Mastering the Distal Chevron Osteotomy: An Intraoperative Guide for Hallux Valgus Correction
Key Takeaway
This masterclass guides fellows through the Distal Chevron Osteotomy for symptomatic hallux valgus. We'll cover preoperative planning, precise patient positioning, detailed surgical anatomy, and step-by-step intraoperative execution from incision to fixation. Emphasis is placed on preserving critical neurovascular structures, achieving stable osteotomy, and managing potential complications. Postoperative care and rehabilitation protocols are also thoroughly discussed.
Comprehensive Introduction and Patho-Epidemiology
The distal chevron osteotomy remains one of the most enduring, reliable, and widely utilized surgical interventions in the orthopedic armamentarium for the correction of mild to moderate hallux valgus deformities. Originally conceptualized in the late 1970s and subsequently popularized by Austin and Leventen in 1981, this "V-shaped" osteotomy of the distal first metatarsal has undergone decades of refinement. Today, it stands as a foundational masterclass in biomechanical realignment, requiring an intricate understanding of forefoot kinematics. It is not merely a structural shift of bone, but a comprehensive rebalancing of the dynamic forces that act upon the first ray. As orthopedic surgeons, our objective with this procedure is to restore the mechanical axis of the first metatarsophalangeal (MTP) joint, reduce the intermetatarsal angle (IMA), and re-establish the critical weight-bearing function of the first ray without compromising its delicate vascular supply.
Hallux valgus is a complex, progressive patho-anatomical cascade rather than a simple osseous prominence. The deformity is characterized by the lateral deviation and pronation of the proximal phalanx coupled with the medial deviation and pronation of the first metatarsal. This divergence disrupts the finely tuned balance of the intrinsic and extrinsic musculature. As the metatarsal head drifts medially, it escapes the stabilizing cradle of the sesamoid complex. The adductor hallucis, inserting on the base of the proximal phalanx and the fibular sesamoid, becomes a deforming force, further pulling the phalanx laterally. Concurrently, the extensor hallucis longus (EHL) and flexor hallucis longus (FHL) bowstring laterally across the joint, exacerbating the valgus thrust. The medial capsule attenuates and fails, while the lateral structures become rigidly contracted.
Epidemiologically, hallux valgus is pervasive, particularly in shoe-wearing populations, with a distinct predilection for the female demographic. The etiology is multifactorial, encompassing genetic predisposition, ligamentous laxity, specific forefoot morphotypes (such as a long first metatarsal or a rounded metatarsal head), and extrinsic factors like constrictive footwear. While conservative measures can alleviate symptoms, they do not halt the progression of the deformity. Surgical intervention becomes necessary when pain, functional limitation, and difficulty with footwear severely impact the patient's quality of life. The distal chevron osteotomy, when executed with precision, addresses the osseous and soft tissue components of this pathology, offering a definitive solution for a carefully selected patient cohort.
Understanding the progressive nature of hallux valgus is crucial for appropriate procedure selection. A distal osteotomy is highly effective when the primary pathology is localized to the distal aspect of the first ray and the deformity remains within specific angular parameters. However, in cases of severe deformity or inherent instability at the first tarsometatarsal (TMT) joint, a distal procedure will invariably fail, leading to rapid recurrence. Therefore, mastering the distal chevron osteotomy begins long before the first incision; it begins with a profound comprehension of forefoot patho-epidemiology and a rigorous, evidence-based approach to patient selection.
Detailed Surgical Anatomy and Biomechanics
A masterful execution of the distal chevron osteotomy is predicated upon an uncompromising respect for the surgical anatomy of the first metatarsal, particularly its precarious vascular supply. The first metatarsal head receives its arterial inflow through a complex, dual-source network. The dorsal blood supply is primarily derived from the first dorsal metatarsal artery, which gives off capsular branches. However, the most critical vascular contribution to the metatarsal head originates from the plantar aspect. The first plantar metatarsal artery, a branch of the deep plantar arch, supplies a dense capsular network that enters the metatarsal head at its plantar-lateral and plantar-medial reflections.
