Mastering Tendon Transfers for Ulnar Nerve Palsy: An Intraoperative Guide
Key Takeaway
This masterclass guides fellows through tendon transfers for ulnar nerve palsy, focusing on restoring thumb adduction and correcting claw deformity. We meticulously cover surgical anatomy, patient positioning, and step-by-step intraoperative execution, including brachioradialis-to-APB transfer and FPL-EPL tenodesis. Critical pearls, potential pitfalls, and comprehensive postoperative care are emphasized, ensuring a thorough understanding of this intricate hand procedure.
Introduction and Epidemiology
Ulnar nerve palsy represents a profoundly debilitating condition that strips the hand of its fine motor coordination, grip strength, and key pinch capabilities. It is characterized by the loss of sensory and motor function following injury to the ulnar nerve anywhere along its anatomical course. Clinically, it is categorized as either a high or low ulnar nerve palsy depending on whether the lesion is proximal or distal to the motor branches supplying the flexor digitorum profundus (FDP) and flexor carpi ulnaris (FCU). Often referred to in surgical literature as the "musician's nerve," the ulnar nerve is critical for controlling the intrinsic muscles of the hand, which execute the complex, independent digital movements required for high-level dexterity and power grip.
Epidemiologically, ulnar neuropathy at the elbow (cubital tunnel syndrome) is the second most common compression neuropathy in the upper extremity, following median nerve compression at the carpal tunnel. However, traumatic etiologies—such as glass lacerations at the wrist, severe traction injuries associated with brachial plexus trauma, and complex distal humerus or forearm fractures—frequently lead to profound and irreversible ulnar nerve palsy. Furthermore, systemic neuropathies (e.g., Hansen’s disease, severe diabetic neuropathy, Charcot-Marie-Tooth disease) can present with analogous intrinsic wasting.
When primary nerve repair, nerve grafting, or distal nerve transfers fail, or when the patient presents in a delayed fashion (typically greater than 12 to 18 months post-injury), Wallerian degeneration and subsequent motor endplate fibrosis render the intrinsic muscles irreversibly atrophied. In these chronic scenarios, tendon transfers become the absolute gold standard for restoring hand biomechanics, synchronizing digital flexion, and re-establishing functional pinch and grip strength.
Surgical Anatomy and Biomechanics
Ulnar Nerve Course and Innervation
The ulnar nerve is the terminal continuation of the medial cord of the brachial plexus, carrying motor and sensory fibers predominantly from the C8 and T1 nerve roots. It provides no motor innervation in the arm. As it courses distally, it passes behind the medial epicondyle through the cubital tunnel (beneath Osborne’s ligament) and enters the forearm between the two heads of the flexor carpi ulnaris. In the proximal forearm, it gives off its first motor branches to the FCU and the FDP of the ring and small fingers.
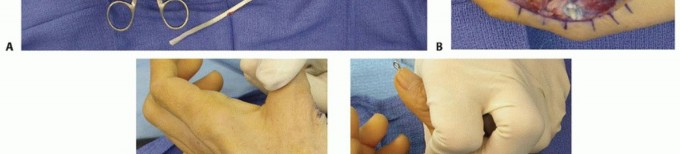
At the wrist, the ulnar nerve enters Guyon’s canal, bordered by the pisiform ulnarly and the hook of the hamate radially, where it bifurcates into superficial (sensory) and deep (motor) branches. The deep motor branch dives beneath the hypothenar fascia to supply the hypothenar muscles (abductor digiti minimi, flexor digiti minimi, opponens digiti minimi), all dorsal and palmar interossei, the third and fourth lumbricals, the adductor pollicis, the deep head of the flexor pollicis brevis, and terminates at the first dorsal interosseous. The sensory fibers supply the volar aspect of the small finger and the ulnar half of the ring finger. Notably, the dorsal ulnar cutaneous nerve (DUCN) branches approximately 5 to 7 cm proximal to the wrist joint to supply the dorsoulnar aspect of the hand; preservation of this branch is critical during distal forearm exposures.
