Orthopedic Trauma: A Comprehensive Guide to Low and High-Velocity Gunshot Wound Management
Key Takeaway
Low-velocity gunshot wounds cause direct tissue disruption, with minimal cavitation and localized damage. High-velocity injuries involve massive kinetic energy transfer, creating extensive temporary cavitation, widespread tissue devitalization, and severe comminuted fractures far beyond the bullet path. This distinction is crucial for orthopedic surgical planning, impacting limb salvage and infection prevention.
Introduction and Epidemiology
Gunshot wounds represent a significant and growing challenge in orthopedic trauma, contributing substantially to morbidity, disability, and healthcare burden globally. The fundamental principle distinguishing management strategies for ballistic injuries is the kinetic energy transferred to the tissues, which dictates the extent of tissue destruction. Ballistic injuries are broadly classified into low-velocity and high-velocity wounds, a distinction paramount to effective orthopedic surgical decision-making and limb salvage protocols.
Low-velocity ballistic injuries are typically caused by handguns and shotguns fired at significant range, with muzzle velocities generally below 2,000 feet per second or 610 meters per second. These wounds primarily result from direct tissue disruption along the projectile's path, creating a permanent cavity. The energy transfer is relatively low, leading to less extensive collateral tissue damage compared to high-velocity injuries. Fractures are often simple, oblique, or comminuted but tend to be contained within the immediate trajectory. Soft tissue injury is typically limited to the bullet track, and these injuries frequently behave similarly to closed fractures or low-grade open fractures depending on the degree of contamination.
High-velocity ballistic injuries are caused by military-grade rifles, hunting rifles, or other weapons with muzzle velocities exceeding 2,000 feet per second. The defining characteristic is the massive kinetic energy transfer to tissues, leading to a phenomenon known as cavitation. As the projectile traverses tissue, it creates a temporary cavity significantly larger than its diameter, followed by the formation of a permanent cavity. This temporary cavitation effect causes widespread tissue stretching, tearing, and microvascular disruption far beyond the immediate bullet path. The result is extensive devitalization of muscle, fascia, and periosteum, leading to large soft tissue defects, severe comminuted or segmental bone fractures, and a high risk of deep infection and nonunion. Projectile characteristics such as yaw, tumble, and fragmentation further amplify energy transfer and tissue destruction.
Epidemiologically, ballistic trauma is disproportionately associated with urban environments and conflict zones. While low-velocity injuries remain the most common presentation in civilian emergency departments, high-velocity injuries are increasing with the proliferation of high-powered civilian firearms. Orthopedic surgeons frequently manage ballistic trauma affecting the appendicular skeleton, pelvis, and spine. Associated injuries are highly prevalent and include vascular compromise, peripheral nerve injury, visceral trauma, and severe hemorrhage. Initial assessment must rigidly adhere to Advanced Trauma Life Support protocols, prioritizing hemodynamic stability, airway, breathing, and circulation. The orthopedic surgeon's definitive role begins after life-threatening conditions are addressed, focusing on damage control orthopedics, limb salvage, fracture stabilization, and the prevention of deep musculoskeletal infection.
Surgical Anatomy and Biomechanics
Understanding the biomechanical principles of energy transfer and the specific anatomical tissue responses to ballistic trauma is critical for predicting injury patterns, determining the zone of injury, and planning surgical debridement.
Principles of Ballistic Energy Transfer
Kinetic energy is directly proportional to the mass of the projectile and the square of its velocity, as described by the formula KE = 1/2 mv squared. This non-linear relationship underscores why velocity is the dominant factor in determining the destructive potential of a projectile. However, kinetic energy alone does not dictate the wound profile; the efficiency of energy transfer to the host tissue is equally critical. Energy transfer is maximized when a bullet deforms, fragments, or alters its trajectory within the tissue.