This anatomical reality dictates our surgical approach. Aggressive stripping of the lateral capsule during the lateral release, combined with an intra-articular or overly proximal osteotomy that violates the plantar capsular attachments, can catastrophically disrupt this blood supply. The resulting avascular necrosis (AVN) of the metatarsal head is a devastating complication that leads to joint collapse, severe pain, and the eventual need for complex salvage arthrodesis. Therefore, the osteotomy must be meticulously planned to remain extra-articular and specifically designed to preserve the plantar-lateral soft tissue hinge. The capital fragment must be translated laterally while maintaining its vital tether to the plantar capsular arterial network.
Biomechanically, the first MTP joint is the linchpin of the foot's windlass mechanism, essential for efficient propulsion during the terminal stance phase of gait. As the hallux dorsiflexes, the plantar fascia is wound around the metatarsal head, elevating the longitudinal arch and locking the midtarsal joints to create a rigid lever for push-off. In a hallux valgus foot, the medial deviation of the metatarsal head and the lateral subluxation of the sesamoids severely compromise this mechanism. The first ray becomes incompetent, leading to a transfer of mechanical load to the lesser metatarsals, clinically manifesting as transfer metatarsalgia.
The distal chevron osteotomy restores this biomechanical integrity. By translating the metatarsal head laterally, we reduce the IMA and physically relocate the metatarsal head back over the sesamoid apparatus. This realignment restores the effective lever arm of the intrinsic muscles, particularly the flexor hallucis brevis (FHB), which encases the sesamoids. Furthermore, by correcting the articular alignment, we optimize joint congruency, allowing for smooth, pain-free sagittal plane motion. Achieving this biomechanical restoration requires not just a lateral shift, but an awareness of the sagittal and coronal planes; the osteotomy can be tailored to slightly plantarflex the head to increase weight-bearing on the first ray, or to de-rotate a pronated metatarsal, ensuring a truly three-dimensional correction.
Exhaustive Indications and Contraindications
Patient selection is the absolute cornerstone of success in forefoot reconstruction. The distal chevron osteotomy is not a panacea for all hallux valgus deformities; it is a highly specific tool designed for a specific magnitude of pathology. The ideal candidate is a patient with symptomatic hallux valgus who has failed a comprehensive trial of conservative management, including shoe wear modification, orthotics, and non-steroidal anti-inflammatory medications. The pain should be localized primarily to the medial eminence (the bunion) during ambulation and shoe wear.
Radiographically, the primary indication is a mild to moderate deformity. This is classically defined by an Intermetatarsal Angle (IMA) of less than 15 degrees and a Hallux Valgus Angle (HVA) of less than 30 to 40 degrees. Crucially, the first metatarsocuneiform (TMT) joint must be clinically and radiographically stable. If there is evidence of hypermobility or significant gaping at the TMT joint on weight-bearing views, a distal procedure will be overwhelmed by the proximal instability, leading to inevitable recurrence. In such cases, a Lapidus procedure (first TMT arthrodesis) is the biomechanically sound choice.
Furthermore, the distal chevron osteotomy is uniquely suited for correcting an abnormal Distal Metatarsal Articular Angle (DMAA). A high DMAA indicates that the articular cartilage is oriented laterally. A standard lateral translation will correct the IMA but leave the joint incongruent. By modifying the chevron cut into a biplanar osteotomy (removing a small medially based wedge from the proximal fragment), the surgeon can rotate the articular surface medially, restoring congruency. However, the procedure is strictly contraindicated in the presence of advanced degenerative joint disease (hallux rigidus), as joint-sparing osteotomies will only exacerbate arthritic pain.
