Masterclass: Precision Reconstruction of Boutonnière and Swan-Neck Deformities
Key Takeaway
Step into the operating theater for an in-depth masterclass on reconstructing Boutonnière and Swan-Neck deformities. This guide covers comprehensive anatomy, meticulous preoperative planning, real-time intraoperative execution, critical pearls and pitfalls, and comprehensive postoperative management. Fellows will gain a granular understanding of techniques to restore digital function and stability, addressing both post-traumatic and rheumatoid etiologies with precision.
Comprehensive Introduction and Patho-Epidemiology
Welcome to the operating theater. Today, we confront two of the most technically demanding and functionally devastating digital pathologies encountered in hand surgery: the Boutonnière and Swan-Neck deformities. These conditions are far from mere cosmetic anomalies; they represent a profound, progressive collapse of the intricate biomechanical equilibrium governing the extrinsic and intrinsic tendon systems of the digit. When this finely tuned kinematic chain is disrupted, the result is an intercalated segmental instability that severely compromises grip strength, fine motor dexterity, and overall hand function. Our objective as orthopedic surgeons is not simply to achieve aesthetic realignment, but to meticulously restore the delicate force vectors across multiple joint axes, ensuring durable, long-term functional recovery for the patient.
The etiology of these deformities is broadly categorized into traumatic and systemic inflammatory origins. Rheumatoid arthritis (RA) remains a classic and formidable culprit. RA is a poorly understood, chronic autoimmune disease characterized by aggressive synovial proliferation, neoangiogenesis, and dense lymphocytic infiltration. This hyperplastic synovium, or pannus, releases a cascade of proteolytic enzymes and inflammatory cytokines (such as TNF-alpha and IL-6) that relentlessly degrade articular cartilage, erode periarticular bone, and attenuate capsuloligamentous restraints. In the hand, this inflammatory milieu leads to profound ligamentous laxity and spontaneous tendon ruptures, systematically dismantling the extensor and flexor mechanisms. Understanding this systemic pathophysiology is critical, as it dictates a surgical approach that must account for poor tissue quality and the potential for progressive disease.
Conversely, traumatic etiologies present a different set of challenges, often involving acute avulsions, lacerations, or crush injuries to structurally robust tissues. A forceful hyperflexion injury to an actively extending digit, for instance, can cleanly avulse the central slip from its insertion at the middle phalanx, initiating the Boutonnière cascade. Similarly, an untreated mallet finger can lead to a secondary Swan-Neck deformity due to proximal retraction of the extensor apparatus. Regardless of whether the inciting event is a systemic inflammatory storm or a sudden mechanical failure, the resulting pathoanatomy demands absolute surgical precision.
Mastering the reconstruction of these deformities requires an encyclopedic knowledge of digital anatomy and a nuanced appreciation of spatial biomechanics. The surgeon must be adept at evaluating the flexibility of the deformity, distinguishing between correctable soft-tissue imbalances and fixed, arthritic contractures. We must anticipate the secondary contractures that inevitably develop, such as the tightening of the oblique retinacular ligaments or the volar plate. Ultimately, our success hinges on our ability to navigate this complex architectural landscape, utilizing precise soft-tissue rebalancing techniques, tenodesis, or when necessary, salvage arthrodesis, to restore a functional arc of motion to the compromised digit.
Detailed Surgical Anatomy and Biomechanics
Before a scalpel ever touches the skin, a profound understanding of the intricate anatomy of the digit is mandatory. This is not merely academic theory; it is the fundamental blueprint that guides every dissection, release, and reconstruction. The digital architecture is a marvel of biomechanical engineering, relying on a precarious balance between osteoarticular constraints and dynamic musculotendinous forces.
Osteoarticular Architecture and Ligamentous Restraints
The foundation of digital kinematics lies in its joint morphology and static restraints. The Metacarpophalangeal (MCP) joint is a diarthrodial condyloid joint, permitting a wide arc of flexion-extension and crucial radioulnar deviation for digital splaying. Its stability is dictated by the unique cam-shaped geometry of the metacarpal head. The collateral ligaments originate dorsally on the metacarpal head and insert volarly on the proximal phalanx; due to the cam effect, they are lax in extension and maximally taut in 90 degrees of flexion. This dictates that any immobilization of the MCP joint must be done in flexion to prevent catastrophic collateral ligament contracture.