Yaw refers to the deviation of a bullet's longitudinal axis from its line of flight. Tumble occurs when the bullet rotates end-over-end within the tissue. Both yaw and tumble dramatically increase the presenting surface area of the projectile, maximizing drag and kinetic energy dumping. Fragmentation, commonly seen in high-velocity rifle rounds or hollow-point handgun ammunition, creates multiple secondary projectiles. Each fragment creates its own permanent cavity and temporary cavitation wave, exponentially increasing the volume of destroyed tissue.
Low Velocity Tissue Response
In low-velocity trauma, energy transfer occurs primarily by crushing and tearing tissues directly in the projectile's path. Temporary cavitation is minimal, and the permanent cavity closely approximates the diameter of the projectile.
Muscle tissue sustains direct laceration and contusion, with devitalized tissue typically confined to the immediate track. Bone fractures are generally simpler, often presenting as spiral, oblique, or localized butterfly patterns. Comminution, if present, is usually highly localized to the point of impact. Periosteal stripping is minimal, preserving the local osteogenic potential and blood supply. Consequently, low-velocity fractures often possess a biological environment conducive to primary bone healing once stabilized.
High Velocity Tissue Response
High-velocity trauma induces catastrophic tissue failure through the shockwave and subsequent temporary cavitation. The temporary cavity can expand to 10 to 12 times the diameter of the projectile within milliseconds, creating sub-atmospheric pressure that sucks debris, clothing, and environmental contaminants deep into the wound tract.
Muscle tissue subjected to this extreme stretching undergoes severe microvascular disruption, leading to extensive coagulative necrosis far beyond the visible permanent cavity. Bone acts as a secondary source of energy transfer; when struck by a high-velocity projectile, bone shatters, and the resulting osseous fragments become secondary missiles that further destroy surrounding soft tissues. Fractures are typically highly comminuted, segmental, and associated with massive periosteal stripping. The resulting avascular bone fragments serve as a nidus for infection.
Neurovascular Anatomy Considerations
Vascular structures are highly susceptible to cavitation forces. While a low-velocity bullet must directly strike a vessel to cause laceration or transection, a high-velocity projectile can cause severe vascular injury without direct contact. The temporary cavity stretches adjacent arteries, causing intimal tearing, subintimal hematoma, and subsequent thrombosis, even if the adventitia remains intact.
Peripheral nerves exhibit a similar vulnerability. Direct transection is possible, but neuropraxia or axonotmesis secondary to the extreme stretch of the cavitation wave is common. The zone of injury for neurovascular structures in high-velocity wounds is notoriously difficult to accurately assess during the initial presentation, frequently requiring serial examinations and delayed exploration.
Indications and Contraindications
The decision-making process for managing ballistic fractures requires synthesizing the velocity of the weapon, the anatomical location, the degree of soft tissue compromise, and the patient's overall hemodynamic status.
Operative Indications
Operative intervention is mandatory for specific ballistic injury patterns to ensure limb salvage, restore function, and prevent catastrophic complications. High-velocity injuries universally require formal surgical debridement due to the extensive zone of necrosis.
Intra-articular projectiles represent an absolute indication for operative retrieval and joint lavage. Retained intra-articular lead leads to third-body wear, severe mechanical articular cartilage damage, and the dissolution of lead into the synovial fluid, causing systemic lead toxicity (plumbism) and local lead arthropathy.
Fractures associated with vascular compromise requiring repair mandate immediate orthopedic stabilization, typically via external fixation, to protect the vascular anastomosis. The development of compartment syndrome, a frequent complication in high-velocity extremity trauma, necessitates emergent fasciotomy. Unstable fracture patterns, severe comminution precluding conservative management, and fractures with massive soft tissue defects requiring flap coverage are also clear operative indications.
Non Operative Indications
Non-operative management is frequently appropriate for isolated, low-velocity ballistic fractures that are length-stable and possess acceptable alignment. If the fracture pattern is amenable to cast or brace immobilization (e.g., non-displaced tibial shaft fractures, isolated fibula fractures, certain humeral shaft fractures), conservative care is highly successful.