Below is a comprehensive table outlining the strict indications and contraindications for the distal chevron osteotomy to guide clinical decision-making.
| Category | Specific Criteria | Rationale |
|---|---|---|
| Indications | Symptomatic medial eminence pain | Failed conservative management, impacting daily activities. |
| Mild to Moderate Deformity (IMA < 15°, HVA < 30-40°) | Distal translation limits the amount of angular correction possible compared to proximal osteotomies. | |
| Abnormal DMAA (with modification) | Biplanar chevron can reorient the articular cartilage to restore joint congruency. | |
| Congruent or subluxated (but reducible) MTP Joint | The joint must be salvageable; rigid subluxation may require more aggressive soft tissue balancing. | |
| Contraindications | Severe Deformity (IMA > 15°, HVA > 40°) | Insufficient bone width for adequate lateral translation without causing instability or "falling off" the metatarsal shaft. |
| First Ray Hypermobility (TMT instability) | Proximal instability will cause rapid recurrence of the deformity; requires a Lapidus arthrodesis. | |
| Advanced Degenerative Joint Disease (Hallux Rigidus) | Altering mechanics in an arthritic joint will increase pain; arthrodesis or arthroplasty is indicated. | |
| Active Infection or Severe Peripheral Vascular Disease | High risk of non-union, osteomyelitis, or catastrophic ischemic complications. | |
| Spasticity or Neuromuscular Disorders | Unpredictable deforming forces will lead to high recurrence rates. |
Pre-Operative Planning, Templating, and Patient Positioning
Meticulous preoperative planning is the blueprint for intraoperative success. Before the patient ever enters the surgical suite, the surgeon must have a definitive, mathematically sound plan. This process begins with high-quality, standardized, weight-bearing anteroposterior (AP) and lateral radiographs of the foot. Non-weight-bearing films are virtually useless for evaluating forefoot biomechanics, as they fail to demonstrate the true extent of ligamentous laxity and angular deformity under physiological load.
On the AP radiograph, we systematically evaluate several key parameters. First, we measure the Intermetatarsal Angle (IMA) between the longitudinal axes of the first and second metatarsals. We then measure the Hallux Valgus Angle (HVA) between the first metatarsal and the proximal phalanx. We critically assess the Distal Metatarsal Articular Angle (DMAA) to determine if a biplanar correction is required. The position of the sesamoids is evaluated using the Hardy and Clapham classification; ideally, the tibial sesamoid should be restored to position 1 or 2 beneath the metatarsal head. Finally, we assess the relative length of the first metatarsal compared to the second. A significantly short first metatarsal is a relative contraindication for a standard chevron, as the osteotomy inherently shortens the bone slightly, potentially exacerbating transfer metatarsalgia.
Digital or acetate templating is highly recommended. By superimposing templates over the preoperative radiographs, the surgeon can simulate the osteotomy, calculate the exact amount of lateral translation required (typically 3 to 5 millimeters, or roughly one-third the width of the metatarsal shaft), and anticipate the size and trajectory of the fixation hardware. This templating phase allows the surgeon to visualize the final construct and ensures that the planned translation will not result in less than 50% bony apposition, which would compromise the stability and healing potential of the osteotomy.
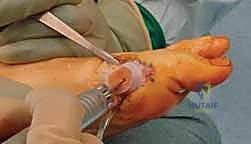
Patient preparation and positioning require equal attention to detail. The procedure is overwhelmingly performed on an outpatient basis. Prophylactic intravenous antibiotics (typically a first-generation cephalosporin like Cefazolin) are administered within one hour of the initial incision to mitigate surgical site infection risks. To ensure a pristine, bloodless surgical field—which is absolutely vital for identifying delicate neurovascular structures and precisely executing the osteotomy—a pneumatic thigh tourniquet is applied and inflated after exsanguination of the limb. The patient is positioned supine on the operating table. A critical positioning adjunct is the placement of a sandbag or heavy bump beneath the ipsilateral gluteal region. This internally rotates the lower extremity, neutralizing the natural external rotation of the hip. The goal is to have the hallux pointing directly toward the ceiling, providing the surgeon with a perfect orthogonal view of the medial forefoot and preventing inadvertent rotational malalignment during the osteotomy fixation.
Step-by-Step Surgical Approach and Fixation Technique
Distal Soft Tissue Release (Lateral Release)
The operation commences with the distal soft tissue release, executed through a dorsal longitudinal incision in the first web space. This step is paramount for mobilizing the rigidly contracted lateral structures that perpetuate the valgus deformity. The incision is deepened through the subcutaneous tissue, taking extreme care to identify and retract the terminal branches of the deep peroneal nerve and the first dorsal metatarsal artery. Blunt dissection is utilized to reach the lateral aspect of the first MTP joint.