Biomechanics of the Intrinsic Minus Hand
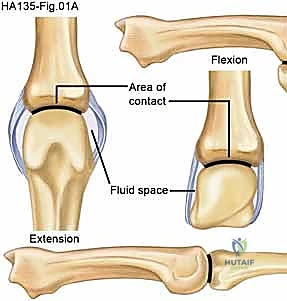
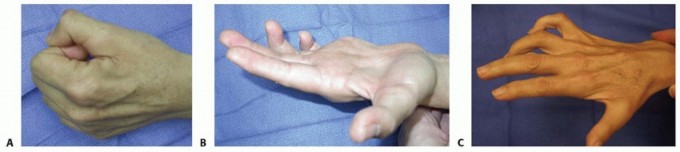
The pathognomonic hallmark of ulnar nerve palsy is the "intrinsic minus" or claw hand deformity. A precise understanding of the biomechanics of clawing is mandatory for rational surgical planning. In the normal hand, the intrinsic muscles (lumbricals and interossei) flex the metacarpophalangeal (MCP) joints and extend the proximal (PIP) and distal interphalangeal (DIP) joints. They achieve this complex action by passing volar to the MCP joint axis of rotation and dorsal to the PIP joint axis via their insertion into the lateral bands of the extensor mechanism.
When ulnar motor function is lost, the extensor digitorum communis (EDC) acts unopposed at the MCP joint, driving it into severe hyperextension. Concurrently, the FDP and flexor digitorum superficialis (FDS) act unopposed at the interphalangeal joints, driving them into flexion. This asynchronous motion creates the "roll-up" phenomenon: the fingertips curl into the palm before the MCP joints can flex around an object, effectively pushing large objects out of the grasp and severely diminishing grip strength.
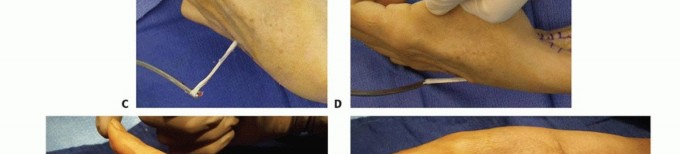
Anomalous Innervation Patterns
Surgical planning must meticulously account for anomalous innervation patterns, which can alter the clinical presentation and mask the severity of the palsy. The Martin-Gruber anastomosis involves motor fibers crossing from the median to the ulnar nerve in the proximal forearm. Depending on the specific anatomical subtype, a high ulnar nerve injury may present with unexpectedly preserved intrinsic function if those muscles are innervated by fibers traveling distally with the median nerve. Conversely, the Riche-Cannieu anastomosis involves distal connections between the deep branch of the ulnar nerve and the recurrent motor branch of the median nerve in the palm, frequently resulting in dual innervation of the adductor pollicis or the first dorsal interosseous.
Indications and Contraindications
Tendon transfers for ulnar nerve palsy are indicated when there is an irreversible loss of intrinsic muscle function that significantly impairs hand mechanics and activities of daily living. The primary reconstructive goals are fourfold: prevent MCP joint hyperextension (anti-claw procedures), restore key pinch strength (adductorplasty), correct the abducted posture of the small finger (Wartenberg deformity correction), and, in cases of high palsy, restore DIP joint flexion to the ulnar digits.
Contraindications center around the fundamental biomechanical principles of tendon transfers. A transferred tendon will not mobilize a stiff joint; therefore, full passive range of motion must be established preoperatively through aggressive hand therapy. Furthermore, the donor muscle must possess adequate strength (Medical Research Council [MRC] Grade 4 or 5), sufficient excursion, and an expendable native function to prevent unacceptable donor site morbidity.
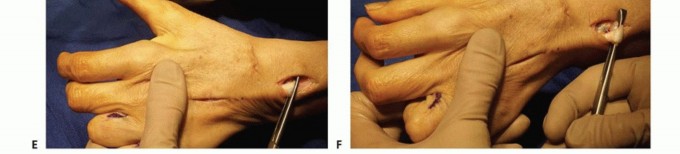
| Indication Category | Specific Clinical Scenarios |
|---|---|
| Operative Indications | Chronic ulnar nerve palsy over 12-18 months duration |
| Failure of primary nerve repair, grafting, or nerve transfers | |
| Severe clawing preventing gross grip and object acquisition | |
| Profound weakness of key pinch (positive Froment sign) | |
| Bothersome Wartenberg sign (small finger catching on pockets) | |
| Contraindications | Fixed joint contractures lacking passive range of motion |
| Donor muscle strength less than Medical Research Council Grade 4 | |
| Poor soft tissue envelope, severe scarring, or active infection | |
| Severe cognitive impairment preventing postoperative rehabilitation compliance |
Pre Operative Planning and Patient Positioning
Clinical Evaluation and Diagnostic Signs
A rigorous preoperative clinical evaluation dictates the specific modular choice of tendon transfers. The surgeon must document the presence of classic eponymous signs that highlight specific biomechanical deficits.