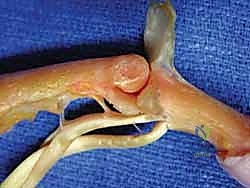
Moving distally, the Proximal Interphalangeal (PIP) joint acts as a pure bicondylar hinge joint. It is inherently more stable than the MCP joint due to the highly congruent articulation between the bicondylar head of the proximal phalanx and the dual concave facets (separated by a median ridge) of the middle phalanx base. The volar plate is a robust, fibrocartilaginous structure originating from the proximal phalanx (via the checkrein ligaments) and inserting firmly into the volar base of the middle phalanx. It serves as the primary static restraint against PIP joint hyperextension. The collateral ligaments of the PIP joint, unlike the MCP, remain under relatively constant tension throughout the arc of motion, providing critical coronal plane stability.
The Distal Interphalangeal (DIP) joint mirrors the PIP joint as a hinge articulation, though with a smaller arc of motion. It is stabilized by its own collateral ligaments, a thinner volar plate, and the terminal insertions of the extensor and flexor mechanisms. The interplay between the PIP and DIP joints is complex and interdependent; the position of one joint directly influences the resting tension and functional capacity of the tendons crossing the other. This intercalated relationship is the very reason why a primary injury at the PIP joint (as in a Boutonnière deformity) inevitably leads to secondary, predictable alterations at the DIP joint.
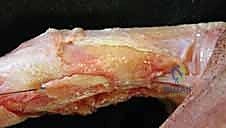
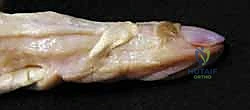
The Dorsal Extensor Apparatus and Retinacular Systems
The dorsal digital extensor apparatus is arguably the most complex and unforgiving soft-tissue envelope in the human body. It is a highly integrated web of extrinsic tendons and intrinsic musculature. The extrinsic Extensor Digitorum Communis (EDC) tendon trifurcates over the proximal phalanx. The central slip (CS) continues distally to insert onto the dorsal base of the middle phalanx, serving as the primary extensor of the PIP joint. The two lateral slips diverge and are joined by the intrinsic contributions.
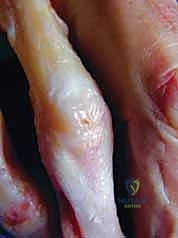
The intrinsic system comprises the interosseous and lumbrical muscles. The sagittal bands anchor the extrinsic extensor tendon centrally over the MCP joint, preventing lateral subluxation during flexion. The intrinsic muscles contribute transverse fibers (which flex the MCP joint) and oblique fibers. These oblique intrinsic fibers merge with the lateral slips of the extrinsic extensor to form the conjoined lateral bands. These bands travel dorsolateral to the PIP joint axis of rotation and eventually converge over the middle phalanx to form the terminal tendon, which inserts into the dorsal base of the distal phalanx to extend the DIP joint.
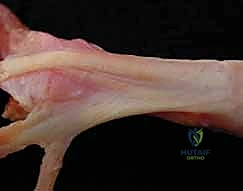
Crucial to the stability of this apparatus are the retinacular ligaments. The Triangular Ligament spans the dorsal interval between the conjoined lateral bands over the middle phalanx, preventing them from subluxating volarly. Conversely, the Transverse Retinacular Ligament (TRL) tethers the lateral bands to the volar capsular structures, preventing them from migrating too far dorsally. Finally, the Oblique Retinacular Ligament (ORL), or Landsmeer's ligament, is a static structure linking the volar PIP joint to the dorsal DIP joint. It coordinates the simultaneous extension of the PIP and DIP joints; as the PIP extends, the ORL tightens, passively extending the DIP joint.