Once the lateral capsule is visualized, a sharp capsulotomy is performed. We then identify the conjoined tendon of the adductor hallucis as it inserts into the base of the proximal phalanx and the fibular sesamoid. Using a #15 blade, this tendon is meticulously released from its phalangeal insertion. If the sesamoids remain rigidly subluxated, the fibular suspensory ligament may also be released.
It is absolutely imperative that the surgeon avoids aggressive stripping of the soft tissues directly off the lateral aspect of the metatarsal head. The lateral release must be confined to the joint capsule and the adductor insertion. Overzealous dissection in this region will obliterate the terminal capsular branches of the plantar arterial network, drastically increasing the risk of avascular necrosis. The goal is a targeted release of deforming vectors, not a complete skeletonization of the lateral joint space.
Medial Approach and Eminence Resection
With the lateral structures mobilized, attention is turned to the medial approach. A longitudinal incision is made over the medial aspect of the first MTP joint, centered over the medial eminence. The incision extends from the mid-shaft of the first metatarsal distally to the mid-shaft of the proximal phalanx. The subcutaneous dissection must be deliberate to identify and protect the dorsal medial cutaneous nerve of the hallux. Injury to this nerve guarantees a postoperative course complicated by intractable neuropathic pain or neuroma formation.
Once the nerve is safely retracted dorsally, a longitudinal capsulotomy is performed.

The capsule is sharply elevated off the medial eminence, exposing the hypertrophic bone and the articular surface. Using an oscillating saw, the medial eminence is resected. The trajectory of this cut is critical; it should be oriented in a sagittal plane, originating at the parasagittal groove (sulcus) just medial to the articular cartilage.
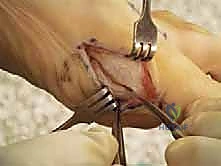
Resecting too much bone will compromise the structural integrity of the metatarsal head and leave insufficient bone stock for the subsequent osteotomy. Resecting too little will fail to eliminate the symptomatic prominence. Following the resection, the plantar capsule is gently mobilized to expose the plantar aspect of the metatarsal neck, ensuring the vital plantar vascular attachments remain undisturbed and tethered to the capital fragment.
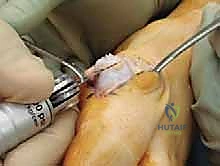
Osteotomy Execution
The execution of the chevron osteotomy requires precise geometric planning. The apex of the "V" is marked with a sterile pen in the center of the metatarsal head, determined by drawing an imaginary ellipse over the articular surface.
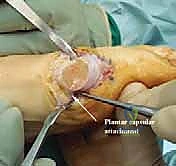
This apex must be located centrally to ensure adequate bone mass in both the dorsal and plantar limbs of the capital fragment. The first cut is the plantar (or transverse) limb. Using a fine-toothed oscillating saw blade, the cut is directed proximally and plantarly from the apex.
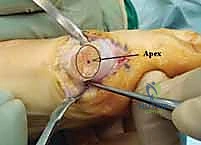
This cut must remain strictly extra-articular and must exit dorsal to the preserved plantar vascular bundle. Next, the vertical (dorsal) limb is executed. The saw blade is initially positioned at 90 degrees to the plantar cut, then angled back to create an intersection angle of approximately 60 to 80 degrees.

During this dorsal cut, the extensor hallucis longus (EHL) tendon must be meticulously protected with a retractor, as the saw blade exits the dorsal cortex.
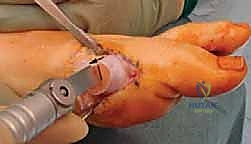
Both limbs of the osteotomy are completed through the lateral cortex, ensuring a complete, clean release of the capital fragment without creating stress risers.
Translation, Fixation, and Capsulorrhaphy
Once the osteotomy is complete, the capital fragment is manually translated laterally.