Froment sign becomes evident when the patient attempts a strong key pinch against resistance; due to adductor pollicis paralysis, the patient involuntarily recruits the median-innervated flexor pollicis longus (FPL), resulting in marked hyperflexion of the thumb interphalangeal joint. Jeanne sign is the concurrent hyperextension of the thumb MCP joint during key pinch, caused by the loss of the volar stabilizing effect of the adductor pollicis and the deep head of the flexor pollicis brevis.
Wartenberg sign is the persistent, involuntary abduction of the small finger. It results from the unopposed action of the extensor digiti minimi (EDM), which possesses an ulnar line of pull, acting against the paralyzed third palmar interosseous muscle.
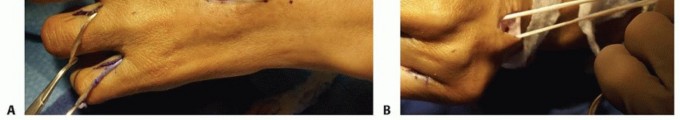
The Bouvier Test
The Bouvier test is the single most critical physical examination maneuver for surgical planning of an anti-claw tendon transfer. The examiner passively blocks the patient's MCP joints in slight flexion (eliminating the hyperextension force of the EDC) and instructs the patient to actively extend the interphalangeal joints.
If the patient can fully extend the PIP and DIP joints, the test is Bouvier positive. This indicates that the extensor mechanism (specifically the central slip) remains intact and competent. In a Bouvier positive hand, a simple MCP joint block procedure (such as a Zancolli lasso) is sufficient to correct the clawing. By preventing MCP hyperextension, the native EDC is mechanically permitted to transmit its force distally to extend the interphalangeal joints.
If the patient cannot extend the interphalangeal joints despite MCP stabilization, the test is Bouvier negative. This indicates chronic attenuation of the central slip secondary to prolonged deformity. In a Bouvier negative hand, an MCP block alone will fail; the tendon transfer must be routed distally into the lateral bands to directly provide active interphalangeal joint extension.
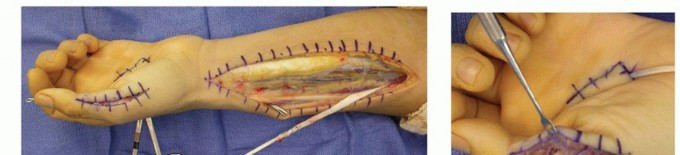
Principles of Tendon Transfer
The surgeon must strictly adhere to the classic Boyes and Brand principles of tendon transfer. The donor muscle must have a straight line of pull to maximize mechanical efficiency and minimize vector loss. It must have adequate excursion to match the recipient bed; wrist flexors and extensors typically possess 33 mm of excursion, while finger flexors possess approximately 70 mm. The transfer should ideally cross only one joint to avoid energy dissipation. Utilizing synergistic transfers (e.g., using a wrist extensor to provide finger flexion) facilitates significantly easier cortical re-education during postoperative rehabilitation.
Patient Positioning and Preparation
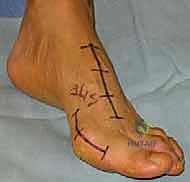
The patient is positioned supine with the operative extremity extended on a radiolucent hand table. A well-padded pneumatic tourniquet is applied to the proximal arm. Skin preparation must include the entire arm up to the axilla; this allows the surgeon to intraoperatively range the wrist and elbow to assess the resting cascade and accurately judge tendon tensioning. Loupe magnification (minimum 2.5x to 3.5x) is highly recommended for identifying the delicate structures of the extensor mechanism, lateral bands, and deep transverse metacarpal ligament.
Detailed Surgical Approach and Technique
Surgical reconstruction of the ulnar nerve deficient hand is highly modular. The surgeon must synthesize combinations of procedures to address the unique constellation of deficits in the individual patient.
Correction of Claw Deformity
The overarching goal of anti-claw transfers is to synchronize finger flexion by neutralizing MCP hyperextension and restoring interphalangeal extension.
For Bouvier positive hands, the Zancolli Lasso procedure is highly effective and carries a lower risk of over-tensioning complications. The FDS of the middle or ring finger is harvested. A transverse palmar incision is made at the level of the distal palmar crease. The A1 and proximal A2 pulleys are identified. The FDS tendon is divided at its distal insertion, withdrawn into the palm, and split longitudinally into two or four slips depending on the number of involved digits. Each slip is routed volar to the deep transverse metacarpal ligament (DTML), passed through the A1 or proximal A2 pulley from proximal to distal, folded back on itself, and sutured under appropriate tension. Tensioning is critical: with the wrist in neutral, the MCP joints should rest in 30 to 45 degrees of flexion.
