per 100,000 children, with a notable male predominance, typically presenting at a ratio of 2:1 to 3:1 compared to females. The peak age of presentation is between 10 and 14 years. However, with the increasing participation of young females in competitive, year-round sports, the gender gap is steadily narrowing. Bilateral involvement is observed in 15% to 25% of patients, necessitating a thorough evaluation of the contralateral asymptomatic knee during the initial clinical assessment.
Clinical Presentation and Physical Examination
The clinical presentation of JOCD is often insidious, with patients typically reporting a several-month history of vague, poorly localized, activity-related knee pain. A classic clinical vignette involves a 12-year-old male presenting with medial knee pain that limits his ability to participate in sports, without a distinct history of acute trauma. Patients may report intermittent swelling, stiffness, and mechanical symptoms such as catching or locking, which usually indicate an unstable lesion or a loose body. On physical examination, the patient often demonstrates a trace to mild joint effusion. Tenderness to direct palpation over the involved condyle is a hallmark sign; for medial femoral condyle lesions, this is best elicited with the knee flexed to 90 degrees.
The Wilson test is a classic, albeit variably sensitive, provocative maneuver used to diagnose medial femoral condyle OCD lesions. The test is performed by flexing the patient's knee to 90 degrees, internally rotating the tibia, and slowly extending the knee. The test is considered positive if the patient experiences pain at approximately 30 degrees of flexion, which is subsequently relieved by externally rotating the tibia. This phenomenon occurs because internal rotation impinges the tibial spine against the classic location of the OCD lesion on the lateral aspect of the medial femoral condyle, while external rotation disengages it. A comprehensive examination must also include an assessment of knee range of motion, ligamentous stability, and lower extremity alignment, as genu varum or valgum can significantly alter the biomechanical forces across the affected compartment.
Detailed Surgical Anatomy and Biomechanics
Osseous and Chondral Anatomy of the Knee
A profound understanding of the distal femoral anatomy is essential for the accurate diagnosis and surgical management of JOCD. The distal femur expands into the medial and lateral condyles, which articulate with the tibial plateau and the patella. The articular cartilage covering these condyles is thickest at the weight-bearing zones. The classic location for an OCD lesion—the lateral aspect of the medial femoral condyle—is subjected to unique biomechanical stresses. This area lies adjacent to the intercondylar notch and is intimately related to the insertion of the posterior cruciate ligament. The subchondral bone plate in this region is critical for attenuating impact loads and supporting the overlying hyaline cartilage. In the pediatric population, the distal femoral physis is responsible for approximately 70% of the longitudinal growth of the femur and 37% of the total growth of the lower extremity. Surgical interventions, particularly drilling, must be meticulously planned to avoid iatrogenic injury to this vital growth center.
Vascular Supply to the Distal Femoral Epiphysis
The vascular anatomy of the distal femoral epiphysis plays a critical role in the pathogenesis and healing potential of JOCD. The epiphysis is primarily supplied by the superior and inferior genicular arteries, which form an anastomotic ring around the knee. The intraosseous blood supply to the secondary center of ossification is derived from epiphyseal vessels that penetrate the perichondrium. During development, the vascular supply to the subchondral bone is somewhat tenuous, forming functional end-arteries. This creates a watershed zone, particularly in the lateral aspect of the medial femoral condyle, rendering it highly susceptible to ischemic insults. When an OCD lesion forms, the subchondral bone becomes avascular and necrotic. The fundamental goal of drilling—whether antegrade or retrograde—is to breach this sclerotic, avascular zone and create channels into the healthy, vascularized cancellous bone marrow. This stimulates angiogenesis and the migration of mesenchymal stem cells, thereby facilitating revascularization and creeping substitution of the necrotic fragment.