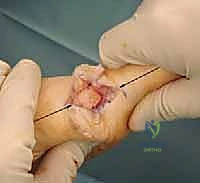
The amount of translation is dictated by the preoperative templating, typically shifting the head laterally by 3 to 5 millimeters, or up to 50% of the metatarsal shaft width. The surgeon must ensure that the fragment is not inadvertently dorsiflexed or plantarflexed during this shift, unless a specific sagittal plane correction was planned. Once the desired position is achieved, the fragments are provisionally stabilized.
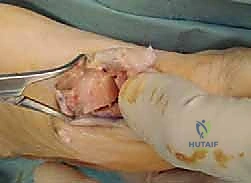
Fixation is typically achieved using a single compression screw, a headless screw, or smooth Kirschner wires, depending on surgeon preference and bone quality. The trajectory of the hardware usually runs from dorsal-proximal to plantar-distal, compressing the osteotomy site. Following rigid fixation, the medial overhanging bone of the proximal metatarsal shaft is resected flush with the newly positioned metatarsal head.
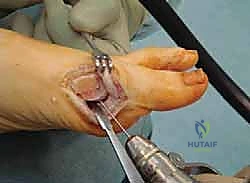
The final, crucial step is the medial capsulorrhaphy. The redundant medial capsule is imbricated and sutured tightly using heavy absorbable suture. This soft tissue plication acts as a dynamic restraint, holding the hallux in its newly corrected, rectilinear alignment and reinforcing the osseous correction.
Complications, Incidence Rates, and Salvage Management
Despite its high success rate in experienced hands, the distal chevron osteotomy is not without inherent risks. Complications can range from minor aesthetic dissatisfactions to catastrophic structural failures requiring complex salvage reconstruction. Thorough preoperative counseling regarding these risks is a mandatory component of the surgical process.
The most feared complication is Avascular Necrosis (AVN) of the metatarsal head. While modern techniques emphasizing the preservation of the plantar-lateral soft tissue hinge have reduced the incidence to roughly 1-3%, it remains a devastating outcome. AVN presents as insidious, worsening pain months after the procedure, with radiographic evidence of sclerosis, cystic changes, and eventual collapse of the articular surface. Management of late-stage AVN inevitably requires a first MTP joint arthrodesis to eliminate the painful, crumbling joint.
Another significant complication is the overcorrection of the deformity, resulting in iatrogenic Hallux Varus. This typically occurs due to a combination of excessive lateral translation of the capital fragment, an overzealous lateral soft tissue release (particularly if the fibular sesamoid is inadvertently excised), and overly tight imbrication of the medial capsule. Hallux varus is highly symptomatic, causing the toe to rub against the medial toe box of the shoe. Mild, flexible cases may be managed with soft tissue releases (e.g., abductor hallucis release) and tendon transfers (e.g., EHB transfer). However, rigid, arthritic hallux varus deformities necessitate MTP joint fusion.
Undercorrection or recurrence of the hallux valgus deformity is also a recognized risk, often stemming from poor patient selection (e.g., performing a chevron in the presence of an unrecognized hypermobile first TMT joint or an excessively large IMA). Nonunion or malunion of the osteotomy site is rare due to the large cancellous surface area of the chevron cut, but it can occur in patients with compromised bone healing, such as active smokers or poorly controlled diabetics. Fixation failure or hardware irritation may necessitate a secondary procedure for hardware removal.