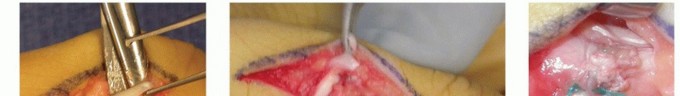
For Bouvier negative hands, a transfer inserting directly into the lateral bands is mandatory. The Modified Stiles-Bunnell procedure utilizes the FDS routed through the native lumbrical canals to insert onto the radial lateral bands of the extensor mechanism. Alternatively, the Brand Transfer utilizes the extensor carpi radialis longus (ECRL) or brevis (ECRB), extended with free tendon grafts (typically plantaris or fascia lata). The grafts are routed dorsally through the intermetacarpal spaces, passed volar to the DTML, and sutured into the lateral bands. Routing volar to the DTML is the biomechanical crux of this procedure; it creates a volar moment arm at the MCP joint to provide flexion, while the distal insertion directly provides interphalangeal extension.

Restoration of Key Pinch
Restoring adductor pollicis function is essential for powerful key pinch and stable object manipulation. The Smith-Hastings procedure is a robust adductorplasty. The ECRB is detached from its insertion at the base of the third metacarpal. A free tendon graft is often required to reach the thumb insertion. The tendon is routed volarly through the second or third intermetacarpal space to provide a transverse line of pull mimicking the adductor pollicis transverse head. It is inserted into the adductor tubercle of the proximal phalanx of the thumb.
Another excellent, single-stage option is utilizing the FDS of the ring finger, which can be routed across the palm and inserted into the adductor tubercle. This provides exceptional excursion and power without the morbidity of harvesting a free tendon graft. Tensioning is performed with the wrist in neutral and the thumb held tightly adducted against the radial aspect of the index finger middle phalanx.
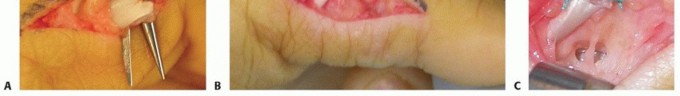
Correction of Wartenberg Deformity
Wartenberg sign can be corrected via dynamic or static means. A common dynamic transfer involves harvesting the ulnar slip of the EDM. The tendon is divided proximally, routed volar to the DTML between the ring and small fingers, and inserted into the radial collateral ligament or the radial lateral band of the small finger. This effectively redirects the EDM from an abducting force vector to an adducting force vector.
If a static correction is preferred (often in older patients or those with multiple complex transfers), a tenodesis of the radial lateral band of the small finger to the ulnar lateral band of the ring finger can be performed. The surgeon must ensure the tension holds the small finger in a neutral, adducted posture alongside the ring finger during all phases of finger flexion and extension.
Management of High Ulnar Nerve Palsy
In high ulnar nerve palsy, the patient suffers the additional deficit of absent FDP function to the ring and small fingers, resulting in absent DIP joint flexion and profound weakness in power grip. Tendon transfer for this specific deficit involves a side-to-side tenodesis in the distal forearm. The paralyzed ulnar-innervated FDP tendons of the ring and small fingers are sutured to the intact, median nerve-innervated FDP tendons of the index and middle fingers. The tension is meticulously set to recreate the normal resting cascade of the hand, where the ulnar digits are progressively more flexed than the radial digits.
Complications and Management
Tendon transfers in the hand are technically demanding, and complications frequently arise from errors in intraoperative tensioning, improper routing, or non-compliant postoperative rehabilitation. The margin of error for tensioning, particularly in lateral band transfers, is exceedingly narrow.
A transfer that is tensioned too tightly will result in a debilitating intrinsic plus deformity. If a lateral band transfer is excessively tight, the patient will develop an iatrogenic swan neck deformity, characterized by fixed MCP flexion and PIP joint hyperextension. This severely limits the patient's ability to make a full fist or grasp small objects. Conversely, a transfer tensioned too loosely will fail to correct the clawing, leaving the patient with persistent asynchronous finger motion and a "roll-up" grasp.