Biomechanical Forces and Microtrauma
The human knee is a complex hinge joint subjected to immense axial, shear, and rotational forces during ambulation and athletic activities. During the stance phase of the gait cycle, the medial compartment bears approximately 60% to 70% of the axial load. In the context of athletic activities involving cutting, pivoting, and jumping, these forces are exponentially magnified. The tibial eminence can impinge upon the lateral aspect of the medial femoral condyle during internal rotation and extension, a biomechanical reality that underpins both the pathogenesis of the classic OCD lesion and the mechanics of the Wilson test. Furthermore, subtle malalignments, such as genu varum, can shift the mechanical axis medially, increasing the compressive forces on the medial condyle and predisposing the subchondral bone to fatigue failure. Understanding these biomechanical principles is crucial not only for diagnosis but also for postoperative rehabilitation, where altering load-bearing mechanics (e.g., through unloader bracing) can optimize the healing environment.
Diagnostic Imaging and Classification Systems
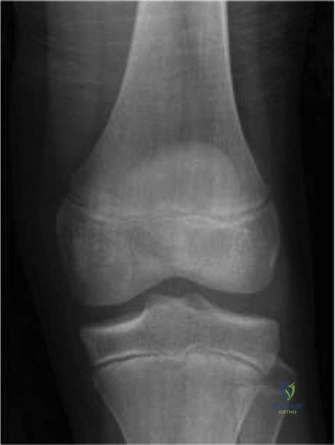
Radiographic Evaluation
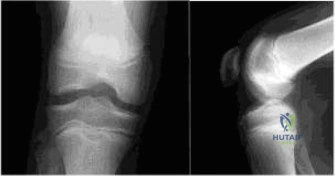
The initial diagnostic workup for a pediatric patient with suspected JOCD must always begin with a comprehensive radiographic series. Standard views should include a weight-bearing anteroposterior (AP), a true lateral, a Merchant or skyline view of the patellofemoral joint, and, crucially, a posteroanterior (PA) flexion weight-bearing view (notch or tunnel view). The tunnel view, taken with the knee flexed to 40 to 50 degrees, is absolutely essential because it profiles the posterosuperior articular surface of the medial and lateral condyles. Since the majority of OCD lesions are located posteriorly on the condyle, they can easily be obscured by the overlapping bony anatomy on a standard AP radiograph. On plain films, an OCD lesion typically appears as a well-circumscribed area of subchondral radiolucency, often containing a central radiodense osseous fragment. Radiographs are also vital for assessing skeletal maturity (via the distal femoral and proximal tibial physes) and overall mechanical alignment.
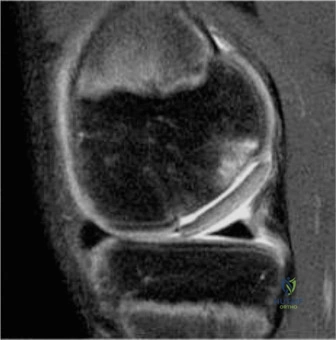
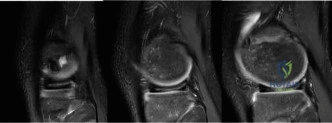
Magnetic Resonance Imaging
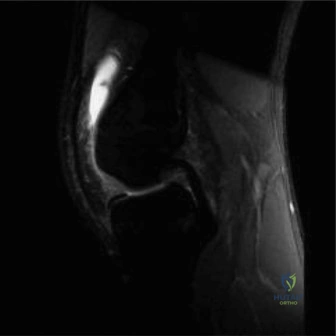
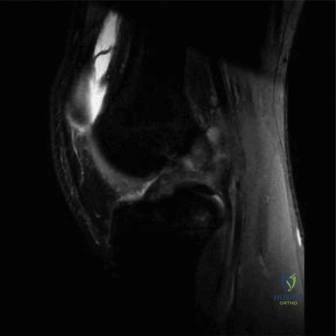
When radiographs confirm the presence of an OCD lesion, Magnetic Resonance Imaging (MRI) is the gold standard for further characterizing the lesion, assessing its stability, and guiding treatment decisions. MRI provides exquisite detail of both the articular cartilage and the underlying subchondral bone. Standard protocols should include T1-weighted, T2-weighted, and proton density (PD) fat-suppressed sequences in the sagittal, coronal, and axial planes. The primary objective of the MRI is to determine the stability of the lesion. Signs of instability include a high-signal-intensity line (fluid) interposing between the OCD fragment and the parent bone on T2-weighted images, focal cystic changes deep to the lesion, cartilage surface fractures, and the presence of a loose body. Conversely, a stable lesion in a juvenile patient will typically show intact overlying cartilage with surrounding bone marrow edema, but without a discrete fluid cleft.