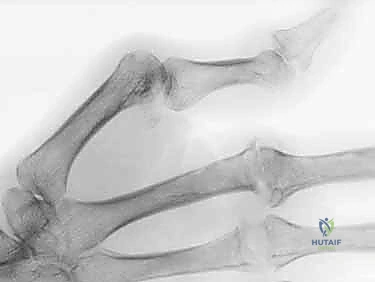
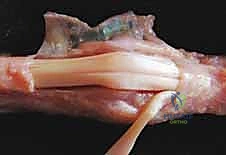
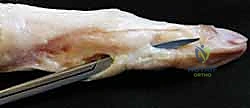
The Flexor Tendon System and Neurovascular Topography
Volar to the osteoarticular axis lies the flexor tendon system, housed within a sophisticated fibro-osseous sheath. The Flexor Digitorum Superficialis (FDS) and Flexor Digitorum Profundus (FDP) tendons must glide seamlessly within this tight corridor. At the level of the A1 pulley, the FDS tendon flattens and bifurcates, allowing the FDP tendon to pass through Camper's chiasm to reach its insertion at the distal phalanx. The bifurcated slips of the FDS then rotate 180 degrees, decussate, and insert into the volar margins of the middle phalanx.
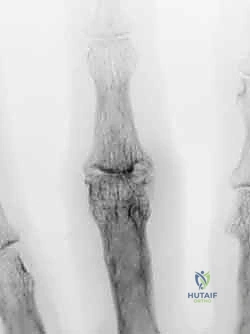
This anatomical arrangement is not merely a spatial curiosity; it has profound implications for reconstructive surgery. The FDS insertion provides a robust anchor point that can be utilized for tenodesis procedures to correct PIP hyperextension in Swan-Neck deformities. Furthermore, the integrity of the flexor pulleys (particularly A2 and A4) is paramount; any iatrogenic injury during volar approaches will result in bowstringing and a devastating loss of digital flexion power.
Navigating this terrain requires meticulous respect for the neurovascular bundles. The proper digital arteries and nerves run volarly, immediately adjacent to the flexor sheath, sending critical transverse branches dorsally to supply the extensor apparatus and overlying integument. Dorsal approaches require careful elevation of full-thickness flaps to preserve these delicate arborizations. Ischemia of the extensor mechanism or skin flap necrosis is a catastrophic complication that can rapidly convert a reconstructive triumph into an unsalvageable failure.
Pathogenesis of Digital Deformities
Understanding the exact sequence of mechanical failure is the prerequisite for rational surgical intervention. Both Boutonnière and Swan-Neck deformities represent a breakdown in the balance between flexor and extensor forces, but they initiate at different points in the kinematic chain and progress through distinct pathological cascades.
The Boutonnière Deformity Cascade
The Boutonnière, or "buttonhole," deformity is clinically defined by flexion of the PIP joint and hyperextension of the DIP joint. The pathognomonic initiating event is the loss of integrity of the central slip of the extensor mechanism. This can occur via acute traumatic rupture (often with a volar avulsion fracture of the middle phalanx base), laceration, or chronic attenuation secondary to rheumatoid synovitis.

Once the central slip is compromised, the primary extensor force on the PIP joint is lost. The PIP joint begins to rest in a flexed position. This flexion posture places abnormal stress on the triangular ligament, which normally holds the lateral bands dorsal to the PIP joint's axis of rotation. Over time, or acutely in severe trauma, the triangular ligament stretches or ruptures. This allows the conjoined lateral bands to subluxate volarly, dropping below the axis of rotation of the PIP joint.

This volar subluxation is the critical biomechanical turning point. The lateral bands, originally extensors of the PIP joint, now become paradoxical flexors of the PIP joint, exacerbating the deformity. Furthermore, because the lateral bands have displaced proximally and volarly, all extensor force from the extrinsic and intrinsic muscles is now bypassed past the PIP joint and concentrated entirely on the terminal tendon. This concentrated force causes the characteristic hyperextension of the DIP joint. If left untreated, the volar plate and collateral ligaments of the PIP joint contract, and the ORL tightens, converting a flexible, correctable imbalance into a rigid, fixed deformity.