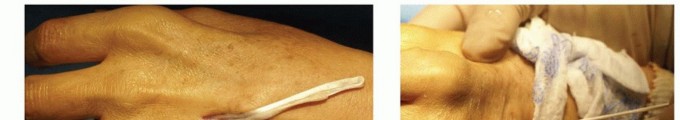
Adhesions are a ubiquitous risk in all tendon surgery. Strict adherence to atraumatic tissue handling, meticulous hemostasis, and early controlled mobilization protocols are essential to minimize restrictive scar formation. If severe adhesions occur and halt progress, surgical tenolysis may be required; however, this must be delayed for at least 6 to 12 months to allow complete scar maturation and to maximize the benefit from conservative hand therapy.
| Complication | Estimated Incidence | Prevention and Salvage Strategies |
|---|---|---|
| Tendon Adhesions | 15 to 30 percent | Atraumatic technique, early controlled mobilization. Salvage via delayed surgical tenolysis. |
| Over-tensioning (Swan Neck) | 5 to 10 percent | Careful intraoperative assessment of resting cascade. Salvage via tendon lengthening or central slip tenotomy. |
| Under-tensioning (Recurrent Claw) | 10 to 15 percent | Suture with wrist in neutral, MCPs appropriately flexed. Salvage via revision transfer or static capsulodesis. |
| Donor Site Morbidity | 5 percent | Select expendable donors. FDS harvest may cause PIP hyperextension; consider leaving one FDS slip intact to prevent this. |
| Joint Stiffness | 10 to 20 percent | Aggressive preoperative therapy to achieve full passive ROM. Postoperative dynamic extension splinting. |
Post Operative Rehabilitation Protocols
The ultimate functional success of tendon transfers for ulnar nerve palsy is equally dependent on flawless surgical execution and rigorous, specialized postoperative rehabilitation. The therapy protocol is generally divided into three distinct phases.
Phase One: Immobilization
Immediately postoperatively, the hand and forearm are immobilized in a custom thermoplastic splint or a bulky plaster dressing. The specific positioning of the splint is dictated by the transfers performed. For anti-claw transfers, a dorsal block splint is utilized. The wrist is typically placed in 15 to 30 degrees of flexion to remove tension from the volar repairs. The MCP joints are immobilized in 70 to 90 degrees of flexion. Crucially, the interphalangeal joints are left free to allow full active extension within the constraints of the dorsal block, which prevents adhesions of the extensor mechanism and lateral bands. This protective phase lasts for 3 to 4 weeks.
Phase Two: Early Mobilization
At 3 to 4 weeks, the protective splint is modified to be removable for supervised therapy sessions. Active range of motion exercises are initiated. The focus is heavily on "place and hold" exercises, where the hand therapist passively places the hand into the desired functional position (e.g., MCP flexion with IP extension) and the patient actively fires the transferred muscle to hold the posture. Cortical re-education is the primary goal during this phase. If a synergistic transfer was used (such as a wrist extensor to provide finger flexion), the patient is instructed to perform the native action of the donor muscle (extend the wrist) to facilitate neurological activation of the transfer.
Phase Three: Strengthening
At 6 to 8 weeks postoperatively, the tendon repairs have achieved sufficient tensile strength to withstand resistance. Strengthening exercises are progressively introduced, utilizing therapy putty, grip dynamometers, and functional task practice. The protective dorsal block splint is discontinued during the day but may be worn at night for an additional 2 to 4 weeks if there is a clinical tendency toward recurrent claw posturing. Full unrestricted activity is typically permitted by 10 to 12 weeks, though the surgeon should counsel the patient that maximum functional improvement and seamless cortical re-education may take up to a full year.
Summary of Key Guidelines
The foundational principles of tendon transfers for ulnar nerve palsy were established through the pioneering work of Paul Brand and Eduardo Zancolli. Brand's exhaustive biomechanical analyses elucidated the concept of the intrinsic minus hand and established the necessity of routing transfers volar to the transverse metacarpal ligament to create an effective flexion moment at the MCP joint. His work established the use of wrist extensors prolonged with free grafts as a durable, powerful solution for severe, Bouvier-negative clawing.
Zancolli revolutionized the management of the Bouvier positive hand with the introduction of the lasso procedure. By demonstrating that stabilizing the MCP joint in flexion was sufficient to allow the native extensors to straighten the interphalangeal joints, he provided a technically simpler and highly reliable alternative to lateral band insertions, significantly reducing the risk of postoperative swan neck deformities.
Contemporary literature, including extensive systematic reviews of pinch restoration, strongly supports the use of the FDS or the ECRB for adductorplasty. Studies indicate that while normal key pinch strength is rarely fully restored to pre-injury levels, patients reliably achieve a functional pinch that eliminates the Froment sign and allows for stable, powerful object manipulation. Current academic consensus emphasizes that the choice of transfer must be highly individualized, guided strictly by the Bouvier test, the availability of MRC Grade 5 donor muscles, and the specific functional deficits and occupational demands of the patient.
You Might Also Like