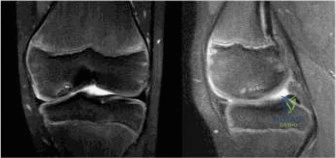
Classification Systems
Several classification systems exist to categorize OCD lesions, aiding in both communication and treatment planning. The Clanton and DeLee classification is based on radiographic appearance, ranging from a depressed osteochondral fracture (Type I) to a completely detached loose body (Type IV). However, the most clinically relevant classifications today are based on MRI and arthroscopic findings. The International Cartilage Repair Society (ICRS) classification is widely utilized during arthroscopy:
* Grade I: Stable lesion with a continuous but softened area of cartilage.
* Grade II: Stable lesion with partial discontinuity of the cartilage.
* Grade III: Unstable lesion with complete discontinuity of the cartilage, but the fragment remains in situ ("dead in situ").
* Grade IV: Empty defect with a loose body within the joint.
The ROCK (Research in OsteoChondritis of the Knee) study group has also developed a comprehensive arthroscopic classification system that further refines these categories to guide specific surgical interventions, such as drilling versus fixation.
Exhaustive Indications and Contraindications
Decision Making in Juvenile Osteochondritis Dissecans
The management of JOCD is dictated by the patient's skeletal maturity, the stability of the lesion, and the clinical symptoms. The initial approach for a stable JOCD lesion in a skeletally immature patient is almost universally non-operative. This consists of a period of activity modification, restriction from impact sports, and potentially a period of protected weight-bearing or immobilization for 3 to 6 months.
Surgical intervention, specifically subchondral drilling, is considered when conservative management fails to yield clinical or radiographic improvement after a dedicated 3 to 6 month trial, or if the patient presents with an unstable lesion (ICRS Grade II or III) but the cartilage is largely intact. Drilling is also indicated for stable lesions in patients who are approaching skeletal maturity, as their potential for spontaneous healing is significantly diminished. The choice between extra-articular retrograde drilling and transarticular antegrade drilling depends on the integrity of the articular cartilage, the location of the lesion, and the surgeon's preference. Retrograde drilling is preferred when the articular cartilage is pristine, as it avoids iatrogenic chondral injury. Antegrade drilling is utilized when the cartilage is already fibrillated or breached, or when the lesion is difficult to access via a retrograde approach.
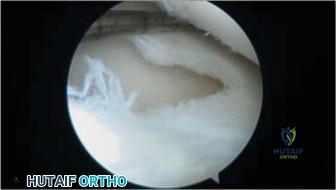
Table: Indications and Contraindications for Drilling
| Parameter | Indications for Drilling (Antegrade or Retrograde) | Contraindications for Drilling |
|---|---|---|
| Clinical Status | Persistent pain after 3-6 months of conservative management; worsening mechanical symptoms. | Asymptomatic incidental finding; initial presentation of a stable lesion in a very young patient. |
| Lesion Stability | Intact or slightly softened cartilage (Grade I/II); stable on probing. | Completely detached fragment (Grade IV); loose body; severe comminution of the fragment. |
| Skeletal Maturity | Open physes (JOCD) failing conservative care; approaching skeletal maturity. | Closed physes with significant instability (often requires fixation or osteochondral grafting). |
| MRI Findings | Sclerotic rim without wide fluid cleft; persistent bone marrow edema without healing. | Massive subchondral cysts >5mm (may require bone grafting); wide T2 fluid clefts indicating gross instability. |
| Approach Specifics | Retrograde: Pristine articular cartilage. Antegrade: Fibrillated/breached cartilage. | Retrograde: Inability to safely bypass the open physis. Antegrade: Perfectly intact cartilage in a very young child (relative contraindication). |
Pre-Operative Planning, Templating, and Patient Positioning
Patient Evaluation and Counseling
Pre-operative planning begins with a thorough discussion with the patient and their parents. It is critical to manage expectations regarding the timeline for return to sports, which can often exceed 6 to 9 months following surgical intervention. The surgeon must explain the biological rationale of the procedure—that drilling creates pathways for bone marrow elements to heal the necrotic subchondral bone—and that the success of the surgery is heavily dependent on strict adherence to postoperative weight-bearing restrictions. Informed consent must cover the risks of failure to heal, progression to osteoarthritis, and the potential need for secondary procedures such as osteochondral autograft transfer (OATS) or autologous chondrocyte implantation (ACI) if the drilling fails.