Retained projectiles embedded deeply within muscle bellies or soft tissues, without intra-articular involvement, neurovascular impingement, or location within a weight-bearing surface (e.g., plantar aspect of the foot), should generally be left in situ. The surgical morbidity associated with exploring healthy tissue to retrieve a sterile, inert low-velocity bullet often exceeds the risk of retention.
Operative Versus Non Operative Decision Matrix
| Clinical Scenario | Recommended Management Strategy | Rationale and Key Considerations |
|---|---|---|
| Low-Velocity, Stable Fracture | Non-Operative (Cast/Brace) | Minimal soft tissue damage; fracture heals similarly to closed trauma. Local wound care and short-course antibiotics suffice. |
| High-Velocity Extremity Wound | Operative (Debridement + Stabilization) | Extensive cavitation and necrosis mandate formal OR debridement to prevent sepsis. Temporary external fixation often required. |
| Intra-Articular Projectile | Operative (Arthrotomy/Arthroscopy) | Prevents lead arthropathy, systemic plumbism, and mechanical third-body wear of articular cartilage. |
| Ballistic Fracture with Vascular Injury | Operative (Damage Control Orthopedics) | Rapid external fixation required to stabilize the limb prior to or immediately following vascular shunting/repair. |
| Retained Bullet in Muscle Belly | Non-Operative (Observation) | Bullets are generally sterilized by heat of firing. Attempted removal causes unnecessary iatrogenic tissue damage. |
| Bullet in Spinal Canal with Deficit | Operative (Decompression) | Removal indicated if causing progressive neurological deficit or if located in the cauda equina to prevent lead toxicity. |
Pre Operative Planning and Patient Positioning
Thorough preoperative planning is essential to mitigate the high complication rates associated with ballistic trauma. The approach must be systematic, addressing life-threatening injuries before focusing on the extremity.
Initial Evaluation and Imaging
Evaluation begins with the identification of hard and soft signs of vascular injury. Hard signs (pulsatile bleeding, expanding hematoma, absent distal pulses, palpable thrill, or audible bruit) mandate emergent surgical exploration. Soft signs (history of hemorrhage, proximity of the bullet tract to major vessels, asymmetric pulses, or an Ankle-Brachial Index less than 0.9) necessitate advanced imaging, typically Computed Tomography Angiography.
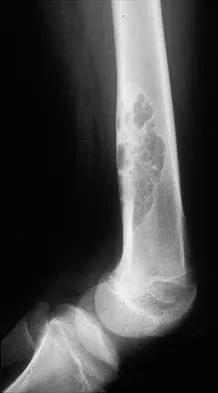
Standard orthogonal plain radiographs encompassing the joint above and below the injury are the foundation of orthopedic assessment. Radiographs identify the fracture pattern, the location of retained projectiles, and the presence of radiopaque debris. Computed Tomography is highly recommended for periarticular fractures to assess joint congruity, identify intra-articular fragments, and plan definitive fixation.
Antimicrobial Prophylaxis
The administration of prophylactic antibiotics is a cornerstone of ballistic trauma management. While the heat of firing theoretically sterilizes the projectile, the vacuum effect of the temporary cavity introduces skin flora, clothing, and environmental debris into the wound tract.
For low-velocity injuries without gross contamination or severe comminution, a short course (24-48 hours) of a first-generation cephalosporin (e.g., Cefazolin) is standard. High-velocity injuries, shotgun blasts at close range, or wounds with gross environmental contamination require broader coverage. The addition of an aminoglycoside (e.g., Gentamicin) is indicated for high-velocity or highly comminuted wounds. If there is concern for soil contamination or bowel injury (in the setting of pelvic/lower extremity trauma), Penicillin or Metronidazole should be added for anaerobic coverage, specifically targeting Clostridium species. Tetanus prophylaxis must be updated according to current guidelines based on the patient's immunization history.