The Swan-Neck Deformity Paradigm
The Swan-Neck deformity presents as the exact biomechanical opposite: hyperextension of the PIP joint combined with flexion of the DIP joint. While a Boutonnière deformity typically begins with dorsal pathology (central slip), a Swan-Neck deformity frequently originates from volar pathology—specifically, insufficiency of the PIP joint volar plate. This laxity can be congenital, secondary to generalized hypermobility (e.g., Ehlers-Danlos syndrome), caused by trauma (recurrent dorsal PIP dislocations), or driven by rheumatoid synovitis stretching the volar capsule.
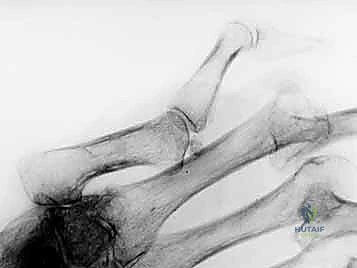
When the volar plate fails to check PIP extension, the joint hyperextends. This hyperextension alters the tension on the extensor apparatus. The transverse retinacular ligaments (TRL) stretch, allowing the conjoined lateral bands to subluxate dorsally, concentrating all extensor force on the PIP joint and further driving it into hyperextension.
Simultaneously, the hyperextension of the PIP joint relatively lengthens the path of the FDP tendon, increasing its resting tension and exerting a stronger flexor force on the DIP joint. Furthermore, the dorsal displacement of the lateral bands reduces their effective excursion at the distal phalanx. In some cases, a primary mallet injury (terminal tendon rupture) can initiate a Swan-Neck deformity by allowing the extensor mechanism to retract proximally, concentrating extensor forces on the central slip and driving the PIP joint into hyperextension. As with the Boutonnière, chronic Swan-Neck deformities lead to secondary contractures, particularly of the intrinsic muscles and dorsal PIP joint capsule, resulting in a stiff, non-functional digit.
Exhaustive Indications and Contraindications
The decision to operate on complex digital deformities is never taken lightly. It requires a rigorous assessment of the patient's functional deficit, the flexibility of the deformity, the quality of the articular cartilage, and the patient's capacity to comply with demanding postoperative rehabilitation. Surgical intervention is generally indicated when conservative measures (such as dynamic splinting and hand therapy) have failed, and the deformity significantly impairs activities of daily living, grip strength, or fine pinch mechanics.
For Boutonnière deformities, acute closed injuries are often managed non-operatively with strict PIP extension splinting for 6 weeks. However, operative intervention is indicated for acute open lacerations of the central slip, avulsion fractures involving more than 30% of the articular surface, or cases where closed reduction cannot be maintained. In chronic cases, surgery is indicated for progressive, symptomatic deformities. The choice of procedure depends entirely on the flexibility of the joints. Flexible deformities are amenable to soft-tissue reconstructions (e.g., Fowler tenotomy, central slip reconstruction). Fixed deformities require sequential joint releases before any tendon balancing can be attempted; if the joint surfaces are destroyed (e.g., advanced RA), arthrodesis or arthroplasty is indicated.
For Swan-Neck deformities, the Nalebuff classification system guides surgical decision-making in rheumatoid patients. Type I (flexible PIP, regardless of MCP position) is treated with PIP volar tenodesis or dermodesis. Type II (PIP flexion limited by MCP position due to intrinsic tightness) requires intrinsic release combined with PIP stabilization. Type III (stiff PIP joint with preserved joint space) necessitates joint manipulation or release prior to soft-tissue reconstruction. Type IV (stiff PIP with severe articular destruction) mandates salvage procedures like arthrodesis or arthroplasty.
Contraindications must be strictly respected to avoid catastrophic outcomes. Absolute contraindications include active local or systemic infection, severe medical comorbidities precluding anesthesia, and profound non-compliance. Operating on a patient who cannot adhere to the rigorous postoperative splinting and therapy protocols is a guarantee of failure, often leaving the patient worse off than before surgery. Relative contraindications include severe, unmanageable complex regional pain syndrome (CRPS) or profound neurovascular compromise of the digit.