Imaging Templating and Trajectory Planning
Meticulous templating using pre-operative MRI and radiographs is mandatory, particularly when planning a retrograde extra-articular approach. The surgeon must assess the exact size, depth, and anatomical location of the lesion relative to the distal femoral physis. In a retrograde approach, the drill trajectory must start from the non-articular surface of the femoral condyle, pass through the epiphysis, and enter the lesion without violating the articular cartilage or the open physis. Advanced 3D imaging or intraoperative navigation systems are increasingly being utilized to plan these complex trajectories. The surgeon must determine the appropriate drill size (typically 0.045-inch or 0.062-inch Kirschner wires) and estimate the depth of penetration required to breach the sclerotic rim of the lesion.
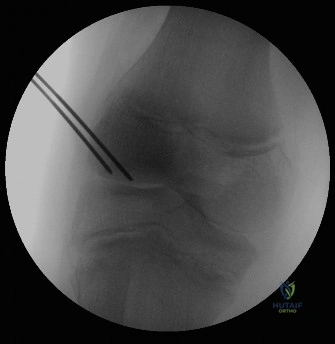
Operating Room Setup and Positioning
The patient is placed in the supine position on a standard radiolucent operating table. A thorough examination under anesthesia (EUA) is performed to assess range of motion and ligamentous stability. A non-sterile tourniquet is applied to the proximal thigh. The operative leg is prepped and draped in a standard sterile fashion. A lateral post or a leg holder is utilized to secure the thigh, allowing for full flexion and extension of the knee, as well as the application of valgus and varus stress to open the respective compartments. The arthroscopy tower is positioned opposite the surgeon. A C-arm fluoroscopy unit must be available and positioned on the contralateral side, draped sterilely, to allow for orthogonal intraoperative imaging, which is absolutely critical for verifying drill trajectories and avoiding physeal injury.
Step-by-Step Surgical Approach and Fixation Technique
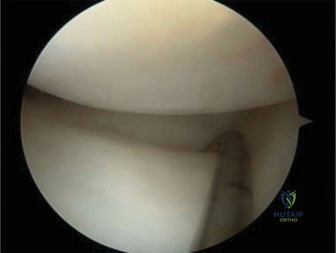
Diagnostic Arthroscopy and Lesion Probing
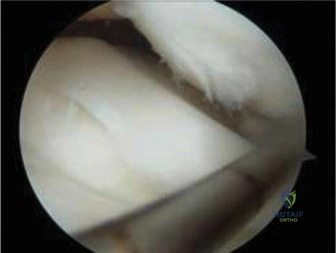
The procedure commences with a systematic diagnostic arthroscopy using standard anterolateral and anteromedial portals. The entire joint is inspected for concomitant pathology, such as meniscal tears or loose bodies. The arthroscope is then directed to the affected condyle. The articular surface overlying the OCD lesion is meticulously evaluated visually and tactilely using an arthroscopic probe. The surgeon assesses for softening, fibrillation, ballottement, and any breaks in the cartilage surface. The stability of the lesion is graded according to the ICRS or ROCK classification. If the cartilage is pristine and the lesion is stable, retrograde drilling is the procedure of choice. If the cartilage is breached or the lesion exhibits minor instability but remains in situ, antegrade drilling, potentially combined with bioabsorbable fixation, is indicated.