Operating Room Setup and Positioning
Patient positioning is dictated by the anatomical location of the injury and the planned intervention. A fully radiolucent flat Jackson table is frequently preferred over a fracture table for high-velocity or polytrauma patients, as it allows for unhindered fluoroscopic access, simultaneous multi-cavity procedures, and rapid conversion to damage control interventions.
A sterile tourniquet should be available for extremity procedures. However, routine inflation is discouraged during the initial debridement phase. Assessing tissue viability relies heavily on observing active bleeding; a tourniquet obscures this critical assessment. Tourniquet use should be reserved for life-threatening hemorrhage control or for specific, precise reconstructive phases of the operation after debridement is complete.
Detailed Surgical Approach and Technique
The surgical management of ballistic fractures is frequently a staged process, particularly for high-velocity injuries. The initial operation focuses on debridement and temporary stabilization, followed by definitive reconstruction once the soft tissue envelope has declared itself.
Wound Debridement and Irrigation
The primary goal of the initial surgery is the meticulous excision of all devitalized tissue, foreign bodies, and unattached bone fragments. The surgical approach should utilize standard, extensile internervous and intermuscular planes. Traumatic wounds should be extended longitudinally to allow full visualization of the zone of injury.
Muscle viability is assessed using the classic "Four Cs": Color, Consistency, Contractility, and Capacity to bleed. Devitalized muscle is dark, mushy, fails to contract when stimulated with electrocautery, and does not bleed when incised. All such tissue must be aggressively excised until healthy, bleeding margins are reached.
Bone fragments lacking soft tissue attachment (devoid of periosteal blood supply) should be removed, as they will act as sequestra and promote osteomyelitis. However, large articular fragments should be preserved and provisionally stabilized if possible. Copious low-pressure irrigation using normal saline is essential to reduce the bacterial bioburden and flush out micro-debris. High-pressure pulsatile lavage should be avoided, as it can drive contaminants deeper into the tissue planes and further damage the microcirculation.
Fracture Stabilization Strategies
The choice of fracture stabilization depends heavily on the velocity of the injury, the degree of soft tissue loss, and the patient's physiological status.
Damage Control Orthopedics: For hemodynamically unstable polytrauma patients, patients with vascular injuries, or those with massive soft tissue defects from high-velocity weapons, immediate external fixation is the gold standard. External fixation provides rapid, rigid stability, protects soft tissues, allows access for subsequent wound care, and spans the zone of injury without introducing hardware into a highly contaminated field. Pins should be placed outside the anticipated zone of definitive fixation and future flap coverage.
Intramedullary Nailing: For isolated, low-velocity diaphyseal fractures (e.g., femur or tibia), immediate intramedullary nailing is often safe and effective, provided the wound is adequately debrided and there is no gross contamination. The biomechanical advantages of load-sharing and preservation of the fracture hematoma make this an excellent choice for low-energy ballistic fractures.
Open Reduction and Internal Fixation: Plate osteosynthesis is generally avoided in the acute setting for high-velocity ballistic fractures due to the risk of placing extensive hardware in a compromised soft tissue envelope. ORIF is typically reserved for the delayed, definitive reconstruction phase, particularly for periarticular fractures, once the soft tissues are clean and granulating.
Soft Tissue Management and Coverage
Primary closure of ballistic wounds is strictly contraindicated due to the high risk of enclosing anaerobic bacteria and necrotic tissue, which inevitably leads to deep space infection or gas gangrene.
Following debridement, the wound should be managed with Negative Pressure Wound Therapy or packed open with sterile dressings. NPWT is highly effective in managing exudate, reducing tissue edema, and promoting angiogenesis. The patient is typically returned to the operating room every 48 to 72 hours for serial debridements until the wound bed is entirely viable.
Once the wound is clean, definitive coverage is achieved via delayed primary closure, split-thickness skin grafting, or flap transfer. High-velocity injuries with exposed bone, tendon, or neurovascular structures frequently require rotational muscle flaps (e.g., gastrocnemius or soleus for the tibia) or free tissue transfer (e.g., anterolateral thigh flap) in coordination with plastic surgery.