| Complication | Estimated Incidence | Etiology / Risk Factors | Salvage / Management Strategy |
|---|---|---|---|
| Avascular Necrosis (AVN) | 1% - 3% | Excessive lateral stripping; violation of plantar capsular vessels. | Early: Offloading. Late/Collapse: First MTP Arthrodesis. |
| Hallux Varus (Overcorrection) | 2% - 5% | Over-resection of eminence; excessive lateral release; tight medial plication. | Flexible: Soft tissue release / tendon transfer. Rigid: Arthrodesis. |
| Recurrence / Undercorrection | 5% - 10% | Poor patient selection (hypermobility, high IMA); inadequate lateral translation. | Revision osteotomy (proximal) or Lapidus arthrodesis. |
| Nonunion / Delayed Union | < 1% | Smoking; diabetes; inadequate fixation; thermal necrosis from saw blade. | Prolonged immobilization; bone grafting; revision internal fixation. |
| Hardware Irritation | 5% - 15% | Prominent screw head or K-wire; thin soft tissue envelope. | Hardware removal after radiographic confirmation of union. |
| Transfer Metatarsalgia | 3% - 7% | Excessive shortening or unintentional dorsiflexion of the first metatarsal head. | Orthotics; lesser metatarsal shortening osteotomies (Weil). |
Phased Post-Operative Rehabilitation Protocols
The immediate postoperative phase is focused on protecting the osteotomy, managing edema, and facilitating soft tissue healing. For the first two weeks (Phase I), the patient is placed in a rigid, flat-bottomed postoperative shoe or a controlled ankle motion (CAM) boot. Weight-bearing is strictly limited to heel-touch or side-of-foot ambulation to prevent dorsal displacement of the capital fragment. The foot is maintained in a bulky, compressive dressing that acts as a splint, holding the hallux in neutral alignment. Elevation above the level of the heart is critical during this phase to minimize swelling and throbbing pain.
At the two-week mark, the patient transitions to Phase II (Weeks 2-6). The initial dressings and sutures are removed. Radiographs are obtained to confirm the maintenance of alignment and hardware position. At this juncture, a critical paradigm shift occurs: the initiation of early range of motion (ROM). First MTP joint stiffness is one of the most common postoperative complaints. Patients are instructed to perform active and gentle passive plantarflexion and dorsiflexion exercises of the great toe multiple times a day. The patient may begin progressive, flat-footed weight-bearing in the postoperative shoe, guided by pain tolerance.
Phase III (Weeks 6-12) marks the transition back to normal function. Radiographs at six weeks typically demonstrate early trabecular bridging across the osteotomy site. The patient is transitioned out of the postoperative shoe and into a wide-toed, supportive athletic shoe. Physical therapy may be formally instituted to aggressively address any residual MTP joint stiffness, restore intrinsic foot muscle strength, and normalize the gait pattern. High-impact activities, running, and the use of restrictive footwear (such as high heels) are strictly prohibited until at least 12 weeks postoperatively, and only after radiographic confirmation of complete osseous consolidation.
Summary of Landmark Literature and Clinical Guidelines
The evolution of the distal chevron osteotomy is deeply chronicled in orthopedic literature, transitioning from an empirical technique to a highly scrutinized, evidence-based procedure. The seminal paper by Austin and Leventen in 1981 remains the bedrock of this technique. They reported on a massive series of over 1,000 osteotomies, demonstrating excellent outcomes, minimal shortening, and a very low complication rate, thereby cementing the "Austin osteotomy" into the global orthopedic lexicon. Their emphasis on the 60-degree angle for inherent stability remains a guiding principle today.
Subsequent literature has heavily focused on the vascular safety of the procedure, given the catastrophic nature of AVN. Landmark anatomical studies by researchers such as Shereff and Jones meticulously mapped the extraosseous and intraosseous blood supply of the first metatarsal. Their work unequivocally proved that the primary blood supply to the head enters via the plantar-lateral capsule. This literature directly informed modern clinical guidelines, which now universally mandate the preservation of the plantar soft tissue attachments during the osteotomy and caution against combined aggressive lateral and medial releases.
Long-term outcome studies comparing the distal chevron to other techniques have further refined our clinical algorithms. Comparative analyses by Coughlin and Mann, as well as European literature focusing on the Scarf osteotomy (e.g., Barouk), have established that while the chevron is unparalleled for mild to moderate deformities, it has distinct mathematical limitations in severe cases. Current clinical guidelines from societies such as the American Orthopaedic Foot & Ankle Society (AOFAS) strongly support the distal chevron osteotomy for IMAs less than 15 degrees, emphasizing that adherence to strict patient selection criteria is the primary determinant of long-term patient satisfaction and the prevention of deformity recurrence.