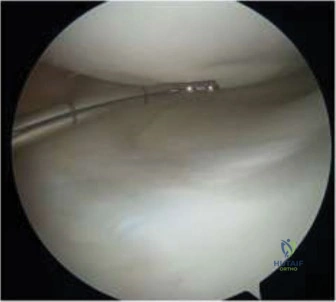
Transarticular Antegrade Drilling
Antegrade transarticular drilling is technically less demanding than the retrograde approach but carries the disadvantage of violating the overlying articular cartilage.
1. Portal Placement: The arthroscope is typically placed in the portal opposite the lesion, while the working portal is established directly over the lesion. Spinal needles are used to localize the optimal trajectory, ensuring that the drill will approach the lesion as perpendicularly as possible.
2. Drilling Technique: A 0.045-inch or 0.062-inch smooth Kirschner wire (K-wire) is introduced through the working portal. Using a power drill, the wire is advanced through the articular cartilage, across the necrotic subchondral bone, and into the healthy, vascularized cancellous bone of the epiphysis.
3. Depth and Pattern: The depth of penetration is typically 15 to 20 millimeters, which can be confirmed with intraoperative fluoroscopy. The drilling is repeated in a uniform, grid-like pattern, with holes spaced approximately 3 to 5 millimeters apart.
4. Biological Confirmation: The tourniquet may be temporarily deflated to observe the egress of fat droplets and marrow blood from the drill holes, confirming adequate penetration into the vascularized marrow space.
Extra-articular Retrograde Drilling
Retrograde extra-articular drilling aims to stimulate subchondral healing while preserving the integrity of the articular cartilage. It is highly technically demanding and relies heavily on precise fluoroscopic targeting.
1. Targeting Guide Application: An anterior cruciate ligament (ACL) tibial or femoral targeting guide is often repurposed for this technique. Under arthroscopic visualization, the intra-articular tip of the guide is placed precisely at the center of the OCD lesion.
2. Incision and Trajectory: A small stab incision is made over the medial or lateral epicondyle, depending on the lesion's location. The guide sleeve is advanced to the extra-articular bone.
3. Fluoroscopic Verification: Before drilling, AP and lateral fluoroscopic views are obtained to ensure that the trajectory of the guide pin will safely bypass the open distal femoral physis and terminate within the lesion without breaching the articular cartilage.
4. Drilling: A guide pin is drilled under continuous or frequent fluoroscopic guidance to a depth approximately 2 to 3 millimeters short of the subchondral bone plate. A cannulated drill bit (typically 2.5 to 3.2 mm) or multiple K-wires are then passed over or parallel to the guide pin to create vascular channels into the lesion.
Fixation of Unstable Lesions
If the diagnostic arthroscopy reveals an unstable lesion (Grade III) that is salvageable, drilling alone is insufficient; the fragment must be stabilized to allow for osseous union.
1. Bed Preparation: The unstable fragment is carefully hinged open like a trapdoor. The fibrous tissue and sclerotic bone at the base of the crater are meticulously debrided using a curette and a motorized burr until healthy, bleeding bone is encountered. The undersurface of the fragment is also gently debrided.
2. Reduction and Fixation: The fragment is anatomically reduced into its bed. Temporary fixation is achieved with K-wires. Permanent fixation is then performed using bioabsorbable compression screws, darts, or variable-pitch titanium screws (which require later removal).
3. Adjunctive Drilling: Once the fragment is securely fixed, supplementary antegrade drilling is performed through the fragment and into the parent bone to maximize the biological healing response.

Complications, Incidence Rates, and Salvage Management
Intraoperative and Early Postoperative Complications
Surgical management of JOCD, while generally safe, carries specific risks. Intraoperative complications primarily revolve around technical errors. During retrograde drilling, the most feared complication is iatrogenic injury to the distal femoral physis, which can lead to premature physeal closure and subsequent angular deformity or limb length discrepancy. Precise fluoroscopic imaging is the only way to mitigate this risk. Another risk is inadvertent penetration of the articular cartilage during retrograde drilling, which negates the primary benefit of the technique. During antegrade drilling, the creation of excessive drill holes can theoretically weaken the subchondral plate, leading to structural collapse of the lesion. Early postoperative complications include hemarthrosis, superficial portal site infections, and deep vein thrombosis (DVT), though the latter is exceedingly rare in the pediatric population.