Management of Retained Projectiles
The extraction of retained projectiles requires careful consideration. Bullets located within a joint space must be removed via arthrotomy or arthroscopy. Bullets located within the spinal canal causing progressive neurological deficit or located below the conus medullaris (cauda equina) should be removed.
Superficial bullets that are easily palpable and causing mechanical irritation may be removed during the debridement process. However, deep surgical exploration solely for the purpose of retrieving a bullet embedded in muscle is contraindicated. The surgeon must utilize intraoperative fluoroscopy to precisely localize any projectile planned for removal to minimize iatrogenic soft tissue dissection.
Complications and Management
Ballistic injuries carry a high complication profile, necessitating vigilant postoperative monitoring and aggressive management strategies.
Infection and Osteomyelitis
Deep infection is the most devastating complication of ballistic fractures. High-velocity injuries carry an infection rate comparable to Gustilo-Anderson Type III open fractures. Osteomyelitis requires a multidisciplinary approach involving radical surgical debridement of infected bone, resulting in a segmental defect, combined with targeted, culture-directed intravenous antibiotic therapy.
Management of the resulting bone defect often utilizes the Masquelet technique (induced membrane technique). The first stage involves placing an antibiotic-impregnated polymethylmethacrylate cement spacer into the defect and stabilizing the limb. After 6 to 8 weeks, a biologically active pseudo-membrane forms around the spacer. The second stage involves removing the spacer and filling the defect with autologous bone graft (typically from the iliac crest) and reamer-irrigator-aspirator (RIA) graft. Alternatively, distraction osteogenesis via Ilizarov bone transport can be utilized for massive segmental defects.
Compartment Syndrome
The massive energy transfer and subsequent tissue edema in high-velocity injuries place patients at high risk for acute compartment syndrome. The leg, forearm, and thigh are particularly vulnerable.
Diagnosis is primarily clinical, characterized by pain out of proportion to the injury, pain with passive stretch, and tense, woody compartments. In obtunded patients, intra-compartmental pressure monitoring is required; a delta pressure (diastolic blood pressure minus compartment pressure) of less than 30 mmHg is diagnostic. Management is emergent multi-compartment fasciotomy. For the lower leg, a standard two-incision, four-compartment fasciotomy is mandatory.
Lead Toxicity
Systemic lead toxicity, or plumbism, is a rare but serious complication associated with retained lead projectiles, particularly those bathed in synovial fluid, cerebrospinal fluid, or pseudocysts. Synovial fluid acts as a solvent, accelerating the dissolution of lead. Symptoms are often insidious and include abdominal colic, anemia, peripheral neuropathy, and encephalopathy. Diagnosis is confirmed via elevated whole blood lead levels. Management requires immediate surgical removal of the retained projectile and, in severe cases, systemic chelation therapy.
Complications and Salvage Strategies
| Complication | Estimated Incidence | Pathophysiology | Salvage Strategy and Management |
|---|---|---|---|
| Deep Infection / Osteomyelitis | 2-5% (Low Vel) 15-30% (High Vel) |
Inadequate debridement, avascular bone acting as nidus, extensive contamination. | Radical debridement, hardware removal if loose, Masquelet technique or bone transport, long-term IV antibiotics. |
| Fracture Nonunion | 5-15% | Extensive periosteal stripping, thermal necrosis of bone ends, infection, inadequate stability. | Revision fixation (exchange nailing or robust plating), autologous bone grafting, optimization of host biology. |
| Acute Compartment Syndrome | 5-10% (High Vel) | Massive tissue edema from temporary cavitation, microvascular hemorrhage. | Emergent multi-compartment fasciotomy. Delayed wound closure or skin grafting. |
| Lead Toxicity (Plumbism) | Rare (<1%) | Dissolution of lead in synovial/CSF fluid leading to systemic absorption. | Surgical extraction of the retained projectile, systemic chelation therapy, multidisciplinary toxicology consult. |
| Lead Arthropathy | High (if intra-articular) | Mechanical third-body wear and direct chondrocyte toxicity. | Arthroscopic or open bullet retrieval, extensive joint lavage. May require delayed arthroplasty if cartilage damage is severe. |
Post Operative Rehabilitation Protocols
Rehabilitation following ballistic orthopedic trauma is highly individualized, depending on the fracture pattern, the method of stabilization, and the extent of soft tissue reconstruction.