| Parameter | Indications for Operative Reconstruction | Contraindications |
|---|---|---|
| Boutonnière Deformity | Acute open laceration of central slip; Displaced avulsion fracture (>30% articular surface); Chronic flexible deformity failing splinting; Fixed deformity with functional impairment. | Active infection; Severe non-compliance; Medically unstable patient; Lack of protective sensation (relative). |
| Swan-Neck Deformity | Symptomatic PIP hyperextension causing locking/snapping; Intrinsic tightness limiting grasp (Nalebuff II); Progressive deformity in RA; Failure of ring splints. | Active infection; Severe vascular insufficiency to the digit; Inability to participate in hand therapy. |
| Salvage (Arthrodesis/Arthroplasty) | Nalebuff Type IV (destroyed joint); Fixed, unyielding contractures; Failed prior soft-tissue reconstruction; Severe pain with motion. | Functionally acceptable painless stiffness; Active osteomyelitis; Insufficient bone stock for fixation (for arthroplasty). |
Pre-Operative Planning, Templating, and Patient Positioning
Meticulous preoperative planning is the hallmark of a master surgeon. The success of these complex reconstructions is largely determined before the first incision is made. This phase involves a comprehensive clinical examination, precise radiographic analysis, and optimal orchestration of the operating room environment.
Clinical Assessment and Radiographic Templating
The clinical examination must be exhaustive. For a suspected Boutonnière deformity, the Elson test is mandatory to assess central slip integrity. The PIP joint is flexed 90 degrees over the edge of a table, and the patient is asked to extend against resistance. If the central slip is intact, the PIP joint extends, and the DIP joint remains flaccid. If the central slip is ruptured, PIP extension is weak or absent, and extensor force is transmitted to the lateral bands, causing rigid DIP hyperextension. For Swan-Neck deformities, the Bunnell-Littler test is crucial to differentiate intrinsic tightness from capsular contracture.
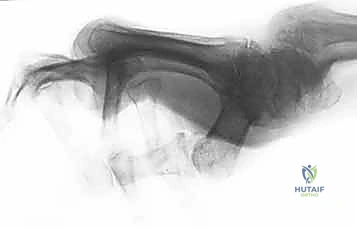
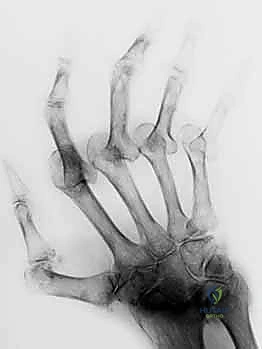
Radiographic evaluation requires high-quality, true AP, true lateral, and oblique views of the individual digit. A "true lateral" is non-negotiable; overlapping digits obscure critical joint space details and subtle subluxations. We evaluate for joint space narrowing, periarticular erosions (classic in RA), osteophytes, and the presence of old avulsion fragments. Templating is particularly important if arthrodesis or arthroplasty is anticipated. We must measure the medullary canal diameter and plan the exact angle of fusion (typically 40° for the index, increasing to 55° for the small finger PIP joint) to optimize the cascade of the hand for a functional grip.
Anesthesia, Positioning, and Hemostatic Control
The choice of anesthesia has evolved significantly. While regional blocks (axillary or supraclavicular) or general anesthesia remain standard, the Wide Awake Local Anesthesia No Tourniquet (WALANT) technique has revolutionized dynamic tendon surgery. Using a mixture of lidocaine and epinephrine injected locally, WALANT provides excellent anesthesia and hemostasis without a tourniquet. Crucially, it allows the conscious patient to actively flex and extend the digit intraoperatively. This provides the surgeon with real-time, dynamic feedback on tendon tensioning, joint stability, and the adequacy of releases, dramatically reducing the risk of over-tightening or under-correction.
If traditional anesthesia is utilized, the patient is positioned supine with the affected extremity extended on a radiolucent hand table. A well-padded pneumatic tourniquet is applied to the proximal arm. Exsanguination with an Esmarch bandage followed by tourniquet inflation to 250 mmHg provides the bloodless field necessary for identifying delicate retinacular structures. Draping must isolate the hand while allowing unhindered manipulation of the wrist and all digits. A C-arm fluoroscope should be positioned perpendicular to the table, entering from the distal end or the contralateral side, allowing for seamless AP and lateral imaging without breaking the sterile field or repositioning the patient.