Late Complications and Treatment Failure
The most significant late complication is the failure of the lesion to heal, resulting in persistent pain, progression to instability, and the eventual detachment of the osteochondral fragment. The incidence of failure following drilling varies in the literature but is generally reported between 10% and 30%, heavily dependent on the initial size of the lesion and the patient's adherence to postoperative weight-bearing restrictions. If a lesion fails to heal and becomes a loose body, the patient is at high risk for early-onset secondary osteoarthritis. Arthrofibrosis, characterized by a significant loss of knee range of motion, can occur if the patient is immobilized for an extended period postoperatively. Hardware complications, such as the migration or breakage of bioabsorbable or metallic implants used for fixation, can cause severe third-body wear on the opposing articular surfaces.
Table: Complications and Salvage Strategies
| Complication | Estimated Incidence | Prevention Strategy | Salvage Management |
|---|---|---|---|
| Non-healing / Progression to Instability | 10% - 30% | Strict adherence to NWB protocols; adequate depth of drilling to vascular marrow. | Revision surgery: Osteochondral Autograft Transfer (OATS), Autologous Chondrocyte Implantation (ACI), or fresh osteochondral allograft. |
| Physeal Arrest / Angular Deformity | < 1% | Meticulous intraoperative fluoroscopy during retrograde drilling; avoiding the physis entirely. | Epiphysiodesis (contralateral or completion); corrective osteotomy (e.g., distal femoral osteotomy) for severe angular deformity. |
| Iatrogenic Cartilage Breach (Retrograde) | 2% - 5% | Frequent fluoroscopic checks; stopping 2-3mm short of the subchondral line. | Convert to antegrade technique principles; monitor closely; usually asymptomatic if small. |
| Hardware Migration / Prominence | 5% - 10% (if fixed) | Countersinking screw heads below the cartilage surface; using appropriate implant lengths. | Arthroscopic hardware removal; debridement of associated chondral damage. |
| Arthrofibrosis / Stiffness | 3% - 8% | Early initiation of passive range of motion (CPM machine); avoiding prolonged casting. | Aggressive physical therapy; arthroscopic lysis of adhesions and manipulation under anesthesia (MUA). |
Phased Post-Operative Rehabilitation Protocols
Phase I: Maximum Protection (Weeks 0 to 6)
The primary goal of the initial postoperative phase is to protect the healing subchondral bone while preventing joint stiffness. Regardless of whether antegrade or retrograde drilling was performed, strict adherence to weight-bearing restrictions is paramount. The patient is typically made non-weight-bearing (NWB) or touch-down weight-bearing (TDWB) on the operative extremity using crutches. A hinged knee brace is often locked in extension during ambulation to prevent accidental loading during a fall. However, early range of motion is critical for cartilage nutrition and preventing arthrofibrosis. Continuous Passive Motion (CPM) machines are frequently prescribed, starting at 0 to 40 degrees and gradually increasing as tolerated. Active-assisted and passive range of motion exercises are initiated immediately under the guidance of a physical therapist. Isometric quadriceps sets and straight leg raises are encouraged to prevent muscular atrophy.
Phase II: Range of Motion and Early Strengthening (Weeks 6 to 12)
At approximately the 6-week mark, follow-up radiographs are obtained to assess for early signs of osseous healing, such as blurring of the sclerotic rim. If clinical symptoms have subsided and imaging is stable, the patient is gradually transitioned to partial weight-bearing and eventually to full weight-bearing over a 2 to 4 week period. The hinged knee brace is unlocked and eventually discontinued once the patient demonstrates adequate quadriceps control without an extensor lag. The focus of physical therapy shifts to achieving full, symmetrical active range of motion and initiating closed kinetic chain exercises, such as mini