Early Mobilization and Weight Bearing
Deep vein thrombosis prophylaxis is mandatory, typically initiated within 24 hours postoperatively unless contraindicated by active hemorrhage or concomitant traumatic brain injury.
For diaphyseal fractures stabilized with intramedullary nailing, early weight-bearing as tolerated is often permissible and encourages fracture healing through cyclic micromotion. Conversely, periarticular fractures treated with plate osteosynthesis or limbs managed with external fixation typically require strict non-weight-bearing or touch-down weight-bearing for 6 to 12 weeks to prevent hardware failure.
Early active and passive range of motion of adjacent joints is critical to prevent arthrofibrosis and tendon adhesions, particularly in injuries involving extensive muscle damage. If a muscle flap or skin graft was utilized, range of motion protocols must be coordinated with the plastic surgery team to avoid placing undue tension on the healing soft tissue envelope.
Long Term Functional Recovery
The long-term functional recovery from high-velocity ballistic trauma is often prolonged and requires a dedicated multidisciplinary team comprising orthopedic surgeons, physical therapists, occupational therapists, and orthotists.
Nerve injuries, whether from neuropraxia or transection, require serial electromyography and nerve conduction studies to monitor recovery. Tendon transfers or custom orthoses (e.g., Ankle-Foot Orthosis for common peroneal nerve palsy) may be required for permanent deficits. Psychological support is also paramount, as ballistic trauma is frequently associated with significant post-traumatic stress disorder and psychosocial barriers to recovery.
Summary of Key Literature and Guidelines
The management of ballistic orthopedic trauma has evolved significantly, heavily influenced by both foundational civilian trauma research and lessons learned from military combat casualty care.
Foundational Orthopedic Trauma Literature
The application of the Gustilo-Anderson classification to ballistic trauma has historically been controversial. Classic literature by Dickey et al. demonstrated that low-velocity gunshot fractures behave fundamentally differently than high-energy blunt trauma open fractures. Their work established that routine operative debridement is not mandatory for all low-velocity fractures, paving the way for the successful non-operative or minimally invasive management of stable, low-velocity ballistic injuries.
Conversely, literature analyzing high-velocity trauma unequivocally supports aggressive, staged surgical management. The principles of Damage Control Orthopedics, initially popularized for blunt polytrauma, have been seamlessly integrated into the management of high-velocity ballistic wounds, emphasizing survival and physiological optimization over immediate definitive fracture reconstruction.
Current Consensus and Military Guidelines
The Orthopaedic Trauma Association (OTA) and the Surgical Infection Society have published extensive guidelines regarding antimicrobial prophylaxis in open fractures, which are directly applicable to ballistic trauma. Current consensus strongly supports limiting prophylactic antibiotics to 24-48 hours for low-velocity injuries without gross contamination, moving away from prolonged courses that promote antimicrobial resistance.
Military guidelines, specifically the Tactical Combat Casualty Care (TCCC) and the Joint Trauma System Clinical Practice Guidelines, have profoundly influenced civilian practice. The aggressive use of tourniquets for pre-hospital hemorrhage control, the rapid deployment of external fixation, and the systematic approach to serial wound debridement and NPWT are direct translations of military experience into the civilian orthopedic trauma armamentarium. These guidelines reinforce that high-velocity ballistic trauma is a distinct clinical entity requiring a specialized, multidisciplinary, and phased surgical approach.