Step-by-Step Surgical Approach and Fixation Technique
The operative execution requires a synthesis of anatomical knowledge and technical finesse. Tissues in chronic deformities, particularly in rheumatoid patients, are often friable and attenuated. Gentle tissue handling, sharp dissection, and the use of fine, non-reactive sutures (e.g., 4-0 or 5-0 braided non-absorbable for tendon work) are imperative.
Operative Reconstruction of the Boutonnière Deformity
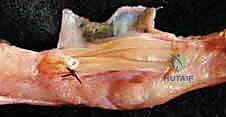
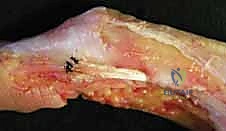
The approach typically involves a dorsal longitudinal or curvilinear incision over the PIP joint, carefully elevating full-thickness skin flaps to protect the dorsal sensory nerve branches and venous drainage. The extensor apparatus is exposed. In a chronic, flexible Boutonnière deformity, the primary goal is to shorten the central slip and relocate the lateral bands dorsally.
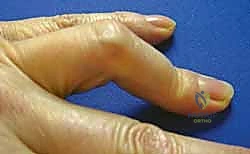
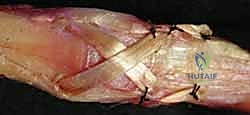
If the central slip is present but attenuated, it can be imbricated or advanced into the base of the middle phalanx using suture anchors. However, if the central slip is irreparably damaged or absent, reconstruction is required. One elegant technique involves mobilizing the lateral bands. The transverse retinacular ligaments are incised longitudinally to free the lateral bands from their volar subluxated position. A slip of one or both lateral bands is then harvested, routed dorsally, and sutured to the base of the middle phalanx to recreate the central slip.
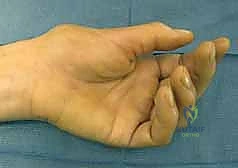
Alternatively, a free tendon graft (e.g., palmaris longus) can be woven through the remaining lateral bands and anchored to the middle phalanx. Following central slip reconstruction, the lateral bands must be stabilized dorsally. This is achieved by repairing or reconstructing the triangular ligament, often using a local tissue flap or a slip of the extensor mechanism.
If the deformity is fixed (stiff PIP flexion), soft-tissue reconstruction alone will fail. The surgeon must first perform a sequential PIP joint release. This involves releasing the collateral ligaments from their proximal origins and excising the contracted volar plate. Only after full, passive PIP extension is achieved can the extensor mechanism be addressed. If joint destruction is severe, we bypass soft-tissue reconstruction entirely and proceed to PIP joint arthrodesis or arthroplasty.
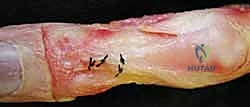
Operative Reconstruction of the Swan-Neck Deformity
The surgical strategy for a Swan-Neck deformity focuses on preventing PIP joint hyperextension and restoring active DIP extension. For a flexible deformity (Nalebuff Type I), volar restraint must be re-established. The Littler FDS tenodesis is a classic and highly effective technique.
A volar zigzag (Bruner) incision is made over the PIP joint. The flexor sheath is opened, carefully preserving the A2 and A4 pulleys. One slip of the FDS tendon is identified and divided proximally (at the level of the A1 pulley). This slip is then left attached to its distal insertion on the middle phalanx. The proximal end of the harvested FDS slip is routed outside the flexor sheath and anchored to the proximal phalanx (either to the bone via drill holes/suture anchors or to the A2 pulley) with the PIP joint held in 20-30 degrees of flexion. This creates a robust, static volar tether that physically blocks hyperextension.
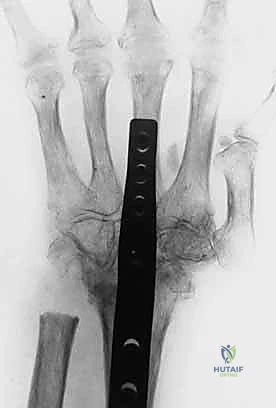
An alternative for addressing both PIP hyperextension and DIP flexion is the Spiral Oblique Retinacular Ligament (SORL) reconstruction
Clinical & Radiographic Imaging Archive